Evaluating a patient’s sputum is an important clinical skill for respiratory therapists because changes in sputum color, consistency, odor, and volume can provide valuable clues about underlying respiratory diseases. Careful sputum assessment helps identify infections, airway inflammation, pulmonary edema, and other lung disorders, allowing clinicians to initiate timely and appropriate treatment.
For the respiratory therapy board exam, students must recognize key sputum characteristics and understand their clinical significance. For example, green, foul-smelling secretions may indicate a lung abscess, while pink, frothy sputum is commonly associated with pulmonary edema.
This guide reviews the most commonly tested sputum characteristics, their associated conditions, and practical board exam tips to help students confidently interpret sputum findings during exam scenarios and in clinical practice.
Take our free course to learn essential tips, insights, and strategies to pass the TMC Exam on your first (or next) attempt.
Understanding Sputum Characteristics
Sputum production is part of the respiratory system’s natural defense mechanism. Mucus helps trap inhaled particles, bacteria, and other irritants so they can be cleared from the airways. However, changes in sputum appearance may indicate underlying respiratory pathology.
Evaluating sputum involves assessing several characteristics, including color, thickness, odor, and volume. Each feature may provide clues that help narrow the differential diagnosis.
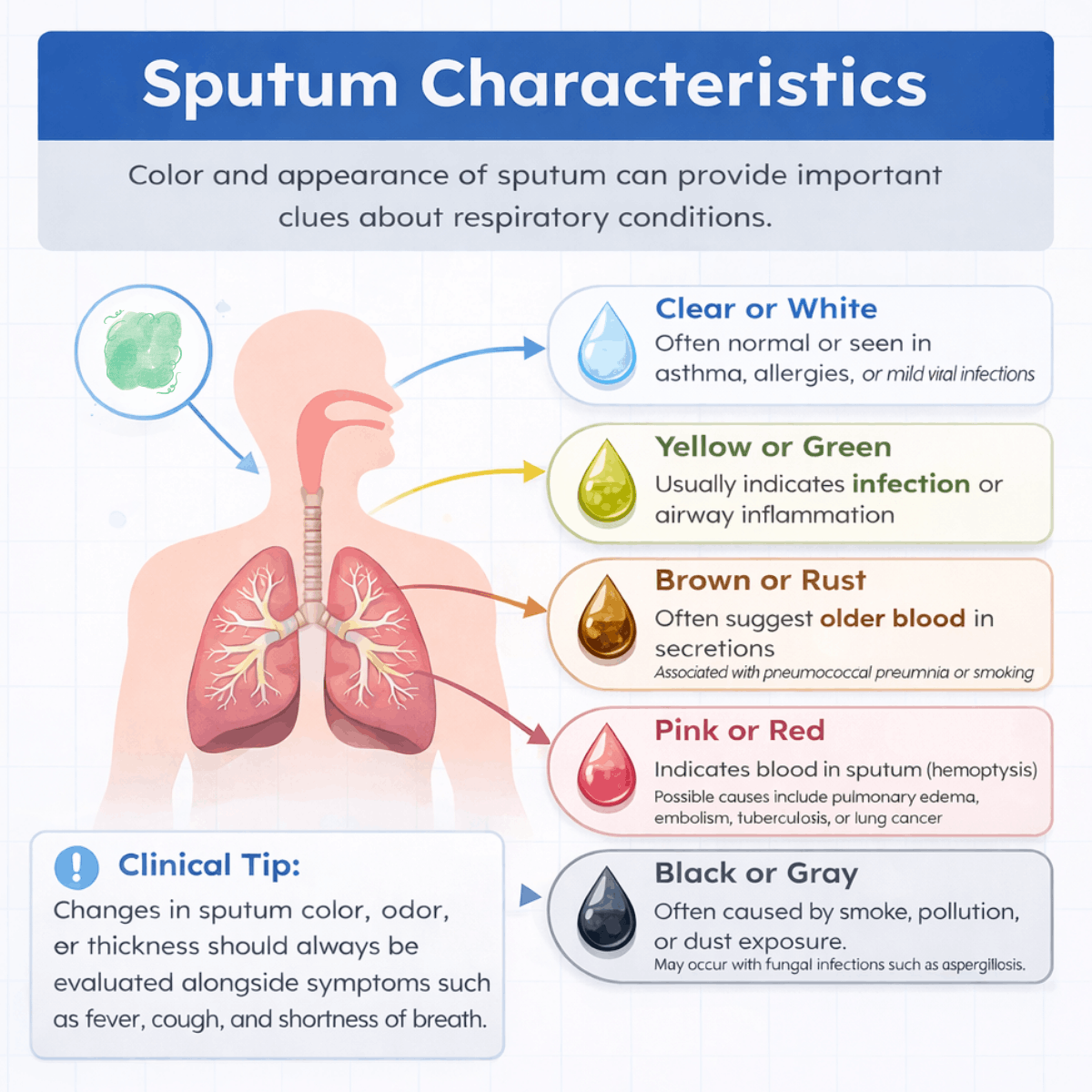
Below are the sputum findings most commonly tested on the board exam and encountered in clinical practice.
1. White or Clear Sputum
- Significance: Often considered normal or associated with nonbacterial conditions.
- Example: Clear or white sputum may be seen in patients with asthma, allergies, or mild viral respiratory infections.
2. Yellow or Green Sputum
- Significance: Usually indicates infection or inflammation within the respiratory tract.
- Examples: Yellow sputum may occur in viral infections or mild bacterial bronchitis. Thick green sputum is commonly associated with bacterial pneumonia. If the sputum is green and foul-smelling, it may suggest a lung abscess caused by anaerobic bacteria.
3. Brown or Rust-Colored Sputum
- Significance: Often indicates the presence of older blood within airway secretions.
- Examples: Rust-colored sputum is classically associated with pneumococcal pneumonia. Brown sputum may also occur in chronic bronchitis, smokers, or patients with previous airway bleeding.
4. Pink or Red-Tinged Sputum
- Significance: Indicates the presence of blood, which may range from mild irritation to serious pathology.
- Examples: Pink, frothy sputum is a hallmark sign of pulmonary edema, often resulting from left-sided heart failure. Bright red sputum may indicate hemoptysis caused by conditions such as pulmonary embolism, tuberculosis, bronchiectasis, or lung cancer.
5. Black or Gray Sputum
- Significance: Usually caused by inhalation of environmental particles or fungal infections.
- Example: Heavy smokers, coal miners, or individuals exposed to significant air pollution may produce dark sputum. Certain fungal infections, including aspergillosis, can also lead to dark-colored secretions.
Sputum Consistency and Odor
In addition to color, the texture, thickness, and smell of sputum can provide additional diagnostic information.
1. Frothy (Bubbly) Sputum
- Significance: Often associated with pulmonary edema due to fluid accumulation within the alveoli.
- Example: Pink, frothy sputum is commonly seen in patients with left-sided heart failure or severe fluid overload.
2. Thick, Tenacious Sputum
- Significance: Indicates impaired mucus clearance or dehydration.
- Example: Thick sputum is frequently observed in chronic bronchitis, asthma, and cystic fibrosis.
3. Purulent (Pus-Filled) Sputum
- Significance: Suggests bacterial infection accompanied by inflammation and neutrophil accumulation.
- Example: Purulent sputum is commonly seen in bronchiectasis, lung abscesses, and severe bacterial pneumonia.
4. Foul-Smelling or Fetid Sputum
- Significance: Often indicates infection with anaerobic bacteria and possible tissue necrosis.
- Example: Lung abscesses frequently produce green, foul-smelling sputum. Patients with bronchiectasis may also produce large amounts of malodorous secretions due to chronic infection.
5. Large Volume Sputum Production
- Significance: Suggests conditions associated with excessive mucus production.
- Example: Bronchiectasis and lung abscesses may produce copious amounts of purulent sputum. Pulmonary edema can also cause sudden increases in pink, frothy secretions.
Take our free course to learn essential tips, insights, and strategies to pass the Clinical Simulation Exam (CSE) on your first (or next) attempt.
Board Exam Tips for Sputum Evaluation
Questions about sputum characteristics frequently appear on the respiratory therapy board exam. These questions typically present a short clinical scenario that describes sputum color, odor, consistency, or volume. Your task is to identify the most likely diagnosis based on these clues.
To answer these questions correctly, focus on recognizing common sputum patterns and understanding the conditions they most strongly suggest.
1. Memorize Key Color and Disease Associations
Many board exam questions require matching sputum color with a specific respiratory condition. Learning the most common associations can help you quickly eliminate incorrect answer choices.
- Rust-colored sputum → Pneumococcal pneumonia (Streptococcus pneumoniae)
- Pink, frothy sputum → Pulmonary edema
- Green sputum → Bacterial infection such as pneumonia
- Green, foul-smelling sputum → Lung abscess
- Yellow sputum → Mild infection, asthma, or bronchitis
- Brown sputum → Chronic bronchitis or previous airway bleeding
- Black sputum → Smoke inhalation, environmental exposure, or fungal infection
Note: Remembering these associations helps you quickly identify the correct answer when sputum color is the main clue in a clinical scenario.
2. Pay Attention to Odor Descriptions
Board exam questions sometimes include details about sputum odor. This information can strongly suggest a specific diagnosis.
- Foul-smelling sputum often indicates anaerobic bacterial infection, such as a lung abscess or severe bronchiectasis.
- Sweet-smelling sputum may suggest infection with Pseudomonas aeruginosa, which is commonly associated with cystic fibrosis.
Note: When an exam question describes sputum with a strong or offensive odor, consider infections involving tissue necrosis or chronic bacterial colonization.
3. Recognize When Hemoptysis Is Concerning
Blood-streaked sputum or frank hemoptysis can signal a range of respiratory conditions. Some causes are relatively mild, while others require urgent evaluation.
Important conditions associated with hemoptysis include:
- Pulmonary embolism with sudden chest pain and shortness of breath
- Tuberculosis with chronic cough, night sweats, and weight loss
- Lung cancer with persistent hemoptysis and smoking history
- Bronchiectasis with recurrent infections and blood-streaked sputum
Note: In severe cases of hemoptysis, patients may require oxygen therapy, airway protection, and bronchoscopy for evaluation and management.
4. Differentiate Conditions With Similar Sputum Findings
Some respiratory conditions can produce similar sputum characteristics. In these cases, the patient’s history and accompanying symptoms help determine the most likely diagnosis.
- Asthma vs. bronchitis: Both conditions may produce yellow sputum, but asthma is more likely when wheezing and a history of allergies are present.
- Pulmonary edema vs. pneumonia: Both may cause dyspnea. Pulmonary edema is more likely if the patient produces pink, frothy sputum and has a history of heart failure. Pneumonia is more likely when fever, chills, and purulent sputum are present.
- Lung abscess vs. bronchiectasis: Both can cause foul-smelling sputum. Lung abscess typically involves localized lung necrosis, whereas bronchiectasis causes chronic airway dilation with recurrent infections.
Note: Carefully reading the entire clinical scenario helps identify additional clues that distinguish between similar conditions.
5. Evaluate Sputum Volume and Consistency
Some board exam questions emphasize sputum quantity or texture rather than color. Recognizing the significance of these descriptions can guide the correct diagnosis.
- Large-volume sputum suggests bronchiectasis or lung abscess rather than pneumonia.
- Thick, tenacious sputum is commonly associated with cystic fibrosis or chronic bronchitis.
- Thin, frothy sputum strongly indicates pulmonary edema.
6. Watch for Trick Questions
Exam questions sometimes include misleading information designed to test your clinical reasoning. Carefully analyze all details before selecting an answer.
- If sputum is yellow but there are no signs of infection, asthma may be more likely than pneumonia.
- If blood-streaked sputum is mentioned without severe symptoms, chronic bronchitis may be considered before more severe diagnoses.
- If foul-smelling sputum is described without mention of color, conditions such as lung abscess or bronchiectasis should still be considered.
Note: Carefully reading the full question and avoiding assumptions will help prevent common mistakes on the board exam.
Take our free course to master essential pathology concepts with TMC/CSE exam tips and helpful practice questions.
Final Thoughts
Understanding sputum characteristics is an essential skill for respiratory therapists. Changes in sputum color, odor, consistency, and volume can provide important clues about a patient’s respiratory condition.
Recognizing these patterns helps clinicians identify conditions such as pneumonia, bronchiectasis, lung abscess, and pulmonary edema. It also supports faster clinical decision-making in urgent situations such as hemoptysis or severe infection.
For students preparing for the respiratory therapy board exam, mastering these associations allows for quicker interpretation of case scenarios and more confident selection of correct answers. Developing this knowledge will also strengthen clinical judgment and improve patient care in real-world respiratory practice.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Spies R, Potter M, Hollamby R, van der Walt S, Hohlfeld A, Ochodo E, Van Zyl-Smit R. Sputum Color as a Marker for Bacteria in Acute Exacerbations of Chronic Obstructive Pulmonary Disease: A Systematic Review and Meta-analysis. Ann Am Thorac Soc. 2023.




