Lung sounds are a fundamental part of respiratory assessment, offering valuable insight into airflow, lung tissue integrity, and potential underlying disease. By listening carefully with a stethoscope, clinicians can identify normal breath patterns as well as adventitious sounds that signal obstruction, inflammation, fluid accumulation, or changes in lung density.
Each sound—whether soft and normal or harsh and abnormal—carries diagnostic meaning that helps guide clinical decisions. Understanding the different types of lung sounds and the conditions that cause them is essential for accurate auscultation and early recognition of respiratory problems.
This article provides a detailed overview of the major lung sound categories and explains what each one reveals about a patient’s respiratory status.
What are Lung Sounds?
Lung sounds are the audible vibrations created as air moves through the respiratory system, and they are heard during auscultation with a stethoscope. These sounds offer valuable clues about airway openness, lung tissue health, and the presence of fluid, inflammation, or obstruction.
Normal lung sounds include tracheal, bronchovesicular, and vesicular patterns, each reflecting airflow through specific regions of the lungs. Abnormal lung sounds such as crackles, wheezes, rhonchi, stridor, and pleural friction rubs often indicate conditions like pneumonia, asthma, heart failure, or pleural irritation.
Changes in pitch, loudness, or location can show altered ventilation or airway narrowing. Because lung sounds often change before physical symptoms develop, auscultation remains essential for effective diagnosis and clinical monitoring.
What is Auscultation?
Auscultation is a clinical assessment technique in which a healthcare provider listens to internal body sounds, most commonly from the lungs, heart, and abdomen, using a stethoscope. It allows clinicians to evaluate airflow, cardiac function, and bowel activity by identifying normal and abnormal sound patterns.
In respiratory care, auscultation helps detect conditions such as airway obstruction, fluid in the lungs, consolidation, or pleural inflammation by revealing specific breath sounds like crackles, wheezes, or diminished airflow. The technique requires a quiet environment, proper stethoscope placement, and systematic comparison of sounds between both sides of the body.
Note: Auscultation is an essential bedside skill that supports early detection of disease, guides treatment decisions, and helps monitor a patient’s response to therapy.
Normal Lung Sounds
Normal lung sounds provide a baseline for interpreting all other breath sounds during auscultation. They reflect healthy airflow through the airways and vary depending on where they are heard in the respiratory tract. The three primary types of normal lung sounds include:
- Vesicular Breath Sounds: Soft, low-pitched, and heard mainly during inspiration, with a short and faint expiratory phase. These sounds dominate the peripheral lung fields and represent normal airflow through small airways and alveoli.
- Bronchovesicular Breath Sounds: These sounds have moderate pitch and intensity, with equal durations of inspiration and expiration. They are normally heard over the upper sternum and between the scapulae, where medium-sized airways lie close to the chest wall.
- Tracheal Breath Sounds: Loud, high-pitched, and tubular because air moves rapidly through the rigid trachea. They have equal inspiratory and expiratory phases and are heard only when auscultating directly over the trachea. Hearing these sounds elsewhere is abnormal.
Note: Understanding these normal patterns makes it easier to recognize abnormal or adventitious lung sounds.
Adventitious Lung Sounds
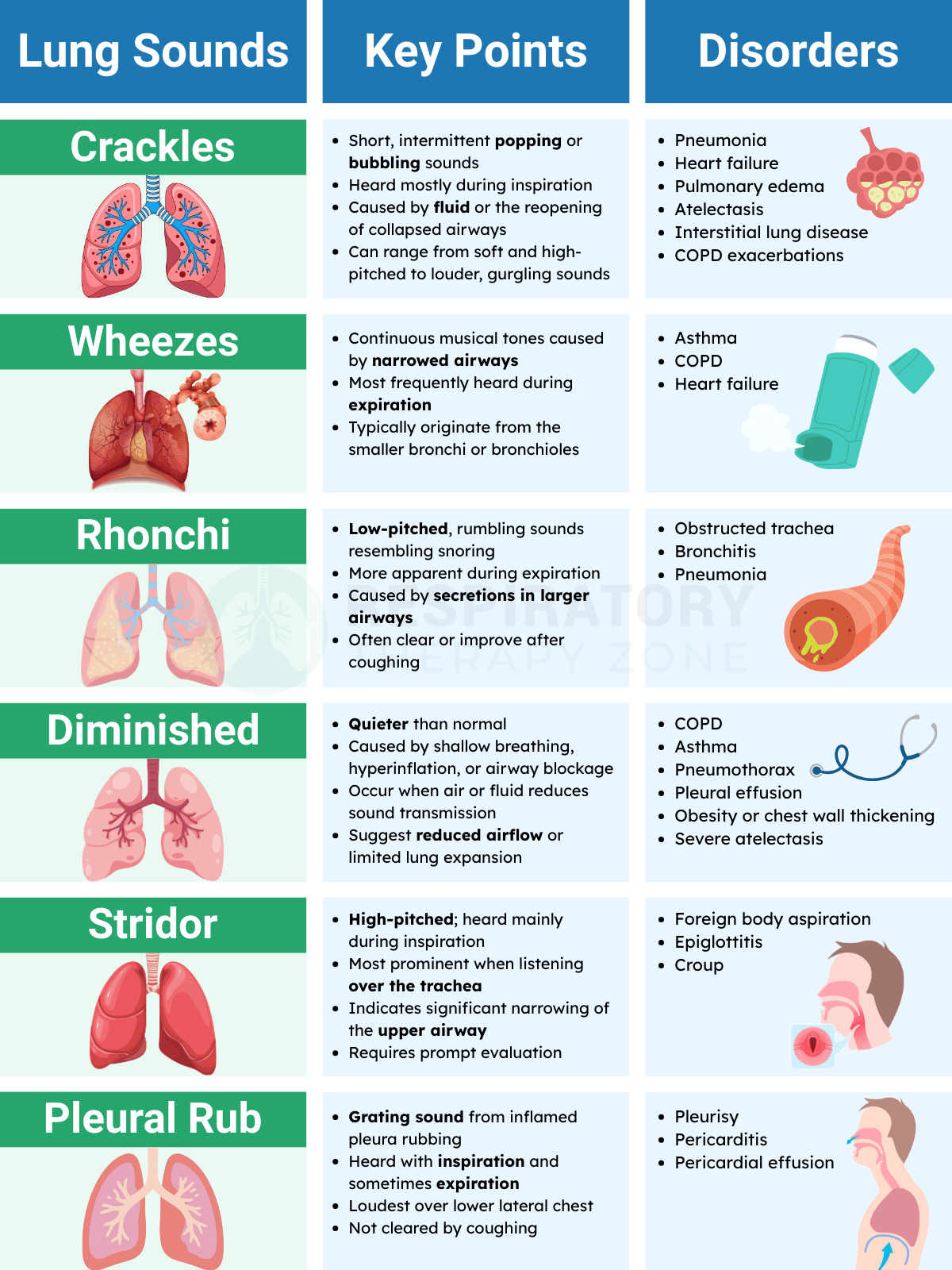
Adventitious lung sounds are abnormal breath sounds heard during auscultation and often indicate airway obstruction, fluid accumulation, inflammation, or changes in lung tissue. These sounds include:
- Crackles: Short, discontinuous popping or bubbling sounds produced when air moves through fluid, mucus, or collapsed airways that reopen during inspiration. They may be fine or coarse and are commonly associated with pneumonia, heart failure, or atelectasis.
- Wheezes: High-pitched, musical sounds caused by air flowing through narrowed or constricted airways. They are most often heard during expiration and are associated with asthma, COPD, and other obstructive airway diseases.
- Rhonchi: Low-pitched, coarse, snoring-like sounds created when air passes through airways obstructed by thick secretions. They often improve or clear with coughing and are frequently heard in bronchitis or pneumonia.
- Stridor: A loud, high-pitched sound produced by turbulent airflow through a narrowed upper airway, typically the larynx or trachea. It is most often inspiratory and may signal a serious obstruction from croup, foreign bodies, or airway swelling.
- Pleural Friction Rub: A harsh, grating sound caused by inflamed pleural surfaces rubbing together during breathing. It does not change with coughing and is usually associated with pleurisy, pulmonary embolism, or trauma.
Note: These adventitious sounds help clinicians determine the presence, severity, and possible cause of respiratory impairment.
Types of Lung Sounds
Lung sounds are categorized based on their location, pitch, intensity, and the conditions that produce them. Understanding each type is essential for accurate respiratory assessment because different sounds reveal different physiological changes in the airways and lung tissue.
Vesicular
Vesicular breath sounds are the soft, low-pitched sounds normally heard over the peripheral lung fields and represent healthy airflow through the small bronchioles and alveoli. These sounds are characterized by a long, gentle inspiratory phase followed by a short, faint expiratory component, typically about one-third the length of inspiration.
The spongy nature of normal lung tissue filters out high-frequency vibrations created in the larger airways, producing the muffled quality that defines vesicular breathing. Because vesicular sounds dominate most lung regions, they serve as the baseline for identifying abnormalities.
When vesicular sounds are diminished, absent, or replaced by harsher patterns, it may indicate consolidation, pleural effusion, pneumothorax, or hyperinflation. Accurate recognition of vesicular breath sounds is essential for evaluating normal versus pathological findings during auscultation.
Bronchovesicular
Bronchovesicular breath sounds are normal lung sounds heard over the upper sternum anteriorly and between the scapulae posteriorly, where medium-sized bronchi lie close to the chest wall. These sounds have a moderate pitch and intensity, falling between the harsher bronchial sounds and the softer vesicular sounds.
A key feature is that the inspiratory and expiratory phases are roughly equal in length, which helps distinguish them from vesicular sounds that are primarily inspiratory. Bronchovesicular sounds reflect healthy airflow in the central airways and are considered normal only within their expected anatomical locations.
When heard in the peripheral lung fields, they may indicate early consolidation, increased lung density, or partial atelectasis that improves sound transmission. Their presence outside normal areas warrants further clinical assessment.
Tracheal
Tracheal breath sounds are the loudest and highest-pitched of all normal lung sounds and are heard exclusively over the trachea. They have a harsh, tubular quality because air moves rapidly through the rigid, large-diameter tracheal airway with minimal filtering from surrounding tissues. The inspiratory and expiratory phases are nearly equal in duration, and both are distinctly audible.
These sounds provide a reference point for comparing all other breath sounds during auscultation. Hearing tracheal-like sounds in areas away from the trachea is abnormal and often indicates consolidation, increased lung tissue density, or lung collapse that allows tracheal sounds to transmit into the peripheral lung fields. Tracheal breath sounds, when heard only over the trachea, represent normal airflow through the central airway.
Crackles (Rales)
Crackles, also known as rales, are abnormal, discontinuous breath sounds that resemble popping, bubbling, or crackling noises. They occur when air moves through fluid, mucus, or secretions in the airways, or when collapsed alveoli suddenly pop open during inspiration.
Crackles are classified as fine or coarse. Fine crackles are soft, high-pitched, and brief, often associated with pulmonary fibrosis, early congestive heart failure, or small airway collapse. Coarse crackles are louder, lower-pitched, and longer in duration, commonly linked to pneumonia, bronchitis, or significant airway secretions.
Unlike rhonchi, crackles generally do not clear with coughing unless secretions shift into larger airways. The timing of crackles—early, mid, or late inspiration—helps identify the underlying condition. Crackles are a key indicator of disrupted ventilation and often signal fluid accumulation or loss of alveolar stability.
Wheezes
Wheezes are high-pitched, musical breath sounds produced when air flows through narrowed or partially obstructed airways. They result from rapid airflow causing the airway walls to vibrate, much like a reed instrument.
Wheezes are most commonly heard during expiration, although severe airway narrowing can make them audible during inspiration as well. These sounds are strongly associated with obstructive conditions such as asthma, COPD, bronchospasm, and airway inflammation. Wheezes may be monophonic, suggesting a single narrowed airway, or polyphonic, indicating widespread narrowing in multiple airways.
The pitch and duration of wheezing can provide clinical clues about the severity of obstruction. Because wheezing reflects impaired airflow, its presence requires careful evaluation, and changes in wheeze intensity can help monitor response to bronchodilator therapy or disease progression.
Rhonchi
Rhonchi are low-pitched, coarse, snoring or gurgling breath sounds caused by airflow moving through airways obstructed by thick mucus or secretions. These sounds typically occur during expiration but may also be heard throughout the entire breathing cycle when secretions are abundant. Rhonchi are commonly associated with conditions such as chronic bronchitis, pneumonia, COPD exacerbations, or any disorder that leads to increased mucus production.
One distinguishing feature is that rhonchi often improve or clear with coughing, as coughing can mobilize or remove the secretions causing the obstruction. This makes rhonchi functionally different from crackles, which usually persist despite coughing. The presence of rhonchi suggests inadequate airway clearance and reduced airflow, prompting clinicians to consider interventions such as suctioning, hydration, or airway clearance therapy.
Stridor
Stridor is a loud, high-pitched respiratory sound caused by turbulent airflow through a significantly narrowed upper airway, typically at the level of the larynx, trachea, or subglottic region. It is most often heard during inspiration and may be audible without a stethoscope, making it one of the most recognizable and urgent respiratory sounds.
Stridor commonly occurs in conditions such as croup, epiglottitis, laryngeal edema, foreign body aspiration, or post-extubation airway swelling. Because the upper airway is a narrow structure, even slight swelling or obstruction can produce pronounced stridor and lead to respiratory distress.
Patients may also exhibit retractions, hoarseness, or difficulty breathing. Stridor requires prompt evaluation and intervention because it can rapidly progress to complete airway obstruction if the underlying cause is not treated.
Diminished
Diminished breath sounds are fainter or quieter than normal lung sounds and indicate reduced airflow or impaired transmission of sound through the lungs or chest wall. They may occur when a patient is breathing shallowly, when airflow is obstructed by mucus plugging, or when lung tissue is hyperinflated, as seen in conditions such as asthma or COPD.
Diminished sounds can also result from pleural abnormalities, including pneumothorax, pleural effusion, or hemothorax, which block sound conduction. Additionally, a thick chest wall due to obesity, muscle mass, or generalized edema can muffle sound intensity.
Identifying diminished breath sounds is clinically important because they often signal decreased ventilation or early respiratory compromise. When combined with other findings such as tachypnea, dyspnea, or changes in oxygen saturation, diminished sounds may indicate the need for further evaluation or intervention.
Bronchial
Bronchial breath sounds are loud, high-pitched, tubular breath sounds with an expiratory phase that is equal to or longer than the inspiratory phase. They are normally heard only over the trachea, where airflow through the large, rigid airway produces strong vibrations with minimal filtering.
When heard in the peripheral lung fields, bronchial breath sounds are abnormal and usually indicate increased lung tissue density that allows central airway sounds to transmit more easily. This often occurs in conditions such as pneumonia, lung consolidation, or moderate atelectasis.
The presence of bronchial breath sounds outside their normal location is clinically significant because it suggests that air is not filling the alveoli normally. Recognizing this sound pattern helps clinicians identify areas of consolidation or collapse and guides decisions regarding imaging, therapy, and further respiratory assessment.
Pleural Friction Rub
A pleural friction rub is a harsh, grating, or creaking sound produced when inflamed pleural surfaces rub against each other during breathing. Under normal conditions, the pleura glide smoothly due to a thin layer of lubricating fluid. When inflammation occurs, as in pleurisy, pneumonia, pulmonary embolism, or trauma, the surfaces become rough and irritated, generating friction with each breath.
Pleural rubs are typically heard during inspiration but may be audible during both phases of respiration if inflammation is severe. The sound is usually localized to a small area of the chest wall and often corresponds with sharp, pleuritic chest pain.
Unlike crackles or rhonchi, a pleural friction rub does not change with coughing, which helps identify its origin. Detecting a pleural friction rub is important because it indicates pleural inflammation that may require imaging or further evaluation.
Causes of Abnormal Lung Sounds
Abnormal lung sounds often reflect underlying pathology that alters airflow, lung tissue density, or the movement of the pleural surfaces. Understanding the common causes helps clinicians interpret auscultation findings more accurately.
Airway Narrowing or Obstruction
One of the most common reasons for abnormal breath sounds is narrowing or blockage of the airways. Asthma, COPD, bronchospasm, inflammation, and mucus buildup reduce the diameter of the airways, which increases airflow velocity and creates turbulence. This turbulence causes the airway walls to vibrate and produces musical sounds such as wheezes or coarse, rumbling noises such as rhonchi.
Wheezes are typically associated with bronchospasm or airway hyperreactivity, while rhonchi point to the presence of secretions that partially obstruct airflow. In severe obstruction, airflow may become so limited that breath sounds are markedly diminished.
Fluid in the Airways or Alveoli
Crackles occur when fluid or secretions accumulate in the lower airways or when alveoli collapse and then reopen with each breath. Pneumonia, pulmonary edema, heart failure, and fluid overload commonly lead to this finding.
As air moves through moisture or pops open unstable alveoli, it creates the characteristic popping or bubbling sound. Fine crackles often indicate small airway or interstitial involvement, while coarse crackles usually reflect larger amounts of fluid or secretions in the bronchi.
Lung Tissue Consolidation
When the lung becomes denser due to infection, collapse, or inflammation, sound travels through it differently. Pneumonia, for example, replaces air-filled alveoli with inflammatory debris, allowing harsh bronchial sounds to transmit into peripheral lung regions.
Atelectasis has a similar effect, especially when airways remain partially open. This increased density reduces the filtering effect of normal lung tissue and causes breath sounds to shift from soft vesicular patterns to louder bronchial or bronchovesicular patterns. Consolidated areas may also transmit crackles more clearly.
Pleural Inflammation
Inflammation of the pleural surfaces alters how they move during breathing. In conditions such as pleurisy, pulmonary embolism, or trauma, the pleura become roughened, producing a distinctive pleural friction rub. This grating or creaking sound is often localized and becomes louder with deep breathing, reflecting increased contact between inflamed surfaces.
Upper Airway Obstruction
Stridor is a hallmark of upper airway narrowing caused by swelling, infection, trauma, or foreign body aspiration. The small diameter of the larynx or trachea means that even mild narrowing can cause intense, high-pitched airflow sounds. Stridor often signals a potentially serious or life-threatening obstruction.
Note: Recognizing the cause of abnormal lung sounds is crucial for determining the severity of the condition, guiding further testing, and initiating timely treatment.
Clinical Significance of Lung Sounds
Lung sounds are a powerful diagnostic tool because they provide immediate, noninvasive insight into a patient’s respiratory status. Recognizing the meaning behind different sound patterns helps clinicians identify early signs of disease, monitor progression, and evaluate response to treatment.
Identifying Airflow Obstruction
Wheezes, rhonchi, and stridor signal varying degrees of airway narrowing. Detecting these sounds helps clinicians determine the severity of obstruction and the need for interventions such as bronchodilators, suctioning, or airway management.
Detecting Fluid or Consolidation
Crackles and abnormal transmission of bronchial breath sounds indicate conditions such as pneumonia, pulmonary edema, or atelectasis. These findings help prioritize imaging, guide therapeutic decisions, and evaluate the effectiveness of treatments like diuretics or lung expansion therapy.
Monitoring Disease Progression
Changes in lung sounds over time can reveal improvement or worsening. For example, diminished breath sounds may progress to absent sounds in pneumothorax, or coarse crackles may transition to rhonchi as secretions mobilize.
Guiding Immediate Action
Stridor and severely diminished breath sounds may indicate life-threatening airway compromise or impending respiratory failure. Rapid recognition allows for swift intervention, protecting the patient from rapid deterioration.
Supporting Comprehensive Respiratory Assessment
While lung sounds alone do not confirm a diagnosis, they are essential clues when combined with inspection, percussion, medical history, and imaging. Auscultation remains one of the most valuable bedside skills for detecting respiratory abnormalities.
Fine Crackles vs. Coarse Crackles
Fine crackles and coarse crackles are two types of discontinuous adventitious lung sounds heard during auscultation. Although they may sound similar to an untrained ear, they arise from different mechanisms and often point to different clinical conditions. Understanding how they differ is essential for accurate respiratory assessment.
Fine Crackles
Fine crackles are soft, high-pitched, brief popping sounds typically heard during late inspiration. They resemble the sound of rubbing hair between your fingers near the ear. Fine crackles occur when small airways or alveoli that have collapsed or are fluid-filled suddenly pop open as the patient inhales. These sounds do not usually clear with coughing, which helps distinguish them from sounds caused by secretions.
Fine crackles are commonly associated with conditions such as pulmonary fibrosis, early congestive heart failure, interstitial lung disease, or dependent atelectasis. Their presence suggests reduced lung compliance or fluid within the interstitial or alveolar spaces.
Coarse Crackles
Coarse crackles are louder, lower-pitched, and longer in duration compared with fine crackles. They often sound like bubbling, rattling, or the noise of Velcro being pulled apart. Coarse crackles occur when air moves through larger airways filled with thick secretions. Because these sounds reflect mucus movement, they frequently improve or disappear after coughing or suctioning.
Coarse crackles are commonly associated with bronchitis, pneumonia, COPD exacerbations, or any condition that increases airway secretions. Unlike fine crackles, which are usually heard late in inspiration, coarse crackles may be audible during both inspiration and expiration.
Clinical Importance
Distinguishing between fine and coarse crackles helps clinicians identify the underlying cause of abnormal lung sounds. Fine crackles often point to issues with alveolar stability or fluid overload, whereas coarse crackles indicate excessive mucus or impaired airway clearance.
Note: Recognizing the difference aids in selecting appropriate treatments, such as diuretics for pulmonary edema or airway clearance therapy for secretion retention.
How to Perform Auscultation
Auscultation is the process of listening to internal body sounds, and in respiratory care it is a critical bedside skill for assessing lung function. It is noninvasive, quick to perform, and highly sensitive to changes in airflow, lung tissue density, and pleural movement.
Using a stethoscope, clinicians can detect both normal and abnormal lung sounds, making auscultation essential for evaluation and ongoing monitoring.
Prepare the Patient and Environment
Before beginning, ensure the patient is relaxed and sitting upright, which allows for optimal lung expansion. Ask the patient to breathe through the mouth slightly deeper than normal while keeping exhalation passive.
The diaphragm of the stethoscope must be placed directly on the skin because clothing can distort sound quality. Minimize external noise and prevent the tubing or stethoscope from rubbing against objects, as these artifacts may mimic adventitious breath sounds.
Follow a Systematic Auscultation Pattern
A structured approach helps ensure that no lung region is overlooked. Begin at the lung bases, where many abnormalities first appear, and compare breath sounds side to side at each level as you move upward toward the apexes.
Assess the anterior, lateral, and posterior chest to fully evaluate all lobes. At each stethoscope position, listen to one full respiratory cycle. When abnormal sounds are present, listen to several breaths to confirm their characteristics and timing.
Evaluate the Acoustic Features
When interpreting what you hear, focus on the key features of breath sounds: pitch, intensity, and the duration of the inspiratory and expiratory phases. These acoustic qualities help differentiate normal breath sounds, such as vesicular, bronchovesicular, and tracheal patterns, from abnormal ones including crackles, wheezes, rhonchi, stridor, diminished sounds, and pleural friction rubs.
Note: Recognizing normal patterns is essential because detecting subtle changes depends on understanding how healthy lungs should sound.
Develop Skill Through Practice
Effective auscultation requires repetition and close attention to detail. As clinicians become more familiar with the range of normal and abnormal lung sounds, their diagnostic accuracy improves.
Performed systematically and interpreted thoughtfully, auscultation provides immediate clinical insight and plays a central role in respiratory assessment and monitoring the effects of therapy.
Lung Sounds Practice Questions
1. What is the primary purpose of normal lung sounds during auscultation?
They serve as a baseline for identifying abnormal or adventitious breath sounds.
2. Which three types of normal lung sounds are recognized in respiratory assessment?
Vesicular, bronchovesicular, and tracheal breath sounds.
3. How are vesicular breath sounds best described?
Soft, low-pitched sounds heard mainly during inspiration with a short, faint expiratory phase.
4. Where are vesicular breath sounds normally heard?
Over the peripheral lung fields.
5. What do vesicular breath sounds represent physiologically?
Normal airflow through small airways and alveoli.
6. How do bronchovesicular breath sounds differ from vesicular breath sounds?
They have moderate pitch and intensity with equal inspiratory and expiratory phases.
7. Where are bronchovesicular breath sounds normally auscultated?
Over the upper sternum anteriorly and between the scapulae posteriorly.
8. What type of airways primarily generate bronchovesicular breath sounds?
Medium-sized airways close to the chest wall.
9. How are tracheal breath sounds best described?
Loud, high-pitched, and tubular with equal inspiratory and expiratory phases.
10. Where should tracheal breath sounds normally be heard?
Directly over the trachea.
11. What does hearing tracheal breath sounds over the lung periphery indicate?
An abnormal finding suggesting increased lung density or consolidation.
12. What are adventitious lung sounds?
Abnormal breath sounds indicating altered airflow, fluid, inflammation, or tissue changes.
13. What mechanism primarily produces crackles?
Air moving through fluid, mucus, or collapsed airways that reopen during inspiration.
14. How are crackles classified?
As fine or coarse based on sound intensity and quality.
15. What conditions are commonly associated with crackles?
Pneumonia, heart failure, and atelectasis.
16. What causes wheezes to occur?
Airflow through narrowed or constricted airways.
17. During which phase of breathing are wheezes most commonly heard?
Expiration
18. Which conditions are commonly associated with wheezing?
Asthma, COPD, and other obstructive airway diseases.
19. How are rhonchi best described?
Low-pitched, coarse, snoring-like sounds caused by thick airway secretions.
20. What happens to rhonchi after effective coughing or suctioning?
They often improve or clear.
21. What distinguishes stridor from wheezing?
Stridor originates from the upper airway and is louder and higher-pitched.
22. During which phase of breathing is stridor most often heard?
Inspiration
23. What conditions commonly cause stridor?
Croup, foreign body obstruction, and upper airway swelling.
24. What produces a pleural friction rub?
Inflamed pleural surfaces rubbing together during breathing.
25. How does a pleural friction rub differ from crackles?
It does not change or clear with coughing.
26. Where are bronchial breath sounds normally auscultated?
Directly over the trachea.
27. Which breath sounds are normally heard over the bronchi and are located anteriorly at the 1st and 2nd intercostal spaces and posteriorly between the scapulae?
Bronchovesicular breath sounds
28. Which breath sounds are normally heard throughout the peripheral lung fields, both anteriorly and posteriorly?
Vesicular breath sounds
29. What does the presence of bronchial breath sounds in the peripheral lung fields most strongly suggest?
Increased lung density due to consolidation, such as pneumonia.
30. Why are bronchial breath sounds considered abnormal when heard outside the tracheal area?
They indicate abnormal transmission of sound through consolidated or collapsed lung tissue.
31. Which lung sounds are classified as discontinuous adventitious sounds?
Fine crackles, coarse crackles, and pleural friction rubs.
32. True or False: Low-pitched wheezes are polyphonic and usually clear with coughing.
False
33. How are low-pitched wheezes best described?
Monophonic, continuous sounds that usually do not clear with coughing.
34. Which lung sound is continuous, high-pitched, musical, polyphonic, and heard mainly during expiration but may occur during inspiration?
High-pitched wheeze.
35. A high-pitched, harsh, monophonic sound heard only during inspiration is known as what?
Stridor
36. What is the most appropriate bedside maneuver to distinguish a pleural friction rub from a pericardial friction rub?
Ask the patient to hold their breath and listen for persistence of the sound.
37. If a harsh, grating sound persists when the patient holds their breath, what is the most likely source?
A pericardial friction rub.
38. True or False: Auscultation of the anterior chest primarily assesses the upper lobes, while the posterior chest primarily assesses the lower lobes.
True
39. Where should the stethoscope be placed to auscultate the lung apices anteriorly?
Slightly above the clavicles.
40. Where is the right middle lobe best auscultated?
Anteriorly on the right side at the 4th intercostal space.
41. When auscultating the posterior chest, between which vertebral levels are the upper lobes primarily assessed?
Between C7 and T3.
42. True or False: The left lung has three lobes.
False
43. What is the correct number of lobes in the left lung?
Two lobes: upper and lower.
44. What term describes the clinical process of listening to internal body sounds using a stethoscope?
Auscultation
45. What are the four basic components of a stethoscope?
The bell, diaphragm, tubing, and earpieces.
46. Which part of the stethoscope is best for detecting low-pitched sounds such as heart sounds?
The bell
47. Which part of the stethoscope is preferred for lung auscultation due to high-frequency sound transmission?
The diaphragm
48. What is the ideal length of stethoscope tubing to optimize sound transmission?
Approximately 25–35 cm (11–16 inches).
49. Why should lung auscultation begin at the bases of the lungs?
Abnormal sounds in the lower lobes may change or disappear after several deep breaths.
50. What three key sound characteristics should be identified during lung auscultation?
Pitch, intensity, and the duration of inspiratory and expiratory phases.
51. What is the typical pitch of vesicular breath sounds?
Low
52. What is the typical intensity of vesicular breath sounds?
Soft
53. Where are vesicular breath sounds normally heard?
Over the peripheral lung fields.
54. Soft, muffled breath sounds heard over healthy lung parenchyma are known as what?
Vesicular breath sounds.
55. Compared to bronchovesicular sounds, vesicular breath sounds are lower in pitch and intensity and are heard primarily during which phase of breathing?
Inspiration
56. Approximately how long is the expiratory component of vesicular breath sounds compared to inspiration?
About one-third the duration of inspiration.
57. What is the typical pitch of bronchovesicular breath sounds?
Moderate
58. What is the typical intensity of bronchovesicular breath sounds?
Moderate
59. Where are bronchovesicular breath sounds normally heard?
Around the upper sternum anteriorly and between the scapulae posteriorly.
60. Breath sounds heard over the upper sternum and between the scapulae that resemble tracheal sounds are referred to as what?
Bronchovesicular breath sounds.
61. Compared to tracheal breath sounds, bronchovesicular sounds are slightly lower in pitch and have what inspiratory-to-expiratory relationship?
Equal inspiratory and expiratory components.
62. What is the typical pitch of tracheal breath sounds?
High
63. What is the typical intensity of tracheal breath sounds?
Loud
64. Where are tracheal breath sounds normally heard?
Directly over the trachea.
65. Loud, tubular breath sounds heard over the trachea are referred to as what?
Tracheal breath sounds.
66. How does the expiratory phase of tracheal breath sounds compare to the inspiratory phase?
Equal to or slightly longer than inspiration.
67. What term describes breath sounds that are reduced in intensity?
Diminished
68. What term describes breath sounds that are extremely reduced or not heard at all?
Absent
69. What term is used when breath sounds are abnormally increased in intensity?
Harsh
70. When harsh breath sounds have an expiratory phase equal to inspiration, they are described as what?
Bronchial breath sounds
71. What term describes added sounds produced by airflow through abnormal airways?
Adventitious lung sounds
72. Adventitious lung sounds are classified into what two broad categories?
Continuous and discontinuous
73. How are discontinuous adventitious lung sounds best described?
Intermittent, crackling, or bubbling sounds of short duration.
74. What is the common name for discontinuous adventitious lung sounds?
Crackles (or rales)
75. What term is used to describe continuous adventitious lung sounds?
Wheezes
76. What term describes a quasi-musical or musical-note lung sound?
Wheeze
77. What term (now less favored) describes low-pitched, snoring-like continuous sounds caused by secretions?
Rhonchi
78. Which lung sound is synonymous with coarse crackles?
Rhonchi
79. What lung sound is loud, high-pitched, and may be heard without a stethoscope?
Stridor
80. Where is stridor most prominently heard?
Over the larynx and trachea during inhalation.
81. Is stridor classified as a continuous or discontinuous adventitious sound?
Continuous
82. Stridor is most indicative of obstruction in which part of the airway?
The larynx or trachea.
83. In which population is stridor most commonly encountered?
Infants and young children.
84. During which phase of breathing is stridor most commonly heard?
Inspiration
85. What term refers to faint, low-intensity crackles?
Fine crackles
86. What term refers to louder, more pronounced crackles?
Coarse crackles
87. Normal breath sounds originate primarily from what physiological process?
Turbulent airflow in the larger airways.
88. Diminished breath sounds occur when airflow velocity is reduced or when what is impaired?
Sound transmission through the lung or chest wall.
89. Why does shallow or slow breathing reduce breath sound intensity?
It generates less turbulent airflow.
90. Which conditions can reduce sound transmission and lead to diminished breath sounds?
Mucus plugging, hyperinflation, pleural air or fluid, anasarca, and obesity.
91. Which two adventitious sounds result from high-velocity airflow through narrowed airways?
Wheezes and stridor
92. Which adventitious lung sound signals a potentially compromised upper airway?
Stridor
93. What is the most common cause of chronic stridor?
Laryngomalacia
94. What is the most common cause of acute stridor?
Croup
95. Inspiratory stridor is most consistent with narrowing in which location?
Above the glottis
96. Expiratory stridor suggests narrowing of which airway structure?
The lower trachea
97. In adults, stridor most commonly results from what condition?
Laryngeal or subglottic edema, often following airway trauma or prolonged intubation.
98. Why should lung sounds always be compared side-to-side during auscultation?
To identify asymmetry that may indicate unilateral pathology such as pneumothorax, atelectasis, or consolidation.
99. What does a sudden change from diminished breath sounds to coarse crackles after therapy most likely indicate?
Mobilization of secretions into the larger airways.
100. Why is auscultation performed during both inspiration and expiration?
Some abnormal sounds are phase-specific and may only be heard during one part of the respiratory cycle.
Final Thoughts
Lung sounds offer vital information about airflow, lung tissue health, and potential respiratory pathology, making auscultation an essential skill for clinicians and respiratory therapists. By recognizing the characteristics of normal breath sounds and identifying adventitious sounds such as crackles, wheezes, rhonchi, stridor, and pleural friction rubs, healthcare providers can detect early signs of disease, evaluate severity, and guide appropriate treatment.
Understanding the causes behind each sound, whether obstruction, fluid, consolidation, or pleural inflammation, enhances diagnostic accuracy and supports more effective patient care.
Mastery of lung sound interpretation, combined with a systematic approach to auscultation, strengthens clinical assessment and contributes to faster, safer interventions for patients experiencing respiratory issues.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Zimmerman B, Williams D. Lung Sounds. [Updated 2023 Aug 28]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025.
- Sarkar M, Madabhavi I, Niranjan N, Dogra M. Auscultation of the respiratory system. Ann Thorac Med. 2015.