A pulmonary embolism (PE) is a serious and often sudden condition that can rapidly compromise both respiratory and cardiovascular function. Because its presentation may be subtle at first yet escalate quickly, early recognition is critical.
In respiratory care, a pulmonary embolism is especially important due to its direct effects on pulmonary circulation, gas exchange, and oxygen delivery. Respiratory therapists are frequently at the bedside when changes in breathing, oxygenation, or hemodynamics occur.
A clear understanding of this pathology equips clinicians to identify warning signs early, support timely diagnosis, and deliver appropriate respiratory interventions that can be life-saving.
What Is a Pulmonary Embolism?
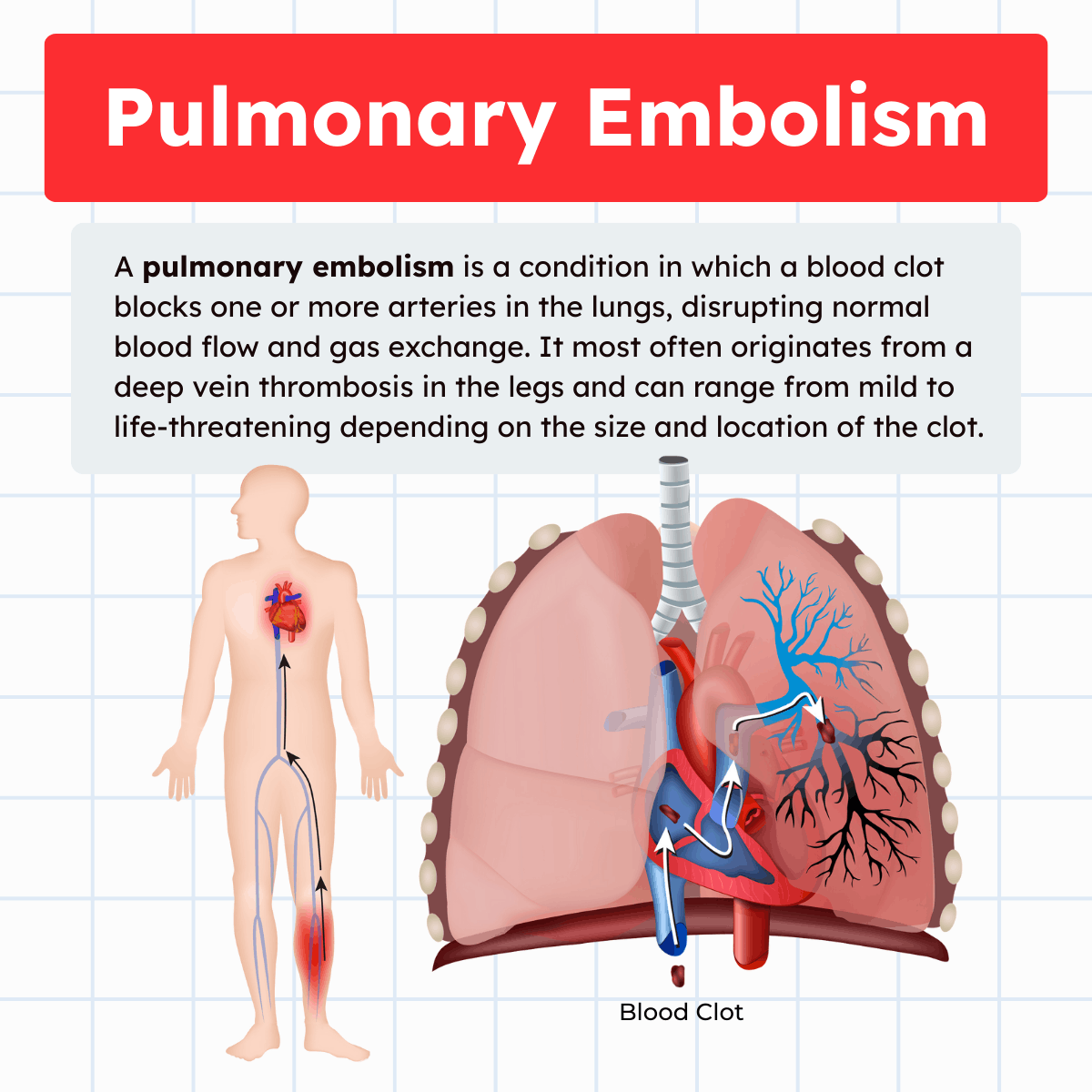
A pulmonary embolism occurs when a blood clot obstructs one or more pulmonary arteries, impairing blood flow through the lungs. In most cases, the clot originates as a deep vein thrombosis (DVT) in the lower extremities or pelvis and travels through the venous system to the lungs. Once lodged in the pulmonary vasculature, the clot increases pulmonary vascular resistance and disrupts normal gas exchange.
The severity of a PE varies widely. Small emboli may cause minimal symptoms, while large or multiple clots can result in acute right heart failure, severe hypoxemia, and sudden death. The clinical impact depends on clot size, location, the number of vessels involved, and the patient’s underlying cardiopulmonary reserve.
Why a Pulmonary Embolism Is So Dangerous
A pulmonary embolism is dangerous because it affects both circulation and respiration simultaneously. Blood flow is diverted away from ventilated alveoli, creating areas of increased dead space where ventilation is present but perfusion is absent. This ventilation–perfusion mismatch leads to impaired oxygenation and inefficient carbon dioxide elimination.
In severe cases, obstruction of pulmonary blood flow causes a sudden increase in pulmonary artery pressure. The right ventricle, which is not designed to pump against high resistance, may fail acutely. This leads to decreased cardiac output, systemic hypotension, and shock. Without rapid intervention, the condition can quickly become fatal.
Relevance to Respiratory Therapists
A pulmonary embolism is highly relevant to respiratory therapists because it directly affects oxygenation, ventilation, and hemodynamics. Respiratory therapists are often responsible for monitoring oxygen saturation, evaluating arterial blood gases, managing oxygen therapy, assisting with diagnostic testing, and supporting patients with ventilatory failure.
RTs are also frequently involved in the care of high-risk populations, including postoperative patients, immobilized patients, those with chronic cardiopulmonary disease, and critically ill individuals. Recognizing subtle changes in respiratory status and understanding how a PE alters pulmonary physiology allows respiratory therapists to play a key role in early detection and management.
Risk Factors and Predisposing Conditions
A pulmonary embolism is closely linked to venous thromboembolism. Common risk factors include prolonged immobility, recent surgery, trauma, malignancy, pregnancy, obesity, smoking, and the use of estrogen-containing medications. Hospitalized patients are particularly vulnerable due to reduced mobility and systemic inflammation.
A prior history of DVT or PE significantly increases the risk of recurrence. Genetic clotting disorders and chronic inflammatory conditions also raise the likelihood of thrombus formation. Understanding these risk factors helps respiratory therapists maintain a high index of suspicion when evaluating sudden respiratory changes.
Clinical Presentation and Symptoms
The presentation of a pulmonary embolism can range from mild to catastrophic, but symptoms often develop suddenly. Dyspnea is the most common complaint and may occur at rest or with minimal exertion. Chest pain, especially pleuritic in nature, is frequently reported and may worsen with deep breathing.
Other signs include tachypnea, tachycardia, diaphoresis, hemoptysis, and anxiety. Hypotension, cyanosis, syncope, and arrhythmias suggest a massive or high-risk PE. Respiratory therapists should be particularly alert when a patient suddenly develops unexplained shortness of breath, hypoxemia, or respiratory distress.
Hemodynamic Effects of a Pulmonary Embolism
A pulmonary embolism causes characteristic hemodynamic changes. Obstruction of pulmonary blood flow increases pulmonary artery pressure and central venous pressure while reducing cardiac output. As right ventricular strain worsens, left ventricular filling may decrease, further compromising systemic perfusion.
These changes explain why patients with a severe PE may present with hypotension, shock, or signs of right-sided heart failure. Monitoring trends in heart rate, blood pressure, oxygenation, and clinical status is essential for identifying deterioration early.
Effects on Gas Exchange and ABG Findings
From a respiratory standpoint, a pulmonary embolism is strongly associated with hypoxemia. Increased dead space ventilation leads to inefficient gas exchange, even when minute ventilation is elevated. Patients often hyperventilate in response to hypoxemia, resulting in respiratory alkalosis on arterial blood gas analysis.
Typical ABG findings include decreased PaO₂, decreased PaCO₂, and an elevated pH. However, normal ABG values do not rule out PE, particularly in early or smaller emboli. Respiratory therapists must interpret ABGs in the context of clinical presentation and overall risk.
Diagnostic Evaluation
Several diagnostic tools are used to evaluate a suspected pulmonary embolism. CT pulmonary angiography is the most commonly used imaging modality and can directly visualize clots in the pulmonary arteries. Pulmonary angiography remains the gold standard but is less frequently performed due to its invasive nature.
A ventilation–perfusion (V/Q) scan is useful when CT is contraindicated. A classic finding is normal ventilation with absent perfusion in affected lung regions. Chest X-rays are often obtained to rule out other causes of symptoms, though they may appear normal in PE.
Laboratory testing often includes a D-dimer assay, which can help rule out PE in low-risk patients. Capnography may show decreased end-tidal CO₂ due to increased dead space, providing additional bedside clues for respiratory therapists.
Treatment and Management
The primary goal of treatment is to prevent clot extension, reduce recurrence, and restore adequate cardiopulmonary function. Anticoagulation therapy is the cornerstone of management and is typically initiated as soon as a pulmonary embolism is suspected, unless contraindicated. Common agents include heparin, low-molecular-weight heparin, warfarin, and newer oral anticoagulants.
In severe or life-threatening cases, thrombolytic therapy may be used to rapidly dissolve the clot. Patients with hemodynamic instability may require positive inotropic agents to support cardiac output.
Respiratory support is often necessary. Oxygen therapy is used to correct hypoxemia, and in cases of respiratory failure, intubation and mechanical ventilation may be required. Respiratory therapists play a critical role in selecting appropriate oxygen delivery devices, managing ventilator settings, and monitoring patient response.
Prevention and Prophylaxis
Preventing a pulmonary embolism is a major focus in hospitalized patients. Pharmacologic prophylaxis with anticoagulants significantly reduces the risk of venous thromboembolism. Mechanical measures such as early ambulation and pneumatic compression devices are also effective.
Compression stockings are commonly recommended to reduce venous stasis in at-risk patients. Respiratory therapists contribute by encouraging mobility when appropriate and recognizing early signs of a DVT or PE during routine patient care.
Clinical Insight for Respiratory Therapists
One of the most important clinical clues for pulmonary embolism is sudden onset. When a patient suddenly develops dyspnea, chest pain, tachycardia, or hypoxemia without an obvious cause, a PE must be considered. This is especially true in postoperative or immobilized patients.
Respiratory therapists are uniquely positioned to notice abrupt changes in breathing patterns, oxygen requirements, and gas exchange. Prompt communication of concerns to the healthcare team can lead to earlier diagnosis and life-saving treatment.
Pulmonary Embolism Practice Questions
1. What is a pulmonary embolism characterized by?
A pulmonary embolism is characterized by the blockage of one or more arteries in the lungs by a blood clot, which usually originates from a deep vein thrombosis (DVT) in the legs or pelvis.
2. What does PE stand for?
Pulmonary embolism
3. What are the most common emboli?
Thrombi from the femoral veins.
4. Apart from thrombi, what else can embolize into the pulmonary arteries?
Tumors, fat from bone fractures, amniotic fluid, and foreign materials.
5. What factors can cause alterations in blood flow, increasing the risk of deep vein thrombosis?
Immobilization (e.g., surgery, injury, or pregnancy), obesity, and cancer.
6. What factors can increase the coagulability of the blood?
Genetic thrombophilia, antiphospholipid syndrome, nephrotic syndrome, and cancer.
7. What is the name of the score for predicting PE?
Geneva score
8. What happens in the lung after a PE blocks the pulmonary artery?
Lung tissue is ventilated but not perfused, and the non-perfused area stops producing surfactant, so its alveoli collapse, exacerbating hypoxia.
9. What can happen to the heart during a pulmonary embolism?
It can undergo ischemia and systemic hypoxia, and reduced accessible pulmonary circulation causes an increase in pulmonary artery pressure and, thus, reduced cardiac output.
10. What is the difference between a small or medium PE and a massive PE?
Small or medium PEs affect a terminal pulmonary vessel, while a massive PE affects a large pulmonary vessel, even the pulmonary artery itself.
11. What are the symptoms of a small or medium PE?
Dyspnea, tachypnea, pleuritic chest pain, cough, and hemoptysis.
12. What are the symptoms of a massive PE?
Severe central chest pain, shock, paleness and sweating, cyanosis, collapse, circulatory instability, and sudden death.
13. How can a pulmonary embolism be investigated?
Chest x-ray, ECG, blood tests, and ABG.
14. How is a pulmonary embolism managed?
High-flow oxygen, analgesia, IV fluids, and fibrinolytic therapy with IV streptokinase.
15. How can a pulmonary embolism be prevented in at-risk patients?
Prevention of pulmonary embolism in at-risk patients typically involves using anticoagulants to inhibit clot formation and employing compression stockings to promote circulation, especially when immobilized, alongside lifestyle changes like regular exercise and hydration.
16. What are the causes of a pulmonary embolism?
Dehydration, venous stasis from prolonged immobility or surgery, birth control pills, clotting disorders, and heart arrhythmias (e.g., AFib).
17. Where do 95% of pulmonary emboli come from?
Veins in legs (i.e., DVT)
18. What is a D-dimer test?
A D-dimer test is a blood test that measures the presence of fibrin degradation products, which are typically found in the blood after a blood clot is broken down by the body.
19. What does an increased D-dimer mean?
Elevated D-dimer levels can indicate recent or ongoing blood clot formation and breakdown in the body, and the test is often used to rule out conditions like pulmonary embolism or deep vein thrombosis. However, a high D-dimer level is not specific to these conditions and can be elevated in other situations such as inflammation, pregnancy, or recent surgery.
20. What is a VQ scan?
A VQ scan, or ventilation-perfusion scan, is a medical imaging test that uses a radioactive material to examine airflow (ventilation) and blood flow (perfusion) in the lungs.
21. What does a VQ scan look at?
It looks at the blood flow to the lungs.
22. When may a CT or CT angiography be needed to diagnose a pulmonary embolism?
If inconclusive VQ scan or D-dimer cannot be used.
23. Why does pulse rate increase during a pulmonary embolism?
Hypoxia
24. What promotes clotting in the veins?
Virchow’s triad: stasis, hypercoagulability, and venous injury.
25. Why does a pulmonary embolism lead to hypoxemia?
Blood that cannot get to the alveoli due to an occlusion must go somewhere else; this increases the perfusion in the new area and makes a low VQ mismatch, which is shunting that lowers O2 content.
26. How do emboli prevent gas exchange?
They block circulation to certain parts of the lung, causing no gas exchange in that area.
27. What are the risk factors for a pulmonary embolism?
Venous blood stasis, increased coagulation, and damage to the vessel wall.
28. What are other types of thrombi?
Venous, air embolus, fat embolus, septic embolus, and tumor.
29. What is the pathophysiology of a pulmonary embolism?
The pathophysiology of pulmonary embolism centers on blood clots blocking pulmonary arteries, impairing lung blood flow and gas exchange, increasing pressure on the heart’s right ventricle, and potentially leading to lung tissue death and right heart failure.
30. Why do clots tend to form at the bottom of the lung?
Because there is decreased perfusion in that region.
31. What causes an increase in ventilation?
An increase in dead space.
32. What does occlusion of blood flow lead to?
Increased pulmonary vascular resistance, which causes the redistribution of blood flow and pulmonary shunting, and blood returns to systemic circulation with inadequate O2.
33. What can a large embolus lead to?
Hemodynamic collapse, causing decreased cardiac output.
34. What is the treatment for an acute pulmonary embolism?
IV heparin to prolong the clotting time.
35. What is the treatment for a long-term pulmonary embolism?
Warfarin
36. What are the EKG findings for a possible pulmonary embolism?
Tachycardia, right axis deviation, inverted T waves, and right bundle branch block.
37. What are the consequences of a pulmonary embolism?
Right-sided heart strain, complete resolution, infarction, recurrent emboli, pulmonary hypertension because of the chronic strain on the heart, and death.
38. When should contrast not be used during a CT angiogram?
Kidney failure or allergies.
39. What can be noted in a D-dimer test?
It shows increased thrombolytic activity in the body. This test is often done in the ER and may show false positives, but is helpful if negative.
40. What are the medications for a pulmonary embolism?
Heparin, synthetic pentasaccharide, coumadin, warfarin, and thrombolytics.
41. What condition is CT angiogram not helpful during diagnosis?
Small peripheral emboli.
42. What are the strong risk factors for a pulmonary embolism?
Fracture to a lower limb, hospitalization with AF or heart failure, THR, major trauma, myocardial infarction in the past 3 months, and previous DVT.
43. What are the moderate risk factors for a pulmonary embolism?
Autoimmune disease, blood transfusion, paralytic stroke, and infection.
44. What scoring system is used to determine the likelihood of a PE?
Wells score
45. What would be the presentation of a massive PE?
A patient presents with sudden severe chest pain, shortness of breath, and syncope. They are hypertensive with raised JVP and have the S1Q3T3 pattern on an ECG.
46. What initial tests should be performed for a suspected PE?
Chest x-ray, ECG, ABG, D-dimer, and CT pulmonary angiogram.
47. What is the best test for diagnosing a pulmonary embolism?
CTPA is the gold standard
48. What additional tests may be done after a pulmonary embolism diagnosis for prognostic purposes?
Echocardiogram looking for right ventricular dysfunction and troponin looking for signs of cardiac damage; both are associated with a higher risk for early mortality.
49. What is an alternative approach to treating a PE that does not involve regular blood testing?
Immediately start apixaban or rivaroxaban and stay on them long term.
50. For how long should warfarin be continued after a PE?
At least 3 months, then reassess if there is a need for continued use.
51. What is a thrombus?
A blood clot that forms and remains in a vein.
52. What is the definition of an embolus?
A blood clot that becomes dislodged and travels to another part of the body.
53. What is a pulmonary infarction?
When the tissue of the lung dies.
54. Besides clots, what are some possible causes of a pulmonary embolism?
Fat, air, amniotic fluid, bone marrow, and tumor fragments.
55. What are three things that can cause blood clot formation?
Increased tendency of blood to form clots, injury to the endothelial cells that line the vessels, and slowing or stagnation of blood flow through the veins.
56. What term describes the increased tendency of blood to form clots?
Hypercoagulability
57. What clotting factors in the blood might increase and cause a clot?
Prothrombin and polycythemia
58. What is a natural anticoagulant that may cause clotting if it is deficient?
Protein
59. How does the slowing of blood flow make clots more likely to form?
It allows platelets more time in contact with the endothelium.
60. What can cause venous stasis?
Inactivity, CHF, varicose veins, and thrombophlebitis.
61. How does a chest x-ray help diagnose a pulmonary embolism?
It is often normal but can be used to rule out conditions with the same symptoms.
62. What does a D-dimer test look for, and what is considered positive results?
It tests for protein fibrinogen, and values higher than 500 ng/mL are positive.
63. What test is used to differentiate between blood and clots?
Magnetic resonance angiography (MRA)
64. What results from venous admixture developing in a pulmonary embolism?
It causes bronchial smooth muscle constriction.
65. What is the effect of a pulmonary embolism on venous admixture?
It causes increased venous admixture.
66. What is abnormal about heart sounds with PE patients?
Increased S2 due to the valve closing more forcefully, increased splitting of S2, and a third heart sound.
67. What portion of the heart works harder when there is increased pressure in the lungs?
Right ventricle
68. What is the most common abnormal ECG pattern that may suggest the possibility of a PE?
Sinus tachycardia
69. What are some possible x-ray findings in a patient with a PE?
Increased density, hyper radiolucency distal to the embolus, dilation of pulmonary arteries, pulmonary edema, cor pulmonale, and pleural effusion.
70. What diagnostic imaging procedure uses a radioactive compound that is inhaled into the lungs?
V/Q scan
71. What is heparin?
A fast-acting anticoagulant.
72. What is the name of a slow-acting, oral anticoagulant that can be taken preventatively at home?
Warfarin (i.e., Coumadin, Panwarfin)
73. What do thrombolytic agents do?
They actually dissolve the clot.
74. What thrombolytic agents can dissolve clots?
Streptokinase, urokinase, alteplase, and reteplase.
75. What are some preventative measures that can be taken to avoid a pulmonary embolism?
Early ambulation, walking, exercise, drinking fluids, compression stockings, vein filters, and pneumatic compression.
76. What is a pulmonary embolectomy?
The surgical removal of clots in the lungs.
77. Can a pulmonary embolism result in death?
Yes, it is fatal in one-third of patients who are undiagnosed and untreated.
78. What are the breathing patterns for a pulmonary embolism?
Dyspnea and tachypnea
79. What are three diagnostic tests for a pulmonary embolism?
V/Q scan, angiography, and ABG.
80. What types of medications can be administered to treat a pulmonary embolism?
Anticoagulants, thrombolytic agents, analgesics, and inotropic agents.
81. What is the primary goal of acute pulmonary embolism treatment?
To prevent clot extension, restore pulmonary blood flow, and reduce mortality.
82. Why is oxygen therapy commonly required in patients with a pulmonary embolism?
To correct hypoxemia caused by ventilation–perfusion mismatch.
83. What laboratory finding may suggest right ventricular strain in a pulmonary embolism?
Elevated cardiac troponin levels.
84. What echocardiographic finding suggests a high-risk pulmonary embolism?
Right ventricular dilation with reduced systolic function.
85. Why can a pulmonary embolism cause hypotension?
Obstruction of pulmonary blood flow reduces left ventricular preload and cardiac output.
86. What is a paradoxical embolism?
An embolus that crosses from the venous to the arterial circulation through a cardiac shunt, such as a patent foramen ovale.
87. Why are elderly patients at higher risk for a pulmonary embolism?
They are more likely to have immobility, comorbid disease, and hypercoagulable states.
88. What is a submassive pulmonary embolism?
A PE with right ventricular dysfunction but without systemic hypotension.
89. What finding differentiates a massive from a non-massive pulmonary embolism?
Presence of sustained hypotension or shock.
90. Why is PE considered a cause of increased physiologic dead space?
Ventilated alveoli receive little or no perfusion.
91. What role does bedside ultrasound play in a suspected pulmonary embolism?
It may identify right ventricular strain or deep vein thrombosis.
92. What is the significance of sudden unexplained hypoxemia in a hospitalized patient?
It should raise suspicion for pulmonary embolism.
93. Why is hemoptysis considered an uncommon symptom of a PE?
Pulmonary infarction is relatively rare due to dual blood supply of the lungs.
94. What is chronic thromboembolic pulmonary hypertension (CTEPH)?
Pulmonary hypertension caused by unresolved or recurrent pulmonary emboli.
95. Why is PE risk increased after major orthopedic surgery?
Venous stasis and endothelial injury promote clot formation.
96. What is the role of inferior vena cava (IVC) filters in PE management?
To prevent emboli from reaching the lungs when anticoagulation is contraindicated.
97. What complication may occur from untreated recurrent pulmonary emboli?
Development of pulmonary hypertension and right heart failure.
98. Why is clinical probability assessment important before imaging?
It helps guide appropriate testing and reduces unnecessary radiation exposure.
99. What finding suggests an acute rather than chronic pulmonary embolism?
Sudden onset of symptoms with no prior cardiopulmonary disease.
100. Why must anticoagulation therapy be carefully monitored?
To balance the prevention of clot extension with the risk of bleeding.
Final Thoughts
A pulmonary embolism is a critical condition that sits at the intersection of respiratory physiology and cardiovascular function. Its sudden onset, variable presentation, and high mortality make early recognition essential.
For respiratory therapists, understanding how PE affects ventilation, perfusion, gas exchange, and hemodynamics is fundamental to effective patient care. By recognizing key signs, interpreting ABG and monitoring data, and providing timely respiratory support, RTs play a vital role in improving outcomes for patients with pulmonary embolism.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Shah IK, Merfeld JM, Chun J, Tak T. Pathophysiology and Management of Pulmonary Embolism. Int J Angiol. 2022.

