Vital signs are among the most fundamental measurements in healthcare, offering an immediate snapshot of a patient’s physiological status. They reflect how well the body’s essential systems are functioning and often provide the first clues that something is wrong.
For respiratory therapists, vital signs are especially important because changes in breathing, oxygenation, and circulation frequently appear early in respiratory illness.
Understanding what vital signs are, how to measure them accurately, and how to interpret trends is a core skill that directly impacts patient safety and clinical decision-making in respiratory care.
What Are Vital Signs?
Vital signs are objective clinical measurements that indicate the state of a patient’s basic bodily functions. They are called “vital” because they are essential to life and because abnormalities often signal acute or chronic disease. In most healthcare settings, vital signs are assessed repeatedly over time to monitor stability, detect deterioration, and evaluate response to treatment.
While different facilities may include additional parameters, the core vital signs traditionally include body temperature, heart rate (pulse), respiratory rate, and blood pressure. In modern respiratory and critical care, oxygen saturation is commonly considered a fifth vital sign due to its direct relevance to oxygen delivery and gas exchange.
For respiratory therapists, vital signs are not isolated numbers. They must be interpreted in the context of the patient’s diagnosis, clinical presentation, and overall trends. A single abnormal value may be less important than a pattern of gradual change over time.
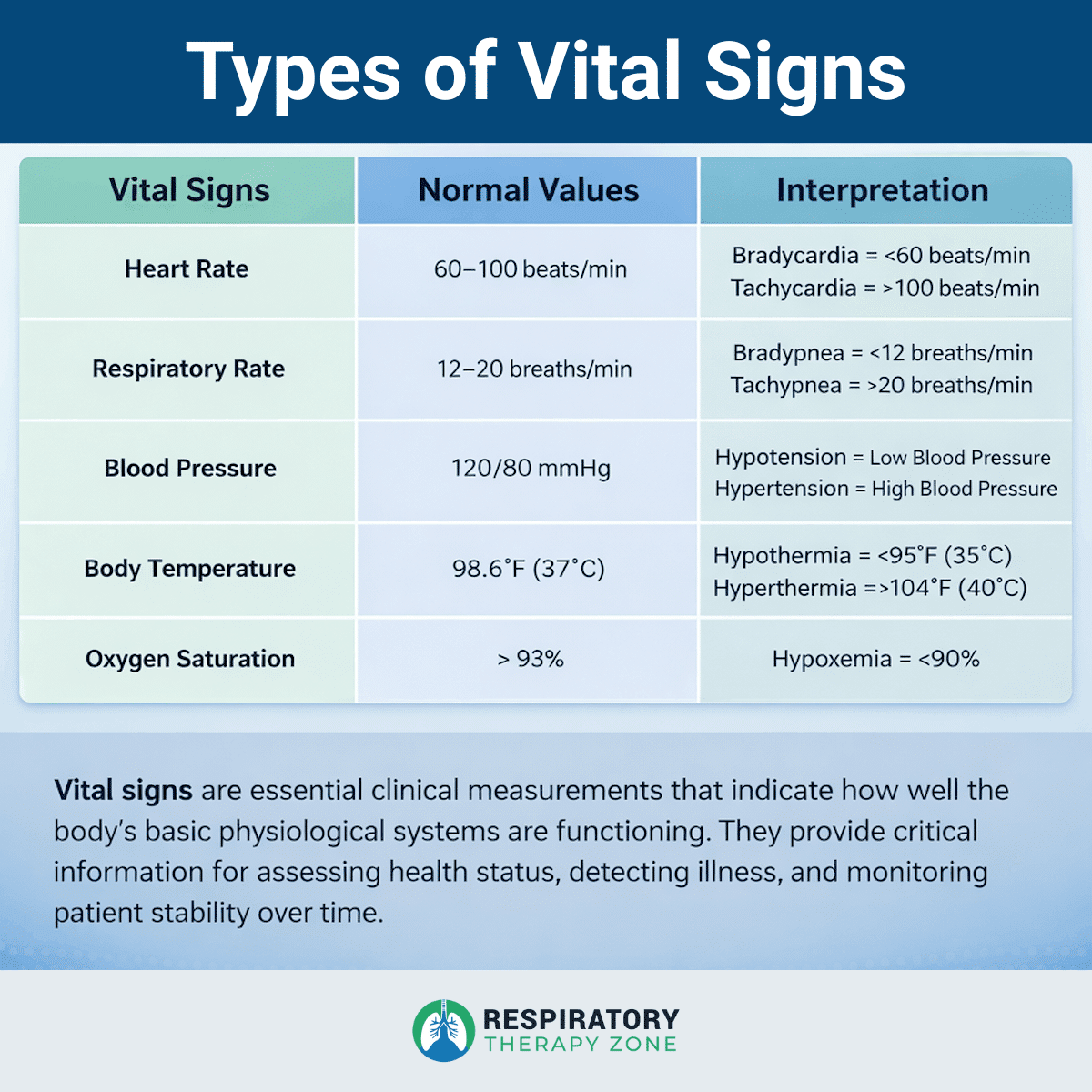
Types of Vital Signs
Body Temperature
Body temperature reflects the balance between heat production and heat loss. Normal core body temperature typically ranges around 36.5–37.5°C (97.7–99.5°F), though slight variations occur depending on the measurement site and time of day.
An elevated temperature (fever) often indicates infection or inflammation, both of which can significantly affect respiratory function. Fever increases metabolic demand and oxygen consumption, which may worsen hypoxemia in patients with underlying lung disease. Conversely, abnormally low temperature (hypothermia) can depress respiratory drive and impair gas exchange.
For respiratory therapists, recognizing temperature abnormalities is important when managing patients with pneumonia, sepsis, acute respiratory distress, or postoperative complications.
Heart Rate (Pulse)
Heart rate represents the number of times the heart beats per minute and reflects cardiovascular response to metabolic needs. In adults, a normal resting heart rate typically ranges from 60 to 100 beats per minute.
Tachycardia (elevated heart rate) may occur in response to hypoxemia, fever, anxiety, pain, or increased work of breathing. Bradycardia (slow heart rate) may be seen with hypoxia, certain medications, or advanced conduction abnormalities.
Because oxygen delivery depends on both cardiac output and oxygen content of the blood, heart rate changes are closely linked to respiratory status. Respiratory therapists often correlate pulse trends with oxygen saturation, respiratory effort, and arterial blood gas results.
Respiratory Rate
Respiratory rate is the number of breaths taken per minute and is one of the most sensitive indicators of respiratory distress. Normal adult respiratory rate typically falls between 12 and 20 breaths per minute.
An increased respiratory rate (tachypnea) is often an early sign of hypoxemia, metabolic acidosis, airway obstruction, or pulmonary pathology. A decreased respiratory rate (bradypnea) may indicate central nervous system depression, drug effects, or impending respiratory failure.
For respiratory therapists, respiratory rate is a critical vital sign. It provides insight into ventilatory demand, patient effort, and the effectiveness of interventions such as oxygen therapy, bronchodilators, or mechanical ventilation adjustments.
Blood Pressure
Blood pressure measures the force of blood against arterial walls and reflects the interaction between cardiac output and systemic vascular resistance. It is expressed as systolic pressure over diastolic pressure.
Hypotension may reduce perfusion to vital organs, including the lungs and brain, and can worsen oxygen delivery at the tissue level. Hypertension, while often chronic, can increase cardiac workload and contribute to complications such as heart failure or pulmonary edema.
In respiratory care, blood pressure is particularly relevant when managing patients on positive pressure ventilation. Changes in intrathoracic pressure can affect venous return and cardiac output, leading to fluctuations in blood pressure that must be closely monitored.
Oxygen Saturation (SpO₂)
Oxygen saturation measures the percentage of hemoglobin binding sites occupied by oxygen and is typically assessed using pulse oximetry. Although not part of the original four vital signs, SpO₂ is now widely considered essential in respiratory and critical care.
Normal oxygen saturation levels generally range from 95% to 100% in healthy individuals, though acceptable targets may differ in patients with chronic lung disease. A declining SpO₂ can signal worsening ventilation, impaired gas exchange, or increased shunt or dead space.
For respiratory therapists, oxygen saturation is a cornerstone measurement. It guides oxygen therapy titration, helps evaluate response to interventions, and serves as an early warning sign of respiratory compromise.
Normal Vital Sign Ranges
While normal values can vary based on age, health status, and clinical context, established reference ranges help guide interpretation.
Normal Vital Signs in Adults
- Heart rate: 60–100 beats per minute
- Respiratory rate: 12–20 breaths per minute
- Blood pressure: approximately 120/80 mmHg
- Body temperature: about 98.6°F (37°C)
- Oxygen saturation: greater than 93 percent
Normal Vital Signs in Infants
- Heart rate: 110–160 beats per minute
- Respiratory rate: 30–60 breaths per minute
- Blood pressure: around 60/40 mmHg
- Body temperature: about 98.6°F (37°C)
- Oxygen saturation: greater than 90 percent
Note: Additional neonatal indicators such as blood glucose, gestational age, Apgar score, birth weight, and respiratory assessment scores provide further insight into infant stability and development.
Additional Parameters Sometimes Included
Depending on the clinical setting, other measurements may be monitored alongside traditional vital signs. While not always labeled as vital signs, they provide valuable complementary information, especially in advanced respiratory care and critical care environments.
Pain Level
Pain level is a subjective assessment of a patient’s discomfort or distress, often measured using numerical rating scales, visual analog scales, or descriptive tools. It provides insight into how pain may be affecting breathing patterns, heart rate, and overall physiological stress. Uncontrolled pain can increase oxygen demand and interfere with effective ventilation, making pain assessment an important component of patient monitoring.
Level of Consciousness
Level of consciousness describes a patient’s degree of alertness and awareness of their surroundings. It ranges from fully alert to unresponsive and is commonly evaluated using standardized tools or simple observations. Changes in consciousness may indicate hypoxia, hypercapnia, neurological impairment, or medication effects, all of which are highly relevant in respiratory care.
Blood Glucose
Blood glucose measures the concentration of glucose in the blood and reflects metabolic balance. Abnormal levels can impact respiratory function, particularly in critically ill patients. Hypoglycemia may cause confusion and altered mental status, while hyperglycemia is often associated with stress, infection, or poor disease control and can complicate respiratory illness and recovery.
Skin Color
Skin color provides visual clues about oxygenation, circulation, and perfusion. Pale, mottled, or cyanotic skin may indicate poor blood flow or inadequate oxygen delivery. In respiratory care, bluish discoloration around the lips or fingertips can be an important sign of hypoxemia and warrants immediate assessment and intervention.
Pupillary Assessment
Pupillary assessment evaluates the size, symmetry, and reaction of the pupils to light. It helps identify neurological changes that may result from hypoxia, head injury, or medication effects. Abnormal pupillary responses can signal compromised brain oxygenation, making this assessment particularly relevant in patients with respiratory failure or altered ventilation.
Capillary Refill Time
Capillary refill time measures how quickly blood returns to tissue after pressure is applied, usually assessed at a fingernail or toenail. Normal refill occurs within about two seconds. Delayed refill may suggest poor peripheral perfusion, shock, or circulatory compromise, which can affect oxygen delivery and overall respiratory status.
Height and Weight (BMI)
Height and weight are used to calculate body mass index (BMI), which helps assess nutritional status and body composition. BMI influences respiratory mechanics, lung volumes, and oxygen consumption. Obesity can increase the work of breathing, while low body weight may be associated with muscle weakness and reduced respiratory reserve.
Urine Output
Urine output reflects kidney function and overall fluid balance. Decreased urine output may indicate dehydration, poor perfusion, or organ dysfunction. In respiratory care, fluid status plays a key role in conditions such as pulmonary edema and acute respiratory distress, making urine output an important parameter to monitor.
Mental Status
Mental status refers to a patient’s cognitive function, behavior, orientation, and ability to communicate. Changes such as confusion, agitation, or lethargy may be early signs of hypoxemia, hypercapnia, infection, or metabolic imbalance. Monitoring mental status helps detect respiratory deterioration before more obvious physical signs appear.
Why Vital Signs Matter in Respiratory Care
Vital signs are deeply intertwined with respiratory physiology. The lungs play a central role in oxygenation and acid–base balance, both of which influence heart rate, respiratory rate, and blood pressure. As a result, respiratory conditions often produce recognizable patterns across multiple vital signs.
For example, a patient with worsening asthma may develop tachypnea, tachycardia, and decreasing oxygen saturation before obvious clinical collapse occurs. Early recognition of these changes allows respiratory therapists to intervene promptly, potentially preventing respiratory failure.
Vital signs also help evaluate the effectiveness of respiratory therapies. Improvements in respiratory rate and oxygen saturation after treatment can confirm therapeutic benefit, while lack of improvement may prompt reassessment and escalation of care.
Importance of Trends Over Single Values
One of the most important principles in interpreting vital signs is focusing on trends rather than isolated numbers. A respiratory rate of 22 breaths per minute may not seem alarming on its own, but a steady increase from 16 to 22 over several hours may indicate progressive respiratory distress.
Respiratory therapists routinely monitor these trends, especially in patients receiving oxygen therapy, noninvasive ventilation, or mechanical ventilation. Subtle changes can provide early warning signs that allow for timely intervention and improved outcomes.
Accuracy and Measurement Considerations
Accurate vital sign measurement is essential. Factors such as patient movement, poor probe placement, improper cuff size, or observer error can lead to misleading values. Respiratory therapists must be skilled not only in interpreting vital signs but also in recognizing when a measurement may be unreliable.
Clinical judgment is crucial. If a vital sign does not match the patient’s clinical appearance, reassessment is warranted. For example, a normal oxygen saturation reading in a visibly cyanotic patient should prompt immediate reevaluation of probe placement and overall oxygenation status.
Role of Vital Signs in Clinical Communication
Vital signs serve as a common language among healthcare professionals. Clear reporting of abnormal values and trends allows respiratory therapists to communicate concerns effectively to nurses, physicians, and the broader care team.
In many cases, changes in vital signs are what trigger rapid response teams or escalation to higher levels of care. Respiratory therapists are often central participants in these situations, using their expertise to interpret respiratory-related changes and recommend appropriate interventions.
Vital Signs Practice Questions
1. What are the most common vital signs?
The most common vital signs are pulse rate, respiratory rate, blood pressure, body temperature, and oxygen saturation.
2. What is the normal pulse rate?
The normal pulse rate is 60–100 beats per minute.
3. Where can you find the pulse?
The pulse can be palpated at the radial, brachial, femoral, and carotid arteries.
4. What is the normal respiratory rate?
The normal respiratory rate is 12–20 breaths per minute.
5. What is the normal blood pressure?
Normal blood pressure ranges from 110–120 systolic over 70–80 diastolic.
6. What is the normal body temperature?
Normal body temperature varies by location: Oral: 97.7–99.5°F (36.5–37.5°C); Axillary: 96.7–98.5°F (35.9–36.9°C); Rectal or ear: 98.7–100.5°F (37.1–38.1°C).
7. What is the normal oxygen saturation?
Normal oxygen saturation is 95–99%, or above 93%.
8. What is the normal heart rate?
The normal heart rate is 60–100 beats per minute.
9. A low oxygen saturation is a good indicator of what?
Low oxygen saturation is an indicator of hypoxemia.
10. What are common complications with pulse oximeters?
Complications include low perfusion, incorrect probe placement, non-pulsating vascular beds, dark fingernail polish, and light interference.
11. What is the accuracy range on a pulse oximeter?
The accuracy range on a pulse oximeter is ±4%.
12. What is the heart rate for someone who is bradycardic?
A bradycardic heart rate is less than 60 beats per minute.
13. What is the respiratory rate for someone who is tachypneic?
A tachypneic respiratory rate is greater than 20 breaths per minute.
14. What is the blood pressure for someone with hypotension?
Hypotension is defined as blood pressure below 90/60.
15. What is the breathing pattern of someone who is apneustic?
Apneustic breathing is characterized by prolonged, gasping inhalations with inadequate exhalation.
16. What are the primary causes of eupnea?
Eupnea is simply the normal breathing pattern in healthy individuals.
17. Identify the following breathing pattern: fast and deep breaths with periods of apnea and no set rhythm.
This is known as Biot’s breathing.
18. Which breathing pattern is normal in newborns and elderly individuals but abnormal in healthy adults?
Cheyne-Stokes breathing is normal in newborns and the elderly but abnormal in healthy adults.
19. What tool is required for listening when performing a manual blood pressure measurement?
A stethoscope is required to listen during a manual blood pressure measurement.
20. Which part of a stethoscope allows a practitioner to hear sound during a manual blood pressure measurement?
The chest piece, specifically the diaphragm and bell, is used to hear sounds during blood pressure measurement.
21. What is the normal heart rate for a newborn?
The normal heart rate for a newborn is 90–180 beats per minute.
22. What describes a patient’s heart rate that is greater than 100 beats per minute?
A heart rate greater than 100 beats per minute is described as tachycardia.
23. What is DKA?
DKA stands for Diabetic Ketoacidosis, a condition caused by a shortage of insulin, which leads the body to burn fatty acids and produce acidic ketone bodies.
24. The pulse rate and rhythm can be measured by what?
Pulse rate and rhythm can be measured through auscultation or palpation of any accessible artery.
25. What arteries can be used to check the pulse?
The pulse can be checked at the radial, brachial, femoral, carotid, and pedal arteries.
26. Which artery is most commonly used to check for a pulse?
The radial artery is the most commonly used site for checking the pulse.
27. How is pulse calculated?
To calculate the pulse, count the beats for 15 seconds and multiply by 4 to obtain beats per minute.
28. How is respiratory rate measured?
Respiratory rate is measured by inspecting chest movement for a full minute.
29. What is the normal blood pressure for adults?
The normal blood pressure for adults is 110–120 systolic over 70–80 diastolic.
30. What device is used to measure blood pressure?
A sphygmomanometer is used to measure blood pressure.
31. What are the ways that body temperature can be measured?
Body temperature can be measured orally, rectally, and in the axillary region.
32. What is the normal body temperature?
Normal body temperature is approximately 37°C (98.6°F).
33. What is fever?
Fever, or hyperthermia, is a body temperature higher than the normal range.
34. What is the normal pulse rate for an adult?
The normal pulse rate for an adult is 60–100 beats per minute.
35. What does pulse oximetry estimate?
Pulse oximetry noninvasively estimates the oxygen saturation of hemoglobin in arterial blood.
36. What factors affect the accuracy of a pulse oximetry reading?
Factors affecting accuracy include movement, bright light, extreme cold, extreme darkness, and high levels of methemoglobin.
37. What would you call a respiratory rate less than 12?
Bradypnea
38. What would you call a respiratory rate greater than 20?
Tachypnea
39. What would you call a heart rate less than 60?
Bradycardia
40. What would you call a heart rate greater than 100?
Tachycardia
41. What is hypotension?
Hypotension is defined as blood pressure below 90/60.
42. What is hypertension?
Hypertension is defined as blood pressure above 140/90.
43. What is the normal pulse for a newborn?
The normal pulse for a newborn is 90–170 beats per minute.
44. What is the normal pulse for a 1-year-old?
The normal pulse for a 1-year-old is 80–160 beats per minute.
45. What is the normal pulse for a preschool-age child?
The normal pulse for a preschool-age child is 80–120 beats per minute.
46. What is the normal pulse for a 10-year-old?
The normal pulse for a 10-year-old is 70–110 beats per minute.
47. What is the normal pulse for an adult?
The normal pulse for an adult is 60–100 beats per minute.
48. What is systolic blood pressure?
Systolic blood pressure is the top number, measuring the pressure in the arteries when the heart beats.
49. What is diastolic blood pressure?
Diastolic blood pressure is the bottom number, measuring the pressure in the arteries when the heart is resting between beats.
50. How is the strength (amplitude) of a pulse measured on a scale?
Pulse strength is measured as follows: 4 – bounding, 3 – full, 2 – normal, 1 – diminished, and 0 – absent.
51. What is bradycardia?
Bradycardia is a slower-than-normal heart rate, defined as less than 60 beats per minute.
52. What is tachycardia?
Tachycardia is a faster-than-normal heart rate, defined as greater than 100 beats per minute.
53. What is hypotension?
Hypotension is low blood pressure, which can cause dizziness or fainting, defined as less than 90/60.
54. What is hypertension?
Hypertension is high blood pressure, which can lead to heart disease, defined as greater than 140/90.
55. What is eupnea?
Eupnea is a normal respiratory rate (12-20 breaths per minute) with a regular rhythm, reflecting normal physiology.
56. What is apnea?
Apnea is the absence of breathing, often caused by respiratory or cardiac arrest or increased intracranial pressure.
57. What are the types of pulse oximetry probes?
Types of pulse oximetry probes include finger, foot, toe, forehead, and ear probes.
58. Can cool or heated aerosols affect a body temperature reading?
Yes, both cool and heated aerosols can impact the accuracy of a body temperature reading.
59. Which vital signs provide information about gas exchange?
Oxygen saturation, heart rate, and respiratory rate provide information about gas exchange.
60. What test is helpful in addition to vital signs to assess a patient’s acid-base status?
An arterial blood gas (ABG) test is helpful for assessing acid-base status.
61. What is pulse pressure?
Pulse pressure is the difference between systolic and diastolic blood pressure, indicating the force the heart generates with each contraction.
62. What is considered a normal pulse pressure?
A normal pulse pressure is generally 30-40 mmHg.
63. What is mean arterial pressure (MAP)?
Mean arterial pressure (MAP) is the average pressure in the arteries during one cardiac cycle, important for assessing tissue perfusion.
64. How is mean arterial pressure (MAP) calculated?
MAP can be estimated with the formula: MAP = (Systolic BP + 2 * Diastolic BP) / 3.
65. What is the normal range for mean arterial pressure (MAP)?
A normal MAP range is 70-100 mmHg.
66. What is orthostatic hypotension?
Orthostatic hypotension is a drop in blood pressure when moving from lying down to standing, causing dizziness or lightheadedness.
67. What is the normal range for end-tidal CO2 (ETCO2)?
Normal end-tidal CO2 (ETCO2) ranges from 35-45 mmHg and is used to monitor ventilation.
68. What can cause a decrease in end-tidal CO2 levels?
Decreased ETCO2 levels can result from hyperventilation, pulmonary embolism, or decreased cardiac output.
69. How is core body temperature measured?
Core body temperature can be measured rectally, tympanically (ear), or using an esophageal probe.
70. What is pulse deficit?
Pulse deficit is the difference between the apical pulse and radial pulse, indicating a possible issue with heart function.
71. What is the normal capillary refill time?
Normal capillary refill time is less than 2 seconds, indicating adequate peripheral perfusion.
72. What is cyanosis, and what does it indicate?
Cyanosis is a bluish discoloration of the skin and mucous membranes, indicating low oxygen levels in the blood.
73. What can a high respiratory rate indicate?
A high respiratory rate can indicate conditions such as fever, anxiety, pain, or respiratory distress.
74. What is diurnal variation in body temperature?
Diurnal variation is the normal fluctuation in body temperature throughout the day, usually higher in the late afternoon and lower in the early morning.
75. How is pain assessed as a vital sign?
Pain is assessed using scales such as the Numeric Rating Scale (NRS) or Wong-Baker FACES, and it is often considered the “fifth vital sign.”
76. What is the significance of auscultating breath sounds?
Auscultating breath sounds helps detect abnormalities in the lungs, such as wheezing, crackles, or diminished sounds, indicating potential respiratory issues.
77. What does wheezing indicate when heard on auscultation?
Wheezing typically indicates airway obstruction or narrowing, as seen in conditions like asthma or COPD.
78. What does crackling (rales) sound like, and what does it indicate?
Crackling sounds (rales) are heard on inspiration and often indicate fluid in the lungs, common in pneumonia, heart failure, and pulmonary edema.
79. What is stridor, and what does it suggest?
Stridor is a high-pitched sound heard on inspiration, indicating an obstruction in the upper airway.
80. What is Kussmaul breathing, and what does it indicate?
An abnormal breathing pattern characterized by deep, labored breathing often associated with diabetic ketoacidosis (DKA) and other forms of metabolic acidosis.
81. What is the significance of Cheyne-Stokes breathing?
Cheyne-Stokes breathing, characterized by cyclic periods of apnea and hyperventilation, can indicate brain injury, heart failure, or stroke.
82. What is systolic hypertension?
Systolic hypertension is when the systolic blood pressure is consistently above 140 mmHg, increasing the risk of cardiovascular issues.
83. What is diastolic hypertension?
Diastolic hypertension is when the diastolic blood pressure is consistently above 90 mmHg, also associated with heart and kidney diseases.
84. What factors can influence respiratory rate?
Factors affecting respiratory rate include age, activity level, anxiety, pain, fever, and certain medications.
85. How does pain influence blood pressure?
Pain can cause an increase in blood pressure due to the body’s stress response.
86. What is the normal range for blood pressure in children?
Normal blood pressure in children varies by age but is generally lower than in adults, typically ranging from 90/60 to 110/70 mmHg.
87. What is hypothermia?
Hypothermia is a dangerously low body temperature, typically below 95°F (35°C), which can be life-threatening if not treated.
88. What is hyperthermia?
Hyperthermia is an elevated body temperature, often above 100.4°F (38°C), due to environmental or physical conditions like heat stroke.
89. What is the Glasgow Coma Scale (GCS) used for?
The GCS is used to assess a patient’s level of consciousness, scoring based on eye, verbal, and motor responses.
90. What does a bounding pulse indicate?
A bounding pulse may indicate high blood pressure, fever, or anxiety and suggests strong blood flow or hyperdynamic circulation.
91. What is the significance of a thready pulse?
A thready pulse is weak and difficult to palpate, potentially indicating dehydration, shock, or heart failure.
92. What is pulsus paradoxus?
Pulsus paradoxus is a drop in systolic blood pressure of more than 10 mmHg during inhalation, often seen in cardiac tamponade and severe asthma.
93. What are ronchi, and when are they typically heard?
Ronchi are low-pitched sounds, similar to snoring, indicating mucus or obstruction in the larger airways, often heard in bronchitis.
94. How does anxiety affect respiratory rate?
Anxiety can increase respiratory rate, leading to hyperventilation, which may cause dizziness or lightheadedness.
95. What is clubbing, and what can it indicate?
Clubbing is a thickening of the fingertips and nails, often indicating chronic low oxygen levels, as seen in lung disease and heart disease.
96. What is peripheral cyanosis?
Peripheral cyanosis is a bluish discoloration of the extremities due to poor oxygenation or blood flow in the hands and feet.
97. What is central cyanosis?
Central cyanosis is a bluish discoloration of the lips, tongue, and mucous membranes, indicating low oxygen saturation in the blood.
98. How does dehydration affect blood pressure?
Dehydration can cause low blood pressure (hypotension) due to reduced blood volume.
99. What is the difference between vesicular and bronchial breath sounds?
Vesicular breath sounds are soft and heard over most of the lungs, while bronchial sounds are louder and normally heard over the trachea and larger airways.
100. What is the purpose of capnography?
Capnography measures the concentration of CO2 in exhaled air, providing information about a patient’s ventilation status.
Final Thoughts
Vital signs form the backbone of patient assessment and monitoring in healthcare, particularly in respiratory care. They provide essential insight into how well the lungs, heart, and circulatory systems are functioning and often reveal early signs of deterioration.
For respiratory therapists, mastery of vital signs goes beyond memorizing normal ranges. It involves understanding physiology, recognizing patterns, and interpreting trends within the clinical context.
By using vital signs thoughtfully and consistently, respiratory therapists play a key role in early intervention, effective treatment, and improved patient outcomes across a wide range of clinical settings.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Sapra A, Malik A, Bhandari P. Vital Sign Assessment. [Updated 2023 May 1]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025.

