Functional residual capacity (FRC) is one of the most important yet often overlooked measurements in respiratory physiology. It represents the volume of air remaining in the lungs at the end of a normal, passive exhalation.
Although this moment in the breathing cycle may seem insignificant, FRC plays a critical role in maintaining adequate gas exchange, stabilizing alveoli, and supporting efficient breathing.
For respiratory therapists, understanding FRC is essential for interpreting pulmonary function tests, managing mechanical ventilation, and recognizing pathophysiologic changes in patients with acute and chronic lung disease.
What Is Functional Residual Capacity?
Functional residual capacity (FRC) is the amount of air left in the lungs after a person completes a normal, relaxed exhalation. It is not a maximal effort measurement; rather, it reflects the resting balance between the inward elastic recoil of the lungs and the outward recoil of the chest wall.
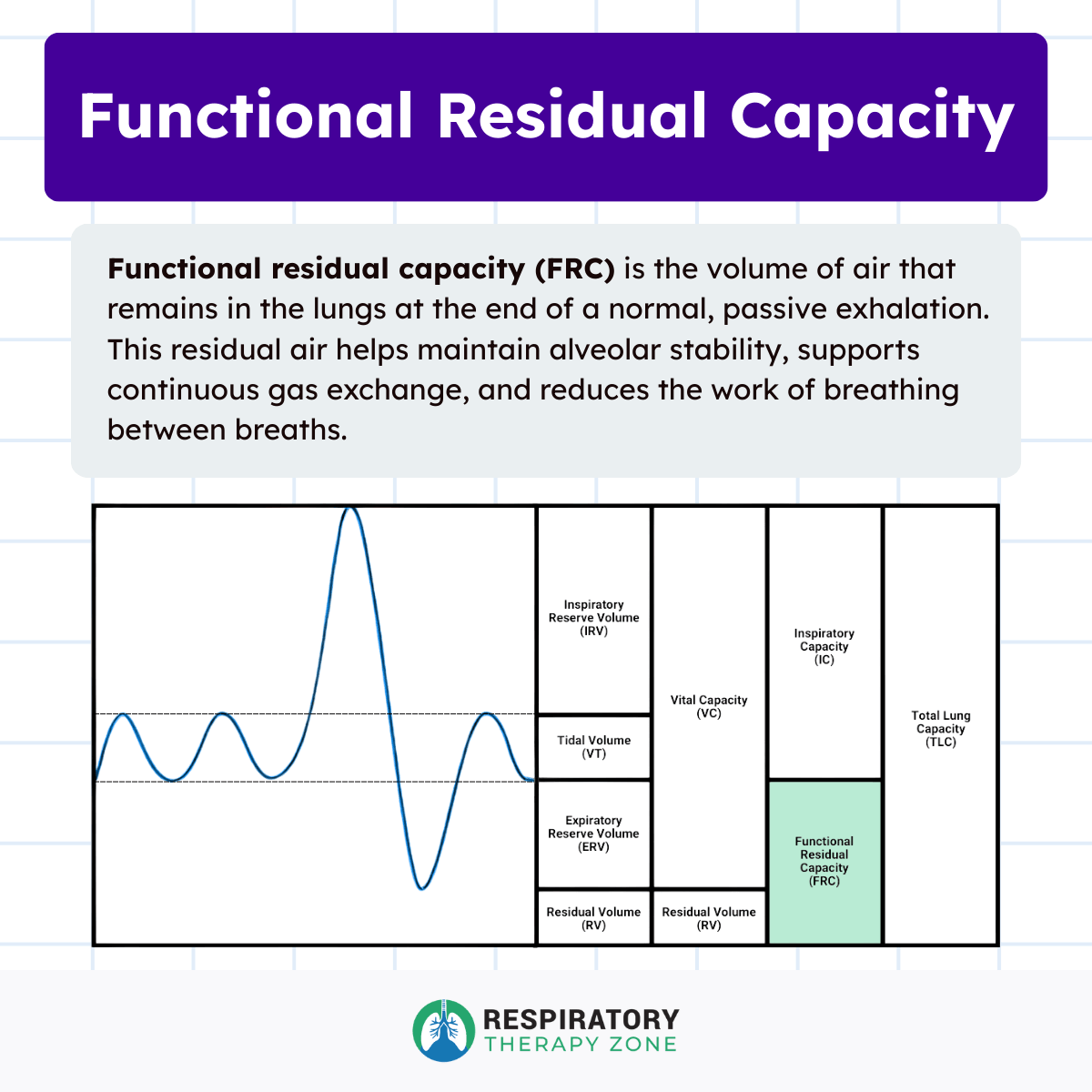
FRC is calculated as the sum of two lung volumes:
- Expiratory Reserve Volume (ERV): The additional air that can be forcibly exhaled after a normal exhalation
- Residual Volume (RV): The air that remains in the lungs even after a maximal exhalation
Mathematically, this relationship is expressed as:
FRC = ERV + RV
Because residual volume cannot be measured directly by standard spirometry, FRC also cannot be measured using spirometry alone. Instead, specialized techniques are required, which highlights its clinical importance and complexity.
Why FRC Matters in Normal Breathing
FRC serves as the body’s oxygen reserve between breaths. Even when airflow temporarily stops at the end of exhalation, gas exchange continues at the alveolar-capillary membrane because oxygen remains available in the lungs.
Several key physiologic functions depend on an adequate FRC:
- Prevention of alveolar collapse: By keeping alveoli partially inflated, FRC helps maintain lung stability
- Continuous gas exchange: Oxygen and carbon dioxide exchange continues between breaths
- Reduced work of breathing: Stable alveoli require less energy to reopen during the next inspiration
Note: When FRC is reduced, alveoli may collapse more easily, leading to atelectasis and impaired oxygenation. When FRC is excessively increased, ventilation becomes inefficient due to air trapping.
Clinical Significance of Functional Residual Capacity
Obstructive Lung Diseases
In conditions such as chronic obstructive pulmonary disease (COPD) and asthma, FRC is often increased. Air trapping occurs when patients cannot fully exhale due to airway obstruction, causing residual volume to rise. As a result, the lungs remain hyperinflated at the end of expiration.
An increased FRC in obstructive disease can lead to:
- Flattened diaphragms
- Increased work of breathing
- Reduced inspiratory capacity
- Dyspnea, especially during exertion
Note: Monitoring changes in FRC can help respiratory therapists assess disease severity and response to treatment.
Restrictive Lung Diseases
In restrictive conditions such as pulmonary fibrosis, acute respiratory distress syndrome (ARDS), or severe obesity, FRC is typically reduced. Decreased lung compliance or restricted chest wall movement limits the amount of air remaining in the lungs after exhalation.
A low FRC is associated with:
- Increased risk of alveolar collapse
- Reduced oxygen reserves
- Impaired gas exchange
- Rapid desaturation during apnea or illness
Note: These patients often require careful ventilatory support and oxygen therapy.
Anesthesia and Surgery
General anesthesia significantly reduces FRC, particularly when patients are positioned supine. Muscle relaxation, loss of diaphragmatic tone, and reduced chest wall movement all contribute to this decrease.
For respiratory therapists working in perioperative or critical care settings, reduced FRC increases the risk of:
- Atelectasis
- Hypoxemia
- Postoperative pulmonary complications
Note: This is one reason why interventions such as positive end-expiratory pressure (PEEP), recruitment maneuvers, and early mobilization are so important.
Critical Care and Mechanical Ventilation
In mechanically ventilated patients, FRC is a key determinant of oxygenation and lung mechanics. Low FRC indicates poor lung recruitment and a higher likelihood of collapsed alveoli.
Respiratory therapists use these strategies to help restore or maintain FRC and improve gas exchange:
- Adjusting PEEP levels
- Optimizing patient positioning
- Monitoring oxygenation trends
Note: Understanding how ventilator settings influence FRC is essential for lung-protective ventilation.
How Functional Residual Capacity Is Measured
Because FRC includes residual volume, it cannot be measured with basic spirometry. Instead, specialized techniques are used.
Body Plethysmography
Body plethysmography is considered the most accurate method for measuring FRC. The patient sits inside an airtight chamber and breathes against a closed shutter. Pressure changes inside the box are used to calculate lung volume.
Advantages:
- Highly accurate
- Measures total gas in the lungs, including trapped air
Limitations:
- Requires specialized equipment
- Not always available in all clinical settings
Nitrogen Washout
In the nitrogen washout technique, the patient breathes 100% oxygen while exhaled nitrogen levels are measured. The amount of nitrogen washed out is used to estimate FRC.
Advantages:
- Less complex than plethysmography
Limitations:
- Underestimates FRC in patients with severe airway obstruction
- Uneven gas mixing affects accuracy
Helium Dilution
This method uses a known concentration of helium, which mixes with the air in the lungs. The dilution of helium allows clinicians to estimate FRC.
Advantages:
- Useful in patients with normal ventilation distribution
Limitations:
- Inaccurate when air trapping is present
- Does not measure non-communicating lung volumes
Imaging-Based Estimates
Chest imaging, including CT scans, can provide estimates of lung volumes, including FRC. However, these are indirect measurements and involve radiation exposure.
Factors That Affect Functional Residual Capacity
Several physiologic and external factors influence FRC:
- Body position: FRC decreases in the supine position compared to standing
- Obesity: Increased abdominal pressure reduces FRC
- Age: FRC tends to increase with age due to changes in lung elasticity
- Pregnancy: Elevated diaphragm reduces FRC
- Disease states: Obstructive diseases increase FRC, restrictive diseases decrease it
Note: Understanding these influences helps respiratory therapists interpret test results accurately.
Why FRC Is Relevant to Respiratory Therapists
Functional residual capacity is not just a theoretical concept; it directly affects patient care. Respiratory therapists rely on FRC knowledge to:
- Interpret pulmonary function tests
- Optimize ventilator settings
- Prevent atelectasis
- Improve oxygenation strategies
- Recognize early signs of respiratory deterioration
Note: Whether managing a ventilated ICU patient, assisting with diagnostic testing, or educating patients about lung health, FRC plays a foundational role in clinical decision-making.
Access our quiz with sample TMC practice questions and detailed explanations to help you master pulmonary function testing (PFT).
Functional Residual Capacity Practice Questions
1. What is functional residual capacity (FRC)?
The volume of air remaining in the lungs at the end of a normal, passive exhalation.
2. At functional residual capacity, what is the relationship between lung and chest wall forces?
The elastic recoil of the lungs and the outward recoil of the chest wall are in equilibrium, requiring no active muscle effort.
3. Which respiratory muscles are active at FRC?
No respiratory muscles are actively contracting at FRC.
4. In what units is functional residual capacity reported?
Liters or milliliters
5. To which gas condition is FRC corrected?
BTPS (Body Temperature and Pressure, Saturated).
6. Which type of lung disease is associated with an increased FRC?
Obstructive lung disease
7. How does aging typically affect functional residual capacity?
FRC increases with age.
8. What is residual volume (RV)?
The volume of air that remains in the lungs after a maximal exhalation.
9. How is residual volume related to functional residual capacity?
Residual volume equals FRC minus expiratory reserve volume (ERV).
10. What does the RV/TLC ratio represent?
The fraction of total lung capacity that cannot be exhaled, expressed as a percentage.
11. In what units is residual volume reported?
Liters or milliliters
12. To which gas condition is residual volume corrected?
BTPS
13. Which lung diseases commonly increase the RV/TLC ratio?
Obstructive diseases such as emphysema and chronic bronchitis.
14. What are the four methods used to measure functional residual capacity?
Nitrogen washout, helium dilution, body plethysmography, and chest imaging (CT).
15. Which method is the most commonly used to measure FRC clinically?
Nitrogen washout
16. What is the principle behind the nitrogen washout method?
Nitrogen is washed out of the lungs by breathing 100% oxygen, and the exhaled nitrogen is measured.
17. During a nitrogen washout test, what gas does the patient breathe?
100% oxygen
18. How long does the nitrogen washout test typically last?
Up to 7 minutes
19. What is another common name for the nitrogen washout test?
The 7-minute washout test
20. What is the approximate nitrogen concentration in the lungs at the start of the washout test?
Approximately 75–80%
21. What must the alveolar nitrogen concentration fall below to end the washout test?
Less than 1.5% for three consecutive breaths.
22. How should the nitrogen concentration change during a successful washout test?
It should decrease continuously over time.
23. Why must washout time be reported during FRC testing?
Failure to wash out nitrogen within the expected time may indicate airflow obstruction.
24. Why is it important for the patient to maintain a tight seal around the mouthpiece?
To prevent air leaks that would invalidate the test results.
25. Why must oxygen be introduced at the end of a normal exhalation during nitrogen washout?
To ensure measurement begins precisely at functional residual capacity.
26. How are nitrogen washout results typically displayed graphically?
On an X–Y graph
27. On a nitrogen washout graph, what does the X-axis represent?
Volume
28. On a nitrogen washout graph, what does the Y-axis represent?
Percentage of nitrogen
29. How does body position affect functional residual capacity?
FRC decreases when a person moves from upright to supine.
30. Why are FRC and RV increased in emphysema?
Loss of lung elastic recoil allows chest wall forces to dominate, increasing lung volume (hyperinflation) and trapping air due to small airway collapse.
31. What term describes increased functional residual capacity?
Hyperinflation
32. What term describes increased residual volume due to incomplete exhalation?
Air trapping
33. Why is vital capacity often reduced in emphysema?
Small airway obstruction causes early airway collapse during exhalation, limiting maximal exhaled volume.
34. Why does nitrogen washout underestimate lung volumes in severe obstructive disease?
Poorly ventilated regions may not effectively wash out nitrogen within the test duration.
35. Which FRC measurement method is considered the most accurate in obstructive lung disease?
Body plethysmography
36. What is the basic principle of the helium dilution method for measuring FRC?
It measures functional residual capacity by allowing helium to equilibrate between the spirometer and the lungs in a closed system.
37. At what point in the breathing cycle must the helium dilution test begin?
At the end of a normal exhalation, which corresponds to functional residual capacity.
38. What gas concentration is typically used in the helium dilution spirometer?
A helium concentration of approximately 5–10%.
39. Why is carbon dioxide removed during the helium dilution test?
CO₂ is absorbed by soda lime to prevent hypercapnia and allow normal breathing during the test.
40. Why is oxygen added during the helium dilution test?
Oxygen is added to maintain a constant end-expiratory level and prevent hypoxemia, typically at about 0.25 L/min.
41. When is equilibration considered complete during helium dilution?
When the helium concentration remains constant for at least 2 minutes.
42. How is FRC calculated in the helium dilution method?
Using the initial and final helium concentrations, the volume of gas in the system, oxygen added, and system dead space.
43. What technical factors are critical for accurate helium dilution testing?
A leak-free spirometer and proper calibration of the helium analyzer.
44. Why may helium dilution underestimate FRC in patients with obstructive lung disease?
Because helium does not reach poorly ventilated or trapped gas regions.
45. What adverse events can occur if CO₂ is not removed or oxygen is not added during helium dilution?
Hypercapnia and hypoxemia
46. What level of repeatability is required for acceptable FRC measurements in adults?
Results should agree within ±500 mL.
47. What factors can invalidate a helium dilution test?
Leaks, poor mouth seal, failure to start at FRC, perforated eardrums, or tracheostomies.
48. How does the nitrogen washout method differ from helium dilution?
It uses an open-circuit system in which nitrogen is washed out while the patient breathes 100% oxygen.
49. At what lung volume must the nitrogen washout test begin?
At functional residual capacity.
50. What measurements are collected during a nitrogen washout test?
Expired nitrogen concentration and expired volume.
51. When is the nitrogen washout test terminated?
After 7 minutes or when alveolar nitrogen falls below 1.0%.
52. Why may nitrogen washout testing take longer in patients with airflow obstruction?
Air trapping delays nitrogen elimination from poorly ventilated lung regions.
53. How is FRC calculated during the nitrogen washout method?
From the total volume of nitrogen washed out divided by the initial alveolar nitrogen fraction.
54. What initial alveolar nitrogen concentration is assumed if the patient has been breathing room air?
Approximately 80%
55. What are common limitations of the nitrogen washout method?
Leaks, poor patient cooperation, depressed ventilatory drive from 100% oxygen, and difficulty maintaining a mouth seal.
56. What indicates a leak during nitrogen washout testing?
An unexpected rise in nitrogen concentration during the test.
57. How long should a patient wait before repeating a nitrogen washout test?
At least 15 minutes.
58. What is the primary advantage of body plethysmography over gas dilution methods?
It measures total thoracic gas volume, including trapped gas.
59. What lung volume is directly measured by body plethysmography?
Thoracic gas volume (TGV).
60. What physical law is used to calculate lung volumes in body plethysmography?
Boyle’s law (P₁V₁ = P₂V₂)
61. How is alveolar pressure measured during body plethysmography?
By measuring mouth pressure while the airway is occluded with a shutter.
62. Why must the patient pant during body plethysmography?
Panting causes measurable pressure changes that allow calculation of thoracic gas volume.
63. What panting frequency is recommended for accurate body box measurements?
Approximately 1 cycle per second.
64. Why must the patient support their cheeks during panting?
To prevent cheek “bowing,” which can distort pressure measurements.
65. What patient-related factor may limit the use of body plethysmography?
Claustrophobia
66. How many acceptable panting maneuvers are required to calculate TGV?
A minimum of three to five reproducible efforts.
67. Why may plethysmographic FRC be higher than gas dilution FRC in emphysema?
Because plethysmography includes trapped gas in bullae or cysts that dilution methods cannot measure.
68. What lung volume does thoracic gas volume (TGV) represent?
It represents the total volume of compressible gas within the thorax at the time of measurement.
69. Why is body plethysmography considered the reference method for measuring lung volumes?
Because it measures all intrathoracic gas, including poorly ventilated or trapped air.
70. What patient instruction is most important before initiating FRC testing?
The patient must breathe normally and avoid deep breaths before the shutter closes.
71. Why must FRC measurements always be corrected to BTPS?
Because lung volumes are affected by body temperature, ambient pressure, and water vapor.
72. What effect does obesity have on functional residual capacity?
Obesity typically reduces FRC due to decreased chest wall compliance.
73. How does anesthesia affect FRC?
Anesthesia decreases FRC by reducing muscle tone and altering chest wall mechanics.
74. Why is FRC clinically important in oxygenation?
It represents the lung volume available for gas exchange between breaths.
75. What happens to FRC when a patient is placed supine?
FRC decreases due to upward displacement of the diaphragm.
76. Why does pregnancy reduce functional residual capacity?
Enlargement of the uterus elevates the diaphragm and reduces lung volume.
77. How does COPD affect functional residual capacity?
COPD increases FRC due to air trapping and loss of elastic recoil.
78. What is hyperinflation in terms of lung volumes?
An abnormal increase in FRC caused by increased end-expiratory lung volume.
79. What is air trapping in terms of lung volumes?
An abnormal increase in residual volume due to premature airway closure.
80. Why is FRC considered the most stable lung volume?
Because it occurs at passive equilibrium between lung and chest wall recoil.
81. What happens to airway resistance at higher lung volumes near FRC?
Airway resistance decreases as lung volume increases.
82. Why is FRC the preferred reference volume for many pulmonary measurements?
It is highly reproducible and independent of patient effort.
83. What patient condition may cause falsely low FRC measurements during gas dilution testing?
Severe airway obstruction with significant trapped gas.
84. How does smoking affect functional residual capacity?
Chronic smoking may increase FRC due to airway inflammation and air trapping.
85. What role does elastic recoil play in determining FRC?
Elastic recoil of the lungs balances chest wall expansion at FRC.
86. How does loss of lung recoil affect FRC?
Reduced lung recoil increases FRC by allowing greater chest wall expansion.
87. What lung volume relationship defines FRC?
FRC equals residual volume plus expiratory reserve volume.
88. Why is accurate mouth sealing critical during FRC testing?
Leaks cause gas loss and lead to underestimation of lung volumes.
89. How does pulmonary fibrosis affect FRC?
Pulmonary fibrosis reduces FRC due to increased lung stiffness.
90. Why should patients avoid talking during FRC measurements?
Talking alters breathing patterns and disrupts volume equilibrium.
91. What clinical scenario would favor nitrogen washout over helium dilution?
Patients with suspected uneven ventilation distribution.
92. Why may nitrogen washout depress ventilatory drive?
Breathing 100% oxygen can reduce hypoxic respiratory drive.
93. What does a prolonged nitrogen washout time suggest?
The presence of airflow obstruction or air trapping.
94. Why is repeatability important in lung volume testing?
It confirms reliability and accuracy of the measurement.
95. What does an increased RV/TLC ratio indicate?
A greater proportion of trapped air relative to total lung capacity.
96. How does kyphoscoliosis affect functional residual capacity?
It reduces FRC by restricting chest wall expansion.
97. Why is imaging not routinely used to measure FRC?
Imaging is less accurate and involves radiation exposure.
98. What patient behavior can falsely elevate FRC measurements?
Panting too forcefully during body plethysmography.
99. Why must calibration be performed before lung volume testing?
To ensure accurate pressure, volume, and gas concentration measurements.
100. How does aging affect functional residual capacity?
FRC increases with age due to decreased lung elastic recoil.
Final Thoughts
Functional residual capacity (FRC) is a fundamental component of respiratory physiology that influences oxygenation, lung stability, and the work of breathing. For respiratory therapists, understanding FRC provides critical insight into lung mechanics across a wide range of clinical scenarios, from pulmonary function testing to mechanical ventilation and critical care management.
Changes in FRC often signal underlying pathology and guide therapeutic interventions. By mastering the principles of FRC, respiratory professionals can make more informed decisions, improve patient outcomes, and deliver safer, more effective respiratory care.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Hopkins E, Sharma S. Physiology, Functional Residual Capacity. [Updated 2022 Dec 26]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025.


