Breathing is usually an automatic, rhythmic process controlled by the brainstem. However, certain neurological injuries can disrupt this rhythm, resulting in abnormal breathing patterns that provide vital diagnostic clues. One such pattern is apneustic breathing, a rare but clinically significant respiratory abnormality.
Understanding this condition is essential for respiratory therapists, as it not only aids in patient assessment but also guides decisions regarding mechanical ventilation and overall care.
What is Apneustic Breathing?
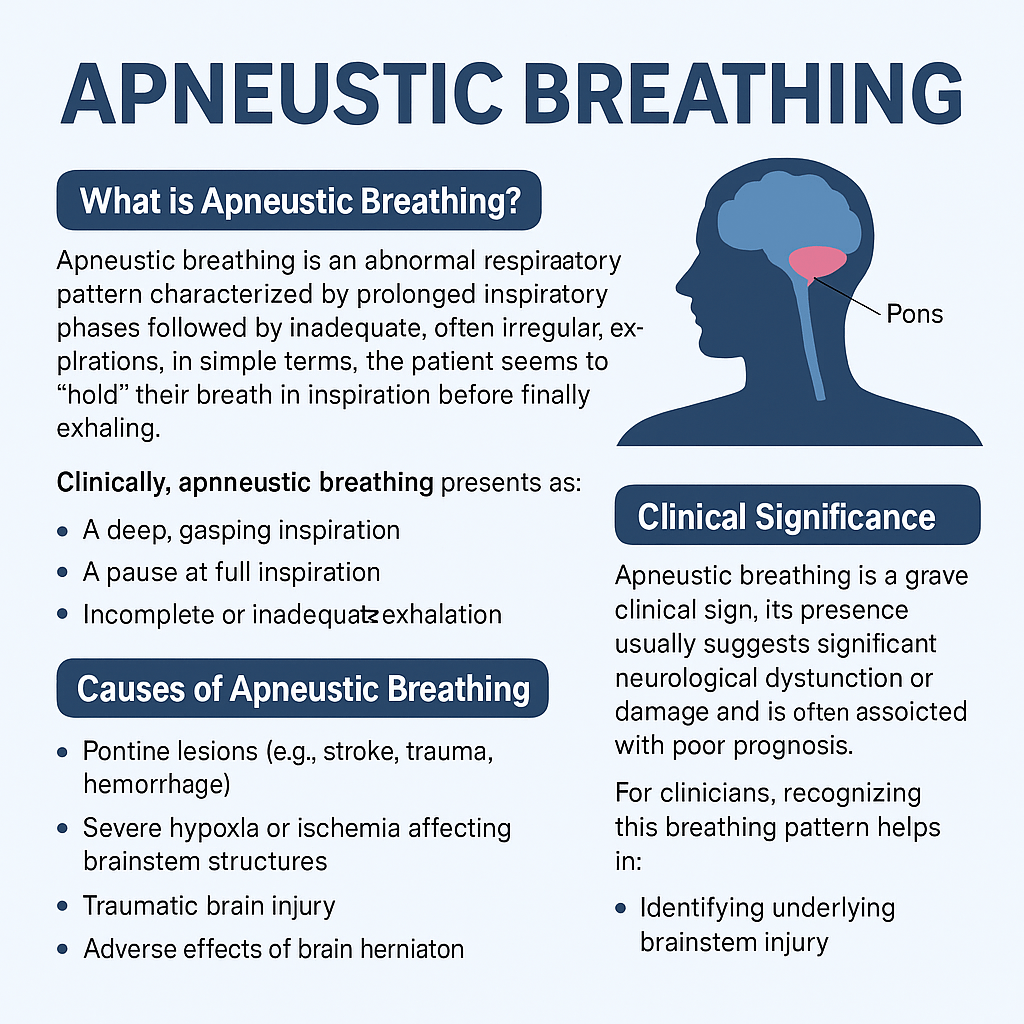
Apneustic breathing is an abnormal respiratory pattern characterized by prolonged inspiratory phases followed by inadequate, often irregular, expirations. In simple terms, the patient seems to “hold” their breath in inspiration before finally exhaling.
This breathing pattern is typically associated with damage to the pons, specifically the lower pons, where critical neural centers for inspiration and expiration are located.
Characteristics
Clinically, apneustic breathing presents as:
- A deep, gasping inspiration
- A pause at full inspiration
- Incomplete or inadequate exhalation
Note: It is often observed in patients with severe neurological injury, particularly pontine lesions, brainstem strokes, or hypoxic brain damage.
Causes of Apneustic Breathing
The primary causes include:
- Pontine lesions (e.g., stroke, trauma, hemorrhage)
- Severe hypoxia or ischemia affecting brainstem structures
- Traumatic brain injury
- Adverse effects of brain herniation
- Drug toxicity (rare cases with CNS depressants)
Note: Because the pons integrates and balances input from higher cortical centers and the medulla, disruption leads to this abnormal inspiratory “holding” pattern.
Clinical Significance
Apneustic breathing is a grave clinical sign. Its presence usually suggests significant neurological dysfunction or damage and is often associated with poor prognosis. For clinicians, recognizing this breathing pattern helps in:
- Identifying underlying brainstem injury
- Determining the severity of neurological compromise
- Deciding when advanced airway management or ventilatory support is necessary
Relevance to Respiratory Therapists
For respiratory therapists, understanding and identifying apneustic breathing is crucial in several ways:
1. Patient Assessment
Abnormal breathing patterns are often among the first observable signs of neurological deterioration. Detecting apneustic breathing at the bedside allows respiratory therapists to alert the medical team promptly, ensuring rapid diagnostic and therapeutic interventions.
2. Ventilatory Support
Patients exhibiting apneustic breathing often require mechanical ventilation due to inadequate spontaneous ventilation and oxygenation. RTs play a central role in setting up and monitoring ventilators, ensuring appropriate tidal volumes, pressures, and oxygen delivery.
3. Neurological Monitoring
Because apneustic breathing directly points to pontine dysfunction, it provides insight into the neurological status of critically ill patients. Respiratory therapists, who closely monitor ventilatory patterns, become vital contributors in multidisciplinary neurocritical care teams.
4. Education and Advocacy
RTs also help educate families and healthcare staff about the implications of abnormal breathing patterns. This advocacy role is important in settings where decisions about prognosis and care planning are being made.
Implications for Respiratory Care
- Early recognition: Quick identification of apneustic breathing can accelerate diagnostic imaging and treatment.
- Airway protection: These patients are at high risk of hypoventilation and hypoxemia, often requiring intubation.
- Long-term outlook: Persistent apneustic breathing usually indicates poor prognosis, but in reversible cases (e.g., drug toxicity), aggressive supportive care can lead to recovery.
Apneustic Breathing Practice Questions
1. What is the apneustic center best described as?
The site in the lower pons is responsible for integrating afferent signals that regulate the duration of inspiration
2. What breathing pattern results when the vagus nerve is severed in conjunction with the apneustic center?
Apneustic breathing
3. What happens if only the apneustic center is severed, but the vagus nerve remains intact?
Apneustic breathing does not occur
4. How is apneustic breathing best described?
A breathing pattern marked by prolonged, deep inspiratory efforts followed by delayed or incomplete exhalation
5. What causes apneustic breathing, and why is this clinically important?
It is caused by the disruption of the inspiratory cutoff mechanism in the lower pons, indicating serious brainstem damage
6. What is the hallmark clinical presentation of apneustic breathing?
Deep gasping inspiration, a pause at full inspiration, and inadequate exhalation
7. Apneustic breathing is most commonly associated with damage to which area of the brain?
The lower pons
8. True or False: Apneustic breathing is typically seen in patients with damage to the medulla oblongata.
False — it is associated with pontine damage
9. What are some common causes of apneustic breathing?
Pontine stroke, trauma, brain herniation, hypoxic brain injury, and drug toxicity
10. Why is apneustic breathing considered a grave clinical sign?
It typically reflects severe neurological damage and is associated with a poor prognosis
11. What abnormal breathing pattern consists of short, brisk inhalations followed by a prolonged pause before exhalation?
Apneustic breathing
12. How does apneustic breathing impact the need for airway management?
It often necessitates intubation and mechanical ventilation due to hypoventilation and poor oxygenation
13. What is the role of a respiratory therapist in identifying apneustic breathing?
Early detection at the bedside and rapid communication with the healthcare team
14. Why might patients with apneustic breathing require mechanical ventilation?
Due to ineffective spontaneous breathing and risk of hypoxemia
15. What neurological insight can apneustic breathing provide to the clinical team?
It helps localize injury to the pons and assess severity of brainstem dysfunction
16. What does the apneustic center in the pons do under normal conditions?
It prolongs inspiration and regulates the rhythm of breathing
17. True or False: Apneustic breathing can be reversed in some cases, such as drug toxicity.
True
18. What is the difference between apnea and apneustic breathing?
Apnea is the complete cessation of breathing, while apneustic breathing is prolonged inspiration with delayed expiration
19. Which respiratory pattern is characterized by alternating periods of apnea and uniformly deep breaths?
Biot respirations
20. What is the function of the blood-brain barrier?
It allows selective entry of substances into the brain while keeping harmful agents out
21. What do central chemoreceptors respond to in the regulation of breathing?
Changes in the concentration of carbon dioxide and hydrogen ions in cerebrospinal fluid
22. What is Cheyne-Stokes respiration?
A breathing pattern with cyclic periods of increasing and decreasing depth, followed by apnea
23. In apneustic breathing, what part of the respiratory cycle is abnormally prolonged?
Inspiration
24. What type of brain injury most commonly leads to apneustic breathing?
Pontine lesions, particularly those affecting the lower pons
25. What ventilatory pattern may develop in patients with severe brainstem strokes?
Apneustic breathing
26. What important bedside sign can indicate pontine trauma or hypoxia?
Apneustic respiratory pattern
27. What term describes the absence of breathing?
Apnea
28. What should a respiratory therapist do if apneustic breathing is observed?
Immediately alert the medical team and prepare for airway management
29. What does the presence of apneustic breathing suggest about the patient’s neurological status?
Significant compromise or injury to the brainstem with a potentially poor prognosis
30. Which brain region balances respiratory signals between the cortex and the medulla and is disrupted in apneustic breathing?
The pons
31. What is the function of the dorsal respiratory group (DRG)?
It acts as the inspiratory center and functions during both quiet and forced breathing
32. What is the primary function of the Hering-Breuer reflex?
To protect the lungs from overinflation by terminating inspiration when lung volume is high
33. What do J receptors detect?
They sense changes in pulmonary capillary pressure
34. What is the role of the pneumotaxic center?
It contains neurons in the pons that shorten inspiratory time and increase respiratory rate
35. What does the vagovagal reflex promote?
It enhances gastrointestinal motility and secretions, including increased stomach activity
36. What is the function of the ventral respiratory group (VRG)?
It contains both inspiratory and expiratory neurons and is active only during forced breathing
37. To completely stop all ventilatory activity, where must the brainstem be severed?
Below the medulla
38. If the brainstem is cut above the pons, what happens to breathing?
Spontaneous respiratory effort continues
39. True or False: A clearly defined inspiratory and expiratory center exists in the brainstem.
False — there is no distinct separation
40. What type of neurons does the DRG primarily contain?
Inspiratory neurons
41. What type of neurons are found in the VRG?
Both inspiratory and expiratory neurons
42. What sensory pathway delivers signals to the DRG from the lungs, airways, and peripheral chemoreceptors?
The glossopharyngeal and vagus nerves
43. What does the VRG control, and where is it located?
It controls forced breathing and is located bilaterally in the medulla
44. Where does the VRG send most of its motor impulses?
To the accessory muscles of respiration, including abdominal muscles and internal intercostals
45. What are the two main theories for respiratory rhythm generation?
The pacemaker hypothesis and the network hypothesis
46. How does the inspiratory ramp signal behave?
It gradually increases in strength to create a smooth, controlled inspiratory effort
47. What is the primary role of the pons in respiration?
To regulate and fine-tune the rhythm of breathing
48. How is apneustic breathing characterized?
By long, gasping inspiratory efforts interrupted by infrequent expirations
49. What does the pneumotaxic center control?
It functions as the inspiratory “off switch,” regulating inspiratory time and tidal volume
50. What respiratory reflex is triggered when lung volumes become excessively high?
Hering-Breuer reflex
51. True or False: Tachycardia, coughing, and bronchospasm are common responses during endotracheal suctioning.
True
52. What type of receptors can cause rapid, shallow breathing in chronic lung disease?
J receptors and irritant receptors
53. What is the most common cause of hyperventilation in clinical settings?
Hypoxemia
54. True or False: Oxygen therapy cannot cause a sudden rise in PaCO₂ in patients with severe COPD and chronic hypercapnia.
False — it can lead to a dangerous rise in CO₂ levels
55. What blood gas component indirectly drives minute-to-minute breathing regulation?
Arterial carbon dioxide (PaCO₂)
56. True or False: Apneustic breathing is a sign of damage to the medulla.
False — it indicates damage to the pons, specifically the lower pons
57. What is the Hering-Breuer reflex?
A protective reflex that prevents over-inflation of the lungs by terminating inspiration when lung stretch receptors are activated
58. What is the deflation reflex?
A reflex triggered by sudden lung collapse, leading to strong inspiratory efforts and hyperpnea, often observed in conditions like pneumothorax
59. What is Head’s paradoxical reflex?
A reflex that may help maintain large tidal volumes during activities like exercise and deep sighs
60. In Head’s paradoxical reflex, what is the purpose of periodic sighs?
They help prevent alveolar collapse (atelectasis)
61. What do irritant receptors stimulate when activated?
Bronchospasm, coughing, sneezing, tachypnea, and narrowing of the glottis
62. True or False: Both the apneustic and pneumotaxic centers are located in the pons.
True
63. At what partial pressure of oxygen (PaO₂) does stimulation of breathing typically begin?
At approximately 60 mmHg
64. What are peripheral receptors, and where are they found?
They are located in muscles, tendons, joints, and pain receptors, and they stimulate hyperpnea during movement
65. What substances cannot cross the blood-brain barrier, and what can?
Hydrogen ions (H⁺) and bicarbonate (HCO₃⁻) cannot cross, but carbon dioxide (CO₂) can freely diffuse
66. What do peripheral chemoreceptors respond to primarily?
Decreased oxygen levels (low PaO₂) in arterial blood
67. What condition maximally stimulates peripheral chemoreceptors?
A combination of hypoxemia, hypercapnia, and acidosis
68. What is the ventilatory response to a sudden rise in PaCO₂?
An increase in minute ventilation (VE)
69. In which type of patients may oxygen therapy cause a sudden rise in PaCO₂, and why?
In patients with end-stage COPD and chronic hypercapnia, because it may suppress their hypoxic drive
70. During strenuous exercise, how much can CO₂ production and O₂ consumption increase?
Up to 20-fold
71. What are potential causes of central neurogenic hyperventilation?
Severe brain hypoxia, head trauma, or reduced cerebral perfusion
72. What conditions may cause central neurogenic hypoventilation?
Head trauma, cerebral hypoxia, or suppression by narcotics
73. True or False: An increase in CO₂ causes cerebral blood vessel dilation, while a decrease causes constriction.
True
74. What part of the brain is primarily responsible for the abnormal pattern seen in apneustic breathing?
The lower pons
75. What is the classic hallmark of apneustic breathing observed during physical assessment?
Prolonged inspiratory phase followed by a pause before expiration
76. What type of brain injury is most commonly associated with apneustic breathing?
Pontine stroke or trauma
77. True or False: Apneustic breathing typically results in hyperventilation.
False — it results in irregular, inadequate ventilation
78. What is the typical outcome or prognosis for patients exhibiting apneustic breathing?
Poor — it often indicates severe brainstem injury
79. In what type of neurological event might apneustic breathing be the first sign?
Brainstem stroke
80. What action should a respiratory therapist take upon observing apneustic breathing?
Notify the medical team immediately and prepare for possible airway management
81. What causes the prolonged inspiratory “hold” seen in apneustic breathing?
Loss of inhibitory signals from the pneumotaxic center
82. Which breathing control center, if damaged, can lead to apneustic breathing?
The apneustic center in the lower pons
83. What term describes deep gasping inhalations followed by delayed exhalation?
Apneustic breathing
84. What is a common ventilator strategy used in managing patients with apneustic breathing?
Assist-control mode to ensure adequate minute ventilation
85. What additional neurologic signs might accompany apneustic breathing?
Altered mental status, coma, or decerebrate posturing
86. Which reflex pathway is disrupted in apneustic breathing?
The inspiratory “off switch” involving the pneumotaxic center and vagus nerve
87. What type of injury does apneustic breathing usually suggest — reversible or irreversible?
Usually irreversible or indicative of severe damage
88. What diagnostic imaging is often warranted in patients with apneustic breathing?
CT or MRI of the brain to evaluate brainstem lesions
89. True or False: Patients with apneustic breathing typically maintain normal oxygenation without support.
False — they often require ventilatory assistance
90. What is one key difference between apneustic and Cheyne-Stokes respiration?
Apneustic breathing features prolonged inspiration; Cheyne-Stokes shows waxing and waning breathing patterns
91. What role does the vagus nerve play in apneustic breathing?
Vagal input helps inhibit prolonged inspiration; loss of this input may worsen apneusis
92. What surgical event could unintentionally cause apneustic breathing?
Brainstem damage during neurosurgery
93. What is one key respiratory care goal in treating apneustic breathing?
Maintain adequate oxygenation and ventilation
94. What is a potential differential diagnosis for apneustic breathing?
Brain herniation
95. What type of brain herniation may cause apneustic breathing?
Central or transtentorial herniation affecting the pons
96. Why is early recognition of apneustic breathing critical in neurocritical care?
It signals brainstem involvement requiring immediate intervention
97. What conditions can mimic apneustic breathing in appearance but are caused by different mechanisms?
Obstructive sleep apnea or certain seizure types
98. How can sedative drugs complicate recognition of apneustic breathing?
They may mask neurologic signs or mimic irregular respiratory patterns
99. What is one bedside clue that may distinguish apneustic breathing from normal deep breathing?
A prolonged inspiratory pause that appears involuntary
100. What brainstem control centers interact to prevent apneustic breathing under normal conditions?
The apneustic and pneumotaxic centers, along with vagal afferents
Final Thoughts
Apneustic breathing is a rare but critical abnormal respiratory pattern that signals pontine damage or brainstem dysfunction. For respiratory therapists, recognizing this pattern is more than an academic exercise—it is a clinical responsibility that can influence life-saving interventions.
By understanding its causes, clinical presentation, and implications, respiratory therapists can play a decisive role in patient outcomes, particularly in neurocritical care settings.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Mador MJ, Tobin MJ. Apneustic breathing. A characteristic feature of brainstem compression in achondroplasia? Chest. 1990.

