Hypoxemia occurs when the level of oxygen in the blood is lower than normal. Oxygen is essential for every cell in the body, and even small reductions can affect how organs function.
While the term may sound complex, the underlying causes are often tied to how well the lungs bring in oxygen, how effectively it moves into the bloodstream, and how it is delivered throughout the body.
Understanding the causes of hypoxemia can help individuals recognize potential problems early and seek appropriate care before serious complications develop.
Download our free guide that has over 100+ of the best tips for healthy lungs.
What Is Hypoxemia?
Hypoxemia refers specifically to a decrease in the partial pressure of oxygen in arterial blood, commonly measured as PaO2. This is different from hypoxia, which describes a lack of oxygen at the tissue level. While hypoxemia can lead to hypoxia, the two are not always the same.
In simple terms, hypoxemia means that not enough oxygen is getting into the blood from the lungs. This can happen for several reasons, including problems with breathing, lung function, or the surrounding environment.
Oxygen enters the body through the lungs, passes into the bloodstream, binds to hemoglobin in red blood cells, and is transported to tissues. Any disruption along this pathway can result in reduced oxygen levels in the blood.
How Oxygen Normally Enters the Blood
To understand the causes of hypoxemia, it helps to first understand how oxygen normally moves through the body.
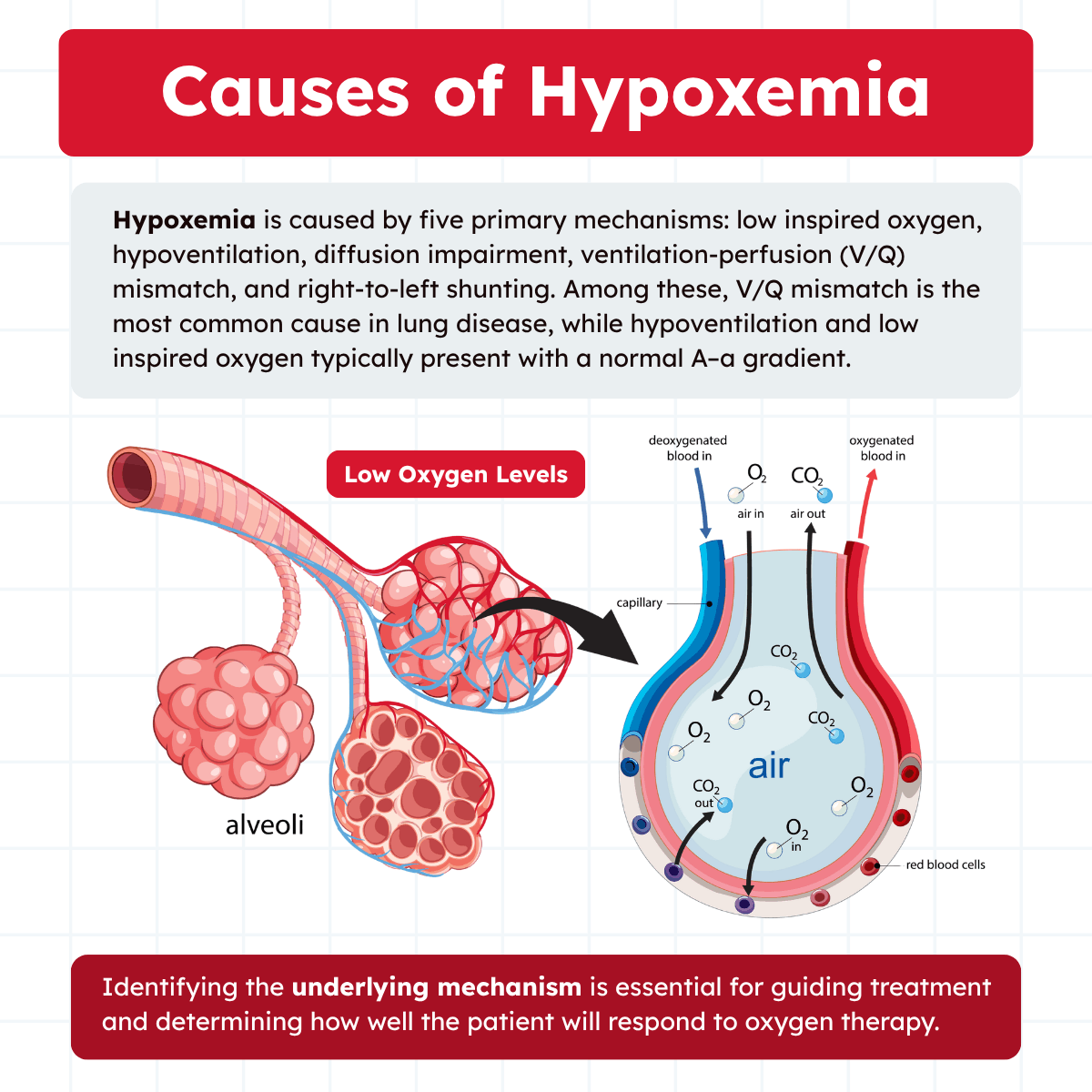
When you inhale, air travels down the airways into tiny air sacs in the lungs called alveoli. These alveoli are surrounded by small blood vessels known as capillaries. Oxygen passes from the air in the alveoli into the blood through a thin barrier called the alveolar capillary membrane.
At the same time, carbon dioxide moves from the blood into the alveoli to be exhaled. This exchange depends on several key factors:
- Adequate oxygen in the air being inhaled
- Proper airflow into the lungs
- Healthy alveoli for gas exchange
- Sufficient blood flow to the lungs
- Normal hemoglobin levels to carry oxygen
Note: When any of these factors are disrupted, hypoxemia can occur.
Major Causes of Hypoxemia
Hypoxemia is not a single disease but rather a result of several underlying mechanisms. These causes can be grouped into five main categories:
- Low inspired oxygen levels
- Hypoventilation
- Ventilation-perfusion mismatch
- Shunting
- Diffusion impairment
Note: Each of these affects a different part of the oxygen delivery process.
Low Inspired Oxygen (Low FiO2)
One of the simplest causes of hypoxemia is breathing air that contains less oxygen than normal. This is known as low inspired oxygen or low FiO2.
At sea level, the air contains about 21 percent oxygen, which is usually sufficient for normal oxygenation. However, as altitude increases, the pressure in the atmosphere decreases. This reduces the amount of oxygen available in each breath.
How It Causes Hypoxemia
Even though the percentage of oxygen in the air remains the same at higher altitudes, the lower atmospheric pressure reduces the partial pressure of oxygen. This means less oxygen is available to move into the bloodstream.
As a result:
- The oxygen pressure in the alveoli decreases
- The oxygen pressure in the blood decreases
- Oxygen delivery to tissues may be reduced
Common Examples
- High altitude travel
- Mountain climbing
- Air travel in unpressurized environments
- Hypoxia chambers used for training
Note: In this type of hypoxemia, the difference between oxygen levels in the alveoli and the blood remains normal. The issue is simply that there is not enough oxygen available to begin with.
Hypoventilation
Hypoventilation occurs when a person is not breathing deeply or frequently enough to meet the body’s needs. This leads to a buildup of carbon dioxide and a decrease in oxygen levels.
How It Causes Hypoxemia
When breathing is reduced:
- Carbon dioxide accumulates in the blood
- Oxygen levels in the alveoli decrease
- Less oxygen is available to enter the bloodstream
Note: There is a direct relationship between carbon dioxide and oxygen in the lungs. When carbon dioxide rises, oxygen tends to fall.
Common Causes of Hypoventilation
- Drug overdose, especially opioids or sedatives
- Neuromuscular disorders that weaken breathing muscles
- Brain injuries affecting the respiratory center
- Severe obesity, which restricts chest movement
- Sleep apnea
Note: Hypoventilation causes a normal gradient between the alveoli and the blood. The problem is reduced airflow rather than a defect in gas exchange.
Ventilation Perfusion (V/Q) Mismatch
Ventilation perfusion mismatch is the most common cause of hypoxemia in lung disease. It occurs when airflow and blood flow in the lungs are not properly matched.
Understanding V/Q Balance
- Ventilation refers to air reaching the alveoli
- Perfusion refers to blood reaching the alveoli
Note: For optimal oxygen exchange, these two processes must be balanced.
How It Causes Hypoxemia
When there is a mismatch:
- Some areas of the lung receive oxygen but not enough blood
- Other areas receive blood but not enough oxygen
- The result is inefficient gas exchange
Note: Even if some lung regions function normally, poorly functioning areas can lower the overall oxygen level in the blood.
Common Causes
- Chronic obstructive pulmonary disease
- Asthma
- Pneumonia
- Pulmonary embolism
- Aging-related lung changes
Note: This type of hypoxemia usually improves with supplemental oxygen, making it an important distinction in clinical settings.
Why V/Q Mismatch Is So Important
The lungs naturally have some degree of mismatch, even in healthy individuals. However, in disease states, the imbalance becomes more severe.
A key concept is that poorly ventilated areas have a greater impact on oxygen levels than well ventilated areas can compensate for. This is because hemoglobin becomes nearly fully saturated under normal conditions, so adding more oxygen to already well ventilated areas provides little additional benefit.
This explains why conditions like COPD and pneumonia can significantly lower oxygen levels, even if some parts of the lungs are still functioning well.
Shunting (Right-to-Left Shunt)
Shunting occurs when blood passes through the lungs without being exposed to oxygen. In this situation, blood flows from the right side of the heart to the left side without participating in gas exchange.
How It Causes Hypoxemia
Normally, blood travels through the lungs and picks up oxygen in the alveoli. In a shunt, some blood bypasses these ventilated areas entirely. As a result:
- Oxygen levels in that portion of blood remain low
- This poorly oxygenated blood mixes with oxygenated blood
- The overall oxygen level in the arterial blood decreases
Note: This mixing process is often referred to as venous admixture.
Types of Shunts
There are two main types of shunting:
Anatomic Shunt
An anatomic shunt occurs when blood physically bypasses the lungs. This can happen due to structural abnormalities in the heart or blood vessels.
Examples include:
- Congenital heart defects
- Abnormal vascular connections
Physiologic Shunt
A physiologic shunt occurs when blood flows through areas of the lung that are not ventilated.
Examples include:
- Atelectasis, where alveoli collapse
- Severe pneumonia, where alveoli fill with fluid
- Acute respiratory distress syndrome (ARDS)
Note: Shunting does not significantly improve with supplemental oxygen. Since the blood never reaches ventilated alveoli, increasing oxygen levels in the air has little effect on that portion of blood.
Diffusion Impairment
Diffusion impairment occurs when oxygen cannot efficiently pass from the alveoli into the blood. This process depends on a thin and healthy alveolar capillary membrane.
How It Causes Hypoxemia
Oxygen must cross a very thin barrier to enter the bloodstream. When this barrier becomes thicker or damaged:
- Oxygen transfer slows down
- Less oxygen enters the blood
- Oxygen levels in the blood decrease
Note: This effect is more noticeable during exercise, when the body requires more oxygen.
Common Causes
- Pulmonary fibrosis
- Emphysema
- Interstitial lung disease
- Pulmonary edema
Note: Diffusion problems often improve with supplemental oxygen because increasing the oxygen concentration helps drive more oxygen across the impaired membrane.
Age-Related Changes in Oxygen Levels
As people age, normal oxygen levels in the blood gradually decline. This is a natural process and does not always indicate disease.
Why Oxygen Levels Decrease With Age
Several factors contribute to this change:
- Reduced surface area for gas exchange
- Increased ventilation-perfusion mismatch
- Changes in lung elasticity
Note: Because of these factors, what is considered a normal oxygen level for a young adult may be different for an older adult.
Estimating Normal Oxygen Levels
A commonly used formula to estimate expected oxygen levels is:
Expected PaO2 = 100 − (0.323 × age in years)
This means that a PaO2 of 85 mm Hg may be normal for a 60-year-old but could indicate hypoxemia in a younger individual.
The Role of Carbon Dioxide in Hypoxemia
Carbon dioxide plays an important role in regulating oxygen levels in the lungs.
The Relationship Between CO2 and O2
Inside the lungs:
- An increase in carbon dioxide leads to a decrease in oxygen
- A decrease in carbon dioxide allows oxygen levels to rise
Note: This relationship explains why hypoventilation leads to hypoxemia. When breathing slows, carbon dioxide builds up, and oxygen levels drop.
Hyperventilation as Compensation
In some cases, the body responds to low oxygen levels by increasing the breathing rate. This reduces carbon dioxide levels and can slightly improve oxygenation. However, this compensation is limited and cannot fully correct severe hypoxemia.
Why Some Causes Are More Common Than Others
Not all causes of hypoxemia occur with the same frequency. In clinical practice, certain mechanisms are seen more often than others.
Most Common Cause: V/Q Mismatch
Ventilation-perfusion mismatch is the most common cause of hypoxemia in patients with lung disease. This is because many respiratory conditions disrupt the balance between airflow and blood flow.
Less Common Causes
- Diffusion impairment is less common at rest but becomes more significant during physical activity
- Shunting is less common but often more severe
- Low inspired oxygen is usually limited to environmental conditions
Clinical Importance
Understanding which cause is most likely helps guide treatment. For example:
- Oxygen therapy is often effective for V/Q mismatch and diffusion problems
- Shunting may require more advanced interventions
- Hypoventilation requires improving ventilation rather than just increasing oxygen
Summary of Key Mechanisms
To better understand hypoxemia, it is helpful to summarize the main causes and how they differ:
- Low inspired oxygen reduces the amount of oxygen available to the lungs
- Hypoventilation decreases airflow and raises carbon dioxide levels
- V/Q mismatch disrupts the balance between ventilation and perfusion
- Shunting allows blood to bypass oxygenation
- Diffusion impairment limits oxygen transfer across the lung membrane
Note: Each of these mechanisms affects oxygenation in a different way, but all can lead to reduced oxygen levels in the blood.
Hemoglobin and Oxygen Carrying Capacity
While hypoxemia is defined by low oxygen levels in the blood, it is important to understand that oxygen delivery depends not only on oxygen pressure but also on hemoglobin. Hemoglobin is the protein in red blood cells that binds and carries oxygen to the tissues.
Even if oxygen levels in the lungs and blood appear normal, problems with hemoglobin can reduce the amount of oxygen actually delivered to the body.
Absolute Hemoglobin Deficiency (Anemia)
An absolute deficiency occurs when there is not enough hemoglobin in the blood.
How It Affects Oxygen Delivery
- Fewer hemoglobin molecules are available to carry oxygen
- Total oxygen content in the blood decreases
- Tissues may not receive enough oxygen
Note: This means a person can have a normal PaO2 but still experience symptoms of oxygen deprivation.
Common Causes
- Blood loss from injury or surgery
- Chronic diseases affecting red blood cell production
- Nutritional deficiencies, such as iron deficiency
- Bone marrow disorders
Relative Hemoglobin Deficiency
Relative deficiencies occur when hemoglobin is present but cannot effectively carry oxygen.
Causes
- Carbon monoxide poisoning, where carbon monoxide binds strongly to hemoglobin
- Methemoglobinemia, where hemoglobin is altered and cannot bind oxygen properly
Note: A decrease in hemoglobin can reduce oxygen delivery as much as a severe drop in oxygen pressure. This highlights the importance of evaluating both oxygen levels and hemoglobin concentration.
Reduced Blood Flow (Perfusion Problems)
Oxygen delivery depends on both the oxygen content of the blood and the amount of blood flowing to the tissues. Even if oxygen levels are normal, reduced blood flow can lead to tissue hypoxia.
Circulatory Failure (Shock)
Shock is a condition where the body cannot maintain adequate blood flow to vital organs.
How It Affects Oxygen Delivery
- Reduced cardiac output limits oxygen delivery
- Tissues are deprived of oxygen
- Cells switch to anaerobic metabolism
Types of Shock
- Cardiogenic shock, caused by heart failure
- Septic shock, caused by severe infection
- Hypovolemic shock, caused by blood or fluid loss
Local Ischemia
Ischemia refers to a localized reduction in blood flow.
Examples
- Heart attack, where blood flow to part of the heart is blocked
- Stroke, where blood flow to part of the brain is interrupted
Effects
- Local tissue damage
- Accumulation of waste products
- Potential tissue death if prolonged
Note: Even when oxygen levels in the blood are normal, inadequate circulation can prevent oxygen from reaching the tissues where it is needed.
Dysoxia (Impaired Cellular Oxygen Use)
Dysoxia is a condition in which cells are unable to use oxygen effectively, even when it is delivered to them.
How It Occurs
In dysoxia:
- Oxygen reaches the tissues
- Cells cannot utilize the oxygen properly
- Energy production is impaired
Common Example: Cyanide Poisoning
Cyanide interferes with the cytochrome oxidase system in cells, which is essential for using oxygen in energy production.
As a result:
- Oxygen remains unused in the blood
- Cells switch to anaerobic metabolism
- Lactic acid builds up
Dysoxia in Critical Illness
In conditions such as severe infection or trauma:
- Oxygen consumption becomes dependent on delivery
- If delivery is insufficient, cells cannot meet their energy demands
- This leads to lactic acidosis
Note: Dysoxia is not caused by a lack of oxygen in the blood but by the inability of cells to use it. However, it still results in tissue hypoxia and can worsen clinical outcomes.
Lactic Acidosis and Oxygen Delivery
Lactic acid levels are often used to assess how well oxygen is being delivered and used in the body.
Why Lactic Acid Increases
When oxygen delivery is insufficient:
- Cells switch to anaerobic metabolism
- Lactic acid is produced as a byproduct
- Blood lactate levels rise
Clinical Importance
- Elevated lactate can indicate poor circulation or oxygen delivery
- Changes in lactate levels over time can help assess treatment effectiveness
- Persistent elevation may signal worsening tissue hypoxia
Signs and Symptoms of Hypoxemia
Hypoxemia can present with a range of symptoms depending on its severity and underlying cause.
Common Symptoms
- Shortness of breath
- Rapid breathing
- Increased heart rate
- Fatigue
- Headache
More Severe Symptoms
- Confusion or altered mental status
- Cyanosis, which is a bluish discoloration of the skin or lips
- Chest pain
- Difficulty performing normal activities
Why Symptoms Occur
These symptoms arise because the body is not receiving enough oxygen to meet its metabolic needs. The body attempts to compensate by increasing breathing and heart rate.
When to Seek Medical Attention
Recognizing the signs of hypoxemia early is important for preventing complications.
Seek Immediate Care If You Notice
- Severe shortness of breath
- Chest pain
- Blue lips or fingernails
- Sudden confusion or difficulty staying awake
Ongoing Monitoring
People with chronic lung or heart conditions may need regular monitoring of oxygen levels using devices such as pulse oximeters.
How Hypoxemia Is Diagnosed
Healthcare providers use several methods to diagnose hypoxemia.
Arterial Blood Gas (ABG)
This test measures:
- PaO2, the oxygen pressure in arterial blood
- PaCO2, the carbon dioxide level
- Blood pH
Note: It provides the most accurate assessment of oxygenation.
Pulse Oximetry
A noninvasive device placed on the finger estimates oxygen saturation in the blood.
Additional Tests
- Chest imaging to identify lung problems
- Pulmonary function tests
- Blood tests to evaluate hemoglobin levels
Treatment Depends on the Cause
The treatment of hypoxemia varies depending on the underlying cause.
Common Treatments
- Supplemental oxygen to increase oxygen levels
- Medications to treat underlying lung or heart conditions
- Mechanical ventilation in severe cases
Targeted Interventions
- Treat infections such as pneumonia
- Remove blockages such as pulmonary embolism
- Manage chronic conditions such as COPD
Note: Understanding the cause is essential for selecting the appropriate treatment.
FAQs About Hypoxemia
What Are the Primary Causes of Hypoxemia?
The primary causes of hypoxemia include hypoventilation, ventilation-perfusion (V/Q) mismatch, shunting, reduced diffusing capacity, and low inspired oxygen, such as high altitude.
Hypoventilation reduces airflow and increases carbon dioxide levels, which lowers oxygen. V/Q mismatch is the most common cause and occurs when airflow and blood flow are not properly aligned.
Shunting allows blood to bypass oxygenation, while diffusion impairment limits oxygen transfer across the lung membrane. Environmental factors like altitude reduce available oxygen in the air.
What Is One of the First Signs of Hypoxemia?
One of the earliest signs of hypoxemia is shortness of breath, especially during activity. As oxygen levels drop, the body responds by increasing breathing rate and heart rate to compensate. Individuals may also feel anxious, restless, or unable to catch their breath.
Mild hypoxemia may cause fatigue or difficulty concentrating. These early symptoms can be subtle, which is why monitoring is important, especially in people with underlying lung or heart conditions.
How Do You Fix Low Oxygen in the Blood?
Fixing low oxygen levels depends on the underlying cause. Supplemental oxygen is commonly used to increase oxygen in the blood. If hypoventilation is the issue, improving ventilation with breathing support or reversing sedative effects may be necessary.
Treating conditions like pneumonia, COPD, or pulmonary embolism is essential. In severe cases, mechanical ventilation may be required. Lifestyle changes, such as quitting smoking and managing chronic conditions, can also help improve oxygen levels over time.
What Is the Most Common Cause of Oxygen Deficiency?
The most common cause of oxygen deficiency in the blood is a ventilation-perfusion (V/Q) mismatch. This occurs when airflow and blood flow in the lungs are not properly matched.
Conditions such as COPD, asthma, pneumonia, and pulmonary embolism often lead to this imbalance.
Even if some parts of the lungs are working normally, poorly functioning areas can lower overall oxygen levels. This makes V/Q mismatch the most frequent cause of hypoxemia in clinical settings.
How Do You Reverse Hypoxemia?
Reversing hypoxemia involves correcting the underlying problem while supporting oxygen levels. Supplemental oxygen is often the first step and can quickly improve blood oxygen levels. Treating the root cause, such as infection, airway obstruction, or fluid buildup, is essential for long-term improvement.
In cases of hypoventilation, assisted ventilation may be required. For chronic conditions, medications and pulmonary rehabilitation can help maintain better oxygenation and prevent future episodes.
How Do You Know If Someone Has Hypoxemia?
Hypoxemia is typically identified through symptoms and medical testing. Common signs include shortness of breath, rapid breathing, fatigue, confusion, and bluish discoloration of the lips or fingertips.
A pulse oximeter can provide a quick estimate of oxygen saturation, while an arterial blood gas test offers precise measurement of oxygen levels in the blood. If symptoms are present or oxygen levels are low, further evaluation is needed to determine the underlying cause.
What Causes Hypoxemia at Night?
Hypoxemia at night is often caused by conditions that affect breathing during sleep. Obstructive sleep apnea is a common cause, where the airway collapses and temporarily blocks airflow.
Other causes include obesity hypoventilation syndrome, chronic lung diseases, and reduced respiratory drive during sleep.
Lying flat can also worsen oxygen levels in some individuals. These factors can lead to repeated drops in oxygen levels throughout the night, disrupting sleep and affecting overall health.
What Causes Hypoxemia in COPD?
In COPD, hypoxemia is primarily caused by ventilation-perfusion mismatch. Damaged airways and alveoli lead to poor airflow in some areas of the lungs while blood flow continues, resulting in inefficient gas exchange.
In more advanced stages, destruction of lung tissue and mucus buildup further impair oxygen transfer. Some patients may also develop shunting or hypoventilation. Over time, these changes reduce oxygen levels in the blood and may require long-term oxygen therapy.
Can Someone Die From Hypoxemia?
Yes, severe or untreated hypoxemia can be life-threatening. When oxygen levels drop too low, vital organs such as the brain and heart cannot function properly. This can lead to confusion, loss of consciousness, organ failure, and eventually death.
The risk depends on how low the oxygen levels are and how long they remain untreated. Prompt recognition and treatment are critical to prevent serious complications and improve outcomes.
What Medical Conditions Cause Hypoxemia?
Many medical conditions can cause hypoxemia, particularly those affecting the lungs, heart, or blood. Common examples include COPD, asthma, pneumonia, pulmonary embolism, pulmonary fibrosis, and acute respiratory distress syndrome.
Heart conditions that affect blood flow can also contribute. In addition, anemia and carbon monoxide poisoning can impair oxygen delivery. These conditions disrupt different parts of the oxygen pathway, leading to reduced oxygen levels in the blood.
When to See a Doctor for Hypoxemia?
You should seek medical attention if you experience persistent or worsening shortness of breath, chest pain, confusion, or bluish discoloration of the lips or skin. Sudden or severe symptoms require immediate emergency care.
Individuals with chronic lung or heart conditions should monitor their oxygen levels regularly and report any significant changes. Early evaluation and treatment can help prevent complications and ensure that underlying causes are properly managed.
Final Thoughts
Hypoxemia is a condition that reflects a disruption in the body’s ability to deliver oxygen to the blood and ultimately to the tissues. It can result from environmental factors, breathing problems, lung diseases, circulation issues, or even cellular dysfunction.
Each cause affects a different step in the oxygen delivery pathway, which is why identifying the underlying mechanism is so important.
By understanding the causes and recognizing early signs, individuals can take appropriate action, and healthcare providers can deliver targeted treatment to restore adequate oxygen levels and protect vital organ function.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Sarkar M, Niranjan N, Banyal PK. Mechanisms of hypoxemia. Lung India. 2017.


