Laryngopharyngeal reflux (LPR) is a condition in which stomach contents flow backward beyond the esophagus and into the throat and larynx, leading to irritation and inflammation of the upper airway.
Often referred to as “silent reflux,” LPR may occur without the classic symptoms of heartburn that are commonly associated with gastroesophageal reflux disease (GERD). Instead, patients frequently report chronic throat clearing, hoarseness, a persistent cough, or the sensation of a lump in the throat.
Because these symptoms overlap with many respiratory and ear, nose, and throat disorders, LPR is sometimes overlooked or misdiagnosed. Understanding its causes, presentation, and clinical implications is essential for accurate diagnosis and effective management.
Download our free guide that has over 100+ of the best tips for healthy lungs.
What is Laryngopharyngeal Reflux?
Laryngopharyngeal reflux (LPR) is a condition in which stomach contents, including acid and digestive enzymes such as pepsin, flow backward past the esophagus and into the larynx and pharynx. Unlike gastroesophageal reflux disease, LPR does not always cause heartburn, which is why it is often referred to as “silent reflux.” Instead, it commonly presents with throat-related and respiratory symptoms.
Patients with LPR may experience chronic throat clearing, hoarseness, a persistent dry cough, excess mucus, difficulty swallowing, or the sensation of a lump in the throat, known as globus sensation. The tissues of the larynx are more sensitive than the esophagus, so even small amounts of reflux can lead to significant irritation and inflammation.
Because its symptoms overlap with allergies, asthma, and other upper airway conditions, LPR can be challenging to diagnose. Early identification and appropriate treatment are important to prevent ongoing inflammation and voice or airway complications.
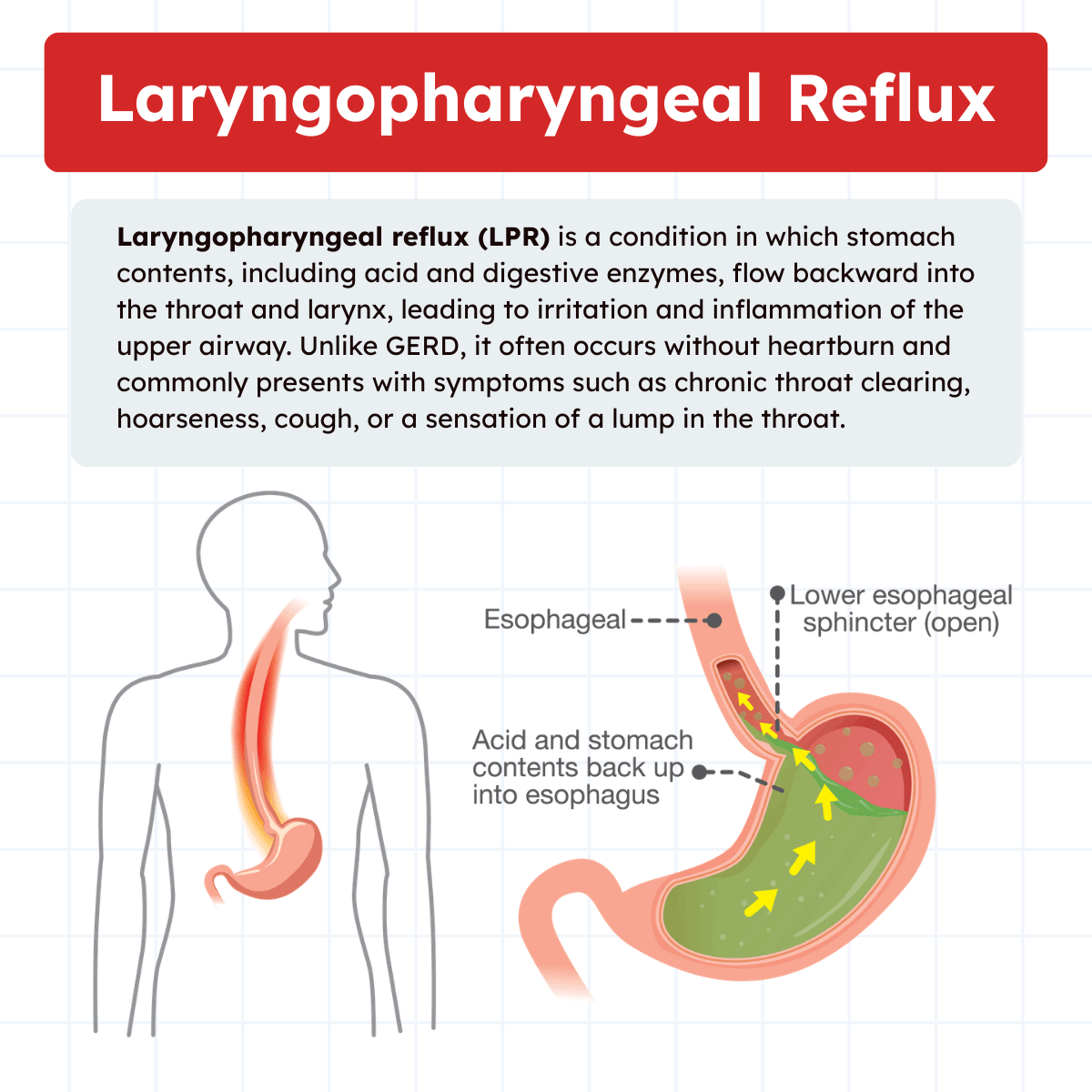
Laryngopharyngeal Reflux vs. Gastroesophageal Reflux
LPR and GERD both involve reflux, but they differ in symptom patterns and tissue involvement. GERD primarily affects your esophagus and usually causes heartburn and regurgitation.
In LPR, you often do not experience classic heartburn. Instead, you develop throat and voice symptoms. This difference can delay diagnosis because you may not associate your symptoms with reflux.
GERD typically worsens when you lie flat at night. LPR can occur during the day in upright positions, often after meals or voice use. The reflux in LPR may be less acidic but still damaging to delicate throat tissues.
Note: While GERD focuses on esophageal injury, such as erosions, LPR commonly leads to vocal cord inflammation, redness, and thickened tissue seen on laryngoscopy.
Prevalence
LPR affects a significant portion of adults, though exact numbers vary due to underdiagnosis. Studies estimate that up to 10% of patients seen by ear, nose, and throat specialists show signs consistent with LPR.
Many people with chronic hoarseness or persistent cough have underlying reflux as a contributing factor. Because symptoms overlap with allergies, asthma, and postnasal drip, clinicians may initially treat other conditions.
You face higher risk if you have obesity, frequent alcohol use, high caffeine intake, or a diet high in acidic and fatty foods. Smoking also increases your risk by weakening protective reflexes and irritating throat tissue.
Note: Early recognition matters because ongoing exposure can lead to chronic voice problems and airway irritation.
Causes and Risk Factors
Laryngopharyngeal reflux (LPR) develops when stomach contents move upward into your throat and voice box instead of staying in your stomach. Several physiological, lifestyle, and medical factors can weaken natural barriers and increase this backflow.
Physiological Triggers
Your body relies on the lower esophageal sphincter (LES) and the upper esophageal sphincter (UES) to keep stomach contents from traveling upward. When these muscles weaken or relax inappropriately, acid and digestive enzymes can reach your throat.
Even small amounts of reflux can irritate throat tissue. Unlike the esophagus, your larynx lacks strong protective lining against acid and pepsin. Delayed stomach emptying also raises pressure inside your stomach. This pressure increases the likelihood that contents will move upward, especially after meals.
Body position plays a role. Lying flat, bending over, or speaking for long periods after eating can allow reflux to reach higher into your airway. Some people produce more acid or have heightened tissue sensitivity. In these cases, even normal reflux levels may cause noticeable symptoms.
Lifestyle Influences
Your daily habits strongly affect reflux frequency. Large meals stretch your stomach and increase internal pressure, which promotes upward flow.
Certain foods and beverages can relax the LES. Common triggers include:
- Caffeine
- Alcohol
- Chocolate
- Fried or high-fat foods
- Carbonated drinks
- Spicy foods
Smoking weakens sphincter function and reduces saliva production. Saliva helps neutralize acid, so reduced levels increase irritation. Eating late at night raises risk because gravity no longer helps keep stomach contents down. Lying down within two to three hours of eating often worsens symptoms.
Note: Excess body weight, particularly around your abdomen, increases pressure on your stomach. This pressure can push contents upward more easily.
Medical Conditions Associated With LPR
Several medical conditions increase your risk of developing LPR. Gastroesophageal reflux disease (GERD) is the most common underlying cause. Hiatal hernia can impair normal sphincter function. When part of your stomach moves above the diaphragm, reflux becomes more likely.
Conditions that delay stomach emptying, such as gastroparesis, allow food and acid to remain in your stomach longer. This increases the chance of backflow. Chronic cough, asthma, and obstructive sleep apnea may also contribute. Repeated pressure changes in your chest and abdomen can force reflux upward.
Certain medications relax the LES or irritate the esophagus. These include some blood pressure drugs, sedatives, and anticholinergic medications.
Note: If you experience persistent throat symptoms, identifying and addressing these contributing factors can reduce irritation and improve control.
Symptoms and Clinical Presentation
Laryngopharyngeal reflux often affects your throat, voice, and airways rather than causing classic heartburn. You may notice persistent irritation, voice changes, or breathing-related symptoms that fluctuate throughout the day.
Throat and Voice Symptoms
You may feel a constant need to clear your throat, even when little mucus is present. This repeated throat clearing can irritate the vocal cords and worsen inflammation. Hoarseness is common, especially in the morning or after prolonged speaking. Your voice may sound rough, weak, or strained, and you may lose vocal endurance more quickly than usual.
Many people describe a lump-in-the-throat sensation (globus). You might feel something stuck in your throat despite normal swallowing. Mild sore throat, burning, or dryness can occur without visible infection. Unlike typical acid reflux, you often do not experience significant heartburn.
Respiratory and Ear Symptoms
Reflux reaching the upper airway can trigger a chronic dry cough. The cough often worsens when you lie down, speak for long periods, or after meals. You may notice frequent throat irritation that leads to coughing fits. Some people develop intermittent wheezing or experience worsening asthma symptoms.
Postnasal drip is commonly reported, although excess mucus may not always be present. Instead, irritation from stomach contents can mimic sinus or allergy problems. Ear discomfort or a sensation of fullness can also occur. In some cases, reflux-related inflammation affects the Eustachian tubes, contributing to pressure changes or mild ear pain.
Atypical Manifestations
Some people develop difficulty swallowing, known as dysphagia. You may feel that food moves slowly or that pills are harder to swallow. Chest discomfort can occur, but it often differs from classic heartburn. The discomfort may be mild, intermittent, and localized higher in the chest or throat.
You might experience increased symptoms without clear dietary triggers. Stress, voice overuse, bending forward, or lying flat can provoke irritation.
In certain cases, symptoms overlap with conditions such as chronic sinusitis, asthma, or vocal cord dysfunction. This overlap can delay recognition because routine tests may appear normal while irritation persists.
Diagnosis of Laryngopharyngeal Reflux
You diagnose laryngopharyngeal reflux (LPR) by combining symptom patterns, laryngeal findings, and selective testing. No single test confirms the condition in every case, so you rely on clinical judgment supported by targeted investigations.
Clinical Evaluation
You begin with a focused history. Patients often report chronic throat clearing, persistent cough, hoarseness, globus sensation, excess mucus, or throat irritation, frequently without classic heartburn.
Symptoms typically worsen after meals, when lying down, or after voice overuse. Many patients describe symptoms that persist for months and do not respond fully to allergy or asthma treatment.
You should perform flexible laryngoscopy to inspect the larynx and pharynx. Common findings include posterior laryngeal erythema, edema, ventricular obliteration, thick endolaryngeal mucus, and interarytenoid hypertrophy. These findings are suggestive but not specific, as inflammation can result from other causes.
Note: Symptom scoring tools such as the Reflux Symptom Index (RSI) can help quantify severity and track response to treatment. You should use them as supportive tools rather than diagnostic proof.
Diagnostic Tests
You reserve objective testing for unclear cases, treatment failures, or when considering long-term therapy. The most useful test is 24-hour ambulatory pH monitoring, ideally with dual probes or impedance-pH monitoring.
Impedance testing detects both acid and non-acid reflux and measures how high refluxate travels in the esophagus. This information helps confirm whether reflux reaches the proximal esophagus or pharynx.
Traditional esophagogastroduodenoscopy (EGD) may appear normal in many patients with LPR. You use EGD primarily to evaluate complications such as esophagitis, strictures, or Barrett’s esophagus rather than to confirm LPR itself.
Empiric therapy with proton pump inhibitors is sometimes used as a diagnostic trial. However, symptom improvement alone does not definitively confirm LPR, since response rates vary and placebo effects occur.
Differential Diagnosis
You must rule out other causes of chronic throat and voice symptoms. Common alternatives include allergic rhinitis, chronic sinusitis, postnasal drip, asthma, chronic bronchitis, and vocal cord dysfunction.
Functional voice disorders and muscle tension dysphonia can mimic LPR, especially in professional voice users. You should also consider smoking-related irritation and environmental exposures.
In persistent or atypical cases, exclude serious conditions such as laryngeal malignancy, particularly in patients with risk factors like tobacco or heavy alcohol use. Careful visualization and biopsy of suspicious lesions are essential.
Note: Accurate diagnosis requires correlating symptoms, laryngoscopic findings, and, when needed, objective testing rather than relying on any single feature.
Complications of Untreated LPR
When you do not treat laryngopharyngeal reflux (LPR), repeated exposure to stomach acid and digestive enzymes can damage delicate throat and airway tissues. This damage may progress from persistent irritation to structural and breathing problems that interfere with daily function.
Chronic Laryngeal Inflammation
Ongoing reflux can keep your larynx in a constant state of irritation. Acid and pepsin repeatedly contact the vocal cords, leading to swelling, redness, and thickening of the tissue.
You may notice persistent hoarseness, frequent throat clearing, chronic cough, or a sensation of a lump in your throat. These symptoms often fluctuate but rarely resolve without treatment. Over time, inflammation can alter how your vocal cords vibrate.
Chronic irritation may lead to vocal cord nodules, granulomas, or contact ulcers. These growths can cause pain when speaking and further voice changes. In severe cases, scarring may develop, which can permanently affect your voice quality.
Note: Persistent inflammation also increases tissue sensitivity. Even small amounts of reflux can trigger exaggerated symptoms once this cycle becomes established.
Airway Complications
Untreated LPR can affect more than your voice. Acid exposure may extend into the lower throat and airway, irritating the upper respiratory tract. You may develop chronic cough, throat tightness, or episodes of laryngospasm, where the vocal cords briefly close and make breathing difficult. These episodes can feel sudden and alarming, especially at night.
In some people, reflux worsens asthma symptoms or contributes to reactive airway disease. Acid particles that reach the airway can trigger bronchial irritation, leading to wheezing or shortness of breath.
Repeated airway exposure may also increase your risk of recurrent respiratory infections. Swollen tissues and excess mucus create an environment where bacteria and viruses can persist more easily, prolonging recovery and increasing symptom frequency.
Treatment Options for Laryngopharyngeal Reflux
You can manage laryngopharyngeal reflux (LPR) with targeted lifestyle changes, medications that reduce acid exposure, and in select cases, surgery. Treatment focuses on reducing irritation in your throat and preventing stomach contents from reaching the larynx.
Lifestyle and Dietary Changes
Lifestyle changes form the foundation of treatment. You need to reduce behaviors that increase pressure on your stomach or relax the lower esophageal sphincter.
Avoid trigger foods such as caffeine, alcohol, chocolate, peppermint, fried foods, tomato products, and citrus. These items can worsen reflux episodes. Eat smaller meals and stop eating at least 3 hours before lying down.
Elevate the head of your bed by 6–8 inches using blocks or a wedge pillow. Extra pillows alone do not work because they bend your neck rather than lift your torso. Maintain a healthy weight. Excess abdominal weight increases pressure on your stomach and promotes reflux. If you smoke, stop. Smoking weakens the sphincter and delays throat healing.
Note: You should also limit throat clearing. Frequent clearing irritates already inflamed tissue and prolongs symptoms.
Medications
Doctors often prescribe proton pump inhibitors (PPIs) as first-line therapy. These medications reduce stomach acid production and allow throat tissue to heal. You typically take them once or twice daily, 30–60 minutes before meals.
Treatment usually lasts at least 8–12 weeks, and some cases require longer courses. Improvement may take several weeks because throat tissue heals slowly.
H2 receptor blockers may help in milder cases or as nighttime add-on therapy. Examples include famotidine. Some clinicians recommend alginate-based therapies. These form a barrier that floats on stomach contents and may reduce reflux into the throat, especially after meals.
Note: Medication works best when you combine it with lifestyle changes. Taking medication alone without diet adjustments often limits results.
Surgical Interventions
Surgery becomes an option if you continue to have significant symptoms despite medical therapy or if testing confirms severe reflux. Your doctor may order pH monitoring or esophageal manometry before recommending surgery. The most common procedure is fundoplication. During this surgery, the upper part of your stomach wraps around the lower esophagus to strengthen the sphincter and reduce reflux.
Less invasive options, such as magnetic sphincter augmentation, may suit selected patients. These procedures aim to restore the barrier between your stomach and esophagus.
Note: Surgery carries risks, including difficulty swallowing, gas bloating, and the need for revision. You and your surgeon should weigh potential benefits against these risks based on objective testing and symptom severity.
Long-Term Management and Prognosis
You manage laryngopharyngeal reflux (LPR) with consistent habits and regular follow-up. Symptoms often improve within several months, but full healing of throat tissues can take longer. Patience and adherence to treatment matter.
Long-term care often includes:
- Dietary adjustments, such as limiting acidic, spicy, and fatty foods
- Weight management if you are overweight
- Elevating the head of your bed
- Avoiding meals within three hours of sleep
Medication may remain part of your plan. You may use proton pump inhibitors, H2 blockers, or alginate therapy for extended periods under medical supervision. Your clinician may adjust doses based on symptom control and side effects.
Some people require treatment for six months or longer. Others transition to on-demand therapy once symptoms stabilize. Regular reassessment helps prevent unnecessary long-term medication use.
If you continue to experience symptoms despite treatment, your clinician may recommend further evaluation. This can include laryngoscopy, pH monitoring, or referral to a specialist. Identifying contributing factors such as allergies, smoking, or vocal strain improves long-term control.
With consistent management, you can reduce throat irritation, protect your voice, and limit recurrence. Early attention to returning symptoms helps prevent complications such as chronic cough, vocal cord changes, or persistent throat discomfort.
Pediatric Considerations
Laryngopharyngeal reflux (LPR) can affect infants, children, and adolescents. In children, symptoms often differ from adults, so you need to look beyond typical heartburn.
Infants may show feeding difficulties, frequent spit-up, chronic cough, or noisy breathing. You might also notice irritability during or after feeds. Poor weight gain can occur in more persistent cases.
In toddlers and school-aged children, LPR may present as:
- Chronic throat clearing
- Hoarseness
- Persistent cough
- Recurrent croup
- Trouble swallowing
Older children may describe a lump-in-the-throat sensation or throat discomfort. Many do not report classic reflux symptoms. Diagnosis often relies on clinical history and physical exam. A pediatric specialist may use flexible laryngoscopy to evaluate throat inflammation. In select cases, pH monitoring or impedance testing helps confirm reflux.
Management focuses on practical steps. You may need to adjust feeding volumes, feeding position, or meal timing. For older children, reducing acidic and processed foods can support symptom control.
Medication decisions require caution. Your child’s clinician will weigh potential benefits and risks before recommending acid-suppressing therapy. Close follow-up ensures symptoms improve without unnecessary long-term treatment.
Prevention Strategies
You can reduce laryngopharyngeal reflux by changing daily habits that trigger acid exposure in your throat. Small, consistent adjustments often lower irritation and protect your vocal tissues.
Start with meal timing and portion control.
- Eat smaller meals.
- Avoid eating within 2–3 hours of lying down.
- Limit late-night snacks.
Choose foods that are less likely to relax the lower esophageal sphincter. Reduce intake of caffeine, alcohol, chocolate, fatty foods, spicy foods, and acidic items such as citrus and tomato products. Track your symptoms to identify personal triggers.
Maintain a healthy body weight. Excess abdominal pressure can push stomach contents upward, increasing reflux episodes. Elevate the head of your bed by 6–8 inches if you experience nighttime symptoms. Use bed risers or a wedge pillow rather than stacking standard pillows, which can bend your neck and increase pressure.
Avoid tight clothing around your waist. Tight belts and waistbands increase abdominal pressure and promote reflux. If you smoke, stop. Tobacco weakens the protective mechanisms that limit acid exposure and irritates throat tissue.
Stay hydrated throughout the day. Adequate fluid intake helps keep throat tissues moist and may reduce irritation from minor reflux events.
Note: Follow prescribed medications exactly as directed if your clinician recommends them. Consistent use improves symptom control and helps prevent flare-ups.
FAQs About Laryngopharyngeal Reflux
Is Laryngopharyngeal Reflux a Lifelong Condition?
Laryngopharyngeal reflux (LPR) is not always a lifelong condition. For many people, symptoms improve significantly with lifestyle changes, dietary adjustments, and appropriate medical treatment.
However, some individuals may experience recurring symptoms, especially if underlying risk factors such as obesity, chronic stress, or anatomical issues persist. Long-term management may be necessary in certain cases.
Note: Early diagnosis and consistent treatment can reduce inflammation and prevent complications, allowing many patients to achieve good symptom control over time.
Is Laryngopharyngeal Reflux Common?
Laryngopharyngeal reflux is relatively common and affects a significant portion of the population. It is often underdiagnosed because its symptoms differ from classic heartburn associated with gastroesophageal reflux disease.
Many people experience throat clearing, hoarseness, or chronic cough without realizing reflux may be the cause. LPR can affect both adults and children. Increased awareness among healthcare providers has improved recognition, but many mild cases likely go unreported or are mistaken for allergies or respiratory conditions.
How Do You Get Rid of Laryngopharyngeal Reflux?
Managing LPR typically involves a combination of lifestyle modifications and medication. Common recommendations include avoiding trigger foods, eating smaller meals, not lying down soon after eating, losing excess weight, and elevating the head of the bed. Reducing caffeine, alcohol, spicy foods, and acidic beverages can also help.
In many cases, doctors prescribe acid-suppressing medications to promote healing. Consistency is important, as symptom improvement may take several weeks. Long-term success often depends on maintaining healthy habits even after symptoms improve.
What Medicine Is Best for Laryngopharyngeal Reflux?
The most commonly prescribed medications for LPR are proton pump inhibitors (PPIs), which reduce stomach acid production. H2 receptor blockers may also be used in some cases. PPIs are often taken once or twice daily for several weeks or months, depending on symptom severity.
While these medications can reduce irritation and promote healing, they are typically most effective when combined with lifestyle changes. The best treatment plan varies by individual, so consultation with a healthcare provider is essential for proper management.
Can Laryngopharyngeal Reflux Be Cured Permanently?
In some individuals, LPR symptoms can resolve completely with proper treatment and lifestyle adjustments. However, others may experience recurring symptoms if underlying risk factors are not addressed. While there is no guaranteed permanent cure for everyone, long-term symptom control is achievable in many cases.
Maintaining dietary modifications, healthy weight, and good eating habits can reduce the likelihood of recurrence. Early and consistent management plays a key role in preventing chronic inflammation and long-term throat or voice complications.
What Are the Triggers for Laryngopharyngeal Reflux?
Common triggers for LPR include acidic foods, spicy meals, caffeine, chocolate, alcohol, carbonated beverages, and high-fat foods. Large meals and eating late at night can also increase the risk of reflux episodes. Smoking and excess body weight further contribute to symptoms.
Stress may worsen reflux by affecting digestion and increasing stomach acid production. Identifying and avoiding personal triggers is an important step in managing symptoms and preventing flare-ups.
What Causes Laryngopharyngeal Reflux to Flare Up?
Flare-ups often occur when dietary or lifestyle habits change. Overeating, lying down after meals, consuming trigger foods, or experiencing high stress can all provoke symptoms. Illness, weight gain, or inconsistent use of prescribed medications may also contribute.
Because the tissues of the throat are sensitive, even small amounts of reflux can cause noticeable irritation. Recognizing patterns and maintaining consistent habits can help minimize flare-ups and improve overall symptom control.
Is Laryngopharyngeal Reflux Worse Than GERD?
LPR and Gastroesophageal Reflux Disease affect different areas of the upper digestive tract, so one is not necessarily worse than the other. GERD primarily affects the esophagus and often causes heartburn, while LPR impacts the throat and voice box.
However, LPR symptoms can be particularly frustrating because they are persistent and may occur without obvious reflux sensations. Both conditions can significantly affect quality of life and require appropriate management.
Does Laryngopharyngeal Reflux Make You Cough?
Yes, LPR can cause a chronic, dry cough. When stomach contents reach the throat and larynx, they irritate sensitive tissues and stimulate the cough reflex. Unlike coughs caused by infections, reflux-related coughs often persist for weeks or months without other typical cold symptoms.
The cough may worsen after meals or when lying down. Proper treatment of reflux often reduces coughing, although improvement may take time as inflammation gradually heals.
Does Laryngopharyngeal Reflux Cause Chest Pain?
LPR primarily affects the throat and voice box rather than the chest. However, some individuals may experience chest discomfort if reflux also involves the esophagus. Chest pain can have many causes, including cardiac conditions, so it should never be ignored.
If chest pain is severe, persistent, or accompanied by shortness of breath, sweating, or dizziness, immediate medical evaluation is necessary. Determining the exact cause ensures appropriate treatment and safety.
Does Laryngopharyngeal Reflux Cause Shortness of Breath?
LPR can contribute to sensations of throat tightness or airway irritation, which some people describe as shortness of breath. Inflammation of the larynx may trigger reflex airway responses, leading to coughing or mild breathing discomfort.
However, true shortness of breath should always be evaluated carefully, as it may signal other respiratory or cardiac conditions. If breathing difficulties are persistent, severe, or worsening, medical evaluation is essential to rule out more serious causes.
When to See a Doctor for Laryngopharyngeal Reflux?
You should see a doctor if symptoms persist for several weeks, worsen despite lifestyle changes, or significantly affect your voice or breathing. Warning signs such as difficulty swallowing, unexplained weight loss, persistent hoarseness, severe chest pain, or coughing up blood require prompt medical attention
Early evaluation can confirm the diagnosis and rule out other conditions. Proper treatment reduces inflammation, protects the airway, and helps prevent long-term complications.
Final Thoughts
Laryngopharyngeal reflux (LPR) is a common yet often misunderstood condition that can significantly affect the throat, voice, and overall airway health. Unlike gastroesophageal reflux disease, it frequently presents without heartburn, which makes careful assessment of symptoms such as chronic cough, hoarseness, and throat irritation especially important.
Early recognition and appropriate management, including lifestyle modifications and targeted medical therapy, can reduce inflammation and prevent long-term complications.
By understanding how reflux impacts the upper airway, healthcare professionals and patients alike can take practical steps to improve symptoms and protect laryngeal function.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Brown J, Shermetaro C. Laryngopharyngeal Reflux. [Updated 2022 Dec 19]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024.


