In critical care and respiratory therapy, accurate monitoring and timely assessment can mean the difference between stability and decline. One tool that plays a vital role in this process is the arterial line, a small catheter placed directly into an artery that allows continuous blood pressure monitoring and frequent sampling of arterial blood gases.
For respiratory therapists, understanding how arterial lines work and why they are used is essential, as this device provides crucial data that guides ventilator management, oxygen therapy, and overall patient care.
What is an Arterial Line?
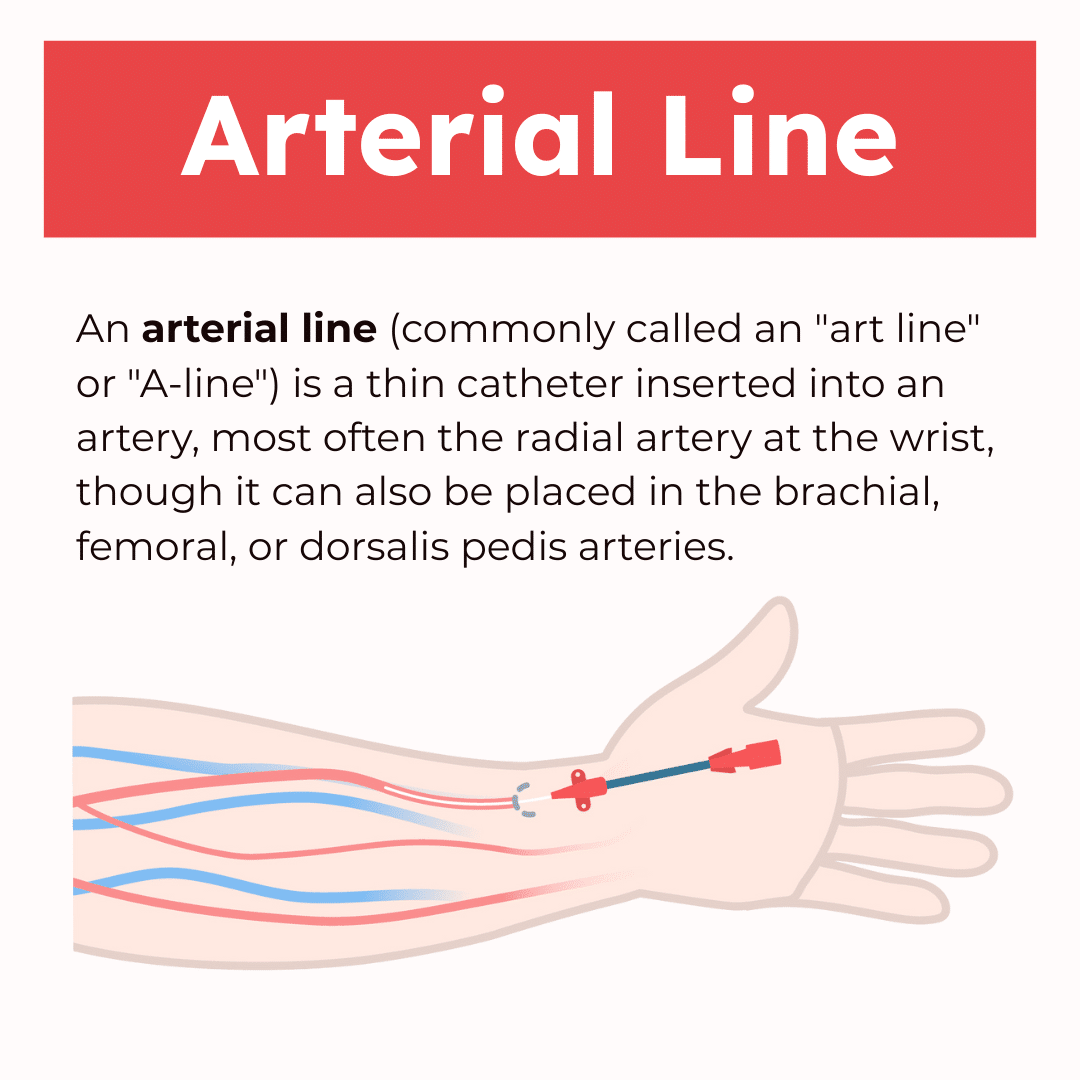
An arterial line (commonly called an “art line” or “A-line”) is a thin catheter inserted into an artery, most often the radial artery at the wrist, though it can also be placed in the brachial, femoral, or dorsalis pedis arteries. Unlike standard intravenous (IV) lines, which go into veins, arterial lines are used specifically for real-time monitoring of a patient’s blood pressure and for obtaining frequent blood samples—particularly arterial blood gases (ABGs).
Because of its ability to provide continuous and accurate data, the arterial line is an essential tool in critical care, surgery, and emergency medicine.
Why Arterial Lines are Important
Arterial lines serve two main purposes:
- Continuous Hemodynamic Monitoring: They provide beat-to-beat blood pressure readings, which are more precise than non-invasive cuff measurements. This is critical for patients who are hemodynamically unstable, receiving vasoactive medications, or undergoing major surgery.
- Frequent Arterial Sampling: Arterial blood gases (ABGs) are a cornerstone in respiratory care. Since arterial lines allow repeated sampling without repeated needle sticks, they reduce patient discomfort and provide quick access to vital data such as PaO₂, PaCO₂, and pH.
Relevance to Respiratory Therapists
For respiratory therapists (RTs), arterial lines are highly relevant in daily practice for several reasons:
- ABG Analysis: RTs often draw blood from arterial lines to assess oxygenation, ventilation, and acid-base balance. These values guide ventilator settings and oxygen therapy adjustments.
- Ventilator Management: Real-time monitoring helps evaluate how changes in ventilator modes, pressures, or FiO₂ impact a patient’s oxygenation and circulation.
- Critical Decision-Making: RTs collaborate with physicians and nurses to interpret ABG results and hemodynamic changes. An abnormal arterial blood pressure tracing or waveform may indicate complications such as hypovolemia, arrhythmias, or changes in vascular tone.
- Reduced Risk and Improved Efficiency: Since arterial punctures (radial sticks) can cause pain and vascular trauma, having an indwelling line improves efficiency and patient comfort while minimizing repeated invasive procedures.
Waveform Interpretation
An added advantage of arterial lines is the arterial pressure waveform, which provides more than just numeric blood pressure. RTs and clinicians can observe waveform characteristics to detect issues such as:
- Damped waveforms – may indicate catheter kinking, air bubbles, or clot formation.
- Overdamped or underdamped readings – can distort blood pressure accuracy.
- Loss of dicrotic notch – may suggest line obstruction or improper transducer setup.
Note: Respiratory therapists who understand these nuances can identify errors and ensure reliable monitoring, especially when managing critically ill patients.
Risks and Considerations
Though invaluable, arterial lines are not without risks. Possible complications include:
- Infection at the insertion site
- Bleeding or hematoma
- Thrombosis and distal ischemia
- Nerve injury in rare cases
Note: Because of these risks, strict aseptic technique, careful monitoring, and regular site assessment are required.
The Role of Arterial Lines in Respiratory Care
In the broader scope of respiratory care, arterial lines represent a bridge between patient assessment and therapeutic intervention. They allow respiratory therapists to:
- Evaluate therapy effectiveness in real time (oxygenation, ventilation, circulation).
- Guide ventilator weaning by trending ABG results and hemodynamic stability.
- Participate in multidisciplinary care by providing essential input on ventilator settings, oxygen therapy, and patient stability.
Note: Ultimately, arterial lines empower RTs to make evidence-based decisions that directly impact patient outcomes in critical care and beyond.
Arterial Line Practice Questions
1. What is an arterial line?
A thin catheter inserted directly into an artery for monitoring and blood sampling
2. What are the primary uses of an arterial line?
To monitor blood pressure continuously, obtain arterial blood gas samples, and allow frequent blood draws
3. What are the most common sites for arterial line placement?
Radial, brachial, and femoral arteries
4. What are the advantages of placing an arterial line in the radial artery?
Easy access, accurate readings, good collateral circulation, easy bleeding control, and better mobility for the patient
5. What are the disadvantages of radial artery arterial lines?
Small diameter, difficult insertion, and risk of thrombosis or nerve damage
6. What are the benefits of a brachial arterial line?
Larger diameter and relatively easy bleeding control
7. What are the disadvantages of a brachial artery line?
Immobilization of the limb, risk of thrombosis, and limited collateral circulation
8. What is a major risk associated with femoral artery lines?
Higher risk of infection and more difficult bleeding control
9. When is femoral arterial line placement typically indicated?
During emergencies when other sites are not feasible
10. What test must be performed before inserting a radial arterial line?
Modified Allen’s test
11. What is the purpose of the modified Allen’s test?
To confirm adequate collateral circulation between the radial and ulnar arteries
12. Describe the steps of the modified Allen’s test.
Elevate the hand, have the patient make a fist for 30 seconds, compress both arteries, release pressure on the ulnar artery and observe for return of color and warmth
13. What does a positive Allen’s test indicate?
Return of color and warmth to the hand, confirming collateral circulation
14. What does a negative Allen’s test indicate?
The hand remains pale or cold, suggesting inadequate collateral circulation
15. What is the dicrotic notch seen on an arterial line waveform?
It represents the closure of the aortic valve
16. When should an arterial line be zeroed or calibrated?
Every shift, every 4 hours, after blood draws, and as needed (PRN)
17. Why is it important to calibrate an arterial line?
To ensure accurate blood pressure measurements
18. How should arterial line readings be verified for accuracy?
By comparing the arterial line reading with a noninvasive blood pressure (NIBP) reading
19. What discrepancy between Art line and NIBP readings is considered inaccurate?
A difference greater than 20 mmHg
20. What can be used as a backup if the arterial line fails?
A noninvasive blood pressure cuff (NIBP)
21. What should be included in a neurovascular assessment?
Pain, pulses, pallor, paresthesia, and paralysis
22. How often should the saline bag and pressure tubing be changed?
Saline bag: daily; tubing: every 72 hours
23. What are the steps for drawing blood from an arterial line?
Waste 10 mL, use a blunt cannula, turn stopcock off to saline bag, draw in correct tube order, flush and re-zero the system
24. What is the correct order of blood tube collection from an arterial line?
Tube without additives, tube with additives, coagulation profile tubes, then ABG syringe
25. What are the indications for removing an arterial line?
Discontinuation of pressure monitoring, decreased need for blood sampling, infection, bleeding, or line malfunction
26. What steps should be followed during arterial line removal?
Confirm physician order, review coagulation labs, maintain sterility, apply pressure for at least 15 minutes, and apply a pressure dressing
27. After removing an arterial line, what should you assess?
Bleeding, bruising, hematoma, and the 5 P’s: pain, pulses, pallor, paresthesia, and paralysis
28. What is arterial pressure monitoring?
A system that reads real-time blood pressure via a transducer connected to an arterial catheter
29. What are some clinical indications for placing an arterial line?
Frequent ABG sampling, severe hypo/hypertension, respiratory failure, and vasoactive medication administration
30. Can you infuse fluids or medications through an arterial line?
No — only flushes (usually heparinized saline) are used to keep the line patent
31. Which artery is most commonly used for arterial line placement?
Radial artery
32. Why is the femoral artery less preferred for arterial line placement?
It carries a higher risk of infection and complications due to proximity to groin structures
33. What is the proper angle for arterial line insertion?
15–30 degrees with the needle bevel facing upward
34. What is the general technique for inserting an arterial line?
Insert needle into artery, thread guidewire, remove needle, advance catheter, remove guidewire, secure line, connect to transducer system
35. Why must the transducer system of an arterial line be zeroed at the level of the heart?
To ensure pressure readings are accurate relative to atmospheric pressure
36. What position should the transducer be placed in for accurate readings?
At the level of the phlebostatic axis (4th intercostal space, mid-axillary line)
37. What is the purpose of the pressure bag attached to an arterial line?
To maintain line patency by applying continuous pressure (typically 300 mmHg) to the saline flush
38. What could cause dampening or flattening of the arterial waveform?
Air bubbles, clots, loose connections, or kinked catheter
39. What should you do if the arterial waveform becomes dampened?
Check the line for air, clots, or kinks, flush the line, and troubleshoot the transducer setup
40. What is indicated if there is sudden loss of waveform on an arterial monitor?
Disconnection, clotting, or catheter displacement
41. What are three common complications associated with arterial line insertion?
Hematoma, arterial spasm, and compartment syndrome
42. What is compartment syndrome and why is it a concern with arterial lines?
A potentially life-threatening condition where pressure builds in the limbs or abdomen, compromising tissue perfusion
43. What are the key steps when drawing blood from an arterial line?
Turn the stopcock toward the flush bag, waste 3–5 mL, draw 2–2.5 mL sample, flush the line, and return stopcock to original position
44. What equipment is essential for proper arterial line setup?
A transducer, transducer holder, flush system, noncompliant tubing, and electronic monitor
45. Where should the transducer be leveled to ensure accurate pressure readings?
At the fourth intercostal space, mid-axillary line (phlebostatic axis)
46. What should a normal arterial pressure waveform include?
A sharp upstroke, a visible dicrotic notch, and a gradual downstroke
47. What does the dicrotic notch represent on an arterial waveform?
Closure of the aortic valve
48. What does a normal arterial pressure reading indicate?
A pressure of around 120/80 mmHg
49. What arterial pressure reading suggests hypertension?
A reading equal to or greater than 160/90 mmHg
50. What arterial pressure reading is considered hypotension?
A reading at or below 90/60 mmHg
51. What could a dampened dicrotic notch or lost waveform indicate?
Line occlusion, air bubbles, catheter kinking, or transducer error
52. What is pulse pressure and what is its normal range?
The difference between systolic and diastolic pressure, normally 30–40 mmHg
53. What does pulse pressure indicate?
It reflects stroke volume and arterial compliance
54. What is mean arterial pressure (MAP) and why is it important?
An average pressure pushing blood through systemic circulation; it reflects tissue perfusion
55. What is the formula to calculate MAP?
MAP = [Systolic + (2 × Diastolic)] ÷ 3
56. What are three complications of arterial pressure monitoring?
Ischemia, hemorrhage, and infection
57. What is the proper analyzer procedure before processing a blood sample?
Verify patient and specimen, check order and time, mix sample by rolling, discard drops, introduce sample, confirm readings
58. What is an angiocath?
An intravenous catheter with a plastic sheath used for vascular access
59. What is the VAMP system and why is it used?
Venous Arterial blood Management Protection system designed to reduce blood waste and needle stick injuries
60. What is a major risk if the arterial line is not properly primed?
Air embolism
61. What are some common indications for placing an arterial line?
Frequent ABGs, hemodynamic monitoring, radiologic procedures, or use of vasoactive drugs
62. What equipment is required for arterial line placement?
Catheter, transducer, noncompliant tubing with stopcocks, flush system, and monitor
63. What are common issues that affect pressure monitoring accuracy?
Improper zeroing, zero drift, and inadequate dynamic response
64. What is a square wave (fast flush) test and what does it evaluate?
A test of system damping and resonance performed by flushing the line and observing waveform oscillation
65. How often should the square wave test be performed?
Every 8 hours or after major events like blood draws or tubing changes
66. What does overdamping of an arterial line waveform suggest?
A kinked catheter, air bubbles, or excessive stopcocks that reduce waveform responsiveness
67. What causes underdamping in an arterial waveform?
Long tubing, excessive inotropy, or low resistance in the monitoring system
68. What is the ideal site for arterial line insertion?
An artery with strong collateral circulation to preserve distal perfusion if thrombosis occurs
69. What are the five most common arterial sites for line placement?
Radial, femoral, axillary, dorsalis pedis, and brachial arteries
70. What might make radial artery cannulation difficult in some patients?
Shock, high-dose vasopressors, or non-palpable pulses
71. What is the anatomical origin of the radial artery?
It is one of the two terminal branches of the brachial artery
72. How can hand ischemia be prevented prior to radial artery catheterization?
Avoid radial access in high-risk patients and perform thorough clinical evaluation of hand circulation
73. How should the hand be positioned for radial arterial line insertion?
30–60 degrees of dorsiflexion using a gauze roll or wrist support while avoiding hyperabduction of the thumb
74. What is the anatomical course of the dorsalis pedis artery?
It runs superficially along the dorsum of the foot from the ankle to the great toe, just lateral to the extensor hallucis longus tendon
75. Where is the brachial artery typically cannulated?
In the bicipital groove proximal to the antecubital fossa, an area lacking collateral circulation
76. What care should follow brachial artery cannulation?
Keep the elbow fully extended and regularly assess distal circulation; remove the catheter if perfusion is compromised
77. What are two common reasons for failed femoral artery cannulation?
Severe atherosclerosis and prior femoral vascular procedures
78. What serious complications are associated with femoral artery cannulation?
Retroperitoneal bleeding and intra-abdominal perforation, often due to poor technique or anatomical variations
79. What is a major risk of axillary artery cannulation?
Cerebral air embolism, especially from right-sided insertion due to proximity to cerebral circulation
80. What flushing technique is recommended for axillary cannulation?
Manual, low-pressure flushing using small fluid volumes
81. What is a contraindication to axillary artery cannulation?
Coagulopathy
82. Which arterial cannulation sites are most commonly associated with thrombosis?
Radial and dorsalis pedis arteries
83. When does arterial thrombosis most commonly occur?
After catheter removal, especially in women
84. What is diagnostic blood loss (DBL)?
Cumulative patient blood loss from frequent sampling, including the 3–5 mL wasted with each draw
85. How can diagnostic blood loss be minimized?
Use reservoir sampling systems, continuous monitoring, point-of-care testing, and micro-sample collection
86. What are some non-infectious complications of arterial cannulation?
Pseudoaneurysm, hematoma, hemorrhage, catheter embolization, HIT, and nerve injury
87. What typically causes infection related to arterial lines?
Skin flora invading the tract, stagnant flush systems, and contaminated tubing used for multiple samples
88. How often should arterial catheters be replaced?
Every 7 days if still needed; use guidewire exchange only for malfunctioning or damaged catheters
89. What is more accurate for blood pressure measurement: arterial lines or non-invasive BP (NIBP)?
Arterial lines provide more accurate readings
90. Why are arterial lines preferred for monitoring blood pressure in critical patients?
They offer continuous, beat-to-beat monitoring and allow easy access for blood draws
91. How common are major complications from arterial line placement?
They occur in fewer than 1% of cases
92. What type of surgery might warrant arterial line access for frequent lab draws?
Parathyroidectomy, due to the need for repeated calcium level monitoring
93. What are the two most common sites for arterial line placement?
Radial and femoral arteries
94. Why is the radial artery the most common site for arterial cannulation?
It’s superficial, anatomically consistent, easily accessible, and has fewer complications
95. Why is the femoral artery the second most common site for arterial line placement?
It is larger, easier to palpate, and has a lower risk of thrombosis or accidental dislodgement
96. Why is it important to level the transducer when setting up an arterial line?
To ensure accurate pressure readings; it must be aligned with the phlebostatic axis at the fourth intercostal space, mid-axillary line
97. What happens if the transducer is placed too high above the phlebostatic axis?
It will result in falsely low blood pressure readings
98. What happens if the transducer is placed too low below the phlebostatic axis?
It will result in falsely high blood pressure readings
99. What does a dampened arterial waveform indicate?
Possible clot, air bubble, kinked catheter, or loose connection causing inaccurate pressure transmission
100. How can you confirm the accuracy of an arterial line waveform?
By performing a square wave (fast flush) test and evaluating for a proper oscillation pattern
Final Thoughts
An arterial line is more than just a monitoring tool—it is a vital lifeline for patients requiring intensive respiratory and hemodynamic support. For respiratory therapists, understanding arterial lines is key to patient assessment, ventilator management, and collaborative decision-making in critical care.
By integrating real-time monitoring with ABG analysis, RTs can play a crucial role in optimizing care for some of the sickest and most vulnerable patients.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Williams C, Pasrija D, Pierre L, et al. Arterial Lines. [Updated 2025 Mar 23]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025.