Chest percussion is a valuable physical assessment technique used by healthcare professionals to evaluate the condition of the lungs and surrounding structures. By tapping on the chest wall and interpreting the resulting sounds, clinicians can gather important information about lung density, air distribution, and the presence of fluid or abnormalities within the thoracic cavity.
For respiratory therapists, chest percussion plays an essential role in bedside assessment and clinical decision-making. This noninvasive technique helps identify respiratory conditions, guides diagnostic testing, and supports effective patient management in a variety of healthcare settings.
What Is Chest Percussion?
Chest percussion is a diagnostic assessment technique that involves tapping on the surface of the chest wall to evaluate the underlying lung tissue and pleural space. The vibrations produced during percussion penetrate several centimeters beneath the chest wall, allowing clinicians to detect changes in lung density, air content, or fluid accumulation.
The technique provides valuable information about the balance between air and tissue or fluid inside the lungs. When performed correctly, chest percussion produces distinct sounds that help clinicians differentiate between normal lung tissue and pathological conditions.
Although modern imaging technologies such as chest radiographs and computed tomography scans are widely used, chest percussion remains an important bedside tool. It allows respiratory therapists and healthcare providers to perform rapid assessments without requiring specialized equipment or exposing patients to radiation.
How Chest Percussion Is Performed
The most commonly used method of chest percussion is called indirect, or mediate, percussion. This technique involves two key steps. First, the clinician places the middle finger of the non-dominant hand firmly against the patient’s chest wall. The finger should be positioned parallel to the ribs while the rest of the hand remains lifted off the chest to avoid dampening the sound.
Second, the clinician uses the middle or index finger of the dominant hand to strike the finger placed on the chest. The movement should originate from the wrist to produce a quick, sharp tap. Proper technique ensures accurate sound production and reliable interpretation.
Chest percussion is typically performed systematically across symmetrical areas of the chest. Comparing one side of the chest to the other helps clinicians identify abnormalities more easily, especially when the problem is unilateral. Percussion is performed over the anterior, lateral, and posterior lung fields while avoiding bony structures and breast tissue, which can interfere with sound transmission.
Note: When assessing the posterior chest wall, patients are often asked to raise their arms to move the scapulae laterally. This positioning improves access to lung fields and enhances assessment accuracy.
Types of Percussion Sounds and Their Meanings
Interpreting percussion sounds is a critical skill for respiratory therapists. Each sound provides valuable clues about the underlying lung condition and helps clinicians identify abnormalities within the thoracic cavity.
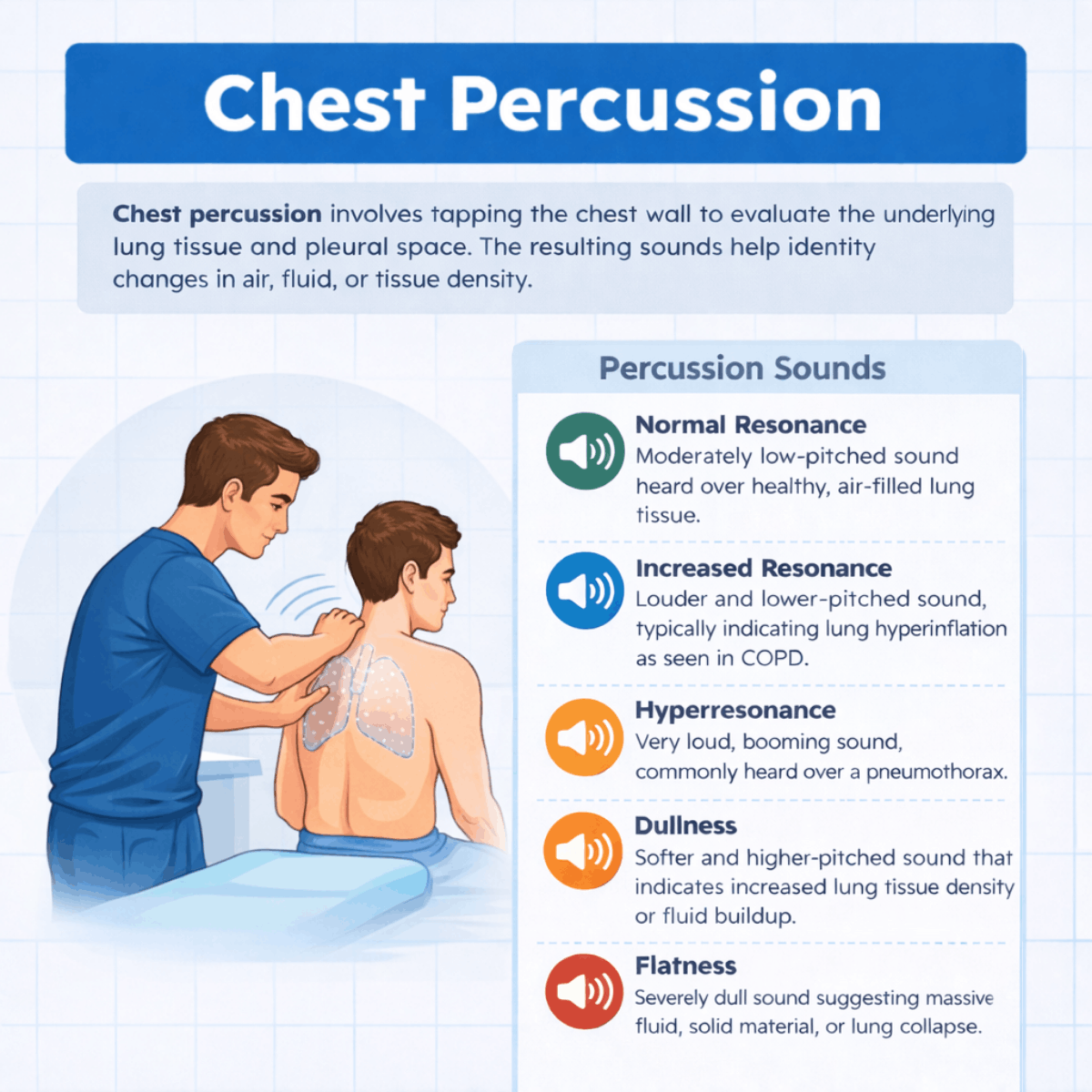
- Normal Resonance: Percussion over healthy, air-filled lung tissue produces a moderately low-pitched sound known as resonance. This sound indicates normal lung aeration and a balanced ratio between air and tissue within the lungs.
- Increased Resonance: Increased resonance is characterized by a louder and lower-pitched sound than normal. This finding typically indicates lung hyperinflation and is commonly heard in patients with obstructive lung diseases such as asthma or chronic obstructive pulmonary disease (COPD).
- Hyperresonance: Hyperresonance produces a very loud, hollow, and booming sound. This percussion note is usually associated with excessive air accumulation in the pleural space and is most commonly heard in patients with pneumothorax.
- Dullness: A dull percussion note is softer, shorter in duration, and higher in pitch. Dullness generally indicates increased lung tissue density or fluid accumulation. This sound is frequently present in conditions such as pneumonia, consolidation, pleural effusion, tumors, or hemothorax.
- Flatness: Flatness to percussion suggests the near absence of air directly beneath the percussed area. This sound is extremely dull and muffled and may indicate significant fluid accumulation in the pleural space, such as pleural effusion or empyema, solid material within the pleural space, such as fibrothorax or mesothelioma, or complete lung collapse as seen in atelectasis.
Note: By carefully analyzing these percussion sounds, respiratory therapists can quickly identify potential respiratory abnormalities and determine whether further diagnostic testing or treatment is necessary.
Clinical Applications of Chest Percussion
Chest percussion plays a significant role in evaluating a patient’s cardiopulmonary status. It helps clinicians detect abnormalities that may not be immediately visible during inspection or palpation.
One major application of chest percussion is the identification of lung consolidation. Consolidation occurs when air within the alveoli is replaced by fluid, pus, or cellular debris, as seen in pneumonia. Percussion over consolidated lung tissue typically produces a dull sound, alerting clinicians to potential infection or inflammation.
Chest percussion is also valuable in detecting pleural effusions. When fluid accumulates in the pleural space, percussion notes become dull or flat over the affected area. This finding can guide further diagnostic evaluation and treatment planning.
Another important application is identifying hyperinflation. Patients with asthma or COPD may demonstrate hyperresonant percussion sounds due to trapped air and increased lung volumes. Recognizing this pattern helps respiratory therapists assess disease severity and monitor treatment effectiveness.
In cases of pneumothorax, where air accumulates in the pleural space, percussion often reveals unilateral hyperresonance. Early detection is crucial because untreated pneumothorax can lead to life-threatening complications.
Assessing Diaphragm Movement Through Percussion
Chest percussion can also be used to evaluate diaphragm function. By percussing downward over the lower lung fields, clinicians can identify the point where percussion sounds transition from resonance to dullness. This change indicates the position of the diaphragm.
Measuring diaphragm excursion involves comparing the diaphragm’s position during full inspiration and full expiration. In healthy adults, diaphragm movement typically ranges from 5 to 7 centimeters. Reduced diaphragm excursion may indicate neuromuscular disorders, severe lung hyperinflation, or other conditions affecting respiratory muscle function.
Note: This assessment provides valuable insight into respiratory mechanics and overall ventilatory efficiency.
Importance of Chest Percussion for Respiratory Therapists
Respiratory therapists play a central role in evaluating and managing patients with cardiopulmonary disorders. Chest percussion is an essential component of the physical examination and allows therapists to gather immediate clinical information at the bedside.
This technique supports rapid decision-making in emergency and critical care settings. For example, detecting hyperresonance in a patient with sudden respiratory distress may raise suspicion for pneumothorax and prompt urgent intervention.
Chest percussion also assists respiratory therapists in monitoring disease progression and treatment response. Changes in percussion findings can indicate improvement or worsening of respiratory conditions, guiding adjustments to therapy.
Additionally, chest percussion is relevant for professional certification examinations, including those administered by the National Board for Respiratory Care (NBRC). Mastery of percussion techniques and interpretation is essential for students preparing for respiratory therapy credentialing exams.
Role of Mechanical Percussion in Airway Clearance
Beyond diagnostic assessment, percussion techniques are also used therapeutically to facilitate secretion clearance. Manual chest percussion, often referred to as chest physiotherapy, helps loosen mucus from airway walls, making it easier for patients to cough and clear secretions.
Mechanical percussors and vibrators are commonly used as alternatives to manual techniques. These devices deliver consistent percussion forces and frequencies, reducing caregiver fatigue and improving convenience, especially in home care settings. While mechanical devices provide similar effectiveness to manual methods, both approaches require proper airway clearance techniques, including directed coughing, to achieve optimal results.
Limitations of Chest Percussion
Despite its usefulness, chest percussion has several limitations. Small or deeply located lung abnormalities may not produce detectable percussion changes. Additionally, percussion findings can be influenced by patient body habitus, chest wall thickness, and clinician technique.
Chest percussion should not be used as a standalone diagnostic tool. Instead, it should be combined with other physical examination techniques, including inspection, palpation, and auscultation. When abnormalities are suspected, imaging studies and laboratory tests are often necessary to confirm diagnoses.
Note: Understanding these limitations helps respiratory therapists interpret percussion findings accurately and avoid misdiagnosis.
Integrating Chest Percussion Into Comprehensive Patient Assessment
Chest percussion is most effective when used as part of a systematic thoracic examination. Respiratory therapists typically combine percussion findings with patient history, vital signs, and other physical assessment results to develop a complete clinical picture.
For example, percussion findings of dullness accompanied by fever, productive cough, and abnormal breath sounds may strongly suggest pneumonia. Similarly, hyperresonance combined with decreased breath sounds and sudden chest pain may indicate pneumothorax.
Note: Integrating percussion with other assessment techniques improves diagnostic accuracy and enhances patient care outcomes.
Chest Percussion Practice Questions
1. What is chest percussion?
Chest percussion is a physical assessment technique that involves tapping on the chest wall to evaluate underlying lung and pleural structures.
2. What information does chest percussion provide?
It produces sound and vibration that help clinicians assess lung tissue density and detect abnormalities within the lungs or pleural space.
3. How deep can vibrations from chest percussion penetrate?
The vibrations created by percussion typically penetrate approximately 5 to 7 cm beneath the chest wall.
4. Is chest percussion performed routinely on all patients?
No, chest percussion is usually reserved for patients with suspected lung abnormalities such as pneumothorax, consolidation, or pleural effusion.
5. What is the most commonly used technique for chest percussion?
Mediate, or indirect, percussion is the most commonly used method.
6. What is the first step in performing mediate percussion?
Place the middle finger of the non-dominant hand firmly against the patient’s chest wall, parallel to the ribs, while keeping the palm and remaining fingers off the chest.
7. What is the second step in performing mediate percussion?
Use the middle or index finger of the dominant hand to strike the finger placed on the chest wall.
8. What part of the finger should receive the percussion strike?
The strike should be delivered near the base of the terminal phalanx of the finger placed on the chest.
9. Where should the motion for percussion originate?
The motion should be generated at the wrist rather than the elbow or shoulder to produce a sharp, controlled strike.
10. Why is percussion performed systematically across both sides of the chest?
Systematic comparison of symmetrical areas allows clinicians to detect abnormalities by comparing findings between the two sides.
11. Why should percussion over bony structures be avoided?
Percussion over bone does not provide useful diagnostic information about underlying lung tissue.
12. Why is percussion typically avoided over the breasts in female patients?
Breast tissue can dampen percussion sounds and reduce diagnostic accuracy.
13. Why are patients often asked to raise their arms during posterior chest percussion?
Raising the arms moves the scapulae laterally, improving access to the lung fields and reducing interference.
14. What characteristic of percussion sounds is primarily evaluated during chest percussion?
The intensity and pitch of the percussion note are evaluated.
15. What sound is normally heard when percussing healthy lung tissue?
Normal lung tissue typically produces a resonant, moderately low-pitched sound.
16. What is hyperresonance during chest percussion?
Hyperresonance is a louder, deeper, and more resonant percussion sound often associated with excess air in the lungs or pleural space.
17. What conditions can produce hyperresonance on chest percussion?
Conditions such as asthma, emphysema, or pneumothorax can produce hyperresonance.
18. What is dullness during chest percussion?
Dullness is a muffled percussion sound that indicates increased tissue density or fluid accumulation.
19. What conditions commonly produce dullness on chest percussion?
Atelectasis, pneumonia, tumors, pleural effusion, or hemothorax can cause dull percussion sounds.
20. Why are unilateral chest abnormalities easier to detect using percussion?
The unaffected side provides a normal reference for comparison, making abnormal findings easier to identify.
21. How can chest percussion assist clinical decision-making?
It provides rapid bedside assessment that may help determine whether further imaging, such as a chest radiograph, is needed.
22. What types of abnormalities may not be detected with chest percussion?
Small abnormalities or lesions located deep beneath the chest surface may not produce detectable percussion changes.
23. How does increased lung tissue density affect percussion sounds?
Increased tissue density reduces resonance and produces a dull percussion note.
24. How does increased air in the pleural space affect percussion sounds?
Excess air increases resonance and produces a hyperresonant percussion note.
25. What components are typically included in the respiratory physical examination?
The respiratory physical examination generally includes vital signs, inspection, palpation, percussion, and auscultation of the chest.
26. What thoracic abnormalities may be identified during chest inspection?
Inspection may reveal abnormalities such as increased anterior-posterior diameter, pectus excavatum, kyphoscoliosis, accessory muscle use, pursed-lip breathing, or cyanosis.
27. What does an increased anterior-posterior (AP) diameter suggest?
An increased AP diameter often indicates chronic lung hyperinflation, commonly seen in patients with COPD.
28. What is pectus excavatum?
Pectus excavatum is a chest wall deformity characterized by a sunken or depressed sternum.
29. What is kyphoscoliosis?
Kyphoscoliosis is a spinal deformity involving both lateral curvature and forward rounding of the spine that can impair lung expansion.
30. What abnormal findings may be detected during chest palpation?
Palpation can detect tracheal deviation, asymmetrical chest expansion, and abnormalities in tactile or vocal fremitus.
31. What does tracheal deviation indicate?
Tracheal deviation may suggest conditions such as pneumothorax, atelectasis, or large pleural effusion.
32. What is tactile fremitus?
Tactile fremitus refers to palpable chest wall vibrations produced when a patient speaks.
33. How does increased tactile fremitus typically present?
Increased fremitus is usually associated with lung consolidation, such as pneumonia.
34. How does decreased tactile fremitus typically present?
Decreased fremitus is commonly associated with pleural effusion, pneumothorax, or airway obstruction.
35. What percussion sound is typically heard over consolidated lung tissue?
Consolidated lung tissue usually produces a dull percussion note that is high-pitched and short in duration.
36. What percussion sound is typically heard over hyperinflated lungs?
Hyperinflated lungs typically produce a hyperresonant percussion note that is low-pitched, loud, and prolonged.
37. What conditions commonly cause bilateral hyperresonance?
Bilateral hyperresonance is commonly associated with asthma exacerbations or COPD.
38. What condition commonly causes unilateral hyperresonance?
A pneumothorax often produces unilateral hyperresonance.
39. Why is it important to percuss lung fields bilaterally during a thoracic examination?
Bilateral percussion allows comparison between sides to help identify localized abnormalities.
40. Why should percussion over bony structures and breast tissue be avoided?
These structures distort percussion sounds and reduce diagnostic accuracy.
41. What is the percussion sound produced over normal air-filled lung tissue?
Normal lung tissue produces a moderately low-pitched, resonant sound.
42. What does increased resonance during percussion typically indicate?
Increased resonance usually indicates lung hyperinflation or the presence of excess air in the pleural space.
43. What does a dull or flat percussion note indicate?
A dull or flat percussion note suggests increased lung tissue density or fluid accumulation.
44. How can percussion help identify the position of the diaphragm?
As percussion moves downward over the posterior thorax, the sound changes from resonance to dullness, indicating the diaphragm level.
45. What is the normal range of diaphragm excursion in adults?
Normal diaphragm excursion typically ranges from 5 to 7 cm.
46. In what conditions is diaphragm motion commonly decreased?
Diaphragm motion is often reduced in patients with neuromuscular disorders or severe lung hyperinflation.
47. How does pleural fluid affect percussion findings?
Pleural fluid decreases resonance and produces a dull percussion note.
48. What is the primary goal of mechanical devices used for secretion clearance?
Mechanical devices help mobilize and loosen secretions to improve airway clearance.
49. Do mechanical secretion clearance devices replace directed coughing?
No, effective secretion clearance still requires directed coughing or other airway clearance techniques.
50. What are handheld percussors and vibrators used for?
They are mechanical devices used to assist secretion mobilization in both pediatric and adult patients.
51. What frequency range is typically used for vibration therapy with handheld devices?
Vibration therapy is commonly delivered at frequencies between 20 and 30 Hz.
52. What advantage do mechanical percussors have over manual chest percussion?
They provide consistent impact force and frequency while reducing caregiver fatigue.
53. In what situations are handheld percussors especially helpful?
They are useful when caregivers cannot effectively perform manual chest percussion, particularly in home care settings.
54. Are handheld percussors more effective than manual percussion techniques?
No, mechanical percussors are generally considered equally effective but not superior to manual techniques for secretion clearance.
55. What is the primary purpose of chest percussion during a respiratory assessment?
The primary purpose is to evaluate underlying lung and pleural structures by identifying changes in sound resonance.
56. How should the patient be positioned for anterior chest percussion?
The patient should sit upright or lie in a semi-Fowler’s position to allow proper access to the anterior chest wall.
57. How should the patient be positioned for posterior chest percussion?
The patient should sit upright and lean slightly forward with arms raised or crossed to move the scapulae laterally.
58. Why is it important to strike the chest wall quickly during percussion?
A quick strike produces clearer vibration and sound, improving diagnostic accuracy.
59. What may cause asymmetrical chest expansion during palpation?
Conditions such as atelectasis, pneumothorax, or pneumonia may result in uneven chest expansion.
60. What is the clinical significance of detecting decreased chest wall movement?
Decreased movement may indicate lung collapse, neuromuscular weakness, or severe airway obstruction.
61. What type of percussion sound is typically heard over the liver?
The liver produces a dull percussion note due to its solid structure.
62. Why is comparing percussion sounds between symmetrical lung fields important?
Comparing symmetrical areas helps detect subtle differences that may indicate localized disease.
63. How does lung consolidation affect percussion findings?
Lung consolidation increases tissue density and produces a dull percussion sound.
64. How does emphysema affect percussion findings?
Emphysema increases air trapping and typically produces hyperresonant percussion sounds.
65. What is the clinical importance of identifying hyperinflation during percussion?
Hyperinflation may indicate obstructive lung diseases such as asthma or COPD.
66. How can percussion help detect pleural effusion?
Pleural effusion causes fluid accumulation that produces dullness over the affected area.
67. What is the expected percussion finding over a pneumothorax?
Pneumothorax typically produces hyperresonance due to excess air in the pleural space.
68. Why should percussion strokes be delivered perpendicular to the chest wall?
Perpendicular strikes optimize vibration transmission and improve sound clarity.
69. How can thick chest walls or obesity affect percussion results?
They may dampen percussion sounds and make abnormalities harder to detect.
70. Why should clinicians avoid using excessive force during percussion?
Excessive force may cause patient discomfort and reduce accuracy of sound interpretation.
71. What role does percussion play in identifying lung boundaries?
Percussion helps define the borders between lung tissue and adjacent organs or structures.
72. How does atelectasis affect percussion findings?
Atelectasis causes lung collapse, resulting in a dull percussion sound.
73. What is the significance of detecting asymmetric diaphragm excursion?
Asymmetric excursion may indicate unilateral lung disease or diaphragmatic dysfunction.
74. Why is percussion less effective for detecting deep lung lesions?
Deep lesions may not significantly alter surface vibrations or percussion sounds.
75. How can chest percussion assist in monitoring disease progression?
Changes in percussion sounds over time may indicate improvement or worsening of lung pathology.
76. What is the difference between resonance and hyperresonance?
Resonance is the normal sound of healthy lung tissue, while hyperresonance indicates excess air.
77. What does flatness during percussion indicate?
Flatness indicates extremely dense structures such as bone or large fluid accumulations.
78. How does hemothorax affect percussion findings?
Hemothorax produces dullness due to blood accumulation in the pleural space.
79. Why is it important to evaluate patient comfort during percussion?
Ensuring patient comfort promotes cooperation and prevents unnecessary pain during assessment.
80. What type of percussion sound is expected over normal gastric air?
Gastric air often produces a tympanic or drum-like sound.
81. How can percussion findings guide further diagnostic testing?
Abnormal percussion findings may indicate the need for imaging studies such as chest X-rays or CT scans.
82. What factors can reduce the reliability of percussion findings?
Patient body habitus, clinician technique, and environmental noise can affect accuracy.
83. How can respiratory therapists use percussion findings to guide therapy?
Percussion results help identify lung abnormalities and assist in selecting appropriate treatments and airway clearance strategies.
84. Why is consistent percussion technique important during repeated assessments?
Using consistent technique ensures reliable comparisons when monitoring patient progress.
85. What is the purpose of assessing tactile fremitus during chest palpation?
Tactile fremitus helps evaluate the transmission of vocal vibrations through the lung tissue to detect consolidation or fluid.
86. How does lung consolidation affect tactile fremitus?
Lung consolidation typically increases tactile fremitus due to improved sound transmission through denser tissue.
87. How does pleural effusion affect tactile fremitus?
Pleural effusion decreases tactile fremitus because fluid dampens vibration transmission.
88. What is the clinical significance of absent breath sounds combined with hyperresonance?
This combination strongly suggests pneumothorax.
89. What is the clinical significance of dullness with bronchial breath sounds?
This finding is commonly associated with lung consolidation such as pneumonia.
90. Why should percussion be performed in a quiet environment?
A quiet environment allows the clinician to accurately hear and interpret subtle changes in percussion sounds.
91. How can percussion findings differ in acute asthma exacerbation?
Acute asthma often produces bilateral hyperresonance due to air trapping.
92. What does symmetric resonance across lung fields generally indicate?
Symmetric resonance typically suggests normal lung aeration.
93. Why is diaphragm excursion measured during percussion?
Measuring diaphragm excursion helps assess diaphragmatic strength and lung expansion capacity.
94. What does reduced bilateral diaphragm excursion suggest?
It may indicate severe hyperinflation, neuromuscular weakness, or restrictive lung disease.
95. How does a large pleural effusion affect diaphragm excursion?
A large pleural effusion may limit diaphragm movement on the affected side.
96. What is the role of percussion in evaluating suspected atelectasis?
Percussion can detect dullness over collapsed lung segments.
97. How can chest wall deformities affect percussion findings?
Chest wall deformities may alter sound transmission and make interpretation more challenging.
98. What percussion finding is expected in severe COPD?
Severe COPD often produces diffuse bilateral hyperresonance.
99. Why is it important to document the location of abnormal percussion findings?
Precise documentation helps correlate physical exam findings with imaging and guides clinical management.
100. How does proper technique improve the reliability of chest percussion?
Accurate finger placement, wrist motion, and consistent force ensure clearer sounds and more dependable assessment findings.
Final Thoughts
Chest percussion remains a fundamental skill in respiratory care that provides valuable insight into lung function and thoracic abnormalities. Although advanced imaging technologies have expanded diagnostic capabilities, bedside percussion continues to offer rapid, noninvasive assessment of lung aeration, fluid accumulation, and tissue density.
Respiratory therapists rely on this technique to support clinical decision-making, monitor treatment effectiveness, and contribute to comprehensive patient evaluations.
By mastering chest percussion and integrating it with other assessment methods, respiratory therapists can enhance diagnostic accuracy, improve patient outcomes, and strengthen their role in delivering high-quality respiratory care.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Tuteur PG. Chest Examination. In: Walker HK, Hall WD, Hurst JW, editors. Clinical Methods: The History, Physical, and Laboratory Examinations. 3rd edition. Boston: Butterworths; 1990.