A chest radiograph, commonly referred to as a chest x-ray, is one of the most frequently performed imaging studies in medicine. It provides a rapid, noninvasive way to visualize the structures within the thoracic cavity, including the lungs, heart, pleura, and surrounding bones.
For respiratory therapists, the chest radiograph is far more than a routine diagnostic test. It is a critical clinical tool that guides airway management, ventilator adjustments, and the assessment of acute and chronic pulmonary conditions.
What Is a Chest Radiograph?
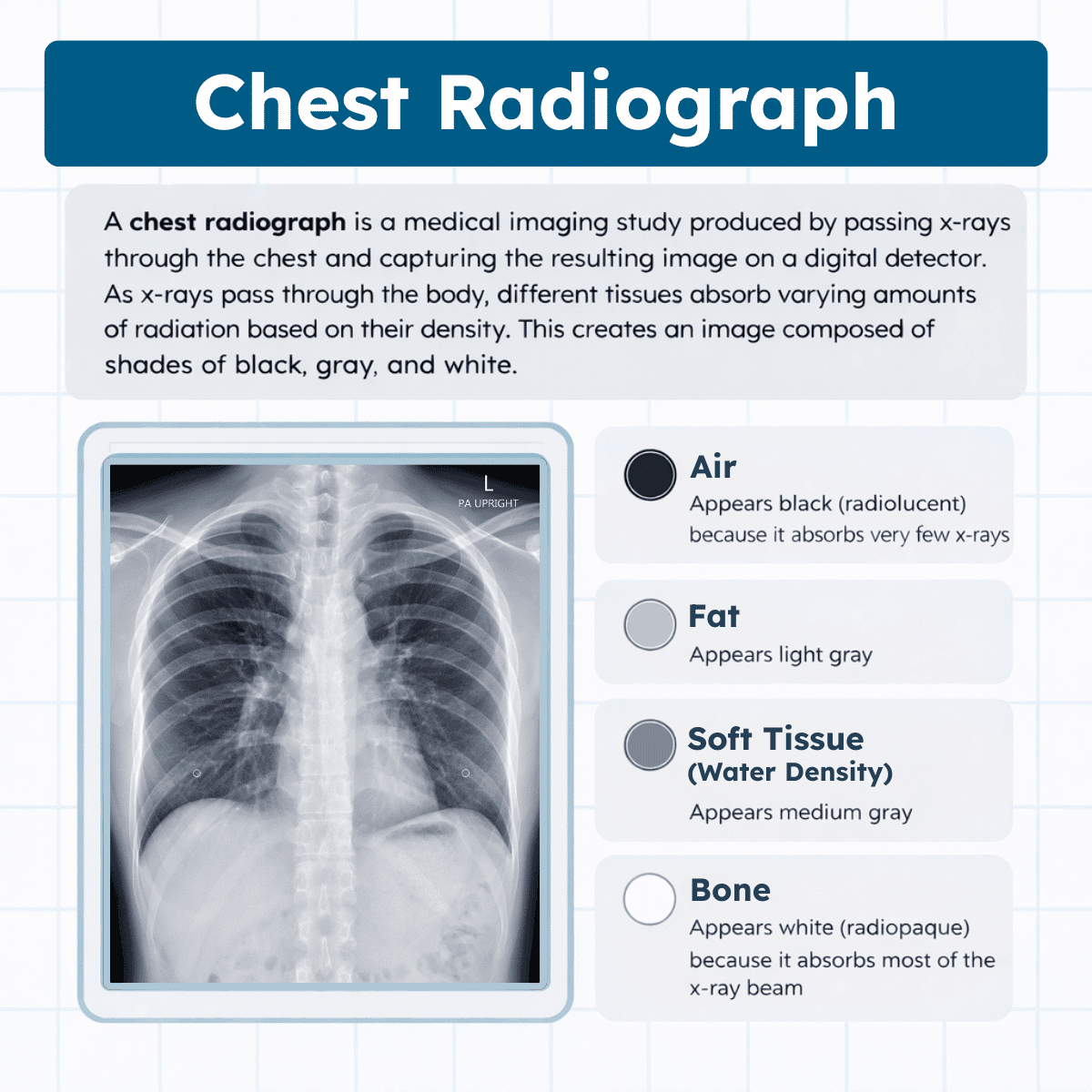
A chest radiograph is a medical imaging study produced by passing x-rays through the chest and capturing the resulting image on a digital detector. As x-rays pass through the body, different tissues absorb varying amounts of radiation based on their density. This creates an image composed of shades of black, gray, and white.
Four primary tissue densities are visible on a normal chest radiograph:
- Air – Appears black (radiolucent) because it absorbs very few x-rays
- Fat – Appears light gray
- Soft tissue (water density) – Appears medium gray
- Bone or metal – Appears white (radiopaque) because it absorbs most of the x-ray beam
The contrast between adjacent tissue densities allows clinicians to identify anatomical borders and detect abnormalities. For example, the heart is visible because it is a soft tissue density surrounded by air-filled lungs. When adjacent structures share the same density, their borders disappear, producing what is known as the silhouette sign, which can help localize disease within the chest.
Today, most chest radiographs are acquired and stored digitally using a picture archiving and communication system (PACS). Digital imaging allows clinicians to adjust brightness, contrast, and magnification to better evaluate subtle findings and compare serial studies over time.
Types of Chest Radiographs
Chest radiographs are typically performed in one of two main projections:
Posteroanterior (PA) View
In a PA film, the x-ray beam passes from back to front while the patient stands upright. This is the preferred method because it provides the most accurate representation of heart size and lung structures.
Anteroposterior (AP) View
AP films are commonly performed using portable machines, especially in intensive care units (ICUs). The x-ray beam passes from front to back while the patient is usually lying down. Because the heart lies anteriorly in the chest, it may appear artificially enlarged on an AP film due to magnification.
Note: Understanding the difference between PA and AP views is essential for respiratory therapists when interpreting cardiac size, lung volumes, and mediastinal contours.
Why Chest Radiographs Are Relevant to Respiratory Therapists
Respiratory therapists work at the bedside, often managing critically ill patients. The chest radiograph plays a central role in guiding clinical decision-making in several key areas:
1. Airway Management
After intubation, an AP chest radiograph is commonly used to confirm proper placement of an endotracheal (ET) tube. Ideally, the tube tip should be positioned approximately 4–6 cm above the carina. Misplacement into a mainstem bronchus or positioning too high in the trachea can lead to serious complications.
Note: Respiratory therapists must be able to quickly assess tube placement, especially in emergency situations.
2. Mechanical Ventilation Monitoring
Changes in plateau pressure, oxygenation, or lung compliance often prompt a chest radiograph. It can reveal:
- Atelectasis
- Pneumothorax
- Pulmonary edema
- Pleural effusion
- Consolidation
Note: In patients receiving mechanical ventilation, recognizing these findings allows the RT to adjust ventilator settings appropriately.
3. Evaluation of Acute Respiratory Distress
Sudden dyspnea or chest pain in the ICU frequently warrants immediate imaging. A chest radiograph can detect life-threatening conditions such as:
- Tension pneumothorax
- Large pleural effusion
- Endotracheal tube displacement
- Pulmonary infiltrates
Note: Rapid interpretation directly impacts patient outcomes.
4. Assessment of Chronic Lung Disease
Although some chronic conditions like emphysema may not always show dramatic findings, chest radiographs can reveal hyperinflation, flattened diaphragms, or increased radiolucency that supports clinical suspicion.
Indications for Obtaining a Chest Radiograph
Chest radiographs are ordered in both outpatient and inpatient settings. Common indications include:
Outpatient Indications
- Unexplained dyspnea
- Persistent severe cough
- Hemoptysis
- Fever with sputum production
- Acute chest pain
- Positive tuberculosis screening
Inpatient Indications
- Placement of endotracheal or tracheostomy tube
- Placement of central venous or pulmonary artery catheter
- Sudden decline in oxygenation
- Elevated or changing plateau pressures
- Acute onset dyspnea or chest pain
Note: Because respiratory therapists are closely involved in patient monitoring, they often recognize when imaging is necessary and may recommend it to the physician.
A Systematic Approach to Reading a Chest Radiograph
A disciplined, step-by-step method is essential to avoid missing subtle but clinically significant findings.
Step 1: Verify Patient Information
Confirm patient identity, date, and orientation markers to ensure the correct film is being reviewed.
Step 2: Assess Technical Quality
Evaluate for:
- Proper positioning (no rotation)
- Adequate penetration
- Full inclusion of the chest
Underpenetrated films may falsely suggest pathology, while overpenetrated films may obscure important findings.
A helpful mnemonic for image quality is R-I-P-E:
- Rotation
- Inspiration
- Projection
- Exposure
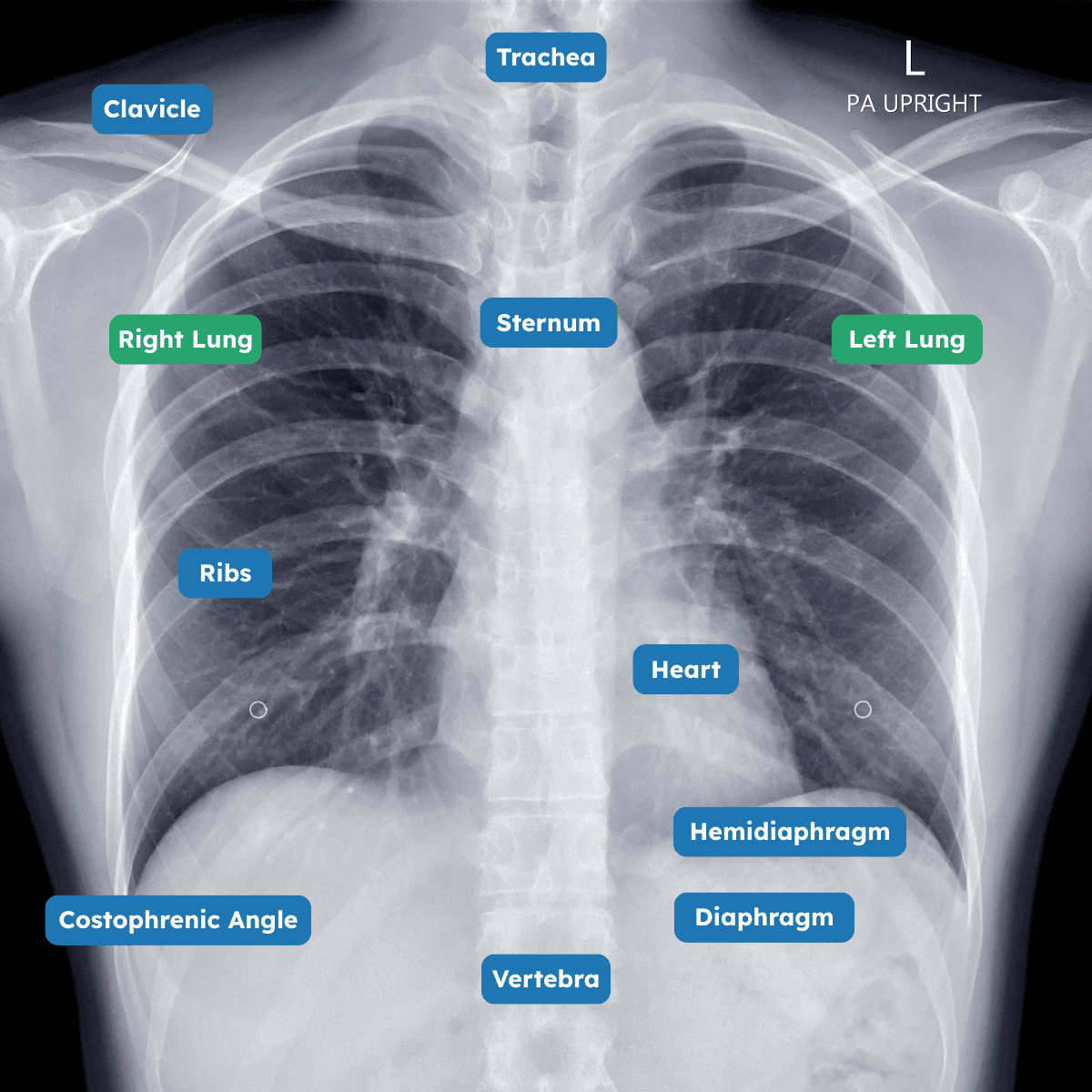
Step 3: Review Anatomical Structures Systematically
A thorough review includes:
- Bones (ribs, clavicles, spine)
- Soft tissues
- Lung fields
- Pleura
- Mediastinum and heart
- Diaphragms
- Upper abdomen
Note: Many clinicians intentionally review the lungs last to ensure other areas are not overlooked.
Common Radiographic Findings in Respiratory Care
Increased Radiopacity (Whiteness)
Conditions that increase tissue density include:
- Atelectasis
- Consolidation
- Pulmonary edema
- Pleural effusion
- Interstitial lung disease
- Tumors
Note: These appear as areas of increased whiteness on the radiograph.
Increased Radiolucency (Darkness)
Conditions associated with increased air or reduced tissue density include:
- Emphysema
- Pneumothorax
- Pneumomediastinum
- Subcutaneous emphysema
Note: These appear darker than surrounding tissues.
Evaluating Heart Size and Mediastinum
The cardiothoracic (CT) ratio is an important measurement on a PA chest radiograph. Normally, the cardiac width should not exceed 50% of the thoracic width. A ratio greater than 50% suggests cardiomegaly.
However, RTs must remember:
- AP films can exaggerate heart size
- Incomplete inspiration can falsely enlarge the heart shadow
- Rotation can distort mediastinal appearance
Note: The mediastinum and trachea may shift toward areas of lung volume loss (e.g., atelectasis) or away from space-occupying lesions (e.g., pneumothorax, large effusion).
Limitations of the Chest Radiograph
Despite its value, the chest radiograph has limitations:
- It provides only a two-dimensional image
- Small nodules may be missed
- Early pneumonia may not appear for 12–24 hours
- Findings may lag behind clinical symptoms
- Some conditions, such as pulmonary embolism, may appear normal
Note: In cases where more detailed imaging is required, computed tomography (CT), ultrasound, magnetic resonance imaging (MRI), or nuclear medicine studies may be indicated.
Special Considerations in Critical Care
Portable AP films are common in the ICU but are often of lower quality than PA films. Patient positioning, limited inspiration, and technical constraints can affect interpretation.
Respiratory therapists must also recognize and evaluate:
- Artificial airways
- Central venous catheters
- Pulmonary artery catheters
- Chest tubes
- Pacemakers
Note: Incorrect device placement can lead to serious complications and must be promptly addressed.
The Role of Serial Imaging
Digital imaging allows side-by-side comparison of chest radiographs over time. This is particularly valuable in monitoring:
- Resolution of pneumonia
- Progression of pulmonary edema
- Changes in lung volumes
- Response to ventilator adjustments
Serial comparison provides critical insight into whether a patient is improving, worsening, or remaining stable. By tracking radiographic changes alongside clinical findings, respiratory therapists can better evaluate treatment effectiveness and guide timely adjustments in care.
This ongoing assessment enhances patient safety and supports more informed, data-driven decision-making in both acute and critical care settings.
Chest Radiograph Practice Questions
1. What is a chest radiograph?
A chest radiograph is a medical imaging study created by passing x-rays through the chest and capturing the resulting image on a digital detector.
2. Why is chest imaging important in pulmonary and critical care medicine?
Chest imaging helps evaluate lung, pleural, and mediastinal structures and guides diagnosis and management of cardiopulmonary conditions.
3. Why must respiratory therapists understand chest radiograph interpretation?
Respiratory therapists use chest radiographs to assess patient status, recognize complications, and make informed clinical recommendations.
4. What are other imaging modalities used to evaluate the chest?
Other modalities include computed tomography (CT), ultrasound, magnetic resonance imaging (MRI), and nuclear medicine studies.
5. What is the normal position of the trachea on a chest radiograph?
The trachea should appear midline, overlying the vertebral column on a properly positioned AP or PA film.
6. How is a chest x-ray image formed?
The image is formed when x-rays pass through the chest and strike a detector, creating varying shades based on tissue density.
7. Why do air-filled lungs appear dark on a chest radiograph?
Air absorbs very few x-rays, allowing more radiation to reach the detector, which results in a darker (radiolucent) appearance.
8. Why do bones appear white on a chest radiograph?
Bone absorbs a large portion of the x-ray beam, preventing it from reaching the detector, resulting in a white (radiopaque) appearance.
9. What are the four basic tissue densities visible on a normal chest x-ray?
The four densities are air, fat, soft tissue (water density), and bone.
10. How does fat appear on a chest radiograph?
Fat absorbs a small amount of x-rays and appears as a light gray shade.
11. How does soft tissue appear on a chest radiograph?
Soft tissue absorbs more x-rays than fat and appears as a medium gray shade.
12. What is PACS?
PACS (Picture Archiving and Communication System) is a digital system used to store, retrieve, and display radiographic images.
13. What advantages do digital radiographs have over traditional film?
Digital images allow adjustment of contrast, brightness, and magnification and enable easier storage and sharing.
14. How can digital radiographs assist in tracking patient progress?
Serial images can be viewed side by side to evaluate changes over time, such as resolving pneumonia.
15. Why is contrast between tissue densities important on a chest x-ray?
Structures are visible only when adjacent tissues have different densities, creating a visible border.
16. What is the silhouette sign?
The silhouette sign occurs when two adjacent structures of the same density obscure each other’s borders on a radiograph.
17. What does loss of the right heart border suggest?
It suggests pathology in the right middle lobe, such as pneumonia or atelectasis.
18. Why might a chest x-ray appear normal in respiratory failure?
Certain conditions, such as pulmonary embolism or early COPD, may not produce obvious radiographic changes.
19. Why can pneumonia initially be absent on a chest radiograph?
Radiographic changes may lag behind clinical symptoms and may not appear until 12 to 24 hours after onset.
20. Why can radiographic abnormalities persist after clinical improvement?
Inflammatory changes may remain visible on imaging for days to weeks after symptoms resolve.
21. What limitation results from the chest x-ray being a two-dimensional image?
It provides limited information about the depth or thickness of lesions or masses.
22. What structures can be evaluated on a chest radiograph?
The lungs, pleura, mediastinum, heart, diaphragm, and bony thorax can all be evaluated.
23. What happens to x-rays when they pass through dense tissue?
Dense tissue absorbs more x-rays, resulting in a lighter appearance on the image.
24. What is radiolucent tissue?
Radiolucent tissue allows x-rays to pass through easily and appears dark on the image.
25. What is radiopaque tissue?
Radiopaque tissue absorbs x-rays and appears white on the image.
26. Why is collaboration important when reviewing digital chest radiographs?
Multiple clinicians can simultaneously review images to coordinate care, especially in critical situations.
27. How can electronic medical records improve access to chest radiographs?
Imaging studies can be accessed across hospital systems, improving continuity of care.
28. Who typically decides when to obtain a chest x-ray?
The attending physician makes the final decision, often with input from bedside clinicians.
29. When might a respiratory therapist suggest obtaining a chest radiograph?
An RT may suggest imaging if a patient deteriorates suddenly or shows unexplained changes in respiratory status.
30. What is a key limitation of chest radiographs in evaluating lung nodules or masses?
Chest x-rays may not accurately determine the exact size, depth, or three-dimensional extent of lesions.
31. What is a common outpatient indication for obtaining a chest x-ray?
Unexplained dyspnea is a common reason to obtain a chest radiograph in the outpatient setting.
32. Why is a chest x-ray indicated in patients with severe persistent cough?
A chest x-ray helps evaluate for pneumonia, malignancy, tuberculosis, or other underlying pathology.
33. Why should hemoptysis prompt a chest radiograph?
Hemoptysis may indicate serious conditions such as infection, malignancy, or pulmonary embolism.
34. Why is a chest x-ray obtained in patients with fever and sputum production?
It helps assess for pneumonia or other infectious processes in the lungs.
35. Why is acute severe chest pain an indication for chest imaging?
A chest radiograph can help evaluate causes such as pneumothorax, pneumonia, or widened mediastinum.
36. Why is chest imaging recommended after a positive tuberculosis test?
A chest x-ray helps determine whether there is active pulmonary tuberculosis.
37. Why is a chest x-ray obtained after endotracheal tube placement?
It confirms proper tube positioning and rules out complications such as mainstem intubation.
38. Why is imaging performed after pulmonary artery catheter placement?
A chest x-ray confirms correct catheter location and identifies complications such as pneumothorax.
39. Why is chest radiography indicated after central venous catheter placement?
It verifies proper catheter tip placement and checks for procedure-related complications.
40. Why should sudden onset of dyspnea in hospitalized patients prompt a chest x-ray?
It may indicate pneumothorax, pulmonary edema, atelectasis, or other acute pathology.
41. Why is a chest x-ray indicated when plateau pressures increase during mechanical ventilation?
Elevated plateau pressures may suggest pneumothorax, pulmonary edema, or worsening lung compliance.
42. Why should a sudden decline in oxygenation prompt imaging?
A chest radiograph can help identify causes such as atelectasis, pneumonia, or pulmonary edema.
43. Why is a systematic approach important when interpreting a chest x-ray?
A disciplined approach reduces the risk of overlooking subtle but clinically significant findings.
44. Why can obvious abnormalities distract from more subtle findings?
Large lesions may draw attention away from smaller abnormalities such as nodules or free air.
45. What is the first step before interpreting a chest radiograph?
Confirm the patient’s identity and verify correct labeling.
46. Why is it important to confirm left and right markers on a chest x-ray?
Correct side identification prevents diagnostic errors, especially in conditions like situs inversus.
47. What should be assessed regarding film centering?
The spinous processes should be aligned midway between the medial ends of the clavicles.
48. How can patient rotation affect interpretation?
Rotation can falsely widen the mediastinum and distort the appearance of pulmonary structures.
49. What is meant by penetration in chest radiography?
Penetration refers to the degree of x-ray beam exposure and its ability to pass through tissues.
50. What indicates proper penetration on a chest x-ray?
Intervertebral disc spaces should be visible through the cardiac silhouette.
51. What is an underpenetrated chest x-ray?
An underpenetrated film appears too white and may obscure mediastinal or lung details.
52. How can an underpenetrated film lead to misinterpretation?
Normal vascular markings may appear abnormal and mimic interstitial disease.
53. What is an overpenetrated chest x-ray?
An overpenetrated film appears too dark, making lung markings and subtle opacities difficult to see.
54. Why must the RT consider whether a film is PA or AP?
Heart size and certain findings may appear exaggerated on AP films.
55. What is the difference between PA and AP chest radiographs?
In a PA film, the x-ray beam passes from back to front; in an AP film, it passes from front to back.
56. Why do AP portable films often show an enlarged cardiac silhouette?
The closer x-ray source and patient positioning cause magnification of the heart shadow.
57. Why are AP films commonly used in the ICU?
Critically ill patients are often unable to stand or travel for standard PA imaging.
58. What should be evaluated regarding the completeness of the film?
Ensure the entire chest, including lung apices and costophrenic angles, is included.
59. How can rotation be assessed on a chest radiograph?
Compare the medial ends of the clavicles to the spinous processes for symmetry.
60. Why is proper positioning critical when interpreting mediastinal width?
Improper positioning can falsely suggest mediastinal widening.
61. How does digital technology improve evaluation of improperly exposed films?
Contrast and brightness adjustments can enhance visibility of certain structures.
62. Why can digital adjustments not fully correct poor exposure?
Important structural details may be permanently lost if the original exposure was inadequate.
63. Why is it recommended to evaluate lung parenchyma last during interpretation?
Examining other structures first reduces the likelihood of missing nonpulmonary abnormalities.
64. What structures should be systematically reviewed on a chest radiograph?
The bones, soft tissues, diaphragm, mediastinum, heart, pleura, and lung fields should all be assessed.
65. Why is it important to recognize technical limitations before diagnosing pathology?
Technical errors can mimic disease and lead to incorrect clinical decisions.
66. What should be assessed after reviewing the technical quality of a chest x-ray?
All visible anatomic structures should be evaluated systematically for normal and abnormal findings.
67. What major bony structures are visible on a chest radiograph?
The ribs, clavicles, scapulae, and vertebrae are the primary bony structures visualized.
68. Why is it important to assess the ribs individually?
Each rib should be traced to identify fractures, lesions, or deformities.
69. What soft tissues can be evaluated on a chest x-ray?
Chest wall tissues, portions of the upper abdomen, and breast shadows can be evaluated.
70. What structures are included when evaluating the lungs on a chest radiograph?
Evaluation includes the trachea, bronchi, and lung parenchyma.
71. Why can lung abnormalities be difficult to detect on a frontal view?
Up to 80% to 90% of the lung parenchyma is overlapped by bone, which can obscure subtle findings.
72. How can a lateral chest view assist in interpretation?
A lateral view helps clarify abnormalities that may be hidden behind the heart or diaphragm on a frontal film.
73. What areas require special attention for subtle lung abnormalities?
The lung apices, retrocardiac region, and posterior costophrenic sulci should be carefully inspected.
74. What pleural abnormalities can be detected on a chest radiograph?
Pleural effusion, hemothorax, and pneumothorax are common pleural abnormalities.
75. What is the pleural space?
The pleural space is the potential space between the visceral and parietal pleura.
76. What structures make up the mediastinum?
The mediastinum contains the heart, great vessels, trachea, esophagus, and lymph nodes.
77. What are the anatomic borders of the mediastinum?
It is bordered anteriorly by the sternum, posteriorly by the vertebral column, superiorly by the thoracic inlet, and inferiorly by the diaphragm.
78. What is the cardiothoracic ratio?
The cardiothoracic ratio is the ratio of the heart’s width to the width of the thoracic cage.
79. What cardiothoracic ratio indicates cardiomegaly on a PA film?
A ratio greater than 50% on a PA chest radiograph suggests cardiomegaly.
80. Why is heart size difficult to assess on an AP film?
The heart appears magnified on AP films due to the closer x-ray source and patient positioning.
81. What radiographic findings suggest congestive heart failure?
Cardiomegaly, upper lobe vascular prominence, Kerley B lines, and pleural effusions suggest heart failure.
82. What are Kerley B lines?
Kerley B lines are short horizontal lines at the lung periphery indicating interstitial edema.
83. How does atelectasis affect mediastinal structures?
Atelectasis pulls the mediastinum and trachea toward the affected side.
84. How do large pleural effusions affect mediastinal position?
Large effusions push the mediastinum away from the affected side.
85. Where should the endotracheal tube tip be positioned on chest x-ray?
The tip should be 4–6 cm above the carina.
86. What vertebral level corresponds to proper endotracheal tube placement?
Proper placement is typically between thoracic vertebrae T2 and T4.
87. Why are radiopaque markers embedded in medical devices?
Radiopaque markers allow visualization of tubes and catheters on radiographs.
88. What are common foreign bodies seen on chest x-ray?
Coins, bullets, teeth, and certain medical devices may appear as radiopaque objects.
89. Why are lateral neck radiographs useful in children?
They help evaluate upper airway obstruction from foreign bodies or infections.
90. What radiographic finding may indicate a perforated gastrointestinal tract?
Air under the diaphragm suggests free intraperitoneal air from perforation.
91. What causes blunting of the costophrenic angles?
Pleural effusion or lower-lobe pneumonia can blunt the costophrenic angles.
92. What causes flattening of a hemidiaphragm?
Hyperinflation or tension pneumothorax can flatten the diaphragm.
93. What conditions may elevate a hemidiaphragm?
Phrenic nerve paralysis, atelectasis, or abdominal organ enlargement can elevate it.
94. What causes increased radiopacity on a chest radiograph?
Atelectasis, consolidation, pleural effusion, tumors, and calcifications increase radiopacity.
95. What causes increased radiolucency on a chest radiograph?
Emphysema, pneumothorax, and subcutaneous emphysema increase radiolucency.
96. Why should pleural effusion films ideally be taken upright?
An upright film allows visualization of the pleural fluid meniscus.
97. How does a pleural effusion appear on a supine film?
It may appear as a diffuse haziness due to posterior fluid layering.
98. What is a lateral decubitus chest x-ray used for?
It helps detect small pleural effusions and assess fluid mobility.
99. How small of a pleural effusion can be detected on a lateral decubitus film?
Effusions as small as approximately 5 mL can be detected.
100. Why is it important to compare current chest radiographs with prior films?
Comparison helps determine whether findings are new, stable, or resolving.
Final Thoughts
The chest radiograph remains one of the most powerful and accessible diagnostic tools in respiratory care. For respiratory therapists, the ability to interpret chest imaging is not optional—it is fundamental to safe and effective practice.
From confirming airway placement to identifying life-threatening complications and guiding ventilator management, the chest x-ray directly influences patient outcomes.
By developing a disciplined, systematic approach and understanding both its strengths and limitations, respiratory therapists can confidently use chest radiographs to enhance clinical decision-making and improve the quality of care they provide.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Kelly B. The chest radiograph. Ulster Med J. 2012.

