A pleural effusion occurs when excess fluid accumulates in the pleural space, the thin area between the lungs and the chest wall. While this condition can significantly impact breathing and lung function, it is not a disease itself but rather a sign of an underlying medical problem.
Pleural effusions can develop from a wide range of causes, including heart conditions, infections, cancer, liver disease, kidney disorders, and inflammatory processes. Identifying the underlying cause is essential because treatment depends on addressing the specific condition responsible for the fluid buildup.
This article explores the most common causes of pleural effusion, helping you understand how they develop, their clinical significance, and why early diagnosis plays a critical role in improving patient outcomes.
Download our free guide that has over 100+ of the best tips for healthy lungs.
What is a Pleural Effusion?
A pleural effusion is a medical condition characterized by the accumulation of excess fluid in the pleural space, which is the thin area between the lungs and the chest wall. Normally, this space contains a small amount of fluid that helps the lungs move smoothly during breathing.
However, certain medical conditions can disrupt the balance of fluid production and removal, causing fluid to build up. Pleural effusions can develop due to heart failure, infections, cancer, liver disease, kidney disease, or lung injury.
As fluid accumulates, it can compress the lung and interfere with normal breathing. Common symptoms include shortness of breath, chest discomfort, cough, and decreased exercise tolerance. Treatment focuses on addressing the underlying cause and removing excess fluid when necessary.
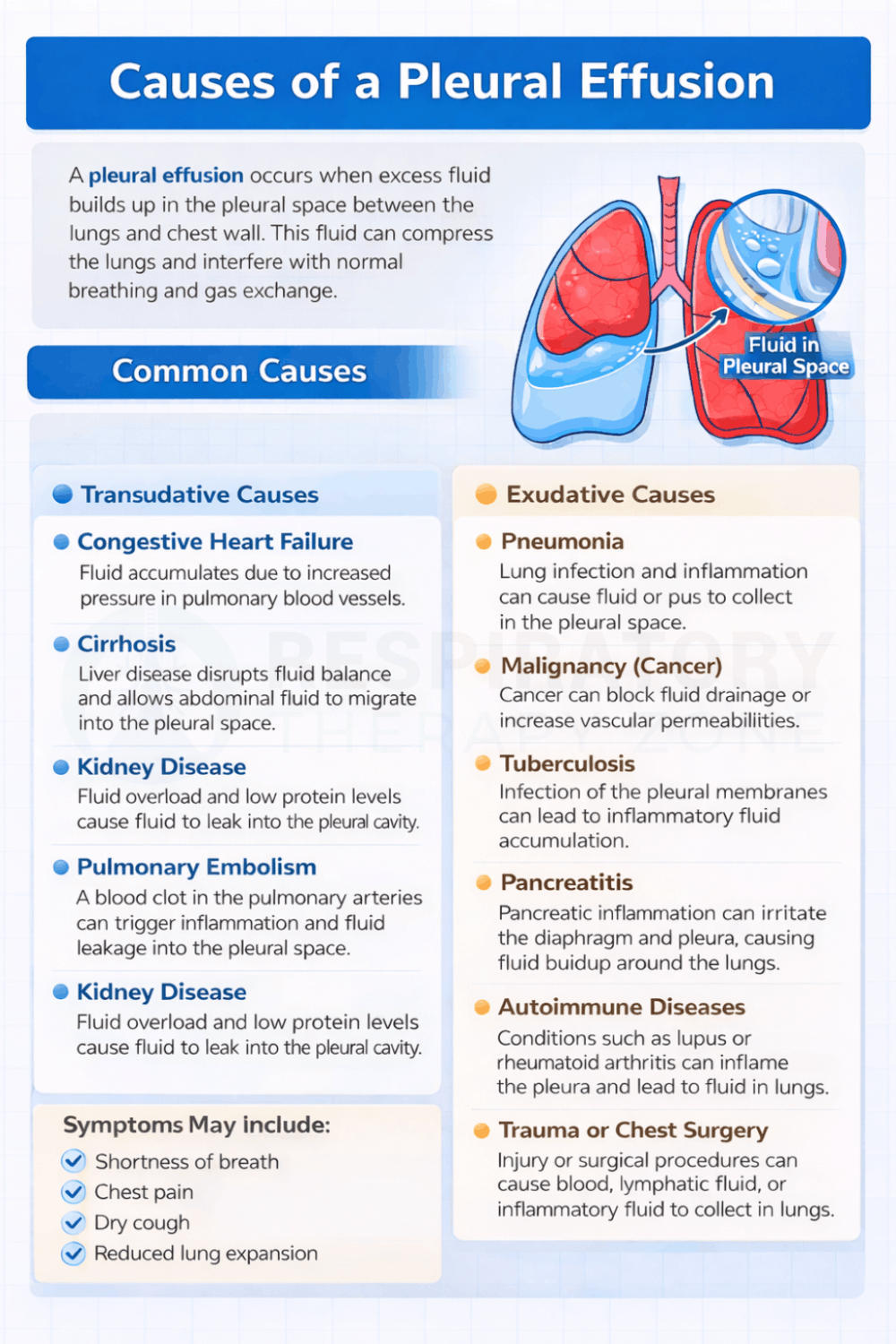
Common Causes of a Pleural Effusion
Pleural effusions can develop from a variety of medical conditions that affect how fluid is produced, circulated, or absorbed within the chest. Understanding the most common causes can help patients and healthcare providers recognize risk factors, guide diagnostic testing, and determine the most effective treatment approach.
Keep reading and watch this video to learn about the leading conditions that contribute to pleural effusion and how each one affects the body. Identifying the underlying cause is essential for proper management and can help prevent complications that may impact breathing and overall lung function.
1. Congestive Heart Failure
Congestive heart failure is the most common cause of pleural effusion and typically results in a transudative fluid accumulation. This condition occurs when the heart cannot pump blood effectively, leading to increased pressure within the pulmonary circulation. As pressure rises in the blood vessels of the lungs, fluid leaks into the pleural space surrounding the lungs.
Pleural effusions caused by heart failure are often bilateral but may be more prominent on the right side. Patients frequently present with shortness of breath, orthopnea, lower extremity swelling, and fatigue.
Treatment usually focuses on managing heart failure through diuretics, fluid restriction, and medications that improve cardiac function. When heart failure is controlled, the pleural effusion often resolves without needing invasive procedures.
2. Pneumonia
Pneumonia is a lung infection caused by bacteria, viruses, or fungi that can lead to inflammation and fluid accumulation in the pleural space, known as a parapneumonic effusion. This type of effusion is classified as exudative because it results from inflammation and increased permeability of pleural membranes.
In more severe cases, infected fluid may collect and form an empyema, which contains pus and requires urgent drainage. Patients with pneumonia-related pleural effusion often experience fever, cough, chest pain that worsens with breathing, and shortness of breath.
Diagnosis typically involves imaging studies and thoracentesis to analyze the pleural fluid. Treatment includes antibiotics and, in complicated cases, chest tube placement or surgical intervention to remove infected fluid and prevent complications.
3. Malignancy (Cancer)
Malignancy is a common cause of exudative pleural effusion and often indicates advanced or metastatic disease. Cancers that most frequently cause pleural effusions include lung cancer, breast cancer, lymphoma, and metastatic tumors from other organs.
Malignant pleural effusions develop when cancer cells invade the pleura, blocking normal fluid drainage or increasing vascular permeability. Patients may experience progressive shortness of breath, chest discomfort, persistent cough, and unexplained weight loss.
Diagnosis typically involves imaging studies and thoracentesis with cytological analysis to detect cancer cells in the pleural fluid. Treatment focuses on managing symptoms and the underlying cancer. Options may include chemotherapy, radiation therapy, repeated thoracentesis, pleurodesis, or placement of an indwelling pleural catheter to help control recurrent fluid buildup.
4. Pulmonary Embolism
Pulmonary embolism occurs when a blood clot, usually originating from the deep veins of the legs, travels to the pulmonary arteries and blocks blood flow to lung tissue. This blockage can cause inflammation, lung tissue injury, and the development of an exudative pleural effusion.
Pleural effusions related to pulmonary embolism are typically small but may contribute to chest pain and breathing difficulty. Patients often present with sudden shortness of breath, sharp pleuritic chest pain, rapid breathing, and sometimes coughing or hemoptysis.
Diagnosis usually involves imaging studies such as CT pulmonary angiography along with laboratory testing. Treatment focuses on anticoagulation therapy to prevent further clot formation. In severe cases, thrombolytic therapy or surgical intervention may be required to restore blood flow and prevent complications.
5. Cirrhosis
Cirrhosis is a chronic liver disease that can lead to pleural effusion, commonly referred to as hepatic hydrothorax. This condition typically causes a transudative effusion and occurs when fluid from the abdominal cavity moves into the pleural space through small defects in the diaphragm. Cirrhosis leads to portal hypertension and reduced production of albumin, which disrupts normal fluid balance and promotes fluid accumulation.
Pleural effusions related to cirrhosis are usually right-sided and may occur even without significant ascites. Patients often experience shortness of breath, fatigue, and abdominal swelling.
Management focuses on treating the underlying liver disease and reducing fluid overload through sodium restriction, diuretics, and therapeutic thoracentesis. In severe or recurrent cases, procedures such as transjugular intrahepatic portosystemic shunt (TIPS) or liver transplantation may be considered.
6. Kidney Disease
Kidney disease, particularly nephrotic syndrome and advanced renal failure, can cause pleural effusion due to fluid retention and decreased protein levels in the blood. These effusions are typically transudative and result from reduced oncotic pressure, which allows fluid to leak from blood vessels into the pleural space.
Patients with kidney-related pleural effusion often present with generalized swelling, weight gain, decreased urine output, and shortness of breath. In individuals receiving dialysis, fluid overload may also contribute to pleural fluid accumulation.
Diagnosis involves imaging studies and laboratory tests that assess kidney function, electrolyte levels, and protein status. Treatment focuses on correcting fluid imbalance through diuretics, dialysis, dietary modifications, and managing the underlying kidney disorder. When fluid overload is controlled, pleural effusions often improve or resolve.
7. Tuberculosis
Tuberculosis is an infectious disease caused by Mycobacterium tuberculosis and is a significant cause of exudative pleural effusion worldwide. Tuberculous pleural effusion develops when the bacteria infect the pleura, triggering inflammation and increased vascular permeability. The pleural fluid in these cases is typically rich in lymphocytes and protein.
Patients often present with symptoms such as persistent cough, fever, night sweats, weight loss, chest pain, and shortness of breath. Diagnosis usually involves chest imaging, pleural fluid analysis, and specialized tests such as acid-fast staining or molecular testing to detect the bacteria.
Treatment requires long-term antibiotic therapy using multiple anti-tuberculosis medications. Early recognition and treatment are essential to prevent complications and reduce the risk of spreading the infection to others.
8. Pancreatitis
Pancreatitis, which is inflammation of the pancreas, can cause pleural effusion when pancreatic enzymes and inflammatory mediators irritate the diaphragm and pleural membranes. This type of effusion is typically exudative and more commonly affects the left side of the chest.
Acute pancreatitis often results from gallstones or excessive alcohol use, while chronic pancreatitis may develop from long-term inflammation. Patients with pancreatitis-related pleural effusion frequently experience severe abdominal pain that radiates to the back, nausea, vomiting, fever, and difficulty breathing.
Diagnosis involves imaging studies and pleural fluid analysis, which may reveal elevated amylase levels. Treatment focuses on managing pancreatitis through supportive care, fluid resuscitation, pain control, and addressing the underlying cause, which often leads to resolution of the pleural effusion.
9. Autoimmune Diseases
Autoimmune diseases such as systemic lupus erythematosus and rheumatoid arthritis can cause pleural effusion by triggering inflammation of the pleural membranes. These conditions occur when the immune system mistakenly attacks healthy tissues, leading to widespread inflammation throughout the body.
Pleural effusions associated with autoimmune disorders are typically exudative and may develop alongside other symptoms such as joint pain, fatigue, skin rashes, or fever. Patients often experience chest pain that worsens with deep breathing and shortness of breath.
Diagnosis usually involves imaging studies, pleural fluid analysis, and laboratory tests that identify autoimmune markers. Treatment focuses on controlling inflammation through corticosteroids, immunosuppressive medications, and disease-specific therapies. When the underlying autoimmune condition is well managed, pleural effusions often improve or resolve.
10. Trauma or Chest Surgery
Trauma or chest surgery can lead to pleural effusion due to direct injury to the lungs, blood vessels, or lymphatic structures within the chest cavity. Injuries such as rib fractures, penetrating chest wounds, or surgical procedures involving the lungs or heart may cause fluid, blood, or lymphatic fluid to accumulate in the pleural space.
Depending on the cause, these effusions may present as hemothorax, chylothorax, or inflammatory fluid accumulation. Patients may experience chest pain, shortness of breath, rapid breathing, and decreased oxygen levels.
Diagnosis typically involves imaging studies such as chest X-ray or CT scan, along with pleural fluid analysis. Treatment depends on the severity and cause but may include chest tube placement, surgical repair, or supportive respiratory care to restore normal lung expansion and function.
FAQs About the Causes of a Pleural Effusion
How Common Is a Pleural Effusion?
Pleural effusion is a relatively common medical condition, particularly among individuals with heart, lung, or systemic diseases. It is estimated that more than one million people develop pleural effusions each year in the United States alone. The condition frequently occurs in hospitalized patients, especially those with congestive heart failure, pneumonia, or cancer.
Because pleural effusion is usually a complication of another illness rather than a primary disease, its frequency varies depending on the prevalence of underlying medical conditions within different populations.
What Are Three Common Causes of a Pleural Effusion?
Three of the most common causes of pleural effusion include congestive heart failure, pneumonia, and cancer. Congestive heart failure often leads to fluid buildup due to increased pressure in blood vessels. Pneumonia causes inflammation that allows fluid or infected material to collect in the pleural space. Cancer can interfere with normal fluid drainage or increase vascular permeability, leading to malignant pleural effusion.
Note: These causes account for a large percentage of cases and are often considered first during medical evaluation.
What Is The Main Cause of Fluid On The Lungs?
The most common cause of fluid around the lungs, also known as pleural effusion, is congestive heart failure. When the heart cannot pump blood effectively, pressure builds up in the pulmonary circulation, forcing fluid into the pleural space.
This fluid accumulation can compress the lungs and make breathing more difficult. While heart failure is the leading cause, other conditions such as infection, cancer, liver disease, and kidney disorders can also contribute to fluid buildup around the lungs.
What Are The Complications of a Pleural Effusion?
Pleural effusion can lead to several complications if left untreated. Large fluid collections may compress the lungs, causing significant breathing difficulty and reduced oxygen levels. Infections can develop within the fluid, resulting in empyema, which may require surgical drainage.
Chronic or recurrent effusions can cause scarring and thickening of the pleural membranes, restricting lung expansion. Additionally, untreated pleural effusions can delay diagnosis of serious underlying conditions such as cancer or tuberculosis, potentially leading to worsened outcomes.
What Are the Symptoms of a Pleural Effusion?
Symptoms of pleural effusion vary depending on the amount of fluid and the underlying cause. Common symptoms include shortness of breath, chest discomfort, and difficulty breathing during physical activity. Some patients experience a persistent cough or chest pain that worsens with deep breathing.
Others may develop fatigue, reduced exercise tolerance, or fever if infection is present. Small pleural effusions may produce few or no symptoms and are sometimes discovered during imaging performed for unrelated medical evaluations.
How Is Fluid Around The Lung Diagnosed?
Fluid around the lung is typically diagnosed using imaging studies such as chest X-ray, ultrasound, or CT scan, which help identify the presence and size of the effusion. Once fluid is detected, a procedure called thoracentesis may be performed to remove a sample for laboratory analysis.
This testing helps determine whether the fluid is transudative or exudative and can reveal infection, cancer cells, or inflammatory markers. Additional blood tests and imaging may also be used to identify the underlying cause.
How Is Fluid Around The Lung Treated?
Treatment for pleural effusion focuses on addressing the underlying cause while relieving symptoms. In mild cases, managing the primary condition, such as heart failure or infection, may allow the fluid to resolve naturally. Larger or symptomatic effusions often require thoracentesis to remove excess fluid and improve breathing.
Recurrent effusions may require procedures such as pleurodesis or placement of an indwelling pleural catheter. In severe cases, surgery may be necessary to remove infected or thickened pleural tissue.
Can a Pleural Effusion Happen For No Reason?
Pleural effusion rarely occurs without an identifiable cause. In most cases, it develops due to underlying medical conditions such as heart failure, infection, cancer, liver disease, or autoimmune disorders.
However, in some situations, the cause may not be immediately apparent, especially if the effusion is small or occurs early in disease progression. Additional testing and monitoring may be necessary to identify the underlying condition. Occasionally, effusions may be labeled idiopathic when no specific cause can be determined.
Who Is Most Likely To Get a Pleural Effusion?
Individuals with chronic medical conditions are most likely to develop pleural effusion. People with congestive heart failure, pneumonia, lung cancer, liver cirrhosis, kidney disease, or autoimmune disorders face a higher risk. Older adults are also more susceptible because they are more likely to have underlying health problems.
Patients who have experienced chest trauma, recent surgery, or infections affecting the lungs are also at increased risk. Lifestyle factors such as smoking can further increase the likelihood of conditions that lead to pleural effusion.
How Can I Lower My Risk Of a Pleural Effusion?
Lowering the risk of pleural effusion involves preventing or managing underlying health conditions. Maintaining heart health through regular exercise, balanced nutrition, and blood pressure control can reduce the risk of heart failure. Avoiding smoking helps protect lung health and lowers cancer risk.
Staying current with vaccinations and practicing good hygiene can reduce respiratory infections. Managing chronic diseases such as liver or kidney disorders with regular medical care can also reduce fluid buildup. Early treatment of infections and respiratory symptoms can further decrease risk.
Final Thoughts
Pleural effusion is a common medical condition that often signals the presence of an underlying disorder affecting the lungs or other organ systems. Causes can range from relatively manageable conditions such as heart failure and infections to more serious diseases like cancer or tuberculosis.
Because symptoms such as shortness of breath, chest discomfort, and fatigue can worsen as fluid accumulates, timely evaluation and diagnosis are essential. Healthcare providers typically rely on imaging studies and pleural fluid analysis to determine the cause and guide treatment.
By identifying and managing the underlying condition, many pleural effusions can be effectively treated or resolved. Understanding the potential causes helps patients and healthcare professionals recognize warning signs early and take appropriate steps to protect respiratory health.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Krishna R, Antoine MH, Alahmadi MH, et al. Pleural Effusion. [Updated 2024 Aug 31]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025.