Mucus plays an essential role in protecting the body, especially within the respiratory system, where it traps dust, allergens, and pathogens before they can cause harm. However, when excess mucus builds up due to allergies, infections, or sinus congestion, it can sometimes affect more than just breathing. Many people wonder whether mucus can also interfere with their hearing.
Because the ears, nose, and throat are closely connected, congestion and mucus accumulation may impact pressure and fluid balance in the middle ear. In this article, we’ll explore whether mucus can cause hearing loss, how it happens, and what you can do about it.
Download our free guide that has over 100+ of the best tips for healthy lungs.
Can Mucus Cause Hearing Loss?
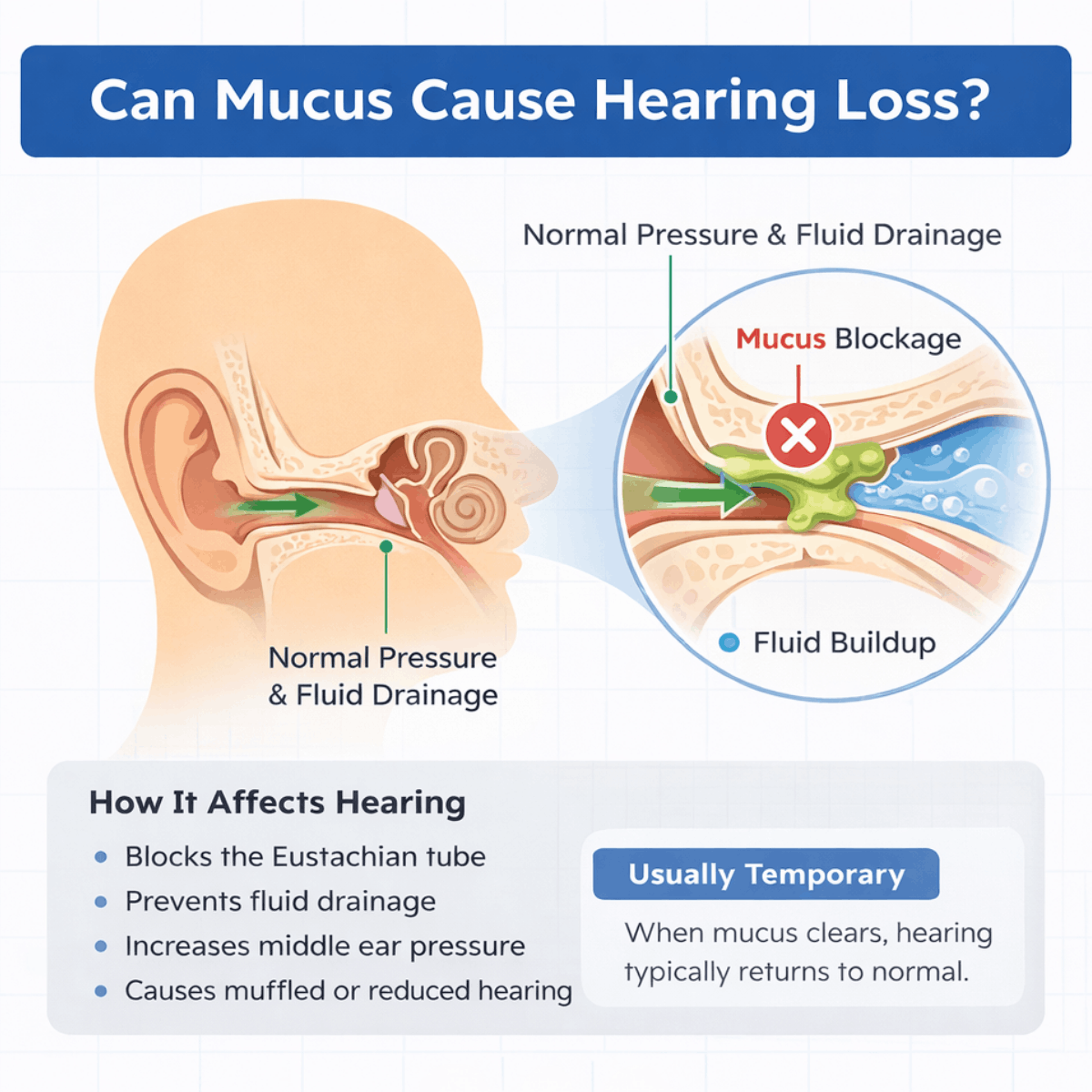
Yes, mucus can contribute to temporary hearing loss in certain situations. The ears, nose, and throat are connected through the Eustachian tubes, which help regulate pressure and drain fluid from the middle ear. When excess mucus develops from a cold, allergies, sinusitis, or an upper respiratory infection, it can block these tubes.
This blockage prevents proper drainage and ventilation, leading to fluid buildup behind the eardrum. As a result, sound vibrations cannot travel as efficiently, causing muffled hearing or a feeling of fullness in the ear.
In most cases, this type of hearing loss is conductive and temporary. Once the mucus clears and normal drainage is restored, hearing typically returns to baseline. However, persistent symptoms should be evaluated by a healthcare professional.
Understanding How Mucus Can Affect Hearing
Mucus can interfere with how sound travels through your ear. When it builds up or becomes trapped, it can block sound movement and disrupt normal ear pressure.
Role of Mucus in the Ear
Your ear naturally produces small amounts of mucus to protect and lubricate tissues. This mucus lines the middle ear and Eustachian tube, which connects your middle ear to the back of your throat.
The Eustachian tube helps equalize pressure and drain fluid. When it works properly, mucus moves out of the middle ear and into your throat, where your body clears it.
Problems begin when inflammation from a cold, allergies, or sinus infection causes swelling. Swelling narrows or blocks the Eustachian tube. Mucus then collects behind the eardrum instead of draining. This trapped fluid changes how your eardrum vibrates. Sound waves cannot move as freely through the middle ear, which reduces how clearly you hear.
In children, the Eustachian tube is shorter and more horizontal. This structure makes mucus buildup more common and increases the risk of fluid-related hearing problems.
Mechanisms of Hearing Loss Caused by Mucus
Mucus usually causes conductive hearing loss. This type of hearing loss happens when sound cannot efficiently travel through the outer or middle ear.
When mucus fills the middle ear, it creates a physical barrier. Sound vibrations weaken before they reach the inner ear, where your hearing nerves process them.
You may notice:
- Muffled or dull sounds
- A feeling of fullness in your ear
- Popping or crackling sensations
- Mild ear pain or pressure
Thick mucus can also limit eardrum movement. If the eardrum cannot vibrate properly, it cannot transmit sound to the tiny middle ear bones. In some cases, negative pressure builds up behind the eardrum. This pressure pulls the eardrum inward, further reducing sound transmission.
Note: The hearing loss from mucus does not usually involve damage to the inner ear. It affects sound conduction rather than nerve function.
Temporary vs. Persistent Hearing Loss Due to Mucus
In most cases, mucus-related hearing loss is temporary. Once swelling decreases and your Eustachian tube opens, fluid drains and hearing returns to normal. This recovery often occurs within a few days to several weeks after a cold or sinus infection. You may notice gradual improvement as pressure and fullness fade.
Persistent hearing loss can develop if fluid remains trapped for months. This condition, called otitis media with effusion, may not cause pain but can still reduce hearing clarity. Long-term fluid buildup increases the risk of repeated infections. In rare cases, chronic pressure changes can affect the eardrum or middle ear structures.
Note: If you experience hearing changes lasting more than a few weeks, you should seek medical evaluation. Early treatment helps prevent complications and supports full recovery.
Causes of Mucus Accumulation in the Ear
Mucus builds up in your ear when normal drainage pathways become blocked or inflamed. The most common triggers involve problems with pressure regulation, sinus inflammation, and respiratory infections that increase mucus production.
Eustachian Tube Dysfunction
Your Eustachian tubes connect the middle ear to the back of your throat. They open and close to regulate air pressure and drain fluid from the middle ear.
When these tubes do not open properly, fluid cannot drain. This condition is called Eustachian tube dysfunction (ETD). Negative pressure can develop in the middle ear, pulling fluid into the space behind your eardrum.
Several factors can cause ETD:
- Swelling from allergies
- Inflammation after a cold
- Structural narrowing of the tubes
- Sudden pressure changes, such as during air travel
Note: You may notice ear fullness, muffled hearing, or popping sounds. If the blockage persists, mucus thickens and remains trapped, increasing the risk of temporary hearing loss or infection.
Sinus Infections and Allergies
Your sinuses and middle ear share drainage pathways. When your sinuses become inflamed, swelling can extend to the Eustachian tubes and restrict airflow. Sinus infections increase mucus production and thicken secretions. This excess mucus can move toward the Eustachian tubes and block them, especially if inflammation narrows the openings.
Allergies trigger a similar process. When your immune system reacts to allergens like pollen or dust, it releases chemicals that cause:
- Nasal swelling
- Increased mucus production
- Congestion in the throat and nasal passages
Note: This swelling interferes with normal ear ventilation. If allergic inflammation continues for weeks, fluid may remain trapped in the middle ear and affect how sound travels to the inner ear.
Upper Respiratory Infections
Colds and other upper respiratory infections commonly lead to mucus buildup in your ears. Viruses infect the lining of your nose and throat, causing swelling and increased mucus production. As congestion worsens, your Eustachian tubes may become blocked. Fluid then accumulates behind the eardrum because it cannot drain properly.
Children experience this more often because their Eustachian tubes are shorter and more horizontal. However, adults can also develop fluid buildup after a cold, especially if symptoms linger. In some cases, bacteria grow in the trapped fluid. This can lead to acute otitis media, which often causes pain, pressure, and noticeable hearing reduction.
Signs and Symptoms of Mucus-Related Hearing Loss
Mucus buildup in the middle ear often changes how you perceive sound and pressure. You may notice reduced sound clarity, physical discomfort, or both at the same time.
Muffled Hearing
You may first notice that sounds seem dull or muted, as if you are listening through a layer of cotton. Voices can lose sharpness, and high-pitched sounds often become harder to detect. This happens when mucus collects behind the eardrum and interferes with its normal vibration. Sound waves cannot move efficiently through the middle ear, which reduces how clearly you hear.
You might turn up the television volume more than usual or ask others to repeat themselves. Children often appear inattentive or unresponsive because they do not hear instructions clearly.
Note: Muffled hearing from mucus usually affects one ear but can involve both. The hearing change often fluctuates, especially if the mucus shifts or pressure changes with swallowing or yawning.
Ear Fullness or Pressure
A feeling of fullness, tightness, or pressure in the ear commonly accompanies mucus-related hearing loss. You may feel as if your ear needs to “pop” but cannot. Mucus buildup disrupts normal air flow through the Eustachian tube, which connects your middle ear to the back of your nose. When this tube does not equalize pressure properly, you feel pressure that does not resolve easily.
The sensation may worsen during altitude changes, such as flying or driving uphill. Swallowing or chewing may briefly relieve the pressure, but often does not eliminate it. This pressure can make your hearing seem even more distorted. Some people also notice mild balance changes or a vague sense of unsteadiness.
Associated Ear Pain
Ear pain varies from mild discomfort to sharp, localized pain. You may feel a steady ache deep inside the ear. Pain develops when mucus buildup increases pressure behind the eardrum or when infection occurs. Inflamed tissue becomes sensitive, and even small pressure changes can cause discomfort.
Children may tug at their ears or become irritable. Adults often describe the pain as worse when lying down, especially at night.
If pain intensifies, becomes severe, or accompanies fever or drainage, it may signal an ear infection rather than simple mucus accumulation. Prompt evaluation helps prevent complications and supports faster recovery.
Diagnosis of Hearing Loss Linked to Mucus
Doctors confirm mucus-related hearing loss by examining your ear, measuring how well you hear different sounds, and checking for fluid behind the eardrum. These steps identify whether mucus blocks sound movement or signals a more complex problem.
Physical Examination and Otoscopy
Your clinician starts with a focused history of your symptoms. You may describe muffled hearing, ear fullness, popping, or pressure that worsens during a cold, sinus infection, or allergy flare.
The physical exam centers on otoscopy, where a handheld instrument with a light allows the clinician to inspect your ear canal and eardrum. They look for fluid behind the eardrum, air bubbles, a dull or cloudy appearance, or reduced eardrum movement.
In some cases, the eardrum appears retracted due to Eustachian tube dysfunction. Thick mucus in the middle ear can limit normal vibration.
Your provider may also gently assess eardrum mobility using pneumatic otoscopy. Reduced movement strongly suggests middle ear fluid, which often causes conductive hearing loss rather than nerve-related loss.
Hearing Tests
If fluid buildup affects your hearing, formal testing measures the degree and type of loss. You typically undergo pure-tone audiometry in a sound-treated room. During this test, you respond to tones at different pitches and volumes. Conductive hearing loss from mucus usually shows greater difficulty hearing softer sounds, especially at lower frequencies.
Tympanometry plays a key role in detecting middle ear fluid. This test changes air pressure in your ear canal to evaluate how your eardrum responds. Results often show a “flat” tracing when fluid limits eardrum movement. This pattern supports a diagnosis of middle ear effusion.
Speech testing may also measure how clearly you understand words. With mucus-related conductive loss, clarity often remains relatively preserved once sound volume increases.
Imaging and Additional Assessments
Imaging is not routine for simple mucus buildup. Your provider orders further studies if symptoms persist, worsen, or suggest complications. A CT scan of the temporal bone may evaluate chronic middle ear disease or structural problems. It can reveal thickened tissue, persistent fluid, or blockage of the Eustachian tube.
If sinus disease contributes to excess mucus, imaging of the sinuses may identify inflammation or obstruction. Treating the sinus condition can improve ear symptoms.
In rare cases, referral to an ear, nose, and throat specialist allows for microscopic examination or endoscopic evaluation of the nasal passages and Eustachian tube openings. These assessments help determine whether ongoing mucus production or blockage requires targeted treatment.
Treatment Options for Hearing Loss Caused by Mucus
You can treat hearing loss from mucus by reducing fluid buildup, clearing blockages, and correcting the cause of excess mucus production. Your treatment plan depends on whether the problem affects the outer ear, middle ear, or Eustachian tube.
Medications and Decongestants
If mucus builds up behind your eardrum, your doctor may recommend medications that reduce swelling and improve drainage. Oral decongestants can shrink swollen nasal passages and help open the Eustachian tubes.
Nasal corticosteroid sprays often work better for long-term control. They reduce inflammation inside your nose and improve airflow between your nose and middle ear.
If infection causes the mucus, your doctor may prescribe antibiotics. Antibiotics treat bacterial infections but do not help with viral causes. You may also benefit from antihistamines if allergies trigger mucus production. These medications lower your body’s allergic response and reduce fluid buildup.
Note: Use medications exactly as directed. Overuse of some decongestant sprays can worsen congestion and delay recovery.
Manual Removal and Surgical Interventions
When mucus or fluid does not clear on its own, your doctor may need to remove it. In children and some adults, persistent middle ear fluid may require a minor procedure.
A common option is tympanostomy tube placement. Your surgeon inserts a small tube into the eardrum to ventilate the middle ear and allow fluid to drain. The procedure usually takes less than 15 minutes. It improves hearing quickly by restoring normal air pressure behind the eardrum.
If thick mucus blocks the ear canal, a clinician may perform manual removal using suction or specialized tools. You should not attempt this at home, as improper removal can damage your ear canal or eardrum.
Note: Surgical treatment targets physical blockage. It does not address the underlying cause of excess mucus.
Management of Underlying Conditions
Long-term improvement depends on controlling the condition that causes mucus buildup. You need to identify whether allergies, sinus infections, chronic sinusitis, or structural issues affect your Eustachian tubes.
If allergies contribute, allergy testing and immunotherapy may reduce repeated episodes. Avoiding known triggers also limits mucus production.
For chronic sinusitis, your doctor may recommend saline nasal irrigation, prescription nasal steroids, or referral to an ear, nose, and throat specialist. In severe cases, sinus surgery can improve drainage and reduce recurrent fluid buildup in your ears.
If acid reflux irritates your upper airway, dietary changes and reflux medications may reduce inflammation.
Note: Addressing the root cause lowers your risk of repeated hearing problems and prevents long-term middle ear damage.
Prevention and Long-Term Management of Ear Mucus Buildup
You can reduce the risk of mucus-related hearing problems by managing nasal congestion, limiting inflammation, and monitoring ear symptoms early. Consistent care helps keep the Eustachian tubes open and supports normal middle ear pressure.
Home Care Strategies
You can manage mild mucus buildup at home by keeping your nasal passages clear. Use saline nasal spray or rinses once or twice daily to thin mucus and improve drainage through the Eustachian tubes. Stay well hydrated. Drinking enough water helps keep mucus less thick and easier to clear.
If you have allergies, use prescribed antihistamines or nasal corticosteroid sprays as directed. These reduce swelling inside the nose and help prevent blockage that traps fluid behind the eardrum. Use steam from a warm shower to ease congestion. Avoid inserting cotton swabs or objects into your ear canal, as this can push wax deeper and worsen blockage.
Rest with your head slightly elevated during colds. This position promotes sinus drainage and may reduce pressure in the middle ear.
Note: Seek medical care if symptoms last longer than a few weeks or worsen despite home treatment.
Environmental and Lifestyle Modifications
Control indoor allergens to reduce chronic inflammation. Use high-efficiency air filters and wash bedding weekly in hot water if you have dust mite allergies. Avoid cigarette smoke and secondhand smoke. Smoke irritates the lining of the nose and throat and increases mucus production.
Manage seasonal allergies early. Start preventive allergy medications before peak pollen seasons if your doctor recommends it. Practice good hand hygiene to lower your risk of upper respiratory infections. Viral colds often trigger mucus buildup that affects hearing.
If you swim regularly, dry your ears gently after water exposure. Tilt your head to let trapped water drain and consider using earplugs designed for swimming if you are prone to ear issues.
Note: Maintain a healthy weight and manage acid reflux if present. Reflux can irritate the throat and contribute to Eustachian tube dysfunction.
Monitoring and Follow-Up
Track symptoms such as ear fullness, muffled hearing, popping sounds, or balance changes. Persistent symptoms lasting more than 2–3 weeks require medical evaluation. Schedule follow-up visits if you experience repeated ear infections or ongoing fluid behind the eardrum. Your clinician may perform tympanometry or hearing tests to assess middle ear function.
Children need closer monitoring. Ongoing fluid can affect speech and learning, so regular pediatric checks are important.
If conservative treatment fails, your doctor may discuss procedures such as ear tube placement to improve ventilation. Early monitoring prevents long-term hearing changes and reduces the risk of complications.
FAQs About Mucus and Hearing Loss
What Causes Mucus Behind the Eardrum?
Mucus behind the eardrum usually develops when the Eustachian tubes become blocked. These small tubes connect the middle ear to the back of the throat and help regulate pressure and drain fluid. Colds, sinus infections, allergies, and upper respiratory infections can cause inflammation and excess mucus production, which prevents proper drainage.
When fluid becomes trapped in the middle ear, it can create a sensation of fullness, muffled hearing, or mild discomfort. Children are especially prone to this because their Eustachian tubes are shorter and more easily obstructed.
How Do You Get Rid of Hearing Loss From a Cold?
Hearing loss from a cold is typically temporary and improves as congestion resolves. Staying well hydrated helps thin mucus, making it easier to drain. Saline nasal sprays, steam inhalation, and humidified air may reduce nasal congestion and support Eustachian tube function.
Over-the-counter decongestants or antihistamines may help in certain cases, though they are not appropriate for everyone. Gentle swallowing, yawning, or chewing gum can also help equalize ear pressure.
Note: If symptoms persist beyond a couple of weeks, medical evaluation is recommended.
What Helps Hearing Loss When Sick?
When you are sick, managing inflammation and congestion is key to improving hearing. Rest and adequate fluid intake support recovery and help thin secretions. Warm compresses over the sinuses may ease pressure. Nasal saline rinses can help clear mucus from the nasal passages, improving drainage through the Eustachian tubes.
Avoid forceful nose blowing, which can worsen ear pressure. If pain, fever, or worsening symptoms occur, a healthcare provider should evaluate for possible middle ear infection.
How Long Does Hearing Loss From a Cold Last?
Temporary hearing loss caused by a cold often lasts a few days to two weeks, depending on how quickly congestion improves. In some cases, fluid may remain behind the eardrum even after other cold symptoms resolve.
This condition, sometimes called otitis media with effusion, can cause muffled hearing for several weeks. Most cases resolve on their own without treatment. However, if hearing changes persist longer than three to four weeks or worsen, it is important to seek medical evaluation.
How Do I Get Rid Of Mucus Behind My Eardrum?
Clearing mucus behind the eardrum usually involves improving Eustachian tube drainage. Treating the underlying cause, such as a cold or allergies, is essential. Hydration, nasal saline irrigation, and humidified air may help thin secretions.
In some cases, a healthcare provider may recommend medications to reduce inflammation. If fluid persists for an extended period or causes significant hearing problems, medical procedures such as ear tube placement may be considered.
Note: Most mild cases improve gradually without invasive treatment.
Can Sinus Congestion Affect Hearing?
Yes, sinus congestion can affect hearing because the sinuses and middle ear share connected drainage pathways. When sinus inflammation causes swelling and mucus buildup, it can block the Eustachian tubes.
This prevents normal pressure equalization in the middle ear, leading to muffled sounds or a feeling of clogged ears. The hearing loss is typically conductive and temporary. Once sinus congestion improves and normal airflow is restored, hearing generally returns to baseline without permanent damage.
Can Allergies Cause Hearing Loss?
Allergies can contribute to temporary hearing loss by causing inflammation and excess mucus production in the nasal passages and Eustachian tubes. When these tubes become swollen or blocked, fluid may accumulate in the middle ear.
This can result in muffled hearing, ear pressure, or popping sensations. Managing allergies with avoidance strategies and appropriate treatment can reduce inflammation and improve drainage. Persistent or severe symptoms should be evaluated to rule out secondary infections.
When To See A Doctor For Mucus-Related Hearing Loss?
You should see a doctor if hearing loss lasts more than a few weeks, worsens over time, or is accompanied by significant pain, fever, dizziness, or drainage from the ear. Sudden hearing loss in one or both ears requires immediate medical attention.
Persistent fluid buildup can sometimes lead to infection or other complications. Early evaluation ensures that underlying conditions are identified and treated appropriately, reducing the risk of long-term hearing problems.
Final Thoughts
In most cases, mucus-related hearing loss is temporary and resolves once congestion improves and the Eustachian tubes begin functioning normally again. Because the ears, nose, and throat are closely connected, excess mucus from colds, allergies, or sinus infections can easily disrupt middle ear pressure and fluid balance.
While this type of hearing loss is usually mild and reversible, persistent ear fullness, pain, or changes in hearing should not be ignored.
Seeking medical evaluation ensures that more serious conditions are ruled out and that appropriate treatment is provided. Managing underlying congestion is often the key to restoring clear, comfortable hearing.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Zhen Z, Zhao T, Wang Q, Zhang J, Zhong Z. Laryngopharyngeal reflux as a potential cause of Eustachian tube dysfunction in patients with otitis media with effusion. Front Neurol. 2022.
- Sooriyamoorthy T, De Jesus O. Conductive Hearing Loss. [Updated 2023 Aug 23]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025.