The esophagus is a vital yet often overlooked structure that plays an important role in both digestion and respiratory health. While it is primarily known as the muscular tube that transports food from the throat to the stomach, its close anatomical and functional relationship with the airway makes it highly relevant to respiratory therapists.
Disorders of the esophagus can directly impact breathing, gas exchange, and airway protection.
Understanding its structure and function helps respiratory care practitioners recognize complications such as aspiration, reflux-related lung disease, and airway-esophageal misplacement during critical procedures.
What Is the Esophagus?
The esophagus is a muscular, collapsible tube that connects the pharynx (throat) to the stomach and serves as a passageway for food, liquids, and saliva. In adults, it measures about 25 centimeters (10 inches) in length and lies directly behind the trachea within the thoracic cavity. Its primary function is to transport swallowed material to the stomach through coordinated, wave-like muscle contractions known as peristalsis.
The esophageal wall is composed of several layers, including mucosa, submucosa, and muscle layers that allow it to expand and contract efficiently. The upper portion contains skeletal muscle, which allows voluntary control during the initiation of swallowing, while the lower portion contains smooth muscle that functions involuntarily.
Two important sphincters, the upper and lower esophageal sphincters, help regulate the passage of material and prevent reflux. Although it belongs to the digestive system, the esophagus is closely related to the airway and plays an important role in protecting the lungs during swallowing.
The Physiology of Swallowing
Swallowing, or deglutition, is a complex process involving both voluntary and involuntary phases. It is tightly coordinated with respiration to prevent aspiration.
There are three primary phases:
- Oral phase – Voluntary movement of food toward the pharynx
- Pharyngeal phase – Reflex closure of the airway and propulsion of the bolus
- Esophageal phase – Peristaltic movement through the esophagus
During swallowing, breathing momentarily stops in a process known as deglutition apnea. The epiglottis closes over the laryngeal inlet, and the vocal cords adduct to protect the airway. The upper esophageal sphincter (UES) relaxes to allow the bolus to enter the esophagus.
Note: The coordinated timing between swallowing and breathing is critical. Disruption of this coordination can result in aspiration, a major concern in respiratory care.
Esophagus vs. Trachea: What’s the Difference?
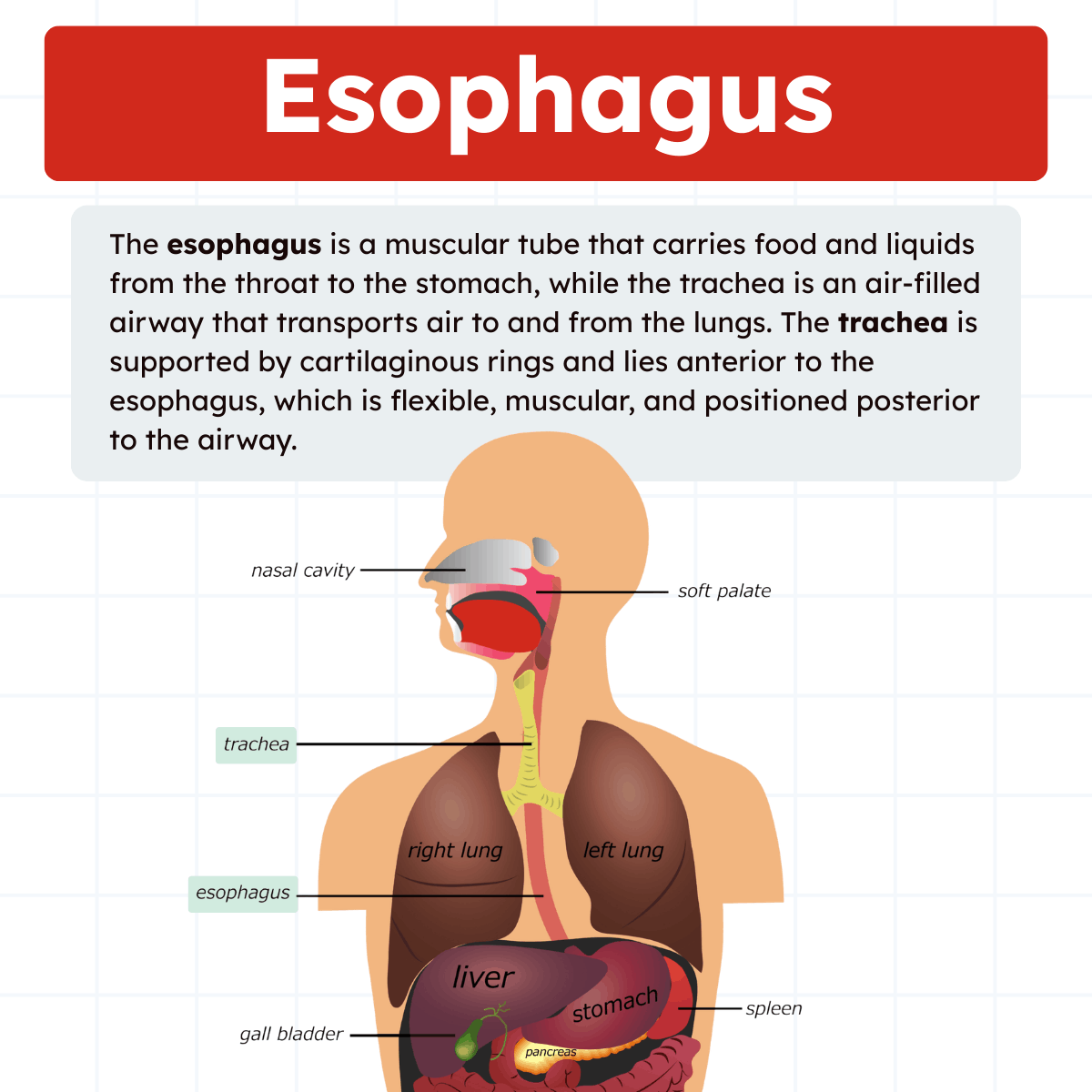
The esophagus and trachea are two separate tubes located in the neck and chest, but they serve very different functions. The esophagus is part of the digestive system and transports food and liquids from the pharynx to the stomach through coordinated muscular contractions called peristalsis. It is a flexible, muscular tube that lies posterior (behind) the trachea and remains collapsed except when swallowing.
The trachea, on the other hand, is part of the respiratory system and carries air from the upper airway to the lungs. It is supported by C-shaped cartilaginous rings that keep it open at all times to allow airflow. The trachea lies anterior (in front of) the esophagus and branches into the bronchi at the carina.
In short, the esophagus moves food to the stomach, while the trachea moves air to the lungs. Their close anatomical relationship is clinically important, especially during airway management and intubation.
Gastroesophageal Reflux and Respiratory Complications
One of the most important esophageal conditions in respiratory care is gastroesophageal reflux disease (GERD). GERD occurs when stomach contents flow backward into the esophagus due to lower esophageal sphincter (LES) dysfunction.
Although GERD is primarily a gastrointestinal condition, it has significant pulmonary consequences. Microaspiration of gastric contents can lead to:
- Chronic cough
- Wheezing
- Bronchospasm
- Recurrent pneumonia
- Exacerbations of asthma or COPD
Acid and pepsin entering the airway can cause inflammation and damage to the bronchial tree. In some patients, especially those who are intubated or mechanically ventilated, reflux increases the risk of ventilator-associated pneumonia (VAP).
Note: Respiratory therapists must be aware of positioning strategies, such as elevating the head of the bed to 30–45 degrees, to reduce aspiration risk.
Aspiration and Its Impact on the Lungs
Aspiration occurs when foreign material, such as food, liquids, or gastric contents, enters the airway. Esophageal dysfunction significantly increases this risk.
Common causes of aspiration include:
- Neurological disorders
- Impaired consciousness
- Stroke
- Sedation
- Mechanical ventilation
- Dysphagia
When aspiration occurs, it can lead to chemical pneumonitis or aspiration pneumonia. The severity depends on the volume and acidity of the aspirated material.
Respiratory therapists often encounter patients with compromised swallowing reflexes in intensive care units. Proper suctioning, cuff pressure monitoring in intubated patients, and collaboration with speech therapy are essential components of care.
Esophageal Disorders Relevant to Respiratory Care
Several esophageal conditions can directly or indirectly affect respiratory function. Because the esophagus lies immediately posterior to the trachea and shares protective mechanisms during swallowing, dysfunction can easily lead to aspiration, chronic airway irritation, or recurrent pulmonary infections.
For respiratory therapists, recognizing these conditions is essential when evaluating unexplained cough, wheezing, or repeated pneumonias.
Achalasia
Achalasia is a motility disorder characterized by failure of the lower esophageal sphincter (LES) to relax and impaired peristalsis. As a result, food and liquids accumulate in the esophagus instead of entering the stomach efficiently. This retained material can regurgitate, particularly when the patient lies flat, increasing the risk of aspiration into the lungs. Chronic microaspiration may lead to persistent cough, bronchospasm, or recurrent aspiration pneumonia.
Esophageal Strictures
Esophageal strictures involve narrowing of the esophageal lumen, often due to chronic inflammation, acid reflux, or scar tissue formation. This narrowing impairs swallowing and may cause food to become lodged. Patients with strictures are at higher risk for choking episodes and aspiration, especially if protective airway reflexes are compromised.
Hiatal Hernia
A hiatal hernia occurs when part of the stomach protrudes through the diaphragm into the thoracic cavity. This anatomical change can weaken the LES and worsen gastroesophageal reflux. Chronic reflux may irritate the airway, contributing to persistent cough, hoarseness, wheezing, or exacerbations of asthma and COPD.
Tracheoesophageal Fistula
A tracheoesophageal fistula (TEF) is an abnormal connection between the trachea and esophagus. This condition may be congenital or acquired, such as from prolonged intubation or trauma. TEF can result in severe aspiration, gastric distention during ventilation, and significant respiratory distress. In neonatal and pediatric respiratory care, congenital TEF is a critical diagnosis requiring immediate airway protection and surgical intervention.
Esophageal Intubation: A Critical Concern
For respiratory therapists, one of the most serious esophageal-related complications is accidental esophageal intubation.
Signs of esophageal intubation include:
- Absence of end-tidal CO₂
- No chest rise
- Epigastric sounds during ventilation
- Rapid desaturation
Prompt recognition and immediate correction are life-saving. Continuous waveform capnography is considered the gold standard for confirming proper tracheal tube placement.
Note: Understanding the anatomy of the esophagus in relation to the trachea helps reduce procedural errors during airway management.
Mechanical Ventilation and Esophageal Considerations
Patients on mechanical ventilation are at increased risk for reflux and aspiration. Positive pressure ventilation can increase intrathoracic pressure, potentially influencing esophageal sphincter function.
Additionally, prolonged supine positioning can promote gastric reflux.
Respiratory therapists must:
- Maintain appropriate head-of-bed elevation
- Monitor gastric residual volumes when applicable
- Ensure proper cuff inflation in endotracheal or tracheostomy tubes
- Be alert for signs of aspiration
Note: Preventing pulmonary complications associated with esophageal dysfunction is a key part of ventilator management.
Esophageal Pressure Monitoring in Respiratory Care
In advanced respiratory care, esophageal pressure monitoring can be used to estimate pleural pressure. A balloon catheter placed in the esophagus allows clinicians to measure pressure changes that reflect intrathoracic pressure.
This technique can help:
- Assess lung compliance
- Optimize ventilator settings
- Evaluate patient effort
- Guide PEEP titration
Note: Although not routinely used in all settings, esophageal pressure monitoring can provide valuable insight into lung mechanics in critically ill patients.
The Esophagus in Pediatric and Neonatal Care
In neonatal respiratory care, esophageal anatomy is particularly important. Premature infants and newborns are at higher risk for:
- Immature swallowing coordination
- Reflux
- Aspiration
Congenital anomalies such as tracheoesophageal fistula require immediate airway protection and surgical correction.
Respiratory therapists working in neonatal intensive care units must be vigilant about airway protection and recognize signs of feeding intolerance or respiratory compromise related to esophageal dysfunction.
Clinical Assessment and Interdisciplinary Collaboration
Because esophageal disorders often overlap with pulmonary symptoms, respiratory therapists must collaborate closely with physicians, nurses, speech-language pathologists, and gastroenterologists.
Symptoms such as chronic cough, unexplained wheezing, or recurrent pneumonia may warrant evaluation for underlying esophageal dysfunction.
Note: A comprehensive approach improves patient outcomes and reduces preventable respiratory complications.
Esophagus Practice Questions
1. What is the primary function of the esophagus?
The esophagus transports food and saliva from the laryngopharynx to the stomach.
2. What is the approximate length and diameter of the adult esophagus?
It is approximately 10 inches (25 cm) long and about 2 cm (¾ inch) in diameter.
3. What is the anatomical relationship of the esophagus to the thoracic vertebrae and trachea?
The esophagus lies anterior to the thoracic vertebrae and posterior to the trachea and heart.
4. As it descends into the thorax, to which side does the esophagus shift slightly?
It shifts slightly to the left as it approaches the stomach.
5. At what vertebral level does the esophagus begin?
It begins at the level of C6, at the inferior border of the cricoid cartilage.
6. At what vertebral level does the esophagus terminate?
It terminates at the cardiac orifice of the stomach at approximately the level of T11.
7. Through which structure does the esophagus pass to enter the abdomen?
It passes through the diaphragm at the esophageal hiatus.
8. In which anatomical plane does the esophagus primarily lie?
It lies primarily in the midsagittal plane (MSP).
9. Into what three anatomical regions is the esophagus divided?
The cervical, thoracic, and abdominal portions.
10. What are the four primary layers of the esophageal wall?
Mucosa, submucosa, muscularis externa, and adventitia.
11. What type of epithelium lines the mucosa of the esophagus?
Stratified squamous epithelium.
12. What is the function of the submucosa in the esophagus?
It contains esophageal glands that secrete mucus for lubrication.
13. What are the muscle fiber orientations in the muscularis externa?
Inner circular fibers and outer longitudinal fibers.
14. How does the muscle composition change along the length of the esophagus?
The upper third is skeletal muscle, the middle third is mixed skeletal and smooth muscle, and the lower third is smooth muscle.
15. What is the function of the upper esophageal sphincter (UES)?
It prevents air from entering the esophagus during respiration and prevents reflux into the pharynx.
16. What is the function of the lower esophageal sphincter (LES)?
It prevents gastric contents from refluxing into the esophagus.
17. What is peristalsis, and how does it relate to esophageal function?
Peristalsis is a series of coordinated, involuntary muscle contractions that propel food toward the stomach.
18. Where does the esophagus begin in relation to the laryngopharynx?
It begins at the distal end of the laryngopharynx at the level of C6.
19. What is the role of mucus in the esophagus?
Mucus lubricates and protects the esophageal lining during swallowing.
20. Why is the adventitia important in esophageal anatomy?
The adventitia anchors the esophagus to surrounding structures within the mediastinum.
21. Where is the esophagus primarily located within the body?
The esophagus is located mostly within the thoracic cavity, with a short terminal portion in the abdominal cavity before entering the stomach.
22. How does the esophagus relate anatomically to the aorta as it descends?
In the upper thorax, it lies to the right of the aorta, then deviates to the left around the level of T7 before passing through the diaphragm at T10.
23. At what vertebral level does the esophagus pass through the diaphragm?
It passes through the esophageal hiatus of the diaphragm at the level of T10.
24. What is the main function of the esophagus?
It transports food and liquids from the pharynx to the stomach through coordinated peristaltic contractions.
25. True or False: The abdominal portion of the esophagus leaves a groove in the left lobe of the liver before entering the stomach.
True
26. What anatomical landmark separates the left margin of the stomach from the fundus?
The cardiac notch.
27. What are the two major esophageal sphincters?
The upper esophageal sphincter (UES) and the lower esophageal sphincter (LES), also known as the cardiac sphincter.
28. Where is the upper esophageal sphincter located, and what is its function?
It is located at the entrance of the esophagus at the level of C6 and prevents air from entering the esophagus during respiration.
29. Where is the lower esophageal sphincter located, and what is its function?
It is located at the distal end of the esophagus and prevents reflux of gastric contents into the esophagus.
30. What is the approximate total length of the adult esophagus?
Approximately 25 cm (10 inches).
31. Into how many anatomical parts is the esophagus divided?
It is divided into cervical, thoracic, and abdominal portions.
32. What structures are anterior to the esophagus in the neck?
The trachea and the recurrent laryngeal nerves.
33. What structures are posterior to the esophagus in the neck?
The vertebral column and prevertebral muscles.
34. What major structures lie lateral to the cervical esophagus?
The thyroid gland, carotid sheath (containing the common carotid artery, internal jugular vein, and vagus nerve), and on the left side, the thoracic duct.
35. What is the arterial supply of the cervical portion of the esophagus?
It is supplied primarily by branches of the inferior thyroid arteries.
36. What is the venous drainage of the cervical esophagus?
It drains into the inferior thyroid veins.
37. What is the lymphatic drainage of the cervical esophagus?
It drains into the deep cervical lymph nodes.
38. What nerves supply the cervical portion of the esophagus?
The recurrent laryngeal nerves and branches of the sympathetic trunks.
39. What are the anterior relations of the thoracic esophagus?
The trachea, left main bronchus, left atrium, and left recurrent laryngeal nerve.
40. What are the posterior relations of the thoracic esophagus?
The vertebral column, thoracic duct, azygos vein, right posterior intercostal arteries, and descending thoracic aorta.
41. What structure does the esophagus pass through to enter the abdominal cavity?
It passes through the esophageal hiatus of the diaphragm at the level of T10.
42. What is the approximate length of the abdominal portion of the esophagus?
Approximately 1 to 2 cm before it enters the stomach.
43. What type of epithelium lines the esophageal mucosa?
Stratified squamous epithelium.
44. What type of muscle is found in the upper third of the esophagus?
Skeletal muscle
45. What type of muscle predominates in the lower third of the esophagus?
Smooth muscle
46. What is the function of peristalsis in the esophagus?
It propels food and liquids from the pharynx to the stomach through coordinated, wave-like contractions.
47. What is the clinical significance of the lower esophageal sphincter in respiratory care?
A weak lower esophageal sphincter increases the risk of gastric reflux and aspiration into the lungs.
48. How can gastroesophageal reflux disease (GERD) affect the respiratory system?
GERD can lead to chronic cough, bronchospasm, aspiration pneumonia, and worsening asthma symptoms.
49. Why is aspiration of gastric contents dangerous to the lungs?
It can cause chemical pneumonitis, airway inflammation, infection, and impaired gas exchange.
50. How does positive pressure ventilation increase the risk of gastric insufflation?
Positive pressure can force air into the stomach if airway pressures exceed esophageal sphincter pressure.
51. Why should bag-valve-mask ventilation be performed carefully in patients at risk for aspiration?
Excessive ventilation pressure may insufflate the stomach and increase aspiration risk.
52. What nerve provides parasympathetic innervation to the esophagus?
The vagus nerve.
53. What is the esophageal plexus?
A network of autonomic nerves formed primarily by branches of the vagus nerves around the esophagus.
54. What is the relationship between the esophagus and the trachea in the thorax?
The esophagus lies posterior to the trachea.
55. Why is knowledge of esophageal anatomy important during endotracheal intubation?
To avoid accidental esophageal intubation, which results in ineffective ventilation.
56. What is the most reliable method to confirm correct endotracheal tube placement and rule out esophageal intubation?
Continuous waveform capnography.
57. What happens if an endotracheal tube is placed in the esophagus?
Air enters the stomach instead of the lungs, leading to hypoxia and gastric distention.
58. How can severe esophageal dilation compress respiratory structures?
It may compress the trachea or bronchi, causing dyspnea or stridor.
59. What is achalasia, and how can it impact breathing?
Achalasia is failure of the lower esophageal sphincter to relax, leading to dilation and possible aspiration.
60. What condition occurs when abdominal contents herniate through the esophageal hiatus?
A hiatal hernia.
61. How can a large hiatal hernia affect respiratory function?
It may reduce lung expansion and contribute to dyspnea or reflux-related aspiration.
62. What vein drains the lower third of the esophagus?
The left gastric vein, a tributary of the portal vein.
63. Why are esophageal varices clinically significant?
They can rupture and cause massive bleeding, potentially leading to aspiration of blood.
64. What is the relationship between the esophagus and the left atrium?
The esophagus lies posterior to the left atrium in the thorax.
65. Why is transesophageal echocardiography (TEE) useful in cardiac imaging?
It provides detailed cardiac images from the esophagus due to its close proximity to the heart.
66. How does the upper esophageal sphincter protect the airway?
It prevents swallowed material from entering the airway during breathing.
67. What is the role of the crura of the diaphragm in esophageal function?
They help reinforce the lower esophageal sphincter and prevent reflux.
68. How can neuromuscular disorders affect the esophagus and respiration?
They may impair swallowing, increasing the risk of aspiration and respiratory complications.
69. What is the significance of the esophagus in patients receiving enteral feeding?
Improper tube placement into the airway instead of the esophagus can cause severe respiratory compromise.
70. Why is assessment of swallowing function important in respiratory patients?
Impaired swallowing increases the risk of aspiration pneumonia and respiratory failure.
71. What is the clinical purpose of inserting a nasogastric (NG) tube into the esophagus?
To decompress the stomach, administer nutrition, or remove gastric contents.
72. Why must proper NG tube placement be verified before use?
To ensure the tube is in the stomach and not in the trachea or lungs.
73. What bedside method is commonly used to help confirm gastric tube placement?
Measuring pH of aspirated contents and confirming placement with radiography.
74. How can esophageal intubation be quickly detected during resuscitation?
By the absence of sustained end-tidal CO2 on capnography.
75. What respiratory complication can result from chronic microaspiration due to reflux?
Recurrent pneumonia or chronic airway inflammation.
76. How does increased intra-abdominal pressure affect the lower esophageal sphincter?
It can promote reflux by overcoming sphincter pressure.
77. Why are mechanically ventilated patients at higher risk for aspiration?
Positive pressure ventilation and sedation can reduce lower esophageal sphincter tone.
78. What is the relationship between the esophagus and the mediastinum?
The esophagus runs through the posterior mediastinum.
79. What condition occurs when the esophagus ruptures and leaks contents into the mediastinum?
Esophageal perforation (Boerhaave syndrome).
80. Why is esophageal perforation life-threatening from a respiratory standpoint?
It can lead to mediastinitis, sepsis, pleural effusion, and respiratory failure.
81. How can severe esophageal reflux worsen asthma symptoms?
Acid irritation can trigger bronchospasm via vagal reflexes.
82. What reflex pathway connects esophageal irritation to bronchoconstriction?
The vagally mediated esophagobronchial reflex.
83. Why is head-of-bed elevation recommended in patients at risk for reflux?
It reduces the likelihood of gastric contents entering the esophagus and airway.
84. What is the normal resting pressure of the lower esophageal sphincter important for?
Preventing reflux and protecting the airway from aspiration.
85. How can obesity contribute to both reflux and respiratory compromise?
Increased abdominal pressure promotes reflux and restricts diaphragmatic movement.
86. What is the significance of the esophagus during bronchoscopy?
Accidental passage of the bronchoscope into the esophagus must be avoided.
87. How does esophageal cancer potentially affect breathing?
Tumor enlargement can compress the trachea or cause aspiration.
88. Why are patients with stroke at high risk for aspiration?
Neurologic impairment can disrupt coordinated swallowing and airway protection.
89. What is the role of the epiglottis in protecting the airway during swallowing?
It helps direct food away from the trachea and toward the esophagus.
90. How can chronic coughing affect the esophagus?
Increased intrathoracic pressure may worsen reflux symptoms.
91. What is a tracheoesophageal fistula?
An abnormal connection between the trachea and esophagus.
92. Why is a tracheoesophageal fistula dangerous in newborns?
It allows milk or secretions to enter the airway, causing aspiration and respiratory distress.
93. How does continuous positive airway pressure (CPAP) potentially affect gastric distention?
Excessive pressures may force air into the esophagus and stomach.
94. Why is careful pressure control important during noninvasive ventilation?
To minimize air swallowing and reduce aspiration risk.
95. What symptom may indicate esophageal compression of the airway?
Stridor or unexplained dyspnea.
96. How does diaphragmatic movement influence the lower esophageal sphincter?
Diaphragmatic contraction helps reinforce sphincter closure during inspiration.
97. Why is swallowing coordination important in patients with chronic lung disease?
Impaired coordination increases aspiration risk and respiratory infections.
98. What is the primary blood supply to the abdominal portion of the esophagus?
Branches of the left gastric artery.
99. How can portal hypertension affect the esophagus?
It can lead to esophageal varices that may rupture and compromise the airway.
100. Why should suction equipment be readily available when managing patients with upper GI bleeding?
To prevent aspiration of blood into the respiratory tract.
Final Thoughts
The esophagus may be part of the digestive system, but its impact on respiratory health is significant. Its close anatomical relationship with the trachea, its role in airway protection during swallowing, and its involvement in conditions such as reflux and aspiration make it highly relevant in respiratory care.
For respiratory therapists, understanding the structure and function of the esophagus enhances patient safety during airway management, mechanical ventilation, and critical care interventions.
By recognizing the connection between esophageal dysfunction and pulmonary complications, clinicians can provide more comprehensive and preventive respiratory care.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Bajwa SA, Toro F, Kasi A. Physiology, Esophagus. [Updated 2023 May 1]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025.

