Barrel chest is a clinical term used to describe a rounded, bulging chest that resembles the shape of a barrel. It is often associated with chronic lung conditions that cause the lungs to remain overinflated, altering the shape of the thorax over time.
While some individuals may naturally have a more prominent chest shape, a true barrel chest is typically a sign of an underlying respiratory issue, such as chronic obstructive pulmonary disease (COPD) or emphysema.
Understanding what causes this physical change, how it’s diagnosed, and what treatment options are available can help patients and caregivers recognize and manage this condition more effectively.
What Is a Barrel Chest?
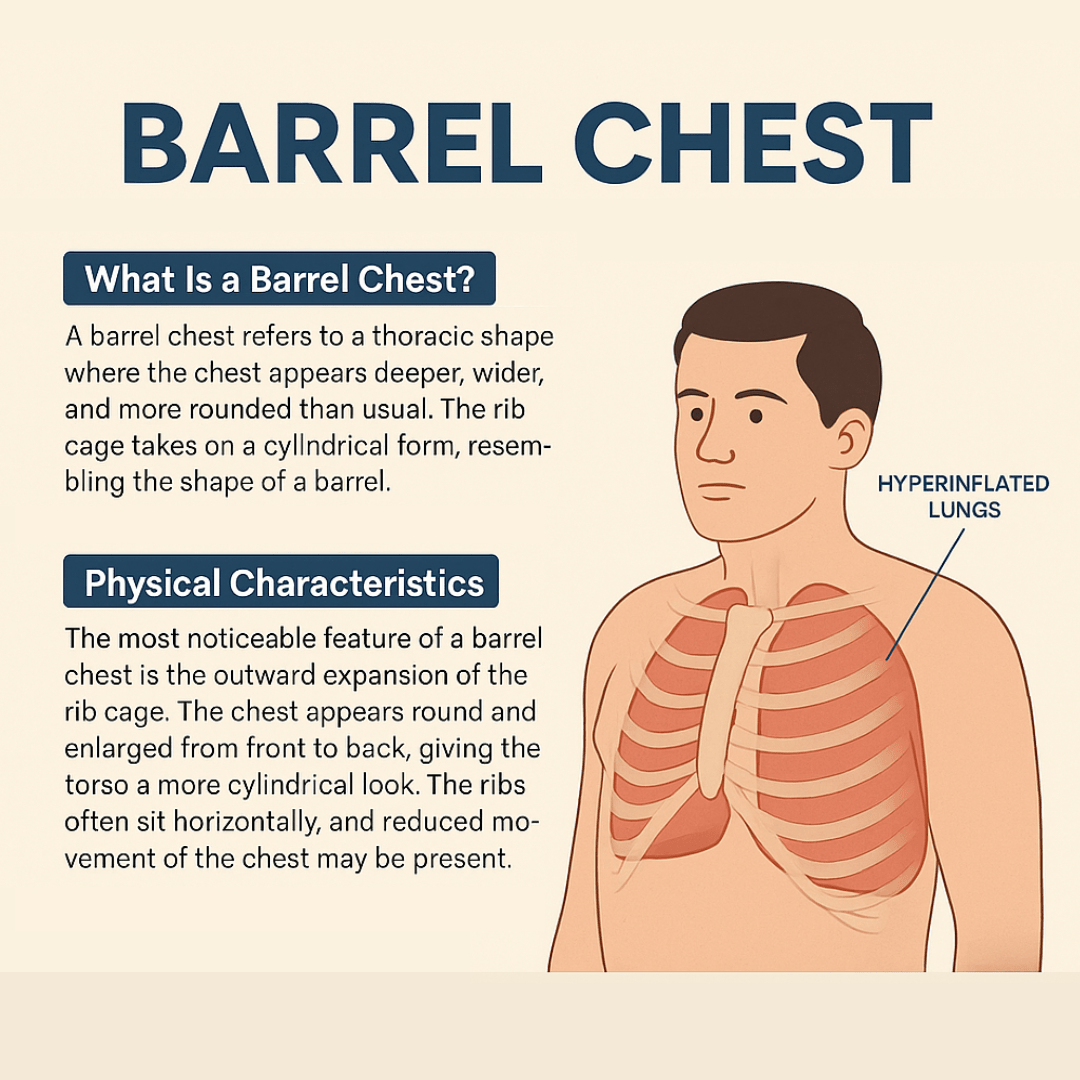
A barrel chest refers to a thoracic shape where the chest appears deeper, wider, and more rounded than usual. The rib cage takes on a cylindrical form, resembling the shape of a barrel.
This change is often linked to chronic lung conditions such as chronic obstructive pulmonary disease (COPD), emphysema, or long-standing asthma. In some cases, it may also be associated with cystic fibrosis in children or with normal aging in adults.
It is not considered a disease by itself but rather a physical sign. Doctors recognize it as an indicator that may point to structural changes in the lungs, rib cage, or surrounding tissues.
Physical Characteristics
The most noticeable feature of a barrel chest is the outward expansion of the rib cage. The chest appears round and enlarged from front to back, giving the torso a more cylindrical look.
In many cases, the ribs sit more horizontally than in a typical chest, and the angle of the ribs relative to the spine may flatten. This can make the chest wall less flexible.
Some individuals may also show reduced movement of the chest during breathing. The change often results from air being trapped in the lungs, which pushes the chest outward over time.
Prevalence
Barrel chest can appear in both children and adults, though the causes differ. In adults, it is most often linked to COPD, emphysema, or age-related changes in bone and muscle structure. Osteoarthritis of the spine and rib joints can also contribute.
In children, it is less common but may develop in those with chronic respiratory conditions such as cystic fibrosis or severe asthma.
Note: Not everyone with lung disease will develop a barrel chest. Its presence depends on the severity of the underlying condition, the duration of the disease, and individual differences in anatomy and health history.
Causes of a Barrel Chest
Barrel chest often develops due to long-term changes in the lungs, bones, and muscles of the chest. It may result from chronic respiratory disease, age-related structural changes, inherited traits, or other medical conditions that affect breathing or chest wall shape.
Chronic Obstructive Pulmonary Disease (COPD)
COPD is the most common cause of barrel chest. Conditions like emphysema and chronic bronchitis trap air inside the lungs, making it harder to exhale fully. Over time, this air trapping forces the chest to expand and remain in a rounded position.
The structural change occurs because the lungs stay partially inflated, which alters the rib cage and diaphragm mechanics. The chest wall adapts to this constant pressure, creating the barrel-like appearance.
This change is usually permanent once it develops. Treatment focuses on slowing disease progression, improving lung function, and managing symptoms rather than reversing the chest shape.
Aging and Natural Changes
Aging can contribute to a barrel chest even without significant lung disease. As people get older, the cartilage between the ribs stiffens, and the muscles supporting breathing weaken. These changes reduce chest wall flexibility.
The lungs also lose some elasticity with age. This natural decline makes it harder to fully empty the lungs, which can mimic the same air-trapping seen in COPD, though usually to a milder degree.
In older adults, a barrel chest may appear gradually and may not always signal serious disease. Still, it can affect breathing efficiency and physical stamina.
Genetic Factors
Genetics can play a role in predisposing someone to develop a barrel chest. Inherited conditions that affect lung structure, such as cystic fibrosis, can lead to long-term changes in chest shape. Children with severe asthma may also develop a rounded chest if the condition is not well controlled.
Some families may have structural differences in rib cage shape or lung function that increase the likelihood of a barrel chest. These genetic influences are less common than COPD or aging, but remain important in younger patients.
Note: Unlike age-related changes, genetic causes may show up earlier in life and may respond better to early treatment of the underlying condition.
Other Medical Conditions
Several other health problems can contribute to a barrel chest. Severe or long-standing asthma can cause similar air-trapping effects as COPD, especially in children. Chronic lung infections, such as tuberculosis, may also damage lung tissue and alter chest shape.
Certain bone and joint disorders, including ankylosing spondylitis, can affect the chest wall structure. Over time, these conditions may reduce flexibility and create a rounded chest appearance.
While less common, these causes highlight that barrel chest is not limited to lung disease alone. It can reflect a range of conditions that impact either lung function or chest wall anatomy.
Diagnosing the Underlying Cause of a Barrel Chest
Barrel chest is not a disease on its own but rather a physical sign that may point to an underlying condition, most commonly related to the lungs or musculoskeletal system. Diagnosis involves evaluating the shape of the chest in conjunction with clinical findings and diagnostic tests to identify the root cause.
Clinical Assessment
The diagnostic process begins with a physical examination. A healthcare provider will observe the chest shape, specifically noting an increased anteroposterior (front-to-back) diameter. This rounded appearance may suggest chronic overinflation of the lungs, particularly in patients with a history of smoking or respiratory symptoms.
During the exam, the clinician may palpate the chest wall to assess symmetry and movement, percuss for abnormal resonance that could indicate hyperinflation, and auscultate the lungs for signs such as wheezing, diminished breath sounds, or prolonged expiratory phases. These clues help determine whether the barrel chest appearance is associated with chronic lung disease, aging, or skeletal conditions.
Imaging Studies
Radiologic imaging is often used to evaluate the structural changes contributing to the chest shape. A chest X-ray may show signs consistent with emphysema, such as hyperinflated lungs, flattened diaphragms, and widened rib spaces. These findings support the presence of chronic obstructive pulmonary disease (COPD) or other conditions that may lead to a barrel chest.
Computed tomography (CT) scans offer more detailed views of the lung parenchyma and chest wall, allowing clinicians to assess for structural deformities, prior injury, or degenerative changes in the spine or ribs. In some cases, imaging helps rule out alternative causes such as kyphosis or osteoarthritis.
Pulmonary Function Testing
If a lung-related cause is suspected, pulmonary function tests (PFTs) can help quantify the degree of impairment. These tests assess airflow, lung volumes, and gas exchange efficiency. In individuals with COPD or other chronic respiratory conditions, PFTs may reveal obstructive patterns, air trapping, and reduced lung compliance—all of which can contribute to a persistently expanded chest shape.
Spirometry, a key component of PFTs, measures how much air a person can forcefully exhale and how quickly. Additional tests, such as lung volume measurements and diffusion capacity studies, help determine whether the chest configuration is due to chronic lung hyperinflation or another physiological change.
Treatment Options for a Barrel Chest
Treatment focuses on controlling the underlying disease, improving breathing efficiency, and maintaining mobility. Approaches often combine medical care, daily habit changes, and structured physical therapy to reduce symptoms and preserve lung function.
Medical Management
Doctors usually start by addressing the condition that causes the chest changes. In people with chronic obstructive pulmonary disease (COPD) or emphysema, inhaled bronchodilators and corticosteroids may help reduce airway inflammation and improve airflow. Oxygen therapy can be prescribed if blood oxygen levels remain low.
For asthma-related cases, long-term control medications such as inhaled steroids or leukotriene modifiers may be used. In cystic fibrosis, treatment may include airway clearance techniques, antibiotics, and medications that thin mucus.
Vaccinations against influenza and pneumonia are recommended to prevent respiratory infections. Regular monitoring with lung function tests helps track disease progression and guide treatment adjustments.
Lifestyle Modifications
Daily habits play a significant role in managing symptoms. Smoking cessation is the most important step for individuals with COPD or emphysema, as it slows further lung damage. Avoiding secondhand smoke, air pollutants, and respiratory irritants also helps protect lung health.
Maintaining a healthy weight supports easier breathing. Excess weight can put pressure on the chest and diaphragm, while being underweight may reduce strength and energy. A balanced diet with adequate protein and nutrients is encouraged.
Structured exercise, such as walking or cycling, can improve endurance. Pulmonary rehabilitation programs often provide supervised exercise and education to help patients build safe routines tailored to their condition.
Physical Therapy
Physical therapy focuses on improving breathing mechanics and mobility. Techniques such as pursed-lip breathing and diaphragmatic breathing help patients control shortness of breath and increase oxygen exchange.
Therapists may guide patients through stretching and posture exercises to counteract stiffness in the chest wall and spine. This can improve chest expansion and reduce discomfort.
Strength training of the upper body muscles also supports respiratory function. In conditions like cystic fibrosis, chest physiotherapy may include percussion or vibration techniques to loosen mucus and aid airway clearance.
Potential Complications
A barrel chest itself does not usually cause pain, but it often signals long-term changes in the lungs and chest wall. These changes can interfere with breathing efficiency and reduce overall lung function. People with this condition may experience shortness of breath, especially during physical activity. Over time, they can develop reduced exercise tolerance and fatigue due to limited oxygen exchange.
When linked to chronic obstructive pulmonary disease (COPD) or emphysema, a barrel chest may increase the risk of frequent respiratory infections. Inflamed or damaged airways make it harder to clear mucus, which can lead to bronchitis or pneumonia.
Some individuals may develop low oxygen levels in the blood. This can contribute to complications such as pulmonary hypertension or strain on the right side of the heart. In children with congenital causes, a barrel chest may affect growth and development, particularly if lung capacity is reduced. Breathing difficulties can also interfere with physical activity and sleep quality.
Note: While not every person with a barrel chest experiences severe problems, the condition often reflects an underlying disease that requires monitoring and management.
Living With a Barrel Chest
People with a barrel chest often need to adjust daily routines and healthcare practices to maintain lung function and comfort. Access to medical guidance, lifestyle strategies, and reliable support networks can help reduce complications and improve quality of life.
Daily Management
Managing barrel chest usually means focusing on the underlying condition, such as COPD or asthma. Regular use of prescribed inhalers, oxygen therapy when needed, and routine checkups with a pulmonologist help prevent worsening symptoms.
Physical activity plays a role, but it should be tailored. Pulmonary rehabilitation programs provide structured exercises that strengthen breathing muscles and improve endurance. Even simple activities like walking or light stretching can support lung health if done consistently.
Breathing techniques, such as pursed-lip breathing, allow patients to move air more efficiently and reduce shortness of breath. Maintaining a healthy weight also lessens the strain on the respiratory system.
At home, small adjustments can make tasks easier. Using chairs for rest breaks, keeping frequently used items accessible, and planning activities during times of higher energy can conserve breath and reduce fatigue.
Support Resources
Access to professional and community resources can make living with a barrel chest more manageable. Pulmonologists, respiratory therapists, and primary care physicians provide guidance on treatment and symptom monitoring.
Support groups, both in-person and online, offer a space to share experiences and coping strategies. Many patients find encouragement by connecting with others who face similar daily challenges.
Educational programs from organizations like the American Lung Association give practical information about managing chronic lung disease. Insurance providers and local health services may also offer coverage for pulmonary rehab or home oxygen equipment.
Family and caregivers play an important role by assisting with daily tasks, attending medical appointments, and providing emotional support. Having a reliable support system helps patients stay consistent with treatment and lifestyle adjustments.
FAQs About a Barrel Chest
What Does a Barrel Chest Indicate?
A barrel chest typically indicates an underlying change in the structure of the chest wall, often due to chronic lung conditions. Most commonly, it is associated with chronic obstructive pulmonary disease (COPD), especially emphysema, where the lungs remain overinflated over time.
It can also be seen with aging or certain musculoskeletal conditions. While a barrel chest itself is not a diagnosis, it serves as a visual sign that prompts further evaluation of lung function or skeletal abnormalities.
Why Do COPD Patients Have a Barrel Chest?
In COPD, especially emphysema, the lungs lose their elasticity, making it difficult to fully exhale air. As air becomes trapped in the lungs, they gradually become hyperinflated. This chronic overexpansion pushes the chest wall outward and increases the front-to-back diameter of the chest, resulting in the barrel chest appearance.
It is a structural adaptation to long-term breathing difficulty. Though it may help accommodate chronically overinflated lungs, it also signals the progression of lung damage over time.
Why Does a Barrel Chest Occur in Emphysema?
Barrel chest occurs in emphysema due to the destruction of alveolar walls and the loss of lung elasticity. This damage prevents the lungs from fully deflating during exhalation, causing air trapping and overinflation.
As the lungs remain chronically expanded, they push against the chest wall, gradually changing its shape. Over time, this leads to a rounded, barrel-like appearance. It’s a physical manifestation of advanced lung damage and typically develops in individuals with long-standing emphysema.
Does a Barrel Chest Affect Breathing?
Yes, a barrel chest can affect breathing, especially when it’s caused by chronic lung disease. The expanded shape of the chest indicates hyperinflated lungs, which means there’s less room for new air to enter with each breath.
This can lead to shortness of breath, especially during physical activity. The diaphragm may also become flattened and less efficient, forcing the body to rely more on accessory muscles for breathing. These changes can increase the work of breathing and fatigue.
Can You Reverse a Barrel Chest?
Barrel chest caused by chronic lung conditions like emphysema is generally not reversible because it results from permanent structural changes in the lungs and chest wall. However, treatment can help manage symptoms and prevent progression.
Pulmonary rehabilitation, bronchodilators, and lifestyle changes such as quitting smoking can improve breathing efficiency. In some cases where barrel chest is related to posture or musculoskeletal issues, physical therapy may help improve flexibility and function, but it won’t fully restore the original chest shape.
Final Thoughts
Barrel chest is more than just a physical characteristic—it’s often a visible sign of an underlying respiratory issue that may require medical attention. While some cases are related to natural aging or body structure, others are linked to chronic lung diseases like emphysema and COPD.
Recognizing the causes, getting an accurate diagnosis, and following an appropriate treatment plan can help manage symptoms and improve breathing function.
If you or someone you know develops changes in chest shape or experiences persistent respiratory symptoms, it’s important to consult a healthcare provider for evaluation and care.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Sarkar M, Bhardwaz R, Madabhavi I, Modi M. Physical signs in patients with chronic obstructive pulmonary disease. Lung India. 2019.