Continuous mandatory ventilation (CMV) is one of the most fundamental modes of mechanical ventilation used in critical care. In this mode, the ventilator provides full ventilatory support by delivering mandatory breaths at preset settings. CMV plays a central role in the management of patients who cannot maintain adequate ventilation on their own.
For respiratory therapists, understanding CMV is essential because it forms the foundation for managing critically ill patients, optimizing gas exchange, preventing complications, and ensuring safe and effective ventilatory support.
What is Continuous Mandatory Ventilation?
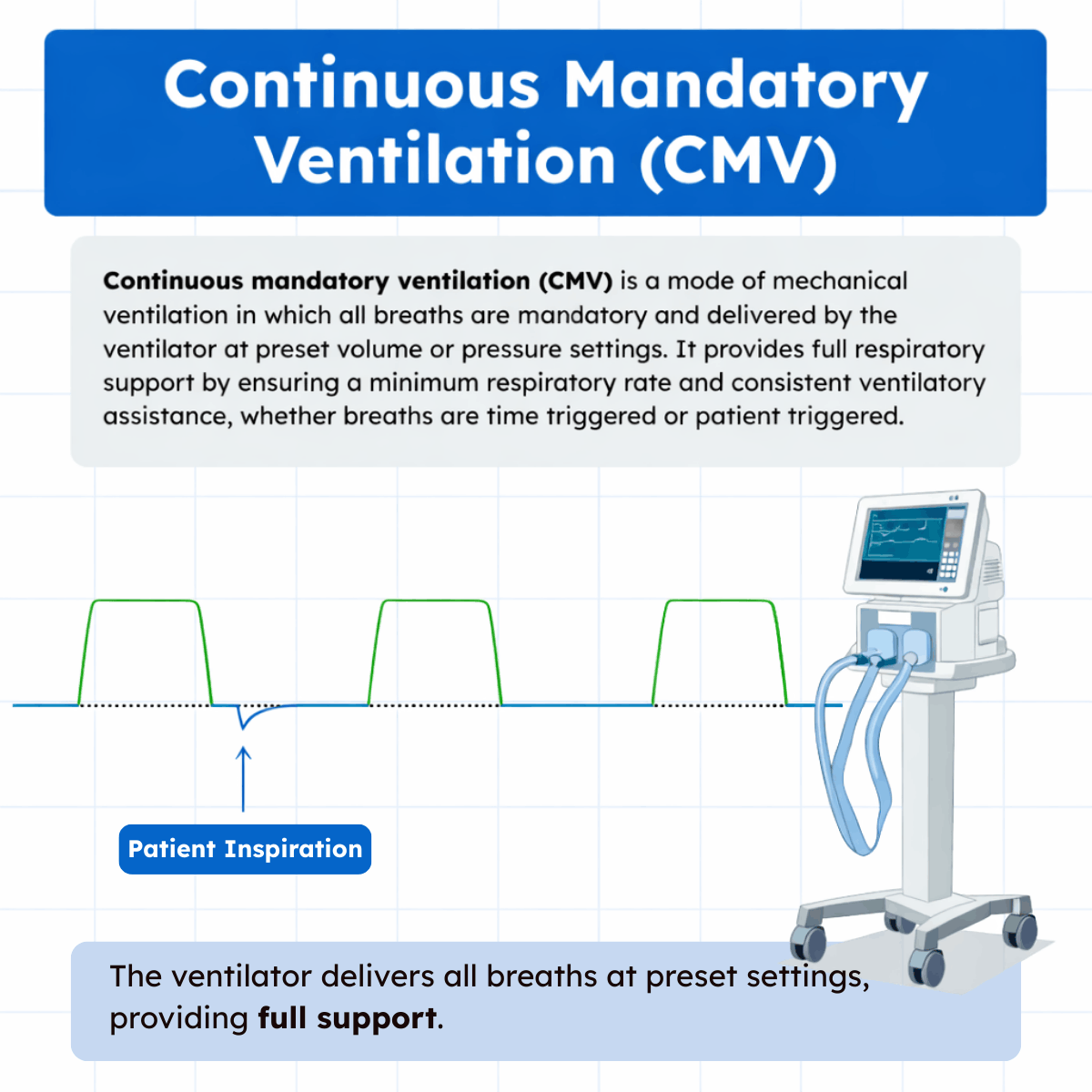
Continuous mandatory ventilation (CMV) is a mode of mechanical ventilation in which the ventilator provides full respiratory support by delivering mandatory breaths at preset settings. In this mode, the clinician determines key parameters such as tidal volume or inspiratory pressure, respiratory rate, inspiratory time, and fraction of inspired oxygen.
Every breath delivered to the patient is a machine breath. Breaths may be time triggered at a fixed rate or patient triggered if the ventilator detects an inspiratory effort, but spontaneous breaths between mandatory breaths are not permitted.
CMV ensures a guaranteed minimum minute ventilation and is commonly used in patients who are apneic, heavily sedated, paralyzed, or unable to sustain adequate spontaneous breathing. Because the patient may be fully dependent on the ventilator, careful monitoring of airway pressures, tidal volume, trigger sensitivity, and alarms is essential to maintain safety and optimize gas exchange.
Key Components of CMV
1. Trigger
The trigger determines how inspiration begins. It may be:
- Time trigger: The ventilator delivers breaths at the preset rate
- Patient trigger: The ventilator senses a change in pressure or flow caused by patient effort
Note: The sensitivity setting must be carefully adjusted. If it is too sensitive, autotriggering may occur. If it is not sensitive enough, the patient must generate excessive negative pressure, increasing work of breathing.
2. Target Variable
CMV can be either:
- Volume targeted
- Pressure targeted
Note: In volume-targeted CMV, a preset tidal volume is delivered with each breath. Airway pressures vary depending on lung compliance and resistance. In pressure-targeted CMV, a preset inspiratory pressure is delivered. Tidal volume varies depending on lung mechanics and patient effort.
3. Cycling
Breaths are typically:
- Volume cycled in volume control
- Time cycled in pressure control
Note: Cycling determines when inspiration ends and expiration begins.
Volume-Controlled CMV
Volume-controlled continuous mandatory ventilation (VC-CMV) guarantees delivery of a preset tidal volume. This makes it useful when maintaining a specific minute ventilation or arterial carbon dioxide level is clinically important.
Advantages
- Predictable tidal volume
- Reliable control of minute ventilation
- Useful when strict PaCO2 control is necessary
Considerations
Airway pressures fluctuate as lung compliance or airway resistance changes. Reduced compliance or increased resistance will raise peak inspiratory pressure. Monitoring plateau pressure and driving pressure is essential to prevent ventilator-induced lung injury.
Another important consideration is inspiratory flow. If the set flow does not meet patient demand, the patient may generate additional effort, increasing work of breathing. A concave pressure waveform may indicate inadequate flow delivery.
Pressure-Controlled CMV
Pressure-controlled continuous mandatory ventilation (PC-CMV) delivers a preset inspiratory pressure for a set inspiratory time. The tidal volume achieved depends on lung compliance, airway resistance, and patient effort.
Advantages
- Decelerating flow pattern may improve gas distribution
- Potential for improved patient-ventilator synchrony
- Better control of peak airway pressure
Considerations
Because tidal volume is not guaranteed, close monitoring is necessary. Changes in compliance, resistance, or patient effort can significantly alter delivered volume. Respiratory therapists must continuously assess tidal volume, minute ventilation, and arterial blood gases to prevent hypoventilation or hyperventilation.
Note: Higher mean airway pressures may affect hemodynamics, particularly in patients with compromised cardiac function.
Indications for CMV
CMV is used when total ventilatory support is required. Common indications include:
- Severe respiratory failure
- Apnea or inadequate spontaneous effort
- Neuromuscular paralysis
- Severe traumatic brain injury requiring controlled ventilation
- Tetanus or seizure activity interfering with spontaneous breathing
- Situations requiring complete respiratory muscle rest
In some patients, CMV is used temporarily to stabilize gas exchange before transitioning to partial support modes.
CMV may also be necessary when patients are fighting the ventilator and experiencing significant asynchrony that cannot be corrected by adjusting settings. In such cases, sedation or neuromuscular blockade may be required.
Relevance to Respiratory Therapists
Continuous mandatory ventilation is highly relevant to respiratory therapists for several reasons.
1. Foundational Knowledge
CMV is often the first mode initiated in critically ill patients. Respiratory therapists must understand how to set initial parameters based on patient size, lung mechanics, and disease process.
2. Patient-Ventilator Synchrony
Therapists must recognize and correct asynchrony. Improper trigger sensitivity, inadequate flow delivery, or inappropriate inspiratory time can increase work of breathing and patient discomfort.
3. Monitoring and Safety
Patients on CMV are often completely dependent on the ventilator. Accidental disconnection or ventilator failure can rapidly lead to hypoxia and apnea. Therapists must ensure that alarms such as low exhaled volume and low inspiratory pressure are appropriately set.
4. Lung Protection
In conditions such as acute respiratory distress syndrome, careful adjustment of tidal volume, plateau pressure, and driving pressure is essential. Respiratory therapists play a critical role in preventing ventilator-induced lung injury.
5. Weaning Readiness Assessment
Although CMV provides full support, therapists must continually evaluate readiness for transition to partial support modes such as synchronized intermittent mandatory ventilation or spontaneous breathing trials.
Complications of CMV
- Diaphragmatic Disuse Atrophy: Prolonged controlled ventilation can lead to rapid atrophy of diaphragm muscle fibers. Studies show that even short periods of inactivity can weaken respiratory muscles. This may complicate weaning.
- Ventilator-Induced Lung Injury: High airway pressures or excessive tidal volumes may result in barotrauma or volutrauma. Monitoring plateau pressure and adjusting settings accordingly is essential.
- Autotriggering: Overly sensitive trigger settings may cause the ventilator to deliver unintended breaths, leading to hyperventilation, air trapping, and respiratory alkalosis.
- Increased Work of Breathing: If trigger sensitivity is too low or inspiratory flow is inadequate, patients may experience increased work of breathing and fatigue.
- Hemodynamic Effects: Elevated mean airway pressure can reduce venous return and cardiac output, particularly in patients receiving higher levels of PEEP.
CMV Compared With Other Breath Sequences
Mechanical ventilation breath sequences can be classified into three categories:
- Continuous mandatory ventilation
- Intermittent mandatory ventilation
- Continuous spontaneous ventilation
In CMV, spontaneous breaths are not allowed between mandatory breaths. In intermittent mandatory ventilation, spontaneous breaths can occur between mandatory breaths. In continuous spontaneous ventilation, all breaths are spontaneous.
Note: Understanding these distinctions helps respiratory therapists select appropriate modes and anticipate patient response.
Clinical Management Principles
Effective management of CMV involves:
- Setting appropriate tidal volume or inspiratory pressure
- Adjusting respiratory rate to meet ventilation goals
- Monitoring plateau pressure and driving pressure
- Optimizing trigger sensitivity
- Matching inspiratory flow to patient demand
- Monitoring arterial blood gases and ventilator waveforms
Note: Therapists must also ensure that backup ventilation is functioning and that alarm limits are correctly set. Frequent reassessment is necessary because patient condition, lung mechanics, and metabolic demands may change rapidly in critical care.
Continuous Mandatory Ventilation Practice Questions
1. What is continuous mandatory ventilation (CMV)?
Continuous mandatory ventilation is a mode of mechanical ventilation in which all breaths are mandatory and delivered at preset parameters, either time-triggered or patient-triggered.
2. What does the ventilator control in CMV?
In CMV, the ventilator controls tidal volume or pressure and the minimum respiratory rate, thereby determining the patient’s minute ventilation.
3. How is minute ventilation calculated in CMV?
Minute ventilation is calculated by multiplying tidal volume by respiratory rate (e.g., 800 mL × 10 breaths/min = 8 L/min).
4. What is the difference between control mode and assist/control (A/C) mode?
Control mode is time-triggered only, whereas assist/control allows patient-triggered breaths in addition to time-triggered mandatory breaths.
5. In control mode ventilation, can the patient initiate spontaneous breaths?
No, in pure control mode, breaths are delivered only at the preset rate and are not patient-triggered.
6. When is CMV commonly indicated?
CMV is indicated when full ventilatory support is required, such as in patients with severe respiratory failure or those requiring complete ventilatory control.
7. Why are sedation and neuromuscular blockade often used with control mode?
They are used to suppress spontaneous respiratory effort and prevent patient-ventilator asynchrony.
8. What does “fighting the ventilator” mean?
It refers to patient-ventilator asynchrony in which the patient’s spontaneous efforts conflict with ventilator-delivered breaths.
9. What can happen if a patient actively exhales during ventilator inspiration?
High airway pressures may occur, potentially leading to premature breath termination or reduced delivered tidal volume.
10. Why should the trigger sensitivity not be set too insensitive?
If set too insensitive, the patient may be unable to trigger breaths, resulting in unintended control ventilation.
11. Why should the trigger sensitivity not be set too sensitive?
If set too sensitive, the ventilator may auto-trigger due to circuit movement, leaks, or cardiac oscillations.
12. What is a key psychological concern with improperly applied control mode?
A conscious patient may feel distress if unable to influence breathing.
13. What is a major hazard of CMV?
If the ventilator disconnects or fails, the patient may develop apnea and hypoxia due to complete dependence.
14. Which ventilator alarms are critical in CMV?
Low exhaled volume and low inspiratory pressure alarms are essential to detect disconnection or leaks.
15. What is diaphragmatic disuse atrophy?
It is muscle weakening that occurs when the diaphragm is inactive during prolonged full ventilatory support.
16. How quickly can diaphragmatic atrophy begin during controlled ventilation?
Evidence suggests significant atrophy can occur within 18 to 69 hours of complete inactivity.
17. What physiologic changes occur with prolonged controlled ventilation?
Oxidative injury, increased proteolysis, and reduced diaphragmatic contractility may develop.
18. What types of targeting can be used in CMV?
Breaths may be volume-targeted or pressure-targeted.
19. What is the primary difference between CMV and spontaneous ventilation modes?
In CMV, all breaths are mandatory, whereas spontaneous modes allow patient-determined tidal volumes and rates.
20. In assist/control mode, what happens if the patient triggers additional breaths?
Each triggered breath delivers the full preset tidal volume or pressure.
21. Why can assist/control mode lead to respiratory alkalosis?
If the patient triggers excessive breaths, minute ventilation may become elevated.
22. What clinical condition may require complete ventilatory rest using CMV?
Severe respiratory distress or the need for complete muscle rest.
23. Why might CMV be used in severe chest wall trauma?
To reduce paradoxical movement and provide stable ventilation.
24. How can tetanus or seizure activity justify CMV?
Uncontrolled muscle activity may interfere with effective ventilation.
25. What happens if a patient becomes disconnected from the ventilator in CMV?
The patient may experience apnea because spontaneous breathing is suppressed.
26. How does CMV affect patient work of breathing?
The ventilator assumes full responsibility, minimizing patient work of breathing.
27. What is time-triggering in CMV?
Breaths are delivered at preset intervals based solely on the set respiratory rate.
28. What is patient-triggering in CMV?
The ventilator senses patient effort and delivers a mandatory breath in response.
29. Why is monitoring ABGs important in CMV?
To ensure adequate ventilation and oxygenation while preventing hypo- or hyperventilation.
30. What is the primary goal of CMV?
To provide full, consistent ventilatory support when the patient cannot adequately breathe independently.
31. What is assist/control (A/C) ventilation?
Assist/control ventilation is a form of continuous mandatory ventilation in which breaths may be patient-triggered or time-triggered, but every delivered breath is a full mandatory breath.
32. What ventilator settings are established in A/C mode?
The clinician sets a minimum respiratory rate, tidal volume or inspiratory pressure, sensitivity level, and other relevant parameters such as inspiratory time or flow.
33. What happens when a patient triggers a breath in A/C mode?
Each triggered breath delivers the full preset tidal volume in volume modes or the preset inspiratory pressure in pressure modes.
34. How does the ventilator detect patient triggering?
The ventilator senses a drop in airway pressure (commonly −1 to −2 cm H2O) or a decrease in flow below baseline to initiate inspiration.
35. What is the purpose of setting a minimum respiratory rate in A/C ventilation?
It guarantees a minimum minute ventilation if the patient does not trigger additional breaths.
36. What is auto-triggering in A/C mode?
Auto-triggering occurs when the ventilator delivers unintended breaths due to excessive sensitivity, leaks, or circuit movement.
37. How is auto-triggering corrected?
By reducing sensitivity so the ventilator requires a slightly greater patient effort to trigger a breath.
38. What indicates that the ventilator sensitivity is set too insensitive?
If the patient must generate a large negative pressure (e.g., −3 to −5 cm H2O) before a breath is delivered.
39. What is the consequence of an insensitive trigger setting?
Increased patient work of breathing and possible fatigue.
40. What is ventilator response time?
Response time is the delay between detection of patient effort and delivery of inspiratory flow.
41. Why is rapid response time important in patient-triggered ventilation?
It reduces patient effort and improves comfort and synchrony.
42. Why may respiratory alkalosis develop in A/C ventilation?
If the patient triggers frequent breaths, minute ventilation may increase excessively, lowering PaCO2.
43. What is the apneic threshold for PaCO2?
It is typically around 32 mm Hg, below which spontaneous respiratory drive may cease in some patients.
44. What is volume-controlled continuous mandatory ventilation (VC-CMV)?
VC-CMV is a mode in which a preset tidal volume is delivered with each mandatory breath.
45. Does VC-CMV eliminate patient work of breathing?
No, patients may still perform a significant portion of inspiratory work, especially if flow is inadequate.
46. How can inadequate inspiratory flow be identified in VC-CMV?
A concave pressure-time waveform during inspiration suggests insufficient flow to meet patient demand.
47. How is inadequate inspiratory flow corrected?
By increasing the set inspiratory flow rate to better match patient demand.
48. What is pressure-controlled continuous mandatory ventilation (PC-CMV)?
PC-CMV is a mode in which breaths are pressure-targeted, time-cycled, and either patient- or time-triggered.
49. What determines tidal volume in PC-CMV?
Tidal volume depends on lung compliance, airway resistance, patient effort, and the set inspiratory pressure.
50. What type of flow pattern is seen in PC-CMV?
A decelerating flow pattern is characteristic of pressure-controlled ventilation.
51. Why might PC-CMV improve gas distribution?
The decelerating flow pattern may enhance alveolar recruitment and distribution of ventilation.
52. How should the maximum pressure limit be set in PC-CMV?
It is typically set about 10 cm H2O above the target inspiratory pressure to prevent excessive airway pressure.
53. What can cause airway pressure to exceed the set inspiratory pressure?
Coughing or active patient effort may transiently increase circuit pressure.
54. What is pressure-control inverse ratio ventilation (PCIRV)?
PCIRV is a form of pressure-controlled ventilation in which inspiratory time exceeds expiratory time.
55. How does inverse ratio ventilation improve oxygenation?
By increasing mean airway pressure and promoting alveolar recruitment.
56. What is a potential consequence of prolonged inspiratory time in PCIRV?
Incomplete exhalation may occur, leading to air trapping and auto-PEEP.
57. In which patients is PCIRV typically reserved?
It is generally reserved for patients with severe lung stiffness who fail conventional ventilation strategies.
58. Why is sedation often required with PCIRV?
The altered inspiratory-to-expiratory ratio may be uncomfortable and poorly tolerated.
59. What was the historical indication for PC-CMV?
It was frequently used in patients with acute respiratory distress syndrome to limit peak pressures.
60. What is a key clinical consideration when selecting between VC-CMV and PC-CMV?
VC-CMV guarantees tidal volume, whereas PC-CMV limits airway pressure but allows tidal volume to vary.
61. When is controlled (time-triggered) ventilation most appropriate?
Controlled ventilation is appropriate when a patient is unable to initiate spontaneous breaths, such as in cases of severe neurologic impairment, drug-induced respiratory depression, or neuromuscular paralysis.
62. Why is “locking out” a patient by making the ventilator completely insensitive rarely advisable?
Because it increases patient discomfort, work of breathing, and anxiety if spontaneous effort is present but not recognized by the ventilator.
63. What clinical conditions may require fully controlled ventilation?
Severe brain injury, spinal cord injury, phrenic nerve injury, profound sedation, or neuromuscular blockade.
64. Why are sedation and neuromuscular blockade sometimes required with controlled ventilation?
To eliminate spontaneous respiratory efforts that interfere with ventilator synchrony or therapeutic goals.
65. In what situation might deliberate hyperventilation be used?
Short-term hyperventilation may be used to lower elevated intracranial pressure by inducing respiratory alkalosis.
66. Why is iatrogenic hyperventilation controversial?
Because prolonged hypocapnia can reduce cerebral blood flow and potentially worsen neurologic outcomes.
67. What monitoring is essential during controlled ventilation?
Continuous monitoring of airway pressures, exhaled tidal volume, oxygen saturation, and appropriate alarm settings.
68. What are the three possible ventilator breath sequences?
Continuous mandatory ventilation (CMV), intermittent mandatory ventilation (IMV), and continuous spontaneous ventilation (CSV).
69. How is CMV defined in terms of breath sequence?
All breaths are mandatory, and spontaneous breaths are not permitted between mandatory breaths.
70. How is IMV different from CMV?
IMV allows spontaneous breaths between mandatory breaths.
71. What defines CSV?
All breaths are spontaneous and initiated by the patient.
72. In CMV, can the total respiratory rate exceed the set rate?
Yes, if the patient triggers additional breaths in assist/control mode.
73. In IMV, can the mandatory breath rate exceed the set rate?
No, the mandatory rate cannot exceed the set rate, though spontaneous breaths may increase total rate.
74. What is a key hazard of CMV?
Complete ventilator dependence, making disconnection or ventilator failure potentially life-threatening.
75. Why must sensitivity be properly adjusted even in controlled modes?
To ensure that minimal patient effort is detected and unnecessary work of breathing is avoided.
76. What is the main advantage of volume-controlled CMV (VC-CMV)?
It guarantees delivery of a preset tidal volume.
77. What happens to airway pressure in VC-CMV when lung compliance decreases?
Peak airway pressure increases to deliver the set tidal volume.
78. Why must inspiratory flow be carefully set in VC-CMV?
Insufficient flow increases work of breathing, whereas excessive flow may shorten inspiratory time inappropriately.
79. What is the primary control variable in VC-CMV?
Tidal volume
80. What is the primary control variable in pressure-controlled CMV (PC-CMV)?
Inspiratory pressure
81. How does PC-CMV affect tidal volume?
Tidal volume varies based on lung compliance, resistance, and patient effort.
82. What waveform characteristic is associated with PC-CMV?
A rectangular pressure waveform with a decelerating inspiratory flow pattern.
83. Why may PC-CMV improve patient-ventilator synchrony?
Because inspiratory flow adapts to patient demand.
84. What parameter is adjusted in PC-CMV to influence CO2 elimination?
Driving pressure, typically the difference between plateau pressure and PEEP.
85. Why is tidal volume monitoring essential in PC-CMV?
Because tidal volume is not fixed and may fluctuate with changes in lung mechanics.
86. How can higher mean airway pressure affect hemodynamics?
It may decrease venous return and reduce cardiac output.
87. What risk is associated with insufficient expiratory time at high mandatory rates?
Air trapping and development of auto-PEEP.
88. How does auto-PEEP impair hemodynamics?
By increasing intrathoracic pressure and reducing venous return.
89. Why might PC-CMV be preferred when airway leaks are present?
Because pressure targeting can reduce variability in delivered volume caused by leaks.
90. What happens to delivered tidal volume in PC-CMV if compliance improves?
Tidal volume increases unless inspiratory pressure is adjusted.
91. What happens to delivered tidal volume in PC-CMV if resistance increases?
Tidal volume decreases for the same set inspiratory pressure.
92. Why must cardiac index and oxygen consumption be monitored in controlled ventilation?
Changes in mean airway pressure and ventilation strategy can impact cardiac output and metabolic demand.
93. What is the primary goal of controlled ventilation?
To provide full ventilatory support while maintaining stable gas exchange.
94. Why may sedation be required in poorly tolerated CMV?
To reduce anxiety, minimize ventilator asynchrony, and decrease work of breathing.
95. What is a major physiologic difference between VC-CMV and PC-CMV?
VC-CMV guarantees tidal volume with variable pressure, whereas PC-CMV limits pressure with variable tidal volume.
96. Why must clinicians remain vigilant when using pressure-control inverse ratio ventilation?
Because prolonged inspiratory time can cause air trapping, auto-PEEP, and hemodynamic compromise.
97. What is the defining characteristic of CMV regardless of trigger type?
All breaths delivered are mandatory breaths, whether time-triggered or patient-triggered.
98. Why is low exhaled tidal volume alarm especially important in CMV?
Because the patient is fully dependent on the ventilator, and a drop in exhaled volume may indicate disconnection, leak, or ventilator malfunction.
99. How can autotriggering in assist/control mode affect a patient?
It can lead to unintended hyperventilation, respiratory alkalosis, and potential air trapping.
100. Why is careful monitoring of plateau pressure important in VC-CMV?
Because elevated plateau pressures increase the risk of ventilator-induced lung injury due to excessive alveolar distending pressure.
Final Thoughts
Continuous mandatory ventilation (CMV) is a core mode of mechanical ventilation that provides complete ventilatory support when patients cannot breathe adequately on their own. It requires careful attention to trigger sensitivity, tidal volume or pressure settings, inspiratory flow, and safety alarms.
For respiratory therapists, mastery of CMV is essential because it directly affects patient stability, gas exchange, and long-term outcomes. Proper management minimizes complications such as lung injury and diaphragmatic weakness while ensuring that critically ill patients receive safe and effective ventilatory support.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Chatburn RL, Hatipoğlu U. The Evolution of Intermittent Mandatory Ventilation: Update and Implications for Home Care. Respir Care. 2024.

