Throwing up mucus can be an unpleasant and confusing experience, especially if it happens unexpectedly. In many cases, the mucus you vomit does not originate from the stomach but from the respiratory system or sinuses, where it is produced to trap dust, bacteria, and other irritants.
When excess mucus builds up in the throat or stomach, it can trigger nausea and vomiting as the body tries to clear it.
Understanding why this happens can help you identify the underlying cause and determine whether it is related to a temporary condition, such as a cold or sinus infection, or something that may require medical attention.
Download our free guide that has over 100+ of the best tips for healthy lungs.
Can Mucus Cause Vomiting?
Yes, mucus can sometimes cause vomiting, especially when it accumulates in large amounts in the throat or stomach. Excess mucus is often produced during respiratory infections, sinus drainage, allergies, or postnasal drip. When this mucus is swallowed repeatedly, it can irritate the stomach lining and trigger nausea.
In some cases, the body responds by vomiting in an attempt to clear the mucus from the digestive tract. Thick mucus in the throat may also stimulate the gag reflex, which can lead to retching or vomiting.
While this is usually temporary and related to conditions like colds or sinus infections, persistent vomiting of mucus may indicate an underlying issue and should be evaluated by a healthcare professional if it continues.
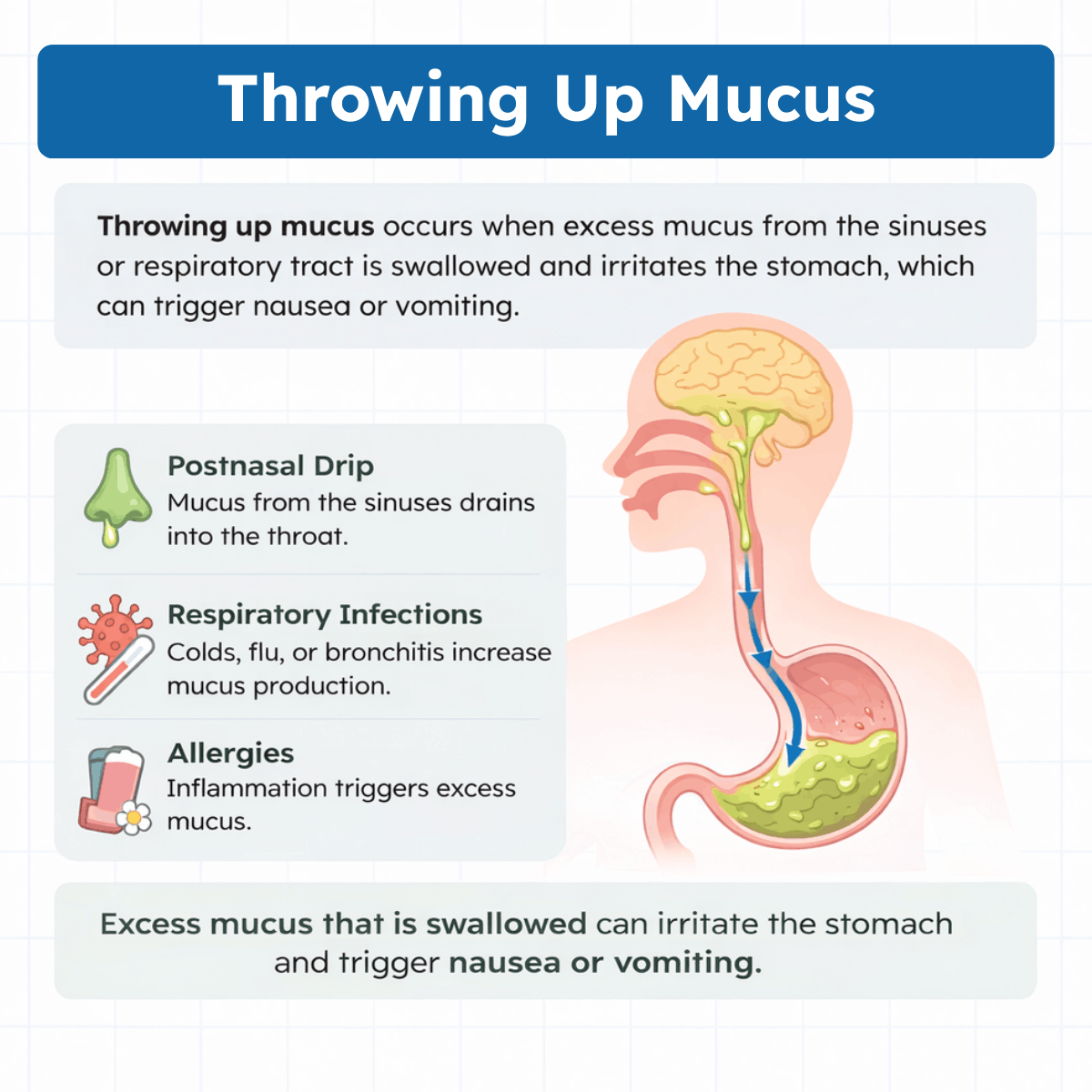
Why Is There Mucus in My Vomit?
Mucus may appear in your vomit when excess mucus from the respiratory tract or sinuses is swallowed and mixes with stomach contents. This commonly happens during conditions such as colds, sinus infections, allergies, or postnasal drip, where the body produces more mucus to trap and remove irritants, bacteria, and viruses.
As the mucus drains down the throat, it can be swallowed and accumulate in the stomach, which may irritate the stomach lining and trigger nausea or vomiting. In some cases, coughing or gagging caused by thick mucus can also lead to vomiting.
Note: While this is often temporary and related to minor illnesses, persistent vomiting of mucus may indicate an underlying problem and should be evaluated by a healthcare professional.
Understanding Throwing Up Mucus
Throwing up mucus involves expelling thick, slippery fluid instead of typical food contents. It often relates to irritation in the stomach, throat, or sinuses and may signal infection, inflammation, or excess drainage.
What Is Mucus Vomiting
Mucus vomiting occurs when a person expels clear, white, or yellowish phlegm-like material during an episode of nausea or retching. The material may come from the stomach, but it often includes mucus that drains from the nose or throat and is then swallowed.
The stomach naturally produces mucus to protect its lining from acid. When irritation develops—such as from viral gastroenteritis, gastritis, or food poisoning—the body may empty stomach contents that include this protective fluid.
Postnasal drip can also contribute. Excess sinus mucus collects in the throat, gets swallowed, and later appears during vomiting. In some cases, a person may vomit mucus even when little or no food remains in the stomach. This commonly happens after repeated vomiting episodes or prolonged nausea.
Common Characteristics
Mucus in vomit usually appears thick, stringy, or gelatinous. It may look clear or milky white, though yellow or green tinges can appear when bile or sinus drainage mixes in. People often report a sour or bitter taste. The texture feels slippery rather than chunky, which distinguishes it from partially digested food.
Other symptoms often occur at the same time. These may include:
- Nausea
- Abdominal cramping
- Coughing or throat clearing
- Sinus congestion
- Fever in cases of infection
The amount varies. Some people expel only small streaks mixed with fluid, while others bring up larger volumes after repeated retching.
Note: If blood appears red or dark brown, medical evaluation becomes important. Persistent vomiting, dehydration, or severe abdominal pain also requires prompt care.
How It Differs From Regular Vomiting
Regular vomiting typically contains partially digested food, stomach acid, and bile. It often follows overeating, food intolerance, infection, or motion sickness. Mucus vomiting, by contrast, contains little solid material. The expelled fluid looks smoother and more uniform.
Timing can also differ. A person may vomit mucus after the stomach empties completely, especially during ongoing nausea. In respiratory infections, coughing can trigger gagging that brings up mucus without true stomach illness.
The underlying cause helps distinguish the two. Gastrointestinal disorders mainly produce food and bile, while sinus infections, postnasal drip, and throat irritation increase visible mucus content.
Note: Recognizing the texture, color, and associated symptoms helps determine whether the source is digestive, respiratory, or both.
Causes of Throwing Up Mucus
Several conditions can lead to vomiting mucus, especially when the body produces excess secretions or the stomach becomes irritated. In most cases, respiratory infections, digestive disorders, allergies, or ongoing postnasal drip explain the symptom.
Respiratory Infections
Respiratory infections often increase mucus production in the nose, throat, and lungs. When this mucus drains downward or triggers persistent coughing, it can irritate the throat and stomach lining.
Viral infections such as the common cold, influenza, and COVID-19 frequently cause thick nasal discharge and chest congestion. Bacterial infections like bronchitis or pneumonia can also lead to heavy mucus buildup.
Repeated coughing strains the stomach muscles and may trigger gagging or vomiting. When the stomach is mostly empty, the person may expel clear, white, or yellowish mucus instead of food.
Fever, sore throat, chest tightness, and fatigue often appear alongside these infections. If vomiting mucus continues after other symptoms improve, lingering airway inflammation may still be driving mucus production.
Gastrointestinal Issues
Certain digestive conditions directly irritate the stomach and increase mucus secretion. The stomach naturally produces mucus to protect its lining, but inflammation can increase this output.
Gastritis, which involves inflammation of the stomach lining, often results from infection, alcohol use, frequent NSAID use, or severe stress. It can cause nausea, abdominal discomfort, and vomiting of clear or foamy mucus.
Acid reflux and gastroesophageal reflux disease (GERD) can also contribute. Stomach acid that repeatedly flows back into the esophagus irritates both the esophageal lining and throat, sometimes leading to excess mucus and gagging.
Food poisoning and stomach viruses may cause repeated vomiting after the stomach empties. At that stage, the body may expel bile mixed with mucus.
Note: Persistent abdominal pain, blood in vomit, or black stools require urgent medical evaluation.
Allergic Reactions
Allergic reactions commonly increase mucus production in the airways. When the immune system reacts to allergens such as pollen, dust mites, or pet dander, it triggers inflammation and fluid release. This response leads to nasal congestion, sneezing, itchy eyes, and throat irritation. Thick mucus may collect in the back of the throat and provoke nausea, especially in children.
Severe coughing or repeated throat clearing can stimulate the gag reflex. In some cases, this results in vomiting mucus rather than food.
Food allergies may also cause nausea and vomiting. Unlike mild environmental allergies, food-related reactions can include hives, swelling, abdominal pain, or breathing difficulty.
Note: Any signs of throat swelling, wheezing, or trouble breathing require immediate emergency care.
Postnasal Drip
Postnasal drip occurs when excess mucus from the nasal passages drains down the back of the throat. It often develops from colds, sinus infections, allergies, or exposure to irritants such as smoke. The constant flow of mucus irritates the throat and can trigger chronic coughing. Over time, this irritation may stimulate nausea.
Mucus that collects overnight frequently causes morning gagging or vomiting. The vomit often appears clear, white, or slightly yellow and may feel thick or sticky.
People with chronic sinusitis may experience facial pressure, nasal blockage, and reduced sense of smell in addition to mucus buildup. Treating the underlying sinus or allergy issue typically reduces both postnasal drip and mucus-related vomiting.
Associated Symptoms
Throwing up mucus often occurs alongside respiratory or throat symptoms. These signs help identify whether the cause relates to infection, irritation, or excess mucus production in the airways.
Coughing and Congestion
Coughing commonly accompanies mucus vomiting, especially when the source is the upper or lower respiratory tract. The body produces excess mucus in response to infection, allergies, or irritation, and a persistent cough can trigger gagging or vomiting.
Congestion in the nose or chest often worsens this cycle. Thick nasal discharge may drain down the back of the throat, a process known as postnasal drip. This drainage irritates the throat and stomach, leading to nausea or retching.
Chest congestion may also cause a person to cough forcefully to clear mucus from the lungs. Repeated coughing increases abdominal pressure and can result in vomiting mucus rather than food.
Key features to watch for include:
- Frequent throat clearing
- Thick, cloudy, or greenish mucus
- A cough that worsens at night
- A feeling of mucus stuck in the throat
Note: When coughing lasts more than three weeks or produces blood, medical evaluation becomes important.
Fever and Fatigue
Fever suggests that infection plays a role in mucus production. Viral illnesses such as the common cold, influenza, or COVID-19 often cause both increased mucus and systemic symptoms. A temperature above 100.4°F (38°C) signals active inflammation. The body raises its temperature to fight pathogens, but this response also increases fluid loss and overall weakness.
Fatigue often develops alongside fever. The immune system consumes energy, leaving the person feeling tired, achy, and less alert. In children, fatigue combined with vomiting mucus may appear as irritability or reduced activity.
Persistent high fever, shaking chills, or symptoms lasting more than several days may indicate bacterial infection. Conditions such as sinusitis or pneumonia can produce thick mucus along with significant exhaustion.
Sore Throat
A sore throat frequently develops when mucus irritates the lining of the throat. Continuous drainage or coughing creates inflammation and discomfort. The pain may feel scratchy, raw, or burning. Swallowing can worsen the discomfort, and repeated gagging or vomiting may further irritate the tissue.
Redness and mild swelling often appear in the back of the throat. In some cases, enlarged tonsils or white patches suggest bacterial infection, such as strep throat.
Dry indoor air, smoking exposure, or acid reflux can intensify throat irritation. When throat pain becomes severe, interferes with breathing, or lasts longer than a week, a healthcare professional should assess the cause.
When to Seek Medical Attention
Throwing up mucus often relates to irritation in the stomach, throat, or sinuses, but certain symptoms signal a more serious problem. Prompt evaluation helps prevent dehydration, infection, or complications involving the lungs or digestive tract.
Warning Signs
Seek medical care if vomiting mucus lasts longer than 24–48 hours in adults or more than 8–12 hours in young children. Persistent vomiting can quickly lead to dehydration, especially if the person cannot keep fluids down.
Watch for blood in the vomit, dark brown material that looks like coffee grounds, or bright red streaks. These signs may indicate bleeding in the digestive tract and require immediate evaluation. Severe abdominal pain, a rigid abdomen, high fever above 101°F (38.3°C), or a stiff neck also require prompt attention. These symptoms can point to infections, inflammation, or obstruction.
Breathing problems are another urgent concern. If the person coughs persistently, wheezes, or feels short of breath after vomiting mucus, aspiration into the lungs may have occurred.
Signs of dehydration demand quick treatment. These include dry mouth, minimal urination, dizziness, rapid heartbeat, and extreme fatigue.
Potential Complications
Repeated vomiting of mucus can irritate the esophagus and throat. Ongoing irritation may cause inflammation, small tears, or worsening acid reflux symptoms. Aspiration presents a serious risk. When mucus or stomach contents enter the airway, they can trigger aspiration pneumonia, which may cause cough, chest pain, fever, and difficulty breathing within hours or days.
Chronic sinus infections or severe postnasal drip may also underlie persistent mucus vomiting. Without treatment, infection can spread or become recurrent.
Electrolyte imbalances can develop after prolonged vomiting. Low potassium levels may cause muscle weakness, irregular heart rhythms, or confusion.
People with underlying conditions—such as diabetes, kidney disease, or compromised immune systems—face higher risks from fluid loss and infection. They should seek care sooner rather than waiting for symptoms to worsen.
Pediatric Concerns
Infants and young children require closer monitoring because they dehydrate faster than adults. Fewer wet diapers, absence of tears when crying, sunken eyes, or a sunken soft spot on an infant’s head signal urgent dehydration.
Projectile vomiting, green or bright yellow bile, or forceful vomiting after every feeding requires immediate medical evaluation. These signs may indicate obstruction or other serious gastrointestinal conditions. If a child appears unusually sleepy, difficult to wake, irritable, or confused, medical assessment is necessary. Behavioral changes often signal more than simple stomach upset.
Any breathing difficulty, persistent cough after vomiting, or bluish discoloration around the lips calls for emergency care. Children can aspirate quickly, and early treatment reduces complications.
Diagnosis of Mucus Vomiting
Clinicians identify the cause of mucus vomiting by combining a focused history, a targeted physical exam, and selected laboratory tests. This approach helps distinguish minor irritation from infections, gastrointestinal disorders, or more serious disease.
Medical History
A detailed medical history guides the evaluation. The clinician asks when the vomiting started, how often it occurs, and whether it contains clear, white, yellow, or green mucus. The presence of blood, bile, fever, abdominal pain, weight loss, or dehydration is critical.
They also assess recent respiratory infections, sinus congestion, persistent cough, or postnasal drip. Swallowed mucus from upper airway inflammation commonly triggers nausea and vomiting, especially in children.
Dietary habits, recent food intake, alcohol use, medication changes, and exposure to sick contacts provide further clues. Chronic conditions such as asthma, acid reflux, gastritis, or food allergies may contribute.
In infants and young children, feeding patterns, formula changes, and growth history matter. For adults, pregnancy status, recent travel, and stress levels may also influence symptoms.
Physical Examination
The physical exam focuses on hydration, abdominal findings, and signs of respiratory illness. The clinician checks vital signs, including temperature, heart rate, and blood pressure, to identify infection or dehydration.
Inspection of the nose and throat may reveal inflamed nasal passages, sinus tenderness, or thick mucus. Lung examination can detect wheezing or crackles that suggest lower respiratory involvement.
Abdominal palpation helps identify tenderness, guarding, or distention. Localized pain may indicate gastritis, appendicitis, or obstruction.
Note: The clinician also evaluates skin turgor, dry mucous membranes, and capillary refill time. These findings help determine whether fluid loss requires urgent treatment.
Laboratory Tests
Laboratory testing depends on symptom severity and duration. Mild, short-term mucus vomiting often requires no tests.
If symptoms persist or worsen, clinicians may order blood tests to assess electrolyte levels, kidney function, and markers of infection such as white blood cell count. Abnormalities can signal dehydration or systemic illness.
A stool test may help when diarrhea accompanies vomiting, especially if bacterial or viral infection is suspected. In selected cases, testing for food intolerances or Helicobacter pylori may be appropriate.
Imaging studies, such as abdominal ultrasound or X-ray, are reserved for cases with severe pain, suspected obstruction, or unclear diagnosis. These tests help rule out structural causes that require immediate care.
Treatment Options
Treatment depends on the cause of the mucus and the severity of symptoms. Most cases improve with simple measures, but persistent or severe vomiting may require medical care.
Home Remedies
If mucus vomiting stems from a cold, postnasal drip, or mild stomach irritation, home care often helps. Rest allows the body to recover and reduces strain on the digestive system.
Hydration remains essential. Small, frequent sips of water, oral rehydration solutions, or clear broths help replace lost fluids and thin thick mucus. Warm liquids such as herbal tea or broth can loosen congestion and soothe throat irritation.
Humid air can reduce nasal and throat dryness. A cool-mist humidifier or a steamy shower may ease mucus buildup linked to sinus congestion. They should avoid large meals, greasy foods, alcohol, and caffeine until symptoms improve. Eating bland foods such as rice, toast, bananas, or applesauce can reduce stomach irritation.
Medical Treatments
A clinician will first identify the underlying cause. They may review symptoms, examine the throat and abdomen, and order tests if they suspect infection, reflux disease, or another condition.
If postnasal drip drives mucus production, treatment may target sinus inflammation or allergies. For suspected gastroesophageal reflux disease (GERD), lifestyle adjustments and acid-reducing therapies often reduce both nausea and mucus irritation.
When dehydration develops, medical staff may provide intravenous fluids. This step becomes important if the person cannot keep liquids down or shows signs such as dizziness, dry mouth, or reduced urination.
Persistent vomiting, severe abdominal pain, blood in vomit, or high fever requires prompt evaluation. These signs may point to conditions that need urgent treatment.
Prescription Medications
Doctors may prescribe medications based on the diagnosed cause. For bacterial sinus infections, they may use antibiotics when symptoms meet clinical criteria.
For chronic acid reflux, providers often prescribe proton pump inhibitors (PPIs) or H2 blockers. These drugs reduce stomach acid and limit irritation that can trigger nausea and mucus production.
If severe nausea continues, antiemetic medications such as ondansetron may help control vomiting. These drugs work by blocking signals in the brain that trigger the vomiting reflex.
In cases linked to allergies, prescription-strength antihistamines or nasal corticosteroids may reduce mucus production. They target inflammation in the nasal passages, which decreases drainage into the throat and stomach.
Preventing Mucus Vomiting
Preventing mucus vomiting requires reducing excess mucus production and limiting triggers that irritate the stomach and throat. Consistent daily habits can lower inflammation, control postnasal drip, and support normal digestion.
Lifestyle Adjustments
Daily routines directly affect mucus production and stomach sensitivity. He or she should avoid smoking and secondhand smoke, as tobacco irritates the respiratory lining and increases thick mucus.
Eating smaller, balanced meals helps prevent reflux, which can mix stomach acid with mucus and trigger vomiting. Spicy foods, fried items, and heavy late-night meals often worsen symptoms. Limiting these reduces throat irritation and nausea.
Elevating the head during sleep can reduce nighttime postnasal drip and acid reflux. A wedge pillow or adjustable bed works better than stacking regular pillows.
Regular physical activity also improves sinus drainage and digestion. Moderate exercise, such as brisk walking for 30 minutes most days, supports respiratory health without overstimulating the stomach.
Note: Stress management plays a role as well. Chronic stress can worsen nausea and gastrointestinal sensitivity, increasing the likelihood of vomiting mucus.
Controlling Allergens
Allergies often drive excess mucus production. Identifying and limiting exposure to triggers reduces postnasal drip and throat irritation.
Common indoor allergens include dust mites, mold, pet dander, and cockroaches. Washing bedding weekly in hot water, using allergen-proof mattress covers, and vacuuming with a HEPA filter can lower exposure. Keeping indoor humidity between 30% and 50% also helps prevent mold growth.
Outdoor allergens such as pollen require different strategies. He or she should check daily pollen counts and keep windows closed during high levels. Showering and changing clothes after spending time outdoors removes pollen from skin and hair.
Air purifiers with HEPA filters can reduce airborne particles in frequently used rooms. For persistent symptoms, a healthcare provider may recommend antihistamines or nasal corticosteroids to control inflammation and limit mucus buildup.
Proper Hydration
Adequate fluid intake keeps mucus thin and easier to clear. Thick, sticky mucus is more likely to accumulate in the throat and trigger gagging or vomiting.
Most adults benefit from steady fluid intake throughout the day rather than large amounts at once. Water remains the best option. Warm fluids, such as herbal tea or broth, can soothe throat irritation and promote drainage.
He or she should limit beverages that dehydrate, including excessive caffeine and alcohol. These can thicken mucus and irritate the stomach lining.
During illness, fluid needs often increase. Signs of adequate hydration include pale yellow urine and regular urination. Maintaining consistent hydration supports normal mucus consistency and reduces the likelihood of buildup that leads to nausea and vomiting.
Impact on Daily Life
Throwing up mucus can disrupt daily routines and lower overall comfort. The act itself often causes fatigue, throat irritation, and a lingering bad taste. These effects can make it harder to focus at work or school.
Many people feel uneasy about eating. Nausea or fear of another episode may lead them to skip meals or limit certain foods. This can reduce energy levels and affect concentration.
Sleep may also suffer. Nighttime coughing, postnasal drip, or stomach discomfort can wake them repeatedly. Poor sleep can lead to daytime drowsiness and irritability.
Social situations sometimes become stressful. They may avoid gatherings if symptoms feel unpredictable or embarrassing. This avoidance can reduce participation in normal activities.
Physical symptoms often overlap with other issues, such as:
- Sore throat or hoarseness
- Chest discomfort or heartburn
- Persistent cough
- Dehydration from repeated vomiting
Note: Frequent episodes may also increase anxiety about underlying health problems. Ongoing worry can affect mood and reduce productivity. When symptoms continue, daily planning often revolves around managing triggers and staying near restrooms. This adjustment can limit travel, exercise, or long meetings.
Throwing Up Mucus in Children
Children often throw up mucus when they have a cold, flu, sinus infection, or seasonal allergies. Their bodies produce extra mucus, and they may swallow it throughout the day. This buildup can irritate the stomach and trigger vomiting.
Infants and toddlers are especially prone to this because they spend more time lying down. Mucus can pool in the back of the throat and lead to gagging or coughing. The vomit may look clear, white, yellow, or slightly green.
Common causes include:
- Upper respiratory infections
- Postnasal drip
- Crying for long periods
- Coughing fits
- Mild stomach viruses
If a child vomits mucus but remains active, drinks fluids, and has normal urine output, the cause is often minor. Parents should still watch for dehydration. Signs include dry lips, fewer wet diapers, or dark urine.
Medical care is important if the child has:
- A high or persistent fever
- Severe abdominal pain
- Trouble breathing
- Signs of dehydration
- Blood or dark green bile in the vomit
Infants under 3 months who vomit repeatedly require prompt evaluation. Persistent vomiting, even without other symptoms, also needs medical review.
Note: Most cases improve as the underlying illness clears. Keeping the child hydrated and managing nasal congestion can reduce mucus buildup and related vomiting.
FAQs About Throwing Up Mucus
How Do You Get Rid of Mucus in Your Stomach?
Mucus in the stomach is often caused by swallowing excess mucus from the sinuses or respiratory tract. Treating the underlying cause, such as a cold, allergies, or postnasal drip, can help reduce mucus buildup. Drinking plenty of fluids can thin mucus and make it easier for the body to clear.
Warm liquids, saline nasal sprays, and humidifiers may also help reduce mucus production. If mucus buildup is persistent or accompanied by severe symptoms such as vomiting, abdominal pain, or fever, it is important to consult a healthcare provider for proper evaluation.
Why Am I Throwing Up Yellow Mucus?
Yellow mucus in vomit often contains stomach fluids or bile mixed with mucus. This can happen when the stomach is empty and the body continues to retch or vomit. Respiratory infections, postnasal drip, and sinus drainage can also cause mucus to be swallowed and later expelled during vomiting.
The yellow color may indicate digestive juices mixing with mucus in the stomach. While occasional episodes may occur during illness, frequent vomiting of yellow mucus could signal irritation of the stomach or another medical issue that should be evaluated by a healthcare professional.
How Do I Stop Throwing Up Clear Mucus?
Clear mucus in vomit is often related to swallowed mucus from postnasal drip, allergies, or respiratory infections. Staying well hydrated can help thin mucus and make it easier to clear from the throat.
Treating congestion with saline sprays, antihistamines, or other recommended treatments may also reduce mucus production. Eating small, bland meals may help calm the stomach if nausea is present.
Note: If clear mucus vomiting happens repeatedly, lasts for several days, or occurs alongside other concerning symptoms, it is best to seek medical advice for further evaluation.
Why Am I Throwing Up Foam and Mucus?
Foamy vomit mixed with mucus can occur when air, saliva, and stomach fluids combine during episodes of nausea or vomiting. This may happen when excess mucus from the respiratory tract is swallowed and irritates the stomach. Conditions such as postnasal drip, respiratory infections, or severe coughing can contribute to this symptom.
In some cases, an empty stomach may produce foamy vomit when there is little food present. While it is often temporary, persistent foamy vomiting or other symptoms like severe pain or dehydration should be evaluated by a healthcare professional.
Will Throwing Up Get Rid of Mucus in the Throat?
Vomiting may temporarily remove some mucus that has been swallowed or accumulated in the throat, but it is not an effective or healthy way to clear mucus. The body normally removes mucus through coughing, swallowing, or the mucociliary clearance system in the airways.
Repeated vomiting can irritate the throat and stomach and may worsen symptoms over time. Instead, staying hydrated, using humidified air, and treating the underlying cause—such as allergies or infection—are safer ways to help reduce mucus and improve comfort.
Can Mucus Cause Nausea?
Yes, excess mucus can sometimes lead to nausea, especially when large amounts are swallowed. Postnasal drip from sinus infections, allergies, or colds may cause mucus to drain into the throat and eventually reach the stomach. When mucus accumulates in the stomach, it can irritate the stomach lining and trigger feelings of nausea.
In some cases, this irritation may even lead to vomiting. Managing the source of mucus production, such as treating congestion or sinus inflammation, can help reduce nausea and prevent further digestive discomfort.
What Medical Condition Is Associated with Mucus in Vomit?
Several medical conditions can lead to mucus appearing in vomit. Common causes include sinus infections, respiratory infections, postnasal drip, allergies, and severe coughing that leads to swallowed mucus. Gastrointestinal irritation, acid reflux, and certain infections may also contribute to nausea and vomiting that contains mucus.
In children, mucus vomiting is often linked to upper respiratory illnesses. While occasional episodes may occur during illness, persistent mucus in vomit may indicate an underlying condition that should be evaluated by a healthcare professional.
Should You Be Concerned About Mucus in Your Child’s Vomit?
Mucus in a child’s vomit is often related to swallowed mucus from a cold, sinus congestion, or postnasal drip. Young children frequently swallow mucus because they cannot easily cough or spit it out.
When enough mucus accumulates in the stomach, it may trigger vomiting. In most cases, this is temporary and resolves as the illness improves. However, parents should seek medical attention if the child has persistent vomiting, signs of dehydration, high fever, severe abdominal pain, or difficulty breathing.
Can You Throw Up Mucus from Your Lungs?
Mucus produced in the lungs is usually removed through coughing rather than vomiting. However, when large amounts of mucus are coughed up and swallowed, it may irritate the stomach and lead to vomiting.
Respiratory conditions such as bronchitis, pneumonia, or severe coughing fits can increase mucus production and contribute to this process. While the mucus itself originates from the respiratory tract, the act of vomiting occurs because the stomach becomes irritated by the swallowed mucus or by intense coughing.
Is Throwing Up Mucus Normal During Pregnancy?
Throwing up mucus can sometimes occur during pregnancy, especially if a person experiences frequent nausea or morning sickness. Hormonal changes during pregnancy can also increase mucus production in the nasal passages and throat.
When excess mucus is swallowed, it may irritate the stomach and contribute to nausea or vomiting. While occasional episodes may not be unusual, persistent vomiting or severe nausea during pregnancy should be discussed with a healthcare provider to ensure proper care and hydration.
Final Thoughts
Throwing up mucus can be uncomfortable, but it is often the result of excess mucus production from conditions such as colds, sinus infections, allergies, or postnasal drip. When mucus accumulates and is swallowed, it can irritate the stomach or trigger the gag reflex, leading to nausea and vomiting.
In most cases, this symptom is temporary and improves as the underlying condition resolves. However, if vomiting mucus occurs frequently, is severe, or is accompanied by other concerning symptoms such as fever, dehydration, or persistent coughing, it is important to seek medical advice. Identifying and treating the underlying cause can help reduce mucus buildup and prevent further discomfort.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Maule WF. Nausea and Vomiting. In: Walker HK, Hall WD, Hurst JW, editors. Clinical Methods: The History, Physical, and Laboratory Examinations. 3rd edition. Boston: Butterworths; 1990.
- McShane A, Bath J, Jaramillo AM, Ridley C, Walsh AA, Evans CM, Thornton DJ, Ribbeck K. Mucus. Curr Biol. 2021.