Emphysema is a chronic lung disease characterized by permanent destruction of the alveoli and loss of elastic recoil, leading to airflow limitation and impaired gas exchange. It is one of the primary conditions included under the broader diagnosis of chronic obstructive pulmonary disease (COPD).
The disease develops gradually, most often as a result of long-term cigarette smoking, but genetic factors such as alpha-1 antitrypsin deficiency can also contribute.
For respiratory therapists, emphysema is highly relevant because it affects ventilation, oxygenation, and long-term respiratory function across multiple care settings.
What is Emphysema?
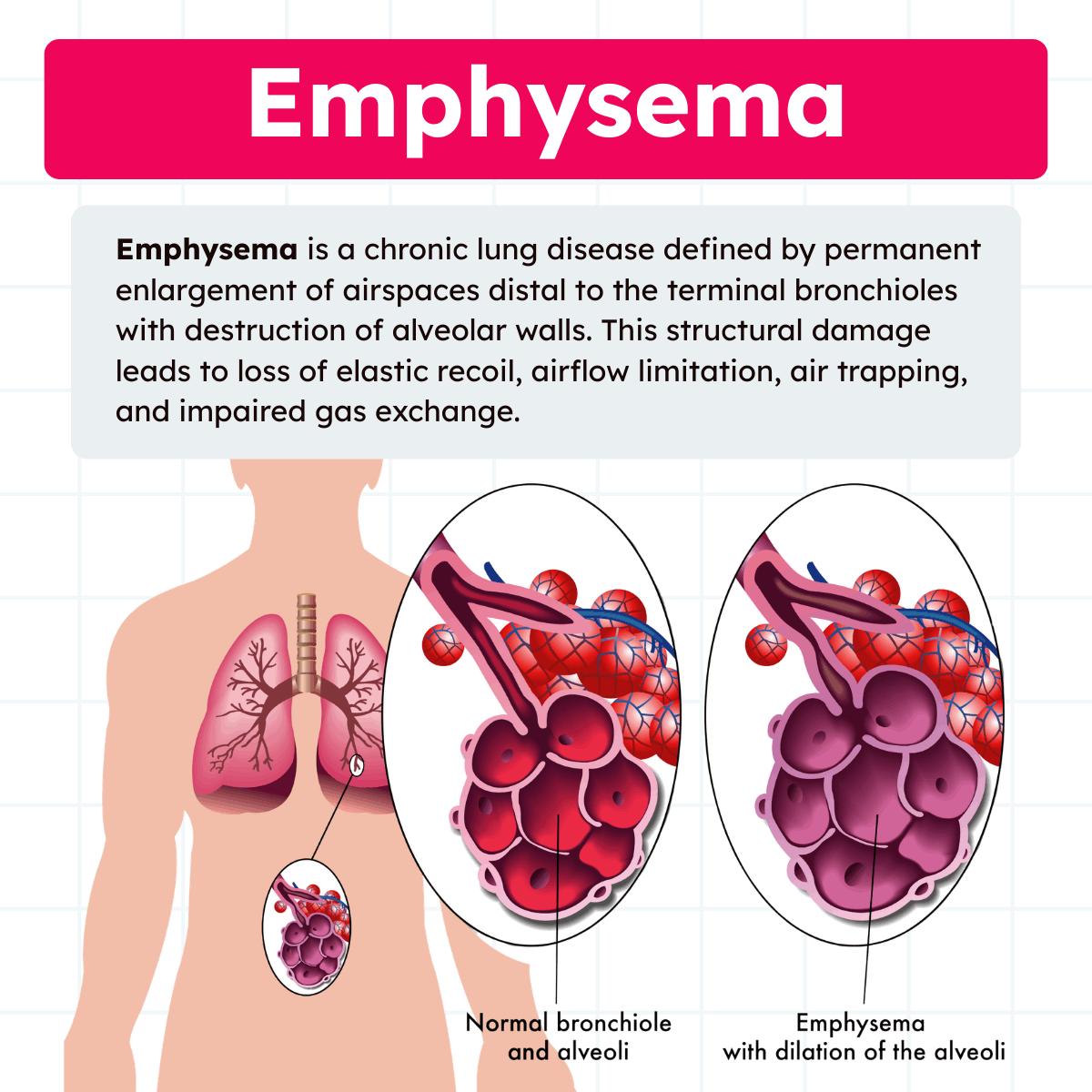
Emphysema is defined anatomically as abnormal, permanent enlargement of the airspaces distal to the terminal bronchioles, accompanied by destruction of alveolar walls and loss of elastic tissue. Unlike chronic bronchitis, which is defined clinically by symptoms, emphysema is defined by structural changes within the lung parenchyma.
The destruction of alveolar walls reduces the surface area available for gas exchange. At the same time, the loss of elastic recoil impairs the lung’s ability to expel air during expiration. Together, these changes lead to airflow limitation, air trapping, and progressive hyperinflation.
Although emphysema most commonly occurs as part of COPD, it can also develop in individuals with alpha-1 antitrypsin deficiency or other less common conditions.
Pathophysiology of Emphysema
Understanding emphysema requires an appreciation of normal lung mechanics. In healthy lungs, elastic fibers within the alveolar walls provide recoil that keeps small airways open during expiration. Gas exchange occurs across thin alveolar-capillary membranes with a large combined surface area.
In emphysema, several pathophysiologic processes occur.
Alveolar Wall Destruction
The defining feature of emphysema is destruction of the alveolar septa. As walls break down, adjacent alveoli merge into larger airspaces. This reduces total alveolar surface area and disrupts the pulmonary capillary bed.
The consequences include:
- Decreased diffusing capacity
- Reduced surface area for oxygen and carbon dioxide exchange
- Increased physiologic dead space
Note: As capillaries are destroyed along with alveoli, ventilation-perfusion relationships become abnormal.
Loss of Elastic Recoil
Elastic fibers are responsible for passive exhalation. When elastin is destroyed, the lungs lose their natural tendency to recoil inward.
Without adequate recoil:
- Small airways collapse prematurely during expiration
- Air becomes trapped distal to collapsed airways
- End-expiratory lung volume increases
Note: This process leads to hyperinflation and increased residual volume. Over time, total lung capacity may also increase.
Dynamic Hyperinflation
As airflow limitation worsens, patients are unable to fully exhale before the next breath begins. This results in dynamic hyperinflation, particularly during exertion when respiratory rate increases.
Dynamic hyperinflation causes:
- Increased work of breathing
- Diaphragmatic flattening
- Mechanical disadvantage of respiratory muscles
- Increased sensation of dyspnea
Note: The diaphragm becomes shortened and less efficient. Accessory muscles of respiration are recruited to maintain ventilation.
Ventilation-Perfusion Abnormalities
Emphysema disrupts both ventilation and perfusion. Destruction of alveoli and capillaries increases dead space ventilation. Although some regions may remain ventilated, they may no longer be adequately perfused.
Note: As disease progresses, ventilation-perfusion mismatch contributes to hypoxemia. Hypercapnia usually develops later, when ventilatory capacity is significantly impaired.
Types of Emphysema
Centriacinar Emphysema
Centriacinar emphysema primarily affects the respiratory bronchioles in the central portion of the acinus. It is most commonly associated with cigarette smoking and typically involves the upper lobes. This is the most common form seen in smokers.
Panacinar Emphysema
Panacinar emphysema involves uniform destruction of the entire acinus. It is classically associated with alpha-1 antitrypsin deficiency and tends to affect the lower lobes more prominently. Because the entire acinus is involved, gas exchange impairment may be significant.
Paraseptal Emphysema
Paraseptal emphysema affects the distal portion of the acinus, often adjacent to pleural surfaces. It may be associated with the formation of bullae and an increased risk of spontaneous pneumothorax. Although less common, this subtype is clinically important in certain patient populations.
Risk Factors
Cigarette Smoking
Cigarette smoking is the primary risk factor for emphysema in developed countries. Long-term exposure to tobacco smoke triggers chronic inflammation within the lungs. Neutrophils and macrophages release proteolytic enzymes, including elastase, which degrade structural proteins in the alveolar walls.
Note: Not all smokers develop emphysema, suggesting genetic susceptibility and variability in inflammatory response.
Alpha-1 Antitrypsin Deficiency
Alpha-1 antitrypsin is a protease inhibitor that protects lung tissue from neutrophil elastase. In individuals with severe deficiency, elastase activity is unopposed, leading to accelerated destruction of alveolar walls.
Patients with alpha-1 antitrypsin deficiency often present with:
- Early-onset emphysema
- Minimal or no smoking history
- Basilar-predominant disease
Note: Respiratory therapists should be aware of this condition, particularly when evaluating younger patients with significant airflow obstruction.
Environmental and Occupational Exposures
Long-term exposure to airborne irritants, including dust, chemical fumes, and biomass fuels, can contribute to emphysema development. In some regions, indoor cooking with poorly ventilated biomass fuels represents a significant risk factor.
Clinical Presentation
Emphysema develops gradually. Symptoms often appear after substantial lung damage has occurred.
Dyspnea
Progressive shortness of breath is the most prominent symptom. Dyspnea initially occurs with exertion and gradually progresses to occur at rest in advanced disease. Patients may limit physical activity to avoid breathlessness, which can lead to deconditioning.
Cough and Sputum
In pure emphysema, cough and sputum production are typically minimal compared to chronic bronchitis. However, many patients have overlapping features of both conditions.
Physical Examination Findings
Common physical findings in advanced emphysema include:
- Increased anteroposterior chest diameter
- Flattened diaphragm
- Decreased breath sounds
- Hyperresonant percussion note
- Prolonged expiratory phase
- Use of accessory muscles
Note: Pursed-lip breathing is often observed. This breathing pattern helps maintain airway patency during expiration by increasing intraluminal pressure.
Emphysema vs. Chronic Bronchitis
Emphysema and chronic bronchitis are the two primary conditions classified under chronic obstructive pulmonary disease, but they differ in their underlying pathology and clinical features.
Emphysema is defined by permanent destruction of alveolar walls and enlargement of distal airspaces, leading to loss of elastic recoil, air trapping, and reduced gas exchange surface area. Patients typically present with progressive dyspnea, minimal sputum production, hyperinflation, and diminished breath sounds.
Chronic bronchitis, in contrast, is defined clinically by a productive cough lasting at least three months per year for two consecutive years. It is characterized by chronic airway inflammation, mucous gland enlargement, and excessive mucus production, which narrow the airways and increase resistance. Patients often have chronic cough, sputum production, wheezing, and may develop hypoxemia earlier. Although many patients exhibit overlapping features of both conditions, emphysema primarily involves alveolar destruction, while chronic bronchitis primarily affects the airways.
Diagnostic Evaluation
Spirometry
Spirometry confirms airflow obstruction. The characteristic finding is a reduced post-bronchodilator FEV1/FVC ratio below 0.70. Severity is further assessed by the percent predicted FEV1.
Lung Volumes
Lung volume measurements typically show:
- Increased residual volume
- Increased total lung capacity
- Evidence of hyperinflation
Note: These findings reflect air trapping and loss of elastic recoil.
Diffusing Capacity
The diffusing capacity for carbon monoxide is often reduced in emphysema due to loss of alveolar surface area and capillary bed. A reduced diffusing capacity helps differentiate emphysema from chronic bronchitis, where it may remain normal.
Imaging
Chest radiography in advanced emphysema may reveal:
- Hyperinflated lungs
- Flattened diaphragms
- Increased retrosternal airspace
- Narrow cardiac silhouette
Note: High-resolution computed tomography provides more detailed visualization of emphysematous changes and can identify bullae or regional patterns of destruction.
Management of Emphysema
Emphysema is a chronic and progressive condition that cannot be reversed once structural damage has occurred. Management focuses on relieving symptoms, improving functional capacity, preventing exacerbations, and slowing disease progression. Treatment plans are individualized based on symptom burden, physiologic impairment, comorbid conditions, and exacerbation history.
Respiratory therapists play an important role in both stable disease management and acute care interventions.
Smoking Cessation
Smoking cessation is the most effective intervention for slowing disease progression in patients with emphysema related to tobacco exposure. Continued smoking accelerates lung function decline and increases the risk of exacerbations, respiratory infections, and mortality.
Respiratory therapists frequently interact with patients during hospitalizations, pulmonary rehabilitation, and outpatient visits. These interactions provide opportunities to:
- Reinforce the link between smoking and symptoms
- Encourage quit attempts
- Refer patients to counseling and pharmacologic support
- Monitor for relapse and provide follow-up support
Note: Even in advanced emphysema, smoking cessation improves outcomes.
Pharmacologic Therapy
Medications used in emphysema are similar to those used in broader COPD management. They aim to reduce airway resistance, improve airflow, and decrease exacerbation frequency.
Bronchodilators
Bronchodilators are the primary pharmacologic treatment for symptomatic patients. Although emphysema is defined by structural destruction rather than airway inflammation alone, many patients exhibit some reversible component of airflow obstruction.
Therapies may include:
- Short-acting beta2-agonists for symptom relief
- Long-acting beta2-agonists for maintenance therapy
- Long-acting anticholinergics to reduce bronchomotor tone
- Combination inhaled regimens for persistent symptoms
Note: Respiratory therapists ensure correct inhaler technique, select appropriate delivery devices, and assess clinical response. Poor technique can significantly limit therapeutic benefit.
Inhaled Corticosteroids
Inhaled corticosteroids are not routinely indicated for all patients with emphysema. They are generally reserved for patients with frequent exacerbations or features suggesting steroid responsiveness.
Respiratory therapists monitor for:
- Reduction in exacerbation frequency
- Signs of oral candidiasis
- Increased risk of pneumonia in susceptible patients
Note: Appropriate patient selection is important to balance benefit and risk.
Pulmonary Rehabilitation
Pulmonary rehabilitation is one of the most effective nonpharmacologic interventions in emphysema. Although it does not improve lung function measurements, it significantly improves exercise tolerance, dyspnea perception, and quality of life.
Core components include:
- Structured exercise training
- Breathing retraining techniques
- Education on medication use
- Nutritional counseling
- Psychosocial support
Note: Respiratory therapists contribute by teaching breathing strategies such as pursed-lip breathing and diaphragmatic breathing. These techniques can reduce dynamic hyperinflation and improve ventilatory efficiency during exertion.
Oxygen Therapy
Long-term oxygen therapy is indicated in patients with severe resting hypoxemia. In appropriately selected patients, it can improve survival and reduce complications of chronic hypoxemia.
Indications typically include:
- Resting PaO2 less than 55 mmHg
- Resting oxygen saturation less than 88 percent
- Slightly higher thresholds in the presence of cor pulmonale or polycythemia
Note: Respiratory therapists perform oxygen assessments, titrate flow rates, and educate patients on safe oxygen use. They also reassess oxygen needs after acute exacerbations to determine whether long-term therapy remains necessary.
Advanced and Surgical Therapies
In selected patients with advanced emphysema, more aggressive interventions may be considered.
Lung Volume Reduction Surgery
Lung volume reduction surgery involves removal of diseased, nonfunctional lung tissue. This can reduce hyperinflation and improve the mechanical efficiency of the remaining lung.
Patients most likely to benefit typically have:
- Upper lobe–predominant emphysema
- Significant hyperinflation
- Poor exercise capacity despite rehabilitation
Note: Careful patient selection is critical because surgery carries substantial risk.
Bronchoscopic Lung Volume Reduction
Less invasive bronchoscopic techniques have been developed to achieve lung volume reduction without open surgery. These methods may involve placement of one-way endobronchial valves to collapse targeted areas of lung.
Benefits may include:
- Reduced hyperinflation
- Improved exercise tolerance
- Improved symptom control
Note: Respiratory therapists assist in pre- and post-procedure assessment, monitoring lung function and oxygenation.
Lung Transplantation
Lung transplantation may be considered in patients with end-stage emphysema who remain severely limited despite maximal therapy.
Evaluation generally includes:
- Severe airflow limitation
- Poor functional status
- Acceptable surgical risk
- Absence of significant contraindications
Note: Although transplantation can improve quality of life, it carries risks such as rejection, infection, and complications related to lifelong immunosuppression.
Acute Exacerbations of Emphysema
Patients with emphysema are vulnerable to acute exacerbations characterized by worsening dyspnea, increased sputum production, and increased cough. These events are often triggered by infection or environmental irritants.
Initial Management
Management strategies include:
- Supplemental oxygen titrated to appropriate targets
- Short-acting bronchodilators
- Systemic corticosteroids
- Antibiotics when bacterial infection is suspected
Note: Respiratory therapists monitor oxygenation, assess work of breathing, and evaluate response to bronchodilator therapy.
Noninvasive Ventilation
In patients who develop hypercapnic respiratory failure, noninvasive ventilation may be indicated. It can reduce the work of breathing, improve alveolar ventilation, and correct acidemia.
Therapist responsibilities include:
- Selecting appropriate interface
- Adjusting inspiratory and expiratory pressures
- Monitoring for air trapping and patient-ventilator synchrony
- Coaching the patient to improve tolerance
Note: A primary goal is improvement in pH and reduction in respiratory distress rather than immediate normalization of PaCO2.
Mechanical Ventilation
If noninvasive support fails, invasive mechanical ventilation may be required. Ventilator management must account for airflow limitation and risk of dynamic hyperinflation.
Key principles include:
- Allowing sufficient expiratory time
- Avoiding excessive respiratory rates
- Monitoring for intrinsic PEEP
- Minimizing barotrauma
Note: Respiratory therapists play a central role in monitoring ventilator waveforms, adjusting settings, and identifying complications.
Relevance to Respiratory Therapists
Emphysema directly affects lung mechanics, gas exchange, and ventilatory control. These are core elements of respiratory therapy practice.
Respiratory therapists contribute through:
- Performing and interpreting pulmonary function tests
- Delivering and evaluating bronchodilator therapy
- Titrating oxygen therapy safely
- Supporting noninvasive and invasive ventilation
- Educating patients on breathing techniques and device use
- Assisting in advanced therapy evaluation
Note: Because emphysema patients often move between outpatient, inpatient, and critical care settings, respiratory therapists provide continuity and physiologic expertise across the continuum of care.
Emphysema Practice Questions
1. What is emphysema?
Emphysema is a chronic lung disease characterized by permanent enlargement of airspaces distal to the terminal bronchioles, accompanied by destruction of alveolar walls without significant fibrosis.
2. What is the primary cause of emphysema?
Long-term cigarette smoking.
3. What genetic condition is strongly associated with early-onset emphysema?
Alpha-1 antitrypsin deficiency
4. What environmental exposures can contribute to emphysema?
Chronic exposure to tobacco smoke, air pollution, occupational dusts, and chemical irritants.
5. What are the two main anatomic types of emphysema?
Centrilobular (centriacinar) and panlobular (panacinar) emphysema.
6. Which type of emphysema is most commonly associated with cigarette smoking?
Centrilobular emphysema
7. Which type of emphysema is most commonly associated with alpha-1 antitrypsin deficiency?
Panlobular emphysema
8. Which lung regions are most commonly affected in centrilobular emphysema?
The upper lobes, particularly the respiratory bronchioles.
9. Which lung regions are typically involved in panlobular emphysema?
The lower lobes, with uniform involvement of the entire acinus.
10. What is the key pathophysiologic change in emphysema?
Destruction of alveolar walls leading to reduced surface area for gas exchange and loss of elastic recoil.
11. How does emphysema affect elastic recoil?
Elastic recoil is decreased due to destruction of elastin fibers.
12. What happens to lung compliance in emphysema?
Lung compliance increases.
13. What happens to total lung capacity (TLC) in emphysema?
Total lung capacity increases due to hyperinflation.
14. What happens to residual volume (RV) in emphysema?
Residual volume increases because of air trapping.
15. What pulmonary function test finding is characteristic of emphysema?
Reduced FEV1 and reduced FEV1/FVC ratio.
16. What is a bulla?
A large air-filled space within the lung parenchyma greater than 1 cm in diameter.
17. What is a bleb?
A small subpleural air collection within the visceral pleura.
18. What is bullous emphysema?
A form of emphysema characterized by large bullae that may compress adjacent lung tissue.
19. What physical exam finding is commonly seen in advanced emphysema?
Barrel chest due to increased anteroposterior diameter.
20. What breathing technique is commonly used by patients with emphysema to improve ventilation?
Pursed-lip breathing
21. Why do patients with emphysema use accessory muscles during breathing?
To compensate for airflow limitation and reduced elastic recoil.
22. What percussion finding is typical in emphysema?
Hyperresonance due to increased air trapping.
23. What happens to alveolar-capillary surface area in emphysema?
It is significantly reduced.
24. Is the alveolar damage in emphysema reversible?
No, it is permanent and irreversible.
25. How does emphysema impair gas exchange?
By decreasing alveolar surface area and disrupting the pulmonary capillary bed.
26. What are major risk factors for developing emphysema?
Cigarette smoking, alpha-1 antitrypsin deficiency, advancing age, secondhand smoke exposure, occupational dusts and fumes, and air pollution.
27. What physical characteristics are commonly associated with advanced emphysema?
Thin body habitus, barrel chest, pursed-lip breathing, hyperresonant percussion, diminished breath sounds, prolonged expiration, and use of accessory muscles.
28. Is asthma a common cause of emphysema?
No, asthma is not a typical cause of emphysema, though long-standing uncontrolled asthma may contribute to airway remodeling.
29. What is Hoover sign and what does it indicate in emphysema?
Hoover sign is the paradoxical inward movement of the lower lateral rib cage during inspiration, indicating severe hyperinflation.
30. Do all smokers develop emphysema?
No, only a subset of smokers develop emphysema, often due to genetic susceptibility and cumulative exposure.
31. How does emphysema typically progress?
It has a gradual, progressive onset over many years.
32. What complication may occur in later stages of emphysema?
Recurrent respiratory infections.
33. How is emphysema definitively diagnosed?
By spirometry showing airflow obstruction and imaging, particularly CT scan demonstrating alveolar destruction.
34. How should oxygen therapy be administered in patients with emphysema and chronic hypercapnia?
Titrated carefully to maintain SpO2 between 88% and 92%, rather than using a fixed low flow rate.
35. Is digital clubbing a typical finding in uncomplicated emphysema?
No, clubbing is uncommon in isolated emphysema and suggests another underlying condition.
36. What structural change occurs in alveoli in emphysema?
Alveoli become enlarged due to destruction of septal walls, leading to air trapping.
37. What exposure is most strongly linked to the development of emphysema?
Long-term tobacco smoke exposure.
38. What systemic effects may be seen in advanced emphysema?
Weight loss, muscle wasting, and decreased appetite due to increased work of breathing.
39. What breathing pattern is commonly observed in emphysema?
Prolonged expiration with pursed-lip breathing.
40. What term describes an increased anterior-posterior chest diameter?
Barrel chest
41. What dietary recommendation is often helpful for patients with severe emphysema?
Small, frequent meals to reduce dyspnea associated with eating.
42. Why is adequate hydration important in emphysema?
To help thin respiratory secretions and facilitate airway clearance.
43. Are patients with emphysema typically cyanotic in early disease?
No, many maintain near-normal oxygenation early and are historically described as “pink puffers.”
44. What factors influence life expectancy in emphysema?
Severity of airflow limitation, smoking status, exacerbation frequency, and presence of comorbidities.
45. At what age is emphysema most commonly diagnosed?
Typically after age 40, especially in individuals with a significant smoking history.
46. What is usually the earliest symptom of emphysema?
Progressive exertional dyspnea.
47. What nonpharmacologic therapy improves exercise tolerance in emphysema?
Pulmonary rehabilitation
48. How is hypoxemia managed in emphysema?
With carefully titrated supplemental oxygen therapy.
49. What surgical option may benefit selected patients with severe upper-lobe–predominant emphysema?
Lung volume reduction surgery (LVRS).
50. Can severe or recurrent lung infections worsen emphysema?
Yes, infections can accelerate lung damage and precipitate exacerbations.
51. What happens to diffusing capacity for carbon monoxide (DLCO) in emphysema?
DLCO is decreased due to destruction of the alveolar-capillary membrane and reduced surface area for gas exchange.
52. Why is DLCO typically more reduced in emphysema than in chronic bronchitis?
Because emphysema destroys alveolar walls and capillaries, whereas chronic bronchitis primarily affects the airways.
53. What is the protease–antiprotease imbalance theory of emphysema?
It states that excessive protease activity, such as elastase, overwhelms protective antiproteases, leading to alveolar destruction.
54. Which inflammatory cells are central to the development of emphysema?
Neutrophils and macrophages.
55. Which enzyme released by neutrophils contributes to alveolar wall destruction?
Neutrophil elastase
56. What happens to physiologic dead space in emphysema?
It increases due to loss of functional alveolar-capillary units.
57. How does emphysema affect the pulmonary capillary bed?
It reduces capillary density through destruction of alveolar septa.
58. What is dynamic hyperinflation?
Progressive air trapping during rapid breathing caused by incomplete exhalation.
59. How does hyperinflation impair diaphragmatic function?
It flattens and shortens the diaphragm, reducing its mechanical efficiency.
60. What arterial blood gas pattern may be seen in advanced emphysema?
Chronic respiratory acidosis with metabolic compensation and hypoxemia.
61. Why does hypercapnia usually develop late in emphysema?
Because substantial ventilatory impairment must occur before carbon dioxide retention becomes significant.
62. What is paraseptal emphysema commonly associated with?
An increased risk of spontaneous pneumothorax.
63. What imaging modality best evaluates the extent and distribution of emphysema?
High-resolution computed tomography (HRCT)
64. What chest radiograph finding is typical in advanced emphysema?
Flattened diaphragms with hyperinflated lungs.
65. Why does the cardiac silhouette often appear narrow in emphysema?
Hyperinflated lungs compress and vertically elongate the heart.
66. What is the primary therapeutic goal of bronchodilator therapy in emphysema?
To reduce airflow limitation and improve expiratory flow.
67. Are inhaled corticosteroids indicated for all patients with emphysema?
No, they are generally reserved for patients with frequent exacerbations or features of asthma overlap.
68. What resting PaO2 level commonly indicates eligibility for long-term oxygen therapy?
A PaO2 of 55 mmHg or less, or 59 mmHg or less with evidence of cor pulmonale or polycythemia.
69. What complication can result from large bullae in emphysema?
Compression of adjacent lung tissue or rupture leading to pneumothorax.
70. How is the expiratory phase of breathing altered in emphysema?
It becomes prolonged due to airflow obstruction and reduced elastic recoil.
71. How does pursed-lip breathing improve ventilation in emphysema?
It increases expiratory airway pressure, helping prevent premature airway collapse.
72. What ventilator strategy helps minimize air trapping in severe emphysema?
Prolonged expiratory time with reduced respiratory rate.
73. What is intrinsic positive end-expiratory pressure (auto-PEEP)?
Positive pressure remaining in the lungs at end expiration due to incomplete exhalation.
74. Why must respiratory rate be carefully adjusted in ventilated emphysema patients?
To ensure adequate expiratory time and prevent worsening hyperinflation.
75. What factors most strongly influence prognosis in emphysema?
Severity of airflow limitation, continued smoking, exacerbation frequency, comorbidities, and adherence to therapy.
76. What is the primary anatomic unit affected in emphysema?
The acinus, which includes the respiratory bronchioles, alveolar ducts, and alveoli.
77. Is significant fibrosis a defining feature of emphysema?
No, emphysema is characterized by alveolar destruction without substantial fibrosis.
78. How does emphysema impair expiratory airflow?
By reducing elastic recoil and promoting premature small airway collapse during exhalation.
79. What happens to FEV1 as emphysema progresses?
FEV1 progressively declines.
80. Why are small airways especially prone to collapse in emphysema?
They lack cartilage support and depend on elastic recoil to remain open.
81. How does emphysema contribute to ventilation–perfusion (V/Q) mismatch?
Capillary destruction creates ventilated but poorly perfused regions, increasing physiologic dead space.
82. What symptom most commonly limits physical activity in emphysema?
Exertional dyspnea
83. Why do many patients with advanced emphysema appear cachectic?
Increased work of breathing raises caloric expenditure, contributing to weight and muscle loss.
84. How is emphysema linked to cor pulmonale?
Chronic hypoxemia causes pulmonary hypertension, which may lead to right-sided heart failure.
85. What bedside finding may indicate severe hyperinflation?
Reduced diaphragmatic excursion on percussion or palpation.
86. How does emphysema affect inspiratory capacity?
Inspiratory capacity is reduced due to elevated end-expiratory lung volume.
87. Why does exertion worsen air trapping in emphysema?
Increased respiratory rate shortens expiratory time, limiting complete exhalation.
88. What is a primary goal of pulmonary rehabilitation in emphysema?
To improve exercise tolerance and reduce dyspnea despite fixed airflow limitation.
89. Why must oxygen therapy be carefully titrated in advanced emphysema?
To correct hypoxemia while minimizing the risk of worsening hypercapnia.
90. How does air trapping affect intrathoracic pressure?
It increases intrathoracic pressure, which can reduce venous return and cardiac output.
91. How does chronic hyperinflation alter chest wall mechanics?
It increases anteroposterior diameter and reduces overall respiratory efficiency.
92. What is an early physiologic abnormality seen in emphysema before severe hypoxemia develops?
Reduced diffusing capacity (DLCO).
93. Why are breath sounds often diminished in emphysema?
Hyperinflation decreases airflow turbulence and sound transmission.
94. What happens to the pulmonary vascular bed in advanced emphysema?
It is reduced due to destruction of alveolar capillaries.
95. How does alpha-1 antitrypsin normally protect lung tissue?
By inhibiting proteolytic enzymes such as neutrophil elastase.
96. Why is early identification of alpha-1 antitrypsin deficiency important?
Because augmentation therapy may slow emphysema progression in selected patients.
97. What nutritional complication is common in advanced emphysema?
Unintentional weight loss and muscle wasting.
98. What is subcutaneous emphysema?
Subcutaneous emphysema is the presence of air within the subcutaneous tissue, typically caused by air escaping from the respiratory or gastrointestinal tract into surrounding soft tissues.
99. What is the primary purpose of bronchodilator therapy during an emphysema exacerbation?
To reduce airflow limitation and improve expiratory flow.
100. What long-term outcome is most significantly improved by smoking cessation in emphysema?
Slowing the decline in lung function.
Final Thoughts
Emphysema is a chronic lung disease defined by permanent destruction of alveolar walls and loss of elastic recoil, leading to airflow limitation, hyperinflation, and impaired gas exchange. Although structural damage cannot be reversed, early identification, risk factor modification, and appropriate therapy can significantly improve symptoms and functional capacity.
Respiratory therapists are central to emphysema management through assessment, ventilatory support, oxygen titration, and patient education.
By combining physiologic understanding with practical bedside interventions, RTs help reduce exacerbations, improve quality of life, and support safe long-term care.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Faarc, Kacmarek Robert PhD Rrt, et al. Egan’s Fundamentals of Respiratory Care. 12th ed., Mosby, 2020.
- Rrt, Des Terry Jardins MEd, and Burton George Md Facp Fccp Faarc. Clinical Manifestations and Assessment of Respiratory Disease. 8th ed., Mosby, 2019.
- Pahal P, Avula A, Sharma S. Emphysema. [Updated 2023 Jan 26]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023.