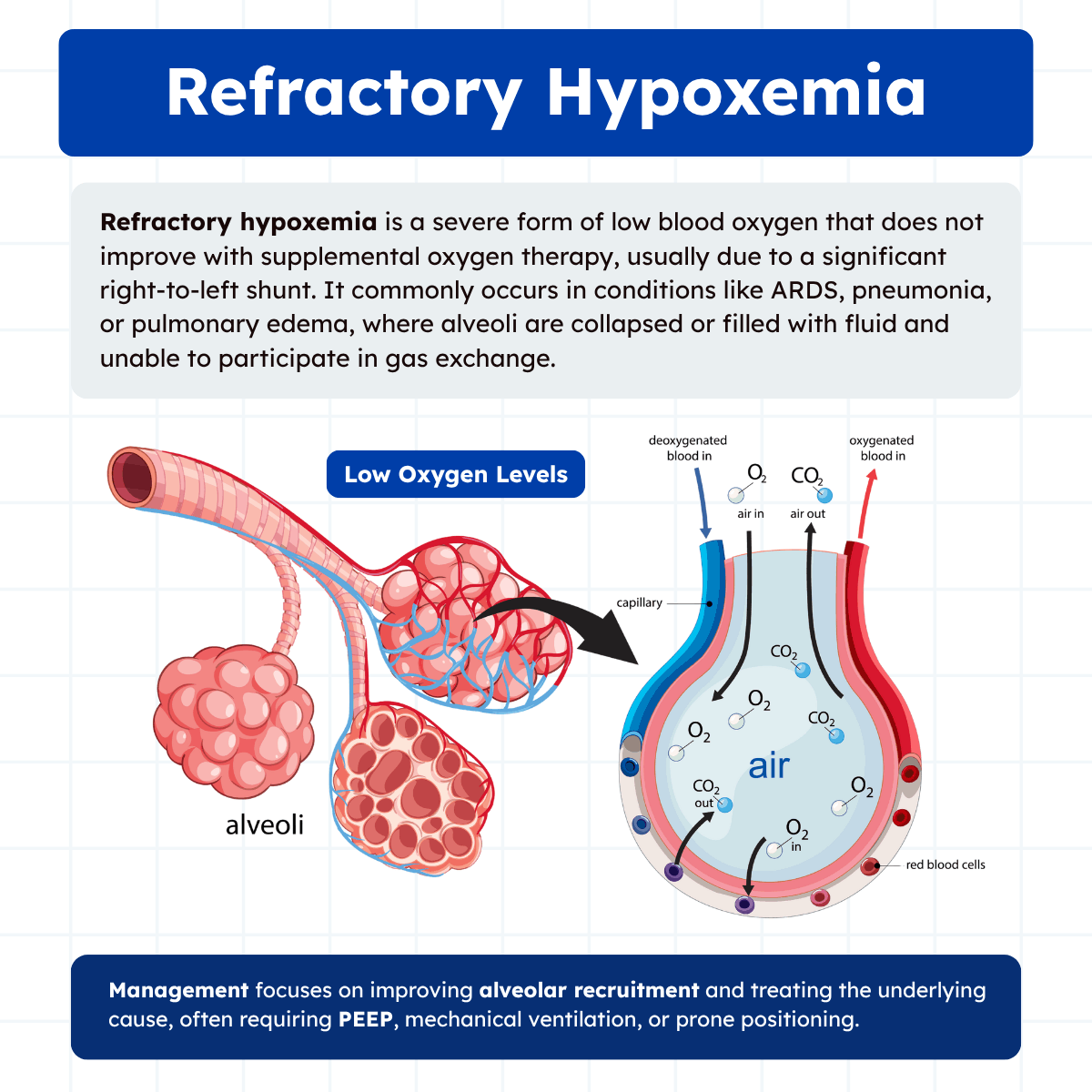
Refractory hypoxemia is a severe and challenging form of impaired oxygenation in which arterial oxygen levels remain low despite the administration of supplemental oxygen. It is most commonly seen in critically ill patients and often signals a significant disruption in normal gas exchange within the lungs.
Unlike more typical forms of hypoxemia, this condition does not respond well to increased inspired oxygen alone, making it more difficult to manage. Understanding the underlying physiology, causes, and treatment strategies is essential for clinicians who care for patients with severe respiratory failure.
What Is Refractory Hypoxemia?
Refractory hypoxemia is defined as a persistent decrease in arterial oxygen tension that does not significantly improve with supplemental oxygen therapy. In clinical practice, this is often recognized when a patient remains hypoxemic despite receiving high concentrations of inspired oxygen, such as an FiO₂ of 0.60 or greater.
This condition typically indicates a severe impairment in gas exchange, most often due to right-to-left shunting or extensive alveolar dysfunction. In these cases, oxygen cannot effectively reach the bloodstream, regardless of how much is delivered to the lungs.
Refractory hypoxemia is frequently associated with acute respiratory failure and is considered a hallmark feature of several life-threatening pulmonary conditions.
How Refractory Hypoxemia Differs From Other Forms
Most types of hypoxemia improve when the fraction of inspired oxygen is increased. For example, patients with ventilation-perfusion mismatch or mild diffusion impairment often respond well to supplemental oxygen because at least some alveoli are still functioning and capable of gas exchange.
In contrast, refractory hypoxemia does not respond adequately to oxygen therapy. This is because a significant portion of blood is passing through areas of the lung where ventilation is absent or severely impaired.
In these situations:
- Oxygen cannot enter the affected alveoli
- Blood leaving these regions remains deoxygenated
- Mixing of oxygenated and deoxygenated blood lowers overall PaO₂
Note: Even if other areas of the lung are well ventilated, they cannot compensate for the poorly functioning regions. This limitation is largely due to the fact that hemoglobin is already nearly fully saturated in healthy lung units.
What Is a Shunt?
A shunt occurs when blood moves from the right side of the circulation to the left without being oxygenated in the lungs. This can happen either through abnormal vascular connections or through lung regions that are perfused but not ventilated.
In refractory hypoxemia, physiologic shunting is the most common mechanism. This occurs when alveoli are:
- Collapsed
- Filled with fluid
- Obstructed
Note: As a result, blood flows through these areas without participating in gas exchange.
Why Shunting Causes Severe Hypoxemia
Shunting leads to the mixing of deoxygenated venous blood with oxygenated arterial blood. This process, often referred to as venous admixture, lowers the overall oxygen content of the blood.
Because the shunted blood never comes into contact with alveolar oxygen, increasing FiO₂ has little effect. This is the defining feature of refractory hypoxemia.
Shunt Fraction
The severity of shunting can be estimated by calculating the shunt fraction, which represents the proportion of cardiac output that bypasses ventilated alveoli.
Note: A higher shunt fraction indicates more severe impairment and is often associated with poorer outcomes.
Common Causes of Refractory Hypoxemia
Refractory hypoxemia is most often seen in conditions that cause widespread alveolar dysfunction or collapse.
Acute Respiratory Distress Syndrome (ARDS)
ARDS is one of the most common causes of refractory hypoxemia. It is characterized by:
- Diffuse inflammation
- Increased permeability of the alveolar-capillary membrane
- Accumulation of fluid in the alveoli
Note: These changes lead to extensive shunting and severe impairment of oxygenation.
Severe Pneumonia
In severe pneumonia, alveoli may become filled with inflammatory exudate, preventing ventilation. This creates regions of low or zero ventilation relative to perfusion.
As the disease progresses, the degree of shunting increases, making oxygenation more difficult to maintain.
Pulmonary Edema
Pulmonary edema, whether cardiogenic or noncardiogenic, results in fluid accumulation within the alveoli. This fluid interferes with gas exchange and contributes to shunt physiology.
Patients with pulmonary edema often require more than supplemental oxygen to correct hypoxemia.
Atelectasis
Atelectasis refers to the collapse of alveoli, which eliminates ventilation in affected areas. When blood continues to flow through these regions, a physiologic shunt develops.
Atelectasis is common in postoperative patients, those with prolonged immobility, and individuals with airway obstruction.
Other Causes
Additional causes of refractory hypoxemia include:
- Pulmonary contusion
- Aspiration of gastric contents
- Severe asthma with mucus plugging
- Diffuse alveolar hemorrhage
Note: In each of these conditions, the underlying problem involves impaired ventilation of perfused lung units.
Pathophysiology of Refractory Hypoxemia
Alveolar Collapse and Flooding
In many cases, refractory hypoxemia results from alveoli that are either collapsed or filled with fluid. These alveoli are unable to participate in gas exchange, even when oxygen is delivered at high concentrations.
This leads to a mismatch between ventilation and perfusion, with some areas effectively having a V/Q ratio of zero.
Impaired Gas Exchange
The presence of fluid, inflammation, or structural damage within the lungs increases the distance that oxygen must travel to reach the blood. In severe cases, oxygen transfer becomes so limited that it cannot meet the body’s needs.
Loss of Functional Surface Area
As more alveoli become nonfunctional, the overall surface area available for gas exchange decreases. This further worsens hypoxemia and contributes to the severity of the condition.
Inflammatory Response
In conditions such as ARDS, the inflammatory response plays a major role in disrupting normal lung function. Cytokines and other inflammatory mediators increase vascular permeability and promote edema formation.
Note: This process creates a cycle of worsening gas exchange and increasing oxygen requirements.
Clinical Presentation
Patients with refractory hypoxemia are often critically ill and may present with severe respiratory distress.
Common findings include:
- Marked shortness of breath
- Rapid, labored breathing
- Use of accessory muscles
- Cyanosis
- Restlessness or agitation
- Altered mental status
- Tachycardia
In severe cases, patients may develop respiratory failure requiring ventilatory support. Because refractory hypoxemia often develops in the setting of acute illness, it is frequently accompanied by other signs of systemic dysfunction, such as hypotension or organ impairment.
Diagnostic Evaluation
Arterial Blood Gas Analysis
Arterial blood gas analysis is essential for identifying refractory hypoxemia. It typically reveals:
- Low PaO₂ despite high FiO₂
- Possible respiratory alkalosis or acidosis depending on ventilation
Note: The failure of PaO₂ to improve with oxygen therapy is a key diagnostic feature.
Oxygenation Indices
Clinicians often use indices such as the PaO₂/FiO₂ ratio to assess the severity of hypoxemia. A low ratio indicates severe impairment in oxygenation and is commonly used in the diagnosis of ARDS.
Imaging Studies
Chest imaging plays a critical role in identifying the underlying cause. Common findings may include:
- Bilateral infiltrates in ARDS
- Consolidation in pneumonia
- Fluid accumulation in pulmonary edema
- Areas of collapse in atelectasis
Additional Testing
Further evaluation may include:
- Echocardiography to assess cardiac function
- Laboratory tests to evaluate infection or inflammation
- Bronchoscopy in selected cases
Note: A comprehensive approach is necessary to determine the cause and guide treatment.
Management of Refractory Hypoxemia
Supplemental Oxygen
Although refractory hypoxemia does not respond well to oxygen therapy alone, supplemental oxygen is still an essential first step. Increasing the fraction of inspired oxygen can improve oxygenation in partially functioning lung units, even if it does not fully correct the problem.
Patients are often placed on high concentrations of oxygen early in management. Delivery methods may include:
- Nonrebreather mask
- High-flow nasal cannula
- Noninvasive ventilation
- Mechanical ventilation
Note: Clinicians must recognize that oxygen therapy alone is rarely sufficient in cases of refractory hypoxemia.
Positive End-Expiratory Pressure (PEEP)
PEEP is one of the most important interventions for refractory hypoxemia. It works by maintaining pressure in the lungs at the end of expiration, which helps keep alveoli open.
Benefits of PEEP include:
- Recruitment of collapsed alveoli
- Increased functional residual capacity
- Improved ventilation-perfusion matching
- Reduction in shunt fraction
Note: By reopening previously collapsed alveoli, PEEP allows more blood to pass through ventilated regions of the lung, improving oxygenation. Careful titration is required, as excessive PEEP can reduce cardiac output and cause lung injury.
Mechanical Ventilation
When hypoxemia cannot be corrected with noninvasive measures, mechanical ventilation is often required.
Ventilator strategies focus on:
- Lung-protective ventilation with low tidal volumes
- Adequate PEEP to maintain alveolar recruitment
- Avoidance of excessive airway pressures
Note: These strategies are especially important in conditions such as ARDS, where the lungs are highly susceptible to injury. Mechanical ventilation supports oxygenation while allowing time to treat the underlying cause.
Prone Positioning
Prone positioning involves placing the patient on their abdomen rather than their back. This technique has been shown to significantly improve oxygenation in patients with severe refractory hypoxemia, particularly in ARDS.
Benefits include:
- Improved distribution of ventilation
- Better matching of ventilation and perfusion
- Recruitment of dorsal lung regions
- Reduction in shunt
Note: Prone positioning is now a standard intervention in severe cases and has been associated with improved outcomes when used appropriately.
Recruitment Maneuvers
Recruitment maneuvers involve temporarily increasing airway pressure to open collapsed alveoli. These maneuvers can improve oxygenation by increasing the number of functional lung units.
They are often used in conjunction with PEEP to maintain the newly opened alveoli. While beneficial in some cases, recruitment maneuvers must be used cautiously due to the risk of barotrauma and hemodynamic instability.
Treating the Underlying Cause
Effective management of refractory hypoxemia requires identifying and treating the underlying condition.
Examples include:
- Antibiotics for severe pneumonia
- Diuretics for pulmonary edema
- Anti-inflammatory strategies in ARDS
- Airway clearance for mucus plugging
- Treatment of aspiration or hemorrhage
Note: Without addressing the root cause, supportive measures alone are unlikely to provide sustained improvement.
Advanced and Rescue Therapies
- Neuromuscular Blockade: Short-term use of neuromuscular blocking agents may improve oxygenation by reducing patient-ventilator dyssynchrony and decreasing oxygen consumption.
- Inhaled Vasodilators: Inhaled nitric oxide or prostacyclin can improve oxygenation by selectively dilating pulmonary vessels in well-ventilated areas, improving V/Q matching.
- Extracorporeal Membrane Oxygenation (ECMO): Provides external support for gas exchange by circulating blood through an artificial lung. It is used in life-threatening cases when conventional therapies fail. Although resource-intensive, ECMO can be life-saving in carefully selected patients.
Monitoring and Ongoing Assessment
Management of refractory hypoxemia requires continuous monitoring and reassessment.
Key parameters include:
- Arterial blood gases
- Oxygen saturation
- PaO₂/FiO₂ ratio
- Respiratory rate and effort
- Hemodynamic status
Clinicians must also monitor for complications related to therapy, including ventilator-induced lung injury, oxygen toxicity, and hemodynamic instability.
Note: Frequent reassessment allows for timely adjustments in treatment and helps prevent further deterioration.
Complications of Refractory Hypoxemia
Organ Dysfunction
Prolonged tissue hypoxia can impair the function of vital organs, including:
- Brain
- Heart
- Kidneys
- Liver
Note: This may result in confusion, arrhythmias, renal failure, and other forms of organ dysfunction.
Respiratory Failure
As hypoxemia worsens, patients may lose the ability to maintain adequate ventilation and oxygenation, leading to respiratory failure. This often necessitates mechanical ventilation and intensive care support.
Increased Mortality
Refractory hypoxemia is associated with high mortality rates, particularly in conditions such as ARDS and severe sepsis. Early recognition and aggressive management are critical to improving outcomes.
Prognosis
The prognosis of refractory hypoxemia depends on several factors, including:
- The underlying cause
- The severity of lung injury
- The patient’s overall health
- The timeliness of intervention
Note: Some patients recover fully with appropriate treatment, while others may develop long-term complications such as fibrosis or chronic respiratory impairment. In severe cases, refractory hypoxemia can be fatal despite optimal care.
Clinical Significance
Refractory hypoxemia represents a critical challenge in respiratory care. It requires a thorough understanding of pulmonary physiology, careful assessment, and prompt intervention.
For clinicians, recognizing this condition is essential because it signals:
- Severe impairment in gas exchange
- The need for advanced respiratory support
- A higher risk of complications
Note: Effective management depends on identifying the mechanism, optimizing oxygen delivery, and treating the underlying disease.
Refractory Hypoxemia Practice Questions
1. What is refractory hypoxemia?
Refractory hypoxemia is severe hypoxemia that does not significantly improve despite administration of high concentrations of oxygen.
2. What is the primary cause of refractory hypoxemia?
Intrapulmonary shunting
3. What is an intrapulmonary shunt?
Blood passes through the lungs without being oxygenated due to non-ventilated alveoli.
4. Why does oxygen therapy fail in refractory hypoxemia?
Because oxygen cannot reach blood flowing through non-ventilated alveoli.
5. What PaO₂ level is typically seen in refractory hypoxemia?
PaO₂ remains low despite high FiO₂ (often <60 mmHg).
6. What disease is most commonly associated with refractory hypoxemia?
Acute Respiratory Distress Syndrome (ARDS)
7. How does ARDS cause refractory hypoxemia?
Alveoli fill with fluid and collapse, creating shunt conditions.
8. What is the hallmark feature of refractory hypoxemia?
Poor response to supplemental oxygen.
9. What happens to the A-a gradient in refractory hypoxemia?
It is significantly increased.
10. What is the role of alveolar collapse in refractory hypoxemia?
It prevents ventilation, leading to shunt.
11. How does pulmonary edema contribute to refractory hypoxemia?
Fluid-filled alveoli impair gas exchange and create shunt.
12. What is the effect of pneumonia on refractory hypoxemia?
Consolidation of lung tissue leads to shunting.
13. What is the difference between V/Q mismatch and shunt?
V/Q mismatch can improve with oxygen; shunt cannot.
14. What percentage of shunt typically causes refractory hypoxemia?
Large shunts (greater than 20–30%).
15. What is PEEP?
Positive end-expiratory pressure used to keep alveoli open.
16. How does PEEP help refractory hypoxemia?
It recruits collapsed alveoli and reduces shunt.
17. What is alveolar recruitment?
Opening collapsed alveoli to improve gas exchange.
18. What is prone positioning?
Placing the patient face-down to improve oxygenation.
19. How does prone positioning improve refractory hypoxemia?
It improves ventilation-perfusion matching and alveolar recruitment.
20. What is the role of mechanical ventilation in refractory hypoxemia?
It supports oxygenation and allows application of PEEP.
21. What is FiO₂?
Fraction of inspired oxygen
22. Why is high FiO₂ alone insufficient in refractory hypoxemia?
Because shunted blood bypasses ventilated alveoli.
23. What complication can result from prolonged high FiO₂?
Oxygen toxicity
24. What is ECMO?
Extracorporeal membrane oxygenation
25. When is ECMO used in refractory hypoxemia?
When conventional therapies fail.
26. What is the effect of refractory hypoxemia on organs?
It can lead to multi-organ failure.
27. What is the role of nitric oxide in refractory hypoxemia?
It improves pulmonary blood flow to ventilated areas.
28. What is permissive hypoxemia?
Accepting lower oxygen levels to avoid ventilator-induced injury.
29. What is the relationship between refractory hypoxemia and mortality?
It is associated with high mortality rates.
30. What is the primary goal in treating refractory hypoxemia?
To improve oxygenation by reducing shunt and recruiting alveoli.
31. What is the typical response of refractory hypoxemia to 100% oxygen?
Minimal or no improvement in PaO₂.
32. What type of lung units are responsible for shunt in refractory hypoxemia?
Perfused but non-ventilated alveoli.
33. What is consolidation in the lungs?
Filling of alveoli with fluid, pus, or debris, impairing ventilation.
34. How does consolidation affect oxygenation?
It creates areas of true shunt.
35. What is the role of surfactant in refractory hypoxemia?
Loss of surfactant leads to alveolar collapse.
36. What condition causes surfactant dysfunction leading to refractory hypoxemia?
ARDS
37. What is lung compliance in refractory hypoxemia?
It is typically decreased (stiff lungs).
38. How does decreased compliance affect ventilation?
It makes the lungs harder to inflate.
39. What ventilator strategy is used for refractory hypoxemia?
Low tidal volume ventilation.
40. Why is low tidal volume ventilation used?
To prevent ventilator-induced lung injury.
41. What is ventilator-induced lung injury (VILI)?
Damage caused by excessive pressure or volume during mechanical ventilation.
42. What is barotrauma?
Lung injury caused by high airway pressures.
43. What is volutrauma?
Lung injury caused by excessive tidal volumes.
44. What is atelectrauma?
Injury from repeated opening and closing of alveoli.
45. What is biotrauma?
Inflammatory injury caused by mechanical ventilation.
46. What is plateau pressure?
The pressure measured in the lungs during a pause in inspiration.
47. Why is plateau pressure monitored in refractory hypoxemia?
To avoid lung overdistention.
48. What plateau pressure is considered safe?
Typically less than 30 cm H₂O.
49. What is driving pressure?
The difference between plateau pressure and PEEP.
50. Why is driving pressure important?
Lower driving pressures are associated with better outcomes.
51. What is a recruitment maneuver?
A temporary increase in airway pressure to open collapsed alveoli.
52. When are recruitment maneuvers used?
In severe refractory hypoxemia to improve oxygenation.
53. What risk is associated with recruitment maneuvers?
Barotrauma and hemodynamic instability.
54. What is the effect of sedation in refractory hypoxemia?
It reduces oxygen demand and improves ventilator synchrony.
55. What is neuromuscular blockade used for?
To eliminate patient-ventilator dyssynchrony.
56. When is paralysis considered in refractory hypoxemia?
In severe ARDS with poor oxygenation.
57. What is the effect of fluid overload on refractory hypoxemia?
It worsens pulmonary edema and oxygenation.
58. What is conservative fluid management?
Limiting fluids to reduce lung edema.
59. How does cardiac function affect refractory hypoxemia?
Poor cardiac output reduces oxygen delivery.
60. What is the importance of early recognition of refractory hypoxemia?
It allows timely intervention to prevent worsening respiratory failure.
61. What type of V/Q ratio is present in true shunt?
A V/Q ratio of 0 (no ventilation).
62. How does blood flow behave in shunt conditions?
It passes through alveoli without gas exchange.
63. What is the effect of increasing FiO₂ in a true shunt?
It has little to no effect on oxygenation.
64. What bedside indicator suggests refractory hypoxemia?
Persistently low SpO₂ despite high oxygen therapy.
65. What is the typical FiO₂ level used before labeling hypoxemia as refractory?
High levels such as ≥0.60–1.0.
66. What is lung recruitment dependent on?
Adequate PEEP and airway pressure.
67. What happens if PEEP is too low in refractory hypoxemia?
Alveoli collapse, worsening shunt.
68. What happens if PEEP is too high?
It can impair cardiac output and cause overdistention.
69. What is the effect of overdistention of alveoli?
It can worsen V/Q mismatch and cause lung injury.
70. What is permissive hypercapnia?
Allowing elevated CO₂ levels to reduce ventilator-induced injury.
71. Why is permissive hypercapnia used?
To minimize lung damage from aggressive ventilation.
72. What is the relationship between ARDS severity and refractory hypoxemia?
More severe ARDS leads to more severe refractory hypoxemia.
73. What imaging finding is common in refractory hypoxemia?
Diffuse bilateral infiltrates on chest X-ray.
74. What is “white-out” lung?
Severe diffuse opacification seen in ARDS.
75. What is the effect of gravity on lung perfusion?
More blood flows to dependent lung regions.
76. How does this relate to prone positioning?
Prone positioning redistributes perfusion and improves oxygenation.
77. What is the role of alveolar ventilation in refractory hypoxemia?
It is severely reduced in affected lung regions.
78. What happens to functional residual capacity (FRC) in refractory hypoxemia?
It is decreased.
79. Why is decreased FRC problematic?
It promotes alveolar collapse.
80. What is closing volume?
The lung volume at which small airways begin to collapse.
81. How is closing volume affected in lung disease?
It increases, leading to airway closure.
82. What is the effect of aging on hypoxemia risk?
Older patients are more susceptible due to decreased lung elasticity.
83. What is the role of inflammatory mediators in refractory hypoxemia?
They increase permeability and cause lung injury.
84. What is capillary leak syndrome?
Leakage of fluid into alveoli due to inflammation.
85. How does capillary leak worsen oxygenation?
It fills alveoli with fluid, impairing gas exchange.
86. What is the effect of sepsis on refractory hypoxemia?
It can trigger ARDS and worsen oxygenation.
87. What is the role of corticosteroids in refractory hypoxemia?
They may reduce inflammation in certain cases.
88. What is inhaled prostacyclin used for?
To improve pulmonary blood flow to ventilated areas.
89. What is differential lung ventilation?
Ventilating each lung separately in severe cases.
90. When is differential lung ventilation considered?
In severe unilateral lung disease with refractory hypoxemia.
91. What is the effect of alveolar flooding on oxygen diffusion?
It significantly impairs diffusion by increasing the distance oxygen must travel.
92. What is the role of hemoglobin saturation in refractory hypoxemia?
It remains low despite high FiO₂ due to shunting.
93. What is the impact of microatelectasis in refractory hypoxemia?
It contributes to widespread alveolar collapse and shunt.
94. What is the effect of high oxygen concentrations on nitrogen in the lungs?
It can wash out nitrogen and promote absorption atelectasis.
95. What is absorption atelectasis?
Collapse of alveoli due to the removal of nitrogen and rapid oxygen absorption.
96. How does obesity affect refractory hypoxemia?
It decreases lung volumes and promotes atelectasis.
97. What is the role of chest wall mechanics in refractory hypoxemia?
Impaired mechanics can reduce effective ventilation.
98. What is the effect of abdominal pressure on lung function?
Increased abdominal pressure can reduce lung expansion and worsen oxygenation.
99. What is the purpose of monitoring PaO₂/FiO₂ ratio?
To assess the severity of hypoxemia and ARDS.
100. What PaO₂/FiO₂ ratio indicates severe refractory hypoxemia (ARDS)?
Less than 100 mmHg.
Final Thoughts
Refractory hypoxemia is a severe form of impaired oxygenation that does not respond adequately to supplemental oxygen, most often due to significant shunting and widespread alveolar dysfunction. It is commonly seen in conditions such as ARDS, pneumonia, pulmonary edema, and atelectasis, where portions of the lung are unable to participate in gas exchange.
Management requires more than increasing oxygen levels and often involves PEEP, mechanical ventilation, prone positioning, and treatment of the underlying cause. A clear understanding of the underlying physiology allows clinicians to guide therapy effectively and improve patient outcomes in this high-risk condition.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Mehta C, Mehta Y. Management of refractory hypoxemia. Ann Card Anaesth. 2016.

