A metered-dose inhaler (MDI) is a widely used device for delivering aerosolized medications directly into the lungs. It plays an essential role in the treatment of respiratory conditions such as asthma and chronic obstructive pulmonary disease (COPD).
By providing a precise, premeasured dose of medication with each actuation, MDIs offer a reliable and efficient method of drug delivery. However, their effectiveness depends heavily on proper technique, coordination, and patient understanding.
This article provides a comprehensive overview of MDIs, including how they work, their advantages and limitations, and their role in clinical practice.
What Is a Metered-Dose Inhaler?
A metered-dose inhaler, often referred to as a pressurized metered-dose inhaler (pMDI), is a handheld device designed to deliver a specific amount of medication to the respiratory tract in aerosol form. Each time the inhaler is activated, it releases a fixed dose of medication, ensuring consistency and accuracy.
MDIs are commonly used to administer medications such as bronchodilators, corticosteroids, and combination therapies. These medications are essential for both the acute relief and long-term management of respiratory diseases. Because of their portability and ease of use, MDIs are frequently prescribed for home and outpatient use.
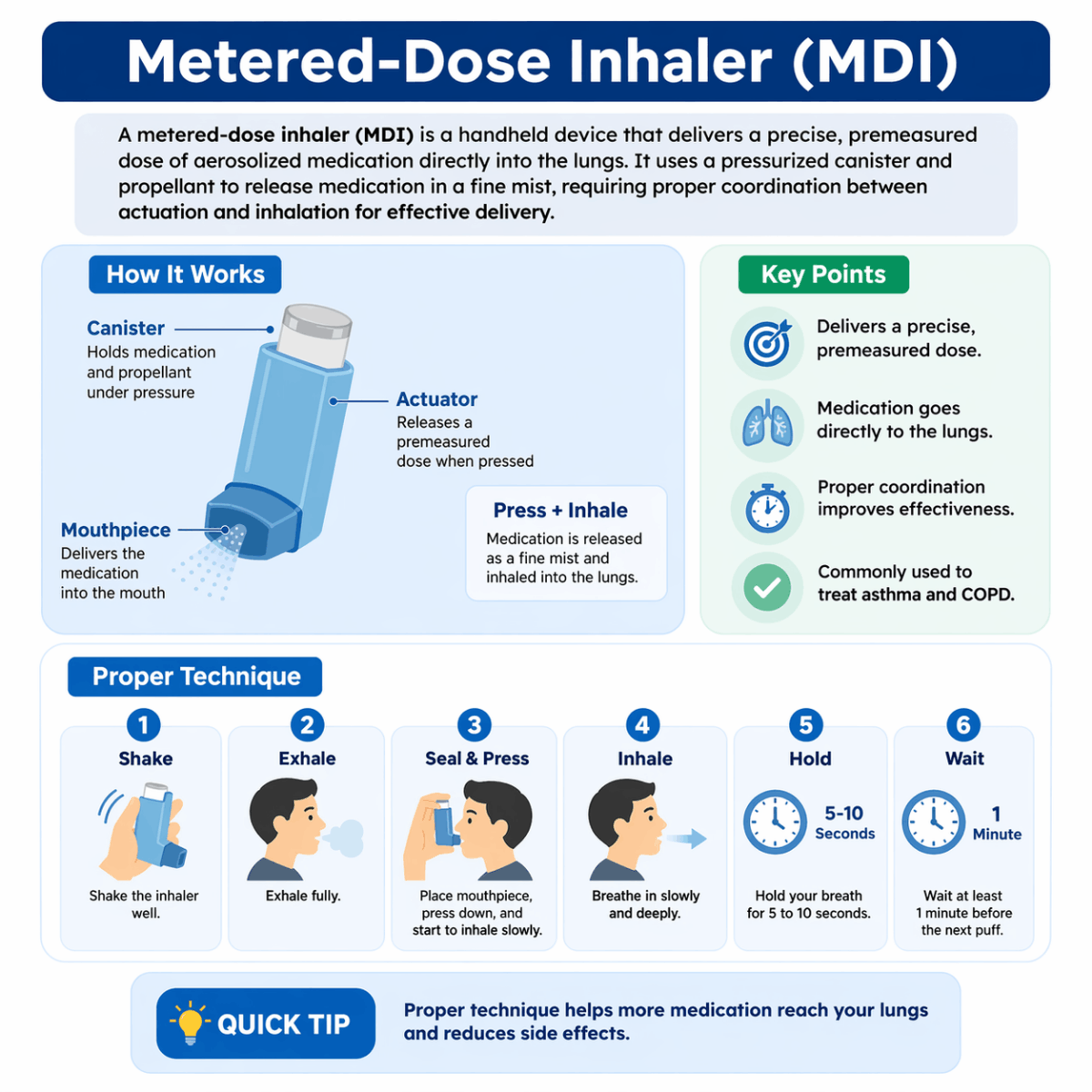
Components of an MDI
Pressurized Canister
The canister contains the medication mixed with a propellant under pressure. The medication may be dissolved or suspended within the propellant, depending on the formulation.
Metering Valve
The metering valve is a critical component that ensures a consistent dose is released with each actuation. It measures a fixed volume of the medication-propellant mixture before it is expelled.
Actuator (Mouthpiece)
The actuator is the plastic housing that holds the canister and directs the aerosolized medication into the patient’s mouth. It includes the mouthpiece through which the patient inhales the medication.
Propellant
Modern MDIs use hydrofluoroalkane (HFA) as a propellant. This replaced older chlorofluorocarbon (CFC) propellants due to environmental concerns. HFA propellants produce a softer and warmer aerosol plume, which can improve patient comfort and drug delivery.
How Does an MDI Work?
The operation of an MDI is based on the rapid expansion of a pressurized propellant. When the patient presses down on the canister, the metering valve releases a fixed amount of medication. The propellant then expands quickly, converting the liquid formulation into a fine aerosol spray.
This aerosol contains small particles that can be inhaled deep into the lungs. The goal is to deposit the medication in the lower airways, where it can exert its therapeutic effect.
The efficiency of this process depends on several factors, including particle size, inhalation technique, and timing. Proper coordination between actuation and inhalation is necessary to ensure that the medication reaches the target areas within the lungs.
Types of Medications Delivered by MDIs
- Short-Acting Bronchodilators: Short-acting beta-agonists, such as albuterol, are commonly delivered via MDIs for rapid relief of bronchospasm. These medications work quickly to relax the smooth muscles of the airways.
- Long-Acting Bronchodilators: These are used for maintenance therapy in chronic respiratory conditions. They help keep the airways open over an extended period.
- Inhaled Corticosteroids: These reduce inflammation in the airways. They are a key component of long-term management for conditions such as asthma.
- Combination Medications: Some MDIs contain a combination of medications, such as a bronchodilator and a corticosteroid. These provide both immediate relief and long-term control.
Advantages of Metered-Dose Inhalers
- Portability: MDIs are compact and lightweight, making them easy to carry. This allows patients to use them whenever needed, including during acute episodes.
- Rapid Drug Delivery: Medication is delivered quickly, often producing effects within minutes. This is especially important for rescue medications.
- Precise Dosing: Each actuation delivers a consistent, premeasured dose. This helps ensure accurate and predictable treatment.
- Cost-Effectiveness: Compared with some other aerosol delivery systems, MDIs are relatively inexpensive. They also require minimal setup and maintenance.
- Short Treatment Time: Unlike nebulizers, which may take several minutes to deliver medication, MDIs can be used in a matter of seconds.
Limitations and Challenges
- Coordination Requirement: One of the most significant challenges is the need to coordinate inhalation with actuation. The patient must begin inhaling slowly and deeply at the exact moment the inhaler is activated. Poor coordination can result in reduced drug delivery to the lungs.
- Oropharyngeal Deposition: Because the aerosol is released at high velocity, a portion of the medication may deposit in the mouth and throat rather than reaching the lungs. This can reduce effectiveness and increase the risk of side effects.
- Technique Dependence: Proper technique is essential for optimal drug delivery. Incorrect use can significantly reduce the amount of medication that reaches the lower airways.
- Physical Limitations: Some patients may have difficulty using MDIs due to conditions such as arthritis, weakness, or neuromuscular disorders. These limitations can make it challenging to actuate the device properly.
- Dose Monitoring: Not all MDIs have built-in dose counters. This can make it difficult for patients to determine how much medication remains in the canister.
Proper MDI Technique
Using an MDI correctly is essential for effective treatment. The following steps outline proper technique:
- Remove the cap and inspect the mouthpiece
- Shake the inhaler thoroughly
- Exhale fully to functional residual capacity
- Place the mouthpiece in the mouth and seal the lips around it
- Begin a slow, deep inhalation
- Actuate the inhaler at the start of inhalation
- Continue inhaling slowly and deeply
- Hold your breath for 5 to 10 seconds
- Exhale slowly
Note: If more than one dose is prescribed, the patient should wait at least one minute between puffs. This allows the airways to reopen and improves the effectiveness of subsequent doses.
Priming the Inhaler
Priming is an important step that ensures accurate dosing. It is required when:
- The inhaler is used for the first time
- The inhaler has not been used for several days
- The inhaler has been dropped
Note: Priming involves shaking the inhaler and releasing one or more test sprays into the air. This ensures that the metering chamber is properly filled with the medication-propellant mixture. Failure to prime the inhaler can result in an incomplete or inconsistent dose.
Common Errors in MDI Use
Improper technique is common and can significantly reduce treatment effectiveness. Some of the most frequent errors include:
- Failing to shake the inhaler before use
- Inhaling too quickly
- Poor coordination between actuation and inhalation
- Not holding the breath after inhalation
- Taking multiple puffs too quickly without waiting
Note: Studies have shown that a large percentage of patients do not use their inhalers correctly. This highlights the importance of patient education and regular reassessment of technique.
Role of Spacers and Holding Chambers
Spacers and valved holding chambers are devices that attach to the MDI to improve drug delivery. They act as reservoirs that hold the aerosol after it is released, allowing the patient to inhale it more easily.
Benefits of using a spacer include:
- Reduced need for precise coordination
- Improved delivery of medication to the lungs
- Decreased deposition in the mouth and throat
- Reduced risk of side effects, especially with corticosteroids
Note: Valved holding chambers include one-way valves that prevent exhalation into the device. These are particularly useful for children and patients who have difficulty coordinating inhalation.
Breath-Actuated and Soft-Mist Inhalers
- Breath-Actuated Inhalers: These devices release medication automatically when the patient inhales. This eliminates the need for manual coordination and can improve ease of use.
- Soft-Mist Inhalers: Soft-mist inhalers use mechanical energy rather than a propellant to generate a slow-moving aerosol. This results in a longer spray duration and improved deposition in the lungs.
Note: These alternatives may be recommended for patients who have difficulty using traditional MDIs.
Clinical Considerations and Device Selection
The choice of an aerosol delivery device should be based on the patient’s individual needs and abilities. Factors to consider include:
- Age
- Coordination
- Cognitive function
- Inspiratory flow
- Severity of disease
Note: No single device is ideal for all patients. The most effective device is the one that the patient can use correctly and consistently. Respiratory therapists and healthcare providers play a critical role in assessing patients, selecting appropriate devices, and providing education on proper use.
Cleaning and Maintenance of MDIs
Proper cleaning and maintenance of a metered-dose inhaler are essential for ensuring consistent drug delivery and preventing device malfunction. Over time, medication residue can accumulate in the actuator and nozzle, leading to blockage or altered spray patterns. This can reduce the amount of medication delivered to the patient.
To maintain proper function, the mouthpiece and actuator should be cleaned regularly. The general recommendation is to remove the canister and rinse the plastic actuator under warm running water. It should then be allowed to air dry completely before reassembly. The metal canister should not be submerged in water, as this can damage the internal components and affect performance.
Failure to clean the inhaler properly can result in clogging, which may lead to reduced dosing or complete obstruction of the spray. Regular maintenance helps ensure that the device continues to deliver medication effectively.
Environmental and Storage Considerations
Environmental factors can influence the performance of MDIs. Because these devices rely on pressurized propellants, temperature plays a significant role in their function. Exposure to extreme cold can reduce the pressure inside the canister, resulting in a weaker spray and decreased drug delivery. On the other hand, excessive heat can increase pressure and potentially damage the device.
Patients should be advised to store their inhalers at room temperature and avoid leaving them in places such as cars, where temperatures can fluctuate significantly. Proper storage helps maintain consistent dosing and prolongs the lifespan of the device.
Humidity and contamination are also important considerations. Keeping the mouthpiece clean and covered when not in use can prevent the introduction of dust, debris, or microorganisms that could interfere with medication delivery.
Monitoring Dose and Device Function
One challenge associated with MDIs is determining how much medication remains in the canister. Some modern inhalers include built-in dose counters that display the number of remaining actuations. These counters provide a reliable way for patients to track usage and avoid running out of medication unexpectedly.
For inhalers without dose counters, patients may attempt to estimate remaining doses based on the number of puffs used. However, this method is less accurate and can lead to the use of an empty or nearly empty inhaler during a critical moment.
Patients should be educated on the importance of monitoring their inhaler and replacing it before it becomes empty. Inconsistent dosing toward the end of a canister is a known issue, as the amount of medication delivered may decrease even if some propellant remains.
Note: Healthcare providers should also periodically assess device function and patient technique to ensure that the inhaler is being used correctly and is delivering medication as intended.
Comparison With Other Aerosol Delivery Devices
In clinical practice, MDIs are often compared with other aerosol delivery systems, particularly small-volume nebulizers (SVNs) and dry powder inhalers (DPIs). Each device has its own advantages and limitations, and the choice depends on patient-specific factors.
MDIs vs. Small-Volume Nebulizers
Small-volume nebulizers deliver medication over a longer period, typically several minutes, and do not require coordination between actuation and inhalation. This makes them useful for patients who are unable to use MDIs effectively.
However, nebulizers are less portable, require a power source or compressed gas, and take longer to administer medication. In contrast, MDIs are quick to use, portable, and convenient for daily use.
When used correctly, MDIs are generally considered to be as effective as nebulizers for delivering many respiratory medications. This makes them a preferred option for many patients.
MDIs vs. Dry Powder Inhalers
Dry powder inhalers are breath-actuated devices that rely on the patient’s inspiratory effort to disperse the medication. This eliminates the need for coordination between actuation and inhalation.
However, DPIs require a sufficient inspiratory flow rate to be effective. Patients with severe respiratory distress or limited inspiratory capacity may not be able to generate enough flow to use these devices properly.
MDIs, on the other hand, can be used with spacers or holding chambers to improve delivery, making them more versatile for a wider range of patients.
Patient Education and Training
Patient education is one of the most critical factors in ensuring the effectiveness of MDI therapy. Even though MDIs are simple in design, improper use is common and can significantly reduce treatment outcomes.
Healthcare providers, particularly respiratory therapists, are responsible for teaching patients how to use their inhalers correctly. This process should include:
- Demonstrating proper technique step by step
- Observing the patient perform a return demonstration
- Providing clear and simple instructions
- Reinforcing correct use during follow-up visits
Education should not be a one-time event. Patients should have their technique reassessed regularly, as errors can develop over time. Studies consistently show that a large percentage of patients use their inhalers incorrectly, which can lead to poor disease control.
Note: Special attention should be given to populations at higher risk of improper use, including children, elderly patients, and individuals with cognitive or physical limitations.
Special Populations and Considerations
Pediatric Patients
Children often have difficulty coordinating inhalation with actuation. The use of spacers or valved holding chambers is strongly recommended in this group. In some cases, a mask attachment may be used to facilitate administration.
Elderly Patients
Older adults may have reduced dexterity, strength, or cognitive function, which can make it challenging to use an MDI properly. Simplified instructions and the use of assistive devices can improve outcomes.
Patients With Severe Respiratory Distress
Patients who are unable to generate adequate inspiratory effort may not benefit fully from MDI therapy. In these cases, alternative devices such as nebulizers may be more appropriate.
Patients Using Inhaled Corticosteroids
Patients using corticosteroid MDIs should be instructed to rinse their mouth after use. This helps reduce the risk of local side effects such as oral candidiasis.
Troubleshooting Common Problems
Patients may encounter issues when using their MDIs. Understanding how to identify and correct these problems is important for maintaining effective therapy.
- Weak or No Spray: This may be caused by a clogged nozzle or an empty canister. Cleaning the actuator or replacing the inhaler may be necessary.
- Poor Symptom Control: This may result from improper technique, inadequate dosing, or disease progression. A reassessment of technique and medication regimen is required.
- Unpleasant Taste or Throat Irritation: This is often due to medication depositing in the oropharynx. Using a spacer can help reduce this issue.
- Difficulty Coordinating Use: Patients who struggle with timing should be evaluated for the use of a spacer, breath-actuated inhaler, or alternative device.
Role of Respiratory Therapists
Respiratory therapists play a central role in optimizing MDI therapy. Their responsibilities include:
- Assessing patient ability to use inhalers
- Selecting the most appropriate device
- Educating patients on proper technique
- Monitoring adherence and effectiveness
- Reassessing technique during follow-up care
Note: By providing ongoing support and education, respiratory therapists help ensure that patients receive the full benefit of their prescribed medications.
Key Clinical Concepts
Several key concepts should be emphasized when considering MDI use in clinical practice:
- MDIs deliver a precise, premeasured dose with each actuation
- Proper technique is essential for effective drug delivery
- Coordination between actuation and inhalation is a common challenge
- Spacers and holding chambers improve delivery and reduce side effects
- Device selection should be based on patient ability, not preference alone
- Regular reassessment of technique is necessary for optimal outcomes
Note: These principles are important not only for patient care but also for success on respiratory therapy board examinations.
Metered-Dose Inhaler (MDI) Practice Questions
1. What is a metered-dose inhaler (MDI)?
A handheld device that delivers a precise, premeasured dose of aerosolized medication to the lungs.
2. What does each actuation of an MDI provide?
A fixed, consistent dose of medication.
3. What is another name for a metered-dose inhaler?
Pressurized metered-dose inhaler (pMDI).
4. What types of conditions are commonly treated with MDIs?
Asthma and chronic obstructive pulmonary disease (COPD).
5. What component of the MDI ensures a consistent dose is delivered?
The metering valve.
6. What type of propellant is used in modern MDIs?
Hydrofluoroalkane (HFA)
7. Why were chlorofluorocarbon (CFC) propellants phased out?
Due to environmental concerns.
8. What is the role of the actuator in an MDI?
It directs the aerosolized medication into the patient’s mouth.
9. How is the medication stored inside an MDI canister?
Dissolved or suspended in a propellant.
10. What must occur at the same time for proper MDI use?
Actuation and inhalation.
11. What happens if coordination between actuation and inhalation is poor?
Reduced drug delivery to the lungs.
12. What is a common site of unwanted drug deposition with improper MDI use?
The oropharynx.
13. What percentage of patients may use MDIs incorrectly?
Up to 75%
14. What is the first step before using an MDI?
Shake the inhaler.
15. Why is shaking the inhaler important?
To evenly distribute the medication within the propellant.
16. What should the patient do before inhaling the medication?
Exhale fully
17. How should the patient inhale when using an MDI?
Slowly and deeply
18. How long should a patient hold their breath after inhalation?
Approximately 5 to 10 seconds.
19. Why is breath-holding important after inhalation?
To allow medication to deposit in the airways.
20. How long should a patient wait between puffs?
At least one minute.
21. What is priming an MDI?
Releasing test sprays before use to ensure proper dosing.
22. When is priming required?
Before first use or after a period of nonuse.
23. What can happen if an MDI is not primed?
It may deliver an inaccurate dose.
24. What device can be attached to an MDI to improve drug delivery?
A spacer.
25. How do spacers improve medication delivery?
They reduce coordination requirements and improve lung deposition.
26. What is the primary function of a spacer with an MDI?
To act as a reservoir that holds aerosolized medication for easier inhalation.
27. What type of spacer includes one-way valves?
A valved holding chamber (VHC).
28. Who benefits most from using a valved holding chamber?
Children, elderly patients, and those with poor coordination.
29. How do spacers reduce oropharyngeal deposition?
By slowing down aerosol velocity before inhalation.
30. What local side effect can occur from corticosteroid MDIs?
Oral candidiasis
31. How can oral candidiasis be reduced when using corticosteroids?
By using a spacer and rinsing the mouth after use.
32. What is a breath-actuated inhaler?
A device that releases medication automatically during inhalation.
33. What advantage do breath-actuated inhalers provide?
They eliminate the need for coordination between actuation and inhalation.
34. What is a soft-mist inhaler (SMI)?
A device that uses mechanical energy to create a slow-moving aerosol.
35. How does a soft-mist inhaler differ from a traditional MDI?
It does not rely on a propellant.
36. What is one benefit of the slower aerosol from SMIs?
Improved lung deposition.
37. What is a major advantage of MDIs over nebulizers?
They are more portable and faster to use.
38. What is a disadvantage of small-volume nebulizers (SVNs)?
They require more time and equipment to deliver medication.
39. Why might a nebulizer be preferred over an MDI?
If the patient cannot coordinate inhalation and actuation.
40. What factor determines the best aerosol device for a patient?
The patient’s ability to use it correctly.
41. What is meant by “device selection is patient-dependent”?
The best device depends on the patient’s abilities, not the device itself.
42. What can clog an MDI and affect its performance?
Medication buildup in the actuator or nozzle.
43. How should the actuator be cleaned?
With warm water and allowed to air dry.
44. Should the metal canister be submerged in water?
No, it can damage the device.
45. What happens if the nozzle becomes blocked?
Medication delivery may be reduced or stopped.
46. Why should MDIs be stored at room temperature?
To maintain proper propellant pressure and performance.
47. What can happen if an MDI is exposed to extreme cold?
Reduced spray strength and decreased drug delivery.
48. What is a potential risk of exposing an MDI to excessive heat?
Increased pressure and possible device damage.
49. What feature helps patients track remaining doses?
A dose counter.
50. Why are dose counters important?
They help prevent use of an empty inhaler.
51. What is the purpose of the propellant in an MDI?
To expel the medication as an aerosol spray.
52. What happens to the propellant when the inhaler is actuated?
It rapidly expands and aerosolizes the medication.
53. What determines how deeply particles travel into the lungs?
Particle size and inhalation technique.
54. Why is a slow inhalation recommended with MDIs?
To improve deposition in the lower airways.
55. What happens if a patient inhales too quickly?
More medication deposits in the oropharynx.
56. What is the benefit of inhaling to total lung capacity?
It helps deliver medication deeper into the lungs.
57. What should be checked before using an MDI?
The mouthpiece for debris or obstruction.
58. What is the risk of using an unclean mouthpiece?
Reduced drug delivery and possible contamination.
59. Why should the cap be replaced after using an MDI?
To keep the mouthpiece clean and protected.
60. What is one sign that an inhaler may be empty?
A weak or absent spray.
61. Why is shaking especially important for suspension MDIs?
To evenly mix the medication particles with the propellant.
62. What can happen if a patient exhales into a spacer?
It can disrupt the aerosol and reduce drug delivery.
63. How do valved holding chambers prevent exhalation issues?
They allow inhalation but block exhalation into the chamber.
64. What type of inspiratory effort is needed for proper MDI use?
A slow and controlled inhalation.
65. Why might patients with severe respiratory distress struggle with MDIs?
They may not achieve proper inhalation or coordination.
66. What is the advantage of MDIs in emergency situations?
They provide rapid medication delivery.
67. What is a key disadvantage of MDIs without spacers?
High oropharyngeal deposition.
68. What role do respiratory therapists play in MDI use?
They educate patients and assess inhaler technique.
69. What is a return demonstration?
When a patient shows they can correctly use the inhaler.
70. Why is repeated education important for MDI users?
Because technique errors can develop over time.
71. What is one benefit of combination inhalers?
They simplify treatment by delivering multiple medications.
72. What can reduce the effectiveness of an MDI dose?
Poor timing between inhalation and actuation.
73. What is the purpose of waiting between puffs?
To allow airways to open and improve drug delivery.
74. What is a common error when taking multiple puffs?
Administering them too quickly without waiting.
75. Why is consistent technique important with every use?
To ensure reliable and effective medication delivery.
76. What is the purpose of the metering chamber in an MDI?
To hold a fixed volume of medication before it is released.
77. What happens if the canister is not properly seated in the actuator?
The inhaler may fail to deliver medication correctly.
78. Why should patients avoid spraying MDIs into the air unnecessarily?
It wastes doses and reduces the number of available treatments.
79. What is the recommended inhalation duration when using an MDI?
Several seconds during a slow, deep breath.
80. What can happen if a patient does not inhale deeply enough?
Less medication reaches the lower airways.
81. What is the advantage of HFA propellants over CFCs in terms of patient experience?
They produce a softer and warmer aerosol plume.
82. What is one reason MDIs are considered cost-effective?
They deliver multiple doses from a single device.
83. Why is it important to keep track of the number of doses used?
To avoid running out of medication unexpectedly.
84. What can happen if an MDI is used past its labeled number of doses?
The delivered dose may become inconsistent or inadequate.
85. What type of patients may struggle with actuating an MDI?
Those with arthritis or reduced hand strength.
86. What is a common solution for patients who cannot press the canister easily?
Use of assistive devices or alternative inhalers.
87. What is the benefit of using an MDI for maintenance therapy?
It allows consistent delivery of long-term control medications.
88. What is the main goal of aerosol therapy with an MDI?
To deliver medication directly to the lungs.
89. What can interfere with aerosol delivery if the inhaler is not held upright?
Improper positioning can affect dose accuracy.
90. Why should patients avoid biting the mouthpiece during use?
It can block airflow and reduce medication delivery.
91. What is a potential consequence of not sealing the lips around the mouthpiece?
Medication may escape and reduce effective dosing.
92. What technique can be used instead of placing the mouthpiece in the mouth?
The open-mouth technique.
93. What is the risk of using incorrect technique repeatedly?
Poor disease control and reduced treatment effectiveness.
94. What is the importance of observing spray pattern during priming?
To confirm the inhaler is functioning properly.
95. What should be done if no mist appears during priming?
Check for blockage or device malfunction.
96. What is the purpose of a protective cap on an MDI?
To keep the mouthpiece clean and free of debris.
97. What is a key reason MDIs are widely used in outpatient settings?
Their portability and ease of use.
98. What can happen if moisture enters the actuator?
It may affect spray consistency or cause blockage.
99. Why is patient preference considered in device selection?
It can improve adherence and proper use.
100. What is the ultimate goal of proper MDI use?
To achieve optimal therapeutic outcomes through effective drug delivery.
Final Thoughts
The metered-dose inhaler (MDI) remains one of the most widely used and effective devices for delivering aerosolized medications in respiratory care. Its ability to provide a precise dose in a portable and convenient format makes it suitable for both acute and long-term management of respiratory diseases.
However, its effectiveness is highly dependent on proper technique, patient coordination, and consistent use. With appropriate education, regular reassessment, and the use of adjunct devices when needed, MDIs can provide reliable and efficient drug delivery. Ensuring that patients understand how to use their inhalers correctly is essential for achieving optimal therapeutic outcomes.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Ahmed M, Munir M, Sufyan A, Ayyaz J, Arshad I Sr, Bukhari M, Umar M, Khurram M, Tariq A, Hamza M. Metered Dose Inhaler Technique: A Priority Catch for Physicians. Cureus. 2020.

