Excess phlegm after eating is a common but often misunderstood problem that can range from mildly annoying to persistently uncomfortable. Many people notice throat clearing, coughing, or a sensation of mucus buildup shortly after meals, yet are unsure why it happens or whether it signals a health concern.
In reality, post-meal phlegm can stem from several factors, including food sensitivities, acid reflux, postnasal drip, or underlying respiratory conditions.
Understanding how digestion, the immune system, and the airways interact helps explain why certain foods or eating habits trigger mucus production. This article explores the most common causes of phlegm after eating, associated symptoms, when to seek medical care, and practical ways to reduce and prevent it.
Download our free guide that has over 100+ of the best tips for healthy lungs.
What Causes Phlegm After Eating?
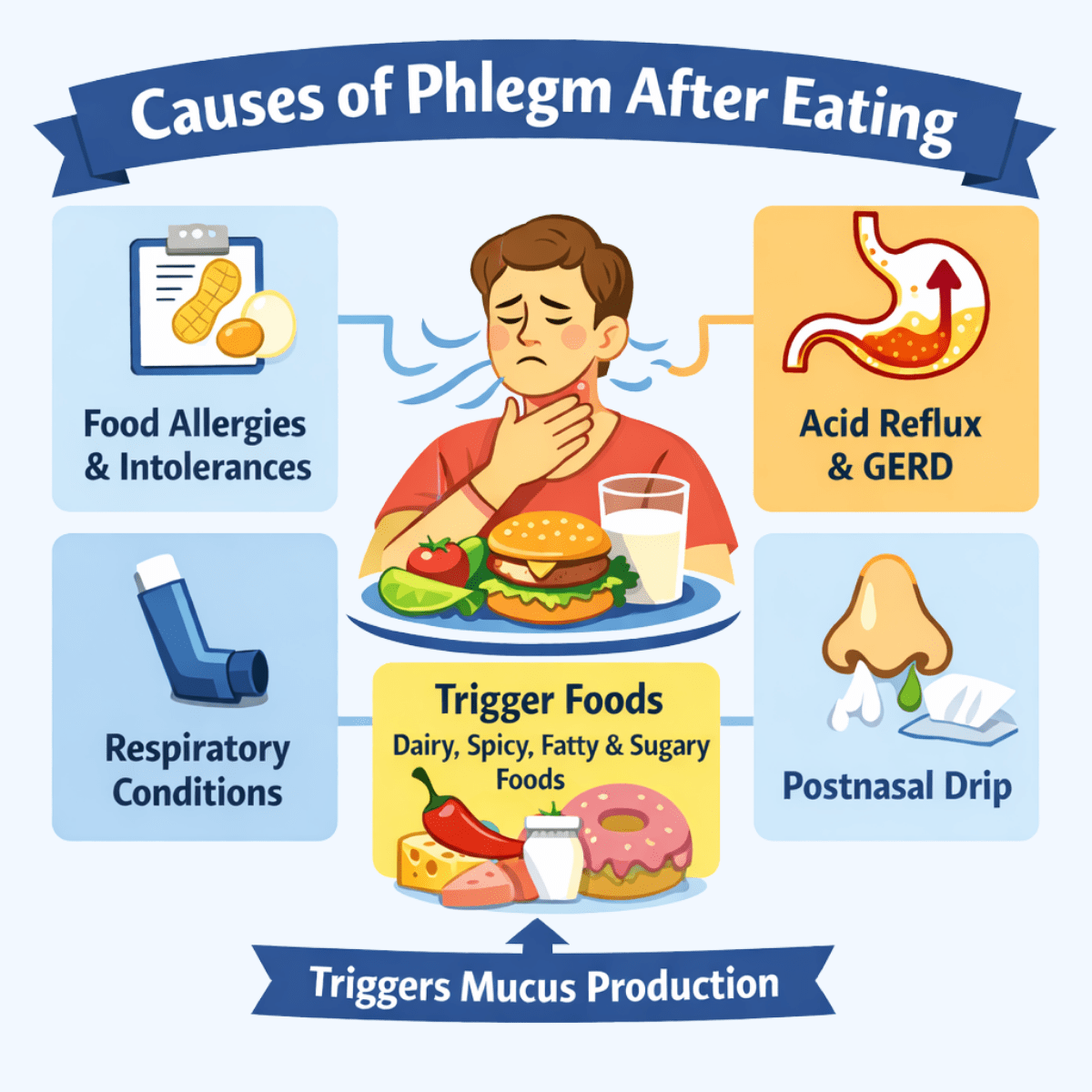
Phlegm after eating is typically caused by irritation or sensitivity in the digestive or respiratory systems. Common triggers include food allergies or intolerances, which can stimulate mucus production as the body reacts to certain ingredients.
Acid reflux and gastroesophageal reflux disease (GERD) are also frequent causes, as stomach acid can irritate the throat and prompt protective mucus secretion. Some foods, such as dairy, spicy meals, or high-fat and sugary foods, may thicken mucus or make it more noticeable.
Postnasal drip can also increase after eating, especially in people with sinus issues. In addition, underlying respiratory conditions like asthma or chronic sinusitis can heighten airway sensitivity, making phlegm more apparent after meals.
Food Allergies and Intolerances
Food allergies and intolerances can trigger mucus buildup as the body’s immune or digestive system reacts to specific ingredients. When someone with a food allergy, such as to milk, eggs, or nuts, eats that food, the immune system releases histamines that can cause inflammation in the airways and sinuses. This leads to excess mucus production and throat irritation.
Food intolerances, like lactose or gluten sensitivity, do not involve the immune system but can still cause similar symptoms. These reactions may irritate the gut or throat, prompting the body to secrete more phlegm.
In some cases, even mild sensitivities can create noticeable throat mucus if consumed repeatedly. People often find relief by identifying and avoiding specific trigger foods. Keeping a food diary can help track which meals or ingredients cause the problem.
Note: A physician or allergist can confirm sensitivities through elimination diets or blood tests for specific antibodies.
Acid Reflux and GERD
Acid reflux and gastroesophageal reflux disease (GERD) are frequent causes of post-meal phlegm. When stomach acid travels upward into the esophagus, it irritates the throat lining and prompts mucus production. This reaction protects the tissue from additional acid exposure but results in persistent throat clearing or a feeling of buildup.
Certain foods—such as fried foods, caffeine, citrus, and tomato-based dishes—can worsen this condition. Eating large portions or lying down soon after eating often makes symptoms more noticeable.
Managing reflux-related mucus involves adjusting meal habits. Smaller, earlier dinners, avoiding known triggers, and elevating the head during rest can reduce acid movement. For continued issues, physicians may recommend antacid or proton pump inhibitor (PPI) therapy to reduce acid levels and limit irritation.
Postnasal Drip Triggered by Food
Some foods can cause temporary nasal congestion and excess mucus drainage into the throat, known as postnasal drip. Spicy foods containing capsaicin or hot soups can increase nasal secretions as part of the body’s natural cooling response. For others, dairy or high-fat items may thicken mucus and make it more noticeable.
People who experience frequent postnasal drip after meals might have sensitivities to temperature or spice levels rather than an immune issue. In this case, mucus production increases briefly and then subsides once the trigger food clears.
Note: Drinking water during meals can help thin mucus and reduce discomfort. If nasal congestion is frequent, saline sprays or antihistamines may relieve swelling and slow mucus flow.
Respiratory Conditions Related to Eating
Existing respiratory conditions, such as asthma, chronic bronchitis, or chronic obstructive pulmonary disease (COPD), can make mucus more noticeable after eating. For example, certain foods or strong aromas may stimulate airway inflammation and increase mucus secretion. Cold beverages or high-fat meals can also cause airway constriction, leading to coughing or throat congestion.
People with asthma may find symptoms worsen when eating around known triggers like sulfites in wine or preservatives in processed foods. The body’s airway sensitivity causes inflammation that produces thicker mucus and short-term breathing discomfort.
Monitoring patterns between meals and breathing changes can help identify aggravating factors. Healthcare providers may adjust inhaler routines or suggest dietary changes that minimize airway irritation after eating.
Common Foods That Increase Phlegm Production
Certain foods can cause the body to produce more mucus, making phlegm feel thicker or more noticeable after eating. Ingredients that trigger extra mucus often contain specific proteins, fats, or chemical compounds that can irritate the throat or stimulate mucus glands.
Dairy Products
Dairy products such as milk, cheese, and cream can make mucus feel thicker in some individuals. This effect relates to the emulsified fat and protein content that can coat the mouth and throat, leaving a sticky sensation often mistaken for increased phlegm. While dairy doesn’t directly cause mucus overproduction in everyone, people sensitive to milk proteins may experience more noticeable buildup.
Individuals with mild lactose intolerance may also have irritation in the upper airways. This irritation can prompt the body to release mucus as a protective reaction. Low-fat or lactose-free dairy versions can reduce the effect for sensitive individuals.
When congestion worsens after consuming dairy, limiting intake of high-fat products like whole milk or aged cheese can help. Keeping track of symptoms through a food diary can assist in identifying whether dairy plays a role.
Spicy Foods
Spicy foods containing chili peppers, hot sauces, or wasabi can briefly increase mucus flow. Capsaicin, the compound that creates heat in spices, irritates the mucous membranes in the mouth, throat, and nasal passages. This stimulation encourages glands to release mucus and thin secretions to flush out the irritant.
Although the reaction is temporary, it can make phlegm more noticeable immediately after eating. For those with chronic throat clearing or sinus congestion, the effect may feel uncomfortable. Drinking water or milk can reduce the irritation more effectively than ignoring it.
Some people benefit from mild spice intake since it can help loosen mucus, but larger amounts often worsen post-meal symptoms. Moderation and attention to tolerance levels are key.
Sugary and Processed Foods
Foods with high sugar levels or refined carbohydrates, including soft drinks, pastries, and packaged snacks, may promote thicker mucus. Large sugar intake can influence inflammation and lead to stickier secretions that linger in the throat. Processed foods often contain additives and preservatives that dry or irritate mucous membranes.
Artificial sweeteners, flavor enhancers, and trans fats can further stress the respiratory system in sensitive individuals. This may trigger mild swelling in nasal or throat tissues, increasing mucus sensation after eating. Reducing these foods can gradually decrease the stickiness of phlegm over time.
Replacing sugary desserts with fresh fruit, whole grains, or unsweetened yogurt helps maintain mucus balance while improving hydration and digestion.
Medical Conditions Linked to Phlegm After Eating
Certain respiratory and digestive disorders can cause phlegm to increase after eating. These conditions often involve inflammation, mucus overproduction, or reflux that irritates the throat and airways.
Sinusitis
Sinusitis causes inflammation of the sinus lining, leading to trapped mucus that can drip down the back of the throat. This postnasal drip may become more pronounced after meals, especially if the food is hot or spicy. Eating can stimulate blood flow and mucus secretion in the nasal passages, intensifying symptoms.
People with chronic sinusitis often notice congestion, facial pressure, and thick nasal discharge. When mucus drains after eating, it can create a sensation of phlegm buildup in the throat. Identifying sinus infections or chronic irritation helps prevent ongoing discomfort.
Treatment usually includes nasal saline rinses, prescribed corticosteroid sprays, or antibiotics when bacterial infection is confirmed. Managing allergies, staying hydrated, and avoiding irritants like smoke can further reduce mucus accumulation and improve nasal drainage.
Asthma
Asthma involves airway inflammation and hypersensitivity that can worsen after consuming certain foods or drinks. Temperature changes from hot or cold meals and additives like sulfites may narrow airways or trigger excess mucus production. This can leave a lingering feeling of phlegm or cough shortly after eating.
People with asthma often experience wheezing, shortness of breath, and a tight chest, but digestive triggers can make throat clearing more frequent. In some cases, aspiration of trace food particles or reflux-related irritation worsens airway inflammation.
Managing asthma-related phlegm includes following a doctor-prescribed inhaler regimen and identifying dietary triggers. Recording symptoms after meals can help find connections between foods and post-meal mucus buildup. Stable asthma management generally reduces post-eating respiratory symptoms.
Laryngopharyngeal Reflux (LPR)
Laryngopharyngeal reflux (LPR) occurs when stomach acid or digestive enzymes move up into the throat, irritating the larynx and pharynx. Unlike classic acid reflux, LPR often lacks heartburn but can produce persistent throat clearing, hoarseness, and thick mucus after meals.
The phlegm results from tissue irritation that prompts protective mucus formation. Symptoms frequently worsen after eating fatty foods, caffeine, or late-night meals. Swallowing may feel difficult, and mucus may seem hard to clear.
Treatment focuses on lessening reflux episodes through dietary modification, elevating the head during sleep, and possibly using acid-suppressing medication. When managed well, inflammation subsides, and mucus production typically decreases.
Symptoms Accompanying Phlegm After Eating
Some people experience additional discomfort when phlegm builds up after meals. These symptoms often involve reactions in the throat and voice that can indicate irritation or mild inflammation.
Coughing or Throat Clearing
Frequent coughing or repeated throat clearing soon after eating may signal that mucus is thickening in the throat or upper airway. When digestion triggers excess mucus, it can cause a need to clear the throat to restore normal airflow. This behavior may become habitual if the underlying cause is not addressed.
People often notice that these episodes occur after eating dairy, fried foods, or meals high in fat or spice. The body may respond by increasing mucus production to protect the throat from irritation. If coughing continues even after drinking water or changing posture, it can suggest postnasal drip or acid reflux rather than a short-term reaction.
Persistent throat clearing can irritate the vocal cords further. Over time, this may lead to mild soreness or a tickling sensation that reinforces the urge to cough. Monitoring meal-related patterns helps narrow down food sensitivities or reflux as triggers.
Sore Throat or Hoarseness
A sore throat or voice change after eating often results from stomach acid or mucus affecting the larynx. When acid reflux or postnasal drip reaches the throat, it can cause swelling and mild inflammation. The tissue may feel dry or tender, and the voice might sound rough or strained.
Individuals sometimes describe needing to strain to speak clearly after meals. This usually improves once the throat is cleared or after drinking water. Mucus coating the vocal cords can interfere with vibration, leading to temporary hoarseness or reduced vocal strength.
Note: If these symptoms occur frequently, they may indicate irritation from gastroesophageal reflux disease (GERD) or chronic sinus drainage. Reducing acid-triggering foods, eating smaller portions, and staying upright after meals can minimize the discomfort and restore normal throat function.
When to See a Doctor About Phlegm After Eating
Medical attention becomes important when phlegm after meals signals underlying conditions rather than a temporary reaction. Recognizing warning signs early can prevent complications and help identify causes like allergies, reflux, or respiratory issues.
Signs of Severe Allergic Reaction
Phlegm that develops suddenly after eating may point to a food allergy. If this occurs alongside hives, facial swelling, dizziness, wheezing, or difficulty breathing, immediate medical care is needed. These symptoms can indicate anaphylaxis, a life-threatening emergency that requires prompt treatment with epinephrine and evaluation at the hospital.
Even mild allergic reactions should not be ignored when they repeat after specific foods such as shellfish, nuts, eggs, or dairy. Over time, exposure can cause stronger responses. A doctor may recommend allergy testing to identify triggers and prescribe medications or dietary changes to prevent recurrence.
Note: If throat tightness or changes in voice occur, the airway could be narrowing. Anyone experiencing these signs should seek emergency medical help rather than waiting for them to pass.
Persistent or Worsening Symptoms
Phlegm that lingers for weeks or grows thicker and more frequent after meals may signal a chronic condition. Gastroesophageal reflux disease (GERD), chronic sinus inflammation, or infections can increase mucus production. Ongoing symptoms may also include chest discomfort, hoarseness, or coughing after eating.
When phlegm appears even without illness or persists despite hydration and home care, a physician can assess for structural or digestive problems through imaging or endoscopy. Persistent issues can sometimes stem from sinus blockages, postnasal drip, or food sensitivities.
Note: Medical review becomes essential if mucus production interferes with swallowing, breathing, or daily comfort. Early evaluation helps manage symptoms and prevent long-term irritation of the throat and airways.
Diagnosis of Excess Phlegm After Meals
Doctors determine the cause of phlegm after eating by reviewing symptoms, examining potential allergic or digestive triggers, and using diagnostic tests that show how the upper airways and gastrointestinal tract function. Identifying the source often involves comparing symptom patterns with findings from imaging or endoscopic evaluations.
Medical History and Symptom Tracking
Clinicians start by gathering a detailed medical history to identify possible causes. They ask about the timing of phlegm buildup, types of foods eaten, and any coexisting symptoms such as coughing, heartburn, or throat irritation. This helps distinguish between digestive and respiratory origins.
Patients may be asked to keep a food and symptom diary for one to two weeks. Recording what is eaten, how soon phlegm develops, and other sensations—like postnasal drip or acid taste—can reveal patterns.
A review of past conditions such as sinusitis, asthma, or gastroesophageal reflux disease (GERD) often helps. Doctors may also review medication use, smoking habits, and exposure to environmental irritants. Together, this background directs which diagnostic steps are most useful.
Allergy Testing
If symptoms appear linked to specific meals or ingredients, allergy testing is often recommended. Food allergens can increase mucus production in the throat and upper airway. Skin prick tests or blood tests measuring IgE antibody levels help identify possible triggers like dairy, wheat, eggs, or nuts.
Results are interpreted alongside the patient’s food diary and clinical history. A positive allergen response indicates that avoidance trials or dietary adjustments could clarify whether allergies contribute to mucus buildup.
In some cases, oral food challenges under medical supervision confirm or exclude the suspected allergen. Testing also distinguishes between food intolerance and immune-mediated allergy, which require different management approaches.
Endoscopy and Imaging
When symptoms persist despite initial evaluation, doctors may perform endoscopic or imaging studies. A flexible nasoendoscopy lets specialists view the nasal passages, throat, and upper airway for signs of inflammation, mucus pooling, or structural issues.
If reflux-related causes are suspected, an upper endoscopy may assess the esophagus and stomach lining for irritation or swelling. Imaging techniques such as CT scans or barium swallow studies can reveal sinus blockages, anatomical abnormalities, or hiatal hernias affecting post-meal mucus flow.
Note: These tests provide direct visualization and help confirm whether the source of excess phlegm arises from airway obstruction, reflux disease, or another underlying condition.
Treatment Options for Reducing Phlegm After Eating
Reducing phlegm after meals often involves managing underlying triggers such as diet, mucus overproduction, and lifestyle habits that worsen throat congestion. Effective strategies can include targeted dietary changes, appropriate medication, and practical adjustments to daily routines.
Dietary Adjustments
Certain foods and eating habits can increase mucus production or thicken existing phlegm. Individuals often find relief by identifying and limiting trigger foods such as dairy, fried items, and processed sugars. These foods can irritate the throat and stimulate excess secretion.
Eating in smaller portions helps reduce reflux, which can indirectly lessen post-meal mucus. Choosing warm, non-acidic beverages instead of cold or sugary drinks may soothe the throat and ease mucus movement. Maintaining a balanced diet rich in vegetables, lean proteins, and whole grains supports overall digestive comfort.
People who experience chronic phlegm may benefit from hydrating throughout the day. Water helps thin mucus, making it easier to clear. Avoiding dehydration by limiting caffeine and alcohol also improves mucus consistency. Keeping the diet simple and minimally processed often yields noticeable improvement.
Medications
When dietary changes are not sufficient, medications can provide additional relief. Expectorants such as guaifenesin make mucus thinner and easier to expel. For those with acid reflux, proton pump inhibitors (PPIs) or H2 blockers may reduce stomach acid that aggravates throat irritation and mucus buildup.
In cases of allergies or sinus involvement, antihistamines and nasal corticosteroids can help control inflammation and postnasal drip. However, sedating antihistamines may dry mucus excessively, so non-drowsy options are often preferred. Physicians may suggest saline sprays for gentle nasal moisture balance.
Medication use should align with a doctor’s evaluation, especially for persistent or severe symptoms. Combining treatments under medical guidance helps avoid unnecessary or overlapping drug effects that might worsen dryness or irritation.
Lifestyle Modifications
Daily habits influence how much mucus forms after eating. Keeping an upright posture for at least 30 minutes after meals can prevent reflux-related mucus buildup. Those who smoke should stop, as smoking irritates airway linings and triggers chronic mucus production.
Humidifying the air at home or work can ease mucus clearance by keeping airways moist. Regular gentle exercise supports lung and digestive function, reducing the chance of congestion after eating. Breathing exercises can further help expel residual phlegm.
Consistent sleep habits and stress management also contribute. Stress affects digestion and respiratory patterns, sometimes worsening mucus symptoms. Making these adjustments gradually allows the body to adapt and respond more effectively to other treatments.
Home Remedies to Manage Phlegm
Simple daily habits can help reduce mucus buildup and make it easier for the body to clear phlegm. Adjusting fluid intake, using humid air, and applying saline rinses or gargles can all support comfortable throat and airway function.
Hydration
Drinking enough fluids keeps the mucus thin and easier to expel. Water should be the main source, as sugary or caffeinated drinks may cause mild dehydration. Warm liquids such as herbal teas, broths, or warm water with honey and lemon can soothe throat irritation while aiding mucus clearance.
A person should aim for regular sips throughout the day rather than large amounts at once. For many adults, 6–8 cups of water can serve as a general guide, though needs vary with activity and climate. Clear, pale urine usually indicates sufficient hydration.
Alcohol and caffeinated beverages can be enjoyed in moderation, but they shouldn’t replace water. Staying continuously hydrated prevents phlegm from becoming thick and sticky, reducing coughing and throat discomfort.
Humidification
Dry indoor air often worsens congestion and throat irritation. Using a cool-mist humidifier during sleep or throughout the day helps maintain moisture in the airways. The device should be cleaned every 1–2 days to prevent bacterial or mold buildup.
Taking a warm shower or inhaling steam from a bowl of hot water is another practical option, especially if a humidifier is unavailable. These methods can help loosen mucus, making it easier to clear the chest and throat.
For safety, individuals should avoid direct contact with hot steam to prevent burns. Maintaining indoor humidity between 40–50% provides comfort without encouraging mold growth. This balance improves breathing and reduces throat irritation caused by dry environments.
Enjoy personalized, quiet comfort with this smart humidifier that adapts to your home’s needs, ensuring optimal moisture levels and relief from dry air.
Salt Water Gargles
A salt water gargle helps clear mucus and soothe throat tissues. To prepare, dissolve ½ teaspoon of salt in a cup of warm water. Gargle for 15–30 seconds, then spit out the mixture. This can be repeated up to several times a day as needed.
Salt creates a mild hypertonic solution that draws excess fluid and irritants from the throat lining. It also helps loosen mucus and flush away allergens or food particles that may contribute to phlegm production.
Using warm, not hot, water ensures comfort and prevents irritation. People with high blood pressure or sodium restrictions should avoid swallowing the solution. Regular gargling can provide noticeable relief from lingering mucus after meals.
Prevention Tips for Phlegm After Meals
Eating habits play a major role in reducing post-meal phlegm. They should eat slowly and chew food thoroughly to ease digestion and reduce throat irritation. Smaller bites and mindful eating can help prevent mucus buildup.
Avoiding foods that trigger excessive mucus may also help. Common culprits include dairy products, fried foods, and highly processed snacks. Some people notice fewer symptoms when they limit sugary drinks or alcohol.
Staying hydrated supports thinner mucus that clears more easily. Drinking water before and after meals, rather than during, can prevent a feeling of congestion. Warm fluids such as herbal tea may soothe throat irritation.
Maintaining good posture while eating and remaining upright for at least 30 minutes afterward can minimize reflux-related mucus. Propping the body upright while sitting or taking a gentle walk can aid digestion and comfort.
Environmental changes also make a difference. Keeping indoor air moist but not humid, avoiding smoke, and reducing exposure to strong fragrances or allergens can limit throat irritation and mucus formation.
FAQs About Phlegm After Eating
Why Do I Get Phlegm in My Throat After I Eat?
Phlegm after eating usually occurs when food triggers irritation or inflammation in the throat, airways, or digestive system. Common causes include acid reflux, food sensitivities, postnasal drip, or underlying respiratory conditions.
When stomach acid, allergens, or certain food components irritate the throat, the body responds by producing mucus as a protective mechanism. This can create a sensation of buildup, throat clearing, or coughing shortly after meals. The specific trigger often depends on the type of food eaten and individual sensitivities.
Is It Normal to Have Phlegm After Eating?
Yes, having some phlegm after eating can be normal, especially if it happens occasionally and resolves quickly. Certain foods, such as dairy or spicy meals, can temporarily thicken mucus or make it more noticeable. Eating large meals, eating too quickly, or lying down soon after eating can also contribute.
However, frequent or persistent phlegm after meals may suggest acid reflux, allergies, sinus issues, or respiratory conditions and may warrant further evaluation if symptoms interfere with comfort or daily life.
Why Does Mucus Come Out of My Throat After I Eat?
Mucus may come out of your throat after eating because digestion or food exposure stimulates mucus glands in the throat and upper airways. Acid reflux can irritate the throat lining, prompting protective mucus secretion.
Postnasal drip may also increase after meals, allowing mucus from the sinuses to drain into the throat. In some cases, airway sensitivity or mild inflammation causes mucus to loosen and become more noticeable when swallowing, coughing, or clearing the throat.
Why Do I Get Phlegm After Eating Dairy?
Dairy products can make phlegm feel thicker in some people due to their fat and protein content, which may coat the mouth and throat. This sensation is often mistaken for increased mucus production.
In others, a milk protein sensitivity or lactose intolerance can cause irritation that triggers mucus secretion. While dairy does not universally increase mucus, people who notice consistent symptoms after consuming milk, cheese, or cream may benefit from reducing intake or choosing low-fat or lactose-free options.
What Is the Cause of Excess Mucus in the Throat?
Excess mucus in the throat is commonly caused by postnasal drip, acid reflux, allergies, respiratory infections, or chronic inflammation. Environmental irritants like smoke or dry air can also stimulate mucus production.
Conditions such as sinusitis, asthma, or laryngopharyngeal reflux can lead to ongoing throat mucus due to persistent irritation. Dehydration may further thicken mucus, making it feel excessive even if production has not significantly increased.
What Disease Causes Excessive Mucus Production?
Several medical conditions can cause excessive mucus production, including chronic sinusitis, asthma, chronic bronchitis, gastroesophageal reflux disease (GERD), and laryngopharyngeal reflux (LPR). Allergic rhinitis and respiratory infections can also increase mucus output.
In rare cases, conditions like cystic fibrosis affect mucus thickness and clearance. Identifying the underlying disease is important, as treatment focuses on reducing inflammation, controlling triggers, and improving mucus clearance rather than simply suppressing symptoms.
How Do You Stop the Overproduction of Mucus in Your Throat?
Reducing throat mucus often involves treating the underlying cause. Staying well hydrated helps thin mucus and make it easier to clear. Avoiding trigger foods, especially dairy, spicy foods, and acid-producing items, can reduce irritation.
Managing acid reflux with smaller meals and upright posture after eating is helpful. For allergies or sinus issues, antihistamines or saline rinses may help. If mucus persists, a healthcare provider can recommend targeted treatment based on the cause.
Final Thoughts
Phlegm after eating is usually a manageable issue once its underlying cause is identified. Whether it stems from food sensitivities, acid reflux, postnasal drip, or existing respiratory conditions, the body is often responding to irritation or inflammation in the throat and airways.
Paying attention to symptom patterns, making targeted dietary and lifestyle adjustments, and staying well hydrated can significantly reduce discomfort for many people.
When symptoms persist, worsen, or interfere with breathing or swallowing, medical evaluation is important to rule out chronic conditions and guide appropriate treatment. With the right approach, most individuals can minimize post-meal mucus buildup and restore comfort and confidence during and after meals.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Butler LM, Koh WP, Lee HP, Tseng M, Yu MC, London SJ; Singapore Chinese Health Study. Prospective study of dietary patterns and persistent cough with phlegm among Chinese Singaporeans. Am J Respir Crit Care Med. 2006.



