Asthma is a chronic obstructive airway disease that affects breathing by causing airway inflammation, bronchial hyperreactivity, and episodes of bronchoconstriction. These changes make the airways narrower, which can lead to wheezing, shortness of breath, coughing, chest tightness, and increased work of breathing.
Asthma can range from mild and intermittent to severe and life-threatening. Although it cannot always be cured, it can often be controlled with proper assessment, medication, trigger management, patient education, and regular monitoring. Understanding asthma is important for students, respiratory therapists, clinicians, patients, and caregivers.
What Is Asthma?
Asthma is a chronic disease of the airways that causes variable airflow obstruction. The obstruction is usually caused by a combination of airway inflammation, bronchospasm, mucus production, and airway hyperresponsiveness. Unlike many other obstructive lung diseases, asthma is commonly associated with airflow limitation that is largely reversible with treatment.
This means that a patient with asthma may have significant airway narrowing during an attack, but their lung function may improve after receiving bronchodilator therapy or other appropriate treatment. This reversibility helps separate asthma from chronic obstructive pulmonary disease, or COPD, although the two conditions can overlap in some patients.
Asthma symptoms often occur in episodes. A patient may feel well for long periods, then develop sudden coughing, wheezing, or shortness of breath after exposure to a trigger. Symptoms may vary from day to day and are often worse at night or early in the morning.
Common asthma symptoms include:
- Wheezing
- Shortness of breath
- Chest tightness
- Coughing
- Increased work of breathing
- Difficulty speaking during severe attacks
- Nighttime or early morning symptoms
- Reduced exercise tolerance
Note: Asthma is not simply a problem of bronchospasm. It is also an inflammatory disease. This is why treatment often includes both quick-relief bronchodilators and long-term anti-inflammatory medications.
How Asthma Affects the Airways
In asthma, the airways become overly sensitive to certain triggers. When exposed to these triggers, the airways respond in an exaggerated way. This response may include contraction of the smooth muscle around the bronchi, swelling of the airway lining, and increased mucus production.
These changes narrow the airway lumen, making it harder for air to move in and out of the lungs. The patient may have difficulty exhaling because obstructive airway disease tends to limit expiratory airflow. Air can become trapped in the lungs, which may lead to hyperinflation and increased work of breathing.
The three major airway changes in asthma are:
- Airway inflammation
- Bronchoconstriction
- Mucus production
Airway inflammation makes the bronchial walls swollen and sensitive. Bronchoconstriction occurs when airway smooth muscle tightens, narrowing the airway. Mucus production can further block airflow, especially during an acute exacerbation.
Together, these changes produce the classic symptoms of asthma. During a mild episode, the patient may only have occasional wheezing or coughing. During a severe episode, the patient may have marked respiratory distress, poor air movement, hypoxemia, and signs of ventilatory failure.
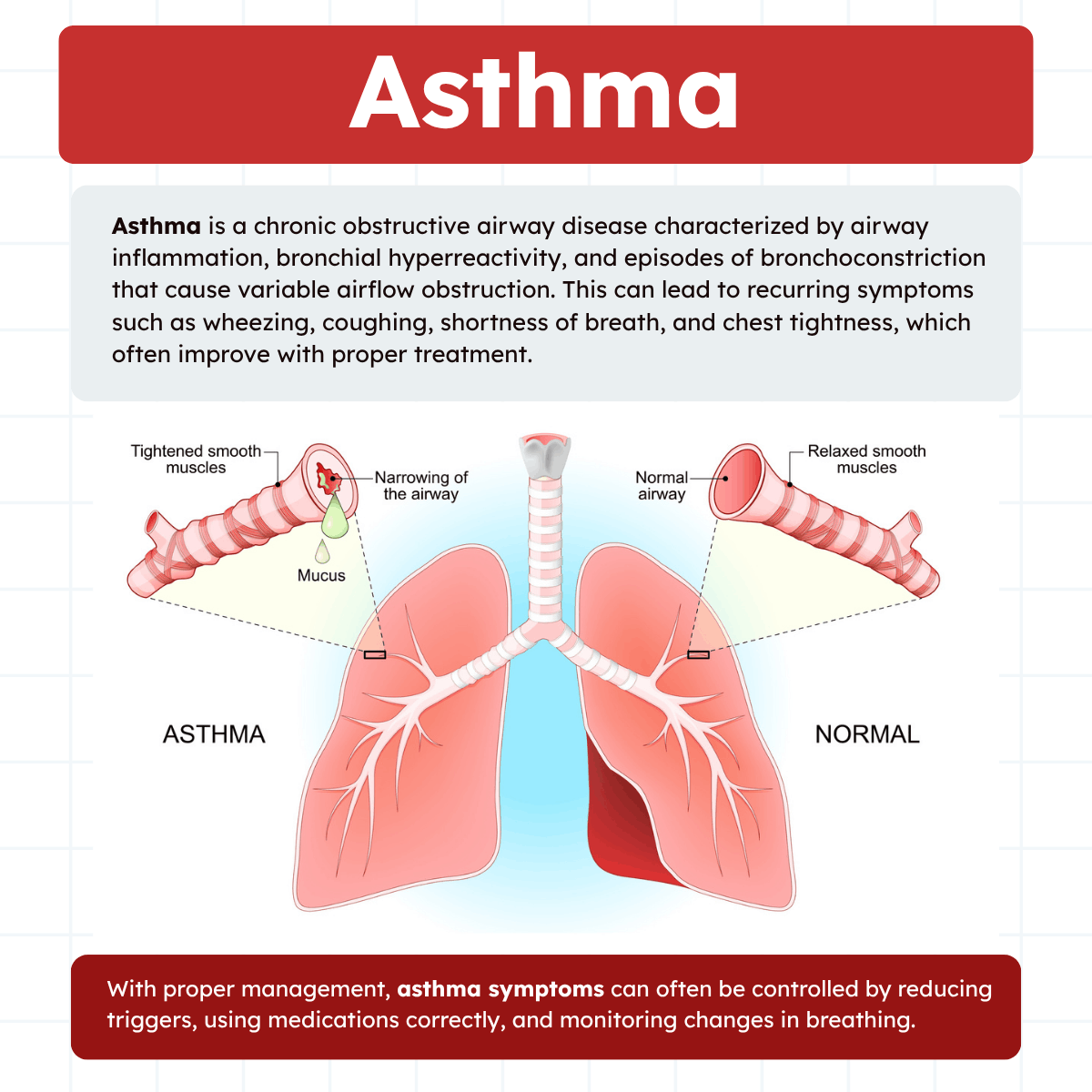
Airway Hyperreactivity in Asthma
Airway hyperreactivity means the airways respond too strongly to stimuli that would not cause major symptoms in a healthy person. For example, cold air, exercise, dust, smoke, pollen, or respiratory infections may trigger bronchospasm in a person with asthma.
This exaggerated response is one reason asthma symptoms can be unpredictable. A patient may tolerate one exposure without difficulty but develop severe symptoms during another exposure, especially if the airways are already inflamed.
Common asthma triggers include:
- Respiratory infections
- Allergens
- Exercise
- Cold air
- Tobacco smoke
- Air pollution
- Dust mites
- Mold
- Animal dander
- Strong odors or fumes
- Occupational exposures
- Certain medications
- Emotional stress
- Weather changes
Note: Not every patient has the same triggers. Part of asthma management is identifying what worsens the patient’s symptoms and helping the patient reduce exposure when possible.
Asthma vs. COPD
Asthma and COPD are both obstructive lung diseases, but they are not the same condition. Asthma often begins early in life and is commonly associated with allergies, rhinitis, eczema, or a family history of asthma. COPD usually begins later in life and is strongly associated with a history of tobacco smoking or long-term exposure to harmful inhaled particles.
Asthma symptoms tend to vary from day to day. They may occur at night, early in the morning, during exercise, or after exposure to a trigger. COPD symptoms are often more persistent and progressive over time. Patients with COPD commonly report chronic cough, sputum production, and exertional dyspnea.
The most important difference is reversibility. Asthma is usually associated with largely reversible airflow obstruction. COPD is usually associated with airflow limitation that is not fully reversible.
However, some patients do not fit neatly into one category. A patient with long-standing asthma may develop fixed airflow obstruction. A patient with COPD may also show bronchodilator responsiveness or features of asthma. This can make diagnosis and treatment more complex.
Asthma-COPD Overlap
Asthma-COPD overlap refers to patients who have features of both asthma and COPD. These patients may have persistent airflow limitation, a smoking history, bronchodilator responsiveness, peak flow variability, eosinophilia, elevated exhaled nitric oxide, or a history of allergies.
This overlap matters because treatment may need to include therapies commonly used for asthma, such as inhaled corticosteroids. In patients with asthma features, anti-inflammatory therapy is especially important because uncontrolled airway inflammation can increase the risk of exacerbations.
Note: Asthma-COPD overlap is not always easy to define, but clinicians should consider it when a patient has symptoms or test results that suggest both conditions.
Causes and Risk Factors
Asthma develops from a combination of genetic, environmental, immune, and airway factors. Some patients develop asthma in childhood, while others develop it later in life. The exact cause is not always clear.
Risk factors for asthma include:
- Family history of asthma
- Personal history of allergies
- Allergic rhinitis
- Eczema
- Exposure to tobacco smoke
- Air pollution
- Occupational exposure to dusts, chemicals, or fumes
- Respiratory infections during childhood
- Obesity
- Premature birth
- Exposure to indoor allergens
- Exercise-induced bronchoconstriction
- Viral respiratory infections
Asthma is commonly associated with allergic disease. Many patients with asthma also have allergic rhinitis or eczema. These conditions reflect an immune system that responds strongly to certain environmental exposures.
Occupational asthma is another important form. This occurs when workplace exposures trigger or cause asthma symptoms. Examples include chemical fumes, dusts, animal proteins, cleaning products, and industrial irritants. Identifying occupational asthma is important because symptoms may improve when exposure is reduced or eliminated.
Common Signs and Symptoms
Asthma symptoms can be mild, moderate, or severe. They may occur occasionally or daily, depending on the level of control and disease severity.
The most common symptoms are wheezing, coughing, shortness of breath, and chest tightness. Wheezing is a high-pitched sound caused by airflow through narrowed airways. Cough may be worse at night or early in the morning. Some patients have cough-variant asthma, where cough is the main symptom rather than wheezing.
Shortness of breath may occur during exercise, after exposure to triggers, during respiratory infections, or during acute attacks. Chest tightness may feel like pressure or discomfort across the chest.
During a severe asthma exacerbation, signs may include:
- Marked dyspnea
- Use of accessory muscles
- Retractions
- Tachypnea
- Tachycardia
- Difficulty speaking in full sentences
- Agitation or anxiety
- Fatigue
- Cyanosis
- Decreased breath sounds
- Silent chest
- Altered mental status
- Low oxygen saturation
- Rising PaCO₂
Note: A silent chest is especially concerning. It may mean that airflow is so limited that wheezing can no longer be heard. In a patient with severe distress, decreased breath sounds are more dangerous than loud wheezing.
Asthma Exacerbations
An asthma exacerbation is a worsening of asthma symptoms and airflow obstruction. Exacerbations may develop gradually over hours or days, or they may occur suddenly after exposure to a trigger.
Common causes of asthma exacerbations include respiratory infections, allergen exposure, poor medication adherence, incorrect inhaler technique, smoke exposure, exercise, and air pollution.
During an exacerbation, the therapist or clinician should assess severity quickly. Important findings include respiratory rate, heart rate, breath sounds, oxygen saturation, work of breathing, mental status, ability to speak, and response to initial bronchodilator therapy.
A mild exacerbation may improve after a short-acting bronchodilator. A moderate exacerbation may require repeated bronchodilator therapy and systemic corticosteroids. A severe exacerbation may require continuous bronchodilator therapy, oxygen, close monitoring, and possible ventilatory support.
Status Asthmaticus
Status asthmaticus is a severe asthma exacerbation that does not respond adequately to usual therapy. It is a medical emergency. Patients with status asthmaticus may have severe bronchospasm, airway inflammation, mucus plugging, hypoxemia, and progressive ventilatory failure.
Signs of status asthmaticus may include:
- Severe shortness of breath
- Poor air movement
- Use of accessory muscles
- Inability to speak full sentences
- Exhaustion
- Agitation or confusion
- Worsening hypoxemia
- Normal or rising PaCO₂
- Silent chest
- Poor response to bronchodilators
A rising PaCO₂ is a serious warning sign. Early in an asthma attack, the patient often hyperventilates, which lowers PaCO₂. If PaCO₂ becomes normal or elevated while the patient remains in distress, it may indicate fatigue and impending ventilatory failure.
Treatment of status asthmaticus usually includes aggressive bronchodilator therapy, systemic corticosteroids, oxygen as needed, continuous monitoring, and escalation to intensive care when necessary.
Diagnosis of Asthma
Asthma diagnosis is based on clinical history, symptoms, physical examination, pulmonary function testing, and response to therapy. No single finding proves asthma in every case, so the diagnosis is made by combining multiple pieces of information.
A typical asthma history may include episodic wheezing, shortness of breath, cough, or chest tightness. Symptoms may worsen at night, early in the morning, during exercise, or after exposure to triggers. The patient may also have allergies, eczema, allergic rhinitis, or a family history of asthma.
Physical examination may show wheezing, prolonged exhalation, tachypnea, or signs of increased work of breathing. However, the exam can be normal when the patient is not having symptoms.
Note: Pulmonary function testing is especially important because it can show airflow obstruction and reversibility after bronchodilator therapy.
Spirometry in Asthma
Spirometry is a key test used to evaluate airflow obstruction. In asthma, spirometry often shows a reduced forced expiratory volume in one second, or FEV₁, and a reduced FEV₁/FVC ratio. These findings suggest obstructive lung disease.
Bronchodilator response testing helps determine whether the obstruction improves after medication. An increase in FEV₁ of at least 12% and at least 200 mL after bronchodilator therapy supports the diagnosis of asthma in the correct clinical context.
Spirometry may also be used to monitor asthma control over time. A patient whose FEV₁ declines may have worsening obstruction, poor control, incorrect medication use, or an unresolved trigger exposure.
Peak Expiratory Flow Monitoring
Peak expiratory flow rate (PEFR) is a quick measurement of how fast a patient can exhale after a full inhalation. Peak flow monitoring is useful for asthma because it can detect worsening airflow obstruction before symptoms become severe.
Peak flow is often compared with the patient’s personal best value. The personal best is the highest peak flow the patient can achieve when asthma is well controlled. This value is then used to guide home monitoring and action plans.
A common traffic-light zone system includes green, yellow, and red zones. The green zone is 80% to 100% of the patient’s personal best. This usually means asthma is controlled. The patient should continue the usual treatment plan.
The yellow zone is 60% to 80% of personal best. This suggests caution. The patient may be developing worsening airway obstruction and may need a temporary step-up in therapy according to the asthma action plan.
The red zone is less than 60% of personal best. This is a medical alert. The patient may need immediate treatment and medical attention, especially if symptoms do not improve after rescue medication.
Note: Peak flow monitoring is especially helpful for patients with moderate to severe asthma, poor symptom perception, or a history of severe exacerbations.
Asthma Severity Classification
Asthma severity can be classified based on symptoms, nighttime awakenings, use of rescue medication, activity limitation, exacerbation frequency, and lung function.
Mild intermittent asthma usually involves symptoms that occur infrequently, with normal lung function between episodes. Mild persistent asthma involves symptoms more often than intermittent asthma, but not daily. Nighttime symptoms may occur occasionally.
Moderate persistent asthma involves daily symptoms, nighttime symptoms more than once per week, daily use of short-acting beta agonists, and some limitation of activity. FEV₁ or PEFR is often greater than 60% but less than 80% predicted.
Severe persistent asthma involves continuous symptoms, frequent exacerbations, frequent nighttime symptoms, activity limitation, and FEV₁ or PEFR at or below 60% predicted.
Note: Severity helps guide initial therapy. However, asthma management also depends on control. A patient’s classification may change over time based on symptoms, lung function, exacerbations, and response to treatment.
Asthma Control
Asthma control refers to how well the disease is managed at a given time. A patient may have severe asthma that is well controlled with treatment, or mild asthma that is poorly controlled because of poor adherence, incorrect inhaler technique, or ongoing trigger exposure.
Good asthma control usually means:
- Minimal daytime symptoms
- Minimal nighttime symptoms
- Little need for rescue medication
- Normal or near-normal activity
- Stable lung function
- Few or no exacerbations
- No emergency visits
- Proper medication use
Poor asthma control may involve frequent symptoms, frequent rescue inhaler use, nighttime awakenings, reduced activity, low peak flow values, or repeated exacerbations.
Frequent use of a rescue bronchodilator can be a warning sign. It may mean that airway inflammation is not controlled and that the maintenance treatment plan needs to be reassessed.
Treatment Goals
The main goals of asthma treatment are to reduce symptoms, maintain normal activity, prevent exacerbations, preserve lung function, reduce mortality risk, and minimize medication side effects.
Asthma treatment usually includes both quick-relief and long-term control strategies. Quick-relief medications treat acute bronchospasm. Long-term control medications reduce airway inflammation and help prevent future symptoms.
Note: Treatment should be individualized based on age, severity, control, triggers, comorbidities, medication technique, and patient preference.
Quick-Relief Medications
Quick-relief medications are used to relieve acute symptoms. The most common quick-relief drugs are short-acting beta agonists, such as albuterol and levalbuterol.
These medications relax airway smooth muscle, producing bronchodilation. They are fast acting and are commonly used during acute bronchospasm, exercise-induced symptoms, or asthma exacerbations.
Short-acting beta agonists may be delivered by metered dose inhaler, nebulizer, or other aerosol device. The best device depends on the patient’s age, coordination, inspiratory flow, severity of distress, and ability to use the device correctly.
Anticholinergic medications, such as ipratropium, may also be used in acute asthma, especially in moderate to severe exacerbations. Ipratropium blocks vagal reflexes and can add bronchodilator effect when combined with beta agonists.
Systemic corticosteroids are also used as quick-relief therapy during moderate to severe exacerbations, although they do not work as immediately as bronchodilators. They reduce airway inflammation and help prevent relapse.
Long-Term Control Medications
Long-term control medications are used to reduce airway inflammation, prevent symptoms, and lower the risk of exacerbations. These medications are taken regularly, even when the patient feels well.
Inhaled corticosteroids are the most important long-term control medications for many patients with persistent asthma. They reduce inflammation, decrease bronchial hyperreactivity, improve symptoms, reduce airflow obstruction, and lower the risk of severe outcomes.
Long-acting beta agonists may be used for maintenance therapy, but they should not be used alone in asthma. They must be combined with inhaled corticosteroids because using long-acting beta agonists without anti-inflammatory therapy can increase the risk of asthma-related death.
Note: Other long-term control medications include leukotriene modifiers, methylxanthines, long-acting antimuscarinic agents, and biologic therapies for selected patients.
Inhaled Corticosteroids
Inhaled corticosteroids are commonly used as first-line therapy for persistent asthma. They target the inflammatory process that drives airway hyperreactivity and recurrent symptoms.
Benefits of inhaled corticosteroids include:
- Reduced airway inflammation
- Decreased bronchial hyperreactivity
- Improved lung function
- Fewer symptoms
- Fewer exacerbations
- Reduced need for rescue medication
- Lower risk of asthma-related death
Although inhaled corticosteroids have fewer systemic effects than oral corticosteroids, side effects can occur. Local side effects include oropharyngeal candidiasis and dysphonia. These can often be reduced by using a spacer with a metered dose inhaler and rinsing the mouth after use.
Note: Long-term high-dose therapy may be associated with other risks, such as bruising, glaucoma, or cataracts. The goal is to use the lowest effective dose that maintains control.
Oral and Intravenous Corticosteroids
Systemic corticosteroids are important during moderate to severe asthma exacerbations. They reduce the severity and duration of exacerbations, decrease the risk of hospitalization, and help prevent relapse after emergency treatment.
Systemic corticosteroids may be given orally or intravenously, depending on the severity of illness and the patient’s ability to take oral medication.
However, long-term oral corticosteroid use should generally be avoided when possible because of significant side effects. These may include osteoporosis, adrenal suppression, immunosuppression, skin bruising, weight gain, hyperglycemia, glaucoma, and cataracts.
Note: In patients with severe asthma who require frequent oral corticosteroids, clinicians may consider advanced therapies such as biologic medications.
Beta Agonists
Beta agonists are bronchodilators that relax airway smooth muscle. Short-acting beta agonists are used for acute relief, while long-acting beta agonists are used for maintenance therapy in combination with inhaled corticosteroids.
Albuterol and levalbuterol are common short-acting beta agonists. They work quickly and are highly effective for acute bronchospasm.
Long-acting beta agonists help maintain bronchodilation over a longer period. However, they do not treat airway inflammation by themselves. This is why they must be paired with inhaled corticosteroids in asthma management.
Note: Possible side effects of beta agonists include tachycardia, tremor, nervousness, palpitations, and hypokalemia. During severe exacerbations or continuous nebulization, close monitoring may be needed.
Leukotriene Modifiers
Leukotriene modifiers target inflammatory mediators involved in asthma. Examples include montelukast, zafirlukast, and zileuton.
These medications may be used for maintenance therapy in mild to moderate asthma. They may also help some patients with exercise-induced bronchoconstriction or allergic asthma.
Leukotriene modifiers do not directly cause bronchodilation, so they are not used as rescue medications during acute bronchospasm. Their role is preventive and anti-inflammatory.
Methylxanthines
Theophylline and aminophylline are methylxanthine drugs that have bronchodilator effects. Historically, they were used more often in asthma care. Today, they are used less frequently because safer and more effective options are available.
Methylxanthines have a narrow therapeutic range, which means the difference between a helpful dose and a toxic dose can be small. Side effects may include nausea, vomiting, tachycardia, tachypnea, nervousness, central nervous system stimulation, arrhythmias, and diuresis.
Current asthma management generally does not use theophylline or aminophylline as routine first-line therapy for exacerbations. Short-acting beta agonists, anticholinergics, and corticosteroids are usually preferred.
Antimuscarinic Agents
Antimuscarinic agents help produce bronchodilation by blocking parasympathetic pathways that contribute to airway narrowing.
Ipratropium is a short-acting antimuscarinic often used with beta agonists during moderate to severe asthma exacerbations. It may provide additional bronchodilation and improve response in acute care settings.
Tiotropium is a long-acting antimuscarinic that may be added to inhaled corticosteroid therapy in some patients with uncontrolled asthma. It can help improve asthma control in selected cases.
Note: These medications do not replace inhaled corticosteroids because they do not address the primary inflammatory process in asthma.
Biologic Therapy for Severe Asthma
Some patients have severe asthma that remains poorly controlled despite standard therapy. These patients may benefit from biologic medications that target specific immune pathways.
Omalizumab is an anti-IgE antibody used in selected patients with allergic asthma. IgE plays an important role in allergic inflammation, and blocking IgE can reduce exacerbations and decrease the need for other medications in certain patients.
Other biologic therapies target eosinophilic inflammation. IL-5 promotes eosinophil activity, which contributes to airway inflammation in some forms of asthma. Medications such as mepolizumab, reslizumab, and benralizumab target IL-5 or its receptor. These may reduce exacerbations and oral corticosteroid use in patients with severe eosinophilic asthma.
Note: Biologic therapy is not for every asthma patient. It is usually reserved for patients with severe disease, specific inflammatory markers, and poor control despite appropriate standard therapy.
Aerosol Therapy in Asthma
Because asthma affects the airways, inhaled therapy is often preferred when possible. Inhaled medications deliver drug directly to the site of disease while limiting systemic exposure.
Common aerosol devices include:
- Metered dose inhalers
- Dry powder inhalers
- Small-volume nebulizers
- Soft mist inhalers
- Spacers and holding chambers
The device must match the patient’s ability. A patient must be able to coordinate inhalation with actuation when using a standard metered dose inhaler. A spacer can make this easier and improve drug delivery. A dry powder inhaler requires adequate inspiratory flow. A nebulizer may be useful during acute distress or for patients who cannot coordinate inhaler technique.
Note: Incorrect inhaler technique is a common cause of poor asthma control. Respiratory therapists play an important role in teaching and assessing inhaler use.
Oxygen Therapy in Acute Asthma
Oxygen may be needed during an acute asthma exacerbation if the patient is hypoxemic. The goal is to correct low oxygen saturation while treating the underlying airflow obstruction.
Oxygen does not reverse bronchospasm or inflammation. Therefore, it should be used along with bronchodilators, corticosteroids, and other indicated therapies.
The respiratory therapist should monitor oxygen saturation, clinical appearance, work of breathing, and response to therapy. In severe cases, arterial blood gases may be needed to assess ventilation and acid-base status.
Heliox in Asthma
Heliox is a mixture of helium and oxygen. Because helium is less dense than nitrogen, heliox can reduce airway resistance and improve gas flow through narrowed airways.
In asthma, heliox may be used in selected severe obstructive cases to reduce work of breathing while other therapies take effect. It does not directly treat inflammation or bronchospasm, so it is not a replacement for bronchodilators or corticosteroids.
Note: Heliox requires correct delivery equipment and flow adjustments because standard flowmeters may not read accurately with helium mixtures.
Mechanical Ventilation in Severe Asthma
Most asthma exacerbations improve with medical therapy, but some patients develop respiratory failure and require ventilatory support. This is more likely in status asthmaticus, severe fatigue, altered mental status, worsening hypoxemia, or rising PaCO₂.
Mechanical ventilation in asthma requires caution because severe airflow obstruction increases the risk of air trapping, dynamic hyperinflation, and auto-PEEP. Ventilator settings often need to allow enough time for exhalation. High respiratory rates, large tidal volumes, or short expiratory times may worsen air trapping.
Note: The goal is to support ventilation while avoiding excessive airway pressures and further hyperinflation. These patients require close monitoring by the respiratory therapist and clinical team.
Pediatric Asthma
Asthma is common in children and may present differently than in adults. Children may have wheezing, coughing, shortness of breath, poor feeding, reduced activity, or symptoms that worsen with viral infections.
Because children have smaller airways, even mild swelling or mucus can significantly increase airway resistance. This means pediatric patients can deteriorate quickly during severe attacks.
Signs of respiratory distress in children include:
- Nasal flaring
- Retractions
- Tachypnea
- Grunting
- Wheezing
- Poor air movement
- Agitation
- Lethargy
- Cyanosis
- Low oxygen saturation
In severe pediatric asthma, continuous bronchodilator therapy, systemic corticosteroids, ICU monitoring, and ventilatory support may be necessary.
Patient and caregiver education is especially important in pediatric asthma. Caregivers must understand medication schedules, inhaler technique, spacer use, trigger avoidance, and when to seek emergency care.
Exercise-Induced Bronchoconstriction
Some patients develop asthma symptoms during or after exercise. This is called exercise-induced bronchoconstriction. Symptoms may include coughing, wheezing, chest tightness, or shortness of breath.
Exercise-induced symptoms do not mean the patient should avoid physical activity completely. Instead, the goal is to manage asthma so the patient can remain active safely.
Strategies may include pre-treatment with a short-acting bronchodilator, warm-up periods, avoiding exercise in cold dry air, and improving long-term asthma control when symptoms are frequent.
Patient Education
Patient education is one of the most important parts of asthma care. A patient who understands asthma is more likely to use medications correctly, recognize worsening symptoms, avoid triggers, and seek care when needed.
Asthma education should include:
- Difference between rescue and controller medications
- Correct inhaler technique
- Spacer or holding chamber use
- Nebulizer use and cleaning
- Trigger identification and avoidance
- Peak flow monitoring
- Asthma action plan instructions
- Early signs of worsening asthma
- When to seek emergency care
- Importance of follow-up visits
- Smoking cessation when applicable
- Medication adherence
Note: Patients should understand that rescue medications provide quick relief but do not control airway inflammation. Controller medications, especially inhaled corticosteroids, help prevent symptoms and exacerbations over time.
Asthma Action Plans
An asthma action plan is a written plan that tells the patient what to do based on symptoms and peak flow values. It usually includes green, yellow, and red zones.
The green zone means asthma is controlled. The patient continues routine medications. The yellow zone means symptoms or peak flow values are worsening. The patient may need rescue medication or a temporary step-up in therapy.
The red zone means the patient is in danger. Severe symptoms, very low peak flow, difficulty speaking, cyanosis, confusion, or poor response to rescue medication should prompt urgent medical care.
Note: Asthma action plans are especially useful for patients with moderate to severe asthma, previous hospitalizations, poor symptom awareness, or frequent exacerbations.
Discharge Criteria After an Asthma Exacerbation
After an asthma exacerbation is controlled, the patient should be assessed carefully before discharge. Important criteria may include stable oxygenation, improved symptoms, stable lung function, and the ability to continue treatment safely outside the hospital.
A patient may be ready for discharge when supplemental oxygen is no longer needed, PaO₂ is greater than 60 mm Hg when measured, PEFR or FEV₁ is stable and close to the patient’s best or greater than 70% predicted, symptoms are returning to baseline, nighttime symptoms are absent, and the patient has remained stable on discharge medications.
Note: Before discharge, the patient should understand medication instructions, inhaler technique, follow-up plans, and warning signs that require urgent care.
Role of the Respiratory Therapist
Respiratory therapists play a major role in asthma care across many settings. They may care for asthma patients in the emergency department, hospital, ICU, outpatient clinic, pulmonary function lab, home care setting, and pulmonary rehabilitation program.
The respiratory therapist’s responsibilities may include:
- Assessing breath sounds and work of breathing
- Measuring oxygen saturation
- Performing spirometry or peak flow testing
- Administering aerosolized medications
- Choosing appropriate aerosol devices
- Teaching inhaler technique
- Monitoring response to bronchodilator therapy
- Recognizing signs of respiratory failure
- Assisting with oxygen therapy
- Supporting mechanical ventilation when needed
- Providing smoking cessation education
- Teaching peak flow monitoring
- Reinforcing asthma action plans
- Helping patients understand medications
Note: For exam purposes, respiratory therapy students should focus on assessment, treatment selection, monitoring, and escalation of care. Asthma questions often test whether the therapist can recognize severity and choose the most appropriate next step.
Asthma and Exam Preparation
Asthma is a high-yield topic for respiratory therapy exams because it connects many important areas: assessment, pharmacology, pulmonary function testing, aerosol therapy, oxygen therapy, emergency care, pediatric care, and mechanical ventilation.
Students should understand that asthma management depends on severity. A mild case may require bronchodilator therapy and reassessment. A moderate case may require repeated bronchodilators and systemic corticosteroids. A severe case may require continuous aerosol therapy, oxygen, monitoring, ICU care, and possible ventilatory support.
Important exam points include:
- Asthma is usually reversible obstructive disease
- FEV₁ and FEV₁/FVC are reduced during obstruction
- Bronchodilator response supports the diagnosis
- Peak flow helps monitor control and worsening obstruction
- Short-acting beta agonists are key rescue bronchodilators
- Inhaled corticosteroids are central for long-term control
- Long-acting beta agonists should not be used alone in asthma
- Systemic corticosteroids are used for moderate to severe exacerbations
- Theophylline and aminophylline are not routine first-line choices for exacerbations
- A normal or rising PaCO₂ during severe distress is dangerous
- Silent chest may indicate life-threatening obstruction
- Reassessment after treatment is required
- Device selection must match the patient’s ability
- Severe pediatric asthma can deteriorate quickly
Note: In exam scenarios, the best answer is usually the action that treats bronchospasm, reduces inflammation, improves oxygenation, monitors response, or prevents deterioration.
Common Mistakes in Asthma Care
Several mistakes can lead to poor asthma control or delayed treatment. One common mistake is relying only on rescue bronchodilators while ignoring airway inflammation. Frequent albuterol use may temporarily relieve symptoms, but it does not treat the inflammatory process.
Another mistake is poor inhaler technique. A patient may be prescribed the correct medication but receive little benefit if the device is used incorrectly. This is why technique should be reviewed regularly.
A third mistake is failing to reassess after treatment. Giving a bronchodilator is not enough. The clinician must determine whether the patient improved by checking breath sounds, respiratory rate, oxygen saturation, work of breathing, peak flow, and overall appearance.
A fourth mistake is missing signs of impending respiratory failure. A patient who becomes quiet, confused, exhausted, or has reduced breath sounds may be worsening even if wheezing is less noticeable.
Prevention and Long-Term Management
Asthma prevention focuses on reducing exacerbations and maintaining control. This requires consistent medication use, trigger management, monitoring, and follow-up.
Long-term management may include:
- Using controller medications as prescribed
- Keeping rescue medication available
- Avoiding known triggers
- Treating allergic rhinitis or other comorbidities
- Receiving recommended vaccinations
- Avoiding tobacco smoke
- Monitoring peak flow when indicated
- Following a written asthma action plan
- Reviewing inhaler technique regularly
- Seeking care early when symptoms worsen
Note: Asthma control can change over time, so treatment plans should be reassessed regularly. A patient who is doing well may need less medication in some cases, while a patient with worsening symptoms may need a step-up in therapy.
When Asthma Becomes an Emergency
Asthma can become life-threatening when airflow obstruction is severe and the patient cannot maintain oxygenation or ventilation.
Emergency warning signs include:
- Severe shortness of breath
- Inability to speak full sentences
- Blue lips or fingernails
- Confusion or drowsiness
- Severe retractions
- Silent chest
- Poor response to rescue medication
- Peak flow in the red zone
- Worsening oxygen saturation
- Normal or elevated PaCO₂ during severe distress
Note: These signs require immediate medical attention. Delayed treatment can lead to respiratory failure, cardiac arrest, and death.
Asthma Practice Questions
1. What is asthma?
Asthma is a chronic respiratory disorder characterized by airway inflammation, bronchial hyperresponsiveness, reversible airflow obstruction, and recurring episodes of wheezing, coughing, chest tightness, and shortness of breath.
2. What are the main pathophysiologic features of asthma?
The main features are airway inflammation, bronchoconstriction, airway hyperresponsiveness, mucus production, and variable airflow obstruction.
3. What does airway hyperresponsiveness mean?
Airway hyperresponsiveness means the airways overreact to triggers, causing bronchoconstriction, bronchospasm, mucosal swelling, and increased mucus production.
4. What causes airflow obstruction in asthma?
Airflow obstruction occurs due to bronchoconstriction, airway edema, mucus plugging, and inflammation of the bronchial walls.
5. Is asthma usually reversible or irreversible?
Asthma is usually reversible, either spontaneously or with treatment, although chronic poorly controlled asthma can lead to airway remodeling and more persistent obstruction.
6. What are the most common symptoms of asthma?
Common symptoms include coughing, wheezing, chest tightness, shortness of breath, and episodes of increased work of breathing.
7. When are asthma symptoms often worse?
Asthma symptoms are often worse at night, early in the morning, during exercise, after exposure to triggers, or during respiratory infections.
8. What is wheezing?
Wheezing is a high-pitched musical breath sound caused by airflow through narrowed airways.
9. Is wheezing always present during an asthma attack?
No. Wheezing may be absent in severe asthma if airflow is extremely limited, which can indicate a life-threatening situation.
10. What does a silent chest suggest in a patient with severe asthma?
A silent chest suggests minimal air movement and may indicate impending respiratory failure.
Access our quiz with sample TMC practice questions and detailed explanations to help you master the key concepts of pathology.
11. What are common signs of an asthma exacerbation?
Signs include tachypnea, wheezing, coughing, accessory muscle use, prolonged expiration, retractions, increased heart rate, decreased oxygen saturation, and difficulty speaking in full sentences.
12. What is prolonged expiration in asthma?
Prolonged expiration occurs because narrowed airways make it harder for the patient to exhale, leading to air trapping.
13. Why does air trapping occur in asthma?
Air trapping occurs when narrowed airways prevent complete exhalation before the next breath begins.
14. What is dynamic hyperinflation?
Dynamic hyperinflation occurs when air trapping causes the lungs to remain overinflated during breathing, increasing the work of breathing.
15. What are common asthma triggers?
Common triggers include allergens, respiratory infections, exercise, cold air, smoke, air pollution, strong odors, occupational exposures, stress, GERD, and certain medications.
16. What are common allergic triggers for asthma?
Common allergic triggers include pollen, mold, animal dander, dust mites, and cockroach droppings.
17. What are common irritant triggers for asthma?
Common irritants include tobacco smoke, wood smoke, air pollution, ozone, chemical fumes, perfumes, household cleaners, paint, and cooking fumes.
18. What is the difference between an allergen and an irritant?
An allergen causes symptoms in people who are sensitized to that substance, while an irritant can affect anyone if the exposure is strong enough.
19. What is extrinsic asthma?
Extrinsic asthma is allergic asthma that is triggered by allergens and is often associated with IgE-mediated inflammation.
20. What is intrinsic asthma?
Intrinsic asthma is nonallergic asthma that may be triggered by factors such as respiratory infections, stress, cold air, smoke, exercise, or irritants.
21. What is atopy?
Atopy is a genetic tendency to develop allergic conditions through an IgE-mediated immune response.
22. What is the strongest predisposing factor for asthma?
Atopy is considered the strongest predisposing factor for asthma.
23. What role does IgE play in allergic asthma?
IgE binds to allergens and triggers mast cell activation, which releases inflammatory mediators that cause bronchoconstriction, mucus production, and airway edema.
24. What happens when inflammatory mediators are released in asthma?
Inflammatory mediators cause bronchoconstriction, airway inflammation, mucosal edema, increased mucus production, and increased airway responsiveness.
25. Which white blood cell is commonly associated with allergic asthma?
Eosinophils are commonly associated with allergic asthma and eosinophilic airway inflammation.
26. What is eosinophilic asthma?
Eosinophilic asthma is a type of asthma characterized by elevated eosinophils and airway inflammation that often responds well to corticosteroids or selected biologic therapies.
27. What is exercise-induced bronchoconstriction?
Exercise-induced bronchoconstriction is airway narrowing that occurs during or after exercise, causing coughing, wheezing, chest tightness, or shortness of breath.
28. How can exercise-induced bronchoconstriction be managed?
It can be managed by warming up before exercise, avoiding cold dry air when possible, and using a prescribed short-acting bronchodilator before activity.
29. What is nocturnal asthma?
Nocturnal asthma refers to asthma symptoms that worsen at night and may interrupt sleep.
30. Why can respiratory infections worsen asthma?
Respiratory infections can increase airway inflammation, mucus production, and bronchial hyperresponsiveness, which may trigger an asthma exacerbation.
31. How can GERD worsen asthma symptoms?
GERD may worsen asthma by causing microaspiration or reflex bronchoconstriction when acid irritates the esophagus.
32. How can obesity affect asthma control?
Obesity can worsen asthma control by increasing respiratory workload, reducing lung volumes, and contributing to systemic inflammation.
33. How can cold air trigger asthma?
Cold, dry air can irritate the airways and cause bronchoconstriction in susceptible patients.
34. What medications can worsen asthma in some patients?
Aspirin, NSAIDs, and nonselective beta-blockers can worsen asthma in some patients.
35. What is aspirin-exacerbated respiratory disease?
Aspirin-exacerbated respiratory disease is a condition in which aspirin or NSAIDs trigger asthma symptoms, often in patients with chronic sinus disease and nasal polyps.
36. What is occupational asthma?
Occupational asthma is asthma caused or worsened by workplace exposures such as dust, fumes, vapors, gases, chemicals, or allergens.
37. How is occupational asthma suspected?
It is suspected when asthma symptoms worsen at work and improve on days off, weekends, or vacations.
38. What are the vital sign changes during an asthma exacerbation?
Patients may have an increased respiratory rate, increased heart rate, elevated blood pressure early in the attack, and decreased oxygen saturation in more severe cases.
39. What is pulsus paradoxus?
Pulsus paradoxus is an exaggerated decrease in systolic blood pressure during inspiration, typically greater than 10 mmHg.
40. Why can pulsus paradoxus occur during a severe asthma attack?
It can occur because severe air trapping and large intrathoracic pressure swings affect venous return and cardiac filling during inspiration.
41. What does peak expiratory flow measure?
Peak expiratory flow measures the highest flow rate a patient can generate during a forceful exhalation.
42. How can a peak flow meter help manage asthma?
A peak flow meter can help monitor airway obstruction, detect worsening asthma early, and guide an asthma action plan.
43. What does spirometry show in asthma?
Spirometry may show airflow obstruction with a decreased FEV1 and a decreased FEV1/FVC ratio.
44. What spirometry finding supports reversible airflow obstruction?
An increase in FEV1 after bronchodilator administration supports reversible airflow obstruction.
45. What happens to residual volume in asthma?
Residual volume may increase due to air trapping.
46. What may happen to FVC during an asthma exacerbation?
FVC may decrease because air trapping prevents complete exhalation.
47. What is a methacholine challenge test?
A methacholine challenge test assesses airway hyperresponsiveness and may help diagnose asthma when baseline spirometry is normal but symptoms suggest asthma.
48. What does a positive methacholine challenge test suggest?
A positive test suggests airway hyperresponsiveness, which supports the diagnosis of asthma when interpreted with the clinical picture.
49. What is the FeNO test?
The fractional exhaled nitric oxide test measures nitric oxide in exhaled breath as a marker of eosinophilic airway inflammation.
50. How can FeNO testing be useful in asthma?
FeNO can help identify eosinophilic inflammation and may help guide inhaled corticosteroid therapy in selected patients.
51. What chest x-ray findings are common in asthma?
A chest x-ray may be normal or may show hyperinflation due to air trapping during an exacerbation.
52. Why is a chest x-ray not always required for asthma?
Asthma is primarily diagnosed clinically and with lung function testing, while chest x-ray is usually reserved for atypical findings, complications, or alternative diagnoses.
53. What ABG pattern is common during a mild asthma exacerbation?
ABG results may show respiratory alkalosis due to hyperventilation, with a low PaCO2 and increased pH.
54. What ABG pattern may occur during a severe asthma exacerbation?
A severe exacerbation may show hypoxemia, rising PaCO2, and respiratory acidosis, indicating fatigue and possible respiratory failure.
55. Why is a rising PaCO2 dangerous during an asthma attack?
A rising PaCO2 suggests the patient is tiring and no longer ventilating adequately, which may signal impending respiratory failure.
56. What is status asthmaticus?
Status asthmaticus is a severe asthma exacerbation that does not respond adequately to initial bronchodilator therapy and can progress to respiratory failure.
57. What are warning signs of life-threatening asthma?
Warning signs include a silent chest, altered mental status, cyanosis, exhaustion, bradycardia, severe hypoxemia, rising PaCO2, and inability to speak.
58. When may intubation be required during an asthma exacerbation?
Intubation may be required for respiratory failure, altered mental status, severe hypoxemia, exhaustion, or inability to protect the airway.
59. Why must mechanical ventilation be used carefully in severe asthma?
Mechanical ventilation must be used carefully because air trapping and dynamic hyperinflation increase the risk of barotrauma and hypotension.
60. What is the first step in asthma management when possible?
The first step is prevention by identifying and avoiding triggers whenever possible.
61. What is an asthma action plan?
An asthma action plan is a written, personalized plan that explains daily treatment, how to recognize worsening symptoms, and what steps to take during an exacerbation.
62. What are the goals of asthma management?
The goals are to prevent symptoms, maintain normal activity, preserve lung function, prevent exacerbations, reduce emergency visits, and minimize medication side effects.
63. What are rescue medications?
Rescue medications are quick-relief drugs used to treat acute asthma symptoms or exacerbations.
64. What are controller medications?
Controller medications are taken regularly to reduce airway inflammation, prevent symptoms, and lower the risk of exacerbations.
65. What are examples of quick-relief medications for asthma?
Examples include short-acting beta-2 agonists such as albuterol and levalbuterol, and inhaled anticholinergics such as ipratropium in selected exacerbations.
66. How do short-acting beta-2 agonists work?
Short-acting beta-2 agonists relax bronchial smooth muscle, producing rapid bronchodilation.
67. What is albuterol used for in asthma?
Albuterol is used as a quick-relief bronchodilator to treat acute bronchoconstriction and relieve wheezing, coughing, and shortness of breath.
68. What is levalbuterol?
Levalbuterol, also known as Xopenex, is a short-acting beta-2 agonist used for bronchodilation in asthma and other obstructive airway disorders.
69. How do anticholinergics help during asthma exacerbations?
Anticholinergics block muscarinic receptors, reduce vagal-mediated bronchoconstriction, and can provide additional bronchodilation when used with beta-2 agonists.
70. What is ipratropium bromide used for in asthma?
Ipratropium bromide may be added during moderate to severe asthma exacerbations to improve bronchodilation.
71. What are inhaled corticosteroids used for in asthma?
Inhaled corticosteroids reduce airway inflammation and are among the most important controller medications for persistent asthma.
72. What are common side effects of inhaled corticosteroids?
Common side effects include hoarseness and oral thrush, which can be reduced by using a spacer and rinsing the mouth after use.
73. What are systemic corticosteroids used for in asthma?
Systemic corticosteroids are used for moderate to severe exacerbations or poorly controlled asthma to reduce airway inflammation.
74. What are long-acting beta-2 agonists?
Long-acting beta-2 agonists are bronchodilators used for long-term control, typically in combination with inhaled corticosteroids.
75. Why should long-acting beta-2 agonists not be used alone for asthma control?
They should not be used alone because they do not treat underlying airway inflammation and may increase risk when used without inhaled corticosteroids.
76. What are leukotriene receptor antagonists?
Leukotriene receptor antagonists, such as montelukast, block leukotrienes that contribute to bronchoconstriction, airway edema, mucus production, and inflammation.
77. What is montelukast used for?
Montelukast is used as a controller medication for asthma, allergic rhinitis, and exercise-induced bronchoconstriction in selected patients.
78. What are mast cell stabilizers?
Mast cell stabilizers, such as cromolyn and nedocromil, help prevent mediator release from mast cells and are used less commonly today.
79. What are methylxanthines?
Methylxanthines, such as theophylline, are bronchodilators that can relax airway smooth muscle but require careful monitoring due to side effects and toxicity risk.
80. What is magnesium sulfate used for in asthma?
Intravenous magnesium sulfate may be used as an adjunct therapy in severe asthma exacerbations that do not respond adequately to initial treatment.
81. What is heliox therapy?
Heliox is a helium-oxygen mixture that may reduce airway resistance and work of breathing in selected patients with severe airflow obstruction.
82. What are biologic medications used for in asthma?
Biologic medications are used for selected patients with moderate to severe asthma, especially allergic or eosinophilic asthma that remains uncontrolled despite standard therapy.
83. What is omalizumab?
Omalizumab is an anti-IgE biologic medication used for selected patients with moderate to severe allergic asthma.
84. When may omalizumab be considered?
Omalizumab may be considered for patients with moderate to severe persistent allergic asthma who remain symptomatic despite appropriate inhaled controller therapy.
85. What is the step-up approach in asthma management?
The step-up approach increases treatment intensity when asthma is not well controlled.
86. What is the step-down approach in asthma management?
The step-down approach reduces treatment intensity after asthma has been well controlled for a sustained period, using the minimum therapy needed to maintain control.
87. What are the traditional severity categories of asthma?
Traditional categories include intermittent, mild persistent, moderate persistent, and severe persistent asthma.
88. What is the “rule of 2” in asthma control?
Asthma may be poorly controlled if the patient uses a rescue inhaler more than 2 days per week, wakes with symptoms more than 2 nights per month, or uses more than 2 rescue inhaler canisters per year.
89. What is the difference between asthma control and asthma severity?
Asthma control refers to how well symptoms and risk are managed currently, while asthma severity reflects the level of treatment needed to maintain control.
90. What is the difference between asthma and COPD?
Asthma is usually characterized by variable and reversible airflow obstruction, while COPD is typically progressive and less reversible, often related to long-term exposure to irritants such as cigarette smoke.
91. What is the difference between asthma and croup?
Asthma affects the lower airways and causes wheezing and bronchoconstriction, while croup is usually a viral upper airway disorder that causes a barking cough and inspiratory stridor.
92. What is the role of oxygen therapy during an asthma exacerbation?
Oxygen therapy is used when the patient has hypoxemia or significant respiratory distress to maintain adequate oxygenation.
93. Why is patient education important in asthma?
Patient education helps patients recognize triggers, use inhalers correctly, follow the asthma action plan, monitor symptoms, and seek care when symptoms worsen.
94. Why is inhaler technique important in asthma management?
Poor inhaler technique can reduce medication delivery to the lungs and lead to poor asthma control.
95. How can a spacer help with asthma inhaler use?
A spacer improves medication delivery from a metered-dose inhaler and reduces medication deposition in the mouth and throat.
96. What role do vaccinations play in asthma management?
Vaccinations can help prevent respiratory infections that may trigger asthma exacerbations.
97. Can children outgrow asthma?
Some children may have fewer symptoms as they grow older, but asthma can persist into adulthood or return later in life.
98. How can environmental control help asthma?
Environmental control reduces exposure to triggers such as tobacco smoke, dust mites, mold, pet dander, pollen, and indoor pollutants.
99. What are the risks of undertreating asthma?
Undertreating asthma can lead to frequent symptoms, severe exacerbations, declining lung function, airway remodeling, emergency visits, and potentially fatal attacks.
100. What is the key concept to remember about asthma?
Asthma is a chronic inflammatory airway disease with variable airflow obstruction, so effective care focuses on trigger control, anti-inflammatory therapy, rescue treatment, monitoring, and early recognition of worsening symptoms.
Final Thoughts
Asthma is a chronic obstructive airway disease marked by inflammation, airway hyperreactivity, and usually reversible airflow obstruction. It can cause mild episodic symptoms or severe life-threatening exacerbations. Effective asthma care requires accurate assessment, proper medication selection, correct aerosol delivery, trigger management, patient education, and careful monitoring of response.
For respiratory therapists, asthma is especially important because it involves bedside assessment, pulmonary function testing, bronchodilator therapy, oxygen therapy, patient teaching, and emergency decision-making. The key is to recognize severity early, treat bronchospasm and inflammation appropriately, reassess often, and escalate care when the patient is not improving.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Goldin J, Cataletto ME. Asthma. [Updated 2024 May 3]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026.
- Sinyor B, Concepcion Perez L. Pathophysiology Of Asthma. [Updated 2023 Jun 24]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026.


