Aspiration is a significant clinical concern in respiratory care that occurs when foreign material enters the lower respiratory tract. This material may include oropharyngeal secretions, gastric contents, food, or liquids.
While small amounts may be tolerated in healthy individuals, aspiration in vulnerable patients can lead to serious complications such as infection, inflammation, and respiratory failure.
Because it intersects with airway management, mechanical ventilation, nutrition, and patient assessment, understanding aspiration is essential for safe and effective clinical practice across a wide range of healthcare settings.
What Is Aspiration?
Aspiration refers to the inhalation of substances into the airway and lungs that are not intended to be there. These substances can vary in composition and severity of impact. For example, aspirating sterile water may cause minimal harm, while aspirating gastric acid or bacteria-laden secretions can result in significant lung injury.
In clinical practice, aspiration is not viewed as a single disease but rather as a pathophysiologic event that can lead to multiple pulmonary complications. The severity depends on the volume and type of aspirated material, as well as the patient’s underlying health and ability to clear the airway.
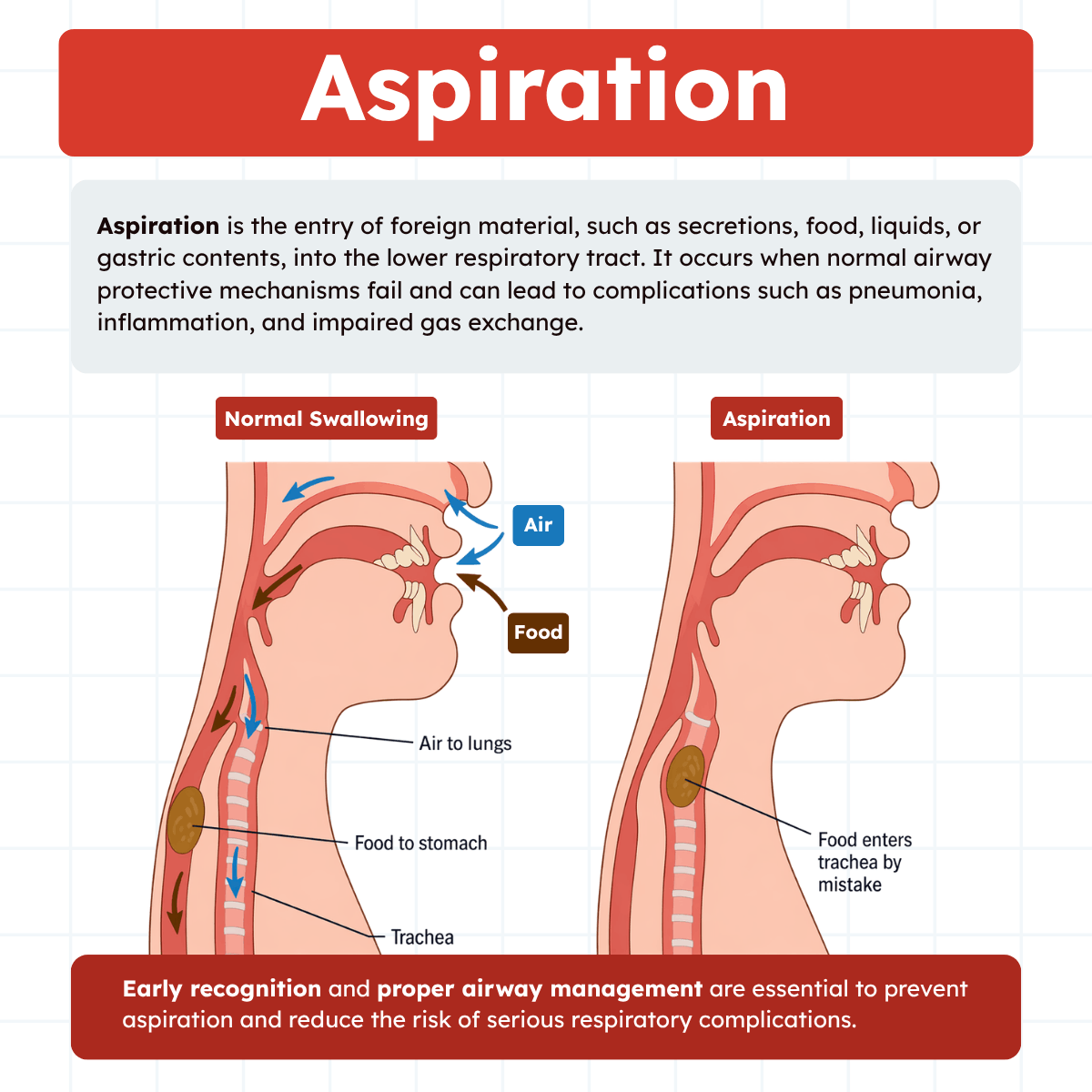
Pathophysiology of Aspiration
Normal Airway Protection
Under normal conditions, the body has several defense mechanisms that prevent aspiration:
- The epiglottis directs food and liquids away from the airway during swallowing
- The vocal cords close to block entry into the trachea
- The cough reflex expels foreign material
- Coordinated swallowing prevents misdirection of contents
Note: These mechanisms work together to maintain separation between the respiratory and digestive systems.
Failure of Protective Mechanisms
Aspiration occurs when these protective mechanisms become impaired. This may happen due to:
- Neurological dysfunction that affects swallowing or reflexes
- Sedation or anesthesia that suppresses airway protection
- Mechanical disruption from airway devices
- Fatigue or weakness that reduces cough effectiveness
Note: When these defenses fail, material can enter the trachea and travel into the bronchi and alveoli. Once in the lungs, the material may obstruct airflow, introduce pathogens, or trigger an inflammatory response.
Silent Aspiration
One of the most concerning aspects of aspiration is that it may occur without obvious signs. This is known as silent aspiration. In these cases, the patient does not cough or show immediate distress, allowing harmful material to accumulate in the lungs unnoticed. Silent aspiration is especially common in patients with neurological impairment or reduced consciousness.
Types of Aspirated Material
The clinical consequences of aspiration depend heavily on what is aspirated. Common categories include:
- Oropharyngeal Secretions: These often contain bacteria from the oral cavity. When aspirated, they can lead to infections such as pneumonia.
- Gastric Contents: Gastric fluid is highly acidic and can cause chemical injury to lung tissue. This often results in inflammation and impaired gas exchange.
- Food and Liquids: Solid or liquid substances can obstruct the airway or contribute to infection if bacteria are present.
- Blood or Foreign Bodies: Less common but potentially severe, these can cause airway obstruction or localized lung injury.
Aspiration and Airway Management
Airway management is central to both preventing and contributing to aspiration risk. The type of airway device and how it is managed play a major role in patient outcomes.
Endotracheal Tubes
Endotracheal intubation is considered the most effective method for protecting the airway. When properly positioned and inflated, the cuff of the tube creates a seal within the trachea that helps prevent foreign material from entering the lungs.
However, this protection is not absolute. Microaspiration can still occur when small amounts of secretions leak around the cuff. This is especially likely if cuff pressure is inadequate or if secretions accumulate above the cuff.
Complications of Artificial Airways
While endotracheal tubes provide airway protection, they also introduce new risks:
- Impaired closure of the vocal cords
- Reduced effectiveness of the cough reflex
- Increased production and retention of secretions
- Potential for secretions to track along the tube into the lungs
Note: These factors can increase the likelihood of aspiration if not carefully managed.
Supraglottic Airway Devices
Devices such as laryngeal mask airways provide ventilation support but do not offer full protection against aspiration. They sit above the vocal cords and do not create a seal within the trachea.
Because of this limitation, they are generally avoided in patients who are at high risk for aspiration, such as those with a full stomach or active vomiting.
Aspiration in Mechanically Ventilated Patients
Patients receiving mechanical ventilation are at increased risk for aspiration due to several factors. The presence of an artificial airway alters normal defense mechanisms, while sedation and critical illness further impair protective reflexes.
Ventilator-Associated Pneumonia (VAP)
Aspiration plays a key role in the development of ventilator-associated pneumonia. This condition occurs when bacteria from the oral cavity or gastrointestinal tract enter the lungs and cause infection.
Microaspiration of contaminated secretions is one of the primary mechanisms behind VAP. Even with an endotracheal tube in place, secretions can accumulate above the cuff and eventually leak into the lower airway.
Contributing Factors
Several factors increase aspiration risk in ventilated patients:
- Supine positioning
- Inadequate cuff pressure
- Poor oral hygiene
- Accumulation of secretions
- Prolonged mechanical ventilation
Prevention Strategies
Reducing aspiration risk is a key component of ventilator care. Common strategies include:
- Maintaining appropriate cuff pressure
- Elevating the head of the bed
- Performing regular oral care
- Suctioning secretions as needed
- Using specialized tubes that allow removal of subglottic secretions
Note: These interventions help minimize the entry of harmful material into the lungs and reduce the risk of infection.
Aspiration in Enteral Nutrition
Aspiration is a major concern in patients receiving enteral nutrition, particularly in critical care settings. Tube feeding introduces nutrients directly into the gastrointestinal tract, but it also creates the potential for regurgitation and aspiration.
Mechanism of Aspiration During Feeding
Aspiration can occur when gastric contents move backward into the esophagus and are then inhaled into the lungs. This is more likely when normal swallowing and airway protection are impaired.
Risk Factors
Patients receiving enteral nutrition may be at higher risk due to:
- Reduced level of consciousness
- Impaired swallowing function
- Delayed gastric emptying
- Improper placement of the feeding tube
- Lying flat during feeding
Prevention Measures
To reduce aspiration risk during enteral feeding, clinicians often:
- Elevate the head of the bed to at least 30 degrees
- Verify proper placement of the feeding tube
- Monitor gastric residual volumes when indicated
- Consider post-pyloric feeding in high-risk patients
Note: These measures are designed to minimize reflux and prevent material from entering the airway.
Clinical Consequences of Aspiration
Aspiration can lead to a range of pulmonary complications, depending on the nature and severity of the event.
Aspiration Pneumonia
Aspiration pneumonia occurs when bacteria enter the lungs and cause infection. It is more common in patients with impaired swallowing or chronic aspiration.
Symptoms may include:
- Fever
- Cough
- Increased sputum production
- Shortness of breath
- Hypoxemia
Note: This condition often requires antibiotic therapy and supportive care.
Chemical Pneumonitis
Chemical pneumonitis results from the aspiration of irritating substances, most commonly gastric acid. This leads to inflammation of the lung tissue and can impair oxygenation.
Patients may develop:
- Rapid onset of respiratory distress
- Decreased lung compliance
- Hypoxemia
- Diffuse infiltrates on imaging
Note: Management typically focuses on supportive care and maintaining adequate oxygenation.
Risk Factors for Aspiration
Aspiration risk is influenced by a combination of patient-related conditions and clinical circumstances. Identifying these factors early allows clinicians to implement preventive strategies and reduce complications.
Neurologic and Neuromuscular Conditions
Patients with neurologic impairment are among the highest risk groups. Conditions such as stroke, traumatic brain injury, amyotrophic lateral sclerosis, and muscular dystrophy can disrupt the coordination of swallowing and weaken the cough reflex. This leads to an inability to protect the airway effectively.
Dysphagia is a common finding in these patients and is a major contributor to chronic aspiration. Even small amounts of aspirated material over time can result in recurrent infections and progressive lung damage.
Reduced Level of Consciousness
Any condition that decreases alertness can impair airway protection. This includes sedation, anesthesia, drug overdose, and coma. When consciousness is reduced, protective reflexes such as coughing and gagging are diminished or absent.
These patients may not respond to secretions, regurgitated material, or foreign bodies entering the airway, making aspiration more likely and often more severe.
Gastrointestinal Factors
Conditions affecting the gastrointestinal system can increase the risk of aspiration. These include:
- Gastroesophageal reflux
- Delayed gastric emptying
- Vomiting
- Increased intra-abdominal pressure
Note: When gastric contents move upward into the esophagus, they may be aspirated into the lungs, especially if the patient is lying flat or has impaired airway reflexes.
Medical Interventions
Certain medical procedures and therapies can increase aspiration risk if not managed properly. These include:
- Endotracheal intubation
- Enteral feeding
- Use of airway adjuncts
- Mechanical ventilation
Note: While these interventions are often necessary, they require careful monitoring to minimize complications.
Aspiration in Emergency Situations
Aspiration is a major concern during emergency care, particularly in situations where airway control is compromised or delayed.
Cardiopulmonary Resuscitation (CPR)
During resuscitation efforts, patients are at high risk for aspiration due to vomiting or regurgitation. Gastric contents can enter the airway if protective reflexes are absent.
Rapid airway management is essential in these cases. Establishing a definitive airway helps reduce the risk of aspiration and allows for better control of ventilation.
Trauma and Acute Illness
Patients with trauma or acute medical conditions may have altered consciousness, active bleeding, or compromised airway anatomy. These factors increase the likelihood of aspiration.
In such scenarios, clinicians must prioritize airway protection and be prepared to suction secretions or perform advanced airway procedures as needed.
Aspiration and Patient Assessment
Effective prevention of aspiration begins with thorough patient assessment. Respiratory therapists and other clinicians must evaluate multiple factors that influence airway protection.
Level of Consciousness
Assessing whether a patient is alert, responsive, or unresponsive provides immediate insight into aspiration risk. Patients who are not fully conscious are less able to protect their airway.
Swallowing Ability
Evaluating swallowing function is critical, especially before initiating oral intake. Signs of impaired swallowing include coughing during meals, drooling, or difficulty managing secretions.
Gag and Cough Reflexes
The presence and strength of protective reflexes are key indicators of airway protection. A weak or absent cough reflex increases the risk of aspiration.
Secretion Management
Patients who cannot effectively clear secretions are at higher risk. This may be due to weakness, fatigue, or underlying disease.
Risk of Vomiting or Reflux
Clinicians should consider whether the patient has conditions that increase the likelihood of regurgitation. This includes recent feeding, gastrointestinal disorders, or certain medications.
Prevention and Clinical Management
Aspiration is often preventable with proper clinical practices. Prevention strategies focus on maintaining airway protection, reducing exposure to risk factors, and intervening early when problems arise.
Patient Positioning
Positioning plays a major role in aspiration prevention. Elevating the head of the bed helps reduce the risk of gastric contents moving into the airway. This is especially important for patients receiving enteral nutrition or mechanical ventilation.
Airway Maintenance
Maintaining a clear airway is essential. This includes:
- Regular suctioning of secretions
- Ensuring proper placement of airway devices
- Monitoring for signs of obstruction
Note: Prompt removal of secretions reduces the likelihood of aspiration and improves ventilation.
Cuff Pressure Management
For patients with endotracheal tubes, maintaining appropriate cuff pressure is critical. If the pressure is too low, secretions may leak around the cuff. If it is too high, it can cause tracheal injury. Routine monitoring helps ensure an adequate seal while minimizing complications.
Oral Care
Oral hygiene reduces the bacterial load in the mouth, which lowers the risk of infection if aspiration occurs. Regular oral care is a standard component of ventilator-associated pneumonia prevention protocols.
Feeding Precautions
When providing enteral nutrition, clinicians should:
- Verify correct tube placement
- Avoid overfeeding
- Monitor tolerance to feeding
- Use appropriate positioning
Note: These steps help minimize the risk of regurgitation and aspiration.
Swallowing Assessment
Before allowing oral intake, patients should be evaluated for their ability to swallow safely. This may involve bedside assessments or formal studies conducted by speech-language specialists.
Aspiration in Special Populations
Aspiration affects different patient populations in unique ways, requiring tailored approaches to prevention and management.
Neonates
In newborns, aspiration can occur during or before birth. One example is meconium aspiration syndrome, in which meconium enters the lungs and causes airway obstruction and inflammation.
This condition can impair oxygenation and may require respiratory support.
Elderly Patients
Older adults often have reduced swallowing function, weaker cough reflexes, and multiple comorbidities. These factors increase the risk of aspiration and its complications. Careful assessment and preventive measures are essential in this population.
Patients With Chronic Illness
Individuals with chronic respiratory or neurologic diseases are at ongoing risk for aspiration. Long-term management focuses on minimizing exposure to risk factors and monitoring for early signs of complications.
Clinical Implications in Respiratory Care
Aspiration is a central consideration in many aspects of respiratory therapy. It influences decisions related to airway management, ventilator care, and patient safety.
Airway Device Selection
Choosing the appropriate airway device is critical. Endotracheal tubes provide the highest level of protection, while supraglottic devices may be suitable only in low-risk situations.
Timing of Extubation
Before removing an endotracheal tube, clinicians must ensure that the patient can protect their airway. This includes the ability to cough, swallow, and manage secretions effectively. Premature extubation increases the risk of aspiration and may lead to respiratory failure.
Secretion Clearance
Effective clearance of secretions is a key component of care. Techniques such as suctioning and airway clearance therapy help reduce aspiration risk and improve lung function.
Aspiration Practice Questions
1. What is aspiration in respiratory care?
Aspiration is the entry of foreign material into the lower respiratory tract.
2. What types of substances are commonly aspirated?
Oropharyngeal secretions, gastric contents, food, and liquids.
3. What is the primary danger of aspiration?
It can lead to infection, inflammation, and impaired gas exchange.
4. What structures normally prevent aspiration?
The epiglottis, vocal cords, and cough reflex.
5. What happens when airway protective mechanisms fail?
Foreign material can enter the trachea and lungs.
6. What is silent aspiration?
Aspiration that occurs without coughing or obvious symptoms.
7. Why is silent aspiration dangerous?
It allows harmful material to accumulate in the lungs unnoticed.
8. What is microaspiration?
Small amounts of secretions leaking into the lower airway, often around an endotracheal tube cuff.
9. What is a major complication of microaspiration in ventilated patients?
Ventilator-associated pneumonia (VAP)
10. How does an endotracheal tube help prevent aspiration?
Its cuff creates a seal in the trachea to block foreign material.
11. What happens if cuff pressure is too low?
Secretions can leak around the cuff and be aspirated.
12. Why can artificial airways increase aspiration risk?
They impair glottic closure and promote secretion buildup.
13. What is a limitation of laryngeal mask airways (LMAs)?
They do not fully protect against aspiration.
14. When should LMAs be avoided?
In patients with a full stomach or high aspiration risk.
15. How does aspiration contribute to ventilator-associated pneumonia?
By introducing bacteria into the lungs from secretions.
16. What position increases aspiration risk in ventilated patients?
Supine positioning
17. What is a key prevention strategy for aspiration in ventilated patients?
Elevating the head of the bed.
18. Why is oral hygiene important in preventing aspiration complications?
It reduces bacterial load that can be aspirated.
19. What role does suctioning play in aspiration prevention?
It removes secretions that could be aspirated.
20. Why are critically ill patients at higher risk for aspiration?
They often have impaired consciousness and weakened reflexes.
21. How can enteral feeding increase aspiration risk?
It can lead to regurgitation of gastric contents.
22. What is a common complication of aspiration during tube feeding?
Pulmonary aspiration leading to pneumonia.
23. What head-of-bed angle is recommended to reduce aspiration risk?
At least 30 degrees.
24. What is chemical pneumonitis?
Inflammation of the lungs caused by aspirating irritating substances like gastric acid.
25. What is aspiration pneumonia?
A lung infection caused by inhaling bacteria-containing material.
26. What is the primary difference between aspiration pneumonia and chemical pneumonitis?
Aspiration pneumonia involves infection, while chemical pneumonitis is inflammation from irritants.
27. What type of aspirated material is most likely to cause chemical pneumonitis?
Gastric acid
28. How does aspiration affect gas exchange in the lungs?
It disrupts alveolar function and reduces oxygenation.
29. What is a common symptom of aspiration pneumonia?
Fever
30. What respiratory symptom may indicate aspiration has occurred?
Shortness of breath
31. Why is delayed gastric emptying a risk factor for aspiration?
It increases the likelihood of regurgitation.
32. How does reduced gag reflex contribute to aspiration risk?
It prevents effective airway protection.
33. What neurological condition can increase aspiration risk due to dysphagia?
Stroke
34. How does sedation increase the risk of aspiration?
It suppresses protective airway reflexes.
35. What is the role of the cough reflex in preventing aspiration?
It expels foreign material from the airway.
36. What may happen if aspirated material obstructs the airway?
Airflow can be partially or completely blocked.
37. What is one sign of impaired swallowing?
Coughing during meals.
38. Why must swallowing ability be assessed before oral feeding?
To ensure the patient can protect their airway.
39. What is a risk of premature extubation?
Aspiration due to inadequate airway protection.
40. What must a patient demonstrate before extubation?
Ability to cough and manage secretions.
41. How can improper feeding tube placement increase aspiration risk?
It may deliver feeding into the wrong location.
42. What is a benefit of post-pyloric feeding?
It reduces the risk of gastric aspiration.
43. Why is monitoring gastric residual volume important?
It helps assess feeding tolerance and risk of regurgitation.
44. What condition in neonates is caused by aspiration of meconium?
Meconium aspiration syndrome
45. What is a key feature of meconium aspiration syndrome?
Airway obstruction
46. How can aspiration lead to pulmonary hypertension in neonates?
Through inflammation and hypoxia affecting pulmonary vessels.
47. Why are elderly patients at increased risk for aspiration?
They often have weaker swallowing and cough reflexes.
48. What is a common cause of chronic aspiration?
Neuromuscular disease
49. What is the priority when aspiration is suspected in an unconscious patient?
Suction the airway immediately.
50. Why is airway protection a priority during emergency care?
To prevent aspiration and maintain ventilation.
51. What is the role of the epiglottis during swallowing?
It directs food and liquids away from the airway.
52. How do the vocal cords help prevent aspiration?
They close to block entry into the trachea.
53. What can happen if secretions accumulate above an endotracheal tube cuff?
They may leak into the lower airway and be aspirated.
54. What type of aspiration involves small, repeated amounts of material?
Chronic aspiration
55. What is a potential outcome of chronic aspiration?
Recurrent respiratory infections.
56. Why are comatose patients at high risk for aspiration?
They lack protective airway reflexes.
57. What is one clinical sign that may suggest aspiration has occurred?
Sudden onset of hypoxemia.
58. How can vomiting increase aspiration risk?
It introduces gastric contents into the airway.
59. What is the function of suctioning in airway management?
To remove secretions and prevent obstruction or aspiration.
60. What is a potential complication of aspirating food particles?
Airway obstruction
61. How does impaired cough strength affect aspiration risk?
It reduces the ability to clear aspirated material.
62. What is a common reason for increased secretion production in ventilated patients?
Irritation from the artificial airway.
63. What should be checked to ensure an endotracheal tube is preventing aspiration?
Cuff pressure
64. Why is patient positioning important during feeding?
It reduces the likelihood of regurgitation.
65. What is one reason mechanical ventilation increases aspiration risk?
It alters normal airway defenses.
66. What is a key goal of aspiration prevention strategies?
To keep foreign material out of the lungs.
67. What is the relationship between aspiration and hypoxemia?
Aspiration can impair oxygen exchange and cause hypoxemia.
68. What type of lung injury can result from aspiration of irritants?
Inflammatory lung injury
69. What is one reason clinicians monitor patients closely after extubation?
To detect signs of aspiration.
70. What role does oral care play in preventing aspiration-related infections?
It reduces harmful bacteria in the mouth.
71. What is a common cause of aspiration during anesthesia?
Loss of airway reflexes.
72. Why are patients with reflux at higher risk for aspiration?
Gastric contents can move into the airway.
73. What is one method to reduce aspiration risk during mechanical ventilation?
Elevating the head of the bed.
74. What is a possible outcome if aspiration is not managed promptly?
Respiratory failure
75. Why is early recognition of aspiration important?
It allows for timely intervention to prevent complications.
76. What is the primary goal of aspiration prevention in respiratory care?
To protect the airway and prevent foreign material from entering the lungs.
77. How does fatigue contribute to aspiration risk?
It weakens the cough and swallowing mechanisms.
78. What is one complication of aspiration that affects lung compliance?
Chemical pneumonitis
79. What is the effect of aspiration on alveoli?
It can cause inflammation and impair gas exchange.
80. What bedside observation may suggest poor secretion control?
Pooling of secretions in the mouth.
81. Why are patients with muscular dystrophy at risk for aspiration?
They have weakened respiratory and swallowing muscles.
82. What is the impact of aspiration on oxygen saturation levels?
It can cause a decrease in oxygen saturation.
83. What intervention helps remove secretions above the endotracheal cuff?
Subglottic suctioning
84. What is one reason patients with ALS are prone to aspiration?
Progressive loss of muscle control affects swallowing.
85. What is a clinical sign of aspiration during feeding?
Coughing or choking
86. Why should feeding be paused if aspiration is suspected?
To prevent further entry of material into the airway.
87. What is the role of the respiratory therapist in aspiration prevention?
To assess risk and manage airway protection.
88. What type of feeding reduces aspiration risk in high-risk patients?
Post-pyloric feeding
89. What is a key feature of aspiration-related lung injury?
Inflammation of lung tissue.
90. What is a common cause of aspiration in hospitalized patients?
Impaired consciousness
91. What is the relationship between aspiration and airway obstruction?
Aspirated material can block airflow.
92. What is one indication for immediate suctioning?
Visible secretions in a patient unable to clear them.
93. What is the effect of regurgitation on aspiration risk?
It increases the chance of gastric contents entering the lungs.
94. What is a potential complication of repeated aspiration events?
Chronic lung disease
95. Why is monitoring ventilated patients important for aspiration prevention?
To detect early signs of complications.
96. What is one benefit of elevating the head of the bed during ventilation?
It reduces aspiration risk.
97. What is a consequence of aspirating bacteria-laden secretions?
Development of pneumonia.
98. What is one reason to assess cough strength before extubation?
To ensure the patient can clear secretions.
99. What is a key factor in determining aspiration risk during assessment?
Ability to protect the airway.
100. Why is aspiration considered a serious clinical event?
It can lead to life-threatening respiratory complications.
Final Thoughts
Aspiration is a complex and clinically significant event that affects patients across all areas of respiratory care. It results from a failure of normal airway protection and can lead to serious complications, including infection, inflammation, and respiratory failure.
Because it is influenced by multiple factors such as patient condition, medical interventions, and clinical practices, it requires continuous assessment and proactive management.
By focusing on airway protection, proper positioning, and effective secretion management, healthcare providers can significantly reduce the risk of aspiration and improve patient outcomes in both acute and long-term care settings.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Kollmeier BR, Keenaghan M. Aspiration Risk. [Updated 2023 Mar 16]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026.

