The dead space to tidal volume ratio (VD/VT) is a key concept in respiratory physiology that reflects how efficiently a patient is ventilating. Rather than simply measuring how much air moves in and out of the lungs, this ratio helps determine how much of that air actually participates in gas exchange.
For respiratory therapists and other clinicians, understanding VD/VT is essential when evaluating ventilation, interpreting arterial blood gases, managing mechanical ventilation, and assessing disease severity in critically ill patients.
What is the Dead Space/Tidal Volume Ratio?
The dead space to tidal volume ratio (VD/VT) is a measure of how much of each breath does not participate in gas exchange. Dead space refers to the portion of inhaled air that remains in the conducting airways or reaches alveoli that are ventilated but not adequately perfused, meaning it does not contribute to carbon dioxide elimination.
Tidal volume is the total amount of air inhaled or exhaled during a normal breath. The VD/VT ratio expresses the fraction of that tidal volume that is wasted ventilation.
It is commonly calculated using arterial carbon dioxide (PaCO₂) and mixed expired carbon dioxide (PECO₂) values with a modified version of the Bohr equation. In healthy adults, the ratio is typically around 0.30. An elevated VD/VT ratio indicates inefficient ventilation and may be seen in conditions such as pulmonary embolism, ARDS, or rapid shallow breathing, all of which impair effective gas exchange.
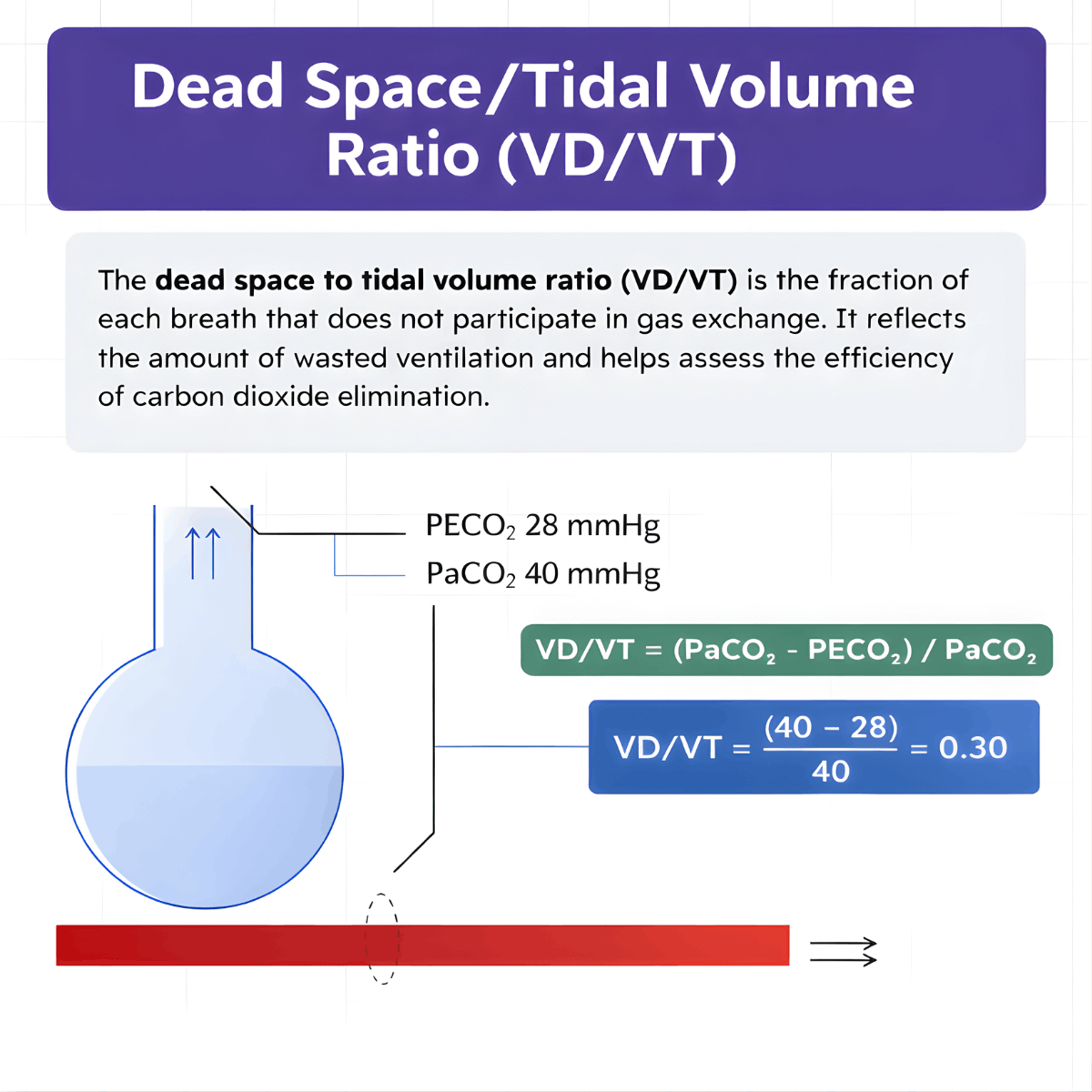
Dead Space/Tidal Volume Ratio (VD/VT) Calculation
The VD/VT ratio is calculated using a modified form of the Bohr equation, often referred to as the Enghoff modification:
VD/VT = (PaCO₂ − PECO₂) / PaCO₂
Where:
- PaCO₂ is the arterial carbon dioxide tension
- PECO₂ is the average carbon dioxide tension in mixed expired gas
PaCO₂ is typically obtained from an arterial blood gas (ABG) sample. PECO₂ can be measured by collecting mixed expired gas or estimated using capnography.
The equation assumes that inspired gas contains no CO₂ and that all CO₂ in expired gas comes from ventilated alveoli. Because dead space air contains little to no CO₂, the average expired CO₂ (PECO₂) is always lower than the arterial CO₂ (PaCO₂). The greater the difference between these two values, the higher the VD/VT ratio.
For example, if PaCO₂ is 40 mm Hg and PECO₂ is 28 mm Hg:
VD/VT = (40 − 28) / 40
VD/VT = 12 / 40
VD/VT = 0.30
Note: This represents a normal value of 30%.
Why the VD/VT Ratio Matters
The VD/VT ratio provides insight into the efficiency of ventilation. A higher ratio means that a larger portion of each breath is wasted and not contributing to CO₂ elimination. This directly impacts alveolar ventilation and PaCO₂ levels.
Alveolar ventilation (VA) is the portion of minute ventilation that actually participates in gas exchange. It depends on tidal volume minus dead space:
VA = (VT − VD) × respiratory rate
When VD increases relative to VT, alveolar ventilation decreases unless compensation occurs. If compensation does not occur, CO₂ retention develops, leading to respiratory acidosis.
Note: For respiratory therapists, this concept is central to clinical decision-making. A patient may have a normal or even elevated minute ventilation, yet still retain CO₂ if the VD/VT ratio is high.
Causes of an Increased VD/VT Ratio
An increase in the VD/VT ratio can occur through two main mechanisms:
1. Decreased Tidal Volume
Rapid, shallow breathing reduces VT while dead space remains relatively fixed. As tidal volume decreases, dead space occupies a greater proportion of each breath.
This pattern is commonly seen in:
- Postoperative patients in pain
- Patients with respiratory muscle fatigue
- Individuals with restrictive lung disease
Note: Even if the respiratory rate increases, alveolar ventilation may fall because most of the ventilation is wasted in dead space.
2. Increased Physiologic Dead Space
Alveolar dead space increases when alveoli are ventilated but not adequately perfused. This creates ventilation-perfusion mismatch.
Common causes include:
- Pulmonary embolism
- Acute respiratory distress syndrome (ARDS)
- Pulmonary hypertension
- Congestive heart failure
- Severe emphysema
Note: In these conditions, more alveoli fail to exchange CO₂ effectively, increasing wasted ventilation.
VD/VT and Mechanical Ventilation
The VD/VT ratio plays a critical role in the management of mechanically ventilated patients.
Added Mechanical Dead Space
Additional tubing, connectors, heat and moisture exchangers, or improperly placed equipment can increase exogenous dead space. This increases VD and may elevate PaCO₂ unless tidal volume or respiratory rate is adjusted.
Weaning and Liberation
The VD/VT ratio has been used to evaluate readiness for liberation from mechanical ventilation. A VD/VT ratio greater than 0.60 is often associated with poor weaning outcomes and may indicate the need for continued ventilatory support.
A high VD/VT suggests that the patient must generate a significantly higher minute ventilation to maintain normal PaCO₂. This increases the work of breathing and oxygen consumption by respiratory muscles.
ARDS and Prognosis
In early ARDS, an elevated VD/VT ratio has been associated with increased mortality risk. This reflects severe ventilation-perfusion mismatch and impaired pulmonary perfusion.
Note: For respiratory therapists working in critical care, monitoring this ratio can provide insight into disease severity and response to therapy.
Exercise and the VD/VT Ratio
In healthy individuals, the VD/VT ratio typically decreases during exercise. Although both tidal volume and dead space increase with increased ventilation, tidal volume increases proportionally more. This reduces the fraction of wasted ventilation.
This physiologic response improves alveolar ventilation efficiency and supports increased metabolic demands.
In contrast, patients with significant pulmonary disease may not experience this beneficial reduction. Instead, they may struggle to increase tidal volume sufficiently, resulting in persistent or worsening hypercapnia during exertion.
Breathing Patterns and Efficiency
The VD/VT ratio helps explain why slow, deep breathing is more efficient than rapid, shallow breathing. When tidal volume increases, a smaller proportion of each breath is occupied by dead space. More of the inhaled air reaches perfused alveoli, improving CO₂ elimination.
Rapid, shallow breathing results in a high proportion of wasted ventilation. Even though minute ventilation may appear adequate, effective alveolar ventilation is low.
This is especially relevant in patients with:
- Neuromuscular weakness
- Postoperative splinting
- Anxiety-induced tachypnea
- Advanced lung disease
Note: Respiratory therapists frequently coach patients to use deeper, controlled breathing to improve ventilatory efficiency.
Work of Breathing and Compensation
When VD/VT increases, the body must compensate to maintain normal PaCO₂. This usually requires increasing minute ventilation. The most effective way to compensate is by increasing tidal volume rather than respiratory rate. However, increasing tidal volume increases the elastic work of breathing and oxygen consumption by respiratory muscles.
In patients with limited cardiopulmonary reserve, this compensation may not be sustainable. If the respiratory muscles fatigue, alveolar ventilation decreases and CO₂ retention worsens. This progression may ultimately require mechanical ventilation.
Clinical Significance in Respiratory Care
For respiratory therapists, the VD/VT ratio provides valuable information in several areas:
- Interpretation of arterial blood gases
- Evaluation of ventilation-perfusion mismatch
- Monitoring disease progression
- Adjusting ventilator settings
- Assessing readiness for extubation
- Evaluating the impact of added equipment
Note: A rising PaCO₂ despite adequate minute ventilation should prompt consideration of an increased VD/VT ratio. Understanding this ratio allows clinicians to look beyond simple respiratory rate and tidal volume values and assess the true efficiency of ventilation.
Dead Space/Tidal Volume Ratio Practice Questions
1. What does the dead space to tidal volume ratio (VD/VT) represent?
The fraction of each tidal breath that does not participate in gas exchange and therefore does not contribute to carbon dioxide elimination.
2. What types of dead space are included in the VD/VT ratio?
Physiologic dead space, which includes both anatomic dead space and alveolar dead space.
3. What equation is used to calculate the VD/VT ratio at the bedside?
The Enghoff modification of the Bohr equation: VD/VT = (PaCO2 − PECO2) / PaCO2.
4. What does PaCO2 represent in the VD/VT calculation?
The arterial partial pressure of carbon dioxide obtained from an arterial blood gas sample.
5. What does PECO2 represent in the VD/VT equation?
The partial pressure of carbon dioxide in mixed expired gas.
6. Why is PECO2 always lower than PaCO2 in normal lungs?
Because expired gas includes air from anatomic and alveolar dead space that contains little or no CO2.
7. What is the normal VD/VT ratio in a healthy adult?
Approximately 0.20 to 0.40, with an average value near 0.30.
8. If a patient has a PaCO2 of 40 mm Hg and a PECO2 of 28 mm Hg, what is the VD/VT ratio?
(40 − 28) / 40 = 0.30, indicating that 30% of the breath is dead space.
9. What would a VD/VT ratio of zero indicate?
That all exhaled gas participates in gas exchange and PECO2 equals PaCO2, which does not occur in normal physiology.
10. How does exercise affect the VD/VT ratio in healthy individuals?
The ratio decreases because tidal volume increases proportionally more than dead space.
11. Why does rapid, shallow breathing increase the VD/VT ratio?
Because a smaller tidal volume increases the proportion of each breath occupied by fixed anatomic dead space.
12. How does an increased VD/VT ratio affect alveolar ventilation?
It decreases alveolar ventilation and leads to impaired CO2 elimination.
13. What happens to PaCO2 if VD/VT increases and minute ventilation does not compensate?
PaCO2 rises, resulting in hypercapnia and potentially respiratory acidosis.
14. What breathing pattern is most efficient for minimizing dead space ventilation?
Slow, deep breathing.
15. How can added ventilator tubing affect the VD/VT ratio?
It increases mechanical (exogenous) dead space and raises the VD/VT ratio.
16. Which lung condition commonly increases alveolar dead space and VD/VT?
Pulmonary embolism
17. Why does pulmonary embolism increase dead space?
Because ventilated alveoli are not perfused, creating areas of wasted ventilation.
18. How does acute respiratory distress syndrome (ARDS) affect VD/VT?
It often increases VD/VT due to ventilation-perfusion mismatch and alveolar damage.
19. How can congestive heart failure influence the VD/VT ratio?
It may increase VD/VT due to ventilation-perfusion abnormalities and pulmonary vascular congestion.
20. Why must minute ventilation increase when VD/VT rises?
To maintain adequate alveolar ventilation and prevent CO2 retention.
21. What is the physiologic consequence of failing to compensate for increased dead space?
Inadequate alveolar ventilation and respiratory acidosis.
22. Why does increasing tidal volume help compensate for increased dead space?
Because a larger portion of each breath reaches perfused alveoli for gas exchange.
23. What is the downside of increasing tidal volume to compensate for high VD/VT?
Increased work of breathing and greater oxygen consumption by respiratory muscles.
24. How can rapid shallow breathing result in hypercapnia despite high minute ventilation?
Because most of the ventilation is wasted in dead space.
25. Why is VD/VT useful when evaluating readiness for liberation from mechanical ventilation?
A high VD/VT indicates inefficient ventilation and difficulty eliminating CO2 independently.
26. What VD/VT value generally suggests a patient may not be ready for ventilator liberation?
A value greater than 0.60.
27. How is PECO2 commonly measured at the bedside?
By collecting mixed expired gas or estimating it using capnography.
28. What assumption is made in the Bohr equation regarding inspired gas?
That inspired gas contains no carbon dioxide.
29. Why does increased physiologic dead space reduce the efficiency of ventilation?
Because a larger fraction of each breath does not participate in CO2 exchange.
30. How is early elevation of VD/VT in ARDS associated with prognosis?
An increased VD/VT early in ARDS is associated with higher mortality risk.
31. What does the dead space to tidal volume ratio (VD/VT) measure?
The fraction of tidal volume that does not participate in gas exchange, representing ventilation without perfusion.
32. What is the normal VD/VT ratio in healthy adults?
Approximately 0.20 to 0.40 (20% to 40%).
33. What VD/VT value is generally considered critical in mechanically ventilated patients?
A value greater than 0.60, indicating severely impaired ventilation efficiency.
34. What is the correct formula for calculating VD/VT using the Enghoff modification of the Bohr equation?
VD/VT = (PaCO2 − PECO2) / PaCO2
35. How is VD/VT expressed if calculated as a percentage?
[(PaCO2 − PECO2) / PaCO2] × 100
36. What does PECO2 represent in the VD/VT calculation?
The partial pressure of CO2 in mixed expired gas.
37. If PaCO2 is 40 mm Hg and PECO2 is 30 mm Hg, what is the VD/VT ratio?
(40 − 30) / 40 = 0.25, or 25%
38. What does an increase in VD/VT suggest clinically?
The presence of increased dead space, often due to ventilation-perfusion mismatch such as pulmonary embolism.
39. If the VD/VT ratio and tidal volume are known, how can dead space volume (VD) be calculated?
VD = (VD/VT) × VT
40. What is minute ventilation (VE) and how is it calculated?
Minute ventilation is the total volume of air breathed per minute and is calculated as VE = VT × respiratory rate.
41. What does the dot over the V (V̇) signify in respiratory physiology?
It indicates flow or volume per unit time, such as ventilation per minute.
42. What is anatomic dead space?
The volume of air in the conducting airways where no gas exchange occurs.
43. What is the approximate anatomic dead space in adults?
About 150 mL or approximately 1 mL per pound of ideal body weight.
44. What is alveolar dead space?
Ventilated alveoli that are not perfused and therefore do not participate in gas exchange.
45. What is physiologic dead space?
The sum of anatomic dead space and alveolar dead space.
46. Why does increased alveolar dead space raise the VD/VT ratio?
Because more ventilated air fails to exchange CO2 with pulmonary capillary blood.
47. How does rapid shallow breathing affect VD/VT?
It increases the ratio because a larger proportion of each small tidal breath is occupied by fixed anatomic dead space.
48. What breathing pattern improves ventilation efficiency in patients with increased dead space?
Slow, deep breathing that increases tidal volume.
49. How does hyperventilation affect PaCO2 levels?
It lowers PaCO2 below the normal range of 35 to 45 mm Hg.
50. What acid-base disturbance is associated with hyperventilation?
Respiratory alkalosis
51. How does hypoventilation affect PaCO2 levels?
It raises PaCO2 above 45 mm Hg.
52. What acid-base disturbance results from hypoventilation?
Respiratory acidosis
53. Why can a patient have a high minute ventilation but still retain CO2?
Because a high VD/VT ratio causes much of the ventilation to be wasted in dead space.
54. How does pulmonary embolism affect ventilation efficiency?
It increases alveolar dead space, raising VD/VT and impairing CO2 elimination.
55. Why is VD/VT an important parameter when assessing readiness for ventilator weaning?
Because a high ratio indicates inefficient ventilation and difficulty maintaining normal PaCO2 independently.
56. How does increased dead space increase the work of breathing?
Because the patient must increase minute ventilation to maintain adequate alveolar ventilation.
57. What happens to alveolar ventilation if dead space increases and tidal volume remains unchanged?
Alveolar ventilation decreases, leading to CO2 retention.
58. Why is VD/VT considered an index of ventilatory efficiency?
Because it quantifies the proportion of each breath that is effectively exchanging CO2.
59. How does mechanical dead space from added tubing affect ventilated patients?
It increases VD/VT and may require adjustments in tidal volume or respiratory rate.
60. Why is understanding VD/VT essential for respiratory therapists?
Because it helps guide ventilator adjustments, assess gas exchange efficiency, and evaluate disease severity.
61. How does acute respiratory distress syndrome (ARDS) typically affect the VD/VT ratio?
It increases the VD/VT ratio due to increased alveolar dead space from impaired perfusion and lung injury.
62. Why does congestive heart failure (CHF) often increase VD/VT?
Because reduced cardiac output decreases pulmonary perfusion, increasing alveolar dead space.
63. What happens to VD/VT during exercise in healthy individuals?
It decreases because tidal volume increases proportionally more than dead space.
64. Why does increasing tidal volume lower the VD/VT ratio?
Because a larger portion of each breath reaches perfused alveoli relative to fixed anatomic dead space.
65. How does severe hypotension affect dead space?
It increases alveolar dead space due to reduced pulmonary blood flow.
66. What is the relationship between alveolar ventilation (VA) and VD/VT?
As VD/VT increases, alveolar ventilation decreases if minute ventilation remains constant.
67. What is the formula for alveolar ventilation (VA)?
VA = (VT − VD) × respiratory rate.
68. How does increasing respiratory rate without increasing VT affect VD/VT?
It increases wasted ventilation and may worsen CO2 retention.
69. Why is PECO2 always lower than PaCO2 in normal lungs?
Because mixed expired gas includes air from anatomic dead space that contains no CO2.
70. What clinical condition is strongly associated with a sudden rise in VD/VT?
Pulmonary embolism
71. How can capnography help estimate VD/VT?
By measuring end-tidal CO2 (PETCO2) as a surrogate for PECO2.
72. Why might PETCO2 underestimate PaCO2 in patients with high dead space?
Because ventilation-perfusion mismatch widens the gradient between arterial and exhaled CO2.
73. What does a widening PaCO2–PETCO2 gradient suggest?
Increasing dead space or worsening ventilation-perfusion mismatch.
74. How does positive pressure ventilation influence dead space?
It may increase alveolar dead space if overdistention reduces capillary perfusion.
75. Why is VD/VT useful in assessing severity of lung disease?
Because higher values indicate greater inefficiency of ventilation.
76. What happens to VD/VT in patients with severe emphysema?
It increases due to destruction of pulmonary capillaries and alveolar dead space.
77. How does auto-PEEP contribute to increased dead space?
By trapping air and reducing effective alveolar ventilation.
78. Why is VD/VT important when adjusting ventilator settings?
Because high dead space may require higher minute ventilation to maintain normal PaCO2.
79. How does adding excessive circuit tubing affect ventilation?
It increases mechanical dead space and raises VD/VT.
80. Why should unnecessary connectors be removed from a ventilator circuit?
To reduce added dead space and improve ventilation efficiency.
81. What effect does shallow breathing have on alveolar ventilation?
It reduces alveolar ventilation by increasing the proportion of dead space ventilation.
82. How does pulmonary hypertension affect VD/VT?
It increases VD/VT by reducing effective pulmonary perfusion.
83. Why is VD/VT elevated in shock states?
Because decreased cardiac output reduces perfusion to ventilated alveoli.
84. What is the physiologic consequence of a VD/VT ratio approaching 1.0?
Nearly all ventilation is wasted and effective gas exchange is minimal.
85. How does increasing inspiratory flow affect dead space?
It does not directly change dead space but may affect patient comfort and synchrony.
86. Why must VT often be increased in patients with high dead space?
To maintain adequate alveolar ventilation and normalize PaCO2.
87. What happens to oxygen consumption when minute ventilation is increased to compensate for dead space?
Oxygen consumption increases due to higher work of breathing.
88. Why is VD/VT monitored in ARDS prognosis?
Because elevated early VD/VT is associated with higher mortality.
89. How does chronic lung fibrosis influence dead space?
It increases physiologic dead space due to impaired perfusion and altered lung architecture.
90. What does a normal VD/VT with elevated PaCO2 suggest?
Hypoventilation rather than increased dead space.
91. Why can obesity contribute to elevated PaCO2 without increasing VD/VT?
Because hypoventilation may occur without significant dead space changes.
92. How does mechanical ventilation with small VT strategy affect VD/VT?
It may increase VD/VT proportionally, requiring adjustment in respiratory rate.
93. Why is VD/VT an indicator of ventilation-perfusion mismatch?
Because increased mismatch increases the fraction of ventilation not participating in gas exchange.
94. How does pulmonary blood flow influence alveolar dead space?
Reduced blood flow increases alveolar dead space.
95. What happens to VD/VT after successful treatment of pulmonary embolism?
It typically decreases as perfusion improves.
96. Why is mixed expired CO2 required for accurate VD/VT calculation?
Because it represents the average CO2 concentration of the entire expired breath.
97. How does severe bronchospasm affect VD/VT?
It may increase physiologic dead space due to uneven ventilation distribution.
98. Why is monitoring VD/VT important during weaning trials?
Because elevated dead space predicts difficulty maintaining normal PaCO2 independently.
99. How does high PEEP potentially affect VD/VT?
Excessive PEEP can overdistend alveoli and reduce perfusion, increasing dead space.
100. Why is VD/VT considered a more sensitive marker of ventilatory efficiency than minute ventilation alone?
Because minute ventilation does not distinguish between effective and wasted ventilation.
Final Thoughts
The dead space to tidal volume ratio provides meaningful insight into ventilatory efficiency and carbon dioxide elimination. An elevated VD/VT ratio indicates that a greater portion of each breath is not contributing to gas exchange, which can lead to increased PaCO₂ if not properly compensated.
In both spontaneous and mechanically ventilated patients, this measurement helps guide adjustments in breathing patterns and ventilator settings. A clear understanding of VD/VT allows respiratory therapists to identify ineffective ventilation early and support appropriate clinical intervention.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Zheng M. Dead space ventilation-related indices: bedside tools to evaluate the ventilation and perfusion relationship in patients with acute respiratory distress syndrome. Crit Care. 2023.