Sleep apnea is a common yet frequently underdiagnosed sleep-related breathing disorder that affects millions of people worldwide. It is characterized by repeated interruptions in breathing during sleep, which can lead to significant health complications if left untreated.
Because sleep apnea directly impacts ventilation, oxygenation, and overall cardiopulmonary function, it holds great importance in respiratory care. Respiratory therapists play a crucial role in identifying, managing, and treating patients with this condition.
Understanding sleep apnea is essential for healthcare providers working to improve patient outcomes, quality of life, and long-term cardiopulmonary health.
What Is Sleep Apnea?
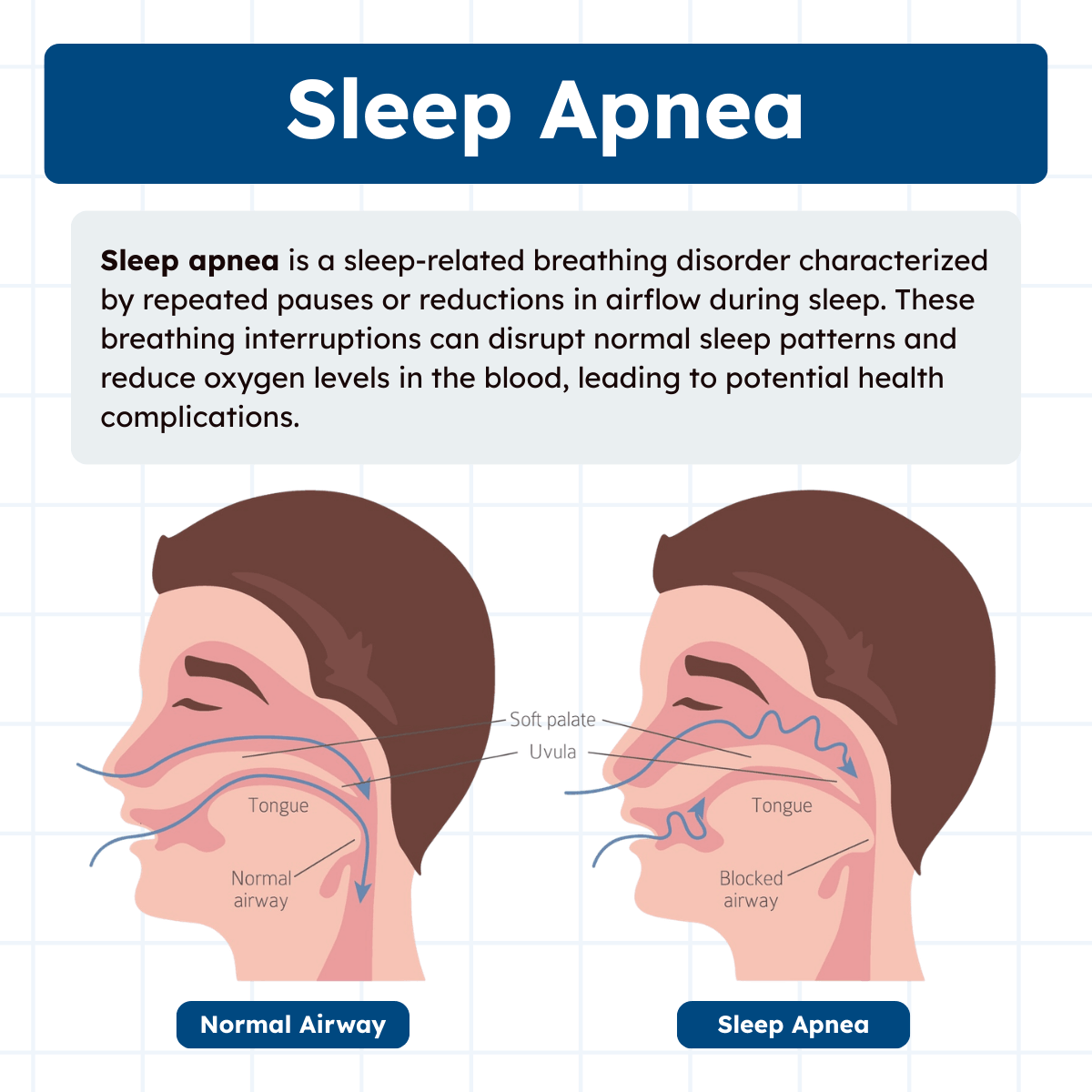
Sleep apnea is a disorder characterized by repeated episodes of airflow cessation or reduction during sleep. Apnea is defined as a complete cessation of airflow lasting at least 10 seconds, while hypopnea refers to a partial reduction in airflow that is often accompanied by oxygen desaturation or arousal from sleep. These repeated breathing disturbances disrupt normal sleep patterns and can cause decreased oxygen levels and increased carbon dioxide levels in the blood.
Sleep apnea can result in fragmented sleep, excessive daytime sleepiness, and impaired cognitive function. Over time, untreated sleep apnea can contribute to serious medical conditions, including cardiovascular disease, metabolic disorders, and respiratory complications. Because breathing is repeatedly interrupted, the body experiences increased stress responses, which can negatively affect multiple organ systems.
Types of Sleep Apnea
There are three primary types of sleep apnea: obstructive sleep apnea, central sleep apnea, and mixed sleep apnea. Each type has unique causes, pathophysiology, and treatment considerations.
Obstructive Sleep Apnea
Obstructive sleep apnea (OSA) is the most common form of sleep apnea and occurs when the upper airway becomes partially or completely blocked during sleep. This obstruction typically results from relaxation of the muscles that support the soft tissues of the throat, including the tongue and soft palate.
Patients with OSA often have anatomical or physiological factors that predispose them to airway collapse. These factors include obesity, enlarged tonsils, craniofacial abnormalities such as a recessed jaw, and increased soft tissue surrounding the airway. During wakefulness, muscle tone helps keep the airway open. However, during sleep, muscle tone decreases, allowing airway narrowing or collapse to occur.
OSA is strongly associated with loud snoring, witnessed breathing pauses, and excessive daytime sleepiness. The repeated airway collapse leads to intermittent hypoxemia, increased intrathoracic pressure, and frequent arousals from sleep. These disturbances can contribute to systemic inflammation, sympathetic nervous system activation, and cardiovascular strain.
Central Sleep Apnea
Central sleep apnea (CSA) is less common than OSA and occurs when the brain temporarily fails to send appropriate signals to the respiratory muscles. Unlike OSA, CSA is not caused by airway obstruction but rather by impaired respiratory drive.
CSA is often associated with underlying medical conditions such as stroke, heart failure, neuromuscular disorders, or chronic opioid use. Patients with CSA frequently demonstrate periodic breathing patterns, including Cheyne-Stokes respiration, which is characterized by alternating periods of increasing and decreasing breathing effort followed by apnea.
Because CSA involves abnormalities in ventilatory control, treatment often focuses on managing the underlying condition and providing ventilatory support through advanced positive airway pressure therapies.
Mixed Sleep Apnea
Mixed sleep apnea involves features of both obstructive and central sleep apnea. These episodes typically begin as central apneas and transition into obstructive events. Mixed sleep apnea requires careful evaluation to determine the most effective treatment strategy.
Risk Factors and Clinical Presentation
Several factors increase the risk of developing sleep apnea. Obesity is one of the most significant contributors, particularly when excess fat accumulates around the neck and upper airway. Other common risk factors include male gender, increasing age, large neck circumference, habitual snoring, hypertension, and genetic predisposition.
Patients with sleep apnea may present with a wide range of symptoms. Common nighttime symptoms include loud snoring, gasping or choking during sleep, restless sleep, and frequent awakenings. Daytime symptoms may include excessive sleepiness, fatigue, morning headaches, difficulty concentrating, irritability, and decreased work performance.
Importantly, not all patients with sleep apnea experience excessive daytime sleepiness, which can make diagnosis challenging. Some individuals may have severe disease with minimal symptoms, highlighting the importance of clinical screening and diagnostic testing.
Diagnosis of Sleep Apnea
The diagnosis of sleep apnea typically involves a combination of clinical assessment and sleep testing. Screening tools such as the STOP-BANG questionnaire help identify individuals at high risk for obstructive sleep apnea by evaluating factors such as snoring, tiredness, observed apneas, blood pressure, body mass index, age, neck circumference, and gender.
The gold standard diagnostic test for sleep apnea is polysomnography, commonly known as a sleep study. This test records multiple physiological variables during sleep, including brain activity, eye movements, muscle activity, airflow, oxygen saturation, heart rhythm, and respiratory effort.
Sleep apnea severity is commonly measured using the apnea-hypopnea index (AHI), which represents the number of apnea and hypopnea events per hour of sleep. Mild sleep apnea is defined as 5 to 14 events per hour, moderate sleep apnea as 15 to 30 events per hour, and severe sleep apnea as more than 30 events per hour.
Note: Home sleep testing is becoming increasingly common and provides a more convenient and cost-effective diagnostic alternative for certain patients.
Treatment and Management
Treatment for sleep apnea depends on the type and severity of the disorder, as well as patient-specific factors. Lifestyle modifications are often recommended as part of treatment, particularly for patients with OSA. Weight loss, avoidance of alcohol and sedative medications, and positional therapy can reduce airway obstruction during sleep.
Continuous positive airway pressure (CPAP) therapy is considered the first-line treatment for obstructive sleep apnea. CPAP delivers a constant flow of air through a mask to keep the airway open during sleep. This therapy is highly effective when patients use it consistently. However, long-term adherence can be challenging, requiring patient education and support.
Bilevel positive airway pressure (BiPAP) therapy may be recommended for patients who have difficulty tolerating CPAP or who require additional ventilatory support. Advanced therapies such as adaptive servo-ventilation are commonly used for central sleep apnea and complex sleep-disordered breathing.
Oral appliances can reposition the jaw or tongue to maintain airway patency in patients with mild to moderate obstructive sleep apnea. Surgical interventions, including upper airway stimulation and soft tissue surgery, may be considered for patients who do not respond to noninvasive therapies.
In patients with central sleep apnea, treatment often focuses on addressing the underlying medical condition. Supplemental oxygen, ventilatory support, and certain medications may help stabilize breathing patterns.
Relevance to Respiratory Therapists and Respiratory Care
Sleep apnea is highly relevant to respiratory therapists because it directly affects ventilation, gas exchange, and overall respiratory function. Respiratory therapists frequently participate in the diagnosis, treatment, and long-term management of patients with sleep-disordered breathing.
Respiratory therapists play a key role in performing and monitoring sleep studies, interpreting respiratory data, and assisting physicians in diagnosing sleep apnea. They are also responsible for initiating and titrating positive airway pressure therapy, selecting appropriate masks and interfaces, and educating patients on equipment use and maintenance.
Patient education is particularly important in improving adherence to therapy. Respiratory therapists help patients understand the benefits of treatment, troubleshoot equipment issues, and address barriers to compliance. Because adherence rates for CPAP therapy can be suboptimal, ongoing follow-up and patient support are essential components of care.
Additionally, respiratory therapists often encounter sleep apnea in patients with other respiratory conditions, such as chronic obstructive pulmonary disease. The coexistence of COPD and obstructive sleep apnea, known as overlap syndrome, is associated with increased morbidity and mortality. Early identification and treatment of sleep apnea in these patients can significantly improve clinical outcomes.
Note: Respiratory therapists also manage patients with neuromuscular disorders and hypoventilation syndromes who may develop sleep-related breathing disorders. Early detection and treatment with noninvasive ventilation can improve quality of life, gas exchange, and survival in these patient populations.
Sleep Apnea Practice Questions
1. What is a condition in which an individual stops breathing while asleep, causing a measurable decrease in blood oxygen levels?
Sleep apnea
2. What are the two main types of sleep apnea?
Obstructive sleep apnea and central sleep apnea
3. Which type of sleep apnea is caused by a blockage in the air passage due to relaxed airway muscles allowing the tongue and palate to block the airway?
Obstructive sleep apnea
4. Which type of sleep apnea is caused by a disorder in the respiratory control center of the brain?
Central sleep apnea
5. What factors increase the severity of sleep apnea and make it more common in men?
Obesity, hypertension, smoking, alcohol ingestion, and the use of sedatives
6. How is sleep apnea diagnosed?
When more than five periods of apnea, each lasting at least 10 seconds, occur during one hour of sleep
7. What effect do apnea periods have on blood oxygen levels?
They reduce the blood oxygen level.
8. What happens to an individual during an apnea event?
The brain awakens the individual, who then gasps for air and snores loudly.
9. What are the daytime consequences of sleep apnea?
Excessive tiredness and drowsiness
10. What are some treatment options for mild sleep apnea?
Losing weight, abstaining from smoking and the use of alcohol or sedatives, and sleeping on the side or stomach
11. How can an oral appliance help in the treatment of sleep apnea?
By maintaining airway patency if worn while sleeping
12. What device is used in more severe cases of obstructive sleep apnea to keep the airway open during sleep?
Continuous positive airway pressure (CPAP)
13. What components make up the CPAP device?
A mask fit securely against the face and tubing connected to a blower device
14. What surgical options are available if CPAP and other treatments are ineffective?
Maxillomandibular advancement surgery (MMA) and uvulopalatopharyngoplasty (UPPP)
15. What extreme measure might be taken in severe life-threatening cases of sleep apnea?
A tracheostomy (surgical opening in the neck)
16. What is the usual treatment for central sleep apnea?
Medications to stimulate breathing
17. What is the most common sleep-related breathing disorder that causes you to repeatedly stop and start breathing while you sleep?
Obstructive sleep apnea (OSA)
18. The most effective treatments for sleep apnea include all of the following EXCEPT:
The use of stimulant drugs.
19. Sleep apnea would be diagnosed in a patient who has which of these findings?
During a sleep study, obstructive sleep apnea (OSA) is confirmed when either of the following two conditions exists: 15 or more apneas, hypopneas, or RERAs per hour of sleep (i.e., the AHI or RDI >15 events/hour) in an asymptomatic patient. More than 75% of the apneas and hypopneas must be obstructive. Or, 5 or more apneas, hypopneas, or RERAs per hour of sleep (i.e., the AHI or RDI >5/hour events/hour) in patients with symptoms (e.g., sleepiness, fatigue, and inattention) or signs of disturbed sleep (e.g., snoring, restless sleep, and respiratory pauses). More than 75% of the apneas and hypopneas must be obstructive.
20. Signs and symptoms of sleep apnea include which of the following?
Loud snoring
21. What is the rationale for using CPAP to treat sleep apnea?
Positive air pressure holds the airway open
22. A 64-year-old obese man is admitted to the hospital for treatment of heart failure secondary to alcoholism. For which of the following negative consequences should you assess?
Obstructive sleep apnea: Factors associated with increased risk for OSA include obesity, diabetes, stroke, Parkinson’s disease, congestive heart failure, genetic predisposition, craniofacial anatomic features, and the use of alcohol or medications that depress the respiratory center.
23. Which problem is associated with obesity, heavy snoring, and shallow breathing?
Sleep apnea
24. A 45-year-old obese man has complaints of daytime sleepiness, difficulty going to sleep at night, and snoring. What is the patient exhibiting manifestation of?
Obstructive sleep apnea
25. A patient with severe sleep apnea has been prescribed continuous positive airway pressure (CPAP). A respiratory therapist adjusts the blower to maintain adequate positive pressure during inspiration and expiration. The respiratory therapist should maintain the pressure in what range?
The pressure required to maintain an adequate positive pressure is 5-25 cm of H2O. This range of pressure is essential to avoid collapse of the airway.
26. A patient’s partner informs the respiratory therapist that the patient wakes up with a startle and gasps for breath several times at night. The respiratory therapist understands the patient is experiencing sleep apnea. What are the common risk factors in this patient for sleep apnea?
The common risk factors for sleep apnea include a BMI greater than 28 kg/m2, a smoking habit, and a neck circumference greater than 17 inches. Sleep apnea is often observed in patients older than 65 years. Occasional consumption of alcohol is not a risk factor by itself.
27. A patient with sleep apnea asks the respiratory therapist, “What can I do to get better sleep?” What is an appropriate response?
“Being overweight is a contributing factor; losing weight can often resolve apnea.”
28. A patient with obstructive sleep apnea tells the respiratory therapist, “I just hate using this continuous positive airway pressure (CPAP) thing, but I know I need it. Is there anything I can do so that I don’t need to use it?” Which of these would be an appropriate suggestion?
Referral to a weight loss program.
29. A patient with sleep apnea is scheduled for surgery that involves excision of the tonsillar pillars, uvula, and posterior soft palate to remove the obstructing tissue. What is this surgery called?
Uvulopalatopharyngoplasty
30. The respiratory therapist is caring for a middle-aged man who complains of excessive daytime sleepiness. The examination reveals that the patient has large tonsils. He jokingly says that his wife complains that he snores. The respiratory therapist hypothesizes that the patient has which of the following disorders?
Obstructive sleep apnea
31. A patient with sleep apnea is given a noninvasive method of monitoring rest and activity cycles. The patient is required to wear a small watch device on the wrist. What is the name of this method?
Actigraphy is a noninvasive method of monitoring rest and activity cycles. In this method, a small actigraph watch is worn on the wrist to measure gross motor activity. An electromyogram records muscle tone. Polysomnography is also used to measure sleep apnea but through electrodes that record the main stages of sleep and wakefulness. Eye movements are recorded with an electrooculogram.
32. Which assessment question is most appropriate when the respiratory therapist is assessing a patient who is receiving care for suspected obstructive sleep apnea (OSA)?
“Do you smoke?”
33. What does hypopnea mean?
A 30% decrease in airflow with a greater or equal to 4% reduction in SaO2, causing arousals.
34. What is a polysomnogram?
A test performed to determine if a patient has sleep apnea, commonly referred to as a sleep study.
35. What is the Respiratory Disturbance Index (RDI) in sleep apnea?
The number of obstructive apneas, hypopneas, and central apneas per hour, used to diagnose sleep apnea. It is considered abnormal if greater than 5 per hour.
36. What is another name for the Respiratory Disturbance Index (RDI)?
Apnea-Hypopnea Index (AHI)
37. What is the most common type of sleep apnea?
Obstructive Sleep Apnea (OSA)
38. Which type of sleep apnea involves respiratory effort but little or no airflow due to upper airway obstruction?
Obstructive Sleep Apnea (OSA)
39. What are some causes of Obstructive Sleep Apnea (OSA)?
Obesity, tonsil or adenoid hypertrophy, a small or recessed chin, and sometimes nasal abnormalities.
40. What is the medical term for a small chin?
Micrognathia
41. What is the medical term for a recessed chin?
Retrognathia
42. What are the signs and symptoms of Obstructive Sleep Apnea (OSA)?
Excessive daytime sleepiness (EDS), lack of restful sleep, memory loss, poor concentration, irritability, fatigue, morning headaches, depression, frequent motor vehicle accidents, arrhythmias, stroke, congestive heart failure (CHF), snoring, choking, gasping, nocturnal reflux, systemic hypertension, hypoxemia, hypercapnia, polycythemia, pulmonary hypertension, and cor pulmonale.
43. OSA is associated with what issues in children?
Poor school performance, developmental delays, aggression, withdrawal, ADHD, and hyperinsulinemia.
44. What is the leading cause of pediatric sleep apnea?
Enlargement of the tonsils.
45. What does a polysomnogram measure?
Bodily functions during sleep, including EEG, EMG (muscle tone), electro-oculogram (EOG), EKG, airflow at the nose and mouth, chest wall effort, SpO2, and audio-visual recordings.
46. How is chest wall effort measured during a polysomnogram?
With an impedance monitor.
47. What is the major difference between OSA and hypopnea?
OSA involves the absence of airflow for 10 seconds with desaturation and increased effort (rib cage), while hypopnea involves a 30% decrease in airflow for 10 seconds with slight desaturation and minimal increase in rib cage effort.
48. What is central sleep apnea?
A condition where the brain fails to send proper signals, leading to no airflow due to a lack of respiratory effort, showing no effort in the rib cage, abdomen, or PES.
49. What causes central sleep apnea?
CNS lesions, stroke, or congestive heart failure (CHF).
50. Which type of sleep apnea is least common?
Central sleep apnea, accounting for 10-15% of all sleep disorders.
51. What is mixed apnea?
A combination of both central and obstructive apnea, generally starting with central sleep apnea followed by upper airway obstruction.
52. What is the effort and airflow pattern in mixed apnea?
No airflow and little effort.
53. What are common treatments for sleep apnea?
Losing weight, stopping alcohol, tobacco, and sedative use, sleeping on your side, elevating the head of the bed, maintaining regular sleep hours, using nasal dilators or saline spray, CPAP, tonsillectomy and adenoidectomy, UPPP (uvulopalatopharyngoplasty), tracheostomy, and orthodontic devices to pull the lower jaw forward.
54. What is the compliance therapy benefit for CPAP?
If used for more than 4 hours per night for 70% of nights.
55. What are common CPAP problems?
Mask discomfort, air leaks, and rhinitis or congestion.
56. What are the reimbursement criteria for CPAP?
An AHI greater than or equal to 15/hour, or an AHI between 5-14 with excessive daytime sleepiness, impaired cognition, mood disorders, hypertension, history of heart disease, or stroke.
57. When would NIPPV be used?
For nocturnal hypoventilation or when lower expiratory pressure may improve compliance to therapy.
58. What sleep-related disorder is quite common and may cause significant mortality and morbidity?
Sleep apnea
59. What percentage of women have obstructive sleep apnea?
4%
60. What percentage of men have obstructive sleep apnea?
9%
61. Sleep apnea is about as common as which condition?
Asthma
62. What does obstructive sleep apnea (OSA) largely contribute to?
Lost productivity at work and vehicular accidents
63. Which sleep apnea occurs when the respiratory centers of the medulla fail to send signals to the respiratory muscles?
Central sleep apnea (CSA)
64. During central sleep apnea, what stops along with airflow through the nose and mouth?
Inspiratory efforts
65. What conditions are associated with central sleep apnea?
Hypothyroidism, brain stem neoplasm or infarction, congestive heart failure (CHF)
66. What is a combination of obstructive and central sleep apneas called?
Mixed sleep apnea
67. What conditions cause hypoxemia and hypercapnia during sleep?
Sleep apnea
68. What are the effects of hypoxemia and hypercapnia on sleep?
They cause the patient to awaken to breathe, resulting in fragmented and restless sleep, and producing daytime sleepiness.
69. How is sleep apnea diagnosed?
Through bloodwork, chest X-ray, and patient history, including input from the patient’s bed partner.
70. When are snoring, sleep disturbances, and daytime sleepiness typically noted?
During the patient’s history.
71. What type of sleep apnea is confirmed with a polysomnogram?
Obstructive sleep apnea (OSA).
72. The diagnosis of OSA is based on which index?
Apnea-Hypopnea Index (AHI)
73. What does the Apnea-Hypopnea Index (AHI) measure?
The average number of hypopneas and apneas per hour of sleep.
74. What are the AHI severity levels?
Normal: <5 episodes per hour, Mild: 5-15 episodes per hour, Moderate: 15-30 episodes per hour, and Severe: >30 episodes per hour.
75. What index measures how long a person’s SpO2 is below 90% during sleep?
Oxygen Desaturation Index
76. What role do cardiac arrhythmias, tachycardia, and bradycardia play in diagnosing sleep apnea?
They are considered during the diagnosis process.
77. What is normal and not normal in obstructive sleep apnea (OSA)?
The diaphragm and intercostal muscles exhibit normal respiratory effort; the airway collapses, blocking airflow to the lungs.
78. How does a person usually figure out they may have sleep apnea?
Their partner complains about their snoring.
79. How long does a person stop breathing with sleep apnea?
20-60 seconds. The person usually awakens to breathe, often gasping or snorting.
80. How often can awakenings due to sleep apnea interrupt the normal sleep cycle?
Up to 20-30 times per hour.
81. What is a person’s chief complaint when they have sleep apnea?
Feeling tired all the time and being sleepy during the day.
82. How is a person diagnosed with sleep apnea?
In a sleep disorders clinic with a sleep study, or you may notice signs of apnea during hospitalization.
83. What are some nursing interventions and teaching points for sleep apnea?
Weight reduction, stopping smoking, sleeping on the side to keep the airway open, avoiding alcohol before bed, and avoiding or decreasing sleep medications if possible.
84. What are some medical therapy options for sleep apnea?
CPAP (continuous positive airway pressure), BiPAP (uses lower pressure during expiration than CPAP), and surgery for severe cases.
85. What are some common complaints about apnea machines?
Nasal congestion, air leaks, pressure marks on the face, pressure intolerance, discomfort, claustrophobia, and getting tangled in tubing, leading to non-compliance.
86. What are some patient teaching points for using apnea machines?
How to apply and wear the mask, when to use the equipment, cleaning the mask and hoses daily, resupplying masks and hoses every 3-6 months, and never stopping use without reevaluation.
87. What does apnea airway surgery do for the patient?
It widens the breathing passage.
88. What are some nursing interventions for the patient post-op?
Monitoring for bleeding, aspiration, edema (narrowing of the airway), and watching for heavy bleeding when scabs form and fall off.
89. What are two types of surgery for severe sleep apnea?
Maxillomandibular advancement and genioglossus advancement surgery.
90. What is central sleep apnea characterized by?
It is caused by brain lesions, is rare, and often causes Cheyne-Stokes respirations (rapid breathing followed by apnea).
91. What is the usual treatment for central sleep apnea?
CPAP is the usual treatment, but CNS lesions may require a diaphragmatic pacemaker or mechanical ventilation.
92. What should be avoided in central sleep apnea?
Sedative and hypnotic drugs.
93. What should be done if someone with apnea is admitted to the hospital?
Have the patient or family bring the CPAP/BiPAP, as the patient’s own machine is best due to the fit of the mask, pre-programmed settings, and cost.
94. Which type of sleep apnea is characterized by both obstructive and central components?
Mixed sleep apnea
95. What percentage of adults are estimated to have sleep apnea but remain undiagnosed?
Approximately 80% of moderate and severe cases remain undiagnosed.
96. What is a common symptom of sleep apnea that can occur during nighttime sleep?
Loud snoring, choking, or gasping for air.
97. How can untreated sleep apnea affect cardiovascular health?
It can lead to high blood pressure, heart disease, and an increased risk of stroke.
98. What lifestyle modification can help reduce the severity of sleep apnea?
Weight loss, as it can decrease the amount of fatty tissue in the throat.
99. What is the role of a mandibular advancement device in treating sleep apnea?
It helps keep the airway open by moving the lower jaw forward.
100. How does positional therapy work in managing sleep apnea?
It involves sleeping in a position (usually on the side) that helps prevent airway obstruction.
Final Thoughts
Sleep apnea is a complex and common disorder that significantly impacts respiratory health, cardiovascular function, and overall quality of life. Despite its prevalence, it remains underdiagnosed, emphasizing the importance of increased awareness and early detection.
Advances in diagnostic tools and treatment options have made sleep apnea highly manageable when identified and treated appropriately.
Respiratory therapists are essential members of the healthcare team in screening, diagnosing, and managing sleep apnea. Through patient education, therapy optimization, and ongoing monitoring, respiratory therapists help improve patient outcomes and reduce the long-term complications associated with sleep-disordered breathing.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Yayan J, Rasche K. A Systematic Review of Risk factors for Sleep Apnea. Prev Med Rep. 2024.

