Flail chest is a serious thoracic injury that significantly disrupts normal respiratory mechanics and gas exchange. It most commonly results from high-energy blunt trauma and is associated with substantial morbidity and mortality.
For respiratory therapists, understanding flail chest is essential because these patients often require aggressive pain management, advanced airway support, and careful ventilatory monitoring.
Early recognition and appropriate respiratory care interventions can prevent complications such as respiratory failure, pneumonia, and prolonged mechanical ventilation.
What is Flail Chest?
Flail chest occurs when at least three or more adjacent ribs are fractured in two or more places, creating a free-floating segment of the thoracic wall. This unstable segment loses its structural continuity with the surrounding chest wall and moves independently during respiration.
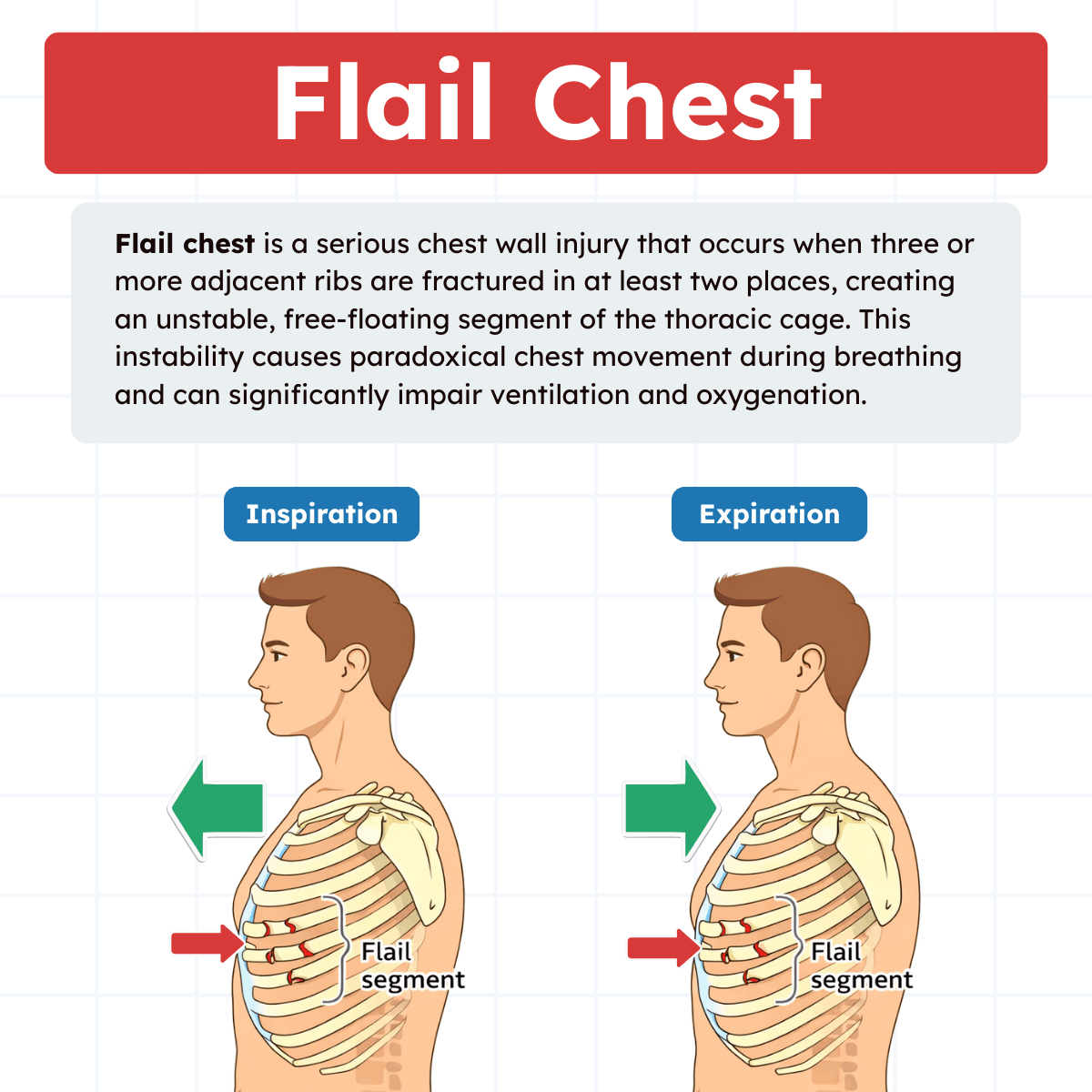
The defining clinical feature of flail chest is paradoxical chest movement. During inspiration, when intrathoracic pressure becomes negative, the flail segment moves inward instead of outward. During exhalation, when pressure becomes positive, the segment moves outward. This abnormal motion interferes with effective ventilation and increases the work of breathing.
Flail chest is typically the result of blunt trauma such as motor vehicle collisions, falls, or crush injuries. It may also be seen in severe physical assaults or industrial accidents. The presence of flail chest often indicates significant force and raises concern for associated injuries.
Pathophysiology and Respiratory Impairment
The mechanical instability of the chest wall directly impairs normal ventilation. Effective breathing depends on coordinated expansion of the rib cage and diaphragm. When part of the chest wall moves paradoxically, several problems arise:
- Reduced tidal volume due to ineffective chest expansion
- Increased work of breathing
- Pain-limited ventilation
- Impaired cough and secretion clearance
In addition to the mechanical problem, pulmonary contusion frequently accompanies flail chest. Pulmonary contusion involves bruising of lung tissue, leading to alveolar hemorrhage, inflammation, and impaired gas exchange. This can cause hypoxemia that may worsen over the first 24 to 48 hours.
The combination of chest wall instability and lung injury often leads to ventilation-perfusion mismatch. Patients may develop hypoxemia despite adequate oxygen delivery. If untreated, respiratory failure can occur.
Clinical Presentation
Patients with flail chest typically present with:
- Severe chest pain
- Visible paradoxical chest wall motion
- Tachypnea
- Shallow breathing
- Hypoxemia
- Crepitus from rib fractures
Pain is often intense and leads to splinting, which further reduces tidal volume. As ventilation decreases, carbon dioxide retention may develop. In more severe cases, patients can show signs of respiratory distress such as accessory muscle use, cyanosis, or altered mental status.
The presence of multiple or bilateral rib fractures, fracture of the first rib, or a flail segment suggests high-energy trauma. These patients are at increased risk for both respiratory and circulatory failure. Associated injuries such as pneumothorax, hemothorax, or major vascular trauma must be considered.
Diagnostic Evaluation
Diagnosis is based on clinical findings and imaging studies.
Physical Examination
Observation of paradoxical chest movement is highly suggestive of flail chest. Palpation may reveal rib instability or crepitus. Auscultation may show decreased breath sounds if pneumothorax or hemothorax is present.
Imaging
Chest radiography can identify rib fractures and associated complications such as pneumothorax or hemothorax. However, computed tomography is more sensitive and can better define the extent of rib fractures and pulmonary contusions.
Respiratory therapists may also assess arterial blood gases to evaluate oxygenation and ventilation status. Progressive hypoxemia or hypercapnia may signal worsening respiratory compromise.
Complications
Flail chest carries a high risk of complications, including:
- Pneumothorax from laceration of the visceral pleura
- Hemothorax due to internal pleural bleeding
- Pneumohemothorax
- Pulmonary contusion
- Pneumonia
- Acute respiratory failure
Patients receiving anticoagulant therapy are particularly vulnerable to internal bleeding. Accumulation of blood in the pleural cavity requires prompt drainage via chest tube placement. Ongoing bleeding must be monitored closely, and surgical evaluation may be necessary.
Note: Untreated pain and inadequate ventilation increase the risk of atelectasis and pneumonia. These complications can prolong hospital stay and increase mortality.
Management and Treatment
The management of flail chest focuses on stabilizing respiratory function, controlling pain, and addressing associated injuries.
Pain Control
Effective pain management is essential. Without adequate analgesia, patients will not breathe deeply or cough effectively. Options may include:
- Systemic opioids
- Regional nerve blocks
- Epidural analgesia
Note: Improved pain control enhances tidal volume, reduces atelectasis, and lowers the risk of pneumonia.
Oxygen Therapy
Supplemental oxygen is commonly required. Respiratory therapists must titrate oxygen to maintain appropriate saturation while monitoring for signs of worsening hypoxemia.
Noninvasive Support
Continuous positive airway pressure can help stabilize the flail segment by providing internal pneumatic support. Positive pressure reduces paradoxical movement and improves oxygenation. Noninvasive ventilation may be appropriate in select patients who remain hemodynamically stable and able to protect their airway.
Invasive Mechanical Ventilation
Some patients require intubation and invasive mechanical ventilation. Indications include:
- Severe hypoxemia
- Hypercapnia with respiratory acidosis
- Increased work of breathing
- Altered mental status
- Hemodynamic instability
Note: Positive pressure ventilation effectively stabilizes the chest wall internally and allows the injured ribs to heal. However, prolonged mechanical ventilation carries risks such as ventilator-associated pneumonia.
Surgical Stabilization
In certain cases, surgical fixation of rib fractures may be considered. Surgical stabilization can improve chest wall mechanics and reduce time on mechanical ventilation. Decisions regarding surgery involve trauma surgeons and multidisciplinary teams.
Relevance to Respiratory Therapists
Flail chest has direct implications for respiratory therapists in acute care settings.
Airway and Ventilation Management
Respiratory therapists are responsible for assessing ventilation adequacy, monitoring arterial blood gases, and determining when escalation of support is required. Recognition of worsening gas exchange is critical.
Implementation of Positive Pressure Therapy
Therapists play a key role in initiating and managing CPAP or mechanical ventilation. Proper ventilator settings must balance adequate oxygenation with lung protective strategies, especially when pulmonary contusion is present.
Secretion Management
Due to pain and shallow breathing, patients are prone to secretion retention. Respiratory therapists assist with airway clearance techniques, incentive spirometry, and monitoring for atelectasis.
Monitoring for Complications
Continuous assessment for signs of pneumothorax, hemothorax, or worsening respiratory failure is part of routine respiratory care. Sudden changes in breath sounds, oxygen saturation, or ventilator pressures require immediate attention.
Collaboration in Trauma Care
Flail chest patients are typically managed in trauma or intensive care units. Respiratory therapists collaborate with physicians, nurses, and surgeons to optimize respiratory support and prevent complications.
Prognosis
The prognosis of flail chest depends on the severity of associated injuries, the extent of pulmonary contusion, patient age, and comorbid conditions. Elderly patients have higher mortality rates due to reduced physiologic reserve.
Early pain control, aggressive pulmonary hygiene, and appropriate ventilatory support significantly improve outcomes. Advances in trauma care and mechanical ventilation have reduced mortality compared to historical data.
Flail Chest Practice Questions
1. What is a flail chest?
Flail chest is a condition in which three or more adjacent ribs are fractured in two or more places, creating a free-floating segment of the chest wall that moves independently during respiration.
2. What mechanical abnormality characterizes flail chest?
Paradoxical chest wall movement.
3. How does a flail segment move during inspiration?
It moves inward due to negative intrathoracic pressure.
4. How does a flail segment move during exhalation?
It moves outward as intrathoracic pressure becomes positive.
5. Why does paradoxical motion impair ventilation?
Because it reduces effective chest expansion and decreases tidal volume.
6. What is the most common cause of flail chest?
Blunt thoracic trauma, such as motor vehicle collisions.
7. Why does flail chest increase the work of breathing?
Because chest wall instability requires greater muscular effort to maintain ventilation.
8. What associated lung injury commonly accompanies flail chest?
Pulmonary contusion
9. What occurs in a pulmonary contusion?
Alveolar hemorrhage, inflammation, and impaired gas exchange.
10. Why can hypoxemia worsen 24–48 hours after injury?
Because pulmonary contusion may progress over time.
11. How does flail chest contribute to ventilation-perfusion mismatch?
By combining impaired chest mechanics with injured lung tissue.
12. What respiratory pattern is commonly observed in patients with flail chest?
Rapid, shallow breathing.
13. Why do patients with flail chest often have shallow respirations?
Severe chest pain leads to splinting.
14. What arterial blood gas abnormality may develop if ventilation is inadequate?
Hypercapnia
15. What physical exam finding strongly suggests flail chest?
Visible paradoxical movement of a chest wall segment.
16. What additional sign may be palpated over fractured ribs?
Crepitus
17. Why must pneumothorax be considered in patients with flail chest?
Rib fragments may lacerate the visceral pleura.
18. What imaging study is most sensitive for detecting rib fractures and pulmonary contusion?
Computed tomography (CT) of the chest.
19. What complication results from bleeding into the pleural space?
Hemothorax
20. Why are patients on anticoagulant therapy at higher risk?
They are more susceptible to significant internal bleeding.
21. What intervention is required for a large hemothorax?
Chest tube placement for drainage.
22. How does flail chest affect cough effectiveness?
Pain and instability impair secretion clearance.
23. What complication may develop from poor secretion clearance?
Pneumonia
24. Why does flail chest increase the risk of respiratory failure?
Due to combined chest wall instability and lung injury.
25. What does the presence of first rib fractures suggest?
High-energy trauma with risk of major associated injuries.
26. What circulatory complication may accompany severe thoracic trauma?
Shock from associated vascular injury.
27. How does decreased tidal volume affect alveolar ventilation?
It reduces effective gas exchange.
28. What is a pneumohemothorax?
The presence of both air and blood in the pleural space.
29. Why is pain management critical in flail chest?
Adequate analgesia improves ventilation and reduces complications.
30. What sign may indicate worsening respiratory distress?
Use of accessory muscles or altered mental status.
31. Why are arterial blood gases important in flail chest management?
They assess oxygenation and ventilation status.
32. What long-term pulmonary complication may occur without adequate treatment?
Atelectasis
33. How does paradoxical movement interfere with diaphragmatic function?
It disrupts coordinated thoracoabdominal mechanics.
34. What is the primary mechanical defect in flail chest?
Loss of structural continuity of the chest wall.
35. Why is early recognition of flail chest important?
To prevent progression to respiratory failure and associated complications.
36. What are the primary goals in the management of flail chest?
To stabilize respiratory function, control pain, and treat associated injuries.
37. Why is adequate pain control essential in patients with flail chest?
Because uncontrolled pain limits deep breathing and effective coughing, increasing the risk of atelectasis and pneumonia.
38. What are common methods of analgesia used in flail chest management?
Systemic opioids, regional nerve blocks, and epidural analgesia.
39. How does improved analgesia affect tidal volume?
It increases tidal volume by allowing deeper, less painful respirations.
40. Why is supplemental oxygen frequently required in a flail chest?
To correct hypoxemia resulting from ventilation-perfusion mismatch and pulmonary contusion.
41. What is the role of the respiratory therapist in oxygen therapy for flail chest?
To titrate oxygen appropriately and monitor for worsening hypoxemia or respiratory distress.
42. How does continuous positive airway pressure (CPAP) help stabilize a flail segment?
By providing internal pneumatic stabilization through positive pressure.
43. What effect does positive pressure have on paradoxical chest movement?
It reduces or eliminates paradoxical motion.
44. In which patients may noninvasive ventilation be considered?
Hemodynamically stable patients who can protect their airway and maintain adequate mental status.
45. What are common indications for endotracheal intubation in flail chest?
Severe hypoxemia, hypercapnia with respiratory acidosis, increased work of breathing, altered mental status, or hemodynamic instability.
46. How does invasive mechanical ventilation stabilize the chest wall?
By applying positive pressure that internally supports the unstable segment.
47. What is a major risk associated with prolonged mechanical ventilation?
Ventilator-associated pneumonia (VAP)
48. When may surgical stabilization of rib fractures be indicated?
In cases of severe instability, failure to wean from ventilation, or persistent respiratory compromise.
49. How can surgical fixation benefit patients with flail chest?
It can improve chest wall mechanics and reduce time on mechanical ventilation.
50. What is the respiratory therapist’s role in airway and ventilation management for flail chest?
To assess ventilation, monitor blood gases, and determine when escalation of support is needed.
51. Why is monitoring arterial blood gases important in these patients?
To evaluate oxygenation, ventilation, and acid-base status.
52. What ventilator strategy is important when pulmonary contusion is present?
Lung-protective ventilation with careful monitoring of pressures and volumes.
53. Why are flail chest patients prone to secretion retention?
Pain and shallow breathing impair effective coughing.
54. What airway clearance strategies may be used in flail chest?
Incentive spirometry, assisted coughing, and other pulmonary hygiene techniques.
55. What sudden change may suggest the development of a pneumothorax?
Abrupt decrease in breath sounds or oxygen saturation.
56. Why is continuous monitoring critical in trauma patients with flail chest?
Because complications such as pneumothorax, hemothorax, or respiratory failure can develop rapidly.
57. In which hospital setting are flail chest patients commonly managed?
In trauma units or intensive care units.
58. What factors influence the prognosis of flail chest?
Severity of associated injuries, extent of pulmonary contusion, age, and comorbid conditions.
59. Why do elderly patients have higher mortality rates with flail chest?
They have reduced physiologic reserve and increased vulnerability to complications.
60. What management strategies have improved outcomes in flail chest over time?
Early pain control, aggressive pulmonary hygiene, and appropriate ventilatory support.
61. What mechanism most commonly causes flail chest?
High-energy blunt thoracic trauma such as motor vehicle collisions.
62. How many rib fractures are required to define a flail segment?
At least three consecutive ribs fractured in two or more places.
63. Why is pulmonary contusion commonly associated with flail chest?
Because the same blunt force that fractures ribs often bruises underlying lung tissue.
64. Over what time frame may hypoxemia from pulmonary contusion worsen?
Within the first 24 to 48 hours after injury.
65. How does paradoxical movement affect minute ventilation?
It reduces effective tidal volume and increases the work of breathing.
66. Why may patients with flail chest develop hypercapnia?
Due to hypoventilation from pain, fatigue, or lung injury.
67. What physical exam finding is classic for flail chest?
Visible inward movement of the injured segment during inspiration.
68. Why is the first rib fracture considered concerning in trauma?
It suggests high-force impact and possible associated vascular injury.
69. How does splinting contribute to respiratory complications?
It limits chest expansion, leading to shallow breathing and atelectasis.
70. What acid-base disturbance may develop if ventilation is inadequate?
Respiratory acidosis
71. Why is early mobilization important in flail chest management?
It helps reduce pulmonary complications such as atelectasis and pneumonia.
72. What ventilator parameter should be closely monitored in patients with pulmonary contusion?
Plateau pressure
73. Why is lung-protective ventilation recommended in flail chest with contusion?
To minimize ventilator-induced lung injury.
74. How can excessive intravenous fluids worsen respiratory status in flail chest?
They may increase pulmonary edema and impair gas exchange.
75. What imaging modality is most sensitive for detecting pulmonary contusion?
Computed tomography (CT)
76. Why is incentive spirometry beneficial in stable flail chest patients?
It promotes deeper breaths and prevents alveolar collapse.
77. What complication can result from sharp rib fragments?
Laceration of the lung leading to pneumothorax.
78. What is a hemothorax?
Accumulation of blood in the pleural space.
79. How does positive end-expiratory pressure (PEEP) benefit flail chest patients?
It helps keep alveoli open and improves oxygenation.
80. Why must hemodynamics be monitored during positive pressure ventilation?
Because increased intrathoracic pressure can reduce venous return and cardiac output.
81. What sign may indicate worsening respiratory fatigue?
Increasing respiratory rate with decreasing tidal volumes.
82. Why is frequent reassessment necessary in flail chest?
Because respiratory status can deteriorate rapidly.
83. What type of respiratory failure is most common in severe flail chest?
Hypoxemic respiratory failure
84. How does chest wall instability affect cough effectiveness?
It reduces the ability to generate adequate expiratory force.
85. What bedside tool can assess oxygenation trends continuously?
Pulse oximetry
86. Why are elderly patients at increased risk of pneumonia after rib fractures?
Due to decreased cough strength and reduced lung reserve.
87. What clinical sign may indicate developing atelectasis?
Diminished breath sounds in affected areas.
88. How does paradoxical motion influence intrathoracic pressure changes?
It disrupts normal pressure gradients needed for effective ventilation.
89. Why is multidisciplinary care important in flail chest management?
Because treatment often involves trauma surgeons, intensivists, nurses, and respiratory therapists.
90. What ventilator mode is commonly used in patients requiring full support?
Assist/control ventilation
91. Why should excessive tidal volumes be avoided in flail chest?
To prevent barotrauma and volutrauma.
92. What role does arterial blood gas analysis play in management?
It helps evaluate oxygenation, ventilation, and acid-base balance.
93. How can inadequate pain control delay recovery?
It limits pulmonary hygiene and increases complication risk.
94. What is the purpose of chest tube placement in flail chest?
To evacuate air or blood from the pleural space.
95. Why may bilateral flail segments be especially dangerous?
They significantly compromise overall chest wall stability.
96. What respiratory pattern is commonly observed in flail chest?
Rapid, shallow breathing.
97. How can sedation improve ventilator synchrony?
By reducing anxiety and excessive respiratory effort.
98. What long-term complication can develop if flail chest is poorly managed?
Chronic pain and reduced pulmonary function.
99. Why is early identification of respiratory deterioration critical?
Because timely intervention reduces morbidity and mortality.
100. What is the overall goal of respiratory management in flail chest?
To maintain adequate oxygenation and ventilation while minimizing complications.
Final Thoughts
Flail chest is a severe thoracic injury characterized by paradoxical chest wall movement resulting from multiple rib fractures. The condition disrupts normal respiratory mechanics and is frequently associated with pulmonary contusion and other traumatic complications.
For respiratory therapists, flail chest represents a complex clinical scenario that demands careful assessment, effective pain management strategies, and appropriate ventilatory support.
Early recognition and timely intervention can prevent respiratory failure and improve patient outcomes. A thorough understanding of this condition is essential for providing safe and effective respiratory care in trauma settings.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Perera TB, Alahmadi MH, King KC. Flail Chest. 2025 Jun 22. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025.

