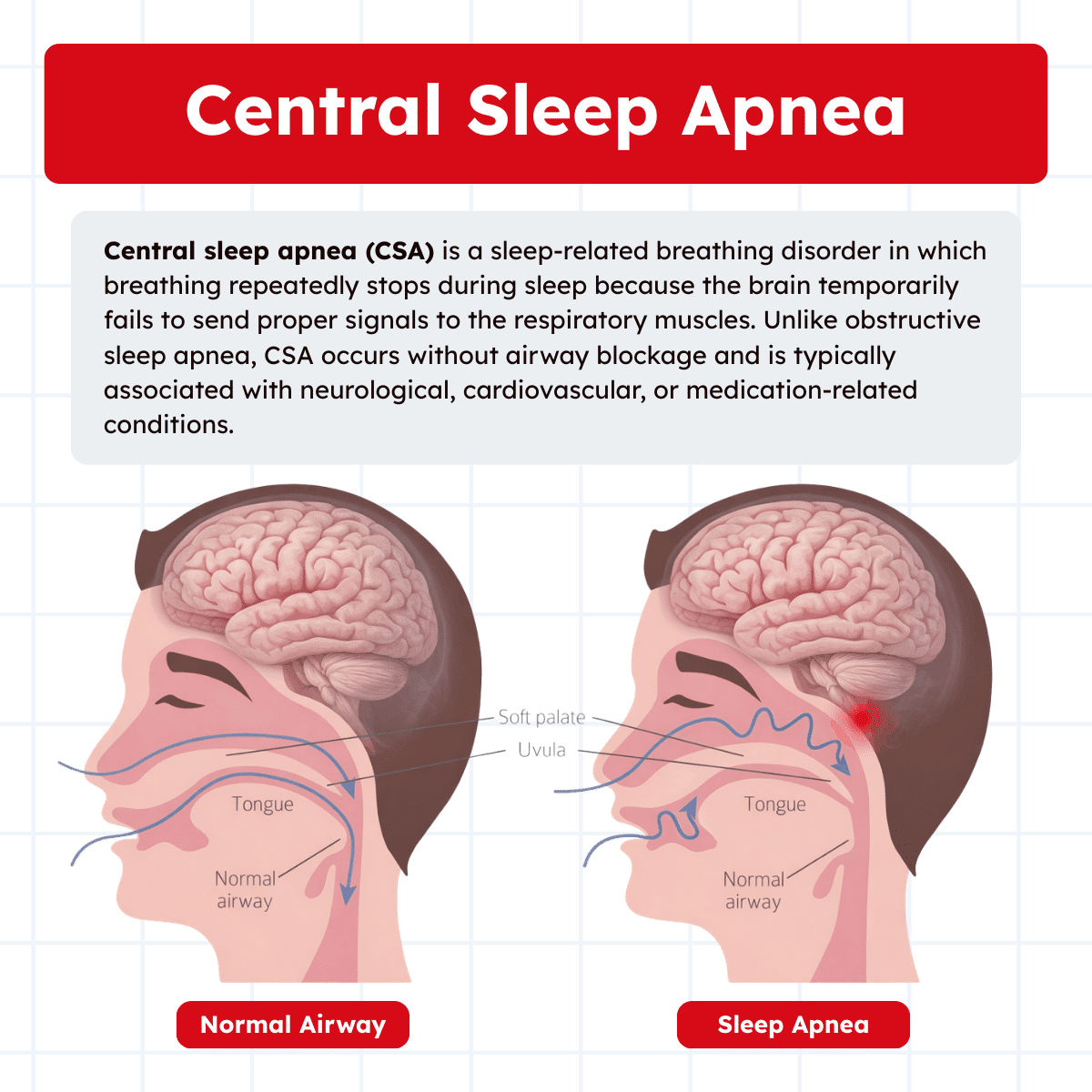
Central sleep apnea (CSA) is a sleep-related breathing disorder characterized by repeated pauses in breathing due to a lack of respiratory effort. Unlike obstructive sleep apnea, which results from airway collapse, CSA occurs when the brain temporarily fails to send appropriate signals to the respiratory muscles.
Although less common than obstructive sleep apnea, CSA is clinically significant because it is often associated with serious underlying conditions such as heart failure, stroke, and neuromuscular disease.
For respiratory therapists, understanding CSA is essential for accurate assessment, ventilatory support, and long-term patient management.
What Is Central Sleep Apnea?
Central sleep apnea is defined by recurrent episodes of complete cessation of airflow lasting at least 10 seconds during sleep, accompanied by an absence of respiratory effort. In other words, the patient stops breathing because the central nervous system fails to stimulate the respiratory muscles, not because of airway obstruction.
These breathing pauses may occur multiple times per hour and often lead to fluctuations in oxygen and carbon dioxide levels. As oxygen levels fall and carbon dioxide rises, the brain eventually triggers a brief arousal from sleep, restoring breathing. These repeated disruptions fragment sleep and prevent normal restorative sleep cycles, leading to fatigue and impaired daytime functioning.
CSA is considered a disorder of ventilatory control. It reflects instability in the body’s respiratory control centers located in the brainstem, which regulate breathing in response to changes in carbon dioxide and oxygen levels.
Pathophysiology of Central Sleep Apnea
The regulation of breathing during sleep depends heavily on carbon dioxide levels in the blood. Under normal circumstances, rising carbon dioxide levels stimulate the respiratory centers to increase ventilatory drive. In CSA, this control system becomes unstable.
One common mechanism involves an oversensitive response to carbon dioxide. If ventilation increases excessively, carbon dioxide levels may fall below the apneic threshold, temporarily suppressing respiratory drive. This results in a central apnea. As carbon dioxide accumulates again, breathing resumes, often in a cyclical pattern.
This waxing and waning of respiratory drive produces a breathing pattern known as periodic breathing. A classic example is Cheyne-Stokes respiration, characterized by a crescendo-decrescendo pattern of tidal volumes alternating with periods of apnea. This pattern is commonly observed in patients with congestive heart failure or following stroke.
Note: Unlike obstructive sleep apnea, CSA does not involve upper airway collapse. Instead, it reflects an imbalance in the neurological control of breathing.
Causes and Risk Factors
Central sleep apnea is frequently secondary to other medical conditions. Congestive heart failure is one of the most common associated conditions, particularly in patients who exhibit Cheyne-Stokes respiration. Reduced cardiac output and prolonged circulation time contribute to instability in ventilatory control.
Neurological disorders such as stroke, brainstem lesions, and neurodegenerative diseases can disrupt the respiratory centers directly. Neuromuscular disorders such as amyotrophic lateral sclerosis, muscular dystrophy, and Guillain-Barré syndrome may impair the ability of respiratory muscles to respond to neural signals.
Chronic opioid use is another important cause, as opioids depress central respiratory drive. High-altitude exposure can also induce central apneas due to altered oxygen and carbon dioxide regulation.
Note: In some cases, CSA occurs without an identifiable cause and is referred to as primary or idiopathic central sleep apnea.
Signs and Symptoms
The clinical presentation of CSA may overlap with other sleep disorders. Patients often report fragmented sleep, frequent nighttime awakenings, and excessive daytime fatigue. Bed partners may notice periods of breathing cessation without the loud snoring typically associated with obstructive sleep apnea.
Because CSA is often associated with underlying cardiovascular or neurological disease, patients may present with symptoms related to those conditions, such as dyspnea, orthopnea, or exercise intolerance in heart failure.
Note: Excessive daytime sleepiness may not be present in all patients with CSA. Some individuals may have significant disease severity with relatively mild subjective symptoms.
Diagnosis of Central Sleep Apnea
Diagnosis of CSA requires objective sleep testing. Polysomnography is the gold standard diagnostic method. During a sleep study, central apneas are identified by the absence of airflow accompanied by the absence of respiratory effort, as measured by chest and abdominal movement sensors.
The apnea-hypopnea index (AHI) is used to quantify severity. Sleep apnea is diagnosed when there are more than five abnormal events per hour of sleep. Mild, moderate, and severe classifications are based on increasing AHI thresholds.
Distinguishing central from obstructive events is critical, as treatment strategies differ significantly. In central apneas, there is no inspiratory effort, whereas obstructive events demonstrate continued effort despite airflow cessation.
Note: In some settings, overnight oximetry may provide supportive information by identifying recurrent oxygen desaturation events, but it cannot reliably differentiate central from obstructive apnea.
Treatment and Management
The management of central sleep apnea focuses on addressing the underlying cause whenever possible. For patients with heart failure, optimizing cardiac function through medical therapy can reduce central apneas and improve breathing stability.
Positive airway pressure therapy plays a central role in management. Continuous positive airway pressure (CPAP) may reduce central events in some patients, particularly those with heart failure. Bi-level positive airway pressure (BiPAP) may be indicated for patients with hypercapnic CSA or hypoventilation syndromes.
Adaptive servo-ventilation (ASV) is specifically designed to treat central sleep apnea and periodic breathing. This advanced modality adjusts pressure support dynamically to stabilize ventilation and maintain consistent breathing patterns. However, ASV must be prescribed carefully, particularly in certain heart failure populations.
Supplemental oxygen may be beneficial in selected patients, particularly those with heart failure–related CSA. Certain medications, such as acetazolamide, may help by stimulating ventilation and lowering the carbon dioxide apneic threshold.
Note: Because CSA often reflects systemic disease, multidisciplinary management is frequently required.
Relevance to Respiratory Therapists and Respiratory Care
Central sleep apnea is highly relevant to respiratory therapists because it directly involves ventilatory control and gas exchange. Respiratory therapists are often responsible for monitoring respiratory effort during sleep studies and assisting in the differentiation between central and obstructive events.
In the sleep laboratory, respiratory therapists help interpret airflow, respiratory effort, and oxygen saturation data. Accurate identification of central apneas is critical in determining appropriate therapy.
Respiratory therapists also play a key role in initiating and titrating positive airway pressure therapy. This includes adjusting settings on CPAP, BiPAP, or ASV devices and ensuring optimal patient comfort and safety.
Education and adherence support are equally important. Patients with CSA may require detailed explanation of their condition and the importance of treating underlying disorders. Respiratory therapists help patients understand equipment use, troubleshoot issues, and improve compliance.
In hospital settings, respiratory therapists may encounter CSA in patients with heart failure, stroke, or chronic opioid use. Recognizing sleep-disordered breathing patterns can improve overall patient management and reduce complications.
Furthermore, respiratory therapists are integral to managing patients with neuromuscular disease and chronic hypoventilation syndromes. Early detection and noninvasive ventilation support can improve quality of life, stabilize gas exchange, and prolong survival.
Complications of Untreated Central Sleep Apnea
Untreated CSA can lead to significant health consequences. Recurrent oxygen desaturation and sleep fragmentation may worsen cardiovascular disease and impair cognitive function. In patients with heart failure, CSA is associated with increased morbidity and mortality.
Chronic sleep disruption contributes to decreased quality of life, mood disturbances, and impaired daytime functioning. Because CSA often signals underlying systemic disease, failure to recognize and treat it may delay appropriate management of serious conditions.
Central Sleep Apnea Practice Questions
1. What is central sleep apnea (CSA)?
Central sleep apnea is a sleep disorder characterized by repeated episodes of absent airflow due to a lack of respiratory effort caused by impaired signaling from the brain’s respiratory centers.
2. How does central sleep apnea differ from obstructive sleep apnea?
Central sleep apnea occurs when the brain fails to send signals to breathe, whereas obstructive sleep apnea results from physical airway obstruction despite respiratory effort.
3. What is the primary cause of central sleep apnea?
The primary cause of central sleep apnea is dysfunction of the central nervous system respiratory control centers located in the brainstem.
4. What is periodic breathing in central sleep apnea?
Periodic breathing is a cyclic pattern of increasing and decreasing respiratory effort and airflow that often alternates with apnea episodes.
5. What is Cheyne-Stokes respiration?
Cheyne-Stokes respiration is a form of periodic breathing characterized by gradual increases and decreases in tidal volume followed by apnea.
6. Which medical condition is most commonly associated with Cheyne-Stokes respiration?
Congestive heart failure is the most commonly associated condition with Cheyne-Stokes respiration.
7. How does stroke contribute to central sleep apnea?
Stroke can damage respiratory control centers in the brain, impairing the regulation of breathing during sleep.
8. What role does the brainstem play in respiration?
The brainstem regulates automatic breathing by controlling respiratory rhythm and ventilatory drive.
9. What is the prevalence of central sleep apnea compared to obstructive sleep apnea?
Central sleep apnea is less common and accounts for approximately 10% to 15% of sleep-disordered breathing cases.
10. What happens to ventilatory effort during central sleep apnea events?
Ventilatory effort decreases or completely stops during central sleep apnea episodes.
11. How does chronic opioid use contribute to central sleep apnea?
Opioids depress the respiratory centers in the brain, reducing the drive to breathe during sleep.
12. What neuromuscular disorders are associated with central sleep apnea?
Conditions such as amyotrophic lateral sclerosis (ALS), muscular dystrophy, and Guillain-Barré syndrome can impair respiratory control and contribute to CSA.
13. How does high altitude contribute to central sleep apnea?
Low oxygen levels at high altitude stimulate unstable respiratory control, leading to periodic breathing and central apnea episodes.
14. What is congenital central hypoventilation syndrome?
It is a rare genetic disorder in which patients lack automatic respiratory drive, especially during sleep.
15. What is mixed sleep apnea?
Mixed sleep apnea involves a combination of central apnea followed by obstructive apnea during the same respiratory event.
16. What diagnostic test is considered the gold standard for diagnosing central sleep apnea?
Polysomnography is the gold standard diagnostic test for central sleep apnea.
17. What physiologic parameters are monitored during polysomnography?
Polysomnography monitors airflow, respiratory effort, oxygen saturation, sleep stages, heart rhythm, and muscle activity.
18. How does carbon dioxide influence respiratory drive?
Elevated carbon dioxide levels stimulate breathing, while low levels can suppress respiratory drive.
19. Why is hypocapnia associated with central sleep apnea?
Low carbon dioxide levels reduce ventilatory drive and may trigger apnea episodes.
20. What cardiovascular complications are associated with untreated central sleep apnea?
Untreated CSA can contribute to arrhythmias, heart failure, hypertension, and increased mortality.
21. How does CSA affect oxygen saturation during sleep?
CSA causes intermittent hypoxemia due to repeated pauses in ventilation.
22. What symptoms are commonly reported by patients with central sleep apnea?
Common symptoms include excessive daytime sleepiness, frequent awakenings, and poor sleep quality.
23. Why may patients with central sleep apnea experience morning headaches?
Morning headaches can result from nighttime hypoxemia and carbon dioxide retention.
24. What is adaptive servo-ventilation (ASV)?
ASV is a specialized positive airway pressure therapy that adjusts ventilation support to stabilize breathing patterns in CSA.
25. When is bilevel positive airway pressure (BiPAP) used in central sleep apnea?
BiPAP may be used when patients require ventilatory support to maintain adequate breathing during sleep.
26. Why is supplemental oxygen sometimes used in CSA treatment?
Supplemental oxygen helps prevent hypoxemia and may stabilize respiratory control in some patients.
27. How does CSA impact sleep architecture?
CSA disrupts normal sleep stages by causing repeated arousals and fragmented sleep patterns.
28. Why is respiratory therapist involvement important in CSA management?
Respiratory therapists assist with sleep study interpretation, PAP therapy management, and patient education.
29. What role does heart failure treatment play in managing CSA?
Optimizing heart failure treatment can reduce CSA severity by improving cardiac output and respiratory stability.
30. How does CSA affect sympathetic nervous system activity?
CSA increases sympathetic activity, which may contribute to hypertension and cardiovascular strain.
31. Why is patient adherence important in PAP therapy for CSA?
Consistent PAP therapy improves symptom control, sleep quality, and long-term outcomes.
32. What clinical findings may suggest central sleep apnea rather than obstructive sleep apnea?
CSA is suggested by absent respiratory effort during apnea events and a lack of upper airway obstruction signs.
33. How can CSA contribute to cognitive impairment?
Repeated sleep disruption and hypoxemia may impair memory, attention, and executive function.
34. Why is early diagnosis of central sleep apnea important?
Early diagnosis allows for targeted therapy that reduces complications and improves quality of life.
35. What is the long-term prognosis for patients with untreated central sleep apnea?
Untreated CSA is associated with increased cardiovascular morbidity, decreased sleep quality, and higher mortality risk.
36. What physiologic mechanism causes ventilatory instability in central sleep apnea?
Ventilatory instability in central sleep apnea is caused by fluctuating carbon dioxide levels that disrupt normal respiratory drive and lead to cycles of hyperventilation followed by apnea.
37. How does delayed circulation time contribute to central sleep apnea in heart failure patients?
Delayed circulation time causes a lag between blood gas changes and respiratory center response, leading to unstable breathing patterns.
38. What is treatment-emergent central sleep apnea?
Treatment-emergent central sleep apnea occurs when central apnea develops after initiating therapy for obstructive sleep apnea, often during CPAP treatment.
39. Why can hyperventilation trigger central apnea episodes?
Hyperventilation lowers carbon dioxide levels below the threshold needed to stimulate breathing, leading to temporary cessation of respiratory effort.
40. How does sleep stage influence central sleep apnea severity?
Central sleep apnea events often worsen during lighter sleep stages and may decrease during deeper stages of sleep.
41. What is the apnea-hypopnea index (AHI)?
The apnea-hypopnea index measures the number of apnea and hypopnea events per hour of sleep to determine the severity of sleep apnea.
42. How is central sleep apnea severity classified using the AHI?
CSA severity is classified as mild, moderate, or severe based on the number of apnea and hypopnea events recorded during sleep.
43. What respiratory pattern is commonly observed in patients with central sleep apnea?
Patients with CSA commonly demonstrate cyclic waxing and waning ventilation patterns.
44. Why are patients with central sleep apnea at increased risk for arrhythmias?
Repeated oxygen desaturation and sympathetic nervous system activation increase the likelihood of abnormal cardiac rhythms.
45. What role does chemoreceptor sensitivity play in central sleep apnea?
Increased or unstable chemoreceptor sensitivity can lead to exaggerated respiratory responses and periodic breathing.
46. How can neurological injury contribute to central sleep apnea?
Neurological injury can impair communication between the brainstem and respiratory muscles, reducing automatic breathing control.
47. What symptom may differentiate central sleep apnea from obstructive sleep apnea during sleep studies?
The absence of thoracic and abdominal respiratory effort during apnea events suggests central sleep apnea.
48. How does CSA affect sleep efficiency?
CSA reduces sleep efficiency by causing frequent arousals and fragmented sleep cycles.
49. Why may patients with CSA experience nocturnal awakenings?
Apnea episodes and changes in oxygen levels often trigger arousals that disrupt continuous sleep.
50. What is the role of arterial blood gas analysis in central sleep apnea evaluation?
Arterial blood gas analysis helps assess oxygenation and ventilation abnormalities that may contribute to CSA.
51. How does CSA impact daytime functioning?
CSA can cause fatigue, impaired concentration, and decreased cognitive performance due to poor sleep quality.
52. Why are patients with CSA at risk for developing systemic hypertension?
Recurrent hypoxemia and sympathetic activation increase vascular resistance and blood pressure.
53. What lifestyle modification may improve symptoms of central sleep apnea?
Weight management, reducing sedative use, and optimizing cardiovascular health may help improve CSA symptoms.
54. How does alcohol consumption affect central sleep apnea?
Alcohol depresses respiratory drive and can worsen apnea episodes during sleep.
55. Why is monitoring oxygen saturation important in CSA patients?
Monitoring oxygen saturation helps detect hypoxemia and guides treatment decisions.
56. What is the significance of ventilatory control instability in CSA?
Ventilatory control instability leads to fluctuating respiratory drive and recurrent apnea episodes.
57. How does CSA affect carbon dioxide regulation during sleep?
CSA causes fluctuations in carbon dioxide levels due to alternating hyperventilation and apnea cycles.
58. Why are central apnea events often longer than obstructive apnea events?
Central apnea events may persist longer because respiratory effort is absent until respiratory drive resumes.
59. How can CSA influence exercise tolerance?
CSA may reduce exercise tolerance due to chronic fatigue and impaired oxygen delivery.
60. What is the impact of CSA on pulmonary hypertension risk?
Chronic hypoxemia associated with CSA may increase the risk of developing pulmonary hypertension.
61. Why is patient education important in managing central sleep apnea?
Patient education improves therapy adherence and helps patients recognize worsening symptoms.
62. How can respiratory therapists evaluate ventilatory effort during sleep studies?
Respiratory therapists analyze thoracic and abdominal movement signals to determine the presence or absence of breathing effort.
63. Why may central sleep apnea worsen during opioid therapy?
Opioids suppress respiratory center activity, reducing automatic breathing drive.
64. What is loop gain and how does it relate to central sleep apnea?
Loop gain refers to the sensitivity of the respiratory control system, and high loop gain increases ventilatory instability associated with CSA.
65. How can CSA affect mood and emotional health?
Chronic sleep disruption from CSA may contribute to depression, irritability, and anxiety.
66. Why is cardiac monitoring important in patients with central sleep apnea?
Cardiac monitoring helps detect arrhythmias and other cardiovascular complications associated with CSA.
67. What role does sleep position play in central sleep apnea?
Although less position-dependent than OSA, certain sleeping positions may influence respiratory control stability.
68. How does aging influence the risk of central sleep apnea?
Aging may reduce respiratory control stability and increase the likelihood of CSA.
69. Why is early intervention important for patients diagnosed with central sleep apnea?
Early intervention helps reduce complications, improve sleep quality, and decrease cardiovascular risks.
70. How does CSA contribute to increased mortality risk?
CSA is associated with cardiovascular complications, arrhythmias, and chronic hypoxemia, all of which increase mortality risk.
71. How does central sleep apnea affect autonomic nervous system activity?
Central sleep apnea increases sympathetic nervous system activity, which can elevate heart rate and blood pressure.
72. Why can central sleep apnea contribute to poor sleep architecture?
Frequent apnea events disrupt normal sleep stages, reducing restorative deep and REM sleep.
73. How does high altitude contribute to central sleep apnea?
High altitude lowers oxygen levels, which can destabilize respiratory drive and trigger periodic breathing patterns.
74. What is high-altitude periodic breathing?
High-altitude periodic breathing is a form of central sleep apnea characterized by cycles of hyperventilation followed by apnea due to reduced oxygen levels.
75. Why is central sleep apnea more common in patients with neurological disorders?
Neurological disorders may impair respiratory center function or disrupt neural pathways controlling breathing.
76. How does central sleep apnea influence oxygen delivery to tissues?
CSA reduces oxygen delivery due to repeated episodes of apnea and intermittent hypoxemia.
77. Why is adaptive servo-ventilation (ASV) used in central sleep apnea management?
ASV helps stabilize breathing by adjusting airway pressure to support ventilation during central apnea events.
78. What caution should be taken when using ASV in heart failure patients?
ASV may increase mortality risk in certain heart failure patients with reduced ejection fraction and must be used carefully.
79. How does chronic hypoxemia from CSA affect organ function?
Chronic hypoxemia can impair cardiac, neurological, and metabolic function over time.
80. What diagnostic tool measures ventilatory effort during sleep studies?
Respiratory inductance plethysmography measures chest and abdominal movement to assess ventilatory effort.
81. How can CSA contribute to insomnia symptoms?
Frequent sleep disruptions caused by apnea events may result in difficulty maintaining sleep.
82. Why are patients with CSA at risk for daytime hypersomnolence?
Interrupted sleep cycles reduce sleep quality, leading to excessive daytime sleepiness.
83. How does CSA influence carbon dioxide sensitivity during sleep?
CSA may alter carbon dioxide sensitivity, causing exaggerated breathing responses and ventilatory instability.
84. What is the relationship between CSA and chronic opioid use?
Chronic opioid use suppresses respiratory centers, increasing the risk of central apnea events.
85. Why is overnight pulse oximetry useful in screening for CSA?
Overnight pulse oximetry detects oxygen desaturation patterns suggestive of sleep-disordered breathing.
86. How does CSA impact cardiovascular workload?
Recurrent hypoxemia and sympathetic activation increase cardiac workload and stress.
87. Why may patients with CSA experience morning headaches?
Morning headaches may result from nocturnal hypoventilation and carbon dioxide retention.
88. How can CSA contribute to impaired memory and cognition?
Chronic sleep fragmentation and hypoxemia may negatively affect brain function and memory processing.
89. Why is polysomnography considered the gold standard for diagnosing CSA?
Polysomnography provides comprehensive monitoring of airflow, respiratory effort, oxygen levels, and sleep stages.
90. How does CSA affect ventilatory drive during REM sleep?
Respiratory drive is reduced during REM sleep, which may increase central apnea episodes.
91. Why is follow-up monitoring important after CSA treatment initiation?
Follow-up monitoring ensures therapy effectiveness and helps adjust treatment settings.
92. How does CSA influence exercise recovery?
Reduced sleep quality and oxygenation impair recovery and physical performance.
93. Why can CSA increase the risk of stroke?
Chronic hypoxemia and blood pressure fluctuations increase cerebrovascular risk.
94. How does CSA affect pulmonary gas exchange?
CSA disrupts normal ventilation patterns, leading to intermittent gas exchange abnormalities.
95. Why is patient adherence important in CSA therapy?
Consistent therapy use improves symptom control and reduces long-term complications.
96. How does CSA affect ventilatory response to hypoxia?
CSA may blunt or destabilize the body’s normal response to low oxygen levels.
97. Why can CSA contribute to metabolic dysfunction?
Repeated hypoxemia and sympathetic activation may impair glucose metabolism and increase insulin resistance.
98. How does CSA affect respiratory muscle activity during apnea events?
Respiratory muscle activity decreases or stops due to loss of central respiratory drive.
99. Why is identifying underlying causes important in CSA management?
Treating underlying neurological or cardiovascular conditions can improve CSA outcomes.
100. How can CSA influence long-term quality of life?
Untreated CSA can cause chronic fatigue, cardiovascular complications, and reduced daily functioning.
Final Thoughts
Central sleep apnea is a complex disorder of ventilatory control that differs fundamentally from obstructive sleep apnea. Although less common, it is often associated with significant underlying medical conditions and carries important clinical implications.
Respiratory therapists play a vital role in identifying central events during sleep studies, initiating appropriate ventilatory support, and educating patients about therapy adherence.
By understanding the mechanisms and management of CSA, respiratory care professionals can improve patient outcomes and help reduce complications associated with sleep-disordered breathing. Early recognition and comprehensive management remain essential in optimizing long-term respiratory and cardiovascular health.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Rana AM, Sankari A. Central Sleep Apnea. [Updated 2023 Jun 11]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025.