The FEV1/FVC ratio is one of the most important values obtained during spirometry. It helps clinicians determine whether airflow obstruction is present and plays a central role in the interpretation of pulmonary function tests.
While FEV1 and FVC each provide useful information individually, their relationship offers deeper insight into the mechanics of ventilation.
For respiratory therapists, understanding the FEV1/FVC ratio is essential for identifying obstructive patterns, guiding treatment decisions, and ensuring accurate interpretation of lung function data in both acute and chronic care settings.
What is the FEV1/FVC Ratio?
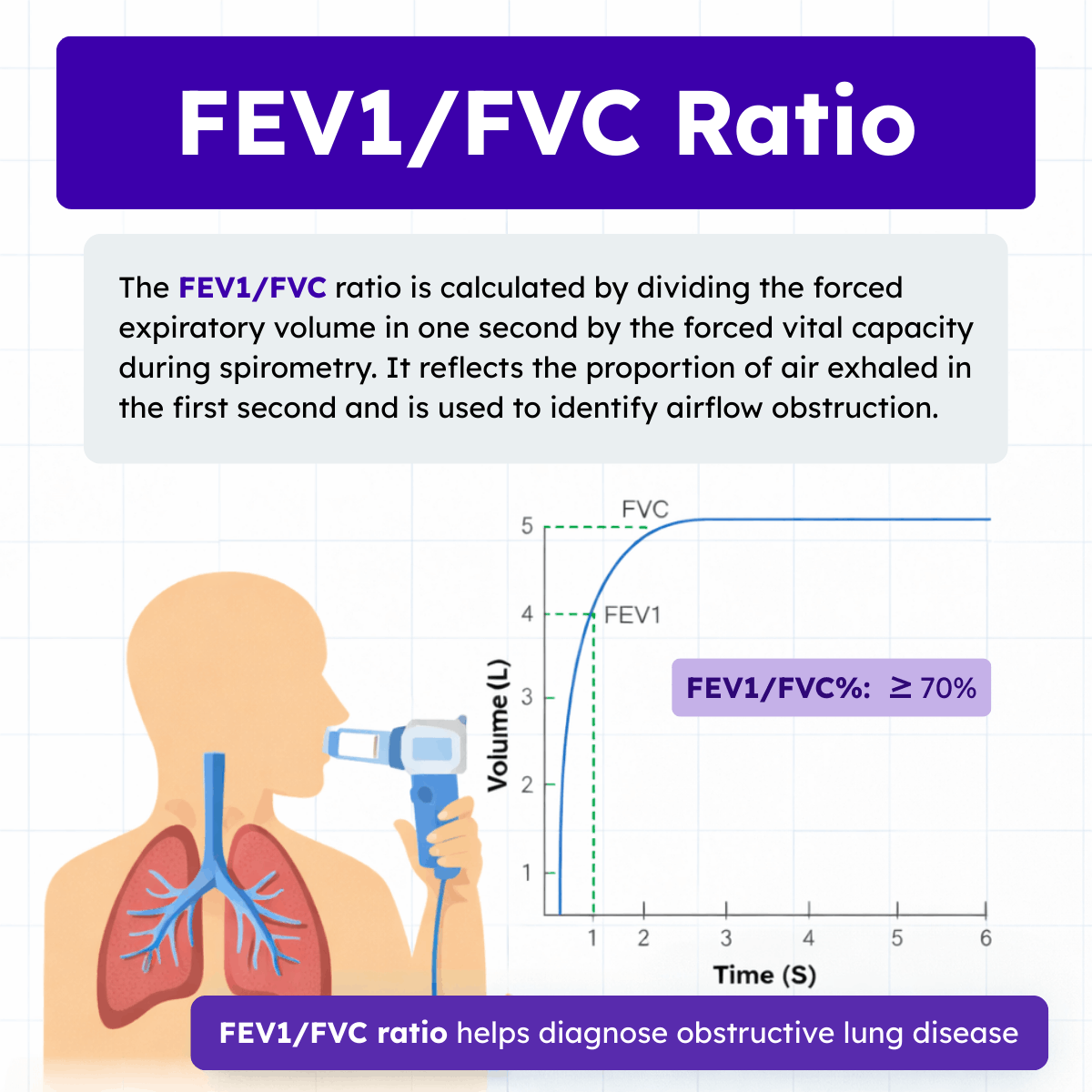
The FEV1/FVC ratio is calculated by dividing the forced expiratory volume in one second by the forced vital capacity. FEV1 represents the volume of air exhaled in the first second of a forced maneuver, while FVC represents the total volume exhaled during the entire forced expiration.
This ratio reflects the proportion of the total exhaled volume that leaves the lungs during the first second. In healthy individuals, a large percentage of the FVC is exhaled within that initial second. As a result, the ratio is relatively high.
The value is typically reported as a decimal, such as 0.78 rather than 78 percent. Interpretation should focus on comparison to the lower limit of normal rather than relying solely on a fixed cutoff.
How the FEV1/FVC Ratio is Measured
The FEV1/FVC ratio is obtained during spirometry. The patient inhales fully to total lung capacity and then exhales as forcefully and completely as possible into the spirometer.
To ensure accuracy, at least three acceptable FVC maneuvers must be performed. The largest acceptable FEV1 and the largest acceptable vital capacity are used in the calculation, even if they come from different trials.
Because spirometry is effort dependent, proper coaching and technique are essential. An inadequate inhalation, hesitation at the start of exhalation, or premature termination can distort both FEV1 and FVC, leading to inaccurate ratios.
Note: Respiratory therapists are responsible for ensuring that maneuvers meet quality standards and that results are reproducible.
Normal Values and Interpretation
In healthy adults, the FEV1/FVC ratio generally ranges from approximately 0.75 to 0.85, depending on age. The ratio naturally declines with aging due to changes in lung elasticity and airway structure.
Modern interpretation emphasizes comparing the measured ratio to the lower limit of normal derived from population-based reference equations. This approach reduces the risk of misclassification.
Historically, a fixed cutoff value of 0.70 was used to diagnose obstruction. However, this method may underdiagnose airflow limitation in younger individuals and overdiagnose it in older adults. For this reason, reliance on the lower limit of normal is recommended.
Note: A ratio below the lower limit of normal indicates airflow obstruction.
FEV1/FVC Ratio in Obstructive Lung Disease
The FEV1/FVC ratio is most useful for identifying obstructive lung disease. In obstructive conditions, airway narrowing increases resistance to airflow. This resistance primarily affects the speed of exhalation.
Because FEV1 reflects the volume exhaled in the first second, it decreases significantly when airflow is limited. FVC may also decrease, especially in more advanced disease, but the reduction in FEV1 is typically greater. As a result, the ratio declines.
Common conditions associated with a reduced FEV1/FVC ratio include asthma and chronic obstructive pulmonary disease. In asthma, airway narrowing may be reversible with bronchodilator therapy. In chronic obstructive pulmonary disease, airflow limitation is often progressive and less reversible.
Note: The degree of reduction in the ratio helps confirm the presence of obstruction, while the severity of airflow limitation is further assessed by examining FEV1.
FEV1/FVC Ratio in Restrictive Lung Disease
In restrictive lung disease, total lung volumes are reduced due to limited lung expansion. Conditions such as interstitial lung disease, chest wall disorders, or neuromuscular weakness can lead to restriction.
In these cases, both FEV1 and FVC are reduced because the total volume of air that can be inhaled and exhaled is smaller than normal. However, the proportion of air exhaled in the first second is usually preserved. Therefore, the FEV1/FVC ratio remains normal or may even be slightly elevated.
A normal ratio with reduced FEV1 and FVC may suggest restrictive physiology, but spirometry alone cannot confirm restriction. Measurement of total lung capacity is required for definitive diagnosis.
Note: This distinction is critical in clinical interpretation and reinforces the importance of evaluating the full pulmonary function test.
The Concept of Pseudorestriction
An important consideration in interpretation is pseudorestriction. In some patients with obstructive lung disease, air trapping prevents complete exhalation during the forced maneuver. As a result, the measured FVC may appear reduced.
If FEV1 and FVC are both reduced and the ratio appears normal, the pattern may resemble restriction. However, the underlying problem may actually be obstructive air trapping rather than true restriction.
Comparing the forced vital capacity to a slow vital capacity can help clarify this situation. A significantly larger slow vital capacity suggests obstruction with air trapping.
Note: Respiratory therapists must recognize this pattern to avoid misinterpretation.
Clinical Applications in Respiratory Care
The FEV1/FVC ratio is widely used in respiratory care because it provides a clear indicator of airflow limitation. Its value extends across outpatient clinics, pulmonary laboratories, hospitals, and occupational health settings.
By comparing the volume exhaled in the first second to the total forced vital capacity, clinicians can quickly determine whether obstruction is present and whether additional evaluation is needed.
Diagnostic Evaluation
One of the primary uses of the FEV1/FVC ratio is in the diagnosis of obstructive lung disease. When the ratio falls below the lower limit of normal, airflow obstruction is confirmed. This finding prompts further assessment of severity, often through evaluation of the absolute FEV1 value.
Identifying obstruction early allows for appropriate initiation of bronchodilator therapy, anti-inflammatory treatment, or referral for additional testing.
Bronchodilator Testing
The ratio also plays an important role during bronchodilator responsiveness testing. Spirometry is performed before and after administration of a bronchodilator medication. An improvement in FEV1 may be observed, and in some cases the ratio increases as well. A meaningful change supports the presence of reversible airflow limitation, which is characteristic of asthma.
Limited or absent change may suggest fixed obstruction, as seen in many patients with chronic obstructive pulmonary disease. These results guide medication selection and long-term management strategies.
Disease Monitoring
For patients with chronic respiratory disorders, serial spirometry allows clinicians to monitor disease progression. Tracking the FEV1/FVC ratio over time helps identify stability or decline in airflow.
A progressively decreasing ratio may indicate worsening obstruction, while a stable value may reflect adequate disease control. Evaluating trends rather than single measurements improves clinical decision making.
Preoperative Assessment
Before major surgery, particularly thoracic or upper abdominal procedures, spirometry is often used to estimate pulmonary risk. A reduced ratio that indicates obstruction may signal increased susceptibility to postoperative pulmonary complications and influence perioperative planning.
Occupational Screening
In occupational health programs, periodic spirometry with calculation of the FEV1/FVC ratio helps detect early airflow limitation in workers exposed to dust, fumes, or chemical irritants. Early recognition allows for intervention, exposure modification, and prevention of long-term lung damage.
Role of Respiratory Therapists
Respiratory therapists play a central role in obtaining and interpreting spirometry data. Accurate measurement of FEV1 and FVC is necessary to calculate a reliable ratio. RTs must ensure proper patient positioning, instruction, and coaching. They are responsible for verifying acceptability and reproducibility of maneuvers according to established standards.
Beyond test performance, therapists often participate in interpretation and patient education. Explaining what the ratio means and how it relates to symptoms can improve patient understanding and adherence to treatment.
In acute care settings, interpretation of spirometry may influence medication adjustments and discharge planning. In outpatient settings, serial measurements help guide long-term management.
Note: Competence in evaluating the FEV1/FVC ratio strengthens clinical decision making and supports high-quality respiratory care.
Limitations of the FEV1/FVC Ratio
Although highly useful, the FEV1/FVC ratio has limitations. It does not measure lung volumes directly and cannot independently diagnose restrictive disease. It is also influenced by patient effort and technique. Poor effort may falsely lower FEV1 and distort the ratio.
Additionally, interpretation must consider age-related changes. A ratio that appears low compared with a fixed cutoff may still fall within the normal range for an older adult when compared to appropriate reference values.
Note: The FEV1/FVC ratio should always be interpreted in conjunction with the full pulmonary function test and the clinical context.
FEV1/FVC Ratio Practice Questions
1. What is the FEV1/FVC ratio?
It is the proportion of the forced vital capacity that is exhaled during the first second of a forced expiratory maneuver.
2. How is the FEV1/FVC ratio calculated?
By dividing the forced expiratory volume in one second (FEV1) by the forced vital capacity (FVC).
3. What does the FEV1/FVC ratio physiologically represent?
It reflects how quickly air can be expelled from the lungs relative to the total exhaled volume.
4. Why is the FEV1/FVC ratio typically high in healthy individuals?
Because most of the forced vital capacity is exhaled within the first second of expiration.
5. How is the FEV1/FVC ratio commonly reported?
As a decimal value, such as 0.78, rather than a percentage.
6. Why should the FEV1/FVC ratio be compared to the lower limit of normal (LLN)?
Because age-related changes in lung function make fixed cutoff values less accurate.
7. What spirometry maneuver is required to obtain the FEV1/FVC ratio?
A maximal inhalation to total lung capacity followed by a rapid and forceful full exhalation.
8. How many acceptable spirometry maneuvers are required for accurate interpretation?
At least three acceptable and reproducible forced vital capacity maneuvers.
9. Which values are used to calculate the FEV1/FVC ratio?
The largest acceptable FEV1 and the largest acceptable FVC, even if obtained from different trials.
10. Why is spirometry considered effort dependent?
Because inadequate inhalation, delayed exhalation, or premature termination can alter results.
11. What is the typical normal range of the FEV1/FVC ratio in healthy adults?
Approximately 0.75 to 0.85, depending on age.
12. How does aging affect the FEV1/FVC ratio?
The ratio gradually declines due to reduced lung elasticity and airway changes.
13. What does a ratio below the lower limit of normal indicate?
Airflow obstruction
14. Why is the fixed 0.70 cutoff no longer preferred for diagnosing obstruction?
Because it may overdiagnose obstruction in older adults and underdiagnose it in younger individuals.
15. How does obstructive lung disease affect the FEV1/FVC ratio?
FEV1 decreases more than FVC, causing the ratio to decline.
16. Why does FEV1 decrease more significantly in obstructive disease?
Because airway narrowing primarily affects the speed of exhalation.
17. Name two common conditions associated with a reduced FEV1/FVC ratio.
Asthma and chronic obstructive pulmonary disease (COPD).
18. How does bronchodilator responsiveness affect interpretation of a reduced ratio in asthma?
Improvement after bronchodilator therapy suggests reversible airway obstruction.
19. In COPD, how does airflow limitation typically respond to bronchodilators?
It is often only partially reversible or not reversible.
20. How does restrictive lung disease affect the FEV1/FVC ratio?
Both FEV1 and FVC decrease proportionally, so the ratio remains normal or slightly elevated.
21. Why can spirometry alone not confirm restrictive lung disease?
Because total lung capacity must be measured to confirm true restriction.
22. What pattern suggests possible restrictive physiology on spirometry?
Reduced FEV1 and reduced FVC with a normal or elevated FEV1/FVC ratio.
23. What is pseudorestriction?
A spirometric pattern that mimics restriction due to air trapping in obstructive disease.
24. How does air trapping contribute to pseudorestriction?
Incomplete exhalation reduces measured FVC, making lung volumes appear falsely low.
25. How can slow vital capacity (SVC) help differentiate pseudorestriction from true restriction?
A significantly larger SVC compared to FVC suggests obstruction with air trapping.
26. Why is recognition of pseudorestriction important?
To avoid misdiagnosing obstructive disease as restrictive disease.
27. What role do respiratory therapists play in ensuring accurate FEV1/FVC interpretation?
They ensure proper technique, reproducibility, and adherence to quality standards.
28. Why must exhalation begin abruptly during spirometry?
To accurately measure airflow during the first second.
29. What effect does early termination of exhalation have on the ratio?
It can falsely reduce FVC and distort the calculated ratio.
30. Why should the FEV1/FVC ratio always be interpreted with other spirometric values?
Because accurate diagnosis requires evaluation of the complete pulmonary function test.
31. Why is the FEV1/FVC ratio widely used in respiratory care?
Because it provides a clear and efficient indicator of airflow limitation across a variety of clinical settings.
32. In which clinical environments is the FEV1/FVC ratio commonly utilized?
Outpatient clinics, pulmonary function laboratories, hospitals, and occupational health programs.
33. What does comparing FEV1 to FVC help clinicians determine?
Whether airflow obstruction is present and if further evaluation is needed.
34. What does a FEV1/FVC ratio below the lower limit of normal confirm?
The presence of airflow obstruction.
35. After identifying a reduced FEV1/FVC ratio, what value is typically assessed next to determine severity?
The absolute FEV1 value.
36. Why is early identification of airflow obstruction important?
It allows timely initiation of bronchodilators, anti-inflammatory therapy, or referral for additional testing.
37. How is the FEV1/FVC ratio used during bronchodilator responsiveness testing?
Spirometry is performed before and after bronchodilator administration to assess changes in airflow.
38. What does a significant improvement in FEV1 after bronchodilator therapy suggest?
Reversible airflow obstruction, commonly seen in asthma.
39. How does the FEV1/FVC ratio typically respond in patients with fixed obstruction such as COPD?
It may show minimal or no significant improvement after bronchodilator therapy.
40. Why are serial FEV1/FVC measurements useful in chronic respiratory disease?
They help monitor disease stability or progression over time.
41. What does a progressively decreasing FEV1/FVC ratio over time suggest?
Worsening airflow obstruction.
42. Why is evaluating trends in the FEV1/FVC ratio more informative than relying on a single value?
Because trends provide a clearer picture of disease trajectory and treatment effectiveness.
43. How is the FEV1/FVC ratio used in preoperative assessment?
To estimate pulmonary reserve and assess the risk of postoperative pulmonary complications.
44. Why might a reduced FEV1/FVC ratio influence perioperative planning?
Because airflow obstruction increases the risk of postoperative respiratory complications.
45. How is the FEV1/FVC ratio applied in occupational health screening?
It helps detect early airflow limitation in workers exposed to respiratory irritants.
46. What is the benefit of detecting airflow limitation early in occupational settings?
It allows for intervention, exposure modification, and prevention of long-term lung damage.
47. What role do respiratory therapists play in obtaining an accurate FEV1/FVC ratio?
They ensure proper patient instruction, technique, and reproducibility of spirometry maneuvers.
48. Why is reproducibility important in spirometry testing?
Because inconsistent efforts can lead to inaccurate FEV1, FVC, and ratio calculations.
49. How does patient effort affect the FEV1/FVC ratio?
Poor effort can falsely lower FEV1 and distort the calculated ratio.
50. Why is patient education important when discussing FEV1/FVC results?
Understanding the meaning of the ratio can improve adherence to treatment plans.
51. In acute care settings, how can FEV1/FVC interpretation influence management?
It may guide medication adjustments and discharge planning.
52. In outpatient settings, how does serial spirometry support long-term care?
It helps evaluate response to therapy and disease control over time.
53. What is a key limitation of the FEV1/FVC ratio regarding lung volumes?
It does not directly measure total lung capacity or residual volume.
54. Can the FEV1/FVC ratio alone confirm restrictive lung disease?
No, measurement of total lung capacity is required for confirmation.
55. Why must age-related changes be considered when interpreting the ratio?
Because the ratio naturally declines with age.
56. What problem may occur when using a fixed cutoff such as 0.70 in older adults?
It may falsely classify normal aging as obstruction.
57. Why should the FEV1/FVC ratio always be interpreted in clinical context?
Because accurate diagnosis requires correlation with symptoms, history, and complete pulmonary function testing.
58. What aspect of spirometry quality control directly affects the ratio?
Proper inhalation to total lung capacity and forceful, sustained exhalation.
59. How can hesitation at the start of exhalation affect results?
It can falsely reduce FEV1 and lower the calculated ratio.
60. Why is competence in interpreting the FEV1/FVC ratio important for respiratory therapists?
Because it strengthens clinical decision making and supports high-quality patient care.
61. What does the FEV1/FVC ratio assess in pulmonary function testing?
It assesses airflow limitation by comparing the volume exhaled in the first second to the total forced vital capacity.
62. What does FEV1 represent in the FEV1/FVC ratio?
The volume of air forcibly exhaled during the first second of a forced expiratory maneuver.
63. What does FVC represent in spirometry?
The total volume of air forcibly exhaled after a full inhalation to total lung capacity.
64. What is another name for the FEV1/FVC ratio?
The Tiffeneau-Pinelli index.
65. In a normal spirometry pattern, how do FEV1/FVC and FVC appear?
Both the FEV1/FVC ratio and FVC are within normal limits.
66. What spirometry pattern is characterized by a decreased FVC with a normal FEV1/FVC ratio?
A restrictive pattern.
67. What spirometry pattern is characterized by a decreased FEV1/FVC ratio?
An obstructive defect.
68. What defines a mixed obstructive and restrictive pattern?
Both a reduced FEV1/FVC ratio and a reduced FVC.
69. Historically, what fixed cutoff value has been used to identify obstruction?
An FEV1/FVC ratio less than 0.70 (70%).
70. Why should interpretation not rely solely on a fixed 0.70 cutoff?
Because the ratio naturally declines with age and should be compared to the lower limit of normal.
71. What is maximal voluntary ventilation (MVV)?
The largest volume of gas a person can voluntarily breathe in and out in one minute.
72. How is MVV typically measured in practice?
The patient breathes rapidly and deeply for 12–15 seconds, and the result is extrapolated to one minute.
73. How is MVV typically affected in obstructive lung disease?
It is usually decreased due to airflow limitation.
74. How is MVV affected in restrictive lung disease?
It may be normal or decreased, depending on severity.
75. What is a typical normal MVV value for a healthy adult male?
Approximately 140–180 L/min, depending on age and body size.
76. What is the purpose of pre- and post-bronchodilator testing?
To determine the reversibility of airflow obstruction.
77. What constitutes a significant bronchodilator response?
An increase in FEV1 or FVC of at least 12% and at least 200 mL from baseline.
78. A significant bronchodilator response is most commonly associated with which condition?
Asthma
79. What does minimal or no bronchodilator response suggest?
Fixed airflow obstruction, such as in chronic obstructive pulmonary disease (COPD).
80. What is the correct formula for percent improvement after bronchodilator administration?
(Post FEV1 − Pre FEV1) ÷ Pre FEV1 × 100.
81. What does the single-breath DLCO test measure?
The diffusing capacity of the lungs for carbon monoxide across the alveolar-capillary membrane.
82. Why is carbon monoxide used in the DLCO test?
Because it binds readily to hemoglobin and allows assessment of gas transfer efficiency.
83. What is the purpose of a methacholine challenge test?
To evaluate airway hyperresponsiveness in suspected asthma.
84. What defines a positive methacholine challenge test?
A 20% or greater decrease in FEV1 from baseline.
85. After a positive methacholine test, what should be administered?
A fast-acting bronchodilator to reverse bronchospasm.
86. What is the first step in spirometry interpretation?
Evaluate the FEV1/FVC ratio using measured (actual) values.
87. If the FEV1/FVC ratio is reduced, what pattern is present?
An obstructive defect.
88. If the FEV1/FVC ratio is normal but FVC is less than 80% predicted, what pattern is suggested?
A restrictive defect.
89. How is the severity of obstruction commonly graded?
By percent predicted FEV1.
90. What percent predicted FEV1 is considered mild obstruction?
70–79% of predicted
91. What percent predicted FEV1 is considered moderate obstruction?
60–69% of predicted
92. What percent predicted FEV1 indicates moderately severe obstruction?
50–59% of predicted
93. What percent predicted FEV1 indicates severe obstruction?
35–49% of predicted
94. What percent predicted FEV1 indicates very severe obstruction?
Less than 35% of predicted.
95. How is the degree of restriction typically determined?
By percent predicted FVC or total lung capacity (TLC).
96. What confirms a true restrictive defect?
A reduced total lung capacity.
97. What percent predicted FVC or TLC indicates mild restriction?
70–79% of predicted.
98. What percent predicted FVC or TLC indicates moderate restriction?
60–69% of predicted.
99. In obstruction with hyperinflation, how are lung volumes typically affected?
TLC, FRC, and/or RV are elevated above 120% of predicted.
100. How is hyperinflation severity classified?
Normal: 80–120%; Mild: 121–130%; Moderate: 131–140%; Moderately severe: 141–150%; Severe: 151–165%; Very severe: >165% of predicted.
Final Thoughts
The FEV1/FVC ratio provides essential information about airflow and is central to identifying obstructive lung disease. By comparing the volume exhaled in the first second to the total forced vital capacity, clinicians can determine whether airflow limitation is present.
For respiratory therapists, understanding how to measure, interpret, and apply this ratio is critical to accurate spirometry analysis and effective patient management.
When used alongside other pulmonary function data and clinical findings, the FEV1/FVC ratio supports informed decision making across diverse respiratory care settings.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- David S, Goldin J, Edwards CW. Forced Expiratory Volume. [Updated 2024 Oct 14]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025.