Panlobular emphysema is a form of chronic obstructive pulmonary disease (COPD) characterized by uniform destruction of the entire acinus, affecting both the respiratory bronchioles and alveoli. It most commonly occurs in the lower lobes of the lungs and is strongly associated with alpha-1 antitrypsin deficiency, a genetic condition that reduces the lung’s ability to protect itself from enzymatic damage.
As the alveolar walls break down, the surface area for gas exchange decreases, leading to progressive shortness of breath and reduced oxygen levels in the blood.
Understanding the underlying causes and clinical features of panlobular emphysema is essential for early diagnosis and appropriate management.
What Is Panlobular Emphysema?
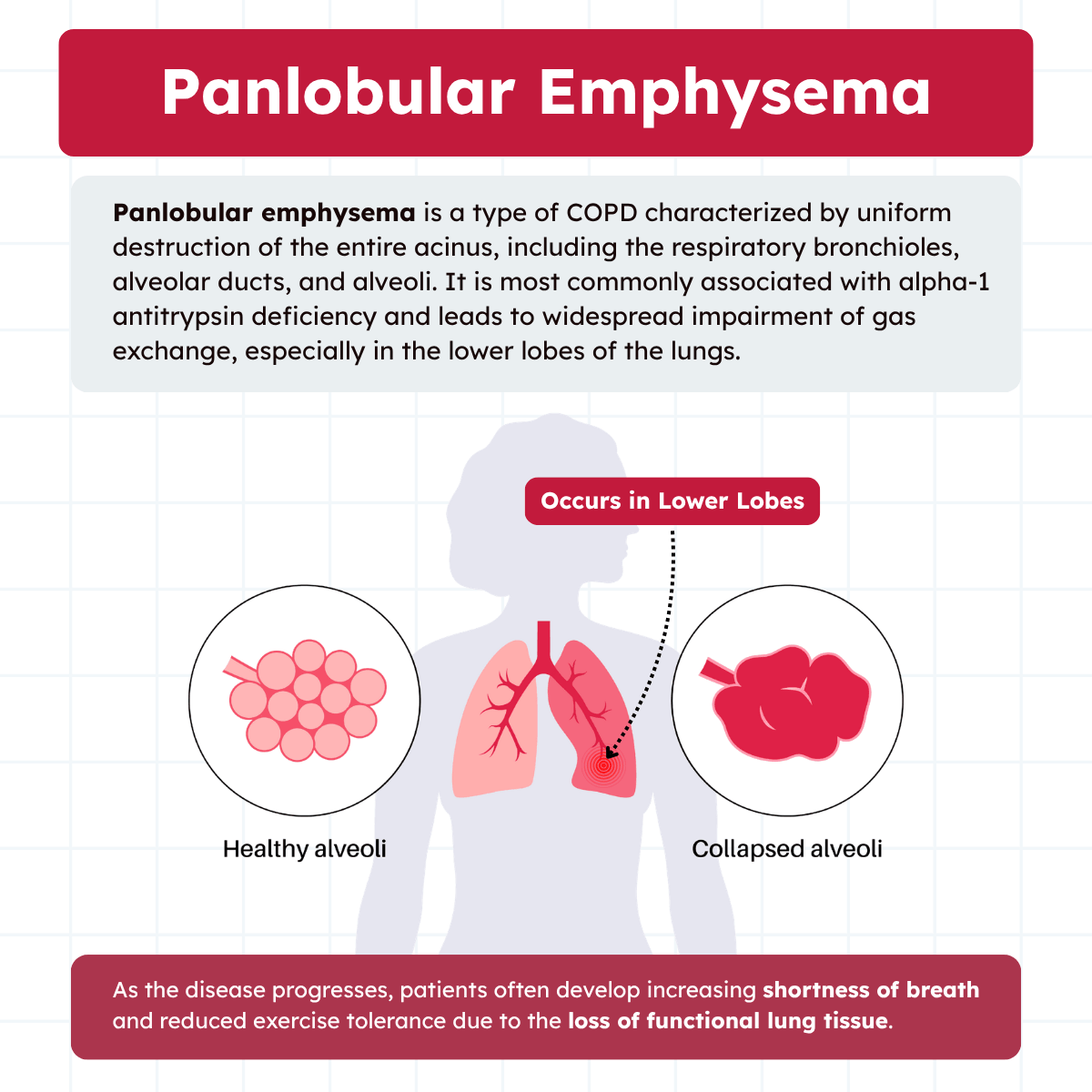
Panlobular emphysema is a type of COPD characterized by uniform destruction of the entire acinus, including the respiratory bronchioles, alveolar ducts, and alveoli. Unlike centrilobular emphysema, which affects only the central portion of the lobule, panlobular emphysema involves the entire structure, leading to more diffuse and widespread lung damage.
This form of emphysema is most commonly associated with alpha-1 antitrypsin deficiency, a genetic disorder that reduces the lungs’ protection against enzymatic injury. It typically affects the lower lobes of the lungs and can develop at a younger age compared to smoking-related emphysema.
As the disease progresses, the loss of alveolar surface area impairs gas exchange, resulting in symptoms such as shortness of breath, fatigue, and decreased exercise tolerance. Early diagnosis and appropriate management are essential to slow progression and improve quality of life.
Distinguishing Features
Panlobular emphysema, also called panacinar emphysema, involves uniform destruction of the pulmonary acinus. The entire lobule is affected rather than specific regions within it.
This type primarily affects the lower lung zones. The alveolar walls undergo widespread destruction, creating large, simplified airspaces throughout the affected areas.
Key distinguishing features include:
- Uniform involvement of the entire acinus
- Predominance in lung bases
- Strong association with alpha-1 antitrypsin deficiency
- Earlier age of onset compared to centrilobular emphysema
Note: The destruction pattern appears homogeneous on imaging studies. This contrasts with the patchy, irregular distribution seen in other emphysema subtypes.
Pathophysiology
The destruction in panlobular emphysema results from an imbalance between proteases and antiproteases in lung tissue. Alpha-1 antitrypsin normally protects the lungs from neutrophil elastase, an enzyme that breaks down elastin.
When alpha-1 antitrypsin levels are deficient, unopposed elastase activity destroys alveolar walls throughout the acinus. This creates permanently enlarged airspaces without obvious fibrosis.
The loss of elastic recoil reduces the lung’s ability to expel air during expiration. Airways collapse prematurely, trapping air and causing hyperinflation. Gas exchange becomes impaired as the surface area for oxygen and carbon dioxide transfer decreases significantly.
Comparison With Other Emphysema Types
Centrilobular emphysema affects the proximal portion of the acinus while sparing distal alveoli. It predominates in upper lung zones and relates strongly to cigarette smoking.
Paraseptal emphysema involves distal acini along the pleura and interlobular septa. It typically occurs in the upper lobes and may cause spontaneous pneumothorax in young adults.
Panlobular emphysema shows no regional preference within the acinus and favors lower lobes. The genetic component is stronger than in other types, with alpha-1 antitrypsin deficiency present in most cases. Patients often develop symptoms at younger ages, particularly when combined with smoking.
Etiology and Risk Factors
Panlobular emphysema develops primarily through genetic deficiencies that compromise lung protection, though environmental exposures can accelerate disease progression in susceptible individuals.
Alpha-1 Antitrypsin Deficiency
Alpha-1 antitrypsin deficiency (AATD) represents the most significant genetic cause of panlobular emphysema. This inherited condition results from mutations in the SERPINA1 gene, leading to reduced production or dysfunctional alpha-1 antitrypsin protein.
The protein normally protects lung tissue from neutrophil elastase, an enzyme that breaks down elastin in alveolar walls. Without adequate protection, elastase destroys lung parenchyma throughout the acini. Individuals with severe AATD, particularly those with PiZZ phenotype, often develop emphysema in their 30s to 50s, decades earlier than typical smoking-related disease.
The condition follows autosomal codominant inheritance patterns. Homozygous individuals face the highest risk, while heterozygous carriers may develop lung disease if combined with smoking or other exposures. AATD accounts for 1-2% of all emphysema cases but should be suspected in patients with early-onset disease or a basilar-predominant distribution on imaging.
Other Genetic Factors
Beyond AATD, several genetic variants influence susceptibility to panlobular emphysema. Polymorphisms in matrix metalloproteinases and tissue inhibitors affect extracellular matrix degradation rates.
Variations in genes regulating oxidative stress responses and inflammatory pathways modify individual risk. These genetic factors typically require environmental triggers to manifest clinically. Family history of emphysema independent of AATD suggests polygenic contributions to disease development.
Environmental and Lifestyle Contributors
Cigarette smoking accelerates panlobular emphysema progression in genetically susceptible individuals, particularly those with AATD. Smoke exposure increases protease activity and oxidative stress while impairing antiprotease defenses.
Occupational exposures to dust, chemicals, and fumes contribute to lung damage. Cadmium and silica exposure show particular associations with emphysema development. Indoor air pollution from biomass fuel combustion affects individuals in developing regions.
Respiratory infections during childhood may increase later susceptibility. Intravenous drug use has been linked to panlobular emphysema through mechanisms involving talc or other contaminants. Nutritional deficiencies and low body weight correlate with increased risk in predisposed populations.
Clinical Presentation
Panlobular emphysema presents with progressive respiratory symptoms that reflect uniform destruction of alveolar tissue throughout the acini. Patients typically exhibit dyspnea and reduced exercise tolerance, with physical examination revealing characteristic signs of hyperinflation and air trapping.
Common Signs and Symptoms
Progressive dyspnea represents the primary complaint in patients with panlobular emphysema. The breathlessness initially occurs during exertion but advances to affect rest as the disease progresses.
Chronic cough may be present, though it tends to be less prominent than in other forms of chronic obstructive pulmonary disease. Sputum production is typically minimal or absent unless concurrent bronchitis develops.
Patients frequently report reduced exercise capacity and fatigue during daily activities. Weight loss and muscle wasting occur commonly, particularly in advanced cases, as the increased work of breathing elevates metabolic demands. Some patients experience a sensation of chest tightness or inability to take a satisfying breath.
Early Versus Advanced Stage Manifestations
Early-stage panlobular emphysema often produces subtle symptoms that patients may attribute to aging or deconditioning. Mild dyspnea during moderate exertion and slightly decreased stamina are typical initial presentations.
As the condition advances, dyspnea becomes more pronounced and occurs with minimal activity. Patients develop visible use of accessory respiratory muscles and pursed-lip breathing to maintain adequate ventilation.
Advanced disease manifests with dyspnea at rest and severe limitation of physical activity. Patients may adopt a characteristic forward-leaning posture to optimize breathing mechanics. Cor pulmonale can develop in late stages, producing peripheral edema and signs of right heart strain.
Physical Examination Findings
Inspection reveals a barrel-shaped chest with increased anteroposterior diameter and hyperinflation. Patients often appear thin with decreased muscle mass, particularly in the extremities and temporal regions.
Percussion produces hyperresonance across lung fields due to increased air trapping. The diaphragm sits in a flattened position, reducing the normal area of cardiac dullness.
Auscultation demonstrates diminished breath sounds bilaterally with decreased intensity throughout all lung fields. Wheezing may be audible but is less prominent than in chronic bronchitis. Heart sounds are often distant or muffled due to hyperinflation.
Note: Cyanosis may appear in advanced cases, typically affecting the lips and nail beds. Digital clubbing is uncommon in pure emphysema and suggests alternative or concurrent pathology.
Diagnostic Methods
Accurate diagnosis of panlobular emphysema requires a combination of imaging studies, lung function measurements, and blood work to assess disease severity and rule out other conditions.
Imaging Techniques
High-resolution computed tomography (HRCT) serves as the gold standard for diagnosing panlobular emphysema. The scan reveals uniform destruction of alveoli throughout the entire acinus, with particular prominence in the lower lung zones. This distribution pattern distinguishes panlobular emphysema from centrilobular emphysema, which affects upper lobes more severely.
Chest X-rays may show hyperinflation, flattened diaphragms, and increased lung lucency. However, these radiographs lack the sensitivity to detect early-stage disease or differentiate between emphysema subtypes. CT imaging provides superior detail of parenchymal destruction and allows quantitative assessment of emphysema extent.
Radiologists evaluate CT scans for areas of low attenuation, vascular pruning, and bullae formation. Quantitative CT analysis measures the percentage of lung tissue below specific density thresholds, typically -950 Hounsfield units. This objective measurement helps track disease progression over time.
Pulmonary Function Tests
Spirometry demonstrates obstructive lung disease with reduced forced expiratory volume in one second (FEV1) and decreased FEV1/FVC ratio. Patients with panlobular emphysema typically show values below 70% of predicted normal.
Lung volume measurements reveal increased total lung capacity (TLC) and residual volume (RV) due to air trapping. The RV/TLC ratio often exceeds 40%, indicating significant hyperinflation. Functional residual capacity also increases as the lungs lose elastic recoil.
Diffusing capacity of the lungs for carbon monoxide (DLCO) shows marked reduction in panlobular emphysema. This test measures gas exchange efficiency across the alveolar-capillary membrane. Values below 40% of predicted suggest severe parenchymal destruction.
Laboratory Assessments
Alpha-1 antitrypsin (AAT) level testing is essential for all patients diagnosed with panlobular emphysema, particularly those under age 45 or with minimal smoking history. Serum AAT levels below 11 micromoles per liter indicate deficiency and warrant genetic testing.
Phenotyping or genotyping identifies specific AAT variants, with PiZZ representing the most severe deficiency state. Testing family members becomes necessary when deficiency is confirmed. Arterial blood gas analysis evaluates oxygen and carbon dioxide levels in advanced disease, guiding supplemental oxygen therapy decisions.
Disease Progression and Complications
Panlobular emphysema follows a progressive course characterized by diffuse alveolar destruction that leads to declining lung function and increasing disability. The disease typically advances through predictable stages while predisposing patients to multiple respiratory and systemic complications.
Natural History
Panlobular emphysema progresses insidiously over years to decades, with lung tissue destruction occurring throughout all portions of the pulmonary acini. Patients experience gradual worsening of dyspnea, initially with exertion and eventually at rest. Pulmonary function testing reveals a steady decline in forced expiratory volume in one second (FEV1), typically decreasing by 50-100 mL annually in continued smokers compared to 25-30 mL in nonsmokers.
The disease preferentially affects the lower lobes in most cases. As destruction advances, patients develop chronic hypoxemia requiring supplemental oxygen. Alpha-1 antitrypsin deficiency-related panlobular emphysema demonstrates particularly aggressive progression, with symptoms often appearing in the fourth or fifth decade of life.
Associated Comorbidities
Patients with panlobular emphysema face elevated risk for several concurrent conditions. Pulmonary hypertension develops in approximately 50% of patients with advanced disease due to hypoxic vasoconstriction and reduced pulmonary vascular bed. Right ventricular dysfunction and cor pulmonale emerge as secondary complications when pulmonary arterial pressures remain chronically elevated.
Pneumothorax occurs with increased frequency due to rupture of emphysematous bullae. Recurrent respiratory infections become more common as mucociliary clearance mechanisms fail and airway defenses weaken. Cardiovascular disease represents a major comorbidity, with patients showing 2-3 times higher risk for coronary artery disease, arrhythmias, and heart failure compared to the general population.
Respiratory Insufficiency
Progressive alveolar destruction leads to declining gas exchange capacity and eventual respiratory failure. Type II respiratory failure with hypercapnia develops as ventilatory demand exceeds the capacity of damaged lungs. Acute exacerbations precipitated by infections or environmental exposures can trigger rapid decompensation requiring mechanical ventilation.
Chronic respiratory insufficiency necessitates long-term oxygen therapy in most patients with advanced disease. Ventilatory support becomes increasingly necessary as muscle fatigue develops from prolonged hyperinflation and increased work of breathing. Survival after onset of chronic respiratory failure averages 2-5 years without lung transplantation.
Treatment Strategies
Managing panlobular emphysema requires a combination of pharmacological interventions and significant behavioral changes to slow disease progression and improve quality of life. Treatment focuses on reducing symptoms, preventing complications, and maximizing lung function.
Medical Management
Bronchodilators form the foundation of pharmacological treatment for panlobular emphysema. Short-acting beta-agonists provide quick relief during acute episodes, while long-acting bronchodilators offer sustained symptom control throughout the day. Anticholinergic medications help reduce airway resistance and mucus production.
Inhaled corticosteroids are prescribed to patients experiencing frequent exacerbations or significant inflammation. These medications reduce airway swelling and may decrease the frequency of acute episodes. Combination inhalers containing both bronchodilators and corticosteroids simplify treatment regimens and improve adherence.
Oxygen therapy becomes necessary when blood oxygen levels fall below target ranges, typically when saturation drops below 88% at rest. Supplemental oxygen improves exercise tolerance, reduces dyspnea, and may prolong survival in patients with severe hypoxemia. Pulmonary rehabilitation programs combine exercise training, education, and breathing techniques to optimize physical function and reduce hospital admissions.
Lifestyle Modifications
Smoking cessation represents the most critical intervention for patients with panlobular emphysema. Stopping tobacco use immediately slows the rate of lung function decline and reduces the risk of respiratory infections. Nicotine replacement therapy, prescription medications, and behavioral counseling increase success rates.
Patients should receive annual influenza vaccinations and pneumococcal vaccines to prevent respiratory infections that can trigger dangerous exacerbations. Avoiding environmental pollutants, secondhand smoke, and occupational irritants protects remaining lung tissue from further damage.
Regular physical activity maintains muscle strength and cardiovascular fitness despite respiratory limitations. Breathing exercises and techniques such as pursed-lip breathing help patients manage dyspnea during daily activities. Nutritional support addresses weight loss and muscle wasting commonly seen in advanced disease.
Advanced Therapies and Interventions
Treatment options for panlobular emphysema extend beyond medication to include structured rehabilitation programs, supplemental oxygen support, and surgical procedures that can improve lung function and quality of life.
Pulmonary Rehabilitation
Pulmonary rehabilitation represents a comprehensive program combining exercise training, education, and behavioral modifications. These programs typically last 6 to 12 weeks and involve supervised exercise sessions 2 to 3 times per week.
Patients engage in aerobic exercises like walking or cycling alongside strength training to improve respiratory muscle function. The programs also teach breathing techniques, energy conservation strategies, and proper medication use.
Studies show participants experience reduced shortness of breath, increased exercise capacity, and fewer hospitalizations. The benefits persist for months after program completion when patients maintain their exercise routines at home.
Oxygen Therapy
Long-term oxygen therapy becomes necessary when blood oxygen levels fall below specific thresholds, typically a partial pressure of oxygen below 55 mmHg or oxygen saturation below 88%. Patients who qualify must use oxygen for at least 15 hours daily to receive maximum benefit.
Oxygen delivery systems include compressed gas cylinders, liquid oxygen tanks, and oxygen concentrators. Portable concentrators allow patients to maintain mobility while receiving continuous oxygen support.
Note: This therapy improves survival rates in patients with severe hypoxemia and reduces strain on the heart. Proper oxygen flow rates must be prescribed and monitored by healthcare providers to prevent complications.
Surgical Options
- Lung volume reduction surgery removes damaged portions of the lung, allowing healthier tissue to expand and function more efficiently. Candidates typically have emphysema predominantly in the upper lobes and low exercise capacity despite rehabilitation.
- Lung transplantation serves as an option for patients with end-stage disease who meet strict eligibility criteria. Single lung transplants are most common for emphysema patients.
- Bronchoscopic interventions offer less invasive alternatives, including endobronchial valve placement and coil implantation. These procedures reduce lung hyperinflation without requiring major surgery.
Note: Patient selection depends on disease distribution, severity, and absence of significant collateral ventilation between lung segments.
Prognosis and Quality of Life
Panlobular emphysema carries a variable prognosis that depends on disease severity, smoking cessation, and comorbidities. Patients with alpha-1 antitrypsin deficiency often develop symptoms earlier in life compared to those with smoking-related disease.
Life expectancy decreases as lung function declines. The FEV1 measurement serves as a key predictor of survival, with lower values indicating worse outcomes. Patients who continue smoking experience faster disease progression than those who quit.
Quality of life deteriorates progressively as the condition advances. Common factors that impact daily living include:
- Persistent dyspnea during routine activities
- Reduced exercise tolerance and physical endurance
- Frequent respiratory infections requiring medical intervention
- Anxiety and depression related to breathing difficulties
- Social isolation due to activity limitations
- Oxygen dependency in advanced stages
Most patients experience significant functional decline over time. Simple tasks like walking, climbing stairs, or personal care become increasingly difficult. Many require supplemental oxygen therapy, which restricts mobility and independence.
Exacerbations accelerate disease progression and worsen prognosis. Each acute episode damages lung tissue further and increases mortality risk. The frequency of exacerbations correlates with faster decline in lung function.
Survival rates vary widely between individuals. Patients with severe panlobular emphysema and very low FEV1 values face a five-year survival rate of approximately 30-40% without lung transplantation. Early diagnosis and aggressive management improve outcomes and maintain functional capacity longer.
Pulmonary rehabilitation programs help preserve quality of life by improving exercise tolerance and reducing symptom burden. However, they do not reverse structural lung damage or halt disease progression.
Current Research and Future Directions
Researchers are investigating several therapeutic approaches to slow or reverse panlobular emphysema progression. Gene therapy targeting alpha-1 antitrypsin deficiency shows promise in early clinical trials, with some studies demonstrating increased protein levels in patients’ lungs.
Stem cell therapies represent another active area of investigation. Scientists are exploring whether mesenchymal stem cells can regenerate damaged lung tissue and reduce inflammation in panlobular emphysema patients.
Key research areas include:
- Development of selective neutrophil elastase inhibitors to prevent further tissue destruction
- Advanced imaging techniques for earlier disease detection
- Biomarker identification for predicting disease progression
- Personalized medicine approaches based on genetic profiles
- Novel anti-inflammatory agents targeting specific cellular pathways
Lung volume reduction surgery techniques continue to evolve, with researchers examining which patient populations benefit most from intervention. New bronchoscopic procedures offer less invasive alternatives to traditional surgery.
Clinical trials are evaluating combination therapies that address multiple disease mechanisms simultaneously. These approaches may include augmentation therapy paired with anti-inflammatory medications and pulmonary rehabilitation protocols.
Artificial intelligence and machine learning algorithms are being developed to predict disease trajectories and optimize treatment timing. These tools analyze imaging data, pulmonary function tests, and genetic information to create individualized risk assessments.
Researchers are also studying the long-term outcomes of lung transplantation in alpha-1 antitrypsin deficiency patients. This work helps identify optimal candidate selection criteria and post-transplant management strategies. Understanding environmental factors that accelerate disease progression remains a priority for prevention-focused research.
FAQs About Panlobular Emphysema
What Is the Difference Between Emphysema and Panlobular Emphysema?
Emphysema is a general term for a type of COPD that involves destruction of the alveoli and impaired gas exchange. Panlobular emphysema is a specific subtype in which the entire acinus is uniformly affected, including the respiratory bronchioles, alveolar ducts, and alveoli.
This form tends to be more diffuse and is often associated with genetic conditions such as alpha-1 antitrypsin deficiency, whereas other types of emphysema may have different patterns and causes.
What Are the Risk Factors for Panlobular Emphysema?
The most significant risk factor for panlobular emphysema is alpha-1 antitrypsin deficiency, a genetic disorder that reduces the lungs’ ability to protect against enzymatic damage. Smoking can worsen the condition and accelerate lung destruction in affected individuals.
Additional risk factors include exposure to air pollutants, occupational dust, and respiratory irritants. A family history of lung disease may also increase the likelihood of developing this condition, particularly when combined with environmental exposures.
What Is the Life Expectancy of a Person with Panlobular Emphysema?
Life expectancy varies depending on the severity of the disease, underlying genetic factors, and whether the condition is properly managed. Individuals with alpha-1 antitrypsin deficiency may develop symptoms at a younger age, which can impact long-term outcomes.
However, early diagnosis, smoking cessation, and appropriate treatment can help slow progression and improve survival. With proper care, many individuals can maintain a reasonable quality of life for years, although advanced disease may significantly reduce life expectancy.
What Is Mild Panlobular Emphysema?
Mild panlobular emphysema refers to the early stage of the disease, where the destruction of the acinus is limited and symptoms may be minimal or not yet noticeable. It is often detected through imaging studies or pulmonary function testing.
At this stage, lung function may still be relatively preserved, allowing individuals to carry out normal activities. Early intervention, including lifestyle changes and medical management, is essential to slow disease progression and maintain lung function over time.
How Serious Is Panlobular Emphysema?
Panlobular emphysema is a serious and progressive lung disease that can significantly impair breathing and oxygen exchange. Because it affects the entire acinus, the damage is often more widespread and can lead to earlier and more severe symptoms compared to other forms of emphysema.
As the condition advances, patients may experience severe shortness of breath, fatigue, and reduced physical capacity. Without proper management, complications such as respiratory failure may occur, making early detection and treatment crucial.
Can Covid-19 Cause Panlobular Emphysema?
COVID-19 does not directly cause panlobular emphysema, but it can lead to lung inflammation and injury that may worsen existing respiratory conditions. In severe cases, COVID-19 can cause long-term lung damage, including scarring, which may resemble or contribute to emphysema-like changes.
However, panlobular emphysema is primarily associated with genetic factors such as alpha-1 antitrypsin deficiency rather than viral infections. Patients with underlying lung disease may experience more severe complications from COVID-19.
Is Panlobular Emphysema a Type of Cancer?
Panlobular emphysema is not a type of cancer. It is a chronic lung condition characterized by the destruction of airspaces and impaired gas exchange. However, some risk factors, such as smoking, can increase the likelihood of both emphysema and lung cancer.
While panlobular emphysema itself does not involve malignant growth, individuals with chronic lung disease may require regular monitoring to detect potential complications or coexisting conditions, including cancer.
How Fast Does Panlobular Emphysema Progress?
The progression of panlobular emphysema varies depending on the underlying cause and individual factors. In cases related to alpha-1 antitrypsin deficiency, the disease may develop earlier and progress more rapidly.
Smoking and environmental exposures can further accelerate lung damage. Without intervention, lung function may decline steadily over time. However, early diagnosis, avoidance of risk factors, and appropriate treatment can significantly slow progression and help preserve lung function.
Is Panlobular Emphysema the Same as COPD?
Panlobular emphysema is not the same as COPD, but it is a type of COPD. COPD is a broad term that includes conditions such as chronic bronchitis and emphysema, all of which cause airflow limitation.
Panlobular emphysema is a specific subtype characterized by uniform involvement of the entire acinus. While all individuals with panlobular emphysema have COPD, not all individuals with COPD have this particular form of emphysema.
Is Panlobular Emphysema Reversible?
Panlobular emphysema is not reversible because the structural damage to the lungs is permanent. Once the alveoli and surrounding tissues are destroyed, they cannot regenerate. However, the progression of the disease can be slowed with proper management.
Treatment strategies include smoking cessation, medications, and, in some cases, augmentation therapy for alpha-1 antitrypsin deficiency. These measures can improve symptoms, enhance quality of life, and reduce the risk of complications.
Final Thoughts
Panlobular emphysema is a progressive lung condition that can significantly affect breathing and overall quality of life, particularly when linked to alpha-1 antitrypsin deficiency. Although the damage to lung tissue is permanent, early diagnosis and appropriate management can help slow disease progression and reduce symptoms.
Avoiding smoking and environmental exposures, along with medical therapies and supportive care, plays a key role in maintaining lung function. With proper treatment and ongoing monitoring, individuals can better manage the condition and improve their long-term outcomes.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Anderson AE Jr, Foraker AG. Centrilobular emphysema and panlobular emphysema: two different diseases. Thorax. 1973.