Chronic obstructive pulmonary disease (COPD) is a progressive lung disorder that makes breathing increasingly difficult and is a leading cause of illness and death worldwide. The condition is most commonly associated with long-term cigarette smoking, although exposure to air pollution, occupational dust, and chemical irritants can also contribute to its development.
COPD is not a single disease but rather a group of disorders that cause persistent airflow limitation and chronic inflammation of the airways and lung tissue. The airflow obstruction typically worsens over time and is not fully reversible.
Take our free course to master essential pathology concepts with TMC/CSE exam tips and helpful practice questions.
The two primary forms of COPD are emphysema and chronic bronchitis. These conditions have distinct clinical characteristics but frequently occur together in many patients.
Understanding the differences between emphysema and chronic bronchitis is essential for students preparing for the respiratory therapy board exam and for healthcare professionals responsible for diagnosing and managing patients with COPD.
This article explains the key features, diagnostic findings, and management strategies associated with each condition while highlighting important board exam tips that help reinforce high-yield concepts.
What is COPD?
Chronic obstructive pulmonary disease (COPD) is a chronic and progressive respiratory disorder characterized by persistent airflow limitation. The disease develops as a result of chronic inflammation that damages the airways, lung tissue, and alveoli.
This damage reduces the ability of air to move efficiently in and out of the lungs, which leads to symptoms such as dyspnea, chronic cough, and excessive mucus production. Over time, lung function gradually declines, particularly if exposure to harmful irritants continues.
Airflow limitation in COPD is typically confirmed through pulmonary function testing, where spirometry shows a reduced FEV1/FVC ratio consistent with obstructive lung disease.
Causes and Risk Factors
- Smoking: The most common cause of COPD. Long-term tobacco exposure leads to airway inflammation and destruction of lung tissue.
- Environmental exposure: Prolonged exposure to secondhand smoke, occupational dust, chemical fumes, and industrial pollutants such as coal dust, silica, or asbestos.
- Air pollution: Chronic exposure to polluted air can accelerate lung damage and worsen symptoms.
- Genetic disorders: In rare cases, alpha-1 antitrypsin deficiency can lead to early-onset emphysema, even in patients who have never smoked.
- Respiratory infections: Recurrent respiratory infections during childhood may increase the risk of developing COPD later in life.
Board Exam Tip: Smoking is the most common cause of COPD and should be the first risk factor considered when answering exam questions. If the question describes a younger patient with emphysema who has little or no smoking history, consider alpha-1 antitrypsin deficiency.
Management of COPD
The primary goals of COPD management are to improve the patient’s quality of life, reduce symptoms, prevent exacerbations, and slow disease progression. Treatment strategies depend on the severity of airflow limitation and whether the patient is stable or experiencing an acute exacerbation.
Conservative Management (Stable COPD)
- Low-flow oxygen therapy such as nasal cannula at 1 to 2 L/min to maintain SpO₂ between 88% and 92%
- Long-acting bronchodilators including beta-agonists and anticholinergic medications to relax airway smooth muscle and improve airflow
- Inhaled corticosteroids to reduce airway inflammation and decrease exacerbation frequency
- Smoking cessation, which is the single most important intervention to slow disease progression
- Pulmonary rehabilitation programs to improve exercise tolerance, respiratory muscle strength, and overall functional capacity
- Patient education focused on medication adherence, avoiding respiratory irritants, and recognizing early signs of exacerbations
- Vaccinations including influenza and pneumococcal vaccines to prevent respiratory infections that can worsen COPD
- Healthy lifestyle habits such as regular physical activity, proper nutrition, and adequate hydration
Management During an Acute Exacerbation
- Increase FiO₂ to correct hypoxemia while maintaining an SpO₂ target of 88% to 92%
- Short-acting bronchodilators such as albuterol and anticholinergics such as ipratropium to relieve bronchoconstriction
- Systemic corticosteroids to reduce airway inflammation and improve airflow
- Chest X-ray to rule out pneumonia, pneumothorax, or other complications
- Arterial blood gas (ABG) analysis to assess ventilation and oxygenation status
- Noninvasive ventilation (BiPAP) for patients experiencing ventilatory failure. This is preferred over intubation when possible.
- Mechanical ventilation if respiratory failure progresses despite noninvasive support
Board Exam Tips: Stable COPD often shows compensated respiratory acidosis on ABG analysis due to chronic CO₂ retention. During an acute exacerbation, ABGs frequently show uncompensated respiratory acidosis. Patients with COPD may also be difficult to wean from mechanical ventilation because of chronic respiratory muscle fatigue.
Signs and Symptoms of an Acute Exacerbation
An acute exacerbation of COPD occurs when respiratory symptoms suddenly worsen beyond the patient’s normal daily variation. These episodes are often triggered by respiratory infections, environmental irritants, or poor adherence to treatment.
Exacerbations can significantly impair gas exchange and frequently require urgent medical evaluation and treatment.
Common Signs and Symptoms
- Dyspnea with a sudden increase in breathing difficulty
- Shortness of breath that may occur even at rest
- Wheezing caused by airway narrowing and bronchospasm
- Chest tightness related to airflow limitation
- Tachypnea or rapid breathing
- Tachycardia due to increased respiratory effort and hypoxemia
- Hypoxemia with reduced oxygen saturation
- Cyanosis, which appears as bluish discoloration of the lips or skin
- Persistent cough with increased frequency
- Increased mucus production that may be thick, yellow, or purulent
- Use of accessory breathing muscles including the sternocleidomastoid and scalene muscles
- Peripheral edema resulting from right-sided heart strain (cor pulmonale)
Key Clinical Considerations
- Always evaluate ABG results to determine whether ventilation is worsening and if CO₂ retention is present.
- A chest X-ray may be required to rule out pneumonia, pneumothorax, or other complications.
- Repeated exacerbations can accelerate the decline in lung function and increase hospitalization risk.
Board Exam Tip: If a patient with COPD presents with worsening dyspnea, wheezing, and hypoxemia, the correct management usually includes supplemental oxygen with a target SpO₂ of 88% to 92%, administration of a short-acting bronchodilator, systemic corticosteroids, and consideration of BiPAP if ventilatory failure develops.
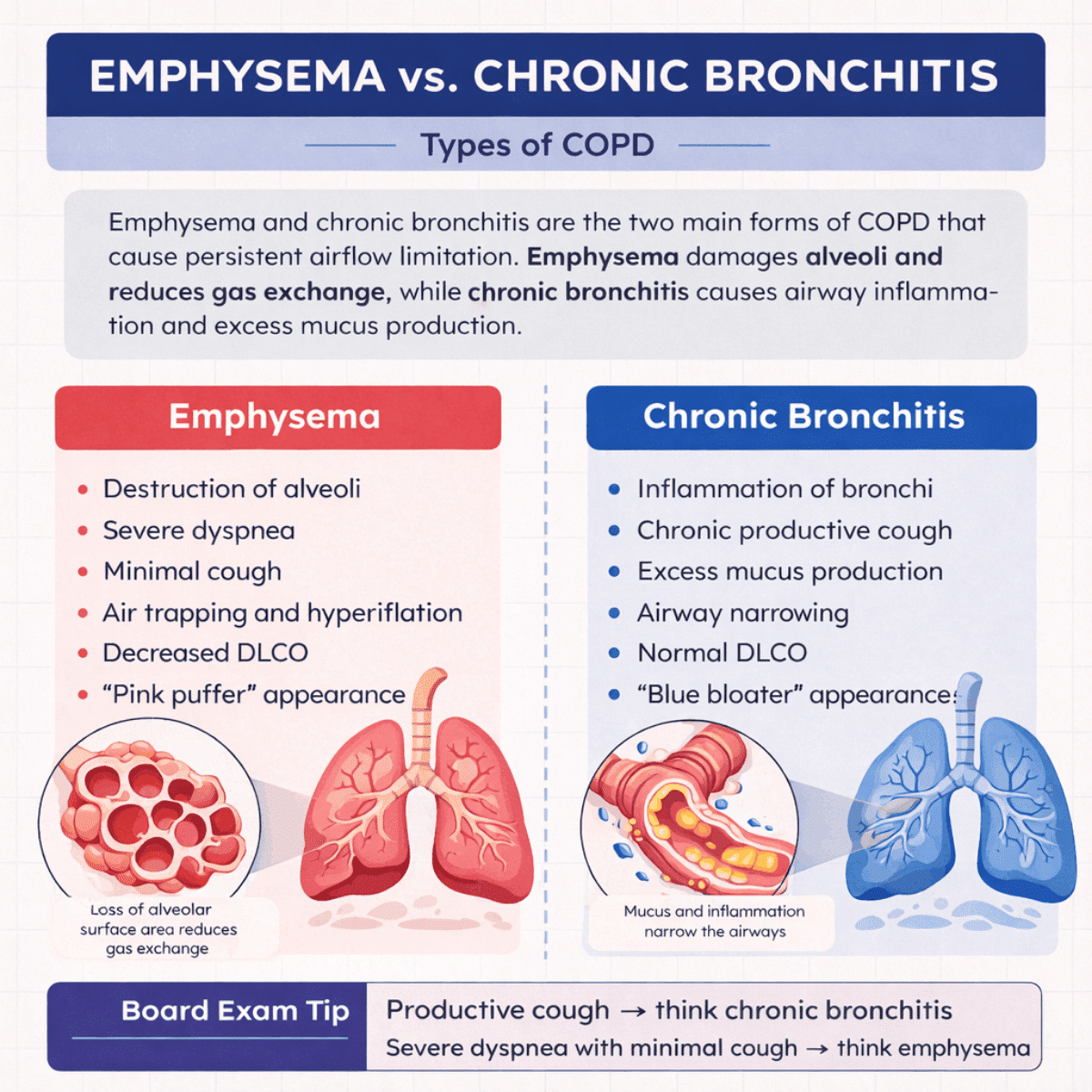
Key Differences Between Emphysema and Chronic Bronchitis
COPD most commonly presents as either emphysema or chronic bronchitis. Many patients exhibit features of both conditions, but understanding their distinguishing characteristics is important for diagnosis and board exam preparation.
Emphysema
Emphysema is characterized by the destruction of alveolar walls and enlargement of airspaces distal to the terminal bronchioles. This structural damage reduces elastic recoil, causes air trapping, and significantly impairs gas exchange.
- Appearance: Often described as a “pink puffer” with a thin body habitus, barrel chest, pursed-lip breathing, and use of accessory muscles
- Dyspnea: Severe and progressive shortness of breath
- Cough: Minimal cough with little mucus production
- Breath sounds: Diminished with possible wheezing
- ABGs: Compensated respiratory acidosis with moderate hypoxemia
- Chest X-ray: Hyperinflation, flattened diaphragm, and a small appearing cardiac silhouette
- Percussion: Hyperresonant
- PFTs: Reduced expiratory flow rates
- Lung volumes: Increased residual volume (RV) and total lung capacity (TLC)
- DLCO: Decreased due to destruction of alveolar surface area
- Lung compliance: Increased because of loss of elastic recoil
Chronic Bronchitis
Chronic bronchitis involves persistent inflammation of the bronchial tubes, excessive mucus production, and narrowing of the airways. The condition is clinically defined as a productive cough lasting at least three months per year for two consecutive years.
- Appearance: Often referred to as a “blue bloater” with a stocky body habitus, chronic hypoxemia, cyanosis, and possible peripheral edema
- Dyspnea: Typically milder compared to emphysema
- Cough: Frequent productive cough with thick mucus
- Breath sounds: Rhonchi and wheezing
- ABGs: Respiratory acidosis with moderate hypoxemia
- Chest X-ray: Enlarged cardiac silhouette and increased cardiothoracic ratio
- Percussion: Usually normal
- PFTs: Reduced expiratory flow rates
- Lung volumes: Increased residual volume
- DLCO: Typically normal
- Lung compliance: Usually normal
Clinical Considerations
- Emphysema patients frequently appear thin because the increased work of breathing requires significant energy expenditure.
- Chronic bronchitis patients are more prone to pulmonary hypertension and right-sided heart failure due to chronic hypoxemia.
- Airway clearance therapy is particularly beneficial for chronic bronchitis because it helps mobilize thick secretions.
Board Exam Tips
- Remember the classic descriptions: pink puffer for emphysema and blue bloater for chronic bronchitis.
- DLCO is a major differentiating factor. It is decreased in emphysema and usually normal in chronic bronchitis.
- On the board exam, severe dyspnea with minimal cough typically suggests emphysema.
- A chronic productive cough with thick mucus strongly suggests chronic bronchitis.
Summary and Board Exam Strategy
Chronic obstructive pulmonary disease (COPD) is a long-term progressive respiratory disorder most commonly caused by cigarette smoking and environmental irritants. The two main forms, emphysema and chronic bronchitis, both cause airflow limitation but differ in their underlying pathology and clinical presentation.
- Emphysema involves destruction of alveolar walls, loss of elastic recoil, severe dyspnea, and decreased DLCO.
- Chronic bronchitis involves airway inflammation, excessive mucus production, and a persistent productive cough.
Management focuses on improving symptoms, preventing exacerbations, and slowing disease progression through therapies such as bronchodilators, corticosteroids, pulmonary rehabilitation, smoking cessation, and supplemental oxygen when needed.
During acute exacerbations, treatment may include increased oxygen therapy, short-acting bronchodilators, systemic corticosteroids, ABG monitoring, and noninvasive ventilation such as BiPAP.
Key Takeaways
- The SpO₂ goal for COPD patients is typically 88% to 92%.
- Stable COPD often shows compensated respiratory acidosis.
- Acute exacerbations frequently show uncompensated respiratory acidosis.
- Emphysema often shows hyperinflation and a small cardiac silhouette on chest X-ray.
- Chronic bronchitis frequently presents with copious mucus production and may lead to cor pulmonale.
Final Thoughts
COPD continues to be a major global health concern, but understanding the pathophysiology, clinical presentation, and treatment strategies of emphysema and chronic bronchitis is essential for both patient care and success on the respiratory therapy board exam.
By recognizing the key differences between these conditions and mastering high-yield clinical concepts, students and healthcare professionals can be better prepared to diagnose, manage, and treat patients with COPD.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Agarwal AK, Raja A, Brown BD. Chronic Obstructive Pulmonary Disease. [Updated 2023 Aug 7]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025.
- Pahal P, Avula A, Afzal M. Emphysema. [Updated 2025 Mar 28]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025.
- Widysanto A, Goldin J, Mathew G. Chronic Bronchitis. [Updated 2025 Feb 6]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025.