Coughing up mucus is a common experience that can range from mildly bothersome to more concerning, depending on the underlying cause. It often occurs during respiratory infections such as the common cold or influenza, but it can also result from allergies, environmental irritants, or chronic lung conditions.
Mucus plays a vital role in protecting the respiratory system. It traps dust, bacteria, viruses, and other harmful particles before they reach deeper parts of the lungs. However, when mucus production increases or becomes persistent, it may indicate an underlying issue that requires attention.
Understanding why you are coughing up mucus is the first step toward choosing the right treatment and protecting your long-term respiratory health.
Download our free guide that has over 100+ of the best tips for healthy lungs.
What It Means to Cough Up Mucus
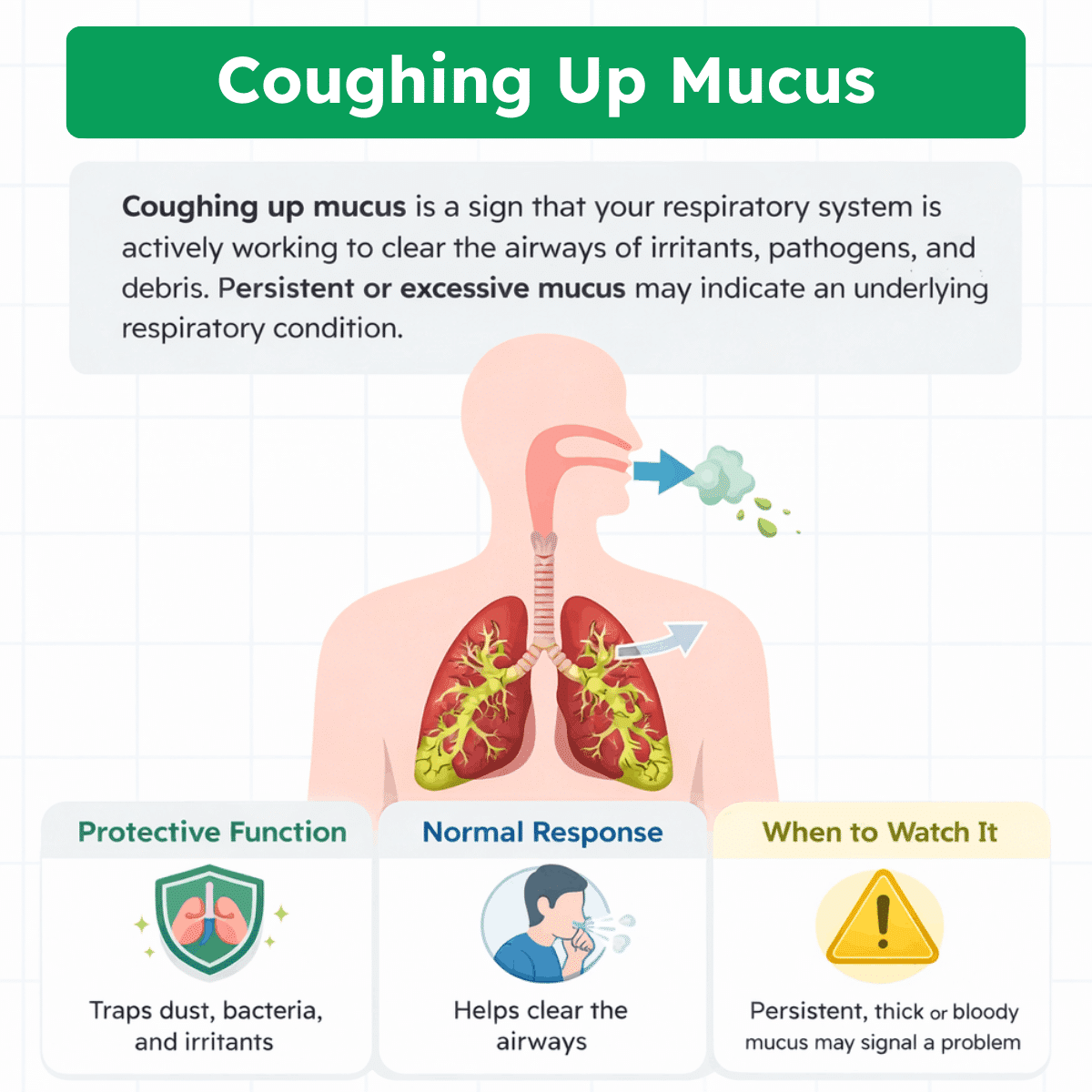
Coughing up mucus is a sign that your respiratory system is actively working to clear the airways. The lining of the lungs and airways produces mucus to trap inhaled particles such as dust, allergens, bacteria, and viruses. When these substances accumulate, the body triggers a cough reflex to expel the mucus and keep the airways clear.
In many situations, this is a normal and protective response. It commonly occurs during infections or after exposure to irritants like smoke or pollution. However, frequent or excessive mucus production may point to an underlying condition such as allergies, chronic bronchitis, or another respiratory disorder.
The color, thickness, and amount of mucus can offer valuable clues about what is happening inside the lungs. These characteristics help guide further evaluation and determine whether treatment is necessary.
Types of Mucus Produced
The appearance of mucus often reflects the underlying cause.
- Clear mucus is commonly seen with viral infections, allergies, or mild airway irritation.
- White or gray mucus may indicate congestion or early-stage infection and is often associated with conditions that slow mucus clearance.
- Yellow or green mucus typically reflects an active immune response. White blood cells release enzymes that can change the color during infection.
- Brown, rust-colored, or blood-streaked mucus may result from old blood, smoking-related airway damage, or more serious conditions such as pneumonia or lung injury. Thick, sticky mucus is more common in asthma, cystic fibrosis, and chronic bronchitis.
Note: Mucus color alone does not confirm a diagnosis. However, changes in color, volume, or consistency can provide important clinical clues.
Normal Mucus vs. Concerning Mucus
Small amounts of clear or white mucus during a cold or allergy flare are usually normal. The body increases mucus production to trap irritants and help clear infection. Mucus becomes concerning when it persists for more than three weeks, increases significantly in volume, or appears alongside additional symptoms. These may include fever above 100.4°F, chest pain, shortness of breath, wheezing, or coughing up blood.
Foul-smelling mucus or thick green sputum with a high fever may suggest a bacterial infection. Blood in the mucus, even in small amounts, should always be evaluated by a healthcare professional.
Chronic daily mucus production, particularly in smokers or individuals with lung disease, often signals ongoing airway inflammation. Changes from a person’s usual pattern are often the most important warning sign.
Causes of Coughing Up Mucus
Coughing up mucus usually indicates irritation or inflammation within the airways. Common causes include infections, chronic lung diseases, environmental exposures, and allergic reactions.
Acute Respiratory Infections
Acute respiratory infections are among the most common causes of mucus production. Viruses such as the common cold, influenza, and respiratory syncytial virus infect the airways and trigger inflammation.
In response, the body produces more mucus to trap and remove pathogens. This mucus may appear clear, white, yellow, or green. These color changes often reflect immune activity rather than a specific type of infection.
Acute bronchitis frequently causes a productive cough that can last up to three weeks. Pneumonia can also lead to thick mucus production, often accompanied by fever, chest pain, and shortness of breath.
Note: Most viral infections improve with rest and supportive care. Antibiotics are only necessary when a bacterial infection is confirmed.
Chronic Conditions
Chronic respiratory diseases are a common cause of persistent mucus production. Chronic obstructive pulmonary disease (COPD), which includes chronic bronchitis and emphysema, leads to long-term airway inflammation and narrowing.
Individuals with chronic bronchitis typically produce mucus daily for at least three months in two consecutive years. Symptoms often worsen in the morning due to mucus accumulation overnight.
Asthma can also contribute to excess mucus production. In this condition, airway inflammation and bronchospasm combine with increased mucus secretion, especially during flare-ups. Bronchiectasis involves permanent widening of the airways. This structural change allows mucus to collect and increases the risk of repeated infections and chronic productive coughing.
Environmental and Lifestyle Factors
Environmental irritants directly stimulate mucus production in the airways. Cigarette smoking remains the leading lifestyle cause of chronic mucus production. Smoke damages the cilia, which are tiny hair-like structures responsible for moving mucus out of the lungs. When cilia function is impaired, mucus accumulates and triggers frequent coughing.
Air pollution, chemical fumes, and occupational dust exposure can produce similar effects. Individuals working in construction, mining, or industrial settings may face increased risk without proper protective measures.
Cold, dry air can also irritate sensitive airways. Repeated exposure may worsen symptoms, particularly in individuals with underlying respiratory conditions.
Allergic Reactions
Allergic reactions increase mucus production through activation of the immune system. When allergens such as pollen, dust mites, mold spores, or pet dander are inhaled, the body releases histamine and other inflammatory mediators.
This response causes swelling of the airways and increased mucus production. The goal is to trap and remove the allergen from the respiratory tract.
Postnasal drip often develops as a result. Mucus drains from the nasal passages into the throat, leading to coughing and a frequent need to clear the throat.
Note: Allergies can also worsen asthma symptoms. This combination may lead to thicker mucus and more frequent productive coughing episodes.
Color and Consistency of Mucus
The color and texture of mucus provide important insight into what is occurring within the respiratory system. These changes often reflect inflammation, infection, irritation, or bleeding.
Clear or White Mucus
Clear mucus is common and often normal. It is continuously produced to trap dust, allergens, and microorganisms. When present during a cold or allergy flare, it typically indicates irritation rather than a bacterial infection.
White mucus is slightly thicker and may develop when nasal passages become swollen, slowing mucus drainage. This often occurs during congestion associated with colds or sinus inflammation.
Thick white mucus can create a sensation of heaviness or blockage in the chest. However, it does not automatically indicate the need for antibiotics. In most cases, hydration, rest, and time allow the body to clear it effectively.
Yellow or Green Mucus
Yellow or green mucus often appears when the immune system is actively responding to infection. White blood cells release enzymes that can change the color of mucus during this process. It is a common misconception that green mucus always indicates a bacterial infection. Viral infections can also produce these colors, especially after several days of symptoms.
The more important factors are duration and severity. Persistent fever, chest pain, shortness of breath, or worsening cough may indicate a more serious condition such as pneumonia or bronchitis.
In chronic conditions such as COPD or cystic fibrosis, changes in mucus color should be evaluated in the context of the individual’s baseline pattern.
Brown, Red, or Pink Mucus
Brown mucus may contain old blood or inhaled particles such as smoke or dust. This is more common in individuals who smoke or work in polluted environments. Red or pink mucus usually indicates the presence of fresh blood. Small streaks may result from irritated airways due to frequent coughing. However, persistent or increasing blood requires medical evaluation.
Possible causes include severe infection, pulmonary embolism, or lung cancer. Pink, frothy mucus may indicate fluid accumulation in the lungs, often seen in heart failure, and requires immediate medical attention.
Associated Symptoms
Coughing up mucus often occurs alongside other respiratory or systemic symptoms. These additional signs help determine whether the cause is mild irritation, infection, or a more serious condition.
Shortness of Breath
Shortness of breath may indicate that mucus is obstructing the airways or that inflammation has narrowed the bronchial passages. It can present as chest tightness, difficulty taking a full breath, or rapid breathing during minimal activity.
As mucus thickens and accumulates, airflow becomes restricted and gas exchange is less efficient. This commonly occurs in asthma, chronic bronchitis, pneumonia, and chronic obstructive pulmonary disease.
Symptoms may worsen when lying flat or during physical exertion. In more severe cases, individuals may struggle to speak in full sentences without pausing for air.
Seek urgent medical care if shortness of breath occurs with:
- Bluish lips or fingertips
- Rapid heart rate
- Confusion or dizziness
- Severe chest retractions
Note: Persistent or worsening breathlessness requires prompt medical evaluation, especially in individuals with a history of lung disease.
Chest Pain
Chest pain associated with mucus production is often caused by airway inflammation or repeated forceful coughing. The discomfort may feel sharp, burning, or aching. Inflamed lung tissue can cause pain that worsens with deep breathing or coughing, which is common in bronchitis and pneumonia.
Prolonged coughing can also strain the muscles between the ribs, leading to localized tenderness that is reproducible with touch.
However, chest pain that feels heavy, crushing, or radiates to the arm, neck, or jaw may indicate a cardiac issue. Pain accompanied by sweating, nausea, or shortness of breath requires immediate medical attention.
Note: Blood-tinged mucus combined with sharp chest pain may suggest a serious condition such as pulmonary embolism or severe infection and should not be ignored.
Wheezing
Wheezing is a high-pitched whistling sound that occurs when air flows through narrowed airways. It is often more noticeable during exhalation. Inflammation, bronchospasm, and mucus buildup can all restrict airflow and lead to wheezing. This symptom is common in asthma and allergic reactions, but may also occur during respiratory infections.
Some individuals experience intermittent wheezing that worsens at night or with exercise, while others may develop persistent wheezing during illness. When wheezing occurs alongside thick mucus production, it may indicate significant airway obstruction. If breathing becomes labored or noisy at rest, medical attention is required.
Note: In smokers, new or worsening wheezing may signal progression of chronic lung disease and should be evaluated.
Fever
Fever is often a sign of infection rather than simple airway irritation. A body temperature above 100.4°F (38°C) typically reflects an active immune response. When fever accompanies a productive cough, conditions such as pneumonia, influenza, or acute bronchitis become more likely. Fever may also occur with sinus infections that lead to postnasal drip.
High fever, chills, fatigue, body aches, and headache often occur together during systemic infections.
Fever lasting more than three days, or temperatures exceeding 102°F, should be evaluated by a healthcare provider. In older adults and immunocompromised individuals, even mild fever can indicate a serious condition.
Note: Monitoring temperature and tracking symptom progression helps guide appropriate treatment decisions.
When to Seek Medical Attention
While many cases of mucus production resolve on their own, certain symptoms require prompt medical evaluation. Recognizing these warning signs can help prevent complications.
Warning Signs
Immediate medical attention is necessary if a person coughs up bright red blood, large amounts of blood, or mucus mixed with clots.
Shortness of breath at rest, chest pain that worsens with breathing, or a persistent feeling of chest tightness also requires urgent care. These symptoms may indicate pneumonia, pulmonary embolism, or another serious condition.
Additional warning signs include high fever above 102°F (39°C), confusion, bluish lips or fingertips, or severe weakness.
Note: Pink, frothy mucus combined with difficulty breathing may signal fluid in the lungs and requires emergency care.
Persistent or Worsening Symptoms
A cough that produces mucus for more than three weeks should not be ignored. Persistent symptoms may suggest chronic bronchitis, asthma, or an unresolved infection. Changes in mucus consistency, color, or odor, especially when accompanied by fever or chest pain, may indicate a bacterial infection.
Worsening cough, increasing fatigue, or new-onset wheezing are also reasons to seek medical evaluation. These changes may indicate that the condition is progressing rather than improving.
Symptoms such as unexplained weight loss, night sweats, or persistent hoarseness alongside mucus production should be investigated further.
Underlying Health Risks
Individuals with chronic lung conditions such as asthma, COPD, cystic fibrosis, or bronchiectasis should contact a healthcare provider if mucus production increases suddenly. Those with heart disease, diabetes, or weakened immune systems are at higher risk for complications and may require earlier intervention.
Smokers and former smokers should seek evaluation if they notice new or changing cough patterns, as persistent mucus production may require imaging or lung function testing.
Infants, older adults, and pregnant individuals should also be monitored closely, as their symptoms may worsen more rapidly.
Diagnostic Process for Coughing Up Mucus
Diagnosing the cause of mucus production involves a detailed medical history, physical examination, and targeted diagnostic testing. Each step helps identify whether the source is infection, chronic disease, or another condition.
Medical History Assessment
The clinician begins by evaluating symptom duration and progression. This helps distinguish acute causes, such as viral infections, from chronic conditions like asthma or COPD.
Questions about mucus characteristics, including color, thickness, volume, and the presence of blood, provide important diagnostic clues. Exposure history is also critical. Smoking status, occupational hazards, environmental exposures, and recent travel may contribute to symptoms.
Associated symptoms such as fever, chest pain, shortness of breath, wheezing, weight loss, and night sweats help narrow the diagnosis.
Medication use and past medical history are also reviewed. Certain medications, such as ACE inhibitors, can trigger cough, while existing lung disease increases the likelihood of chronic mucus production.
Physical Examination
The physical exam focuses on breathing patterns, respiratory effort, and the use of accessory muscles. Lung sounds are assessed using a stethoscope. Wheezing may suggest airway narrowing, while crackles may indicate infection or fluid in the lungs. Decreased breath sounds can point to obstruction or lung collapse.
Oxygen saturation is measured using a pulse oximeter. Low readings may require urgent evaluation.
The clinician also examines the nose and throat for signs of postnasal drip or inflammation. Additional findings, such as swollen lymph nodes or fluid retention, may indicate systemic illness or heart-related causes.
Diagnostic Tests
Diagnostic testing depends on the suspected condition. A chest X-ray is often the first imaging study used to detect pneumonia, masses, or structural abnormalities. If chronic lung disease is suspected, spirometry may be performed to evaluate airflow and diagnose conditions such as asthma or COPD.
Sputum analysis can identify infectious organisms or inflammatory markers. In some cases, cultures may be used to detect bacterial infections. Blood tests may assess infection, inflammation, or allergic responses. In more complex cases, a CT scan provides detailed imaging of lung structures.
Note: These diagnostic tools help confirm the cause and guide appropriate treatment.
Common Conditions Linked to Coughing Up Mucus
Several respiratory conditions commonly cause a mucus-producing cough. While these conditions vary in severity and cause, they all involve inflammation or irritation of the airways.
Bronchitis
Bronchitis occurs when the bronchial tubes become inflamed, leading to increased mucus production. It often develops after a viral respiratory infection.
- Acute bronchitis typically lasts less than three weeks and causes a persistent cough with clear, white, yellow, or green mucus. Other symptoms may include chest discomfort, fatigue, and mild shortness of breath. Most cases are viral, so antibiotics are usually not required. Treatment focuses on rest, hydration, and symptom management.
- Chronic bronchitis is a form of chronic obstructive pulmonary disease. It is defined by a productive cough lasting at least three months per year for two consecutive years. Smoking is the leading cause. Long-term airway irritation leads to excessive mucus production and narrowing of the airways, resulting in daily coughing and breathing difficulty.
Pneumonia
Pneumonia is an infection of the lung tissue that causes the air sacs to fill with fluid or pus. It may be caused by bacteria, viruses, or fungi. A productive cough with thick mucus is common. The mucus may appear yellow, green, or rust-colored, especially in bacterial pneumonia.
Other symptoms include fever, chills, chest pain that worsens with breathing, rapid breathing, and fatigue. Older adults may present with confusion instead of typical respiratory symptoms.
Bacterial pneumonia often requires antibiotics, while viral cases are usually treated with supportive care unless severe.
Note: Individuals with chronic illness, weakened immune systems, or advanced age are at higher risk for complications and should seek prompt evaluation.
Asthma
Asthma is a chronic inflammatory condition that narrows the airways and increases mucus production. It makes the lungs more sensitive to environmental triggers. During an asthma flare, individuals may cough up thick, sticky mucus along with wheezing, chest tightness, and shortness of breath.
Common triggers include allergens, respiratory infections, cold air, smoke, and exercise. Symptoms often worsen at night or early in the morning.
Treatment typically includes inhaled bronchodilators to relax airway muscles and inhaled corticosteroids to reduce inflammation and mucus production.
Note: Consistent management helps prevent flare-ups and improves long-term respiratory function.
Treatment Options
Effective treatment depends on the underlying cause, the thickness of the mucus, and whether infection or inflammation is present. Options range from over-the-counter remedies to prescription medications and supportive home care.
Over-the-Counter Remedies
Over-the-counter treatments can help thin mucus and make it easier to clear. Expectorants such as guaifenesin increase water content in mucus, improving clearance when combined with adequate hydration.
Decongestants like pseudoephedrine reduce nasal swelling and may decrease postnasal drip. Individuals with high blood pressure or heart conditions should use them with caution.
Saline nasal sprays help loosen mucus and reduce irritation. They are safe for regular use and support airway moisture.
Cough suppressants containing dextromethorphan may reduce coughing frequency, but they should be used carefully. Suppressing a productive cough can prevent the body from clearing mucus effectively.
Prescription Medications
When infection is present, targeted medications may be necessary. Antibiotics are used to treat confirmed bacterial infections but are not effective against viruses. Chronic conditions such as asthma or COPD often require inhaled medications. Inhaled corticosteroids reduce inflammation, while bronchodilators improve airflow by relaxing airway muscles.
Mucolytics, such as acetylcysteine, may be prescribed to break down thick mucus and improve clearance. If allergies are the primary cause, prescription antihistamines or nasal steroid sprays can help reduce the immune response and limit mucus production.
Note: Accurate diagnosis ensures appropriate treatment and avoids unnecessary medication use.
Home Care Strategies
Simple home care measures can significantly improve mucus clearance. Staying well hydrated helps keep mucus thin and easier to expel. Using a cool-mist humidifier adds moisture to dry air, which can soothe irritated airways and reduce mucus thickness. Regular cleaning is essential to prevent bacterial or mold growth.
Warm showers or steam inhalation may provide temporary relief by loosening mucus. Care should be taken to avoid overly hot steam.
Note: Rest supports immune function during illness, while avoiding smoke, dust, and strong chemical fumes helps reduce ongoing airway irritation.
Preventive Measures
Preventing excessive mucus production involves minimizing exposure to irritants, maintaining good hygiene, and supporting overall lung health through consistent habits.
Hygiene Practices
Frequent handwashing reduces the spread of viruses and bacteria that cause respiratory infections. Hands should be washed for at least 20 seconds, especially after coughing, sneezing, or being in public places.
Avoid touching the face, as pathogens often enter through the nose and mouth. When soap and water are unavailable, alcohol-based hand sanitizers provide effective protection.
Regular cleaning of frequently touched surfaces, such as phones, keyboards, and door handles, helps reduce exposure. Covering the mouth and nose when coughing and wearing a mask in crowded or poorly ventilated areas can further limit the spread of infection.
Note: Maintaining good indoor air quality by replacing HVAC filters and using air purifiers can also support respiratory health.
Lifestyle Modifications
Avoiding tobacco smoke is one of the most effective ways to reduce mucus production and protect lung function. Both active smoking and secondhand exposure can damage the airways. Staying hydrated supports normal mucus consistency and clearance. Regular fluid intake is important unless restricted by a medical condition.
Engaging in regular physical activity helps improve lung capacity and promotes airway clearance. Activities such as walking, cycling, or swimming support respiratory strength. Managing allergies by avoiding triggers and maintaining a clean environment can reduce chronic mucus production.
Note: A balanced diet, adequate sleep, and overall healthy habits support immune function and respiratory health.
Impact on Daily Life
Coughing up mucus can interfere with daily activities and overall comfort, particularly when symptoms persist or worsen over time.
Sleep Disturbances
Mucus often accumulates at night when lying flat, leading to coughing that disrupts sleep. This can result in frequent awakenings and reduced sleep quality.
Over time, poor sleep may lead to fatigue, irritability, and decreased concentration during the day. Elevating the head during sleep and staying hydrated may help reduce nighttime symptoms.
Effect on Physical Activities
Excess mucus can limit physical endurance by narrowing the airways and making breathing less efficient. Activities such as climbing stairs or exercising may trigger coughing episodes.
Some individuals may avoid physical activity due to discomfort or embarrassment, while others may need to reduce intensity or take frequent breaks. Persistent symptoms can reduce stamina and overall activity levels, especially in those with underlying lung conditions.
Risks of Ignoring Symptoms
Ignoring persistent mucus production can allow underlying conditions to worsen over time. Early evaluation often prevents complications and improves outcomes. Untreated infections such as bronchitis or pneumonia can spread and lead to more severe illness, including breathing difficulty and prolonged recovery.
Chronic conditions such as asthma and COPD may progress if inflammation is not controlled, potentially causing long-term lung damage.
Warning signs that should not be ignored include:
- Blood in mucus
- Mucus lasting more than three weeks
- Unexplained weight loss
- Shortness of breath
- Severe fatigue
Note: Prompt medical evaluation helps identify serious causes and allows for timely treatment.
Long-Term Outlook
The long-term outlook depends on the underlying cause of mucus production. Acute infections typically resolve within a few weeks without lasting effects. Chronic conditions require ongoing management. Individuals with asthma, chronic bronchitis, or COPD may experience recurring symptoms but can maintain stability with proper treatment.
Key factors that influence long-term outcomes include:
- Smoking status
- Exposure to air pollution
- Allergy control
- Medication adherence
- Presence of chronic lung disease
Quitting smoking, avoiding irritants, and following prescribed treatment plans significantly improve outcomes. Some conditions, such as bronchiectasis or cystic fibrosis, require long-term care and regular monitoring. Early diagnosis and consistent follow-up reduce complications.
Changes in mucus color, volume, or consistency should prompt reevaluation. With proper care and healthy lifestyle choices, many individuals can effectively manage symptoms and maintain a good quality of life.
FAQs About Coughing Up Mucus
How Can I Get Mucus Out of My Lungs?
Clearing mucus from the lungs involves thinning it and improving airway clearance. Staying well hydrated helps keep mucus less sticky and easier to cough up. Using a humidifier or inhaling steam can loosen secretions. Gentle activity, deep breathing exercises, and controlled coughing techniques can also help move mucus upward.
In some cases, expectorants like guaifenesin may be useful. If mucus is persistent or difficult to clear, a healthcare provider may recommend airway clearance therapy or prescribe medications.
What Causes Coughing Up Clear Phlegm with Bubbles?
Clear, bubbly phlegm is often associated with excess fluid or mild airway irritation. It commonly occurs with viral infections, allergies, or postnasal drip. In some cases, foamy mucus can also be linked to conditions that involve fluid buildup in the lungs, such as heart failure.
The key is to evaluate accompanying symptoms. If the mucus is persistent or appears alongside shortness of breath, chest discomfort, or fatigue, medical evaluation is recommended to rule out more serious causes.
Why Am I Coughing Up Phlegm but Not Sick?
Coughing up phlegm without feeling sick is often due to non-infectious causes. Common triggers include allergies, postnasal drip, air pollution, smoking, or chronic conditions like asthma or chronic bronchitis.
These factors irritate the airways and increase mucus production even in the absence of infection. Gastroesophageal reflux can also contribute by irritating the throat and airways.
Note: If symptoms persist or worsen over time, it may indicate an underlying condition that requires further evaluation.
What Does It Mean to Cough Up Bloody Mucus?
Coughing up bloody mucus, known as hemoptysis, can range from minor to serious. Small streaks of blood may result from irritated airways after frequent coughing. However, larger amounts or persistent bleeding can signal more serious conditions such as pneumonia, pulmonary embolism, or lung cancer.
It may also occur in chronic lung diseases like bronchiectasis. Any unexplained blood in mucus should be evaluated by a healthcare provider to determine the cause and rule out serious conditions.
Does Coughing Up Mucus Mean I’m Getting Better?
In some cases, coughing up mucus can be a sign that your body is clearing infection or irritants from the airways. As mucus loosens and becomes easier to expel, it may indicate improvement. However, this is not always the case.
Persistent or worsening mucus production, especially when accompanied by fever, shortness of breath, or chest pain, may suggest ongoing illness. The overall trend of symptoms, rather than mucus alone, provides the most accurate indication of recovery.
Can COVID-19 Make You Cough Up Mucus?
Yes, COVID-19 can cause a productive cough, although a dry cough is more common. Some individuals develop mucus production as the infection affects the lower respiratory tract. The mucus may be clear, white, or occasionally colored depending on inflammation and immune response.
In more severe cases, pneumonia associated with COVID-19 can lead to thicker mucus and breathing difficulty. Persistent cough, worsening symptoms, or shortness of breath should prompt medical evaluation.
Is It Good to Spit Out Mucus When Sick?
Yes, it is generally beneficial to spit out mucus rather than swallow it when you are sick. Expelling mucus helps remove trapped bacteria, viruses, and debris from the respiratory system. This supports the body’s natural defense mechanisms and may reduce irritation in the airways.
Note: Swallowing mucus is not harmful, as it will be broken down in the digestive system, but clearing it from the lungs can help improve breathing and reduce coughing.
Can Coughing Up Mucus Make Your Throat Sore?
Yes, frequent coughing and mucus production can irritate the throat and lead to soreness. The repeated force of coughing places strain on throat tissues, while mucus itself can cause inflammation as it passes through.
Postnasal drip can further contribute to throat irritation and discomfort. Staying hydrated, using lozenges, and managing the underlying cause of mucus production can help relieve symptoms. If throat pain is severe or persistent, further evaluation may be needed.
Can Coughing Up Mucus Be a Sign of Pregnancy?
Coughing up mucus is not a typical or direct sign of pregnancy. However, hormonal changes during pregnancy can increase nasal congestion and mucus production, which may lead to postnasal drip and occasional coughing.
This is sometimes referred to as pregnancy rhinitis. If mucus production is accompanied by other respiratory symptoms such as fever, chest pain, or shortness of breath, it is more likely related to an infection or another condition rather than pregnancy.
Does Coughing Up Mucus Always Mean Infection?
No, coughing up mucus does not always indicate an infection. While infections are a common cause, mucus production can also result from allergies, asthma, smoking, air pollution, or chronic lung diseases.
The body produces mucus as a protective response to irritation, not just infection. Evaluating other symptoms such as fever, fatigue, and duration of illness helps determine the cause. Persistent or unexplained mucus production should be assessed by a healthcare provider.
Final Thoughts
Coughing up mucus is often the body’s natural way of clearing the airways, but it can also signal an underlying issue when it becomes persistent or is accompanied by concerning symptoms. Paying attention to changes in mucus color, consistency, and frequency can provide valuable insight into your respiratory health.
While many cases resolve with simple care and time, others may require medical evaluation and targeted treatment. By recognizing warning signs early and adopting healthy habits, you can protect your lungs and maintain optimal breathing function.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- McShane A, Bath J, Jaramillo AM, Ridley C, Walsh AA, Evans CM, Thornton DJ, Ribbeck K. Mucus. Curr Biol. 2021.
- Farzan S. Cough and Sputum Production. In: Walker HK, Hall WD, Hurst JW, editors. Clinical Methods: The History, Physical, and Laboratory Examinations. 3rd edition. Boston: Butterworths; 1990.