Expiratory reserve volume (ERV) is an essential lung volume that reflects the lungs’ ability to expel air beyond normal breathing. It represents the additional amount of air that can be forcefully exhaled after a normal, passive exhalation.
While ERV may receive less attention than tidal volume or vital capacity, it provides valuable insight into lung mechanics, chest wall function, and respiratory efficiency.
For respiratory therapists, understanding ERV is important for interpreting pulmonary function tests, assessing disease severity, and recognizing limitations in ventilation that can affect patient outcomes.
What Is Expiratory Reserve Volume?
Expiratory reserve volume (ERV) is the maximum amount of air that can be exhaled forcefully after the end of a normal, quiet exhalation. In simple terms, after breathing out normally, ERV represents how much additional air the lungs can still push out with effort.
ERV is one of the four primary lung volumes and reflects the functional reserve of the respiratory system during expiration. Unlike tidal volume, which occurs automatically during quiet breathing, ERV requires active effort and the use of expiratory muscles.
In healthy adults, ERV typically ranges from approximately 1,000 to 1,200 mL, though normal values vary based on age, sex, body size, posture, and lung mechanics.
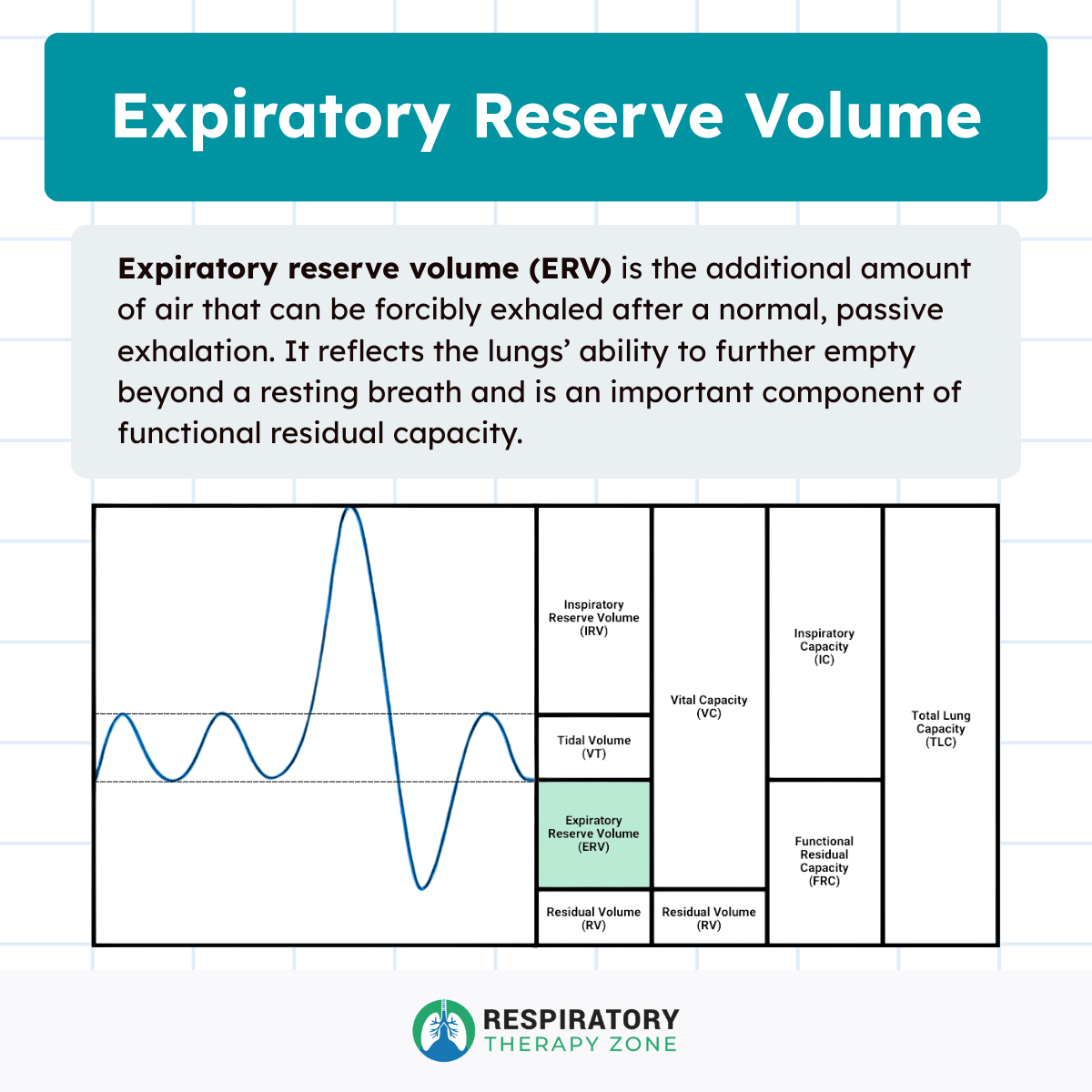
ERV and Lung Volumes and Capacities
Expiratory reserve volume contributes to several important lung capacities commonly assessed in respiratory care and pulmonary diagnostics.
ERV is a component of:
Functional Residual Capacity (FRC):
FRC = ERV + Residual Volume (RV)
Vital Capacity (VC):
VC = Inspiratory Reserve Volume (IRV) + Tidal Volume (VT) + ERV
Note: Because ERV plays a role in both resting lung volume and maximal exhalation capacity, changes in ERV can significantly influence overall respiratory function.
The Physiologic Role of Expiratory Reserve Volume
ERV reflects the lungs’ ability to reduce volume below resting levels. This capability is important for maintaining efficient ventilation, especially during activities that require greater respiratory effort.
Key physiologic roles of ERV include:
- Allowing deeper expiration during exercise
- Supporting effective cough and airway clearance
- Preventing air trapping during normal breathing
- Reflecting chest wall and abdominal muscle function
Note: When ERV is reduced, the lungs may remain more inflated at rest, limiting inspiratory capacity and increasing the work of breathing.
Clinical Importance of Expiratory Reserve Volume
ERV and Obstructive Lung Disease
In obstructive lung diseases such as COPD and asthma, ERV is often reduced. Airflow limitation prevents complete exhalation, leading to air trapping and increased residual volume.
As ERV decreases:
- Functional residual capacity increases
- The diaphragm flattens
- Inspiratory muscles become less efficient
- Dyspnea worsens, especially during exertion
Note: Monitoring ERV helps respiratory therapists identify hyperinflation and assess the severity of obstructive disease.
ERV and Restrictive Lung Disease
In restrictive conditions, including pulmonary fibrosis, scoliosis, obesity, and chest wall disorders, ERV is commonly reduced due to limited lung expansion or restricted chest wall movement.
In obesity, excess abdominal mass limits downward movement of the diaphragm, significantly reducing ERV. This reduction contributes to decreased lung volumes, impaired ventilation, and increased risk of atelectasis.
Note: Understanding ERV changes helps clinicians distinguish between restrictive and obstructive patterns during pulmonary function testing.
ERV and Functional Residual Capacity
Because ERV is a major component of functional residual capacity, changes in ERV directly affect resting lung volume. A reduced ERV lowers FRC, increasing the likelihood of alveolar collapse and impaired oxygenation.
This is especially relevant in:
- Supine positioning
- General anesthesia
- Critical illness
- Postoperative patients
Note: Respiratory therapists use this knowledge to guide positioning, lung expansion therapy, and ventilatory support.
Measuring Expiratory Reserve Volume
ERV is measured using spirometry during pulmonary function testing. The patient is instructed to breathe normally and then exhale as forcefully and completely as possible.
Accurate measurement of ERV depends on:
- Proper patient instruction
- Maximal expiratory effort
- Good seal and technique
Because ERV requires active exhalation, pain, fatigue, or poor cooperation can affect test results. Unlike residual volume, ERV can be measured directly, making it an important and accessible indicator of expiratory function.
Factors That Affect Expiratory Reserve Volume
Several factors influence ERV in both healthy individuals and patients with respiratory disease:
- Body position: ERV decreases in the supine position
- Obesity: Excess abdominal pressure reduces ERV
- Age: ERV may decrease with aging due to reduced chest wall compliance
- Pregnancy: Elevated diaphragm limits expiratory reserve
- Pain: Limits forceful exhalation
- Airway obstruction: Prevents complete expiration
- Chest wall restriction: Reduces expiratory movement
Note: Recognizing these influences allows respiratory therapists to interpret ERV values in proper clinical context.
ERV and Mechanical Ventilation
Although ERV is not a ventilator setting, it has important implications for mechanically ventilated patients. Reduced ERV contributes to increased resting lung volume and hyperinflation, especially in obstructive lung disease.
Low ERV may indicate:
- Increased air trapping
- Elevated intrinsic PEEP
- Reduced inspiratory capacity
- Increased risk of ventilator dyssynchrony
Note: Respiratory therapists must consider ERV-related physiology when adjusting ventilator settings such as respiratory rate, inspiratory time, and PEEP to optimize ventilation and minimize lung injury.
Why Expiratory Reserve Volume Matters to Respiratory Therapists
Expiratory reserve volume provides valuable insight into a patient’s ability to exhale effectively and maintain efficient ventilation. For respiratory therapists, ERV helps with:
- Interpreting pulmonary function tests
- Identifying air trapping and hyperinflation
- Assessing restrictive versus obstructive patterns
- Understanding changes in functional residual capacity
- Guiding lung expansion and airway clearance strategies
Note: Although ERV is often discussed alongside other lung volumes, its clinical significance should not be underestimated.
Access our quiz with sample TMC practice questions and detailed explanations to help you master pulmonary function testing (PFT).
Expiratory Reserve Volume Practice Questions
1. What is expiratory reserve volume (ERV)?
Expiratory reserve volume is the maximum amount of air that can be forcefully exhaled after a normal, quiet exhalation.
2. How does ERV differ from tidal volume (VT)?
Tidal volume represents normal passive breathing, whereas ERV requires active expiratory effort beyond a normal exhalation.
3. Is expiratory reserve volume classified as a lung volume or a lung capacity?
Expiratory reserve volume is classified as a lung volume.
4. Which muscles are primarily involved during expiration of ERV?
The abdominal muscles and internal intercostals actively contract to expel ERV.
5. What does ERV reflect about respiratory mechanics?
ERV reflects chest wall mobility, expiratory muscle strength, and lung elastic recoil.
6. What is the typical range of ERV in a healthy adult?
ERV is usually about 1,000 to 1,200 mL, depending on age, sex, body size, and posture.
7. Which lung capacity is calculated using ERV and residual volume?
Functional residual capacity (FRC)
8. What is the equation for functional residual capacity?
FRC equals expiratory reserve volume plus residual volume (FRC = ERV + RV).
9. Which lung capacity includes ERV, tidal volume, and inspiratory reserve volume?
Vital capacity (VC)
10. Why is ERV considered an active lung volume?
Because it requires muscular effort to exhale air beyond a normal passive breath.
11. How does ERV contribute to effective coughing?
It allows greater expiratory force, helping generate high airflow to clear secretions.
12. What happens to ERV during exercise?
ERV decreases as expiratory reserve is recruited to increase tidal volume.
13. How is ERV typically affected in obstructive lung disease?
ERV is reduced due to airflow limitation and air trapping.
14. Why does air trapping reduce ERV in obstructive disease?
Incomplete exhalation increases residual volume, leaving less air available for ERV.
15. How does a reduced ERV affect the diaphragm?
The diaphragm becomes flattened and less mechanically efficient.
16. What happens to functional residual capacity when ERV decreases in obstructive disease?
Functional residual capacity increases due to rising residual volume.
17. How is ERV affected in restrictive lung disease?
ERV is reduced due to limited lung expansion or restricted chest wall movement.
18. Why does obesity significantly reduce ERV?
Excess abdominal mass limits diaphragmatic movement during expiration.
19. How does reduced ERV increase the risk of atelectasis?
Lower expiratory reserve reduces resting lung volume, promoting alveolar collapse.
20. Why is ERV especially important in postoperative patients?
Pain, anesthesia, and supine positioning can reduce ERV and impair ventilation.
21. How does body position influence expiratory reserve volume?
ERV is typically greater in the upright position than in supine.
22. Why does supine positioning reduce ERV?
Abdominal contents push against the diaphragm, limiting expiratory excursion.
23. How does ERV help differentiate obstructive from restrictive patterns?
Both may reduce ERV, but obstructive disease increases FRC while restrictive disease lowers it.
24. Can ERV be measured directly with spirometry?
Yes, ERV can be measured directly using spirometry.
25. Why is expiratory reserve volume clinically important for respiratory therapists?
It helps assess ventilation efficiency, disease severity, and risk for hyperinflation or atelectasis.
26. How is expiratory reserve volume (ERV) measured during pulmonary function testing?
ERV is measured with spirometry by having the patient exhale forcefully and completely after a normal breath out.
27. What breathing maneuver is required to obtain an accurate ERV measurement?
A normal passive exhalation followed by a maximal, forceful expiration.
28. Why does accurate measurement of ERV depend on patient effort?
Because ERV requires active exhalation, inadequate effort can underestimate the true value.
29. Why is proper patient instruction important when measuring ERV?
Clear instructions ensure maximal effort and improve test accuracy and reproducibility.
30. How does poor mouthpiece seal affect ERV measurements?
Air leaks reduce recorded volume, falsely lowering ERV values.
31. Why can pain interfere with expiratory reserve volume testing?
Pain limits the ability to exhale forcefully and completely.
32. How does fatigue affect ERV measurements?
Fatigue reduces expiratory muscle strength, decreasing measured ERV.
33. Unlike residual volume, why can ERV be measured directly?
Because ERV consists of air that can be exhaled and measured at the mouth.
34. How does body position influence expiratory reserve volume?
ERV decreases in the supine position compared to upright.
35. Why does supine positioning reduce ERV?
Abdominal contents shift upward and limit diaphragmatic movement.
36. How does obesity affect expiratory reserve volume?
Excess abdominal pressure restricts diaphragmatic excursion, reducing ERV.
37. How does aging typically affect ERV?
ERV often decreases due to reduced chest wall compliance and muscle strength.
38. Why does pregnancy reduce expiratory reserve volume?
The elevated diaphragm limits the volume available for forceful exhalation.
39. How does airway obstruction affect ERV?
Airflow limitation prevents complete exhalation, reducing ERV.
40. How does chest wall restriction influence expiratory reserve volume?
Restricted chest wall movement limits the ability to expel air forcefully.
41. Why is understanding factors that affect ERV important for interpretation?
Because ERV varies with physiologic and external conditions independent of disease.
42. Is expiratory reserve volume a ventilator setting?
No, ERV is not directly set on mechanical ventilators.
43. How does reduced ERV contribute to hyperinflation?
Less expiratory reserve leads to higher resting lung volumes.
44. What ventilator-related issue is associated with low ERV in obstructive disease?
Elevated intrinsic PEEP due to air trapping.
45. How does low ERV affect inspiratory capacity?
Reduced ERV increases resting lung volume, limiting inspiratory capacity.
46. Why may low ERV increase the risk of ventilator dyssynchrony?
Patients struggle to fully exhale, causing mismatched timing with the ventilator.
47. Which ventilator settings are influenced by ERV-related physiology?
Respiratory rate, inspiratory time, and PEEP.
48. Why is ERV important for identifying air trapping?
A reduced ERV suggests incomplete expiration and increased residual volume.
49. How does ERV help differentiate restrictive and obstructive lung patterns?
Both reduce ERV, but obstructive disease increases FRC while restrictive disease lowers it.
50. Why is expiratory reserve volume clinically important for respiratory therapists?
It helps assess expiratory function, lung volumes, and risks for hyperinflation or atelectasis.
51. How does expiratory reserve volume change during rapid, shallow breathing?
ERV decreases as less air is exhaled beyond normal tidal breathing.
52. What does a reduced ERV indicate about expiratory muscle performance?
It may suggest weakness or limited effectiveness of the abdominal and internal intercostal muscles.
53. How does ERV influence airway clearance techniques?
Adequate ERV supports stronger cough and more effective secretion removal.
54. Why is ERV important in patients with chronic cough?
Reduced ERV limits expiratory force, decreasing cough effectiveness.
55. How does ERV change during dynamic hyperinflation?
ERV progressively decreases as end-expiratory lung volume rises.
56. What does a low ERV with a normal residual volume suggest?
Restricted expiratory movement without significant air trapping.
57. How does ERV affect inspiratory capacity at rest?
Lower ERV reduces inspiratory capacity by increasing resting lung volume.
58. Why is ERV useful in evaluating patients with abdominal surgery?
Postoperative pain and splinting often reduce ERV, increasing pulmonary risk.
59. How does ERV relate to the work of breathing?
Reduced ERV increases the effort required to maintain effective ventilation.
60. What effect does prolonged bed rest have on ERV?
ERV may decrease due to reduced chest wall mobility and muscle deconditioning.
61. How does ERV respond to effective bronchodilator therapy?
ERV may increase as airflow improves and air trapping decreases.
62. What does an increase in ERV after treatment indicate?
Improved expiratory airflow and lung mechanics.
63. How does ERV differ between males and females of similar age?
Males generally have higher ERV due to larger lung volumes and chest dimensions.
64. How does ERV change in patients with ascites?
Increased abdominal pressure reduces ERV by limiting diaphragmatic motion.
65. Why is ERV important during forced expiratory maneuvers?
It contributes to maximal airflow generation and complete lung emptying.
66. How does ERV relate to expiratory flow limitation?
Lower ERV often accompanies flow limitation due to incomplete exhalation.
67. Why is ERV useful in evaluating obesity-related respiratory impairment?
Obesity disproportionately reduces ERV, even when other volumes are preserved.
68. How does ERV change during general anesthesia?
ERV decreases due to muscle relaxation and supine positioning.
69. Why is ERV important for maintaining alveolar ventilation?
Adequate ERV helps prevent excessive air trapping and uneven ventilation.
70. How does ERV affect breathing efficiency during exertion?
Reduced ERV limits the ability to fully exhale, impairing ventilatory efficiency.
71. What does a declining ERV during monitoring suggest?
Worsening expiratory mechanics or increasing air trapping.
72. How does ERV contribute to lung volume reduction during expiration?
It represents the active portion of exhalation beyond passive recoil.
73. Why is ERV relevant in patients with neuromuscular disease?
Weak expiratory muscles reduce ERV, impairing ventilation and cough.
74. How does ERV change with improved posture and positioning?
ERV often increases with upright positioning and optimized body alignment.
75. Why should ERV be evaluated alongside residual volume?
Together they provide insight into air trapping and resting lung volume.
76. How does ERV affect oxygenation indirectly?
Reduced ERV can promote alveolar collapse and impair gas exchange.
77. What does a normal ERV in the presence of dyspnea suggest?
Dyspnea may be caused by non-expiratory factors such as cardiac disease.
78. How does ERV relate to breathing pattern selection?
Low ERV favors rapid, shallow breathing rather than deep expiration.
79. Why is ERV important in evaluating ventilatory reserve?
It reflects how much additional expiration can occur during increased demand.
80. Why should expiratory reserve volume not be overlooked in respiratory assessment?
Because it provides key insight into expiratory mechanics, lung volumes, and ventilation efficiency.
81. How does expiratory reserve volume change during forced breathing compared to quiet breathing?
ERV is actively recruited during forced breathing, decreasing as expiratory effort increases.
82. Why is ERV important for maintaining effective end-expiratory lung volume?
Adequate ERV helps prevent excessive lung inflation and uneven ventilation.
83. How does ERV influence the effectiveness of incentive spirometry?
Lower ERV limits full expiration, reducing the ability to take deep subsequent breaths.
84. What happens to ERV in patients with severe abdominal distension?
ERV decreases due to restricted diaphragmatic movement.
85. How does ERV relate to the ability to clear atelectasis?
Reduced ERV limits expiratory force, impairing lung re-expansion strategies.
86. Why is ERV useful in evaluating chest wall compliance?
Lower ERV suggests restricted chest wall movement during expiration.
87. How does ERV change with progressive hyperinflation?
ERV steadily declines as residual volume increases.
88. Why may ERV be reduced even when spirometry values appear normal?
External factors such as posture, obesity, or pain can limit expiration.
89. How does ERV contribute to efficient ventilation at rest?
It allows full expiration, maintaining optimal lung volume for gas exchange.
90. What does a low ERV suggest about abdominal muscle recruitment?
It may indicate reduced or ineffective abdominal muscle activation.
91. How does ERV affect inspiratory timing on mechanical ventilation?
Reduced ERV can shorten expiratory time, increasing air trapping.
92. Why is ERV important when assessing ventilator-triggering effort?
Incomplete expiration can increase intrinsic PEEP and make triggering more difficult.
93. How does ERV influence respiratory system compliance?
Lower ERV shifts breathing to higher lung volumes where compliance is reduced.
94. Why is ERV relevant in evaluating breathing during sleep-disordered breathing?
Reduced ERV promotes airway closure and ventilation instability.
95. How does ERV change following effective airway clearance therapy?
ERV may increase as airway patency improves.
96. What does an improving ERV trend indicate during recovery?
Restoration of expiratory function and reduced air trapping.
97. Why is ERV important in patients with rib fractures?
Pain and limited chest wall motion reduce ERV and ventilation effectiveness.
98. How does ERV relate to end-expiratory pressure in the lungs?
Lower ERV increases resting lung volume and intrinsic pressure.
99. Why should ERV be monitored in critically ill patients?
It reflects changes in lung mechanics and risk for hyperinflation or collapse.
100. How does expiratory reserve volume support overall respiratory efficiency?
By allowing complete expiration, it optimizes lung volumes for the next breath.
Final Thoughts
Expiratory reserve volume (ERV) is a critical component of respiratory physiology that reflects the lungs’ ability to expel air beyond normal breathing. Changes in ERV influence resting lung volume, inspiratory capacity, and overall ventilatory efficiency.
For respiratory therapists, understanding ERV enhances the interpretation of pulmonary function tests, supports accurate assessment of lung disease, and informs clinical decision-making across a wide range of care settings.
By recognizing how expiratory reserve volume affects breathing mechanics, respiratory professionals can better anticipate patient needs and deliver more effective, patient-centered respiratory care.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Ponce MC, Sankari A, Sharma S. Pulmonary Function Tests. [Updated 2023 Aug 28]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025.


