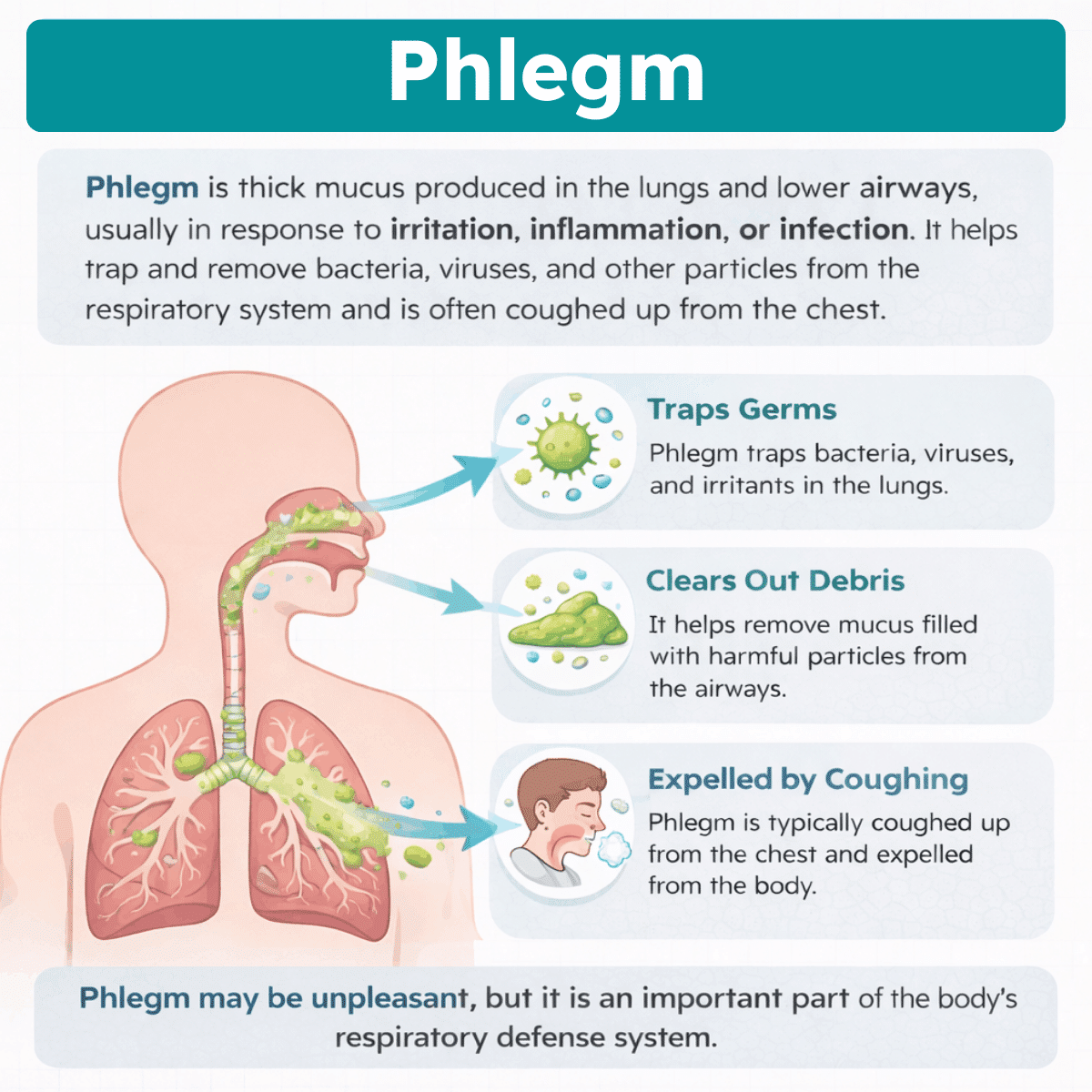
Phlegm is something most people become aware of when they have a cold, cough, or respiratory infection. It is the thick, sticky substance that can build up in the throat or chest and is often coughed up during illness.
While it may seem unpleasant, phlegm actually serves an important purpose in protecting the lungs and airways. It helps trap bacteria, viruses, dust, and other harmful particles so they can be removed from the body.
Understanding what phlegm is, why the body produces it, and what changes in phlegm may mean can help people better recognize normal respiratory responses and potential health concerns.
Download our free guide that has over 100+ of the best tips for healthy lungs.
What Is Phlegm?
Phlegm is a thick type of mucus produced in the lower respiratory tract, particularly in the lungs and bronchial tubes. It is part of the body’s natural defense system and helps protect the airways from harmful substances.
While the terms mucus and phlegm are sometimes used interchangeably, they are not exactly the same. Mucus is a general term for the slippery fluid produced by mucous membranes throughout the body, including the nose, throat, lungs, and digestive tract. Phlegm specifically refers to mucus that originates in the lungs and lower airways.
Phlegm tends to be thicker and more noticeable than normal mucus. It may accumulate in the chest and throat, especially when the body is fighting an infection or responding to irritation.
When phlegm builds up, the body often triggers coughing as a way to clear the airways. This process helps remove trapped particles and microorganisms, allowing the lungs to function more effectively.
Where Does Phlegm Come From?
Phlegm is produced by specialized cells located in the lining of the lower respiratory tract. These cells include goblet cells and mucus-producing glands found in the bronchial tubes. Under normal conditions, small amounts of mucus are constantly produced in the lungs. Most of this mucus moves upward through the airways and is swallowed without a person even noticing.
However, when the airways become irritated or infected, the body may produce larger amounts of thicker mucus, which is then referred to as phlegm. Several structures in the respiratory system play a role in the production and movement of phlegm.
Bronchial Tubes
The bronchial tubes are the main air passages that carry air from the trachea into the lungs. The lining of these tubes contains mucus-producing cells that create a protective layer along the airway walls.
This layer helps trap dust, bacteria, viruses, and other particles that enter the lungs during breathing.
Goblet Cells
Goblet cells are specialized cells that produce mucus. They are found throughout the respiratory tract and release mucus onto the surface of the airways.
When the airways are irritated or inflamed, goblet cells may produce increased amounts of mucus, contributing to the formation of phlegm.
Cilia
Cilia are tiny hair-like structures that line the respiratory tract. They beat in coordinated waves to move mucus and phlegm upward toward the throat.
This movement is part of the body’s natural cleaning system for the lungs. Once the phlegm reaches the throat, it can be swallowed or coughed out.
What Is Phlegm Made Of?
Phlegm is primarily composed of water, but it also contains several other important substances that help protect the respiratory system.
Some of the key components include:
- Water
- Mucins (gel-forming proteins)
- Antibodies
- Enzymes
- Dead cells
- White blood cells
- Trapped bacteria and viruses
- Dust and other particles
Mucins give phlegm its thick, sticky consistency. This allows it to trap microorganisms and debris effectively. White blood cells and antibodies within phlegm help fight infections by attacking harmful microorganisms that become trapped in the mucus.
Note: Because phlegm contains immune cells and trapped pathogens, its appearance can sometimes change depending on what the body is fighting.
What Does Phlegm Do?
Although it may seem unpleasant, phlegm plays several important roles in maintaining healthy lungs.
Protects the Airways
Phlegm forms a protective barrier that lines the respiratory tract. This barrier helps prevent harmful particles from reaching delicate lung tissue. By trapping dust, pollutants, bacteria, and viruses, phlegm helps reduce the risk of infection and irritation.
Helps Remove Harmful Substances
When harmful particles become trapped in phlegm, the body removes them through coughing or swallowing. Coughing is a reflex that helps expel excess phlegm from the airways. This clearing process helps keep the lungs open and functioning properly.
Supports the Immune System
Phlegm contains immune system components such as antibodies and antimicrobial proteins. These substances help neutralize or destroy pathogens that enter the respiratory tract. This makes phlegm an important part of the body’s first line of defense against respiratory infections.
Keeps Airways Moist
Phlegm also helps keep the airways moist and lubricated. This prevents the delicate tissues of the respiratory tract from becoming dry or irritated. Maintaining proper moisture levels helps ensure that breathing remains comfortable and efficient.
Why Does the Body Produce More Phlegm?
The body increases phlegm production when it needs extra protection or when the airways become irritated. In most cases, increased phlegm production is a sign that the body is responding to infection, inflammation, or environmental irritants.
Respiratory Infections
Colds, influenza, bronchitis, and pneumonia often cause increased phlegm production. During infection, the body produces more mucus in an attempt to trap and remove viruses or bacteria from the respiratory tract.
As the immune system fights the infection, the amount of phlegm may increase temporarily before gradually returning to normal.
Irritants in the Air
Exposure to smoke, air pollution, dust, or chemical fumes can irritate the lungs and trigger the production of extra phlegm. This response helps protect the airways by trapping harmful substances before they can cause further damage.
Allergies
Allergic reactions can also lead to increased mucus production. When the immune system reacts to allergens such as pollen or pet dander, inflammation occurs in the respiratory tract. This inflammation stimulates mucus-producing cells and can contribute to the buildup of phlegm.
Chronic Lung Conditions
Certain long-term respiratory diseases are associated with persistent phlegm production.
Examples include:
- Chronic bronchitis
- Chronic obstructive pulmonary disease (COPD)
- Asthma
- Bronchiectasis
- Cystic fibrosis
Note: In these conditions, inflammation and airway damage may cause excessive mucus production and difficulty clearing phlegm from the lungs.
How Phlegm Moves Through the Airways
The body has an efficient system for clearing mucus and phlegm from the lungs. This process relies on the combined action of mucus and cilia. Cilia beat rhythmically to push mucus and trapped particles upward toward the throat. This movement is sometimes referred to as the mucociliary clearance system.
Once the phlegm reaches the throat, it can either be swallowed or expelled through coughing. When this system works properly, the lungs remain clean and clear of debris.
However, certain factors can interfere with this natural cleaning process, including:
- Smoking
- Severe infections
- Chronic lung diseases
- Exposure to pollutants
Note: When phlegm cannot be cleared effectively, it may accumulate in the airways and contribute to symptoms such as coughing, chest congestion, and difficulty breathing.
Phlegm Colors and What They May Mean
The color, thickness, and amount of phlegm can sometimes provide helpful clues about what is happening in the respiratory system. However, phlegm color alone cannot confirm a diagnosis. A change in phlegm may be caused by something minor, such as a cold, or something more serious, such as a lung infection or chronic respiratory condition.
Looking at phlegm as one piece of the overall picture can be useful, especially when combined with other symptoms like fever, cough, shortness of breath, chest pain, or fatigue.

Clear Phlegm
Clear phlegm is usually considered normal or relatively mild. It may appear when the body is producing extra mucus in response to irritation, allergies, or the early stages of a viral infection.
Common causes of clear phlegm include:
- Allergies
- Mild viral illnesses
- Exposure to smoke or air pollution
- Asthma in some cases
Note: Even though clear phlegm is often less concerning than other colors, large amounts of it can still indicate inflammation or irritation in the airways.
White or Gray Phlegm
White or gray phlegm may suggest congestion, inflammation, or irritation in the airways. As mucus thickens and moves more slowly, it may lose its transparent appearance and become cloudy or white.
This type of phlegm is often seen with:
- Colds
- Mild bronchitis
- Sinus drainage that irritates the throat
- Dehydration
Note: Gray phlegm can sometimes occur in people exposed to smoke, dust, or pollution.
Yellow Phlegm
Yellow phlegm often appears when the immune system is actively responding to an infection. The yellow color typically comes from white blood cells that have moved into the mucus to fight off pathogens.
Yellow phlegm may be seen with:
- The common cold
- Bronchitis
- Sinus infections
- Viral respiratory illnesses
Note: Many people assume yellow phlegm means a bacterial infection, but that is not always true. Viral infections can also produce yellow phlegm.
Green Phlegm
Green phlegm often develops when a respiratory infection becomes more established. The green color usually comes from enzymes released by white blood cells during the immune response.
Green phlegm can occur with:
- Bronchitis
- Pneumonia
- Sinus infections
- More intense upper or lower respiratory infections
Note: Although green phlegm may look alarming, it does not automatically mean antibiotics are necessary. The decision to use antibiotics depends on the cause of the illness, the duration of symptoms, and the overall clinical picture.
Brown Phlegm
Brown phlegm may result from old blood, smoke exposure, or inhaled dirt and debris. It can also occur in people who smoke regularly or who have been exposed to heavy air pollution.
Possible causes include:
- Smoking
- Inhaling dust or dirt
- Irritated airways
- Previous bleeding in the airways
Note: Brown phlegm should be taken more seriously if it is persistent, worsening, or accompanied by other concerning symptoms.
Pink or Red Phlegm
Pink or red phlegm suggests that blood is present. Sometimes this happens because intense coughing irritates and breaks tiny blood vessels in the throat or airways.
Possible causes include:
- Severe coughing
- Airway irritation
- Nosebleeds draining into the throat
- Lung infections
- More serious respiratory or cardiovascular problems
Note: Small streaks of blood may not always signal an emergency, but repeated or significant blood in phlegm should be evaluated by a healthcare professional.
Frothy Phlegm
Frothy phlegm may sometimes be associated with fluid in the lungs, especially if it is pink and bubbly. This is more concerning and can sometimes occur with serious heart or lung problems.
This type of phlegm may be associated with:
- Pulmonary edema
- Heart failure
- Severe lung irritation
Note: Frothy pink phlegm should be treated as a warning sign that needs prompt medical attention.
Thick vs. Thin Phlegm
In addition to color, the consistency of phlegm can also matter.
Thin Phlegm
Thin phlegm is often easier to clear and may occur with mild irritation, early infection, or normal mucus production that has increased slightly. Although thin phlegm may be bothersome, it usually does not block the airways as much as thicker secretions.
Thick Phlegm
Thick phlegm can feel heavy, sticky, and difficult to cough up. It may collect in the chest or throat and cause discomfort, noisy breathing, or the sensation that something is stuck.
Thick phlegm is more likely to occur with:
- Dehydration
- Respiratory infections
- Chronic bronchitis
- Cystic fibrosis
- Bronchiectasis
- Dry indoor air
Note: When phlegm becomes very thick, the body may have a harder time clearing it, which can make coughing more frequent and uncomfortable.
Common Conditions That Cause Phlegm
Many different illnesses and conditions can lead to phlegm production. In some cases, phlegm is temporary and goes away as the person recovers. In other cases, it may be a recurring or long-term symptom.
The Common Cold
A cold is one of the most frequent causes of phlegm. At first, symptoms may involve a runny nose and clear mucus, but as the illness progresses, mucus may thicken and drain into the throat or chest.
This can lead to:
- Throat clearing
- Mild coughing
- Chest congestion
- Postnasal drip
Note: In most cases, cold-related phlegm improves on its own within several days to a couple of weeks.
Bronchitis
Bronchitis occurs when the bronchial tubes become inflamed. This often leads to coughing and increased phlegm production.
Acute bronchitis commonly develops after a viral infection and may cause:
- Persistent cough
- Yellow or green phlegm
- Chest discomfort
- Mild shortness of breath
Note: Chronic bronchitis is different. It is a long-term condition, usually linked to smoking or long-term airway irritation, and it often causes regular phlegm production over months or years.
Pneumonia
Pneumonia is an infection that affects the lungs and can lead to significant phlegm production. The phlegm may be yellow, green, rust-colored, or even blood-tinged.
Other symptoms may include:
- Fever
- Chills
- Shortness of breath
- Chest pain
- Fatigue
Note: Because pneumonia can become serious, especially in older adults, young children, and people with weakened immune systems, symptoms should not be ignored.
Asthma
Asthma is often associated with wheezing and shortness of breath, but some people with asthma also produce phlegm. Inflammation in the airways can increase mucus production, especially during flare-ups.
This may happen in response to:
- Allergens
- Cold air
- Exercise
- Respiratory infections
- Smoke or pollution
Note: In asthma, excess phlegm can contribute to airway narrowing and make breathing feel more difficult.
Chronic Obstructive Pulmonary Disease (COPD)
COPD is a long-term lung disease that often includes chronic bronchitis and emphysema. Many people with COPD produce phlegm regularly, especially in the morning.
Symptoms may include:
- Daily cough
- Ongoing phlegm production
- Shortness of breath
- Reduced exercise tolerance
Note: In COPD, excess phlegm can make it harder to breathe and may raise the risk of infections.
Bronchiectasis
Bronchiectasis is a condition in which the airways become damaged and widened, making it harder to clear mucus effectively. As a result, phlegm can build up and become a recurring problem.
People with bronchiectasis often have:
- Chronic productive cough
- Large amounts of phlegm
- Frequent chest infections
- Fatigue
- Shortness of breath
Note: This condition often requires ongoing treatment to help clear the airways and reduce infections.
Cystic Fibrosis
Cystic fibrosis is an inherited condition that causes mucus in the lungs and other organs to become unusually thick and sticky. This makes it difficult to clear phlegm and increases the risk of repeated lung infections.
Although cystic fibrosis is often diagnosed in childhood, its effects on phlegm production help illustrate how important normal mucus consistency is for healthy lung function.
Allergies and Postnasal Drip
Not all phlegm comes directly from the lungs. Sometimes mucus from the nose and sinuses drains down the back of the throat, creating a sensation that resembles phlegm.
This is common with:
- Seasonal allergies
- Sinus congestion
- Upper respiratory infections
Note: Postnasal drip can cause frequent throat clearing, coughing, and the feeling of mucus stuck in the throat.
When Phlegm Lasts Longer Than Expected
Temporary phlegm during a cold or mild respiratory illness is common. But when phlegm lasts for weeks or keeps coming back, it may point to a more persistent issue.
Long-lasting phlegm may be linked to:
- Smoking
- Chronic bronchitis
- Ongoing allergies
- Asthma
- COPD
- Bronchiectasis
- Recurrent infections
- Gastroesophageal reflux
Note: Persistent phlegm should be taken more seriously when it is accompanied by symptoms such as weight loss, shortness of breath, chest pain, fatigue, or repeated infections.
Why Some People Feel Phlegm in the Throat
People often describe having phlegm “in the throat,” even when the source may be the nose, sinuses, or lower airways. This sensation can happen for several reasons.
Common reasons include:
- Postnasal drip
- Frequent throat clearing
- Mucus moving up from the chest
- Dry or irritated throat tissues
- Acid reflux irritating the throat
Note: This sensation can be frustrating because even after swallowing or coughing, it may still feel like something is there. That is often because the tissue itself is irritated, not just because mucus is present.
How to Get Rid of Phlegm
When phlegm becomes excessive or difficult to clear, the goal is not to completely stop the body from making it. Phlegm serves an important purpose, and the body needs some mucus in the airways to stay protected. The real goal is to thin it out, loosen it, and make it easier to remove.
Stay Hydrated
Drinking enough fluids is one of the most effective ways to help manage phlegm. When the body is well hydrated, phlegm tends to stay thinner and easier to cough up.
Water is the best option, but other fluids can also help, such as:
- Warm tea
- Broth
- Warm water with lemon
- Clear soups
Note: When a person is dehydrated, phlegm can become thicker and stickier, making it harder for the body to clear the airways.
Use Warm Moist Air
Warm, moist air can help loosen phlegm and make breathing feel more comfortable. This is one reason many people feel temporary relief in a steamy shower. A humidifier may also help, especially when indoor air is very dry. Moisture in the air can reduce throat and airway irritation while making phlegm less thick.
However, humidifiers should be cleaned regularly. A dirty humidifier can spread mold or bacteria and worsen symptoms instead of helping.
Try Steam Carefully
Steam inhalation is a common home remedy for chest congestion and thick phlegm. Breathing in warm steam may help loosen secretions enough to make them easier to cough out.
Some people use:
- A warm shower
- Steam from a bowl of hot water
- A facial steamer
Note: Steam can offer temporary relief, but it should be used carefully. Hot water and steam can cause burns, especially in children.
Get Plenty of Rest
If phlegm is being caused by a cold, bronchitis, or another respiratory infection, rest gives the body a better chance to recover. Sleep and recovery support the immune system, which helps the body fight infection and reduce inflammation in the airways.
Trying to push through illness without adequate rest can make symptoms feel worse and recovery take longer.
Avoid Smoking and Irritants
Smoke is one of the most common triggers for ongoing phlegm production. Cigarette smoke irritates the airways, damages cilia, and causes the lungs to produce more mucus. Avoiding smoking, secondhand smoke, and other irritants can make a big difference.
Other irritants that can worsen phlegm include:
- Vaping aerosols
- Dust
- Air pollution
- Chemical fumes
- Strong perfumes
- Harsh cleaning products
Note: Reducing exposure to these triggers gives the airways a better chance to heal and clear secretions normally.
Try Gentle Activity
In some cases, gentle movement such as walking can help loosen phlegm in the chest. Lying still for long periods may allow secretions to settle, while light activity can sometimes make it easier to cough them up.
Of course, this depends on how sick a person feels. Someone with fever, weakness, or breathing problems should rest and avoid overexertion.
Home Remedies That May Help
Many people use home remedies to manage phlegm, especially when it is caused by a cold, mild infection, allergies, or throat irritation. These remedies may not cure the underlying cause, but they can help make symptoms more tolerable.
Warm Fluids
Warm drinks can be soothing and may help thin phlegm while easing throat irritation.
Helpful options include:
- Herbal tea
- Warm water with honey
- Broth
- Warm lemon water
Note: These drinks may be especially comforting when phlegm is causing coughing, throat clearing, or that heavy feeling in the chest.
Honey
Honey is commonly used to soothe the throat and reduce coughing. If phlegm is causing throat irritation or frequent coughing, honey may help coat the throat and provide temporary relief.
It is often added to tea or taken by the spoonful in small amounts. However, honey should never be given to infants under one year old.
Saline Nasal Sprays or Rinses
If phlegm is being worsened by postnasal drip, saline sprays or rinses may help. They can flush out mucus, allergens, and irritants from the nose and sinuses, reducing the amount of drainage that runs into the throat.
This may be especially helpful for people with:
- Allergies
- Sinus congestion
- Colds
- Dry nasal passages
Note: Because saline contains no medication, it is often a gentle option for regular use.
Ginger
Ginger is a popular home remedy for coughs and congestion. While it does not directly eliminate phlegm, some people find that it soothes the throat and provides a warming, comforting effect. Ginger tea is a common choice when someone has a cough with mucus.
Chicken Soup
Chicken soup remains a favorite home remedy for respiratory symptoms. It helps with hydration, and the warmth can make congestion and throat discomfort feel a little better. It may not directly remove phlegm, but it often helps people feel more comfortable while they recover.
Elevating the Head at Night
Sleeping with the head slightly raised may help reduce the sensation of phlegm collecting in the throat or chest, especially when postnasal drip or nighttime coughing is part of the problem. This simple change may make it easier to sleep and reduce coughing spells during the night.
Medical Treatments for Phlegm
Sometimes phlegm is stubborn, persistent, or linked to a condition that requires medical treatment. In these situations, over-the-counter or prescription options may be helpful.
Expectorants
Expectorants are medicines that help thin mucus so it can be coughed up more easily. They are commonly used when chest congestion makes phlegm feel stuck.
These medications may help during:
- Colds
- Bronchitis
- Mild chest congestion
Note: They do not stop phlegm production, but they may make it easier for the body to clear it.
Decongestants
If phlegm is related to a cold or sinus congestion, decongestants may help by reducing swelling in the nasal passages. This can improve airflow and reduce some of the drainage that contributes to throat irritation and coughing.
However, decongestants are not right for everyone. People with certain heart conditions, high blood pressure, or other medical concerns should use them cautiously and follow medical advice.
Antihistamines
When allergies are a major cause of mucus or postnasal drip, antihistamines may help reduce symptoms. They can be useful for:
- Sneezing
- Runny nose
- Allergy-related throat clearing
- Postnasal drip
Note: In some cases, antihistamines may make secretions drier and thicker, so they may not always feel helpful for chest phlegm.
Nasal Steroid Sprays
For ongoing allergy symptoms or chronic nasal inflammation, nasal steroid sprays can help reduce swelling and mucus production in the nose.
These are often more effective when used consistently rather than only once in a while.
Antibiotics
Antibiotics may be needed if phlegm is caused by a bacterial infection, but not all cases of phlegm require them. Many colds, bronchitis cases, and upper respiratory infections are caused by viruses, and antibiotics do not help viral illnesses.
This is why phlegm color alone should not be used to decide whether antibiotics are necessary.
Treatments for Chronic Lung Conditions
People with asthma, COPD, bronchiectasis, or cystic fibrosis may need more specialized care when phlegm becomes a long-term problem.
Treatment may include:
- Inhalers
- Nebulized medications
- Airway clearance techniques
- Chest physiotherapy
- Mucus-thinning medications
- Antibiotics for infections when needed
Note: In these cases, the goal is not only to deal with phlegm but also to treat the underlying disease that is causing it.
When Phlegm Can Be a Warning Sign
Phlegm is often harmless and temporary, especially during a cold or mild respiratory infection. Still, there are times when it may signal a more serious issue.
Warning signs include:
- Phlegm lasting more than a few weeks
- Increasing amounts of phlegm over time
- Blood in the phlegm
- Foul-smelling phlegm
- Phlegm with high fever
- Chest pain
- Shortness of breath
- Wheezing that is getting worse
- Unexplained weight loss
- Recurrent lung infections
These symptoms do not always mean something severe is happening, but they should not be ignored.
For example, long-term phlegm in a smoker may point to chronic bronchitis or COPD. Phlegm with fever and chest pain may suggest pneumonia. Blood-streaked phlegm may come from irritation, but repeated bleeding needs medical evaluation.
When to See a Doctor
A healthcare professional should be consulted if phlegm:
- Does not improve after a reasonable time
- Keeps coming back
- Interferes with sleep or daily life
- Is accompanied by repeated cough or infections
- Contains blood
- Is associated with shortness of breath or chest tightness
- Develops along with fever that does not improve
Medical attention is especially important for:
- Infants and young children
- Older adults
- People with weakened immune systems
- People with asthma, COPD, or other lung diseases
Note: Emergency care may be needed if a person has severe trouble breathing, chest pain, confusion, or coughs up a large amount of blood.
Common Myths About Phlegm
There are many misconceptions about phlegm. Understanding what is true and what is not can help people respond more appropriately to symptoms.
Myth: Phlegm Is Always a Sign of Infection
Not always. Phlegm can be caused by allergies, smoke, pollution, asthma, chronic lung disease, postnasal drip, and other forms of irritation.
Myth: Green Phlegm Always Means Antibiotics Are Needed
Green phlegm can happen during viral or bacterial infections. Color alone does not prove that antibiotics are necessary.
Myth: All Phlegm Comes From the Lungs
Sometimes the feeling of phlegm actually comes from mucus draining down from the nose and sinuses. Postnasal drip can closely mimic phlegm from the chest.
Myth: Coughing Up Phlegm Is Always Bad
Coughing up phlegm can actually be helpful. It is one of the body’s ways of clearing the airways and removing irritants or infection-related secretions.
Myth: The Goal Is to Get Rid of All Phlegm
The body needs mucus and phlegm to protect the airways. The goal is not to eliminate it completely but to keep it at a healthy level and make sure it can be cleared properly.
How to Support Healthy Airways
Good daily habits can help reduce unnecessary phlegm and support normal airway function.
Helpful habits include:
- Drinking enough water
- Avoiding smoking and secondhand smoke
- Managing allergies
- Reducing exposure to dust and pollutants
- Washing hands often to reduce infections
- Staying up to date with recommended medical care
- Following treatment plans for chronic respiratory conditions
Note: These simple steps can make a meaningful difference in how well the lungs and airways clear mucus.
FAQs About Phlegm
What Is the Fastest Way to Get Rid of Phlegm?
The fastest way to get rid of phlegm is usually by thinning it so the body can clear it more easily. Drinking plenty of water helps loosen thick mucus in the lungs. Warm fluids such as tea, broth, or lemon water may also help break up phlegm.
Using a humidifier or inhaling steam can add moisture to the airways and loosen secretions. Gentle coughing can help remove phlegm from the chest. In some cases, over-the-counter expectorant medications may also help thin mucus and promote clearance.
Should You Spit Out Phlegm?
Spitting out phlegm can help clear the airways when mucus builds up in the chest or throat. When phlegm contains trapped bacteria, viruses, or debris, coughing it up and spitting it out helps remove those substances from the respiratory system.
However, swallowing phlegm is generally harmless because stomach acid breaks down the material and any microorganisms it contains. Whether you spit it out or swallow it often depends on comfort. The important thing is allowing the body to clear excess secretions from the lungs.
Is Phlegm Good or Bad for You?
Phlegm can be both helpful and uncomfortable. It plays an important role in protecting the lungs by trapping dust, bacteria, viruses, and other harmful particles that enter the airways. When the body produces phlegm, it is often responding to irritation or infection and trying to remove these substances.
However, excessive phlegm can cause coughing, chest congestion, and breathing discomfort. In most cases, phlegm is a normal defense mechanism. Problems usually occur only when too much builds up or when it persists for a long time.
Why Do I Have Phlegm in My Throat?
Phlegm in the throat often occurs when mucus from the lungs or sinuses accumulates and moves upward toward the throat. This can happen during respiratory infections such as colds, bronchitis, or sinus infections. Allergies, air pollution, smoking, and asthma can also increase mucus production and cause phlegm to collect in the throat.
Postnasal drip is another common cause, where mucus drains from the sinuses down the back of the throat. This buildup can create the sensation of needing to cough or clear the throat frequently.
What Medicine Is Good for Phlegm?
Several types of medications may help manage phlegm depending on the underlying cause. Expectorants are commonly used to thin mucus and make it easier to cough up. Mucolytic medications can also help break down thick mucus in the airways.
If phlegm is related to asthma or COPD, bronchodilators may help open the airways and improve mucus clearance. In cases of bacterial infection, a doctor may prescribe antibiotics.
Note: Choosing the right treatment depends on the cause of phlegm and should sometimes involve medical advice.
Do Healthy People Have Phlegm?
Healthy people can produce small amounts of phlegm, although they may not notice it. The respiratory system constantly produces mucus to trap dust, bacteria, and other particles that enter the airways during breathing. This mucus usually moves upward through the airways and is swallowed without being noticed.
Phlegm becomes more noticeable when the body produces extra mucus due to irritation, allergies, infection, or environmental pollutants. Occasional phlegm can be normal, but persistent or excessive phlegm may indicate a respiratory problem.
Will Phlegm Go Away on Its Own?
In many cases, phlegm goes away on its own once the underlying cause improves. Respiratory infections such as the common cold or mild bronchitis often cause temporary phlegm that gradually decreases as the body recovers.
Staying hydrated, resting, and avoiding irritants like smoke can help the body clear mucus more effectively. However, if phlegm lasts for several weeks, becomes unusually thick, or is accompanied by symptoms such as fever, chest pain, or shortness of breath, medical evaluation may be necessary.
Is Phlegm and Mucus the Same Thing?
Phlegm and mucus are closely related but not exactly the same. Mucus is the general term for the slippery substance produced by mucous membranes throughout the body, including the nose, throat, lungs, and digestive system. Phlegm specifically refers to thick mucus produced in the lungs and lower airways, usually during irritation or infection.
Because phlegm originates in the respiratory tract, it may be coughed up from the chest. While people often use the terms interchangeably, phlegm is technically a type of mucus.
When Should I Be Worried About Phlegm Color?
Changes in phlegm color can sometimes indicate infection or other respiratory problems. Clear or white phlegm is often normal or associated with mild irritation. Yellow or green phlegm may appear when the immune system is fighting infection.
However, certain colors may require medical attention. Red or pink phlegm may indicate blood in the airways, while brown or foul-smelling phlegm could signal infection or irritation.
Note: You should seek medical care if unusual phlegm colors persist or occur with symptoms like fever, chest pain, or breathing difficulty.
Final Thoughts
Phlegm may be unpleasant, but it is an important part of the body’s respiratory defense system. It helps trap harmful particles, supports the immune system, and keeps the airways moist. In many cases, phlegm is temporary and appears as part of a normal response to a cold, infection, allergy, or irritation.
However, when phlegm becomes persistent, unusually thick, blood-tinged, or associated with symptoms like shortness of breath or fever, it may point to a more serious problem.
By understanding what phlegm is, what different colors and textures may suggest, and how to manage it safely, people can better tell when it is just a nuisance and when it deserves medical attention.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Shen F, Zubair M, Sergi C. Sputum Analysis. [Updated 2025 May 4]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026.