A fenestrated tracheostomy tube is a specialized airway device designed to help certain tracheostomy patients breathe through the upper airway, speak more effectively, and progress toward possible decannulation.
Unlike a standard tracheostomy tube, it contains an opening called a fenestration that allows air to move from the trachea toward the larynx and vocal cords.
This makes it especially useful during tracheostomy weaning, upper airway assessment, and communication training. However, safe use requires careful attention to cuff deflation, tube position, airway patency, and patient monitoring.
What is a Fenestrated Tracheostomy Tube?
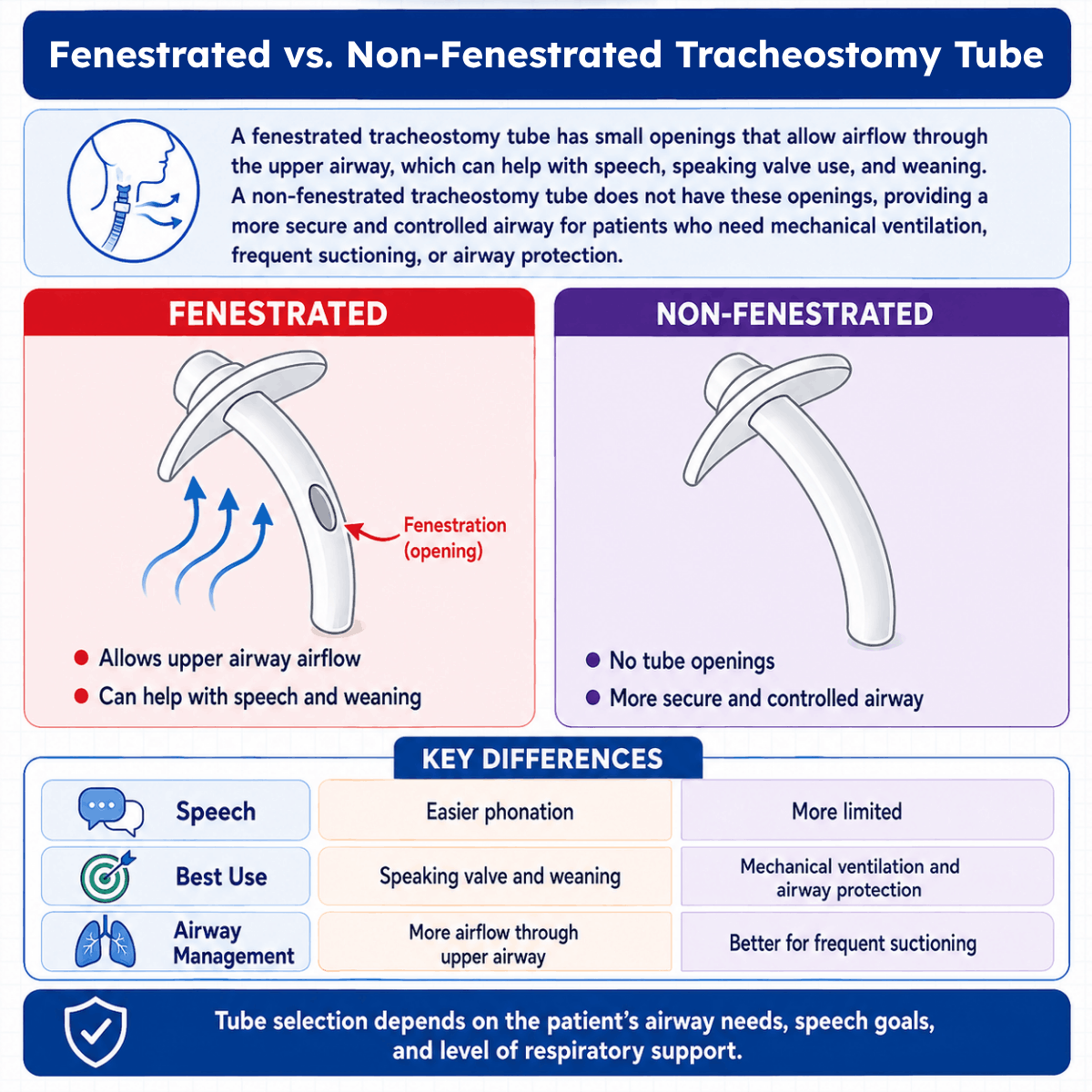
A fenestrated tracheostomy tube is a tracheostomy tube that contains one or more openings in the outer cannula. These openings are called fenestrations. The fenestration is usually located on the posterior wall of the outer cannula above the cuff.
The purpose of the fenestration is to allow airflow to pass from the trachea into the upper airway. This means air can move upward through the larynx and across the vocal cords instead of only moving in and out through the tracheostomy tube.
In simple terms, a fenestrated tracheostomy tube gives air another pathway. A standard tracheostomy tube primarily directs airflow through the tube itself. A fenestrated tube can direct airflow through the tube or through the patient’s natural upper airway, depending on how it is configured.
This design is especially helpful for patients who are improving and may no longer need full-time ventilatory support. It may also be used for patients who need to communicate during the day but still require mechanical ventilation at night.
Basic Structure
Most fenestrated tracheostomy tubes are dual-cannula tubes. This means they have an outer cannula and an inner cannula.
The outer cannula is the main tube that sits inside the trachea. It contains the fenestration, which is the opening that allows air to pass into the upper airway. The outer cannula also usually includes a flange, cuff, inflation line, pilot balloon, and standard 15-mm adapter.
The inner cannula slides into the outer cannula and locks into place. In many fenestrated tracheostomy tubes, the inner cannula blocks the fenestration when it is inserted. When the inner cannula is removed, the fenestration is opened.
This is an important concept. The fenestration does not function properly if it is blocked by the inner cannula. To allow airflow through the opening, the clinician usually removes the inner cannula and deflates the cuff. The outer opening of the tube may then be capped, plugged, or fitted with a speaking valve, depending on the clinical goal.
Note: Some fenestrated tubes may have a fenestrated inner cannula, which allows airflow through the fenestration even while the inner cannula remains in place. However, the specific setup depends on the type of tube being used.
How a Fenestrated Tracheostomy Tube Works
A fenestrated tracheostomy tube works by redirecting airflow through the upper airway.
- With a regular tracheostomy tube, air tends to enter and leave through the tracheostomy tube. This bypasses the nose, mouth, pharynx, larynx, and vocal cords. Because air does not pass normally through the vocal cords, speech is difficult or impossible.
- With a fenestrated tube, air can pass through the opening in the outer cannula and move upward through the larynx. When air passes across the vocal cords, the patient may be able to produce speech.
The basic process usually works like this:
The cuff is deflated, the inner cannula is removed, and the outer opening of the tube is plugged or capped. Once this occurs, air can move through the fenestration and around the tube. This allows air to travel through the upper airway.
Note: This setup can help the patient breathe more normally through the mouth and nose. It can also allow speech, improve airflow through the larynx, support secretion clearance, and help clinicians assess whether the upper airway is open enough for decannulation.
Standard Tracheostomy Tube vs. Fenestrated Tracheostomy Tube
A standard tracheostomy tube provides an artificial airway through the neck directly into the trachea. It may be used to bypass upper airway obstruction, provide access for suctioning, support mechanical ventilation, or help protect the airway when the cuff is inflated.
A fenestrated tracheostomy tube can do many of the same things, but it has an additional function. The fenestration allows air to move through the upper airway when the tube is properly configured.
This makes the fenestrated tube more useful during recovery and weaning. It can help determine whether a patient can tolerate upper airway breathing. It can also help restore speech in selected patients.
Note: The key difference is that a standard nonfenestrated tube does not have an opening in the outer cannula for airflow into the upper airway. A fenestrated tube does.
Main Purposes of a Fenestrated Tracheostomy Tube
Fenestrated tracheostomy tubes are used for several important clinical reasons. These include speech, upper airway assessment, weaning, and decannulation readiness.
One of the most common reasons is to help the patient speak. When air is redirected upward through the larynx, it can pass across the vocal cords. This allows phonation, which is the production of voice.
Another important purpose is to assess upper airway patency. If the patient can breathe through the upper airway while the tube is capped or used with a speaking valve, this suggests that the airway may be open enough to support normal breathing.
Fenestrated tubes can also be useful during tracheostomy weaning. A patient who has been mechanically ventilated for a long time may not be ready for immediate decannulation. A fenestrated tube allows a gradual transition by maintaining tracheostomy access while permitting upper airway breathing.
Note: This can be especially helpful for patients who can breathe spontaneously for extended periods but still require mechanical ventilation at certain times, such as during sleep.
Role in Speech and Communication
One of the major benefits of a fenestrated tracheostomy tube is its ability to help restore speech.
Patients with a tracheostomy often struggle to communicate because airflow bypasses the vocal cords. Even when the patient is awake, alert, and able to form words, sound may not be produced if air is not moving through the larynx.
A fenestrated tube can help solve this problem by allowing air to move upward through the vocal cords. When the cuff is deflated, the inner cannula is removed, and the tube is capped or fitted with a speaking valve, air can move through the fenestration and upper airway.
This allows the patient to talk, cough more naturally, and participate more actively in care. For many patients, the ability to speak can reduce anxiety and improve cooperation with treatment. Speech is not just a comfort issue. It can also improve safety. A patient who can communicate may be able to report pain, shortness of breath, secretion buildup, nausea, anxiety, or worsening respiratory distress.
Fenestrated Tubes and Speaking Valves
A speaking valve is a one-way valve that attaches to the external opening of a tracheostomy tube. It allows air to enter through the tracheostomy tube during inhalation, but it blocks air from leaving through the tube during exhalation.
Because exhaled air cannot exit through the tracheostomy tube, it must move upward through the larynx and out through the mouth or nose. This airflow across the vocal cords allows speech.
Speaking valves can be used with some standard tracheostomy tubes and some fenestrated tracheostomy tubes. However, safe use depends on proper airflow.
With a cuffed standard tracheostomy tube, the cuff must be completely deflated before a speaking valve is placed. If the cuff remains inflated, exhaled air may have no route to escape. This can cause air trapping, respiratory distress, and potentially dangerous airway obstruction.
With a fenestrated tracheostomy tube, the fenestrations must be open. This may require removing a nonfenestrated inner cannula or using a fenestrated inner cannula. The key point is that exhaled air must have a clear pathway through the upper airway.
Note: Speaking valves should be used only when the patient can move air adequately around the tube or through the fenestration. The patient must be monitored closely for distress, oxygen desaturation, increased work of breathing, and changes in vital signs.
Role in Decannulation
Decannulation means removal of the tracheostomy tube. A fenestrated tracheostomy tube can be useful during the process of determining whether a patient is ready for decannulation.
Before a tracheostomy tube is removed, the clinician must determine whether the patient can breathe through the upper airway, manage secretions, protect the airway, and maintain adequate ventilation and oxygenation.
A fenestrated tube helps with this assessment because it allows airflow through the upper airway while still keeping the tracheostomy tube in place. If the patient does well while the tube is capped, plugged, or used with a speaking valve, this suggests that the upper airway may be patent enough for decannulation.
However, tolerating a fenestrated tube does not automatically mean the patient is ready for decannulation. The clinician must assess the full clinical picture.
The patient should have adequate respiratory muscle strength, an effective cough, manageable secretions, a patent upper airway, and an adequate swallow. The patient should also be free from severe respiratory distress and should ideally not have an active pulmonary infection that would make secretion clearance more difficult.
Note: In some cases, bronchoscopy may be used to directly assess the upper airway and confirm tube position.
Role in Tracheostomy Weaning
Some patients can have a tracheostomy removed in one step, especially if the original reason for the tracheostomy has resolved. For example, if a patient had a tracheostomy because of upper airway obstruction and the obstruction is no longer present, the tube may be removed when the patient is clinically stable.
Other patients need a gradual weaning process. This is common in patients who have been mechanically ventilated for an extended period.
These patients may have respiratory muscle weakness, difficulty handling increased anatomic dead space, retained secretions, or impaired glottic function. They may tolerate spontaneous breathing for part of the day but still need ventilatory support at night.
A fenestrated tracheostomy tube is useful in this situation because it allows flexibility. During the day, the inner cannula can be removed, the cuff can be deflated, and the patient can breathe through the upper airway. At night, the inner cannula can be reinserted and the cuff inflated if mechanical ventilation is needed.
Note: This makes the fenestrated tube a transitional airway. It allows the patient to practice more natural breathing while still preserving a secure route for suctioning and ventilatory support.
Example Clinical Scenario
Consider a patient recovering from a neuromuscular condition such as Guillain-Barré syndrome. The patient is awake and improving. They can breathe spontaneously for several hours during the day but still require mechanical ventilation while sleeping.
If the patient has a single-cannula tracheostomy tube, they may not be able to breathe effectively through the upper airway or speak during the day. Removing the tracheostomy tube during the day and reinserting it at night would be too aggressive and could damage tracheal tissue.
In this situation, a fenestrated tracheostomy tube may be recommended. During the day, the cuff can be deflated and the inner cannula removed, allowing the patient to breathe through the upper airway and speak. At night, the inner cannula can be replaced and the cuff inflated so mechanical ventilation can be resumed.
This type of scenario is important for respiratory therapy students because it reflects how fenestrated tubes may appear in board-style questions. The improving patient who can breathe spontaneously during the day but needs nighttime ventilation is a classic clue.
Proper Use and Basic Sequence
The proper sequence for using a fenestrated tracheostomy tube depends on the specific tube and the clinical goal. However, when the goal is to allow upper airway airflow with tube plugging, the general sequence is:
First, deflate the cuff completely. Second, remove the inner cannula if it blocks the fenestration. Third, plug or cap the tube as ordered and clinically appropriate.
This sequence matters because the patient must have a route for air to move in and out. If the tube is plugged while the cuff is inflated, air may not be able to pass through the upper airway. This can lead to respiratory distress.
Note: When mechanical ventilation is resumed, the plug is removed, the inner cannula is replaced, and the cuff is inflated as needed. This closes the fenestration and allows the tube to function more like a standard tracheostomy tube.
Patient Assessment Before Use
Before using a fenestrated tracheostomy tube for upper airway breathing, speech, or decannulation assessment, the patient must be evaluated carefully.
The clinician should assess respiratory status, oxygenation, ventilation, secretion burden, cough strength, airway patency, and level of consciousness. The patient should be able to tolerate cuff deflation and should not have severe airway obstruction.
An effective cough is important because the patient must be able to clear secretions. If secretions are thick, copious, or difficult to manage, the patient may not tolerate plugging or decannulation well.
Swallowing ability should also be considered. Poor swallowing increases the risk of aspiration, which can worsen respiratory status and delay weaning.
The upper airway must be patent. If the patient has laryngeal stenosis, vocal cord paralysis, severe tracheal stenosis, or another obstruction, redirecting airflow through the upper airway may cause distress.
Note: In some cases, bronchoscopy may be needed to evaluate the airway and confirm that the fenestration is positioned correctly.
Monitoring During Use
Patients using a fenestrated tracheostomy tube should be monitored carefully, especially when the tube is first capped or fitted with a speaking valve. The clinician should observe the patient’s respiratory rate, heart rate, oxygen saturation, work of breathing, comfort level, ability to speak, and ability to exhale. Signs of distress should be taken seriously.
Warning signs may include increased respiratory rate, accessory muscle use, anxiety, inability to exhale, oxygen desaturation, tachycardia, cyanosis, stridor, or visible discomfort.
Tracheal pressure during exhalation may be measured when a speaking valve is in place. If expiratory pressure is elevated, this may suggest excessive resistance to airflow. Possible causes include a tube that is too large, poor tube position, incomplete cuff deflation, or upper airway obstruction.
Note: If the patient does not tolerate the valve or plug, it should be removed and the airway should be reassessed.
Safety Considerations
Safety is one of the most important parts of fenestrated tracheostomy tube management.
The cuff must be completely deflated before plugging the tube unless the specific device and clinical situation allow otherwise under expert supervision. In most basic clinical and exam situations, cuff deflation before plugging is the key rule.
If the cuff is inflated while the tube is plugged, the patient may be unable to exhale. This can cause air trapping, respiratory distress, and airway obstruction.
The tube should also be checked before insertion. The cuff should be tested to make sure it inflates and holds pressure properly. The inner cannula, obturator, and plug should fit correctly and should be easy to insert and remove.
A tube with a leaking cuff or faulty valve should not be used.
Secretions, blood, mucus plugs, or foreign material can obstruct the tube. If the patient develops distress, suctioning may be needed. If a suction catheter cannot pass through the tube and the patient is in distress, the tube may need to be removed and replaced by qualified personnel.
Common Problems
One of the most common problems specific to fenestrated tracheostomy tubes is malposition of the fenestration.
The fenestration may be pressed against the tracheal wall or positioned incorrectly between the skin and stoma. If the opening is not aligned within the tracheal lumen, airflow may be impaired.
This can cause respiratory distress, especially when the tube is capped or plugged. If malposition is suspected, the tube may need to be repositioned under bronchoscopic visualization.
Another problem is incomplete cuff deflation. If the cuff is not fully deflated before plugging or speaking valve placement, exhaled air may not be able to escape. This is a serious safety issue and should be checked immediately if the patient develops distress.
Soft tissue can also obstruct the fenestration. If soft tissue blocks the opening, the clinician may feel resistance when trying to insert the inner cannula. The inner cannula should never be forced if abnormal resistance is felt. Forcing it may damage tissue. Instead, the cannula should be withdrawn and the physician or appropriate provider should be notified.
Fenestrated Tube and Positive Pressure Ventilation
A fenestrated tracheostomy tube can sometimes be used in patients who still require mechanical ventilation. However, the tube must be configured correctly.
When positive pressure ventilation is needed, the inner cannula is usually inserted to block the fenestration, and the cuff may be inflated to create a seal. This allows the tube to function more like a standard cuffed tracheostomy tube.
If the fenestration remains open during ventilation, air leak may occur. This can affect delivered tidal volume, PEEP, and ventilator alarms. In some cases, ventilator settings or alarm limits may need adjustment, but this must be done carefully.
Patients using speaking valves during mechanical ventilation require close monitoring. Vital signs and oxygen saturation should be watched closely. Deterioration may indicate airway obstruction, excessive leak, inadequate ventilation, or speaking valve malfunction.
Contraindications and Patient Selection
A fenestrated tracheostomy tube is not appropriate for every patient. It should be used only when the patient can move air safely through the upper airway. Patients with severe upper airway obstruction, laryngeal stenosis, vocal cord paralysis, or severe tracheal stenosis may not tolerate airflow redirection.
It may also be inappropriate for patients with excessive secretions, poor cough, unstable respiratory status, impaired airway protection, or poor level of consciousness.
A patient who cannot tolerate cuff deflation may not be ready for a fenestrated tube setup aimed at speech or upper airway breathing. Likewise, a patient with severe oxygenation or ventilation problems may require more stable airway support before trying a speaking valve or tube plugging.
Note: The decision should be based on careful assessment, provider orders, and institutional policy.
Advantages
A fenestrated tracheostomy tube offers several advantages for selected patients. It can help restore airflow through the upper airway. This supports speech, smell, cough effectiveness, and more normal breathing patterns.
It can help assess upper airway patency before decannulation. If the patient tolerates capping or a speaking valve, this provides useful information about readiness for further weaning.
It can also support a gradual transition away from mechanical ventilation. The patient can breathe through the upper airway during the day while still maintaining tracheostomy access for suctioning or nighttime ventilation.
Another advantage is psychological. Patients who can speak often feel less isolated and more involved in their care. Communication can improve comfort, reduce anxiety, and help the healthcare team better understand the patient’s needs.
Disadvantages and Risks
Despite its benefits, a fenestrated tracheostomy tube has important risks. The fenestration can become malpositioned or obstructed. If the opening is against the tracheal wall or soft tissue, airflow may be limited and the patient may develop distress.
The tube can be more complex to manage than a standard tracheostomy tube. Staff must understand when to remove or replace the inner cannula, when to deflate the cuff, and when to plug or unplug the tube.
There is also a risk of air trapping if the tube is plugged while the cuff remains inflated. This is one of the most important safety concerns.
Secretions can obstruct the airway, and patients may require suctioning. If a suction catheter cannot pass and the patient is in distress, the tube may need urgent replacement.
Note: Because of these risks, fenestrated tubes should be used only with careful monitoring and proper training.
Key Takeaways
For respiratory therapy students, fenestrated tracheostomy tubes are a high-yield airway management topic. The most important point is that a fenestrated tube allows airflow through the upper airway. This makes speech possible and helps assess airway patency.
Another important point is the relationship between the inner cannula and the fenestration. In many tubes, removing the inner cannula opens the fenestration. Reinserting the inner cannula closes it and allows the tube to function more like a standard tracheostomy tube.
The classic sequence for plugging a fenestrated tube is to deflate the cuff, remove the inner cannula, and plug the tube.
If a patient becomes distressed after the tube is plugged, check the cuff first. If the cuff is inflated, it must be deflated so air can pass through the upper airway.
If resistance is felt while inserting the inner cannula, do not force it. This may indicate soft tissue obstruction of the fenestration.
For board-style questions, look for clues such as an improving patient, spontaneous breathing during the day, need for nighttime ventilation, desire to speak, and possible decannulation. These clues often point toward a fenestrated tracheostomy tube.
Fenestrated Tracheostomy Tube Practice Questions
1. What is a fenestrated tracheostomy tube?
A fenestrated tracheostomy tube is a specialized tracheostomy tube with an opening in the outer cannula that allows air to pass from the trachea into the upper airway.
2. What is the opening in a fenestrated tracheostomy tube called?
The opening is called a fenestration.
3. Where is the fenestration usually located?
The fenestration is usually located in the posterior wall of the outer cannula above the cuff.
4. What is the main purpose of the fenestration?
The main purpose is to allow airflow through the upper airway, especially toward the larynx and vocal cords.
5. How does a fenestrated tracheostomy tube help with speech?
It allows air to pass upward through the larynx and across the vocal cords, making phonation possible.
6. What happens when the inner cannula is inserted in many fenestrated tubes?
The inner cannula blocks the fenestration, causing the tube to function more like a standard tracheostomy tube.
7. What happens when the inner cannula is removed?
Removing the inner cannula opens the fenestration, allowing air to pass through the opening into the upper airway.
8. Why must the cuff be deflated before plugging a fenestrated tracheostomy tube?
The cuff must be deflated so air can move through the upper airway. If the cuff remains inflated, the patient may not be able to exhale properly.
9. What is the correct sequence for plugging a fenestrated tracheostomy tube?
The correct sequence is to deflate the cuff, remove the inner cannula, and plug the tube.
10. What can happen if a fenestrated tracheostomy tube is plugged while the cuff is inflated?
The patient may develop air trapping, respiratory distress, or an inability to exhale.
11. How can a fenestrated tracheostomy tube assist with decannulation?
It helps clinicians assess whether the patient can tolerate airflow through the upper airway before the tracheostomy tube is removed.
12. What does decannulation mean?
Decannulation means removal of the tracheostomy tube.
13. Why is upper airway patency important before decannulation?
The upper airway must be open enough to allow adequate airflow after the tracheostomy tube is removed.
14. What patient ability is important for secretion clearance before decannulation?
The patient should have enough muscle strength to generate an effective cough.
15. What peak expiratory pressure suggests an effective cough before decannulation?
A peak expiratory pressure greater than 40 cm H₂O suggests an effective cough.
16. Why are thick or excessive secretions a concern before decannulation?
Thick or excessive secretions may be difficult for the patient to clear and can increase the risk of airway obstruction or respiratory distress.
17. What is one major communication benefit of a fenestrated tracheostomy tube?
It can allow the patient to speak by redirecting airflow through the vocal cords.
18. What is a speaking valve?
A speaking valve is a one-way valve placed on the external opening of a tracheostomy tube that allows inhalation but redirects exhalation through the upper airway.
19. What must be done before placing a speaking valve on a cuffed tracheostomy tube?
The cuff must be completely deflated before placing the speaking valve.
20. Why is a speaking valve dangerous if the cuff is inflated?
Because the valve blocks exhalation through the tracheostomy tube, and an inflated cuff may prevent exhaled air from escaping through the upper airway.
21. What should clinicians monitor after placing a speaking valve?
They should monitor heart rate, respiratory rate, oxygen saturation, work of breathing, and the patient’s ability to exhale.
22. What does elevated tracheal pressure during exhalation with a speaking valve suggest?
It may suggest increased resistance to exhalation caused by a large tube, poor tube position, incomplete cuff deflation, or upper airway obstruction.
23. What tracheal pressure value may indicate excessive expiratory resistance with a speaking valve?
A tracheal pressure greater than 5 cm H₂O may indicate excessive expiratory resistance.
24. What is one common problem specific to fenestrated tracheostomy tubes?
A common problem is malposition of the fenestration.
25. What does malposition of the fenestration mean?
It means the fenestration is not properly aligned within the tracheal lumen, which can impair airflow and cause respiratory distress.
26. Where can a fenestration become incorrectly positioned?
The fenestration may be positioned between the skin and stoma or pressed against the posterior tracheal wall.
27. What should be done if fenestration malposition is suspected?
The tube may need to be repositioned under bronchoscopic observation.
28. Why is bronchoscopy useful with a fenestrated tracheostomy tube?
Bronchoscopy allows direct visualization of the airway and helps confirm proper fenestration placement.
29. What can be adjusted if a fenestrated tube has an adjustable flange?
The flange position can be adjusted to help align the fenestration within the tracheal lumen.
30. What should the clinician do if abnormal resistance is felt while inserting the inner cannula?
The clinician should not force the inner cannula. It should be withdrawn, and the physician should be notified.
31. What may abnormal resistance during inner cannula insertion indicate?
It may indicate that soft tissue is obstructing the fenestration.
32. Why should the inner cannula not be forced when resistance is felt?
Forcing the inner cannula may damage tissue or worsen airway trauma.
33. How does reinserting the inner cannula change a fenestrated tracheostomy tube?
It closes or blocks the fenestration and allows the tube to function more like a standard tracheostomy tube.
34. When may positive-pressure ventilation be resumed through a fenestrated tracheostomy tube?
Positive-pressure ventilation may be resumed after the inner cannula is replaced and the cuff is inflated as needed.
35. Why is a fenestrated tracheostomy tube considered a transitional airway?
It maintains tracheostomy access while allowing upper-airway breathing, speech, and assessment for possible decannulation.
36. What type of patient may benefit from a fenestrated tracheostomy tube during weaning?
A patient who is improving, breathing spontaneously for extended periods, but still needs ventilatory support at certain times may benefit.
37. Why might a patient who needs nighttime ventilation benefit from a fenestrated tube?
The patient can breathe and speak through the upper airway during the day, then use the tube for mechanical ventilation at night.
38. Why is removing and reinserting a tracheostomy tube each day usually inappropriate?
It can damage tracheal tissue and leaves the patient without a secure airway if respiratory status worsens.
39. Why might replacing a tracheostomy tube with a smaller tube not always be the best choice?
A smaller tube can increase airway resistance and work of breathing, which may fatigue the patient.
40. What is one board-style clue that points to a fenestrated tracheostomy tube?
An improving patient who breathes spontaneously during the day but still requires mechanical ventilation at night is a clue.
41. How does a fenestrated tube differ from a speaking-type tracheostomy tube?
A fenestrated tube allows upper-airway breathing through the fenestration, while a speaking-type tube may use another mechanism to permit speech.
42. What is the role of the outer cannula plug?
The plug prevents the patient from breathing through the proximal opening of the tube while still allowing airflow through the fenestration.
43. Does the outer cannula plug cover the fenestration?
No. The plug covers the proximal tube opening but does not cover the fenestration.
44. Why can a plugged fenestrated tube allow speech?
When the tube is plugged, air is redirected through the fenestration and upper airway, allowing it to pass across the vocal cords.
45. What should be checked before inserting a fenestrated tracheostomy tube?
The cuff should be tested, and the obturator, inner cannula, and plug should be checked for proper fit.
46. How is the cuff tested before insertion?
The cuff is inflated with a syringe, checked to make sure it holds air, and then deflated before insertion.
47. What should be done if the cuff or one-way valve leaks?
The tube should not be used.
48. What can obstruct a fenestrated tracheostomy tube?
Secretions, blood, mucus plugs, foreign material, or soft tissue can obstruct the tube or fenestration.
49. What should be done if secretions obstruct the tube?
Suctioning should be performed to remove the obstruction.
50. What may be necessary if a suction catheter cannot pass through the tube and the patient is in distress?
The tracheostomy tube may need to be removed and replaced by qualified personnel.
51. What is the primary airflow pattern created by a fenestrated tracheostomy tube?
A fenestrated tracheostomy tube redirects airflow from the trachea through the fenestration and upward through the upper airway.
52. Why does airflow through the larynx matter for a tracheostomy patient?
Airflow through the larynx allows air to pass across the vocal cords, which is necessary for speech.
53. What happens to normal speech when airflow bypasses the vocal cords?
Speech is reduced or absent because air is not moving across the vocal cords to produce sound.
54. Why may a fenestrated tube improve a patient’s ability to expectorate secretions?
It helps restore airflow through the upper airway, allowing the patient to cough and clear secretions more naturally.
55. What is the relationship between a fenestrated tube and upper airway function?
A fenestrated tube helps clinicians assess whether the patient can move air through the upper airway effectively.
56. Why is upper airway assessment important in tracheostomy weaning?
It helps determine whether the patient may tolerate breathing through the natural airway without the tracheostomy tube.
57. What patient condition may delay successful decannulation after long-term mechanical ventilation?
Respiratory muscle weakness may delay successful decannulation.
58. Why can increased anatomic dead space be a problem during tracheostomy weaning?
The patient may have difficulty adjusting to the increased volume of air that must be moved during upper airway breathing.
59. How can retained secretions affect tracheostomy weaning?
Retained secretions can increase airway obstruction risk and make it harder for the patient to tolerate decannulation.
60. Why are glottic closure problems important before decannulation?
Glottic closure problems may interfere with airway protection and effective breathing through the upper airway.
61. What is one reason a patient with a resolved upper airway obstruction may be decannulated more quickly?
If the original obstruction has resolved and the patient is stable, the tube may sometimes be removed without a prolonged weaning process.
62. What is a tracheostomy button?
A tracheostomy button is a device that may be used during tracheostomy weaning to help maintain stoma access while assessing breathing through the upper airway.
63. What are progressively smaller tracheostomy tubes used for?
They may be used during weaning to gradually increase upper airway airflow and assess tolerance before decannulation.
64. Why is an adequate swallow important before decannulation?
An adequate swallow helps reduce the risk of aspiration after the tracheostomy tube is removed.
65. Why should active pulmonary infection be considered before decannulation?
An active pulmonary infection may increase secretions and respiratory workload, making decannulation less likely to succeed.
66. What does manageable secretion thickness suggest?
It suggests the patient may be better able to clear secretions and tolerate tracheostomy weaning.
67. What is the benefit of maintaining tracheostomy access while using a fenestrated tube?
It allows suctioning, airway access, and possible ventilatory support while the patient practices upper airway breathing.
68. Why is a fenestrated tracheostomy tube useful for a patient who is awake and alert?
It may allow the patient to communicate more effectively by permitting speech.
69. How can speech improve patient care?
Speech allows the patient to report symptoms, discomfort, anxiety, secretion problems, or worsening shortness of breath.
70. What emotional benefit can speech provide for a tracheostomy patient?
Speech can reduce frustration and anxiety by allowing the patient to communicate with caregivers and family.
71. What is the Blom fenestrated tracheostomy tube designed to do?
It is designed to allow certain ventilator-dependent patients to speak, even when the cuff is fully inflated.
72. What special component does the Blom fenestrated tracheostomy tube use?
It uses a special speech cannula with valve mechanisms that control airflow through the fenestrations.
73. What happens during inhalation with the Blom fenestrated tracheostomy tube?
During inhalation, the flap valve opens and the bubble valve expands, blocking the fenestrations.
74. What happens during exhalation with the Blom fenestrated tracheostomy tube?
During exhalation, the flap valve closes and the bubble valve collapses, allowing air to pass through the fenestrations for speech.
75. Why can communication be especially important for ventilator-dependent patients?
Communication helps ventilator-dependent patients participate in care, express needs, and improve comfort and quality of life.
76. What is the main difference between a traditional tracheostomy tube and a fenestrated tracheostomy tube?
A traditional tracheostomy tube does not have an opening for upper airway airflow, while a fenestrated tube has an opening that allows air to pass toward the larynx.
77. What does the term phonation mean?
Phonation means voice production, which occurs when air passes through the vocal cords.
78. Why does a fenestrated tube help restore a more normal airflow pattern?
It allows air to move through the upper airway instead of only entering and exiting through the tracheostomy tube.
79. What is the purpose of capping the proximal opening of a fenestrated tracheostomy tube?
Capping the proximal opening redirects airflow through the fenestration and upper airway.
80. What must be true before capping a fenestrated tracheostomy tube?
The cuff must be fully deflated, and the patient must be able to move air through the upper airway.
81. What is one reason a patient may fail to tolerate a capped fenestrated tube?
The patient may have upper airway obstruction, tube malposition, incomplete cuff deflation, or excessive airway resistance.
82. Why is a fenestrated tube not appropriate for every tracheostomy patient?
Some patients cannot move air safely through the upper airway due to obstruction, poor airway control, excessive secretions, or respiratory instability.
83. What upper airway condition may prevent safe use of a speaking valve?
Laryngeal stenosis may prevent safe use because it limits airflow through the upper airway.
84. Why is vocal cord paralysis a concern with speaking valve use?
Vocal cord paralysis can interfere with airflow and make phonation or exhalation through the upper airway difficult.
85. Why is severe tracheal stenosis a contraindication to speaking valve use?
Severe tracheal stenosis can create excessive resistance to airflow and increase the risk of respiratory distress.
86. What is the purpose of monitoring oxygen saturation after speaking valve placement?
Oxygen saturation helps determine whether the patient is maintaining adequate oxygenation after airflow is redirected.
87. What may oxygen desaturation after speaking valve placement indicate?
It may indicate airflow obstruction, valve malfunction, excessive leak, or inadequate ventilation.
88. Why should respiratory rate be monitored after plugging a fenestrated tube?
An increased respiratory rate may indicate increased work of breathing or poor tolerance of upper airway breathing.
89. Why should heart rate be monitored after speaking valve placement?
Tachycardia may be an early sign of respiratory distress, anxiety, hypoxemia, or increased work of breathing.
90. What does increased work of breathing suggest after a fenestrated tube is plugged?
It suggests that the patient may not be tolerating upper airway breathing or that airflow is being restricted.
91. What should be done if a patient becomes distressed after a speaking valve is placed?
The speaking valve should be removed, the airway should be assessed, and the cause of distress should be corrected.
92. What is one possible cause of high expiratory pressure with a speaking valve?
A tracheostomy tube that is too large can create excessive resistance to exhaled airflow.
93. How can poor tube position affect speaking valve tolerance?
Poor tube position can obstruct airflow around or through the tube, increasing expiratory resistance.
94. Why can incomplete cuff deflation cause problems during speaking valve use?
It can prevent exhaled air from passing around the tube and through the upper airway.
95. What tube change may help if expiratory resistance is too high?
Changing to a smaller tube, cuffless tube, or tight-to-shaft cuff tube may reduce resistance.
96. Why can a fenestrated tube help test upper airway control?
It allows clinicians to observe whether the patient can breathe, exhale, cough, and manage airflow through the natural airway.
97. What does successful tolerance of a plugged fenestrated tube suggest?
It suggests the patient may have adequate upper airway patency and may be progressing toward decannulation readiness.
98. Why should a warning tag be attached to the cap or plug of a fenestrated tube?
A warning tag reminds caregivers that the cuff must be deflated before the tube is plugged.
99. What is the most important safety rule when plugging a fenestrated tracheostomy tube?
The cuff must be completely deflated before the tube is plugged.
100. What is the key exam takeaway about fenestrated tracheostomy tubes?
Fenestrated tracheostomy tubes allow upper airway airflow for speech, airway assessment, weaning, and possible decannulation when used safely.
Final Thoughts
A fenestrated tracheostomy tube is a specialized airway device that helps selected patients transition toward upper airway breathing, speech, and possible decannulation. Its defining feature is the fenestration, an opening in the outer cannula that allows air to move toward the larynx and vocal cords.
When used correctly, it can improve communication and support tracheostomy weaning. However, it must be managed carefully.
The cuff must be deflated before plugging, the fenestration must be open and properly positioned, and the patient must be monitored for respiratory distress. Safe use depends on proper assessment, correct setup, and close observation.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Pandian V, Boisen SE, Mathews S, Cole T. Are Fenestrated Tracheostomy Tubes Still Valuable? Am J Speech Lang Pathol. 2019.

