Hypoxemia refers to a decrease in the partial pressure of oxygen in arterial blood, indicating impaired oxygenation at the level of the lungs. It is a common and clinically significant problem encountered in a wide range of conditions, from acute respiratory failure to chronic lung disease.
Because oxygen is essential for cellular metabolism, even mild reductions in arterial oxygen levels can have important physiological consequences.
Understanding the underlying causes and mechanisms of hypoxemia is essential for accurate diagnosis, effective treatment, and improving patient outcomes in both acute and chronic care settings.
What Is Hypoxemia?
Hypoxemia is a condition in which the level of oxygen in the arterial blood is lower than normal. It is typically measured by the partial pressure of oxygen (PaO2) or oxygen saturation (SpO2). Oxygen is essential for the body’s cells to produce energy, so when levels drop, organs may not function properly.
Hypoxemia is different from hypoxia, which refers to low oxygen at the tissue level, although one can lead to the other. It can result from problems with breathing, lung function, blood flow, or the environment.
Common symptoms include shortness of breath, rapid breathing, and fatigue. If left untreated, hypoxemia can lead to serious complications, including organ damage and death.
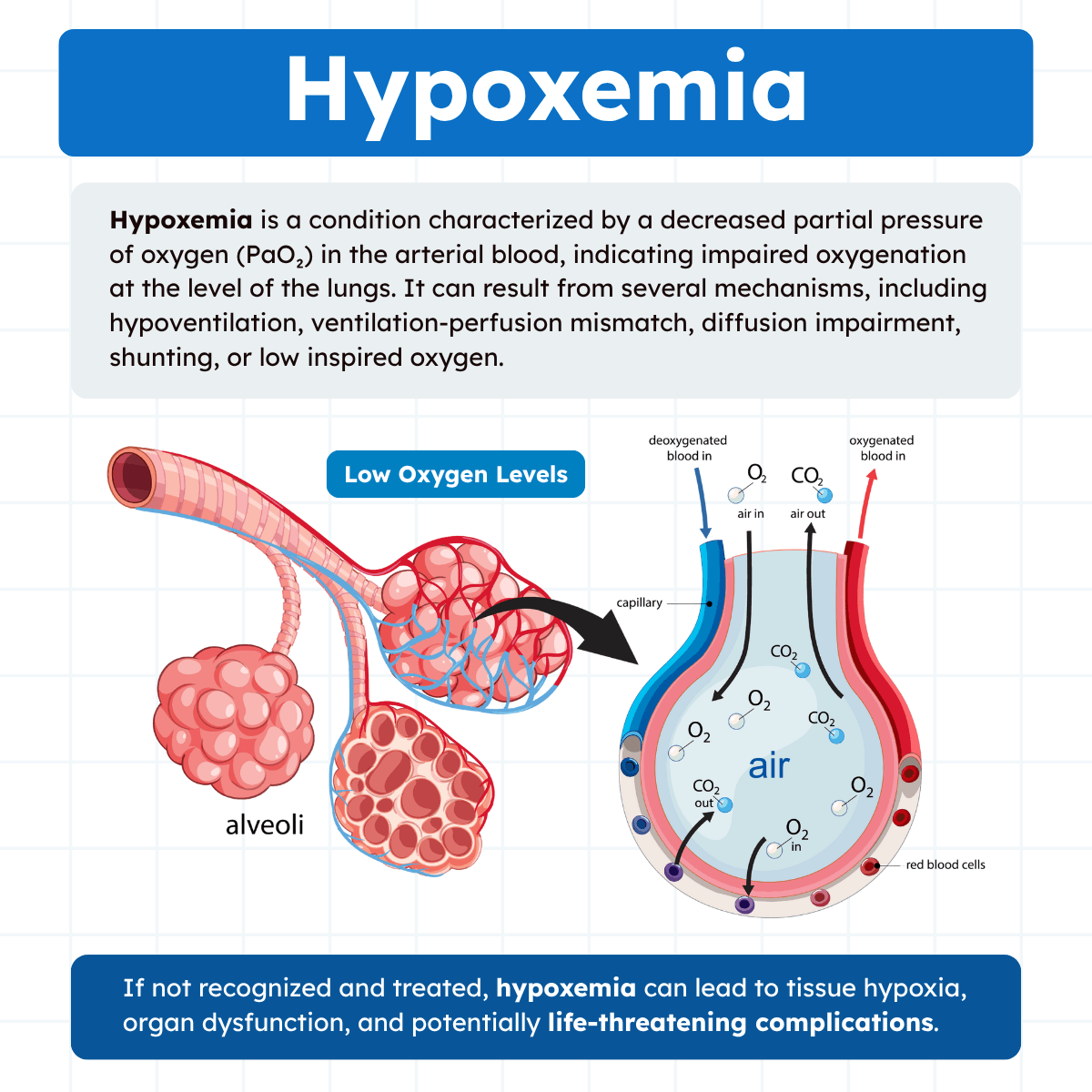
Hypoxemia vs. Hypoxia
Hypoxemia refers specifically to low oxygen levels in arterial blood, whereas hypoxia describes inadequate oxygen delivery to the tissues. While hypoxemia can lead to hypoxia, tissue hypoxia may also occur in the presence of a normal PaO₂ when other factors impair oxygen delivery or utilization.
Arterial oxygenation depends on several factors, including:
- The partial pressure of inspired oxygen (PiO₂)
- Alveolar ventilation
- Diffusion of oxygen across the alveolar-capillary membrane
- Ventilation-perfusion matching
- The presence or absence of shunting
Note: A disruption in any of these components can result in hypoxemia.
Normal Oxygenation and Age-Related Changes
Oxygen levels in the blood are not static throughout life. As individuals age, there is a gradual decline in PaO₂, even in the absence of disease. This is primarily due to subtle changes in lung structure and function, including:
- Reduced alveolar surface area
- Increased ventilation-perfusion mismatch
- Decreased elastic recoil
A commonly used estimate for expected PaO₂ is:
Expected PaO₂ = 100 − (0.3 × age)
For example, a 60-year-old adult may have a normal PaO₂ of approximately 85 mm Hg. This value would be considered abnormal in a younger individual but appropriate for someone of that age.
Note: Because of this variability, clinicians must interpret arterial blood gas values in the context of the patient’s age and clinical condition.
Overview of the Major Causes of Hypoxemia
Hypoxemia can arise from several distinct mechanisms. These are typically grouped into five primary categories:
- Low inspired oxygen (low PiO₂)
- Hypoventilation
- Diffusion impairment
- Ventilation-perfusion (V/Q) mismatch
- Right-to-left shunt
Note: Each mechanism affects oxygenation in a different way and has unique clinical implications.
Low Inspired Oxygen (Low PiO₂)
Low inspired oxygen occurs when the amount of oxygen available in the environment is reduced. This leads to a decrease in PiO₂, which in turn lowers alveolar oxygen tension (PAO₂) and ultimately arterial oxygen tension (PaO₂).
One of the most common causes of low PiO₂ is high altitude. As barometric pressure decreases with altitude, the partial pressure of oxygen in the air also declines, even though the fraction of inspired oxygen remains constant.
This reduction in barometric pressure leads to:
- Decreased PiO₂
- Decreased PAO₂
- Decreased PaO₂
Note: Despite this drop in oxygen levels, the alveolar-arterial oxygen gradient (DA–aO₂) remains normal because the problem originates from reduced oxygen availability rather than impaired gas exchange.
Clinical Example
A classic example is altitude exposure. Individuals traveling to high elevations may develop symptoms such as:
- Shortness of breath
- Headache
- Fatigue
- Dizziness
Note: This condition is often referred to as altitude sickness.
Key Features
- Low PaO₂
- Normal DA–aO₂ gradient
- Improves with supplemental oxygen
Hypoventilation
Hypoventilation occurs when alveolar ventilation is insufficient to remove carbon dioxide effectively. As a result, PaCO₂ increases, which leads to a decrease in PAO₂. This relationship is explained by the alveolar gas equation, where an increase in CO₂ reduces the amount of oxygen available in the alveoli.
Key effects include:
- Increased PaCO₂
- Decreased PAO₂
- Decreased PaO₂
Note: In hypoventilation, the DA–aO₂ gradient remains normal because the primary issue is reduced ventilation rather than impaired diffusion or mismatch.
Causes of Hypoventilation
Hypoventilation can result from a variety of conditions, including:
- Central nervous system depression from drug overdose or sedation
- Neuromuscular disorders such as Guillain-Barré syndrome
- Chest wall abnormalities
- Severe obesity
Clinical Example
A patient with an opioid overdose may experience respiratory depression, leading to elevated PaCO₂ and decreased PaO₂.
Key Features
- High PaCO₂
- Low PaO₂
- Normal DA–aO₂ gradient
- Rapid improvement with increased ventilation
Diffusion Impairment
Diffusion impairment occurs when the transfer of oxygen from the alveoli to the pulmonary capillary blood is limited. This is typically due to damage or thickening of the alveolar-capillary membrane.
Conditions that impair diffusion include:
- Pulmonary fibrosis
- Emphysema
- Interstitial lung disease
- Pulmonary edema
Note: In these conditions, oxygen has difficulty crossing the membrane, especially during periods of increased demand such as exercise.
Physiological Impact
Even when alveolar oxygen levels are normal, diffusion limitation can prevent adequate oxygen uptake, resulting in:
- Decreased PaO₂
- Increased DA–aO₂ gradient
Note: Unlike hypoventilation, diffusion impairment leads to a widened gradient between alveolar and arterial oxygen levels.
Clinical Considerations
Diffusion limitation is often more pronounced during exercise because blood flows more rapidly through the pulmonary capillaries, reducing the time available for oxygen transfer.
At rest, pure diffusion impairment is a relatively uncommon cause of significant hypoxemia. However, it often contributes to hypoxemia in combination with other mechanisms.
Key Features
- Low PaO₂
- Increased DA–aO₂ gradient
- Improves with supplemental oxygen
Ventilation-Perfusion (V/Q) Mismatch
Ventilation-perfusion mismatch is the most common cause of hypoxemia in patients with lung disease. It occurs when the amount of air reaching the alveoli is not appropriately matched with the amount of blood flowing through the surrounding pulmonary capillaries.
In a healthy lung, ventilation and perfusion are not perfectly uniform, but they are balanced well enough to maintain effective gas exchange. In disease states, this relationship becomes more uneven. Some lung units may receive adequate perfusion but too little ventilation, while others may be well ventilated but poorly perfused.
When ventilation is reduced relative to perfusion, blood leaves those lung units with a lower oxygen content. Even if other parts of the lung are functioning normally, they cannot fully compensate for the poorly ventilated regions. This is because hemoglobin is already nearly saturated in the well-ventilated units, limiting how much additional oxygen can be carried. As a result, the mixed arterial blood has a reduced oxygen content and a lower PaO₂.
Why V/Q Mismatch Causes Hypoxemia
The effect of V/Q mismatch is best understood by considering what happens in different lung regions:
- A low V/Q unit has inadequate ventilation relative to perfusion
- A normal V/Q unit has balanced ventilation and perfusion
- A high V/Q unit has more ventilation than perfusion
Blood leaving low V/Q units remains underoxygenated. Blood leaving high V/Q units cannot make up for this deficit because oxygen content does not increase substantially once hemoglobin is nearly fully saturated.
Note: This is why V/Q mismatch causes hypoxemia even when some parts of the lung appear to be overventilated.
Common Causes
V/Q mismatch is seen in many pulmonary disorders, including:
- Chronic obstructive pulmonary disease
- Asthma
- Pneumonia
- Pulmonary edema
- Atelectasis
- Pulmonary embolism
Note: Although pulmonary embolism is often associated with increased dead space, it can also contribute to overall gas exchange abnormalities and hypoxemia.
Clinical Features
Patients with V/Q mismatch often present with:
- Low PaO₂
- Increased alveolar-arterial oxygen gradient
- Improvement with supplemental oxygen
Note: This last feature is important. Because at least some alveoli are still being ventilated, increasing the fraction of inspired oxygen can often improve arterial oxygenation.
Right-to-Left Shunt
A right-to-left shunt occurs when blood passes from the right side of the circulation to the left without being exposed to ventilated alveoli. As a result, deoxygenated venous blood mixes with oxygenated arterial blood, lowering the overall oxygen content and PaO₂.
Shunts can be divided into two general categories:
- Anatomic shunts
- Physiologic shunts
An anatomic shunt occurs when blood bypasses the lungs entirely or travels through abnormal vascular connections. Examples include certain forms of congenital heart disease.
A physiologic shunt occurs when blood flows through pulmonary capillaries that are associated with alveoli receiving no ventilation. In this case, perfusion is present, but ventilation is absent. This represents the extreme form of V/Q mismatch, where the ratio approaches zero.
Examples of Shunt
Common causes of physiologic shunt include:
- Atelectasis
- Severe pneumonia
- Pulmonary edema
- Acute respiratory distress syndrome
Common causes of anatomic shunt include:
- Congenital cardiac defects with right-to-left flow
- Pulmonary arteriovenous malformations
Why Shunt Is Different
Unlike many other forms of hypoxemia, shunt does not respond well to supplemental oxygen. If blood completely bypasses ventilated alveoli, increasing inspired oxygen has limited benefit because the shunted blood never comes into contact with alveolar gas.
Note: This is a key clinical clue. A patient with severe hypoxemia that does not improve much with oxygen therapy may have a significant shunt.
Clinical Features
Shunt-related hypoxemia is typically associated with:
- Low PaO₂
- Increased alveolar-arterial oxygen gradient
- Little or no improvement with supplemental oxygen, especially in severe cases
Note: Recognizing this pattern helps guide treatment and suggests that more aggressive interventions may be needed, such as recruitment maneuvers, positive pressure ventilation, or treatment of the underlying alveolar collapse or flooding.
Alveolar-Arterial Oxygen Gradient
The alveolar-arterial oxygen gradient, often written as A-a gradient or DA-aO₂, is a useful tool for evaluating the cause of hypoxemia. It represents the difference between the oxygen tension in the alveoli and the oxygen tension measured in arterial blood.
This gradient helps determine whether hypoxemia is due to:
- A problem with oxygen entering the alveoli
- A problem with oxygen moving from the alveoli into the blood
Normal and Abnormal Patterns
A normal A-a gradient suggests that the lungs are transferring oxygen appropriately and that the problem may be due to:
- Low inspired oxygen
- Hypoventilation
An increased A-a gradient suggests impaired gas exchange and points toward causes such as:
- V/Q mismatch
- Diffusion impairment
- Right-to-left shunt
Note: This distinction is especially useful in clinical practice because hypoventilation and V/Q mismatch are both common, yet they require different interpretations and management strategies.
Effect of Aging
The normal A-a gradient increases with age. Therefore, what is considered normal in an older adult may be abnormal in a younger patient.
This reinforces the need to interpret arterial blood gas data within the broader clinical context rather than relying on a single fixed number.
Hemoglobin and Oxygen Content
PaO₂ measures the amount of oxygen dissolved in arterial plasma, but most oxygen in the blood is carried bound to hemoglobin. For this reason, arterial oxygen content depends heavily on both hemoglobin concentration and hemoglobin function.
A patient may have a normal PaO₂ and still have inadequate oxygen delivery if hemoglobin is deficient or abnormal.
Absolute Hemoglobin Deficiency
Absolute hemoglobin deficiency occurs when the hemoglobin concentration is lower than normal. This may result from:
- Hemorrhage
- Chronic blood loss
- Bone marrow suppression
- Nutritional deficiencies
- Chronic disease
Note: In these situations, arterial oxygen tension may remain normal, but total oxygen content falls because there is less hemoglobin available to carry oxygen.
Relative Hemoglobin Deficiency
Relative hemoglobin deficiency occurs when hemoglobin is present but cannot effectively bind or carry oxygen. Examples include:
- Carboxyhemoglobin from carbon monoxide poisoning
- Methemoglobinemia
- Other abnormal hemoglobin states
Note: These disorders reduce effective oxygen delivery even when the PaO₂ appears normal.
Clinical Relevance
This is why evaluation of oxygenation should not stop at the arterial blood gas alone. Hemoglobin concentration, oxygen saturation, and the patient’s overall perfusion status must also be considered.
A person with severe anemia may develop signs of tissue hypoxia despite having no true hypoxemia. Conversely, a patient with mild hypoxemia but adequate hemoglobin and cardiac output may tolerate the condition relatively well.
Reduced Blood Flow and Tissue Oxygenation
Oxygen delivery to the tissues depends on more than oxygenation in the lungs. It also depends on adequate circulation.
Even when CaO₂ is normal, tissue hypoxia can occur if blood flow is reduced. This can happen in two major ways:
- Generalized circulatory failure, such as shock
- Localized ischemia due to impaired perfusion to a specific tissue or organ
In shock, tissue oxygen deprivation becomes widespread. The body attempts to preserve perfusion to vital organs, but prolonged circulatory failure eventually leads to organ dysfunction and cell death.
In ischemia, blood flow is reduced to a particular area, such as the heart during myocardial infarction or the brain during stroke. Even with normal lung function and normal arterial oxygenation, the affected tissue becomes hypoxic.
Note: This concept highlights an important clinical principle: oxygen delivery depends on oxygen content and cardiac output working together.
Dysoxia and Impaired Oxygen Utilization
Dysoxia is a form of tissue hypoxia in which oxygen is present in the blood but cannot be adequately used by the cells. In this situation, the problem is not primarily low PaO₂ or poor blood flow, but impaired cellular oxygen utilization.
One of the classic examples is cyanide poisoning. Cyanide interferes with the cytochrome oxidase system inside the mitochondria, preventing cells from using oxygen for aerobic metabolism. Even when oxygen delivery appears adequate, tissues are forced into anaerobic metabolism.
Dysoxia can also occur in severe systemic illness, particularly when oxygen consumption becomes abnormally dependent on oxygen delivery. This has been described in conditions such as:
- Septic shock
- Major trauma
- Acute respiratory distress syndrome
Note: In these settings, cells may be unable to extract and use oxygen normally, contributing to lactate production and organ dysfunction.
Clinical Importance
Dysoxia reminds clinicians that oxygenation is only one part of the bigger picture. A patient may have acceptable arterial oxygen values and still experience serious cellular hypoxia if oxygen cannot be effectively utilized at the tissue level.
This is why evaluation of a critically ill patient often includes more than pulse oximetry and arterial blood gas results. Perfusion, hemodynamics, lactate levels, and evidence of organ dysfunction all help determine whether oxygen delivery and utilization are truly adequate.
Signs and Symptoms of Hypoxemia
The clinical presentation of hypoxemia can vary depending on the severity, duration, and speed of onset. Some patients with mild chronic hypoxemia may have few symptoms, while others with rapidly developing hypoxemia may deteriorate quickly.
Common signs and symptoms include:
- Shortness of breath
- Tachypnea
- Increased work of breathing
- Tachycardia
- Restlessness or anxiety
- Confusion
- Cyanosis in severe cases
- Use of accessory muscles
- Fatigue
- Reduced exercise tolerance
In acute hypoxemia, patients may appear distressed and develop mental status changes as oxygen delivery to the brain declines. Severe hypoxemia can lead to arrhythmias, loss of consciousness, and respiratory failure.
In chronic hypoxemia, symptoms may be more subtle. Patients may report exertional dyspnea, fatigue, or declining activity tolerance. Over time, chronic low oxygen levels can contribute to pulmonary hypertension, secondary polycythemia, and right-sided heart strain.
Note: Because symptoms are not always proportional to the severity of oxygen impairment, objective assessment is essential.
How Hypoxemia Is Diagnosed
Pulse Oximetry
Pulse oximetry provides a noninvasive estimate of arterial oxygen saturation. It is widely used for screening, monitoring, and trending oxygenation status.
Although very useful, pulse oximetry has limitations. It does not directly measure PaO₂, may be affected by poor perfusion or motion artifact, and can be misleading in cases such as carbon monoxide poisoning or methemoglobinemia.
Arterial Blood Gas Analysis
Arterial blood gas analysis remains one of the most important tools for evaluating hypoxemia. It provides direct measurement of:
- PaO₂
- PaCO₂
- pH
- Bicarbonate
- Oxygen saturation, depending on the analyzer
Note: ABG interpretation helps determine not only whether hypoxemia is present, but also whether hypercapnia, acid-base disorders, or abnormal gas exchange mechanisms are contributing.
Alveolar-Arterial Gradient
As discussed earlier, the A-a gradient helps narrow the mechanism of hypoxemia. A normal gradient suggests low inspired oxygen or hypoventilation, while an elevated gradient points toward diffusion impairment, V/Q mismatch, or shunt.
Additional Diagnostic Evaluation
The cause of hypoxemia often requires further testing, depending on the clinical situation. This may include:
- Chest radiograph
- Computed tomography
- Pulmonary function testing
- Echocardiography
- Hemoglobin measurement
- Co-oximetry
- Lactate levels
Note: A complete assessment focuses not only on oxygen levels but also on the underlying disease process and the patient’s ability to deliver oxygen to the tissues.
Common Conditions Associated With Hypoxemia
Hypoxemia can develop in a wide range of cardiopulmonary and systemic disorders. Common examples include:
Pulmonary Disorders
- Chronic obstructive pulmonary disease
- Asthma exacerbation
- Pneumonia
- Pulmonary edema
- Interstitial lung disease
- Atelectasis
- Acute respiratory distress syndrome
- Pulmonary embolism
- Pneumothorax in severe cases
Cardiac and Vascular Disorders
- Congenital heart disease with right-to-left shunt
- Heart failure with pulmonary congestion
- Shock states that impair oxygen delivery
Environmental and Neuromuscular Causes
- High altitude exposure
- Drug-induced respiratory depression
- Spinal cord injury
- Neuromuscular weakness
- Obesity hypoventilation syndrome
Note: Recognizing the likely mechanism in each of these conditions is important because treatment depends on the cause rather than the oxygen level alone.
Treatment of Hypoxemia
Supplemental Oxygen
Supplemental oxygen is often the first-line treatment for hypoxemia. Increasing the inspired oxygen concentration raises alveolar oxygen tension and, in many cases, improves PaO₂.
Oxygen may be delivered through:
- Nasal cannula
- Simple mask
- High-flow nasal cannula
- Nonrebreather mask
- Noninvasive ventilation
- Mechanical ventilation
Note: The method chosen depends on the severity of hypoxemia, the work of breathing, and the underlying condition.
Treating the Underlying Cause
Correcting hypoxemia requires more than administering oxygen. The underlying cause must also be addressed.
Examples include:
- Bronchodilators for bronchospasm
- Antibiotics for pneumonia
- Diuretics for cardiogenic pulmonary edema
- Anticoagulation for pulmonary embolism
- Positive pressure ventilation for alveolar collapse or severe respiratory failure
- Naloxone for opioid-induced hypoventilation
Note: If hypoxemia is caused by a significant shunt, supplemental oxygen alone may be insufficient. Recruitment of collapsed alveoli, positive end-expiratory pressure, or more advanced ventilatory support may be necessary.
Supporting Oxygen Delivery
In some patients, oxygenation is only part of the problem. Tissue oxygen delivery may also require:
- Correction of anemia
- Improvement of cardiac output
- Restoration of perfusion
- Treatment of shock
- Optimization of hemoglobin function
Note: This is especially important in critically ill patients, where hypoxemia, low cardiac output, anemia, and cellular dysfunction may all be present at the same time.
Why Understanding the Mechanism Matters
Not all hypoxemia is managed the same way. Two patients may have the same PaO₂ but require very different treatments depending on the mechanism involved.
For example:
- A patient with hypoventilation may improve rapidly with increased ventilation
- A patient with V/Q mismatch often responds well to supplemental oxygen
- A patient with severe shunt may require alveolar recruitment and positive pressure support
- A patient with normal PaO₂ but severe anemia may need treatment aimed at oxygen content rather than gas exchange
Note: This is why identifying the mechanism of hypoxemia is so important in clinical practice. It helps explain the ABG findings, guides therapy, and improves the ability to predict how the patient will respond to treatment.
Clinical Significance for Respiratory Care
For respiratory therapists and other clinicians, hypoxemia is not just a laboratory abnormality. It is a central problem that influences assessment, monitoring, and intervention across many care settings.
Understanding hypoxemia helps clinicians:
- Interpret arterial blood gases more accurately
- Recognize the difference between oxygenation and ventilation problems
- Distinguish between hypoxemia and tissue hypoxia
- Evaluate whether a patient is likely to respond to oxygen therapy
- Anticipate complications related to gas exchange failure
Whether caring for a patient with COPD, pulmonary edema, pneumonia, ARDS, or shock, the clinician must think beyond the number and understand the physiology behind it.
Note: A solid grasp of hypoxemia also improves decision-making during oxygen titration, ventilator management, and evaluation of worsening respiratory status.
Hypoxemia Practice Questions
1. What is hypoxemia?
Hypoxemia is a decrease in the partial pressure of oxygen in arterial blood (PaO₂) below the normal range for a patient’s age.
2. What is the normal PaO₂ range?
Normal PaO₂ is approximately 80–100 mmHg in healthy adults.
3. How is hypoxemia different from hypoxia?
Hypoxemia refers to low oxygen in arterial blood, whereas hypoxia refers to inadequate oxygen at the tissue level.
4. What are the five major causes of hypoxemia?
Low FiO₂, hypoventilation, diffusion limitation, shunt, and ventilation-perfusion (V/Q) mismatch.
5. What is the most common cause of hypoxemia?
Ventilation-perfusion (V/Q) mismatch.
6. What is V/Q mismatch?
It is an imbalance between ventilation (airflow) and perfusion (blood flow) in the lungs.
7. What is a shunt?
A shunt occurs when blood passes through the lungs without participating in gas exchange.
8. How does hypoventilation cause hypoxemia?
Hypoventilation leads to increased PaCO₂ and decreased PaO₂ due to inadequate ventilation.
9. What is diffusion limitation?
It is impaired movement of oxygen across the alveolar-capillary membrane.
10. What condition commonly causes diffusion limitation?
Diseases like pulmonary fibrosis.
11. What is low FiO₂?
A reduced fraction of inspired oxygen, such as at high altitude.
12. How is hypoxemia detected?
Through arterial blood gas (ABG) analysis and pulse oximetry.
13. What is a normal SpO₂?
Typically 95–100% in healthy individuals.
14. What SpO₂ indicates hypoxemia?
Generally less than 90%.
15. What symptoms are associated with hypoxemia?
Dyspnea, tachypnea, tachycardia, confusion, and cyanosis.
16. What is cyanosis?
A bluish discoloration of the skin due to low oxygen levels.
17. What is the A-a gradient?
The alveolar-arterial oxygen gradient used to assess oxygen transfer efficiency.
18. When is the A-a gradient increased?
In V/Q mismatch, shunt, and diffusion defects.
19. When is the A-a gradient normal?
In hypoventilation and low FiO₂.
20. How does oxygen therapy treat hypoxemia?
By increasing FiO₂ and improving oxygenation.
21. Which causes of hypoxemia respond well to oxygen therapy?
V/Q mismatch, diffusion limitation, and low FiO₂.
22. Which cause does NOT respond well to oxygen therapy?
Shunt
23. What is refractory hypoxemia?
Hypoxemia that does not improve with oxygen therapy.
24. What disease is commonly associated with refractory hypoxemia?
Acute Respiratory Distress Syndrome (ARDS)
25. What is the role of hemoglobin in hypoxemia?
Hemoglobin carries oxygen; low levels worsen oxygen delivery.
26. Can a patient have normal PaO₂ but still be hypoxic?
Yes, in cases like anemia or carbon monoxide poisoning.
27. What is the oxyhemoglobin dissociation curve?
It describes the relationship between PaO₂ and hemoglobin saturation.
28. What causes a right shift of the oxyhemoglobin curve?
Increased temperature, CO₂, acidity, and 2,3-DPG.
29. Why is a right shift beneficial?
It promotes oxygen release to tissues.
30. What is the primary goal in treating hypoxemia?
To improve oxygen delivery to tissues and prevent organ dysfunction.
31. What is the primary mechanism of hypoxemia in COPD?
Ventilation-perfusion (V/Q) mismatch due to uneven airflow and obstruction.
32. How does pneumonia cause hypoxemia?
By creating areas of shunt where alveoli are filled with fluid and not ventilated.
33. What happens to PaO₂ during hypoventilation?
PaO₂ decreases as PaCO₂ increases.
34. What is the relationship between PaCO₂ and PaO₂ in hypoventilation?
They are inversely related; as PaCO₂ rises, PaO₂ falls.
35. What is the significance of a PaO₂ less than 60 mmHg?
It indicates clinically significant hypoxemia.
36. What is oxygen content (CaO₂)?
The total amount of oxygen carried in the blood, including dissolved and hemoglobin-bound oxygen.
37. Why is oxygen content important in hypoxemia?
It determines how much oxygen is delivered to tissues.
38. What condition can reduce oxygen content despite normal PaO₂?
Anemia
39. What is the effect of carbon monoxide poisoning on hypoxemia?
It reduces oxygen-carrying capacity without lowering PaO₂.
40. What is a hallmark sign of severe hypoxemia?
Altered mental status or confusion.
41. What happens to heart rate during hypoxemia?
It increases (tachycardia) to compensate.
42. What is the effect of hypoxemia on respiratory rate?
It increases (tachypnea).
43. What is the role of chemoreceptors in hypoxemia?
They detect low oxygen levels and stimulate increased ventilation.
44. Where are peripheral chemoreceptors located?
In the carotid and aortic bodies.
45. At what PaO₂ do peripheral chemoreceptors strongly respond?
Below approximately 60 mmHg.
46. What is the effect of chronic hypoxemia on erythropoiesis?
It stimulates increased red blood cell production.
47. What condition results from long-term hypoxemia and increased RBC production?
Secondary polycythemia
48. How does hypoxemia affect pulmonary vasculature?
It causes vasoconstriction in poorly ventilated areas.
49. What is hypoxic pulmonary vasoconstriction?
A mechanism that diverts blood from poorly ventilated alveoli to better-ventilated areas.
50. What can prolonged hypoxic pulmonary vasoconstriction lead to?
Pulmonary hypertension
51. What is the effect of hypoxemia on the brain?
It can cause confusion, agitation, or loss of consciousness.
52. What is the effect of hypoxemia on the heart?
It can lead to arrhythmias and myocardial ischemia.
53. What is silent hypoxemia?
Low oxygen levels without obvious symptoms like dyspnea.
54. In which condition is silent hypoxemia commonly observed?
COVID-19
55. What is the first-line treatment for hypoxemia?
Supplemental oxygen therapy.
56. What device delivers low-flow oxygen?
Nasal cannula
57. What device can deliver precise oxygen concentrations?
Venturi mask
58. What is the goal SpO₂ for most patients receiving oxygen therapy?
Typically 92–96% (or 88–92% in COPD patients).
59. Why must oxygen therapy be used cautiously in COPD patients?
To avoid suppressing hypoxic drive and worsening CO₂ retention.
60. What is the ultimate consequence of untreated severe hypoxemia?
Organ failure and death.
61. What is the primary cause of hypoxemia at high altitude?
Reduced inspired oxygen pressure (low FiO₂).
62. How does barometric pressure affect hypoxemia?
Lower barometric pressure decreases the partial pressure of inspired oxygen.
63. What is the alveolar oxygen tension (PAO₂)?
The partial pressure of oxygen in the alveoli.
64. Why is PAO₂ important in hypoxemia?
It determines the driving force for oxygen diffusion into the blood.
65. What happens to PAO₂ in hypoventilation?
It decreases due to increased CO₂ levels.
66. What is the effect of airway obstruction on oxygenation?
It reduces ventilation, leading to V/Q mismatch and hypoxemia.
67. How does atelectasis cause hypoxemia?
Collapsed alveoli create shunt-like conditions.
68. What is the effect of pulmonary edema on oxygenation?
Fluid in alveoli impairs diffusion and causes shunting.
69. What is the difference between true shunt and shunt-like effect?
True shunt has no ventilation, while shunt-like has minimal ventilation.
70. What is the effect of exercise on hypoxemia in lung disease?
It can worsen hypoxemia due to increased oxygen demand and diffusion limitation.
71. What is the significance of mixed venous oxygen (PvO₂)?
It reflects the balance between oxygen delivery and consumption.
72. How does low cardiac output affect hypoxemia?
It reduces oxygen delivery to tissues despite normal oxygenation.
73. What is the oxygen delivery equation dependent on?
Cardiac output and oxygen content.
74. How does fever affect oxygen demand?
It increases metabolic rate and oxygen consumption.
75. What is the effect of hypoxemia on lactic acid levels?
It increases due to anaerobic metabolism.
76. What is a late sign of hypoxemia?
Cyanosis
77. Why is cyanosis considered a late sign?
It requires significant desaturation of hemoglobin to be visible.
78. How does skin pigmentation affect detection of cyanosis?
It can make cyanosis harder to detect visually.
79. What is the role of pulse oximetry in hypoxemia?
It provides noninvasive monitoring of oxygen saturation.
80. What are limitations of pulse oximetry?
It may be inaccurate in poor perfusion, motion, or carbon monoxide poisoning.
81. What is carboxyhemoglobin’s effect on SpO₂ readings?
It falsely elevates oxygen saturation readings.
82. What is methemoglobinemia’s effect on oxygenation?
It impairs oxygen delivery and can distort pulse oximetry readings.
83. What is the effect of hypoxemia on the kidneys?
It may reduce renal function due to decreased oxygen delivery.
84. What compensatory mechanism occurs in chronic hypoxemia?
Increased hemoglobin concentration.
85. What is clubbing, and how is it related to hypoxemia?
Enlargement of fingertips associated with chronic hypoxemia.
86. What lung disease is commonly associated with clubbing?
Interstitial lung disease.
87. What is the effect of hypoxemia on muscle function?
It causes fatigue and weakness.
88. How does hypoxemia affect exercise tolerance?
It decreases the ability to perform physical activity.
89. What is the primary treatment for altitude-related hypoxemia?
Supplemental oxygen or descent to a lower altitude.
90. What is the purpose of long-term oxygen therapy (LTOT)?
To improve survival and quality of life in chronic hypoxemia.
91. What is the primary cause of hypoxemia in a pulmonary embolism?
Ventilation-perfusion (V/Q) mismatch due to blocked blood flow.
92. How does asthma cause hypoxemia?
Airway narrowing leads to uneven ventilation and V/Q mismatch.
93. What is the effect of mucus plugging on oxygenation?
It causes airway obstruction, leading to shunt or V/Q mismatch.
94. What happens to oxygenation during sleep in patients with lung disease?
Hypoxemia may worsen due to decreased ventilation.
95. What is nocturnal hypoxemia?
A drop in oxygen levels during sleep.
96. What is the effect of body position on hypoxemia?
Position can affect V/Q matching; for example, the “good lung down” position improves oxygenation.
97. What is orthodeoxia?
A decrease in oxygen saturation when moving to an upright position.
98. What is platypnea?
Shortness of breath that worsens in the upright position and improves when lying down.
99. What is the effect of hypoxemia on cellular metabolism?
Cells shift from aerobic to anaerobic metabolism.
100. What is the ultimate goal of assessing hypoxemia in clinical practice?
To identify the underlying cause and guide appropriate treatment.
Final Thoughts
Hypoxemia is a reduction in arterial oxygen tension that can result from low inspired oxygen, hypoventilation, diffusion impairment, ventilation-perfusion mismatch, or right-to-left shunting.
Although it is often associated with tissue hypoxia, adequate oxygen delivery also depends on hemoglobin concentration, cardiac output, blood flow, and the ability of cells to use oxygen effectively. For this reason, evaluating hypoxemia requires more than identifying a low PaO₂.
A careful understanding of the underlying mechanism allows clinicians to interpret gas exchange abnormalities correctly, choose appropriate treatment, and better assess the overall impact on tissue oxygenation and patient stability.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Sarkar M, Niranjan N, Banyal PK. Mechanisms of hypoxemia. Lung India. 2017.
- Bhutta BS, Alghoula F, Berim I. Hypoxia. [Updated 2024 Mar 4]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026.

