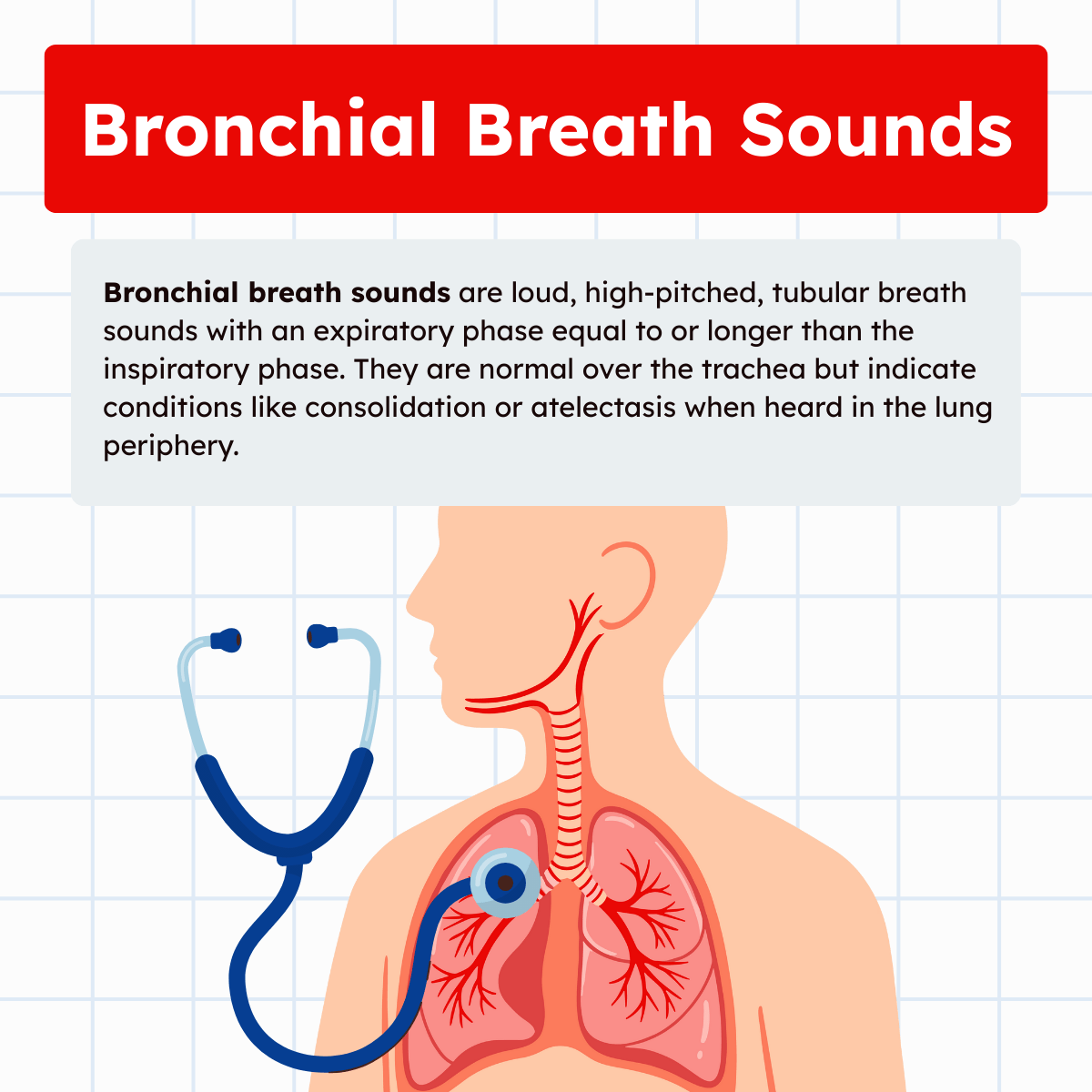
Bronchial breath sounds are loud, high-pitched, tubular respiratory sounds that are normally heard only over the trachea and main bronchi. When these harsh sounds are detected in the lung periphery, however, they become an important clinical sign of underlying pathology.
Conditions such as pneumonia, consolidation, or atelectasis can increase lung tissue density, allowing sound from the larger airways to transmit more clearly to areas where it should not normally be heard.
Because of this, identifying bronchial breath sounds is a key skill for respiratory therapists and clinicians. In this article, we will explore what bronchial breath sounds are, how they develop, and what they reveal about lung function and disease.
What Are Bronchial Breath Sounds?
Bronchial breath sounds are high-pitched, loud, tubular breathing sounds characterized by an expiratory phase that is equal to or longer than the inspiratory phase. These sounds are produced by turbulent airflow within the trachea and larger bronchi. Because of their intensity and tonal quality, they resemble the sound of air moving through a hollow tube.
These breath sounds are normal only when heard over the trachea or right anterior apex, where large airways are close to the chest wall. In these areas, the anatomy naturally allows clear transmission of harsh airway sounds.
However, bronchial breath sounds become abnormal when heard over the lung periphery. In healthy lungs, sound is filtered by the spongy, aerated parenchyma, creating softer vesicular breath sounds. When lung tissue becomes dense, consolidated, or collapsed, this filtering effect is lost, allowing harsh bronchial sounds to be transmitted to peripheral lung fields.
How Bronchial Breath Sounds Are Produced
Bronchial breath sounds result from turbulent airflow moving through large, rigid airways such as the trachea and main bronchi. Under normal conditions, these sounds are loud and high-pitched because there is minimal damping from surrounding tissues. However, when similar sounds are heard in the lung periphery, the mechanism involves changes in lung density and sound transmission rather than changes in airflow alone.
Normal Mechanism
In healthy individuals, bronchial sounds are heard only over the trachea. The large airway diameter and rigid structure allow air movement to create strong, tubular sounds with distinct inspiratory and expiratory phases.
Abnormal Transmission Through Dense Lung Tissue
When lung tissue becomes consolidated or collapsed, it loses its normal spongy, air-filled structure. Dense tissue transmits sound much more efficiently. As a result, harsh bronchial sounds originating in the central airways travel through the abnormal area and reach the chest wall without being filtered.
This explains why bronchial breath sounds are commonly heard in:
- Pneumonia or consolidation
- Moderate atelectasis
- Areas of lung collapse surrounded by denser tissue
Expiratory Dominance
An identifying feature of bronchial breath sounds is that expiration is equal to or longer than inspiration, a key distinction from normal vesicular sounds, which are predominantly inspiratory.
Note: Understanding how these sounds are produced allows clinicians to differentiate true pathology from normal findings and identify the presence of consolidation or collapse early.
Clinical Conditions Associated With Bronchial Breath Sounds
Bronchial breath sounds heard outside the tracheal region strongly suggest an underlying abnormality in the lung parenchyma. They are a key auscultatory sign of conditions that increase lung density or alter normal ventilation patterns.
Pneumonia and Consolidation
Consolidation from pneumonia replaces air-filled alveoli with fluid, inflammatory cells, and debris. This increased density allows sound from the central airways to transmit clearly to the chest wall, producing abnormal bronchial breath sounds. This finding is one of the classic indicators of lobar pneumonia.
Atelectasis
In moderate atelectasis, lung tissue collapses and becomes denser, which enhances sound transmission. Crackles may also be present, and oxygen saturation may drop. Bronchial breath sounds often appear around the margins of severely collapsed lung areas.
Partial Lung Collapse
When portions of the lung collapse due to mucus plugging, tumors, or compression, the affected area may transmit bronchial breath sounds instead of normal vesicular sounds. This change reflects restricted ventilation in that region.
Retained Secretions and Ineffective Cough
Secretions that block airflow can alter breath sounds. In some cases, bronchial breath sounds may be heard along with crackles or coarse airway noises, signaling poor airway clearance. Fever, tachypnea, tachycardia, or labored breathing may accompany these findings.
Note: Because bronchial breath sounds outside their normal location almost always indicate disease, their presence should prompt further clinical evaluation and imaging.
How to Assess Bronchial Breath Sounds
Recognizing bronchial breath sounds requires attentive auscultation and a good understanding of where different breath sounds should normally be heard. Proper assessment helps distinguish normal tracheal sounds from abnormal findings in the lung periphery.
Follow a Systematic Auscultation Pattern
Listen to the chest in a consistent sequence, comparing right and left sides at each level. Bronchial breath sounds heard over the trachea are normal, but the same sounds heard in peripheral lung fields indicate pathology.
Identify Pitch, Loudness, and Phase Duration
Bronchial breath sounds are:
- High-pitched
- Loud and tubular
- Equal in inspiratory and expiratory duration, or with a longer expiratory phase
Note: These qualities help differentiate them from vesicular breath sounds, which are softer and predominantly inspiratory.
Listen for Associated Adventitious Sounds
Consolidation or atelectasis may also produce:
- Crackles
- Diminished breath sounds in surrounding regions
- Increased work of breathing
Note: These clues support the interpretation of abnormal bronchial breath sounds.
Correlate With Clinical Symptoms
Symptoms such as fever, cough, chest discomfort, dyspnea, decreased oxygen saturation, or an ineffective cough strengthen the suspicion of pneumonia, collapse, or retained secretions.
Use Percussion to Support Findings
Dullness to percussion combined with bronchial breath sounds strongly suggests consolidation. Hyperresonance may indicate associated air trapping or partial collapse.
Note: Accurate assessment requires integrating sound characteristics, physical findings, and patient symptoms. When bronchial breath sounds are present in abnormal locations, additional diagnostic testing is usually warranted.
Why Identifying Bronchial Breath Sounds Matters in Respiratory Care
Bronchial breath sounds play an important diagnostic role because they provide direct clues about changes in lung density and ventilation. Recognizing them promptly helps clinicians detect consolidation, collapse, or other pulmonary abnormalities early in their progression.
Early Recognition of Pneumonia and Consolidation
Bronchial breath sounds in the lung periphery are one of the hallmark findings of pneumonia. Detecting these sounds helps clinicians diagnose consolidation sooner, even before imaging results return.
Detecting Atelectasis and Areas of Collapse
Moderate atelectasis may present with tachypnea, low oxygen saturation, and diminished breath sounds. As collapse progresses, bronchial breath sounds often appear along the margins of the affected area. This finding helps clinicians identify regions of poor ventilation that may benefit from lung expansion therapy.
Monitoring Airway Clearance and Ventilation
Patients with retained secretions or ineffective cough may show changes in breath sounds over time. Bronchial breath sounds, especially if they appear suddenly, may indicate worsening consolidation or obstruction that requires prompt intervention.
Supporting Clinical Decision-Making
Bronchial breath sounds help guide diagnostic and therapeutic steps, including:
- Ordering chest imaging
- Initiating antibiotics for suspected pneumonia
- Performing airway clearance therapy
- Adjusting oxygen therapy
- Evaluating the need for bronchoscopy in cases of mucus plugging
Enhancing Overall Respiratory Assessment
Because breath sound interpretation is a core skill in respiratory therapy, accurately identifying bronchial breath sounds helps clinicians provide safer, more effective care. These sounds often act as early warning signs of serious disease.
Bronchial Breath Sounds Practice Questions
1. What are bronchial breath sounds and how do they differ from normal vesicular breath sounds?
Bronchial breath sounds are high-pitched, loud, tubular sounds with a longer expiratory phase, unlike vesicular sounds which are soft and predominantly inspiratory.
2. Where are bronchial breath sounds normally heard in a healthy individual?
Over the trachea and mainstem bronchi.
3. What does it indicate when bronchial breath sounds are heard in the lung periphery?
An abnormal finding that strongly suggests consolidation or atelectasis.
4. Why do bronchial breath sounds appear in areas of consolidation?
Because fluid-filled or solid lung tissue transmits sound more efficiently than aerated lung.
5. What is the typical inspiratory-to-expiratory ratio of bronchial breath sounds?
Expiration is equal to or longer than inspiration.
6. Which lung condition most classically produces bronchial breath sounds in the periphery?
Pneumonia with consolidation.
7. How can atelectasis cause bronchial breath sounds?
Collapsed tissue adjacent to a patent airway increases sound transmission from larger airways.
8. What breath sound change may appear in moderate atelectasis?
Occasional bronchial breath sounds mixed with crackles.
9. What breath sound findings accompany severe atelectasis?
Absent breath sounds over the collapsed area with bronchial sounds around the margins.
10. What additional clinical signs may accompany bronchial breath sounds in pneumonia?
Fever, tachypnea, tachycardia, and productive cough.
11. Which type of breath sound is described as loud, harsh, and high-pitched?
Bronchial breath sound.
12. Why are bronchial sounds considered abnormal outside the tracheal region?
Because normal lung parenchyma filters high-frequency sound, preventing tubular airflow sounds from being heard distally.
13. What is suggested by the presence of bronchial breath sounds plus coarse crackles?
Retained secretions or consolidation.
14. What does an ineffective cough combined with bronchial breath sounds indicate?
Poor airway clearance with possible mucus plugging or infection.
15. Why must clinicians consider location when interpreting bronchial breath sounds?
A sound normal in one region may be abnormal if heard elsewhere.
16. What does increased density of lung tissue imply about auscultated breath sounds?
It enhances transmission of bronchial sounds due to reduced air content.
17. What breath sound pattern is expected in early lobar pneumonia?
Bronchial breath sounds over the affected lobe.
18. How does air-fluid mixture in the lungs alter breath sound transmission?
It reduces filtering of higher-frequency sounds, making bronchial tones audible peripherally.
19. What does the combination of low SpO₂, increased RR, and bronchial breath sounds suggest?
Underlying pathology such as atelectasis or consolidation impairing ventilation.
20. Why are bronchial breath sounds typically louder during expiration?
Expiration in large airways generates higher-velocity airflow and thus louder acoustic resonance.
21. What physiologic factor makes bronchial breath sounds high-pitched?
Turbulent airflow through larger, rigid airway structures.
22. In what condition might bronchial breath sounds reappear after being absent?
Re-expansion of atelectatic lung tissue.
23. What lung finding should be suspected if bronchial sounds accompany egophony?
Lobar consolidation.
24. What underlying problem is suggested when bronchial breath sounds accompany fever and tachycardia?
A likely infectious process such as pneumonia.
25. How can bronchial breath sounds help differentiate between obstructive and restrictive problems?
Bronchial sounds point toward restrictive issues like consolidation, not classic obstruction.
26. What does it indicate if bronchial breath sounds are present along with dull percussion?
Consolidation, not hyperinflation.
27. How do secretions influence bronchial breath sounds?
They may enhance transmission by increasing tissue density.
28. What sound quality best describes bronchial breath sounds?
Tubular and blowing, similar to air moving through a hollow pipe.
29. What patient complaint may correlate with bronchial breath sounds in consolidation?
Pleuritic chest pain or productive cough.
30. How might bronchial breath sounds help localize pathology during auscultation?
They typically overlie the exact area of consolidation or collapsed lung tissue.
31. What does the sudden appearance of bronchial breath sounds in a postoperative patient suggest?
Developing atelectasis or consolidation.
32. What chest condition reduces the likelihood of hearing bronchial breath sounds even in pneumonia?
A large pleural effusion that blocks sound transmission.
33. Why are bronchial breath sounds louder when auscultated over fluid-filled tissue?
Because sound travels more efficiently through liquid than through air.
34. What breath sound pattern is typically absent in COPD but may appear if pneumonia develops?
Bronchial breath sounds in previously hyperinflated regions.
35. What is indicated when bronchial breath sounds are heard in combination with bronchophony?
Lung consolidation.
36. Why are bronchial breath sounds considered an “airspace disease marker”?
They indicate that alveoli are filled with exudate, fluid, or collapse rather than air.
37. What physiological change causes normal vesicular sounds to be replaced by bronchial sounds?
Loss of alveolar air content causing improved sound transmission.
38. How does severe mucus plugging influence bronchial breath sounds?
It may create patchy areas of atelectasis that transmit bronchial tones.
39. Why do bronchial sounds become more prominent when a patient takes a deep breath?
Increased airflow enhances the resonance of large airway sounds.
40. How might bronchial breath sounds assist in confirming lobar involvement during pneumonia?
They localize to the affected lobe due to increased density.
41. What should be suspected when bronchial breath sounds appear suddenly during respiratory distress?
Acute lobar collapse.
42. How do bronchial breath sounds differ from wheezes in terms of mechanism?
Bronchial sounds arise from sound transmission, whereas wheezes arise from airway vibration.
43. What acoustic characteristic helps differentiate bronchial breath sounds from crackles?
Bronchial sounds are continuous, while crackles are discontinuous.
44. What abnormal finding strengthens the diagnosis when bronchial breath sounds are heard over one lung?
Dullness to percussion over the same region.
45. In what lung condition might bronchial breath sounds be heard despite normal chest X-ray findings?
Small-area subsegmental atelectasis not yet radiographically visible.
46. What does the presence of bronchial breath sounds near the spine on posterior exam suggest?
Lower lobe consolidation.
47. Which auscultation maneuver enhances detection of bronchial breath sounds?
Asking the patient to take slow, deep breaths through the mouth.
48. Why do infants with pneumonia often have more diffuse bronchial breath sounds?
Smaller chest cavity transmits airway sounds more broadly.
49. What may cause bronchial breath sounds in a patient recovering from thoracic surgery?
Incomplete lung expansion following anesthesia or pain-limited breathing.
50. How does the presence of bronchial breath sounds guide airway clearance therapy?
It suggests secretion retention or consolidation requiring targeted interventions.
51. In which condition might bronchial breath sounds appear bilaterally?
Diffuse consolidation, such as in severe pulmonary edema.
52. Why do bronchial breath sounds become more noticeable when alveoli are filled with pus or fluid?
The dense medium eliminates the dampening effect normally provided by air.
53. What finding differentiates bronchial breath sounds from pleural friction rub?
Bronchial sounds persist despite breath-holding; rubs do not.
54. What clinical symptom may accompany bronchial breath sounds during consolidation?
Increased tactile fremitus over the affected region.
55. How do bronchial breath sounds relate to airway patency?
They suggest that the proximal airway is open but distal airspaces are abnormal.
56. What lung pathology is suggested when bronchial breath sounds appear with asymmetric chest expansion?
Unilateral lung collapse or consolidation.
57. Why might bronchial breath sounds appear after vigorous chest physiotherapy?
Mobilized secretions increase density temporarily, enhancing sound transmission.
58. What does the combination of fever, productive cough, and bronchial breath sounds imply?
Active infection with airspace involvement.
59. What does the persistence of bronchial breath sounds after treatment suggest?
Incomplete resolution of consolidation or persistent collapse.
60. Why are bronchial breath sounds sometimes described as “tubular”?
They resemble airflow through a hollow tube, reflecting tracheobronchial resonance.
61. What does the absence of vesicular breath sounds combined with the presence of bronchial breath sounds indicate?
Replacement of normal air-filled alveoli with consolidated tissue.
62. What condition is suggested when bronchial breath sounds are heard directly above an area of dull percussion?
Lobar consolidation
63. How does lung density influence the transmission of bronchial breath sounds?
Increased density enhances transmission from central airways to the chest wall.
64. Why are bronchial breath sounds commonly heard near the mediastinum even in healthy individuals?
The trachea and main bronchi naturally produce tubular airflow sounds.
65. What may cause bronchial breath sounds to shift location during serial exams?
Changes in consolidation or improving aeration of the lung.
66. When auscultating a patient with suspected pneumonia, what does localized bronchial breath sounds confirm?
Involvement of a specific segment or lobe.
67. What is implied when bronchial breath sounds remain audible despite improvement in clinical symptoms?
Residual consolidation or incomplete resolution of pathology.
68. What auscultatory finding commonly accompanies bronchial breath sounds in pneumonia?
Increased tactile fremitus.
69. How does airway patency relate to the presence of bronchial breath sounds?
The proximal airways must remain open for the sound to transmit effectively.
70. Why do bronchial breath sounds disappear when a large pneumothorax develops?
Air in the pleural space blocks transmission of central airway sounds.
71. What finding differentiates bronchial breath sounds caused by consolidation from those caused by fibrosis?
Fibrosis produces coarse breath sounds but often retains underlying vesicular character.
72. How might patient position affect detection of bronchial breath sounds?
Supine positioning may shift fluid or secretions, altering sound transmission.
73. What does the presence of bronchial breath sounds in a child often signal?
Lobar pneumonia or segmental atelectasis.
74. How do bronchial breath sounds assist in identifying early lobar pneumonia before radiographic changes appear?
They reveal increased density before X-ray consolidation develops.
75. What combination of findings strongly supports the diagnosis of consolidation?
Bronchial breath sounds, bronchophony, and dull percussion.
76. What change would indicate worsening consolidation on auscultation?
Expansion of the area where bronchial breath sounds are heard.
77. Why might bronchial breath sounds be softer in obese individuals?
Adipose tissue dampens sound transmission.
78. What characteristic of bronchial breath sounds helps distinguish them from vesicular sounds?
Longer, louder expiratory phase.
79. What does the return of vesicular breath sounds after treatment of consolidation indicate?
Restoration of normal aeration.
80. Why are bronchial breath sounds more easily heard over the right upper lobe apex?
Proximity to the trachea and large bronchi.
81. What might cause bronchial breath sounds to appear after thoracic trauma?
Localized areas of collapse or contusion increasing lung density.
82. How can dehydration influence bronchial breath sounds?
Thicker secretions may obstruct airways and alter sound patterns.
83. When bronchial breath sounds are bilateral, what condition should be considered?
Diffuse alveolar filling processes such as severe pulmonary edema.
84. What is suggested when bronchial breath sounds are heard along with egophony?
Airspace replacement with fluid or cellular infiltrates.
85. How does atelectasis contribute to bronchial breath sounds?
Collapsed alveoli increase transmission of central airway sounds.
86. What type of breathing maneuver enhances detection of bronchial breath sounds?
Slow, deep breaths to maximize airflow through central airways.
87. How might airway clearance therapy alter bronchial breath sounds?
Mobilizing secretions can convert bronchial tones back to vesicular sounds.
88. What does a focal area of bronchial breath sounds with normal chest X-ray suggest?
Small-volume collapse or early consolidation not yet radiographically visible.
89. What indicates the resolution of consolidation on auscultation?
Bronchial breath sounds diminish and vesicular sounds return.
90. Why do bronchial breath sounds intensify when alveoli fill with exudate?
Liquid transmits sound more efficiently than air.
91. What does the presence of bronchial breath sounds over an area of suspected pleural effusion indicate?
A small pocket of aerated lung (atelectatic or compressed) above the fluid level.
92. What finding helps distinguish bronchial breath sounds from tracheal breath sounds?
Bronchial sounds are less intense and heard outside the central airway region.
93. What physiologic change makes bronchial breath sounds easier to hear in pneumonia?
Fluid-filled alveoli transmit sound more efficiently than air-filled alveoli.
94. Why is careful comparison of right and left lung fields important when evaluating bronchial breath sounds?
Unilateral changes indicate localized pathology rather than systemic causes.
95. What does the combination of fever, cough, and bronchial breath sounds most strongly suggest?
Airspace consolidation due to infection.
96. Why do bronchial breath sounds diminish in patients with large pleural effusions?
Fluid accumulation blocks transmission of central airway sounds.
97. What respiratory pattern may increase the audibility of bronchial breath sounds?
Slow, deep breathing that enhances airflow through proximal airways.
98. What clinical intervention may cause bronchial breath sounds to appear temporarily where they were previously absent?
Resolution of mucus plugging following airway clearance therapy.
99. What does bronchial breath sounds without accompanying crackles suggest?
Consolidation without significant secretion accumulation.
100. Why is identifying bronchial breath sounds critical before performing bronchodilator therapy?
They indicate reduced lung aeration, guiding expectations for treatment response.
Final Thoughts
Bronchial breath sounds are an important clinical finding that offer valuable insight into lung density and ventilation. While normal when heard over the trachea, these loud, high-pitched, tubular sounds become abnormal when detected in the lung periphery. Their presence often indicates consolidation, pneumonia, or atelectasis, making them a key diagnostic clue during respiratory assessment.
By understanding how bronchial breath sounds are produced, where they should and should not be heard, and what conditions cause them to appear, clinicians can quickly identify underlying pathology and guide appropriate treatment. Accurate recognition of bronchial breath sounds strengthens respiratory evaluations and supports timely, effective patient care.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Zimmerman B, Williams D. Lung Sounds. [Updated 2023 Aug 28]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025.