The trachea, often called the windpipe, is a vital part of the respiratory system that allows air to travel from the upper airway to the lungs. Every breath relies on this flexible yet sturdy structure to maintain open airflow and support normal breathing.
Despite its essential role, the trachea often receives little attention until a problem arises. Numerous conditions can affect the trachea, ranging from inflammation and structural abnormalities to trauma, tumors, and external compression.
Some disorders develop rapidly and require urgent care, while others progress slowly and mimic common respiratory conditions. This article explores how tracheal disorders develop, how they are identified, and how they are effectively managed.
What Is the Trachea?
The trachea, commonly known as the windpipe, is a key structure of the respiratory system that serves as the main passageway for air traveling between the upper airway and the lungs. It begins just below the larynx and extends downward into the chest, where it divides into the right and left main bronchi.
The trachea is supported by C-shaped rings of cartilage that keep the airway open while allowing flexibility during breathing and swallowing. Its inner lining contains mucus-producing cells and tiny hair-like structures called cilia, which work together to trap and remove dust, bacteria, and other particles from inhaled air.
This built-in defense system helps protect the lungs from infection and irritation. By maintaining a clear and stable airway, the trachea plays an essential role in effective breathing and overall respiratory health.
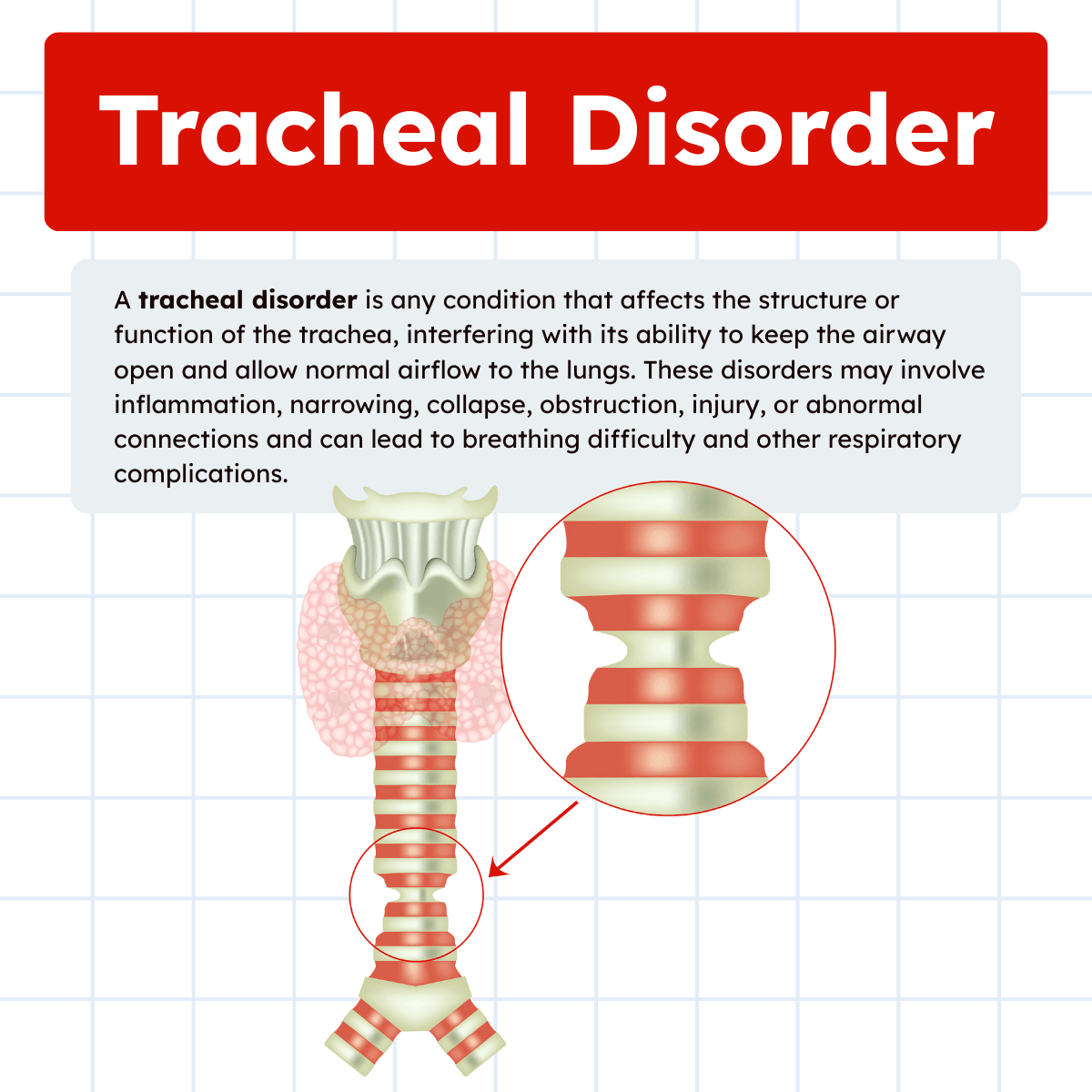
What Is a Tracheal Disorder?
A tracheal disorder is any condition that interferes with the normal structure or function of the trachea. These disorders may involve:
- Inflammation or infection
- Structural narrowing or collapse
- Abnormal connections to nearby organs
- Tumors or growths
- Foreign object obstruction
- Injury or trauma
- External compression
Because the trachea is responsible for conducting air to and from the lungs, any disruption can impair ventilation and oxygen delivery. Some tracheal disorders are congenital and present early in life, while others develop due to medical procedures, chronic disease, trauma, or environmental exposure.
Note: Early recognition and proper management are critical, as untreated tracheal conditions can lead to respiratory failure, recurrent infections, or long-term airway damage.
Common Types of Tracheal Disorders
Tracheal disorders can vary widely in cause, severity, and clinical presentation, but all have the potential to interfere with normal airflow and breathing.
Watch this video and keep reading to learn more about the most common types and how understanding them supports early recognition, accurate diagnosis, and effective management.
Tracheitis
Tracheitis is an acute inflammation of the trachea, most often caused by a bacterial infection. It commonly develops after a viral upper respiratory infection, which weakens the airway’s defenses and allows bacteria to invade. The most frequently implicated pathogen is Staphylococcus aureus.
This condition is especially dangerous in children but can also affect adults, particularly those with compromised immune systems.
Symptoms often develop rapidly and may include:
- High fever
- Severe cough, often described as barking
- Hoarseness
- Difficulty breathing
- Stridor, a high-pitched sound heard during inspiration
Because tracheitis can cause rapid airway swelling and obstruction, it is considered a medical emergency. Diagnosis is usually based on clinical presentation and imaging, and in some cases, direct visualization of the airway.
Treatment typically includes intravenous antibiotics, close airway monitoring, and supportive care. Severe cases may require oxygen therapy or temporary mechanical ventilation. Prompt treatment is essential to prevent respiratory failure.
Tracheal Stenosis
Tracheal stenosis refers to abnormal narrowing of the trachea, which restricts airflow and increases the work of breathing. This condition may be present at birth or acquired later in life.
Acquired tracheal stenosis most commonly results from prolonged intubation or tracheostomy. Pressure from airway devices can damage the tracheal lining, leading to inflammation, scarring, and eventual narrowing. Other causes include trauma, autoimmune disease, infection, or prior surgery involving the airway.
Symptoms depend on the severity of narrowing and may include:
- Shortness of breath, especially with exertion
- Wheezing that does not respond to bronchodilators
- Chronic cough
- Stridor
Because symptoms often resemble asthma, tracheal stenosis is sometimes misdiagnosed. Diagnosis typically involves CT imaging and bronchoscopy to assess the extent and location of the narrowing.
Treatment ranges from minimally invasive procedures, such as balloon dilation or steroid injections, to surgical options like tracheal resection. In some cases, airway stents are used to maintain patency.
Tracheomalacia
Tracheomalacia is characterized by weakness and excessive collapsibility of the tracheal walls. Instead of remaining open during breathing, the airway narrows or collapses, particularly during exhalation.
This condition may be congenital, often associated with other developmental abnormalities, or acquired later in life due to prolonged intubation, chronic inflammation, infection, or external compression.
Symptoms may include:
- Noisy breathing
- Chronic cough
- Difficulty clearing secretions
- Recurrent respiratory infections
- Breathing distress in severe cases
Diagnosis is typically made using bronchoscopy, which allows direct observation of airway collapse during breathing. Management depends on severity. Mild cases may be monitored and managed conservatively, while more severe cases may require surgical interventions such as airway stenting or procedures that stabilize the trachea.
Tracheoesophageal Fistula
A tracheoesophageal fistula is an abnormal connection between the trachea and the esophagus. This condition is most commonly congenital and frequently occurs alongside esophageal atresia, where the esophagus does not fully develop.
Acquired fistulas may result from trauma, malignancy, prolonged intubation, or surgical complications.
Symptoms differ by age:
- In infants: coughing, choking, cyanosis during feeding
- In adults: recurrent pneumonia, chronic cough, difficulty swallowing
Because food and saliva can enter the airway, this condition significantly increases the risk of aspiration and infection. Diagnosis involves imaging studies and endoscopic evaluation. Treatment almost always requires surgical repair to separate the trachea and esophagus and restore normal anatomy.
Tracheal Tumors
Tumors of the trachea are rare but potentially serious. They may be benign or malignant, with malignant tumors posing a higher risk due to aggressive growth and invasion of surrounding tissues.
Benign tumors often grow slowly and may remain asymptomatic for long periods. Malignant tumors tend to cause progressive airway obstruction and systemic symptoms.
Common symptoms include:
- Shortness of breath
- Persistent wheezing
- Cough, sometimes with blood
- Recurrent respiratory infections
Because symptoms often mimic asthma or chronic bronchitis, diagnosis may be delayed. CT imaging and bronchoscopy with biopsy are key diagnostic tools. Treatment depends on tumor type and stage and may include surgical removal, radiation therapy, chemotherapy, or palliative airway management.
Foreign Bodies in the Trachea
Foreign body aspiration is a medical emergency, particularly common in young children. Small objects, food particles, or toys can become lodged in the trachea, causing partial or complete airway obstruction.
Symptoms often include:
- Sudden coughing or choking
- Wheezing
- Inability to speak or breathe
- Cyanosis
Immediate intervention is critical. Emergency techniques such as abdominal thrusts may be lifesaving. In clinical settings, bronchoscopy is used to locate and remove the object. Prevention relies heavily on supervision and age-appropriate safety measures.
Tracheal Trauma
Tracheal trauma can result from blunt or penetrating injuries to the neck or chest, often due to accidents, sports injuries, or violence. Because the trachea is relatively exposed, damage can quickly compromise the airway.
Symptoms may include:
- Breathing difficulty
- Hoarseness
- Neck swelling
- Subcutaneous emphysema
- Coughing up blood
Tracheal trauma requires immediate medical attention. Management focuses on securing the airway and surgically repairing the injury when necessary. Outcomes depend heavily on the speed of diagnosis and treatment.
Tracheal Compression
Tracheal compression occurs when external structures press on the airway, narrowing its diameter. Common causes include enlarged thyroid glands, tumors, lymphadenopathy, vascular abnormalities, or mediastinal masses.
Symptoms may include:
- Progressive shortness of breath
- Stridor
- Chronic cough
- Recurrent infections
Note: Diagnosis relies on imaging studies such as CT or MRI. Treatment focuses on addressing the underlying cause, which may involve medication, surgery, or airway stenting.
Gastroesophageal Reflux Disease (GERD)
Although gastroesophageal reflux disease primarily affects the digestive system, it can also have a significant impact on the trachea. When stomach acid flows upward, it can irritate the airway and trigger inflammation, leading to symptoms such as chronic cough, hoarseness, throat irritation, and increased airway sensitivity.
A related condition, known as laryngopharyngeal reflux, allows acid to reach the upper airway and trachea more directly, often without typical heartburn symptoms. Diagnosis may involve a detailed history, laryngoscopy, or pH monitoring. Management usually includes lifestyle modifications and acid-reducing medications, with surgical options reserved for severe or persistent cases.
Why Tracheal Disorders Matter in Respiratory Care
Airway Management
Tracheal disorders directly affect intubation, extubation, and tracheostomy care. Narrowed or unstable airways increase the risk of difficult intubation, accidental extubation, and post-extubation stridor.
Respiratory therapists must anticipate these challenges and collaborate closely with the healthcare team during airway interventions.
Mechanical Ventilation
Patients with tracheal pathology often require special ventilator considerations. Increased airway resistance, dynamic collapse, or fixed obstruction can alter peak pressures, flow patterns, and patient-ventilator synchrony.
Understanding the underlying tracheal condition helps therapists:
- Interpret abnormal ventilator waveforms
- Adjust pressure support and PEEP appropriately
- Recognize when ventilator alarms reflect airway pathology rather than lung disease
Secretion Clearance
Effective mucociliary clearance depends on a healthy tracheal lining. Many tracheal disorders impair this process, leading to secretion retention and infection.
Respiratory therapists play a key role in:
- Airway suctioning
- Humidification management
- Chest physiotherapy and airway clearance techniques
Emergency Recognition
Tracheal disorders can deteriorate rapidly. Acute airway obstruction is a true respiratory emergency.
Respiratory therapists are often the first clinicians to recognize:
- New-onset stridor
- Sudden increases in work of breathing
- Changes in airflow sounds
- Rising airway pressures
Note: Prompt recognition and escalation of care can be life-saving.
Diagnostic Approaches
Evaluation of tracheal disorders may include:
- Imaging studies such as CT scans
- Bronchoscopy for direct visualization
- Flow-volume loops showing fixed or variable obstruction
- Clinical response to positive pressure ventilation
Note: Respiratory therapists frequently assist with bronchoscopy and provide valuable bedside observations that support diagnosis.
Treatment and Management Strategies
Management depends on the specific disorder and its severity, but may include:
- Airway stenting
- Surgical intervention
- Antibiotic therapy
- Corticosteroids for inflammation
- Noninvasive or invasive ventilation
Note: Supportive respiratory care remains a cornerstone of treatment in nearly all cases.
Tracheal Disorder Practice Questions
1. What is the primary function of the trachea?
The trachea serves as the main airway that conducts air between the upper airway and the lungs.
2. Where does the trachea begin and end anatomically?
It begins just below the larynx and ends where it bifurcates into the right and left main bronchi.
3. Why are C-shaped cartilage rings important to tracheal function?
They maintain airway patency while allowing flexibility during breathing and swallowing.
4. Which structures line the inside of the trachea to help protect the lungs?
Mucus-producing cells and cilia that trap and remove inhaled particles.
5. What role do cilia play in normal tracheal defense?
They move mucus and trapped debris upward toward the upper airway for clearance.
6. What is a tracheal disorder?
Any condition that disrupts the normal structure or function of the trachea.
7. Why can tracheal disorders significantly impair ventilation?
Because obstruction or collapse of the trachea restricts airflow to the lungs.
8. Which tracheal disorders may present suddenly and require urgent intervention?
Conditions caused by trauma, foreign body obstruction, or acute inflammation.
9. How can chronic tracheal disorders mimic common respiratory diseases?
They may cause cough, wheezing, or dyspnea similar to asthma or bronchitis.
10. What types of structural changes can occur in tracheal disorders?
Narrowing, collapse, abnormal connections, or external compression.
11. How can medical procedures contribute to tracheal disorders?
Prolonged intubation or tracheostomy can cause injury, stenosis, or scarring.
12. Why are some tracheal disorders present at birth?
They may be congenital due to abnormal airway development.
13. What is the clinical significance of external compression of the trachea?
It can reduce airway diameter and compromise airflow during breathing.
14. Why is early recognition of tracheal disorders critical?
Delayed treatment can lead to respiratory failure, infection, or permanent airway damage.
15. How does tracheal inflammation affect airflow?
Swelling and increased secretions can narrow the airway and increase resistance.
16. What symptoms commonly suggest a tracheal disorder?
Stridor, cough, dyspnea, wheezing, or recurrent respiratory infections.
17. Why are tumors involving the trachea particularly dangerous?
Even small growths can significantly obstruct airflow.
18. How does tracheal injury impact oxygen delivery?
Restricted airflow limits ventilation, reducing oxygen delivery to the lungs.
19. Why must respiratory therapists remain vigilant for tracheal disorders?
Early airway compromise may be subtle but rapidly life-threatening.
20. What is the overall goal of managing tracheal disorders?
To maintain airway patency, ensure adequate ventilation, and prevent long-term damage.
21. What is tracheitis?
Tracheitis is an acute inflammation of the trachea, most commonly caused by a bacterial infection following a viral upper respiratory illness.
22. Which pathogen is most frequently associated with bacterial tracheitis?
Staphylococcus aureus
23. Why is tracheitis considered a medical emergency?
Because rapid airway swelling can lead to severe obstruction and respiratory failure.
24. What breath sound is commonly associated with tracheitis?
Inspiratory stridor caused by upper airway narrowing.
25. What population is at greatest risk for severe tracheitis?
Children, although immunocompromised adults are also at increased risk.
26. What is tracheal stenosis?
Tracheal stenosis is an abnormal narrowing of the trachea that restricts airflow and increases the work of breathing.
27. What is the most common cause of acquired tracheal stenosis?
Prolonged endotracheal intubation or tracheostomy.
28. Why is tracheal stenosis often misdiagnosed as asthma?
Because symptoms such as wheezing and dyspnea may not respond to bronchodilators.
29. Which diagnostic tests are commonly used to confirm tracheal stenosis?
CT imaging and bronchoscopy.
30. What is tracheomalacia?
Tracheomalacia is a condition characterized by weakness and excessive collapsibility of the tracheal walls.
31. During which phase of breathing does airway collapse most often occur in tracheomalacia?
During exhalation
32. What diagnostic procedure allows direct visualization of airway collapse in tracheomalacia?
Bronchoscopy
33. What is a tracheoesophageal fistula?
An abnormal connection between the trachea and the esophagus that allows aspiration of food or secretions.
34. What symptom is commonly seen in infants with a tracheoesophageal fistula?
Coughing or cyanosis during feeding.
35. Why does a tracheoesophageal fistula increase the risk of pneumonia?
Because food and saliva can enter the airway and lungs.
36. What are tracheal tumors?
Abnormal growths within the trachea that may be benign or malignant and can obstruct airflow.
37. Why are tracheal tumors often diagnosed late?
Because symptoms frequently mimic asthma or chronic bronchitis.
38. What diagnostic tools are essential for identifying tracheal tumors?
CT imaging and bronchoscopy with biopsy.
39. What is the most common cause of foreign body obstruction in the trachea?
Aspiration of food or small objects, particularly in young children.
40. What is the immediate priority in suspected tracheal foreign body aspiration?
Rapid airway clearance and restoration of ventilation.
41. What clinical finding suggests tracheal trauma?
Subcutaneous emphysema with respiratory distress.
42. Why is tracheal trauma considered life-threatening?
Because airway compromise can occur rapidly if the trachea is disrupted.
43. What is tracheal compression?
Narrowing of the trachea caused by pressure from external structures.
44. Which conditions commonly cause tracheal compression?
Enlarged thyroid, mediastinal tumors, lymphadenopathy, or vascular abnormalities.
45. How can gastroesophageal reflux disease affect the trachea?
Acid reflux can irritate the airway, causing chronic cough, hoarseness, and tracheal inflammation.
46. What structural feature helps keep the trachea open during normal breathing?
C-shaped rings of cartilage that prevent airway collapse while allowing flexibility.
47. Why are the cartilage rings of the trachea incomplete posteriorly?
To allow the esophagus to expand during swallowing.
48. What role do cilia play in normal tracheal function?
They help move mucus and trapped particles upward toward the pharynx for clearance.
49. How can prolonged coughing worsen certain tracheal disorders?
It increases intrathoracic pressure and can promote airway collapse or inflammation.
50. What clinical sign suggests fixed upper airway obstruction rather than lower airway disease?
Stridor that does not change significantly with bronchodilator therapy.
51. Why may wheezing from tracheal disorders be unresponsive to bronchodilators?
Because the obstruction is structural rather than due to bronchial smooth muscle constriction.
52. What imaging study is most useful for evaluating extrinsic tracheal compression?
Computed tomography (CT) of the neck and chest.
53. What is the primary risk of untreated tracheal stenosis?
Progressive airflow limitation leading to respiratory failure.
54. How does tracheomalacia differ from tracheal stenosis?
Tracheomalacia involves dynamic airway collapse, whereas stenosis is a fixed narrowing.
55. What clinical feature distinguishes tracheomalacia from asthma?
Symptoms often worsen during expiration rather than inspiration.
56. What finding during bronchoscopy confirms tracheomalacia?
Greater than 50% collapse of the tracheal lumen during exhalation.
57. Why are patients with tracheomalacia prone to recurrent infections?
Ineffective airway clearance due to airway collapse and retained secretions.
58. What complication commonly results from an untreated tracheoesophageal fistula?
Chronic aspiration leading to recurrent pneumonia.
59. What symptom in adults may suggest an acquired tracheoesophageal fistula?
Coughing immediately after swallowing liquids.
60. Why is bronchoscopy preferred for removing tracheal foreign bodies?
It allows direct visualization and controlled removal of the obstruction.
61. What population is at highest risk for foreign body aspiration?
Infants and young children.
62. What early sign may indicate tracheal injury after blunt neck trauma?
Hoarseness or voice changes.
63. Why is subcutaneous emphysema concerning in suspected tracheal trauma?
It suggests air leakage from the airway into surrounding tissues.
64. What is the primary goal when managing acute tracheal trauma?
Securing and protecting the airway.
65. How can large thyroid goiters affect the trachea?
They can compress the trachea externally, narrowing the airway.
66. Why may symptoms of tracheal compression worsen when lying flat?
Gravity and positional changes can increase external pressure on the airway.
67. What condition allows gastric acid to directly irritate the trachea without heartburn?
Laryngopharyngeal reflux
68. How can chronic reflux contribute to tracheal inflammation?
Repeated acid exposure causes mucosal irritation and edema.
69. What symptom suggests nighttime reflux-related tracheal irritation?
Chronic cough that worsens when lying down.
70. Why is early identification of tracheal disorders critical?
Delayed recognition can result in sudden airway compromise and respiratory failure.
71. What portion of the airway does the trachea connect to the lungs?
It bifurcates into the right and left mainstem bronchi.
72. Why is the trachea considered part of the lower airway?
Because it conducts air below the larynx directly into the bronchial tree.
73. What clinical clue suggests tracheal obstruction rather than bronchial disease?
Both inspiratory and expiratory airflow may be equally impaired.
74. How does fixed tracheal obstruction affect the flow-volume loop?
It produces flattening of both the inspiratory and expiratory limbs.
75. What bedside sign may indicate significant tracheal narrowing?
Increased work of breathing with minimal lung auscultation findings.
76. Why can tracheal disorders be mistaken for asthma?
They can cause wheezing, dyspnea, and cough without responding to bronchodilators.
77. What historical clue raises suspicion for post-intubation tracheal stenosis?
A history of prolonged mechanical ventilation or recent extubation.
78. When do symptoms of tracheal stenosis typically become noticeable?
When the tracheal lumen is reduced by approximately 50% or more.
79. Why may exertion worsen symptoms of tracheal stenosis?
Increased airflow demand magnifies the effects of airway narrowing.
80. What diagnostic tool allows direct measurement of tracheal diameter?
Bronchoscopy
81. What is the role of spirometry in suspected tracheal disorders?
It helps identify patterns consistent with upper airway obstruction.
82. Why is stridor considered a high-priority finding?
It indicates critical upper airway narrowing.
83. What breath sound is most commonly associated with tracheal obstruction?
Inspiratory stridor
84. How can chronic tracheal irritation affect voice quality?
It can cause persistent hoarseness.
85. Why are tracheal tumors often diagnosed late?
Symptoms are nonspecific and progress slowly, mimicking common airway diseases.
86. What symptom may suggest malignant tracheal involvement?
Hemoptysis with progressive dyspnea.
87. How does airway stenting help manage certain tracheal disorders?
It mechanically maintains airway patency.
88. What risk is associated with long-term tracheal stent placement?
Mucus plugging or granulation tissue formation.
89. Why is humidification important in patients with tracheal disorders?
Dry air can worsen irritation and impair secretion clearance.
90. What role does coughing play in tracheal defense?
It helps clear secretions and foreign material from the airway.
91. How can ineffective cough worsen tracheal disease?
Secretions accumulate and increase infection risk.
92. Why are patients with neuromuscular disease at risk for tracheal complications?
Weak airway muscles impair airway protection and clearance.
93. What is the primary concern with tracheal edema?
Rapid airway narrowing leading to obstruction.
94. Why may corticosteroids be used in some tracheal disorders?
To reduce inflammation and airway swelling.
95. What occupational exposure can contribute to chronic tracheal irritation?
Inhalation of chemical fumes or industrial dust.
96. Why is airway assessment crucial after neck surgery?
Postoperative swelling can compress the trachea.
97. What finding suggests dynamic airway collapse rather than fixed obstruction?
Symptoms that worsen during expiration.
98. How does obesity potentially worsen tracheal disorders?
Increased soft tissue can contribute to external airway compression.
99. Why is patient positioning important in tracheal disorders?
Upright positioning can improve airway patency and breathing comfort.
100. What is the respiratory therapist’s key role in managing tracheal disorders?
Early recognition, airway assessment, and support of ventilation and oxygenation.
Final Thoughts
The trachea is a vital yet vulnerable component of the respiratory system. Disorders affecting this airway can range from mild and manageable to severe and life-threatening. Because symptoms often mimic more common respiratory conditions, tracheal disorders are frequently underrecognized or misdiagnosed.
A strong understanding of tracheal anatomy, function, and pathology allows for earlier recognition, more accurate diagnosis, and better treatment outcomes. Whether caused by infection, structural abnormalities, trauma, or chronic disease, tracheal disorders demand careful attention due to their direct impact on breathing and quality of life.
Maintaining airway health, seeking prompt evaluation for persistent respiratory symptoms, and understanding risk factors are essential steps in protecting one of the body’s most critical lifelines.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Mieczkowski B, Seavey BF. Anatomy, Head and Neck, Trachea. [Updated 2023 Aug 7]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025.
- Al-Qadi MO, Artenstein AW, Braman SS. The “forgotten zone”: acquired disorders of the trachea in adults. Respir Med. 2013.

