Subcutaneous emphysema is a clinical finding that often alarms patients, families, and inexperienced clinicians due to its dramatic physical presentation. The sudden swelling of the neck, chest, or face, combined with a crackling sensation beneath the skin, can appear severe and life-threatening. However, while subcutaneous emphysema frequently signals underlying lung injury or barotrauma, it is usually not dangerous by itself.
For respiratory therapists, subcutaneous emphysema is highly relevant because it commonly develops in patients receiving mechanical ventilation, those with acute lung injury, and individuals with chest trauma.
Recognizing subcutaneous emphysema, understanding its causes, and responding appropriately are essential skills in respiratory care, particularly in critical care settings.
What Is Subcutaneous Emphysema?
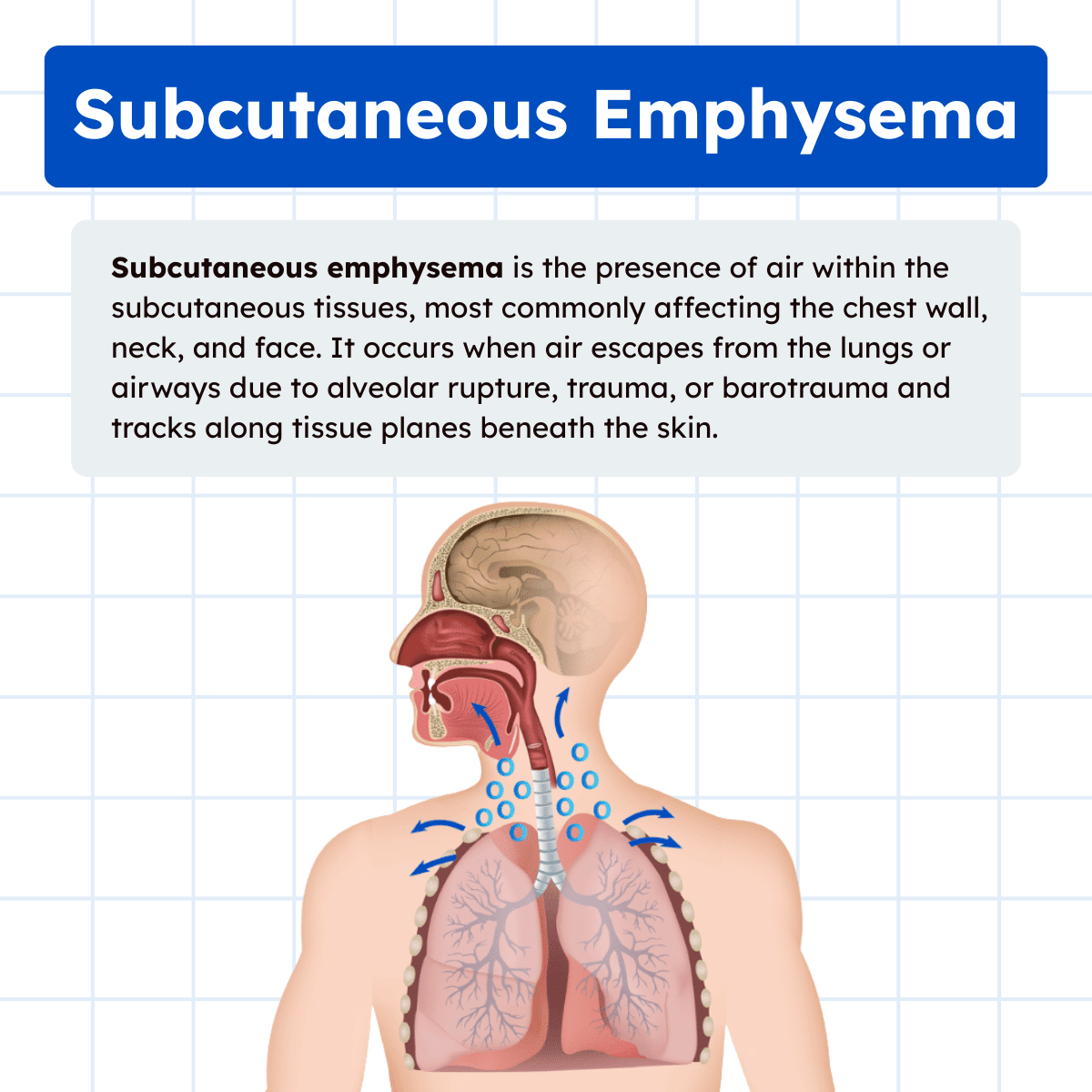
Subcutaneous emphysema occurs when air escapes from the respiratory system and becomes trapped within the subcutaneous tissues, most commonly in the chest wall, neck, face, and upper extremities. The air dissects along tissue planes, creating visible swelling and a characteristic crackling sensation when the area is palpated.
This crackling sensation, known as crepitus, is caused by small air bubbles moving beneath the skin. Crepitus is a classic physical sign associated with barotrauma and extra-alveolar air leaks. Subcutaneous emphysema is not a disease itself but rather a clinical sign that indicates air has escaped from its normal anatomical location, most often due to alveolar rupture.
How Does Subcutaneous Emphysema Develop?
The most common underlying mechanism of subcutaneous emphysema is alveolar disruption. When alveoli rupture, air can escape into surrounding structures rather than remaining within the airways.
Once alveoli rupture, air may follow several potential pathways:
- Into the pleural space, resulting in a pneumothorax
- Along perivascular or peribronchial sheaths toward the mediastinum, resulting in pneumomediastinum
- From the mediastinum into the soft tissues of the neck and chest wall, producing subcutaneous emphysema
The final location of the escaped air determines how the barotrauma is classified. Subcutaneous emphysema represents one of several manifestations of extra-alveolar air. Importantly, a pneumothorax does not always have to be present for subcutaneous emphysema to occur. Air can track directly into soft tissues without accumulating in the pleural space.
Common Causes of Subcutaneous Emphysema
Mechanical Ventilation and Barotrauma
Mechanical ventilation is one of the most common causes of subcutaneous emphysema in hospitalized patients. High airway pressures and excessive end-inspiratory volumes increase the risk of alveolar rupture, particularly in patients with stiff, noncompliant lungs.
Patients with conditions such as acute respiratory distress syndrome (ARDS), severe pneumonia, pulmonary fibrosis, and asthma with air trapping are especially vulnerable to ventilator-induced lung injury.
Barotrauma related to mechanical ventilation includes several possible complications, including pneumothorax, pneumomediastinum, pneumopericardium, and subcutaneous emphysema. All of these conditions result from air escaping the alveoli due to excessive pressure or volume.
Chest Trauma
Blunt or penetrating chest trauma is another major cause of subcutaneous emphysema. Injuries such as rib fractures, lung contusions, or penetrating wounds can allow air to escape from damaged lung tissue into surrounding structures.
In trauma patients, subcutaneous emphysema may develop rapidly and can spread extensively across the chest wall, neck, and face. Its presence should prompt immediate evaluation for associated injuries, including pneumothorax and tracheobronchial rupture.
Airway and Thoracic Procedures
Medical procedures involving the airway or thorax can also introduce air into soft tissues. Examples include:
- Endotracheal intubation
- Tracheostomy placement
- Bronchoscopy
- Chest tube insertion
- Thoracic surgery
Note: Improper placement, airway injury, or excessive airway pressures during these procedures can lead to air leakage and subsequent subcutaneous emphysema.
Spontaneous Causes
In some cases, subcutaneous emphysema may occur spontaneously, especially in individuals with underlying lung disease. Severe coughing, vomiting, or Valsalva maneuvers can generate enough pressure to rupture fragile alveoli.
Although less common, spontaneous subcutaneous emphysema has been reported in patients with asthma exacerbations, infections, and connective tissue disorders.
Clinical Presentation and Assessment
Physical Findings
The hallmark clinical sign of subcutaneous emphysema is crepitus. When palpating affected areas, the clinician feels a crackling or popping sensation beneath the skin, often compared to bubble wrap.
Additional findings may include:
- Swelling of the neck, face, or chest
- A sensation of fullness or tightness
- Voice changes if air accumulates near the larynx
- Periorbital swelling in severe cases
Note: Despite its dramatic appearance, subcutaneous emphysema itself rarely causes significant physiological compromise.
Diagnostic Imaging
Chest radiography is typically the first imaging modality used to evaluate patients with suspected subcutaneous emphysema. X-rays may reveal air in the soft tissues and can identify associated conditions such as pneumothorax or pneumomediastinum.
However, small pneumothoraces can be difficult to detect, particularly when mediastinal air displaces pleural structures. In such cases, computed tomography (CT) is more sensitive and can better identify the source and extent of the air leak.
In critically ill patients who are too unstable to be transported, clinicians may need to rely on clinical judgment and bedside imaging.
Is Subcutaneous Emphysema Dangerous?
One of the most important teaching points for respiratory therapists is that subcutaneous emphysema is usually not dangerous on its own. The trapped air in soft tissues rarely interferes with gas exchange or hemodynamics.
However, its presence is significant because it indicates that alveolar rupture has occurred. The underlying cause, rather than the emphysema itself, is what poses the greatest risk to the patient. In rare cases, massive subcutaneous emphysema can cause discomfort, airway compromise, or difficulty with ventilation monitoring, but these situations are uncommon.
Relevance to Respiratory Therapists
Ventilator Management
Respiratory therapists play a critical role in preventing and managing subcutaneous emphysema related to mechanical ventilation. Vigilance is required when patients are exposed to:
- High peak inspiratory pressures
- Elevated plateau pressures
- Large tidal volumes
- Poor lung compliance
Note: RTs must continuously assess ventilator parameters and collaborate with the healthcare team to implement lung-protective strategies. In patients with ARDS, low tidal volume ventilation and careful monitoring of airway pressures are essential to minimize the risk of barotrauma.
Patient Monitoring and Assessment
Respiratory therapists are often the first clinicians to detect subcutaneous emphysema during routine patient assessments. Palpation of the chest wall and neck, along with observation for sudden swelling or changes in airway pressure, can lead to early recognition.
Any unexplained deterioration in gas exchange, increased airway pressures, or changes in chest mechanics should prompt further evaluation.
Collaboration in Clinical Decision-Making
When subcutaneous emphysema is identified, RTs play a key role in communicating findings to physicians and nurses. Decisions regarding imaging, ventilator adjustments, or chest tube placement often depend on accurate respiratory assessment.
In some cases, a chest tube may be placed even if a pneumothorax is not clearly identified, especially when the patient is unstable, and the potential benefits outweigh the risks.
Subcutaneous Emphysema and Ventilator-Associated Lung Injury
Ventilator-associated lung injury (VALI) refers to lung damage caused by mechanical ventilation. High pressures, excessive volumes, infection, and patient-ventilator asynchrony all contribute to this condition.
Subcutaneous emphysema is one manifestation of VALI and serves as a visible marker of extra-alveolar air leakage. Its presence should prompt immediate reassessment of ventilator settings and lung mechanics.
Note: Understanding VALI is especially important for respiratory therapy students preparing for board examinations, as barotrauma and its complications are frequently tested concepts.
Management and Treatment
Addressing the Underlying Cause
There is no direct treatment required for subcutaneous emphysema itself. Management focuses on identifying and correcting the underlying source of the air leak.
This may include:
- Reducing ventilator pressures or volumes
- Treating pneumothorax with chest tube placement
- Managing airway injuries or trauma
- Adjusting patient positioning
Note: In most cases, subcutaneous emphysema resolves spontaneously once the source of air leakage is controlled.
Patient and Family Education
Because subcutaneous emphysema can look alarming, patient and family reassurance is an important aspect of care. Explaining that the condition is usually benign and temporary helps reduce anxiety.
Respiratory therapists often serve as educators at the bedside and can provide clear explanations of what is happening and why certain interventions are necessary.
Key Takeaways for Respiratory Care
- Subcutaneous emphysema is the presence of air in subcutaneous tissues
- It is most commonly caused by alveolar rupture due to barotrauma or trauma
- Crepitus is the classic physical finding
- A pneumothorax may or may not be present
- The condition itself is rarely physiologically significant
- Its presence signals underlying lung injury that requires evaluation
- Respiratory therapists play a critical role in prevention, detection, and management
Subcutaneous Emphysema Practice Questions
1. What is subcutaneous emphysema?
The presence of air within the subcutaneous tissues, most commonly of the chest, neck, or face.
2. What causes the crackling sensation felt when palpating subcutaneous emphysema?
Fine air bubbles trapped in the soft tissues.
3. What is the tactile sensation associated with subcutaneous emphysema called?
Crepitus
4. Crepitus is considered a classic sign of what ventilator-related complication?
Barotrauma
5. What underlying event must occur for subcutaneous emphysema to develop?
Alveolar rupture with escape of air from the lung.
6. In mechanically ventilated patients, what two ventilatory factors increase the risk of subcutaneous emphysema?
High airway pressures and excessive end-inspiratory volumes.
7. What types of trauma commonly predispose patients to subcutaneous emphysema?
Blunt or penetrating chest trauma.
8. Does the presence of subcutaneous emphysema always indicate a pneumothorax?
No, a pneumothorax is not always present.
9. Why is it difficult to determine which lung is leaking air when subcutaneous emphysema is present without a pneumothorax?
Air can track through tissue planes without localizing to a single lung.
10. Why is subcutaneous emphysema itself usually not physiologically significant?
It does not typically impair ventilation or gas exchange.
11. Why is subcutaneous emphysema still clinically important despite being physiologically benign?
It indicates underlying alveolar disruption and possible barotrauma.
12. What imaging study is most commonly used initially when subcutaneous emphysema is suspected?
Chest radiograph
13. Why can pneumothorax be difficult to detect on chest x-ray when subcutaneous emphysema is present?
Air in the mediastinum can obscure pleural landmarks.
14. What imaging modality is most sensitive for detecting a small pneumothorax?
Chest CT scan
15. Why might a chest tube be placed even if a pneumothorax is not clearly identified?
The potential benefit of preventing deterioration outweighs the risk in unstable patients.
16. What term describes lung injury caused by mechanical ventilation?
Ventilator-associated lung injury (VALI)
17. High ventilatory pressures are most closely associated with which type of ventilator-induced injury?
Barotrauma
18. Subcutaneous emphysema is classified as which type of barotrauma?
Extra-alveolar air
19. How does pneumomediastinum develop following alveolar rupture?
Air dissects along perivascular sheaths into the mediastinum.
20. What additional complication may occur if mediastinal air tracks into the neck and chest wall?
Progression to extensive subcutaneous emphysema.
21. What physical finding most commonly alerts clinicians to the presence of subcutaneous emphysema?
Palpable crepitus over the chest, neck, or face.
22. Where is subcutaneous emphysema most frequently first detected?
Around the clavicles, neck, and upper chest wall.
23. Why can subcutaneous emphysema spread rapidly once it begins?
Air follows fascial planes with little resistance.
24. What ventilator mode–related issue can worsen subcutaneous emphysema?
Excessive pressure delivery leading to alveolar overdistention.
25. What patient population is at especially high risk for developing subcutaneous emphysema?
Patients receiving positive-pressure ventilation.
26. What change in ventilator graphics may suggest worsening air leak?
Increasing peak pressures with reduced delivered volume.
27. How does subcutaneous emphysema differ from pneumothorax in location of air?
Air is in soft tissues rather than the pleural space.
28. What auscultatory finding may accompany subcutaneous emphysema if a pneumothorax is present?
Unilateral diminished or absent breath sounds.
29. Why should sudden onset of subcutaneous emphysema prompt reassessment of ventilator settings?
It may signal excessive pressure or volume delivery.
30. What bedside action should be taken immediately after identifying crepitus?
Assess for pneumothorax and notify the physician.
31. How does coughing affect subcutaneous emphysema?
It does not clear or reduce the trapped air.
32. What complication can occur if subcutaneous emphysema involves the neck extensively?
Airway compromise due to soft tissue swelling.
33. What is the relationship between ARDS and subcutaneous emphysema?
ARDS patients are vulnerable due to stiff lungs and higher pressures.
34. Why may subcutaneous emphysema worsen during recruitment maneuvers?
Increased transpulmonary pressures can extend alveolar rupture.
35. What clinical sign helps differentiate subcutaneous emphysema from edema?
Palpable crackling sensation rather than pitting.
36. What type of barotrauma involves air collecting around the heart?
Pneumopericardium.
37. Why should oxygenation be closely monitored when subcutaneous emphysema is present?
Associated barotrauma can impair ventilation and gas exchange.
38. What ventilator adjustment may reduce progression of subcutaneous emphysema?
Lowering tidal volume and limiting airway pressures.
39. What role does PEEP play in the development of subcutaneous emphysema?
Excessive PEEP can contribute to alveolar rupture.
40. How does subcutaneous emphysema typically resolve once the air leak stops?
Gradual reabsorption of air by surrounding tissues.
41. What sign suggests that subcutaneous emphysema is expanding?
Visible swelling spreading across the chest or neck.
42. Why are patients with COPD susceptible to subcutaneous emphysema?
Air trapping and fragile alveoli increase rupture risk.
43. What complication should be suspected if subcutaneous emphysema appears suddenly after intubation?
Esophageal or tracheal injury.
44. How does pneumomediastinum relate to subcutaneous emphysema?
Mediastinal air can dissect outward into subcutaneous tissues.
45. Why is patient reassurance important when subcutaneous emphysema is identified?
The condition often appears alarming but is usually benign.
46. What physical assessment technique confirms suspected subcutaneous emphysema?
Gentle palpation of the affected area.
47. Why may chest tube placement reduce subcutaneous emphysema?
It relieves pleural air and decreases pressure driving air leakage.
48. What sign indicates subcutaneous emphysema is not the primary problem?
Stable oxygenation and ventilation without distress.
49. How does subcutaneous emphysema affect pulse oximetry readings?
It usually has no direct effect unless gas exchange worsens.
50. What key principle guides management of subcutaneous emphysema?
Identify and correct the underlying air leak source.
51. What imaging study is most commonly used to evaluate suspected subcutaneous emphysema?
Chest X-ray
52. Why can small pneumothoraces be difficult to detect when subcutaneous emphysema is present?
Air in the tissues can obscure pleural markings on imaging.
53. What clinical finding distinguishes subcutaneous emphysema from muscle swelling?
A crackling sensation on palpation.
54. How does subcutaneous emphysema typically affect lung auscultation directly?
It does not produce lung sounds but may coexist with abnormal breath sounds.
55. What airway-related injury can lead to subcutaneous emphysema after intubation?
Tracheal or bronchial rupture.
56. Why should ventilator alarms be closely monitored in patients with subcutaneous emphysema?
They may indicate worsening leaks or rising pressures.
57. What term describes air dissecting along bronchovascular sheaths toward the mediastinum?
Pulmonary interstitial emphysema
58. Why is subcutaneous emphysema considered a marker of underlying pathology rather than a disease itself?
It reflects escaped air from damaged lung or airway structures.
59. What finding suggests subcutaneous emphysema is secondary to barotrauma?
Recent exposure to high airway pressures.
60. How does subcutaneous emphysema affect chest wall compliance?
It can mildly stiffen the chest wall when extensive.
61. What patient complaint may accompany facial subcutaneous emphysema?
A feeling of fullness or tightness under the skin.
62. Why is subcutaneous emphysema more apparent in thin patients?
Less subcutaneous fat makes trapped air easier to palpate.
63. What bedside assessment should be repeated frequently once subcutaneous emphysema is identified?
Breath sounds and chest symmetry.
64. How does positive-pressure ventilation influence the spread of subcutaneous emphysema?
It can drive air further into tissue planes.
65. What clinical clue suggests subcutaneous emphysema is worsening?
Progressive swelling despite stable ventilator settings.
66. Why is subcutaneous emphysema often first noted during physical examination rather than imaging?
Crepitus can be felt before changes are radiographically obvious.
67. What complication may occur if air tracks inferiorly into the abdomen?
Pneumoperitoneum
68. What does stable hemodynamics suggest in a patient with subcutaneous emphysema?
The air leak has not significantly compromised circulation.
69. Why should suctioning be performed carefully in patients with subcutaneous emphysema?
Aggressive suctioning can increase airway pressures.
70. What clinical condition often coexists with subcutaneous emphysema in trauma patients?
Rib fractures with lung injury.
71. How does subcutaneous emphysema affect chest percussion findings?
Percussion is usually unchanged unless a pneumothorax is present.
72. What is the primary goal of ventilator management when subcutaneous emphysema develops?
Limit further alveolar injury
73. Why may subcutaneous emphysema worsen during coughing or agitation?
Sudden increases in intrathoracic pressure force more air into tissues.
74. What sign helps differentiate subcutaneous emphysema from cellulitis?
Lack of redness, warmth, or tenderness.
75. What complication should be suspected if subcutaneous emphysema rapidly progresses with hypotension?
Tension pneumothorax
76. Why is subcutaneous emphysema not usually treated directly?
Management focuses on correcting the underlying cause.
77. What clinical observation suggests subcutaneous emphysema is resolving?
Decreasing crepitus on palpation.
78. Why should the neck be carefully assessed in subcutaneous emphysema?
Air accumulation can threaten airway patency.
79. What role does chest tube patency play in managing subcutaneous emphysema?
Ensures effective evacuation of pleural air.
80. What key assessment finding reassures clinicians despite the presence of subcutaneous emphysema?
Stable oxygenation and ventilation parameters.
81. What physical exam technique is most useful for detecting early subcutaneous emphysema?
Gentle palpation of the chest, neck, and supraclavicular areas.
82. Why can subcutaneous emphysema extend into the face and eyelids?
Air follows fascial planes upward from the chest and mediastinum.
83. What ventilator parameter should be reassessed immediately when subcutaneous emphysema is detected?
Peak airway pressure
84. Why is subcutaneous emphysema more concerning in mechanically ventilated patients than in spontaneously breathing patients?
Positive pressure can worsen ongoing air leaks.
85. What finding suggests subcutaneous emphysema is associated with pneumomediastinum?
Crepitus extending into the neck with chest discomfort.
86. How does subcutaneous emphysema affect skin temperature over the affected area?
Skin temperature is usually normal.
87. What bedside maneuver helps assess airway involvement when neck subcutaneous emphysema is present?
Assessment for voice changes or stridor.
88. Why may subcutaneous emphysema be asymmetrical on physical exam?
The air leak may originate from one lung or airway.
89. What complication should be suspected if subcutaneous emphysema is accompanied by increasing ventilator pressures and hypoxemia?
Worsening alveolar rupture with possible pneumothorax.
90. Why is reassurance important for patients who develop subcutaneous emphysema?
The visible swelling can be alarming despite minimal physiologic impact.
91. What radiographic sign may indicate extensive subcutaneous emphysema?
Streaks of radiolucency outlining muscle or soft tissue structures.
92. How does subcutaneous emphysema affect pulse oximetry readings directly?
It does not directly alter oxygen saturation readings.
93. Why should endotracheal tube position be reassessed when subcutaneous emphysema develops?
Tube malposition can contribute to airway injury.
94. What clinical factor increases the risk of subcutaneous emphysema during mechanical ventilation?
High end-inspiratory pressures.
95. Why is subcutaneous emphysema commonly monitored rather than aggressively treated?
It often resolves once the air leak is controlled.
96. What finding suggests subcutaneous emphysema is secondary to chest tube malfunction?
Persistent or worsening crepitus despite tube placement.
97. Why can subcutaneous emphysema complicate central line placement?
Air in tissues obscures anatomic landmarks.
98. What patient positioning may help limit progression of subcutaneous emphysema?
Maintaining neutral head and neck alignment.
99. How does subcutaneous emphysema differ from edema on palpation?
It produces a crackling sensation rather than pitting.
100. What key clinical priority follows the detection of subcutaneous emphysema?
Identifying and managing the source of the air leak.
Final Thoughts
Subcutaneous emphysema is a striking but often misunderstood clinical finding in respiratory care. While it rarely causes direct harm, it serves as an important warning sign of alveolar disruption and potential ventilator-associated lung injury.
For respiratory therapists, understanding its causes, assessment, and clinical implications is essential for safe and effective patient care.
Through vigilant monitoring, appropriate ventilator management, and clear communication with the healthcare team, RTs help ensure that subcutaneous emphysema is recognized early and managed appropriately, protecting patients from more serious complications.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Kukuruza K, Aboeed A. Subcutaneous Emphysema(Archived) [Updated 2023 Jul 17]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025.

