Vital capacity is one of the most fundamental measurements used to assess lung function, yet its clinical importance often extends far beyond a simple number on a pulmonary function report.
It represents the maximum amount of air a person can move in and out of the lungs and provides valuable insight into respiratory muscle strength, lung compliance, and overall ventilatory capacity.
For respiratory therapists, understanding vital capacity is essential for evaluating patients across a wide range of settings, from routine pulmonary testing to critical care and mechanical ventilation management.
What Is Vital Capacity?
Vital capacity (VC) is the maximum volume of air a person can exhale after taking a maximal inhalation. In simple terms, it reflects how much air the lungs can move when a patient breathes in as deeply as possible and then exhales completely.
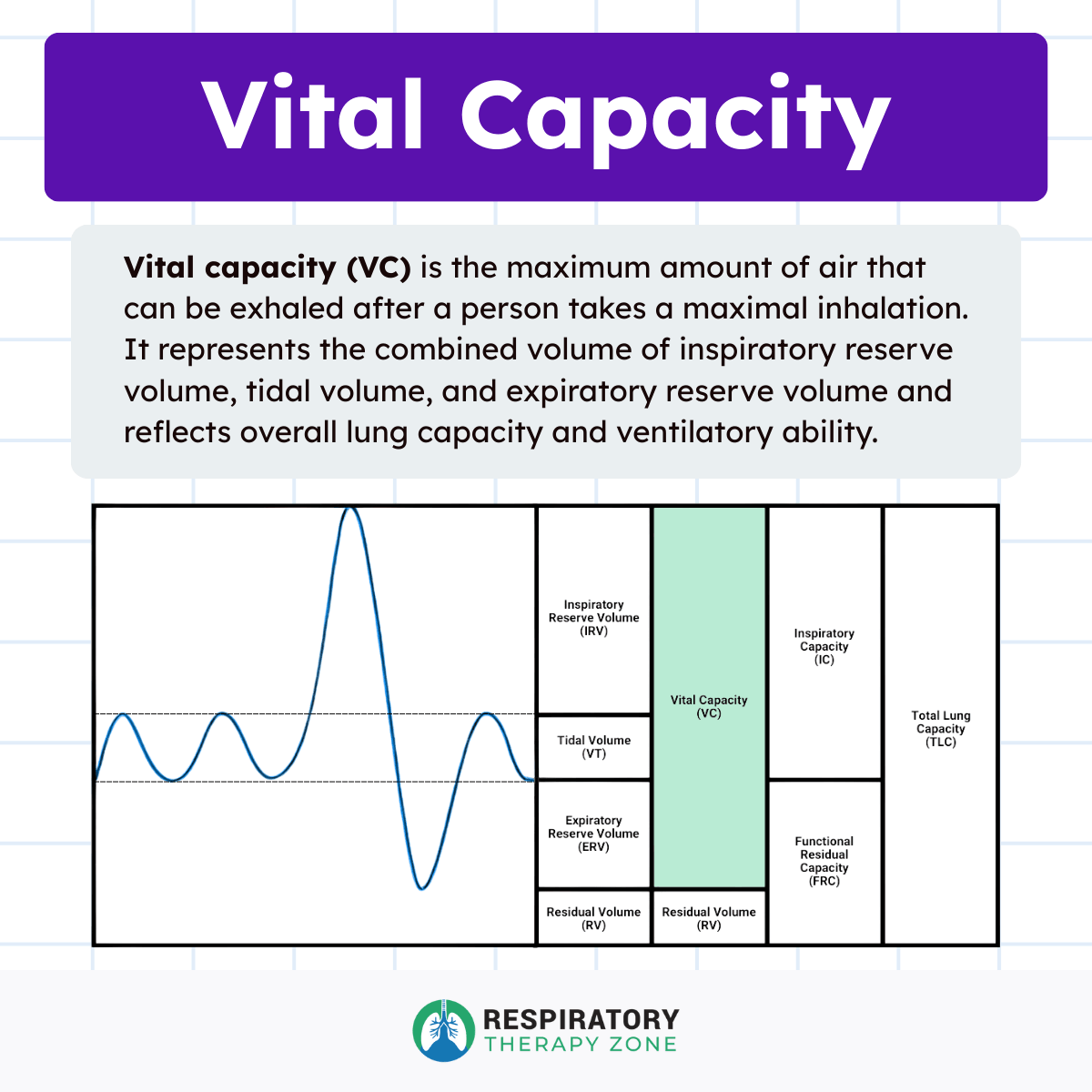
Vital capacity is made up of three lung volumes:
- Inspiratory reserve volume (IRV)
- Tidal volume (VT)
- Expiratory reserve volume (ERV)
Mathematically, it can be expressed as:
Vital Capacity = IRV + VT + ERV
Unlike residual volume, vital capacity can be measured directly using spirometry, making it one of the most accessible and commonly assessed lung volumes in clinical practice.
Normal Values and Variability
Normal vital capacity values depend on several factors, including age, sex, height, body size, and overall health. In healthy adults, vital capacity typically ranges between 3 and 5 liters, though predicted values are calculated using standardized reference equations.
Vital capacity tends to be:
- Higher in taller individuals
- Higher in males compared to females
- Lower with advancing age
- Reduced in the presence of lung or neuromuscular disease
Note: Because of this variability, VC is interpreted as a percentage of the predicted value rather than as a single absolute number.
How Vital Capacity Is Measured
Vital capacity is most commonly measured using spirometry. During the test, the patient is instructed to inhale fully to total lung capacity and then exhale slowly and completely until no more air can be expelled.
There are two commonly reported forms of vital capacity:
Slow Vital Capacity (SVC)
SVC is measured during a slow, controlled exhalation following a maximal inspiration. This method is particularly useful in patients with obstructive lung disease because it minimizes airway collapse and air trapping.
Forced Vital Capacity (FVC)
FVC is measured during a rapid, forceful exhalation after maximal inspiration. It is a key component of standard spirometry and is often used alongside FEV₁ to evaluate airflow obstruction.
In healthy individuals, SVC and FVC values are similar. In obstructive disease, FVC is often lower than SVC due to dynamic airway collapse.
Clinical Significance of Vital Capacity
Vital capacity provides valuable information about the mechanical function of the lungs and chest wall. Changes in VC often reflect underlying pathology and can guide clinical decision-making.
Reduced Vital Capacity
A decreased vital capacity may be seen in several conditions, including:
- Restrictive lung diseases such as pulmonary fibrosis
- Neuromuscular disorders affecting respiratory muscles
- Severe obesity
- Chest wall deformities
- Pleural diseases
In restrictive conditions, lung expansion is limited, reducing the total volume of air that can be inhaled and exhaled. In neuromuscular disease, reduced muscle strength prevents full inspiration or expiration.
Normal or Increased Vital Capacity
Vital capacity may be normal or even increased in early obstructive lung disease. However, as air trapping and hyperinflation worsen, VC can eventually decline due to reduced expiratory reserve volume.
Vital Capacity and Neuromuscular Disease
Vital capacity is especially important in patients with neuromuscular disorders such as muscular dystrophy, amyotrophic lateral sclerosis, and spinal cord injuries. In these patients, VC serves as a key indicator of respiratory muscle strength and ventilatory reserve.
A declining vital capacity may signal impending respiratory failure and the need for interventions such as noninvasive ventilation or airway clearance support. For this reason, serial VC measurements are commonly used to track disease progression.
Role of Vital Capacity in Critical Care
In critical care settings, vital capacity is often used as a bedside assessment tool to evaluate respiratory muscle strength and readiness for ventilatory support changes.
VC measurements can help clinicians:
- Assess the risk of respiratory failure
- Evaluate weaning readiness
- Monitor recovery after intubation
- Identify diaphragmatic weakness
Note: A low vital capacity may indicate inadequate ventilatory reserve, even if other parameters appear stable.
Vital Capacity and Mechanical Ventilation
Vital capacity plays an indirect but important role in mechanical ventilation management. Although VC is not measured while a patient is fully ventilated, it becomes relevant during spontaneous breathing trials and ventilator liberation.
Patients with low vital capacity may struggle to maintain adequate ventilation once support is reduced. Monitoring VC helps respiratory therapists anticipate weaning difficulties and adjust strategies accordingly.
Note: In neuromuscular and postoperative patients, vital capacity is often one of the most reliable predictors of extubation success or failure.
Factors That Influence Vital Capacity
Several physiological and mechanical factors influence vital capacity, including:
- Lung compliance
- Chest wall mobility
- Respiratory muscle strength
- Airway resistance
- Body position
Note: Vital capacity is generally higher in the upright position compared to supine due to improved diaphragmatic mechanics. A sudden drop in VC when lying flat may indicate diaphragmatic weakness or neuromuscular impairment.
Common Misconceptions About Vital Capacity
One common misconception is that vital capacity directly measures how well oxygen is delivered to the blood. While VC reflects ventilatory capacity, it does not directly assess gas exchange or oxygenation.
Another misunderstanding is assuming that a normal VC rules out lung disease. Some obstructive conditions may preserve VC early on, even when airflow limitation is present. Vital capacity should always be interpreted alongside other pulmonary function parameters and clinical findings.
Why Vital Capacity Matters to Respiratory Therapists
For respiratory therapists, vital capacity is more than just a spirometry value. It is a practical, versatile measurement that supports clinical assessment across multiple care environments.
Understanding VC allows therapists to:
- Interpret pulmonary function tests accurately
- Recognize restrictive versus obstructive patterns
- Monitor respiratory muscle strength
- Assist in ventilator weaning decisions
- Identify early signs of respiratory decline
Note: Its simplicity and clinical relevance make it a cornerstone measurement in respiratory care.
Access our quiz with sample TMC practice questions and detailed explanations to help you master pulmonary function testing (PFT).
Vital Capacity Practice Questions
1. What is vital capacity (VC)?
Vital capacity is the maximum volume of air that can be exhaled after a person takes a maximal inhalation.
2. What does vital capacity primarily reflect about lung function?
It reflects the total amount of air the lungs can move voluntarily with maximal effort.
3. Which three lung volumes make up vital capacity?
Inspiratory reserve volume, tidal volume, and expiratory reserve volume.
4. What is the equation for vital capacity?
VC = IRV + VT + ERV
5. Why can vital capacity be measured directly with spirometry?
Because all components of VC involve air that moves in and out of the lungs.
6. How does vital capacity differ from residual volume?
Residual volume cannot be exhaled, whereas vital capacity includes only exhalable air.
7. What is slow vital capacity (SVC)?
The volume of gas measured during a slow, complete exhalation after a maximal inspiration.
8. How does slow vital capacity differ from forced vital capacity (FVC)?
SVC is measured with a slow exhalation, while FVC requires a rapid, forceful exhalation.
9. What is forced vital capacity (FVC)?
The volume of air that can be forcibly exhaled as fast as possible after a full inspiration.
10. Why is FVC considered the most basic spirometry maneuver?
Because it forms the foundation for many spirometric measurements and interpretations.
11. What are the key steps of the FVC maneuver?
A maximal inhalation followed by a rapid, forceful exhalation lasting at least 6 seconds.
12. Which part of the FVC maneuver is most critical for accuracy?
The initial maximal inhalation and the forceful “blast” at the start of exhalation.
13. How is the vital capacity maneuver performed?
The patient inhales maximally and then exhales slowly and completely into the spirometer.
14. What is tidal volume (VT)?
The volume of air inspired or expired during normal, quiet breathing.
15. What is the approximate average tidal volume in a healthy adult?
About 500 mL, which is roughly 15 to 18 percent of vital capacity.
16. What is inspiratory reserve volume (IRV)?
The additional volume of air that can be inhaled with maximal effort after a normal inspiration.
17. Approximately what percentage of vital capacity does IRV represent?
About 60 percent
18. What is expiratory reserve volume (ERV)?
The additional volume of air that can be exhaled forcefully after a normal, quiet exhalation.
19. Approximately what percentage of vital capacity does ERV represent?
About 25 percent
20. What is residual volume (RV)?
The volume of air remaining in the lungs after maximal forceful exhalation.
21. Why is residual volume important for lung function?
It prevents lung collapse and allows continuous gas exchange between breaths.
22. How many lung volumes combined form lung capacities?
Two or more lung volumes combine to form lung capacities.
23. What is inspiratory capacity (IC) ?
The maximum volume of air that can be inhaled after a normal exhalation.
24. What is the equation for inspiratory capacity?
IC = VT + IRV
25. What is functional residual capacity (FRC)?
The volume of air remaining in the lungs after a normal, passive exhalation.
26. What is the equation for functional residual capacity?
FRC = RV + ERV
27. What is total lung capacity (TLC)?
The total volume of air contained in the lungs after maximal inspiration.
28. Which lung volumes make up total lung capacity?
Tidal volume, inspiratory reserve volume, expiratory reserve volume, and residual volume.
29. What factors mainly determine a person’s vital capacity?
Thoracic cavity size, lung and chest wall compliance, and respiratory muscle strength.
30. What is Hutchinson’s spirometer used to measure?
Vital capacity
31. How does a Hutchinson’s spirometer measure lung volume?
Expired air displaces an inner container, allowing volume to be read directly.
32. Why must the nose be closed during vital capacity measurement?
To prevent air leakage and ensure accurate volume measurement.
33. Why are vital capacity measurements typically repeated multiple times?
To ensure consistency and reliability of the results.
34. Why should repeated VC measurements not improve after the first attempt?
Because maximal effort should be achieved on the initial trial.
35. How is percent predicted vital capacity calculated?
(Measured VC ÷ predicted VC) × 100.
36. What percentage of predicted vital capacity is considered normal or athletic?
Approximately 120 to 125 percent.
37. At what percentage of predicted vital capacity is VC considered pathologically low?
Below 70 percent.
38. Why is vital capacity higher in trained athletes?
Due to increased chest wall expansion, lung compliance, and respiratory muscle strength.
39. How does reduced vital capacity affect ventilation?
It limits the amount of air that can be moved, increasing the risk of dyspnea.
40. Why is vital capacity clinically important for respiratory therapists?
It helps assess lung mechanics, respiratory muscle performance, and disease severity.
41. What is forced expiratory volume in one second (FEV1)?
FEV1 is the maximum volume of air exhaled during the first second of a forced expiration following a full inspiration.
42. What is forced vital capacity (FVC)?
FVC is the total volume of air that can be forcibly exhaled after a maximal inhalation.
43. What do FEV1 and FVC together assess?
They assess airflow limitation, lung volumes, and overall ventilatory function.
44. In what units are FEV1 and FVC measured?
They are measured in liters.
45. What does the FEV1/FVC ratio represent?
It represents the proportion of the vital capacity exhaled in the first second of forced expiration.
46. What is the normal value for the FEV1/FVC ratio in healthy adults?
Approximately 75 percent
47. Why is the FEV1/FVC ratio clinically important?
It helps differentiate obstructive from non-obstructive lung disease.
48. What does a reduced FEV1/FVC ratio indicate?
Airflow obstruction
49. For what purposes are FEV1 and FVC commonly measured?
To detect lung disease, assess severity, and evaluate response to treatment.
50. How are spirometry results interpreted in clinical practice?
By comparing measured values to predicted normal values.
51. What factors are used to determine predicted normal spirometry values?
Age, sex, height, weight, and ethnicity.
52. How can serial FEV1 and FVC measurements be clinically useful?
They help determine whether lung function is improving or deteriorating over time.
53. According to GOLD criteria, how is COPD diagnosed using spirometry?
When the FEV1/FVC ratio is less than 0.70.
54. What additional spirometric criterion supports COPD severity assessment?
An FEV1 less than 75 percent of predicted.
55. What equipment is required to measure FEV1 and FVC?
A spirometer, mouthpiece, filter, and optionally a nose clip.
56. Why may a nose clip be used during spirometry?
To prevent air leakage through the nose.
57. Why must contraindications be checked before spirometry?
Because forced maneuvers can worsen certain medical conditions.
58. Why is patient height required before spirometry testing?
Height is needed to calculate predicted normal values.
59. What patient position is recommended during spirometry testing?
A safe, upright seated position.
60. Why is explaining the test to the patient important?
To ensure cooperation and maximal effort.
61. Which acute conditions may interfere with spirometry performance?
Nausea, vomiting, vertigo, or severe coughing.
62. Why is pneumothorax a contraindication for spirometry?
Forced expiration may worsen lung collapse.
63. Why is recent myocardial infarction a contraindication?
Spirometry increases intrathoracic pressure and cardiac stress.
64. Why can recent eye surgery be a contraindication?
Forced exhalation increases intraocular pressure.
65. What risk do aneurysms pose during spirometry testing?
Risk of rupture due to increased pressure.
66. Why is spirometer function checked prior to testing?
To ensure accurate and safe measurements.
67. Why should a new mouthpiece and filter be used for each patient?
To prevent cross infection.
68. What is the first breathing instruction given during an FVC test?
Inhale as deeply as possible to total lung capacity.
69. How should the patient exhale during an FVC maneuver?
As hard and fast as possible until no more air can be expelled.
70. What is the minimum acceptable exhalation time during FVC testing?
At least 6 seconds in adults.
71. Why must the clinician observe the patient during testing?
To ensure proper technique and patient safety.
72. How many acceptable spirometry trials are typically required?
At least three acceptable maneuvers.
73. What defines acceptable repeatability for FVC measurements?
The two largest FVC values must be within 150 mL or 5 percent of each other.
74. What defines acceptable repeatability for FEV1 measurements?
The two largest FEV1 values must be within 150 mL or 5 percent of each other.
75. What is the maximum number of spirometry attempts allowed?
Eight attempts
76. When should spirometry testing be stopped early?
If the patient asks to stop or experiences adverse effects.
77. Which values are reported as final spirometry results?
The largest acceptable FEV1 and FVC values.
78. Why are VC values interpreted as a percentage of predicted?
Because normal values vary widely among individuals.
79. In what lung diseases is vital capacity typically reduced?
Restrictive lung diseases and neuromuscular disorders.
80. Why may FVC be lower than SVC in obstructive lung disease?
Due to dynamic airway collapse during forced exhalation.
81. Why is slow vital capacity useful in obstructive disease?
It minimizes airway collapse and air trapping.
82. How does neuromuscular disease affect vital capacity?
Weak respiratory muscles limit maximal inspiration and expiration.
83. Why is declining vital capacity concerning in neuromuscular patients?
It may indicate impending respiratory failure.
84. How is vital capacity used in critical care?
To assess ventilatory reserve and respiratory muscle strength.
85. Why is vital capacity useful for evaluating weaning readiness?
Low VC suggests inadequate reserve to sustain spontaneous breathing.
86. How does body position affect vital capacity?
VC is higher upright than supine.
87. What does a significant drop in VC when supine suggest?
Possible diaphragmatic weakness.
88. Does vital capacity directly measure oxygenation?
No, it measures ventilatory capacity, not gas exchange.
89. Why can vital capacity be normal in early obstructive disease?
Airflow limitation may occur before lung volumes decline.
90. Why must vital capacity be interpreted with other PFT values?
Because VC alone cannot fully characterize lung disease.
91. How does lung compliance influence vital capacity?
Reduced compliance limits lung expansion and lowers VC.
92. How does chest wall mobility affect vital capacity?
Restricted mobility reduces maximal inhalation and exhalation.
93. Why is vital capacity important after extubation?
It helps assess recovery of respiratory muscle strength.
94. How does severe obesity affect vital capacity?
Excess weight restricts chest wall movement and diaphragm descent.
95. Why is vital capacity a practical bedside measurement?
It is simple, repeatable, and clinically meaningful.
96. How does vital capacity relate to ventilatory reserve?
Higher VC indicates greater ability to respond to increased demand.
97. Why is vital capacity monitored over time in chronic disease?
To track progression and response to therapy.
98. Can vital capacity be increased with respiratory muscle training?
Yes, improved muscle strength can increase VC.
99. Why is vital capacity considered a cornerstone measurement in respiratory care?
It integrates lung mechanics, muscle strength, and ventilatory capacity.
100. What is the primary clinical value of vital capacity for respiratory therapists?
Early identification of respiratory decline and guidance of clinical decisions.
Final Thoughts
Vital capacity is a foundational measurement that provides insight into lung mechanics, respiratory muscle strength, and overall ventilatory capacity. Its ability to be measured easily and interpreted across a wide range of clinical scenarios makes it especially valuable in respiratory care.
For respiratory therapists, understanding how vital capacity changes in health and disease enhances patient assessment, supports timely intervention, and improves outcomes in both acute and chronic settings. Mastery of this concept strengthens clinical judgment and reinforces the essential role of respiratory therapists in patient-centered care.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- David S, Sharma S. Vital Capacity. [Updated 2023 Jul 24]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025.


