Croup and epiglottitis are two pediatric respiratory conditions that can present with similar symptoms but require very different management strategies. For respiratory therapists preparing for the board exam, understanding how to quickly distinguish between these conditions is essential.
Croup, a viral infection, typically presents with a barking cough and inspiratory stridor that develops gradually. Epiglottitis, a bacterial infection, is characterized by sudden onset, high fever, drooling, and severe respiratory distress.
Because these conditions affect the upper airway and can progress rapidly in children, recognizing their differences is critical. Misidentifying epiglottitis as a less severe condition can delay life-saving airway management, while confusing croup with epiglottitis may lead to unnecessary invasive procedures.
Mastering the identification and treatment of these two conditions is therefore essential not only for board exam success but also for providing safe and effective patient care in clinical practice.
Take our free course to learn essential tips, insights, and strategies to pass the TMC Exam on your first (or next) attempt.
Understanding the Difference Between Croup and Epiglottitis
When preparing for the board exam, respiratory therapists must be able to differentiate between croup and epiglottitis—two upper airway disorders that can cause significant respiratory distress in pediatric patients.
Although they share some overlapping symptoms, such as stridor and breathing difficulty, their causes, progression, and treatments differ dramatically.
Croup usually develops slowly and often responds well to medical therapy, while epiglottitis can progress rapidly and may lead to complete airway obstruction if not treated immediately.
Recognizing the clinical patterns associated with each condition allows respiratory therapists to select the correct intervention quickly. This skill is heavily emphasized on the board exam, where you are expected to analyze symptoms, imaging findings, and clinical context to determine the most appropriate next step in patient management.
Causes and Pathophysiology
Croup (Laryngotracheobronchitis)
Croup is a viral infection that causes inflammation and swelling of the larynx, trachea, and bronchi. The most common cause is the parainfluenza virus, although influenza viruses and respiratory syncytial virus (RSV) can also trigger the condition.
Inflammation leads to narrowing of the upper airway, particularly in the subglottic region. Because children have smaller airways than adults, even mild swelling can significantly increase airway resistance.
This narrowing produces the classic symptoms of a barking cough and inspiratory stridor. Symptoms usually develop gradually over several days and often worsen at night.
Epiglottitis
Epiglottitis is a bacterial infection that causes rapid inflammation of the epiglottis, the structure that covers the trachea during swallowing.
The most common causative organism historically has been Haemophilus influenzae type B (Hib), although widespread vaccination has reduced its prevalence. Other bacteria such as Streptococcus and Staphylococcus species may also cause the infection.
Unlike croup, epiglottitis develops quickly and can lead to complete airway obstruction within hours. Swelling of the epiglottis blocks airflow at the level of the larynx, making immediate airway management critical.
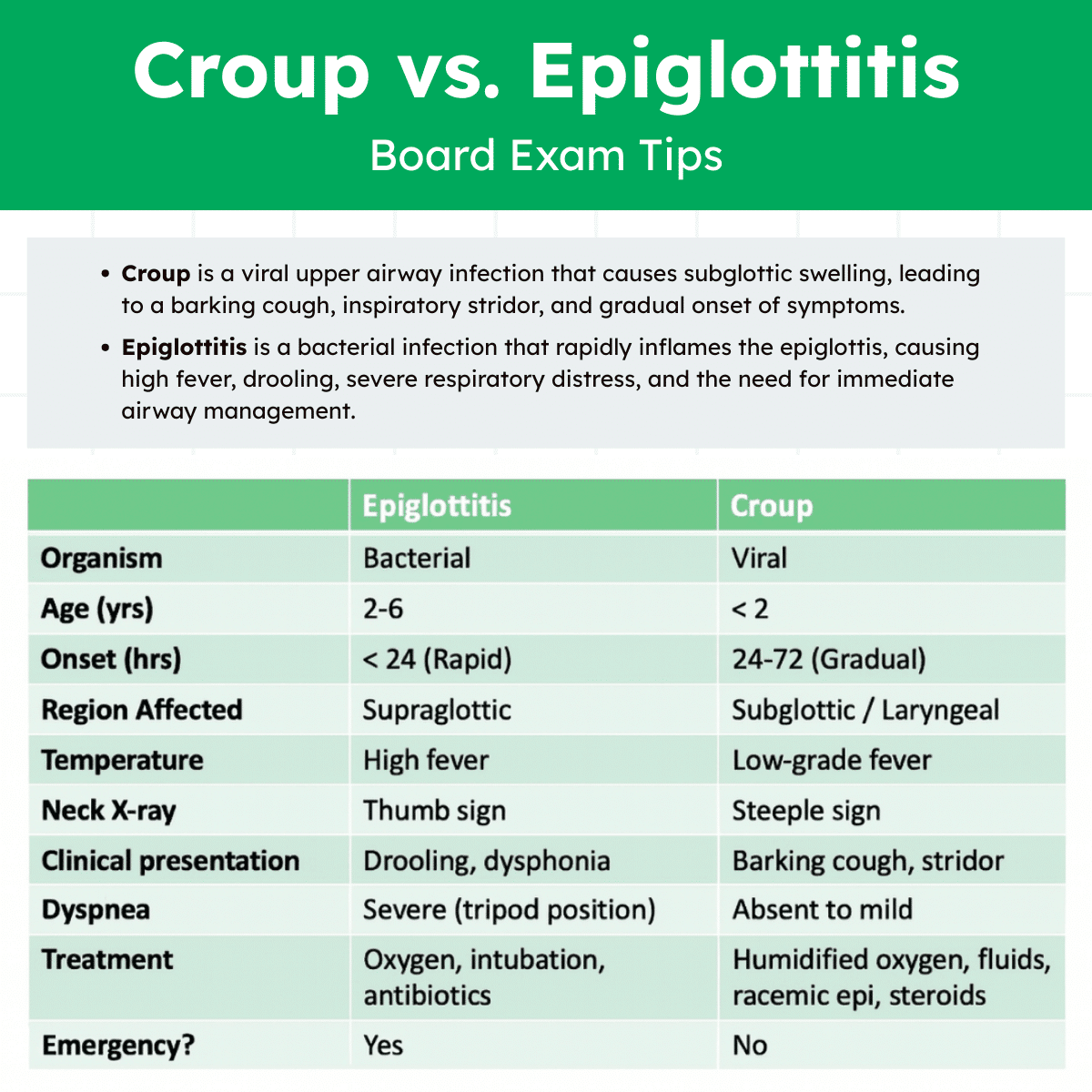
Clinical Presentation
Recognizing the clinical differences between croup and epiglottitis is essential for both the board exam and real-world patient care.
Although both conditions cause upper airway obstruction, their symptom patterns are usually very different.
Croup Symptoms
- Onset: Gradual, typically developing over several days
- Age Group: Most common in children 6 months to 3 years
- Fever: Low-grade fever (rarely exceeds 102°F)
- Cough: Characteristic barking or “seal-like” cough
- Stridor: Inspiratory stridor that worsens with agitation or crying
- Drooling: Typically absent
- Voice: Hoarse voice or weak cry
- Positioning: Child can usually lie flat and may improve with humidified air
Epiglottitis Symptoms
- Onset: Sudden onset with rapid progression
- Age Group: Typically affects children 2 to 6 years but can occur in adults
- Fever: High fever (often >102°F)
- Cough: Minimal or absent
- Stridor: May be soft or absent due to severe airway obstruction
- Drooling: Present due to difficulty swallowing
- Voice: Muffled “hot potato” voice
- Positioning: Tripod position (leaning forward to improve breathing)
Diagnosis
Both conditions require careful assessment to avoid misdiagnosis. On the board exam, you may be presented with symptoms, imaging findings, or clinical clues that help differentiate between croup and epiglottitis.
Croup Diagnosis
- Neck X-ray (AP View): Often shows the classic “steeple sign,” which represents subglottic narrowing of the airway.
- Pulse Oximetry: Oxygen saturation is usually normal unless the obstruction becomes severe.
- Clinical Assessment: Diagnosis is often based on symptoms such as barking cough, inspiratory stridor, and gradual onset.
Epiglottitis Diagnosis
- Neck X-ray (Lateral View): May show the “thumb sign,” indicating a swollen epiglottis.
- Laryngoscopy (Controlled Environment Only): Visualization may reveal a swollen, cherry-red epiglottis.
- Blood Cultures: Used to identify the bacterial pathogen responsible for infection.
Exam Hint: Never attempt to examine the throat with a tongue depressor in a suspected epiglottitis case. This can trigger sudden airway obstruction and respiratory collapse.
Treatment and Management
Once croup or epiglottitis is identified, appropriate treatment must be initiated quickly. The board exam frequently tests your ability to recognize which interventions are appropriate for each condition.
Croup Treatment
Since croup is viral in origin, treatment focuses on reducing airway inflammation and relieving symptoms.
- Mild cases: Supportive care with humidified air, hydration, and antipyretics.
- Moderate to severe cases: Nebulized racemic epinephrine to reduce airway swelling.
- Corticosteroids: Dexamethasone is commonly used to decrease airway inflammation.
- Oxygen therapy: Provided if hypoxemia develops.
- Hospitalization: May be required for patients with persistent stridor or respiratory distress.
Epiglottitis Treatment
Epiglottitis is a medical emergency because rapid swelling can lead to complete airway obstruction.
- Immediate airway management: Controlled endotracheal intubation to secure the airway.
- Emergency airway access: If intubation fails, an emergency tracheostomy or cricothyrotomy may be required.
- Oxygen therapy: Administer humidified oxygen when oxygen saturation is low.
- IV antibiotics: Ceftriaxone or cefotaxime are commonly used to treat the bacterial infection.
- IV fluids: Maintain hydration because swallowing is often impaired.
- ICU monitoring: Close observation is required due to the risk of sudden airway deterioration.
Exam Hint: In suspected epiglottitis, do not delay airway management to obtain imaging studies. If severe respiratory distress is present, securing the airway is the first priority.
Relevance to the Board Exam
Understanding the differences between croup and epiglottitis is a high-yield topic for the respiratory therapy board exam.
Exam questions often test your ability to recognize clinical symptoms, interpret imaging findings, and select the correct intervention.
Key concepts frequently tested include:
- Recognizing the steeple sign (croup) versus the thumb sign (epiglottitis).
- Identifying the appropriate treatment approach for each condition.
- Understanding the urgency of airway management in epiglottitis.
- Avoiding dangerous mistakes such as attempting throat examination in suspected epiglottitis.
Board Exam Tips for Croup and Epiglottitis
To answer board exam questions correctly, you must quickly recognize the clinical differences between these conditions and select the appropriate intervention.
1. Differentiate Based on Symptoms
- Croup: Barking cough, inspiratory stridor, low-grade fever, hoarseness, and gradual onset.
- Epiglottitis: High fever, drooling, muffled voice, rapid onset, and tripod positioning.
Exam Hint: If a child is sitting forward, drooling, and struggling to breathe without a barking cough, suspect epiglottitis and prepare for immediate airway management.
2. Know the Classic Imaging Findings
- Croup: “Steeple sign” caused by subglottic airway narrowing.
- Epiglottitis: “Thumb sign” caused by swelling of the epiglottis.
Exam Hint: If epiglottitis is suspected and severe respiratory distress is present, airway management takes priority over imaging studies.
3. Select the Correct Treatment
- Croup: Racemic epinephrine, corticosteroids, and supportive care.
- Epiglottitis: Immediate airway management followed by IV antibiotics.
Exam Hint: If a question asks for the first-line intervention in epiglottitis and one of the options is immediate intubation, that is usually the correct answer.
4. Avoid Common Pitfalls
- Do not attempt throat examination with a tongue depressor in suspected epiglottitis.
- Do not delay airway management in severe epiglottitis.
- Do not give antibiotics for croup, since it is viral.
Take our free course to learn essential tips, insights, and strategies to pass the Clinical Simulation Exam (CSE) on your first (or next) attempt.
Key Takeaway
- Croup is typically viral and managed with racemic epinephrine, corticosteroids, and supportive care.
- Epiglottitis is a bacterial emergency requiring immediate airway management and IV antibiotics.
- When epiglottitis is suspected, securing the airway always takes priority over diagnostic testing.
How to Instantly Recognize Croup vs Epiglottitis on the Board Exam
Board exam questions often describe a pediatric patient with stridor and respiratory distress, then ask you to determine the most likely condition or the correct intervention. A quick way to differentiate between croup and epiglottitis is to focus on the onset, cough, drooling, and patient positioning.
Use the following quick recognition strategy:
- Barking cough present: Think croup.
- Drooling and difficulty swallowing: Think epiglottitis.
- Gradual symptom onset: More consistent with croup.
- Sudden severe distress with high fever: Suggests epiglottitis.
- Child sitting forward in tripod position: Strong indicator of epiglottitis.
Another useful memory tip is:
- Croup = Cough (barking cough and stridor)
- Epiglottitis = Emergency (rapid airway obstruction requiring immediate airway management)
Note: Recognizing these patterns quickly will help you select the correct diagnosis and intervention when answering board exam questions.
Get instant access to four premium courses designed to help you pass the TMC/CSE exams—CSE Boost Course, TMC Test Bank, TMC Exam Hacks, and Daily Practice Questions. Bundle and save with everything you need for exam success.
Final Thoughts
For respiratory therapists preparing for the board exam, understanding the differences between croup and epiglottitis is essential. Although both conditions involve upper airway obstruction, their causes, progression, and treatment strategies differ significantly.
Croup generally develops gradually and responds well to medications that reduce airway inflammation. Epiglottitis, however, progresses rapidly and requires immediate airway management to prevent life-threatening obstruction.
By recognizing these key distinctions, you can confidently answer exam questions while also preparing to respond effectively in real-world clinical situations.
For more exam preparation strategies and practice resources, explore the materials included in our TMC/CSE Bundle, which provides comprehensive tools to help you achieve a passing score.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Tibballs J, Watson T. Symptoms and signs differentiating croup and epiglottitis. J Paediatr Child Health. 2011.




