Total lung capacity is a fundamental measurement that represents the absolute maximum volume of air the lungs can hold. While it may seem like a straightforward concept, total lung capacity provides critical insight into lung size, mechanics, and the presence of underlying respiratory disease.
For respiratory therapists, understanding total lung capacity is essential for accurately interpreting pulmonary function tests, distinguishing between restrictive and obstructive disorders, and assessing disease severity.
What Is Total Lung Capacity?
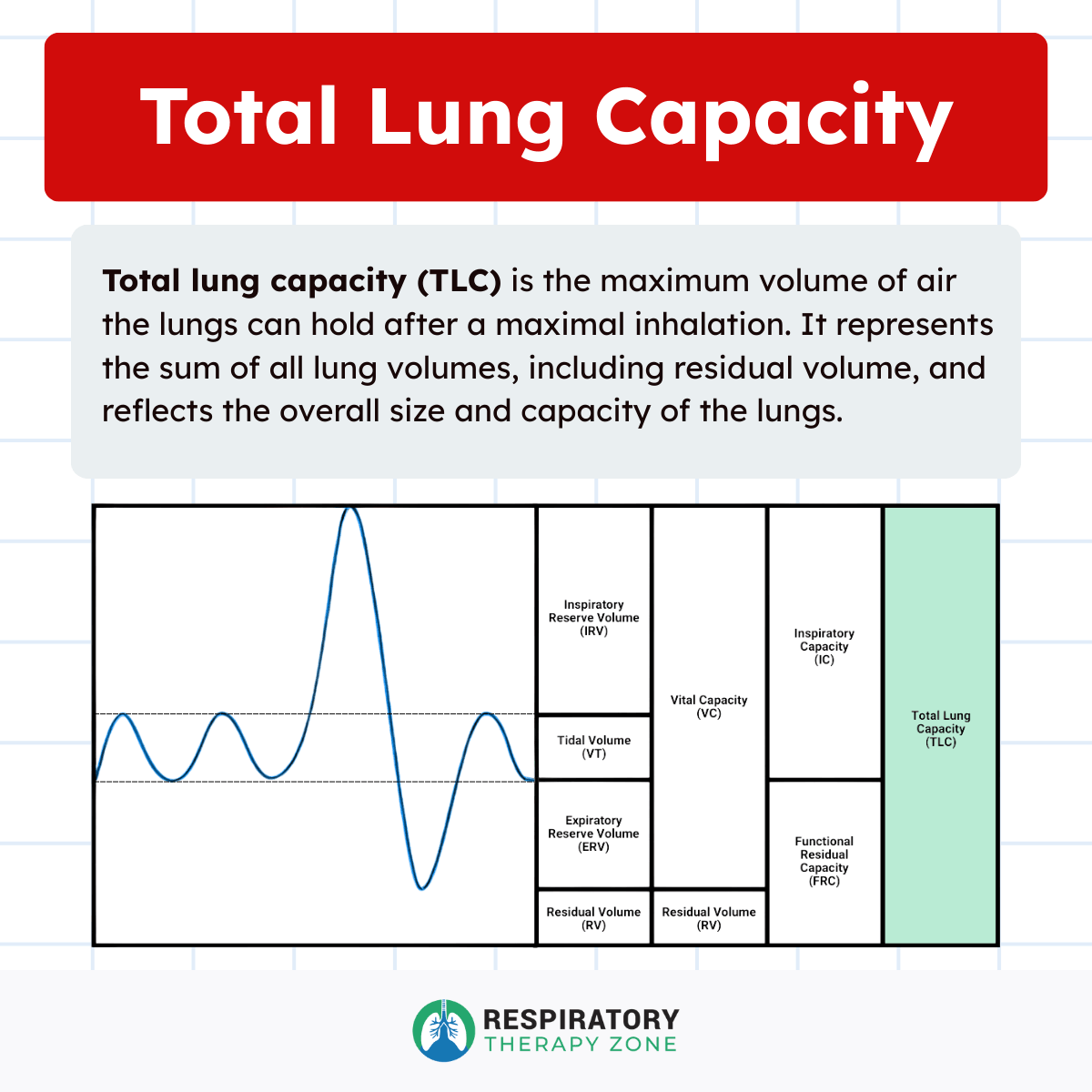
Total lung capacity (TLC) is the total volume of air contained in the lungs after a person takes the deepest breath possible. It represents the sum of all lung volumes and reflects the maximum capacity of the respiratory system.
Total lung capacity is composed of four primary lung volumes:
- Tidal volume (VT)
- Inspiratory reserve volume (IRV)
- Expiratory reserve volume (ERV)
- Residual volume (RV)
This relationship can be expressed as:
Total Lung Capacity = VT + IRV + ERV + RV
Because TLC includes residual volume, it cannot be measured directly with simple spirometry and requires specialized testing methods.
Normal Values and Variability
In healthy adults, total lung capacity typically ranges from about 5 to 6 liters, though normal values vary based on age, sex, height, and body size. Predicted TLC values are calculated using standardized reference equations, and results are interpreted as a percentage of the predicted value.
Total lung capacity tends to be:
- Higher in taller individuals
- Higher in males compared to females
- Lower with advancing age
- Reduced in restrictive lung disease
Note: Because of normal variability, TLC should never be interpreted in isolation and must be evaluated alongside clinical findings and other pulmonary function measurements.
How Total Lung Capacity Is Measured
Since total lung capacity includes residual volume, it cannot be measured using spirometry alone. Instead, it is assessed using specialized lung volume measurement techniques.
Body Plethysmography
Body plethysmography is considered the gold standard for measuring total lung capacity. It measures lung volumes based on pressure changes inside a sealed chamber and can accurately detect trapped gas, making it especially useful in obstructive lung disease.
Gas Dilution Techniques
Helium dilution and nitrogen washout estimate total lung capacity by measuring how a known gas mixes with air in the lungs. These methods may underestimate TLC in patients with significant air trapping.
Imaging-Based Assessment
In some cases, imaging studies such as CT scans can provide indirect estimates of lung volumes, though this approach is not routinely used in clinical practice.
Clinical Significance of Total Lung Capacity
Total lung capacity provides critical information about lung expansion and overall respiratory mechanics. Changes in TLC often indicate underlying pathology and help differentiate disease patterns.
Reduced Total Lung Capacity
A decreased TLC is the defining feature of restrictive lung disease. Conditions commonly associated with reduced TLC include:
- Pulmonary fibrosis
- Interstitial lung disease
- Chest wall deformities
- Neuromuscular disorders
- Severe obesity
Note: In these conditions, lung expansion is limited, reducing the total amount of air the lungs can hold.
Increased Total Lung Capacity
An increased TLC is typically associated with obstructive lung disease, particularly when air trapping and hyperinflation are present. Conditions associated with elevated TLC include:
- Emphysema
- Chronic obstructive pulmonary disease (COPD)
- Severe asthma
Note: In these patients, residual volume increases disproportionately, leading to lung hyperinflation.
Total Lung Capacity and Hyperinflation
One of the most important clinical applications of total lung capacity is assessing lung hyperinflation. Hyperinflation occurs when air becomes trapped in the lungs, increasing residual volume and total lung capacity.
Hyperinflation alters diaphragm mechanics, flattens the diaphragm, and increases the work of breathing. For respiratory therapists, recognizing increased TLC helps explain symptoms such as dyspnea, exercise intolerance, and reduced ventilatory efficiency.
Role of Total Lung Capacity in Pulmonary Function Testing
Total lung capacity is a key component of complete pulmonary function testing. While spirometry alone can suggest restrictive disease, a reduced forced vital capacity does not confirm restriction unless TLC is also reduced.
This distinction is critical, as obstructive lung disease with air trapping can also reduce forced vital capacity. Measuring TLC allows respiratory therapists to accurately classify lung disease and avoid misdiagnosis.
Relevance to Respiratory Therapists
Total lung capacity is especially important to respiratory therapists because it directly influences diagnosis, treatment planning, and patient education.
Understanding TLC helps therapists:
- Differentiate restrictive from obstructive lung disease
- Identify air trapping and hyperinflation
- Interpret full pulmonary function test results
- Assess disease severity and progression
- Explain test results to patients
Note: TLC provides a global view of lung mechanics that complements airflow and gas exchange measurements.
Total Lung Capacity in Critical Care
In critical care settings, total lung capacity provides insight into lung recruitability and disease severity, even though it is not measured routinely at the bedside.
In conditions such as acute respiratory distress syndrome (ARDS), functional lung size may be significantly reduced despite normal predicted TLC values. Understanding the concept of reduced functional lung capacity helps respiratory therapists apply lung-protective ventilation strategies and avoid overdistension.
Factors That Influence Total Lung Capacity
Several physiological and mechanical factors influence total lung capacity, including:
- Lung compliance
- Chest wall compliance
- Respiratory muscle strength
- Body habitus
- Posture
Note: Total lung capacity is generally higher in the upright position and may decrease when supine, especially in patients with obesity or diaphragmatic weakness.
Common Misconceptions About Total Lung Capacity
One common misconception is that a normal total lung capacity means normal lung function. TLC reflects lung size but does not assess airflow limitation or gas exchange.
Another misunderstanding is assuming that a reduced vital capacity always indicates restrictive lung disease. Without measuring TLC, reduced vital capacity may be due to air trapping rather than true restriction.
Note: Total lung capacity must always be interpreted in the context of the full clinical picture.
Access our quiz with sample TMC practice questions and detailed explanations to help you master pulmonary function testing (PFT).
Total Lung Capacity Practice Questions
1. What is total lung capacity (TLC)?
Total lung capacity is the maximum volume of air the lungs can hold after a person inhales as deeply as possible.
2. What does total lung capacity represent clinically?
It reflects lung size, lung mechanics, and the presence or absence of restrictive or obstructive lung disease.
3. Why is total lung capacity an important measurement for respiratory therapists?
Because it helps distinguish between restrictive and obstructive disorders and assess disease severity.
4. What lung volumes make up total lung capacity?
Tidal volume, inspiratory reserve volume, expiratory reserve volume, and residual volume.
5. What is the formula for total lung capacity?
TLC = VT + IRV + ERV + RV
6. Why can total lung capacity not be measured by simple spirometry?
Because spirometry cannot measure residual volume.
7. What specialized methods are required to measure TLC?
Body plethysmography, helium dilution, or nitrogen washout techniques.
8. What lung volume prevents direct measurement of TLC with spirometry?
Residual volume
9. What is the typical range of total lung capacity in healthy adults?
Approximately 5 to 6 liters
10. How are TLC values interpreted in pulmonary function testing?
As a percentage of the predicted value based on age, sex, height, and body size.
11. What factors influence predicted total lung capacity?
Age, sex, height, and overall body size.
12. How does height affect total lung capacity?
Taller individuals generally have a higher TLC.
13. How does sex influence total lung capacity?
Males typically have a higher TLC than females.
14. How does aging affect total lung capacity?
TLC tends to decrease with advancing age.
15. What happens to TLC in restrictive lung disease?
TLC is reduced
16. What happens to TLC in obstructive lung disease?
TLC is often normal or increased due to air trapping and hyperinflation.
17. Why should TLC not be interpreted in isolation?
Because normal variability exists and results must be correlated with clinical findings and other PFT values.
18. What does a TLC less than 80% of predicted typically indicate?
A restrictive ventilatory defect.
19. What does an increased TLC suggest in a patient with airflow obstruction?
Hyperinflation due to air trapping.
20. Which lung volumes contribute most to increased TLC in obstructive disease?
Residual volume and expiratory reserve volume.
21. How does body plethysmography differ from gas dilution methods in measuring TLC?
It measures all intrathoracic gas, including trapped gas.
22. Why may gas dilution techniques underestimate TLC in severe obstruction?
Because poorly ventilated or trapped air is not fully measured.
23. What role does TLC play in assessing disease progression?
Changes in TLC can indicate worsening or improvement of restrictive or obstructive lung disease.
24. Why is TLC considered a static lung volume?
Because it is measured without regard to airflow or time.
25. What other pulmonary function measurements should be reviewed alongside TLC?
Spirometry, lung volumes, diffusion capacity, and clinical symptoms.
26. Why can’t total lung capacity be measured using spirometry alone?
Because spirometry cannot measure residual volume, which is a required component of TLC.
27. What is considered the gold standard method for measuring total lung capacity?
Body plethysmography
28. How does body plethysmography measure total lung capacity?
By using pressure changes inside a sealed chamber to calculate lung volumes based on Boyle’s law.
29. Why is body plethysmography especially useful in obstructive lung disease?
Because it can measure trapped gas that gas dilution methods may miss.
30. What types of lung volumes does body plethysmography measure?
Total thoracic gas volume, including trapped air.
31. What are gas dilution techniques used to estimate total lung capacity?
Helium dilution and nitrogen washout.
32. How do gas dilution techniques estimate total lung capacity?
By measuring how a known gas mixes with air in the lungs during breathing.
33. Why may gas dilution methods underestimate TLC in some patients?
Because trapped or poorly ventilated gas does not equilibrate with the test gas.
34. In which type of lung disease is TLC most likely underestimated by gas dilution?
Severe obstructive lung disease with air trapping.
35. Can imaging studies be used to assess total lung capacity?
Yes, imaging such as CT scans can provide indirect estimates of lung volume.
36. Why is imaging-based assessment of TLC not routinely used?
Because it is less practical and not standardized for routine pulmonary function testing.
37. What does total lung capacity reveal about respiratory mechanics?
It provides information about lung expansion and overall lung size.
38. What does a reduced total lung capacity indicate?
A restrictive ventilatory defect.
39. What is the defining pulmonary function characteristic of restrictive lung disease?
A decreased total lung capacity.
40. Which lung conditions are commonly associated with reduced TLC?
Pulmonary fibrosis, interstitial lung disease, chest wall deformities, neuromuscular disorders, and severe obesity.
41. Why does severe obesity reduce total lung capacity?
Because excess body mass limits chest wall and diaphragmatic movement.
42. What does an increased total lung capacity usually indicate?
Obstructive lung disease with air trapping and hyperinflation.
43. Which lung conditions are associated with increased TLC?
Emphysema, COPD, and severe asthma.
44. What lung volume increases disproportionately in hyperinflation?
Residual volume
45. What is lung hyperinflation?
A condition where air becomes trapped in the lungs, increasing residual volume and TLC.
46. How does hyperinflation affect the diaphragm?
It flattens the diaphragm and reduces its mechanical efficiency.
47. How does increased TLC contribute to dyspnea?
By increasing the work of breathing and reducing ventilatory efficiency.
48. Why is TLC important for interpreting a reduced forced vital capacity (FVC)?
Because a low FVC alone does not confirm restriction unless TLC is also reduced.
49. How can obstructive lung disease falsely appear restrictive on spirometry?
Air trapping can reduce FVC despite a normal or increased TLC.
50. What role does TLC play in avoiding misdiagnosis?
It helps differentiate true restriction from obstruction with air trapping.
51. Why is total lung capacity important for respiratory therapists?
It directly influences diagnosis, treatment planning, and patient education.
52. How does TLC help identify air trapping?
An increased TLC with a high residual volume suggests trapped air.
53. How is TLC used to assess disease severity?
Changes in TLC reflect progression or improvement of lung disease.
54. Why is TLC considered a “global” lung measurement?
Because it reflects overall lung size rather than airflow or gas exchange.
55. How does posture affect total lung capacity?
TLC is generally higher when upright and lower when supine.
56. Why does TLC decrease in the supine position?
Because abdominal contents push against the diaphragm, limiting lung expansion.
57. What mechanical factors influence total lung capacity?
Lung compliance, chest wall compliance, and respiratory muscle strength.
58. How does decreased lung compliance affect TLC?
It reduces the ability of the lungs to expand, lowering TLC.
59. Why does normal TLC not guarantee normal lung function?
Because TLC does not assess airflow limitation or gas exchange.
60. Why is it incorrect to assume reduced vital capacity always means restriction?
Because reduced vital capacity can result from air trapping without reduced TLC.
61. How does TLC contribute to critical care decision-making?
It helps conceptualize lung size and recruitability, even if not measured directly.
62. Why is understanding TLC important in ARDS?
Because functional lung size is reduced, increasing the risk of overdistension.
63. What ventilation strategy is guided by the concept of reduced functional TLC in ARDS?
Lung-protective ventilation with lower tidal volumes.
64. What misconception exists regarding normal TLC values?
That normal TLC always means healthy lungs.
65. Why must TLC always be interpreted with other PFT results?
Because airflow and gas exchange abnormalities may exist despite normal lung size.
66. What lung volumes are added together to calculate total lung capacity?
Tidal volume, inspiratory reserve volume, expiratory reserve volume, and residual volume.
67. Why is residual volume essential when calculating TLC?
Because it represents air that cannot be exhaled and contributes to total lung size.
68. What happens to TLC in early restrictive lung disease?
It may be mildly reduced or borderline before becoming significantly decreased.
69. Can total lung capacity be normal in mild asthma?
Yes, TLC is often normal or mildly increased in asthma.
70. How does emphysema affect total lung capacity?
It increases TLC due to loss of elastic recoil and air trapping.
71. What happens to TLC when elastic recoil of the lungs is lost?
TLC increases because the lungs expand more easily.
72. How does chest wall stiffness affect TLC?
It reduces TLC by limiting thoracic expansion.
73. What role does respiratory muscle weakness play in TLC?
It can reduce TLC by limiting maximal inspiratory effort.
74. Why is TLC useful when evaluating neuromuscular disease?
Because weakened muscles reduce lung expansion, lowering TLC.
75. What pulmonary function pattern shows low TLC with normal FEV1/FVC?
Restrictive lung disease
76. What pattern shows high TLC with low FEV1/FVC?
Obstructive lung disease with hyperinflation.
77. How does air trapping affect TLC measurements?
It increases TLC by raising residual volume.
78. What happens to TLC after lung resection surgery?
It decreases due to loss of lung tissue.
79. How does scoliosis affect total lung capacity?
It reduces TLC by limiting chest wall movement.
80. Why is TLC important when evaluating unexplained dyspnea?
It helps identify restrictive or hyperinflated lungs.
81. Can TLC be normal in pulmonary vascular disease?
Yes, TLC may be normal while DLCO is reduced.
82. What does a normal TLC with reduced DLCO suggest?
Pulmonary vascular disease or anemia.
83. How does pregnancy affect total lung capacity?
TLC usually remains normal despite reduced FRC.
84. What happens to TLC during normal aging?
It gradually decreases due to reduced chest wall compliance.
85. Why must predicted TLC values be used instead of absolute values?
Because lung size varies with height, sex, age, and body size.
86. What percentage of predicted TLC is considered normal?
Approximately 80–120% of predicted.
87. What TLC value confirms restrictive lung disease?
A TLC less than 80% of predicted.
88. Can spirometry alone diagnose restrictive lung disease?
No, TLC must be measured to confirm restriction.
89. What happens to TLC in acute asthma exacerbation?
It may increase due to acute air trapping.
90. Why is TLC helpful in preoperative pulmonary assessment?
It helps estimate lung reserve and surgical risk.
91. What change in TLC would you expect after bronchodilator therapy in emphysema?
Minimal change, as hyperinflation often persists.
92. How does lung fibrosis affect TLC over time?
Progressive fibrosis leads to progressively lower TLC.
93. Why is TLC not routinely measured at the bedside?
It requires specialized equipment and patient cooperation.
94. What is functional lung size in critical illness?
The portion of the lung available for ventilation and gas exchange.
95. Why is functional lung size often reduced in ARDS?
Because alveoli collapse or fill with fluid despite normal predicted TLC.
96. How does hyperinflation increase the work of breathing?
By placing respiratory muscles at a mechanical disadvantage.
97. What clinical symptom is closely linked to increased TLC?
Exercise intolerance
98. How does posture influence TLC measurement?
TLC is highest when upright and lowest when supine.
99. Why must TLC results be repeatable?
To ensure accuracy and reliability of lung volume measurements.
100. What is the key clinical value of total lung capacity?
It defines lung size and distinguishes restrictive from obstructive disease.
Final Thoughts
Total lung capacity (TLC) is an essential measurement in respiratory physiology and pulmonary function testing. By representing the maximum volume of air the lungs can hold, it provides essential insight into lung mechanics, disease patterns, and respiratory limitations.
For respiratory therapists, understanding total lung capacity improves diagnostic accuracy, supports appropriate treatment decisions, and enhances patient education. When combined with spirometry and clinical assessment, TLC helps paint a complete picture of respiratory health in both acute and chronic care settings.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Delgado BJ, Bajaj T. Physiology, Lung Capacity. [Updated 2023 Jul 24]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025.


