The cardiovascular system is one of the most vital systems in the human body, responsible for transporting blood, nutrients, oxygen, and waste products throughout the body.
It consists of the heart, blood vessels, and blood, all working together to ensure that cells receive the oxygen and nutrients they need while removing waste.
Understanding the cardiovascular system is crucial for grasping how the body maintains homeostasis and supports life. In this article, we’ll explore the key components of the cardiovascular system and their essential roles in keeping the body functioning.
What is the Cardiovascular System?
The cardiovascular system, also known as the circulatory system, is a complex network responsible for transporting blood, nutrients, oxygen, hormones, and waste products throughout the body. It consists primarily of the heart, blood vessels (arteries, veins, and capillaries), and blood.
The heart acts as the central pump, propelling oxygen-rich blood from the lungs to the rest of the body through the arteries and returning oxygen-poor blood back to the lungs via veins for re-oxygenation.
This continuous circulation ensures that the body’s tissues receive the essential nutrients and oxygen needed for cellular function, while waste products like carbon dioxide are removed. The cardiovascular system also plays a key role in regulating body temperature, maintaining pH balance, and supporting the immune system.
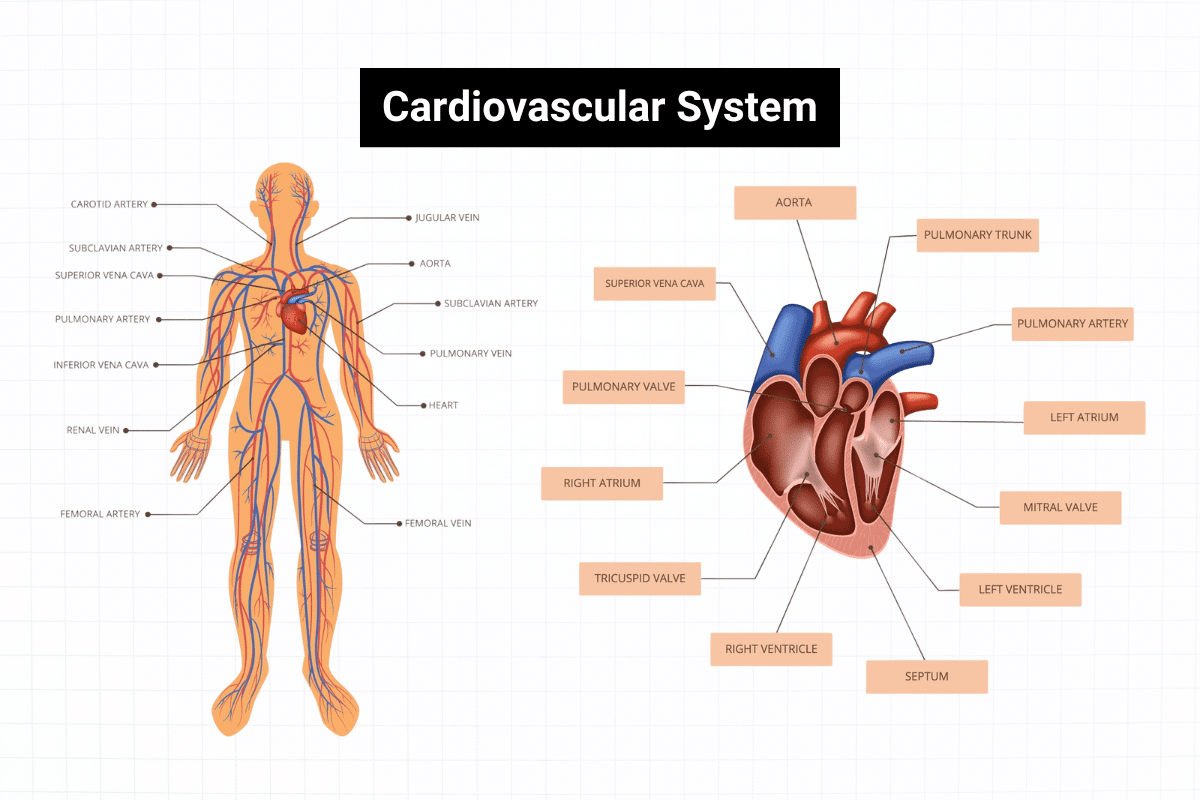
Structures of the Cardiovascular System
The cardiovascular system consists of several key structures that work together to maintain blood circulation and overall health.
These structures include:
- Heart
- Blood vessels
- Blood
- Lymph
- Lymphatic vessels
Heart
The heart is a muscular organ at the center of the cardiovascular system, responsible for pumping blood throughout the body. It has four chambers—two atria and two ventricles—that work together to ensure oxygenated blood is delivered to tissues while deoxygenated blood is sent to the lungs for oxygenation.
The heart functions through a coordinated rhythm of contractions, regulated by electrical impulses, which keeps the circulation steady and efficient.
Blood Vessels
Blood vessels form a vast network of tubes that transport blood to every part of the body. They include arteries, veins, and capillaries, each serving a unique role. Arteries carry oxygen-rich blood away from the heart, while veins return deoxygenated blood back to the heart.
Capillaries are the smallest blood vessels, where the exchange of oxygen, nutrients, and waste products takes place between blood and tissues. This interconnected system ensures that blood is circulated efficiently to maintain proper body function.
Blood
Blood is the life-sustaining fluid that circulates through the cardiovascular system, delivering oxygen and nutrients to cells while removing waste products like carbon dioxide. It consists of red blood cells, white blood cells, platelets, and plasma.
Red blood cells carry oxygen, white blood cells defend the body against infections, platelets help in blood clotting, and plasma is the liquid component that transports nutrients, hormones, and waste. Blood plays a critical role in maintaining homeostasis, regulating body temperature, and supporting immune responses.
Lymph
Lymph is a clear, watery fluid that originates from interstitial fluid surrounding tissues. It plays a crucial role in the body’s immune system by transporting white blood cells and removing waste, toxins, and other unwanted materials from the body.
Unlike blood, lymph circulates through a separate network of vessels known as the lymphatic system, eventually returning to the bloodstream. Lymph is essential for maintaining fluid balance and supporting immune function by filtering harmful substances and aiding in the body’s defense against infections.
Lymphatic Vessels
Lymphatic vessels are part of the lymphatic system, responsible for transporting lymph throughout the body. These vessels work in parallel with blood vessels but carry lymph instead of blood.
Starting as tiny capillaries in tissues, they merge into larger vessels that eventually drain into the bloodstream. Along the way, lymphatic vessels pass through lymph nodes, which filter out harmful pathogens and debris.
The lymphatic system plays a crucial role in immune defense, fluid balance, and the absorption of fats and fat-soluble nutrients from the digestive system.
Blood Flow Through the Heart
Blood flow through the heart is a continuous and coordinated process that ensures oxygen-rich blood is delivered to the body while oxygen-poor blood is sent to the lungs for oxygenation.
It begins when deoxygenated blood from the body enters the right atrium through the superior and inferior vena cavae. From there, the blood passes through the tricuspid valve into the right ventricle.
When the right ventricle contracts, the blood is pushed through the pulmonary valve into the pulmonary arteries and transported to the lungs, where it receives oxygen and releases carbon dioxide.
The now oxygen-rich blood returns to the heart via the pulmonary veins into the left atrium. It then flows through the mitral valve into the left ventricle. When the left ventricle contracts, the blood is ejected through the aortic valve into the aorta, which distributes the oxygenated blood to the rest of the body.
Note: This cyclical process is vital for maintaining oxygen delivery to tissues and organs, ensuring overall health and function.

Cardiovascular System Practice Questions
1. What is the cardiovascular system responsible for?
The cardiovascular system is responsible for transporting metabolites to and from tissues. It regulates blood flow primarily by adjusting the capacity of blood vessels and the volume of blood they contain.
2. What is afterload?
Afterload refers to the resistance the heart must overcome to eject blood during contraction. Higher afterloads reduce the velocity of muscle shortening, making it harder for the heart to pump blood.
3. What are baroreceptors?
Baroreceptors are pressure-sensitive nerve endings located in the walls of the atria, vena cava, aortic arch, and carotid sinus. They detect changes in blood pressure and help regulate heart rate and vascular tone.
4. What is cardiac output?
Cardiac output is the volume of blood pumped by the heart per minute, an essential measure of cardiovascular performance.
5. What is cardiac tamponade?
Cardiac tamponade is a life-threatening condition where the heart is compressed due to the accumulation of blood, fluid, or gas in the pericardial sac, restricting its ability to pump effectively.
6. What are chemoreceptors?
Chemoreceptors are sensory nerve cells that detect changes in the chemical composition of their surroundings. In the carotid arteries, they are sensitive to carbon dioxide levels (PCO2) in the blood and signal the brain’s respiratory center to adjust ventilation accordingly.
7. What is congestive heart failure (CHF)?
Congestive heart failure is a condition in which the heart’s ability to pump blood is impaired, often due to myocardial infarction (MI), ischemic heart disease, or cardiomyopathy, leading to inadequate cardiac output.
8. What is contractility?
Contractility refers to the ability of muscle tissue, particularly the heart muscle, to contract or shorten in response to a stimulus, typically electrical.
9. What is end-diastolic volume (EDV)?
End-diastolic volume is the volume of blood in the ventricles just before they contract.
10. What is end-systolic volume (ESV)?
End-systolic volume is the amount of blood left in the ventricles at the end of systole (contraction).
11. What is negative inotropism?
Negative inotropism refers to a decrease in the contractile strength of the heart, reducing its ability to pump blood effectively.
12. What is the pericardium?
The pericardium is the fibrous, double-layered sac that surrounds the heart and the roots of the great vessels, providing protection and reducing friction during heartbeats.
13. What is positive inotropism?
Positive inotropism refers to an increase in the contractile strength of the heart muscle, improving its pumping efficiency.
14. What is preload?
Preload is the initial stretching of the ventricular walls due to the volume of blood filling the heart at the beginning of ventricular contraction.
15. What is stenosis?
Stenosis refers to the narrowing of a valve or blood vessel, which can restrict blood flow and cause various cardiovascular issues.
16. What is stroke volume?
Stroke volume is the amount of blood ejected from the left ventricle during each contraction.
17. What is vasoconstriction?
Vasoconstriction is the narrowing of blood vessels, particularly arterioles, which increases blood pressure and decreases blood flow.
18. What is vasodilation?
Vasodilation is the widening of blood vessels, typically arterioles, often caused by relaxation of the smooth muscle in the vessel walls in response to nerve impulses or certain drugs.
19. What are the two major subdivisions of the vascular system?
The vascular system is divided into two main subdivisions: the systemic vasculature, which supplies oxygenated blood to the body, and the pulmonary vasculature, which circulates blood between the heart and lungs.
20. What are the three major components of the systemic vasculature?
The three major components of the systemic vasculature are the arterial system, which carries oxygen-rich blood to tissues; the capillary system, where nutrient and gas exchange occurs; and the venous system, which returns deoxygenated blood to the heart.
21. What are the four mechanisms that aid in venous return to the heart?
(1) Sympathetic venous tone, (2) Skeletal muscle pumping, (3) Cardiac suction, and (4) Thoracic pressure differences caused by respiratory efforts.
22. What is an anatomic shunt?
An anatomic shunt occurs when venous blood mixes with arterial blood, reducing the overall oxygen content of the blood.
23. The atrioventricular valves close during what?
The atrioventricular valves close during systole (ventricular contraction) to prevent backflow of blood into the atria. This closure ensures the critical period of isovolumic contraction, during which pressure in the chambers rapidly increases just before blood is ejected.
24. What is the capillary system?
The capillary system, also known as microcirculation, is responsible for the constant exchange of nutrients and waste products between blood and the cells and tissues of the body.
25. What does CHF stand for?
CHF stands for Congestive Heart Failure.
26. What are some common valve problems?
Common valve problems include regurgitation and stenosis.
27. What is conductivity?
Conductivity refers to the ability of myocardial tissue to transmit or spread electrical impulses throughout the heart.
28. What is contractility?
Contractility is the ability of the myocardium to contract in response to an electrical impulse, which is essential for pumping blood.
29. What is the coronary sinus?
The coronary sinus is a large vein that passes left to right across the posterior surface of the heart. It empties into the right atrium between the opening of the inferior vena cava and the tricuspid valve.
30. What is the dicrotic notch?
The dicrotic notch is a small downward deflection in the arterial pressure waveform, caused by the elastic recoil of the arteries after the aortic valve closes.
31. During cardiac contractions, what happens to blood?
During cardiac contractions, blood is ejected from the heart to the lungs through the right-side valves and to the body through the left-side valves.
32. What is the Frank-Starling Law?
The Frank-Starling Law states that the more a cardiac muscle fiber is stretched, the greater the force of contraction it generates when it contracts.
33. The heart is enclosed in a double-walled sac called what?
The heart is enclosed in a double-walled sac called the pericardium.
34. What does HR stand for?
HR stands for Heart Rate.
35. Myocardial tissue possesses what four key properties?
Myocardial tissue possesses four key properties: excitability, inherent rhythmicity, conductivity, and contractility.
36. What is regurgitation?
Regurgitation is the backflow of blood through a valve that is incompetent or damaged.
37. What is stenosis?
Stenosis is the abnormal narrowing or constriction of a valve outlet, leading to increased pressure in the proximal chamber or vessels.
38. What are the thesbesian veins?
The thesbesian veins are small veins that drain directly into all chambers of the heart. Any blood entering the left atrium or ventricle through these veins mixes with oxygenated blood from the lungs.
39. What is the valve between the right atrium and ventricle?
The valve between the right atrium and ventricle is the tricuspid valve.
40. The valves of the heart are flaps of fibrous tissue firmly anchored to what?
The valves of the heart are anchored to the annulus fibrosus cordis, a ring of fibrous tissue located between the atria and ventricles. These are called atrioventricular valves.
41. What is vasoconstriction?
Vasoconstriction is the constriction of smooth muscles in peripheral blood vessels, which causes an increase in blood pressure, even though blood volume remains the same.
42. What is vasodilation?
Vasodilation is the relaxation of smooth muscles in arterioles, leading to a decrease in blood pressure, even though blood volume does not change.
43. What is the venous system?
The venous system consists of small, expandable venules and veins, along with larger, more elastic veins that return blood to the heart.
44. Adrenergic stimulation and release of norepinephrine causes what?
Adrenergic stimulation and the release of norepinephrine cause smooth muscle contraction and an increase in flow resistance.
45. Blood flow through large veins is affected by what?
Blood flow through large veins is affected by changes in abdominal and intrathoracic pressures.
46. What are the functions of blood?
Blood functions to transport electrolytes, proteins, water, and hormones. It contains platelets and clotting factors for hemostasis and transports respiratory gases to and from tissues. Blood also provides antibodies and carries nutrients and waste products to cells.
47. What are conductance vessels?
Conductance vessels are large arteries in the arterial system that have high elasticity and low resistance, allowing efficient blood flow.
48. What are erythrocytes?
Erythrocytes, or red blood cells, are produced in red bone marrow and contain hemoglobin, which is essential for oxygen transport.
49. What is hematocrit?
Hematocrit is the percentage of red blood cells (RBCs) in whole blood by volume. It is typically about three times the total hemoglobin level. Normal ranges are 42-54% for males and 38-47% for females.
50. What is hemoglobin?
Hemoglobin is a protein molecule in red blood cells that allows the transport of oxygen throughout the body.
51. What is plasma?
Plasma is the liquid portion of blood, making up approximately 90% of its volume. It is a yellow, straw-colored fluid that helps transport various substances.
52. What are the major cardiovascular effects of chemoreceptor stimulation?
The major cardiovascular effects of chemoreceptor stimulation include vasoconstriction and an increased heart rate.
53. Smooth muscle relaxation and dilation are the result of what?
Smooth muscle relaxation and dilation result from the stimulation of either cholinergic or specialized beta-adrenergic receptors.
54. Stroke volume is affected by what three factors?
Stroke volume is affected by three factors: preload, afterload, and contractility.
55. What is the thoracic pump?
The thoracic pump is a mechanism that aids venous return by using pressure changes in the thoracic cavity during breathing.
56. To avoid organ/tissue damage and to maintain adequate perfusion pressures, the cardiovascular system balances what?
The cardiovascular system balances relative blood volume and vascular resistance to maintain adequate perfusion pressures and prevent organ or tissue damage.
57. What is the aortic valve?
The aortic valve is a semilunar valve located between the left ventricle and the aorta. It prevents blood from flowing back into the heart from the aorta.
58. How is mean arterial pressure regulated?
Mean arterial pressure is regulated by changes in cardiac output and systemic vascular resistance (SVR).
59. What is the mitral valve?
The mitral valve is a valve that guards the opening between the left atrium and the left ventricle, preventing backflow of blood into the atrium. It is also known as the bicuspid valve.
60. What is myocardial tissue?
Myocardial tissue has four key properties: excitability, inherent rhythmicity, conductivity, and contractility, all essential for heart function.
61. What is the pulmonic valve?
The pulmonic valve separates the right ventricular outflow tract from the pulmonary artery. Under normal conditions, it prevents the regurgitation of deoxygenated blood from the pulmonary artery back into the right ventricle. It is a semilunar valve with three cusps, located anterior, superior, and slightly to the left of the aortic valve.
62. What is the tricuspid valve?
The tricuspid valve, located between the right atrium and right ventricle, has three cusps. It allows blood to flow from the atrium to the ventricle and closes to prevent backflow when the ventricle contracts.
63. The underlying goal of the body’s cardiovascular control mechanisms is to what?
To ensure that all tissues receive appropriate perfusion based on their metabolic needs.
64. What are the heart valves?
The heart valves include the pulmonic valve, aortic valve, mitral valve, and tricuspid valve.
65. What conducts impulses rapidly to ensure synchronous contraction of the ventricles?
Specialized myocardial tissues conduct impulses rapidly to synchronize the contraction of the ventricles.
66. What factors determine cardiac stroke volume?
Stroke volume is determined by preload, afterload, contractility, and heart rate.
67. What happens when chemoreceptors are stimulated?
When chemoreceptors are stimulated, they cause vasoconstriction and an increased heart rate.
68. Which heart chamber has the bulk of muscle mass?
The ventricles, which do most of the pumping to circulate blood, have the bulk of the heart’s muscle mass.
69. Which part of the nervous system is responsible for the central control of blood flow?
The sympathetic division of the autonomic nervous system is responsible for the central control of blood flow.
70. What are the steps of blood flow through the heart?
Blood flows from the right atrium through the tricuspid valve to the right ventricle, then through the pulmonary valve to the pulmonary arteries and lungs. From the lungs, it returns via the pulmonary veins to the left atrium, through the mitral (bicuspid) valve to the left ventricle, and finally through the aortic valve to the aorta and the rest of the body.
71. Where is the aortic valve located?
The aortic valve is located between the left ventricle and the aorta.
72. Where is the bicuspid/mitral valve located?
The bicuspid, or mitral, valve is located between the left atrium and left ventricle.
73. What are chordae tendineae?
Chordae tendineae are strong fibrous strings that attach the cusps of the atrioventricular (AV) valves to the heart wall.
74. What is the description of the average person’s heart?
The average heart is a cone-shaped muscle about the size of a fist.
75. What physiological processes can result from mitral stenosis?
Mitral stenosis causes the left atrium to work harder than the left ventricle, leading to blood backing up, inefficient energy use, and the development of heart murmurs.
76. What is a description of the two atria?
The right atrium receives deoxygenated blood from body tissues, while the left atrium receives oxygenated blood from the lungs.
77. What is a description of the two ventricles?
The right ventricle pumps blood to the lungs, and the left ventricle pumps blood to the body tissues.
78. What is the endocardium?
The endocardium is the inner layer of the heart, composed of epithelium and connective tissue.
79. What is the epicardium?
The epicardium is the outermost covering of the heart.
80. What are the four chambers of the heart?
The four chambers of the heart are the left atrium, left ventricle, right atrium, and right ventricle.
81. What are the four valves found in the heart?
The four valves in the heart are the bicuspid/mitral (AV), tricuspid (AV), aortic (semilunar), and pulmonary (semilunar) valves.
82. What are the functions of all valves in the heart?
The valves ensure that blood flows in one direction, making the heart more efficient and reducing energy usage.
83. What is the myocardium?
The myocardium is the middle layer of the heart, composed of cardiac muscle tissue responsible for contracting and pumping blood.
84. Where is the pulmonary valve located?
The pulmonary valve is located between the right ventricle and the pulmonary trunk.
85. What is the purpose of the semilunar valves?
The semilunar valves ensure one-way blood flow from the ventricles to the large arteries they connect to, such as the aorta and pulmonary artery.
86. What is the purpose of the AV valves?
The AV (atrioventricular) valves ensure that blood flows in one direction from the atria to the ventricles.
87. What are the risk factors for cardiovascular disease?
Risk factors for cardiovascular disease include genetics, hypertension (HTN), elevated cholesterol, diabetes, obesity, smoking, inactivity, and gender (more prevalent in men).
88. What is stenosis?
Stenosis refers to the narrowing of an aperture, often causing partial obstruction of blood flow.
89. What are the three layers of the pericardium?
The three layers of the pericardium are the fibrous, parietal, and visceral layers.
90. What are the three walls of the heart?
The three walls of the heart are the epicardium (outer layer), myocardium (middle layer), and endocardium (inner layer).
91. Where is the tricuspid valve located?
The tricuspid valve is located between the right atrium and the right ventricle.
92. What are the two atrioventricular valves?
The two atrioventricular valves are the bicuspid (mitral) valve and the tricuspid valve.
93. What are the two semilunar valves?
The two semilunar valves are the aortic valve and the pulmonary valve.
94. What is the ultimate function of the cardiovascular system?
The ultimate function of the cardiovascular system is to ensure that all tissues receive adequate perfusion for nutrient and oxygen delivery.
95. What borders the heart in the mediastinum?
The heart is bordered by the lungs, vertebrae, and sternum in the mediastinum.
96. What is the purpose of the fluid in the pericardial cavity?
The fluid in the pericardial cavity lubricates the heart and reduces energy demands by minimizing friction during heartbeats.
97. What separates the two atria?
The two atria are separated by the interatrial septum.
98. What separates the two ventricles?
The two ventricles are separated by the interventricular septum.
99. Where is the apex of the heart?
The apex of the heart is located at the 5th intercostal space.
100. Where is the base of the heart?
The base of the heart is located at the level of the 2nd rib.
Final Thoughts
The cardiovascular system is vital for maintaining the health and functionality of the human body. From the heart’s powerful pumping action to the intricate network of vessels delivering oxygen and nutrients to every cell, each component works together seamlessly to sustain life.
Gaining a deeper understanding of how this system operates allows you to fully appreciate its complexity and significance.
A healthy cardiovascular system is crucial for overall well-being, and mastering its functions is essential for students of biology or anyone aspiring to enter the healthcare field.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Felner JM. An Overview of the Cardiovascular System. In: Walker HK, Hall WD, Hurst JW, editors. Clinical Methods: The History, Physical, and Laboratory Examinations. 3rd edition. Boston: Butterworths; 1990.

