Pulmonary function testing (PFT) is an essential topic for anyone preparing for the respiratory therapy board exam. These tests evaluate how well the lungs move air, exchange gases, and respond to disease. Because respiratory therapists frequently rely on these measurements in clinical practice, the board exam places significant emphasis on your ability to understand and interpret pulmonary function data.
PFTs are commonly used to diagnose, monitor, and manage respiratory conditions such as asthma, COPD, pulmonary fibrosis, and other restrictive lung diseases. They provide objective information about lung volumes, airflow, airway resistance, and gas exchange. A strong understanding of these measurements allows clinicians to identify disease patterns, evaluate treatment effectiveness, and make informed clinical decisions.
In addition to supporting diagnosis, pulmonary function testing helps determine the severity of lung disease, evaluate a patient’s response to bronchodilator therapy, and assess readiness for certain procedures or treatments. Because these tests provide such valuable clinical insight, they are a frequent focus of questions on the respiratory therapy board exam.
In this guide, we will review essential strategies and study tips to help you master the PFT section of the board exam. By understanding how these tests work and how to interpret their results, you can approach exam questions with confidence while moving one step closer to earning your RRT credentials.
Take our free course to learn essential tips, insights, and strategies to pass the TMC Exam on your first (or next) attempt.
Why Pulmonary Function Testing Is Important for the Board Exam
Pulmonary function testing (PFT) is a major topic on the respiratory therapy board exam because it evaluates your ability to interpret lung function data and identify common respiratory disorders. These tests provide objective measurements of airflow, lung volumes, airway resistance, and gas exchange, all of which are essential for diagnosing conditions such as asthma, COPD, and restrictive lung diseases.
On the exam, you may be asked to analyze spirometry results, recognize abnormal patterns, or determine which pulmonary function test should be performed based on a patient scenario.
Understanding concepts such as the FEV1/FVC ratio, lung volumes, and flow-volume loops will help you quickly identify obstructive and restrictive patterns. Mastering these principles will improve both your exam performance and your ability to evaluate patients in clinical practice.
PFT Tips for the Board Exam
- Understand the basics
- Know the normal values
- Use the Lung Box to your advantage
- Understand flow-volume loops
- Understand the FEV1/FVC ratio
Watch this video and keep reading to learn essential tips and strategies for mastering pulmonary function testing on the respiratory therapy board exam.
1. Understand the Basics
Pulmonary function testing (PFT) plays a critical role in assessing lung function and diagnosing a wide range of respiratory disorders. Because these tests provide measurable data about lung mechanics and gas exchange, they are widely used in both clinical practice and board exam scenarios.
The respiratory therapy board exam frequently includes questions that require you to identify which pulmonary function test should be performed for a given patient or how to interpret the results. Therefore, understanding the purpose of each test and what it measures is essential.
Below is an overview of several common pulmonary function tests and their clinical significance.
- Peak Expiratory Flow Rate (PEFR): Measures the maximum speed of exhalation during a forced breath. It is often used to monitor airway obstruction in patients with asthma and can help determine whether airway obstruction improves after bronchodilator therapy.
- Maximum Inspiratory Pressure (MIP): Measures the maximum negative pressure a patient can generate during inspiration. This test evaluates respiratory muscle strength and is commonly used to assess ventilatory muscle function and readiness for ventilator weaning.
- Vital Capacity (VC): Represents the total amount of air a patient can exhale after taking the deepest possible breath. A reduced vital capacity often suggests restrictive lung disease or respiratory muscle weakness.
- Spirometry: One of the most common pulmonary function tests. It measures lung volumes and airflow rates during forced breathing maneuvers. Spirometry provides values such as tidal volume, FEV1, and FVC and is widely used to diagnose and monitor obstructive and restrictive lung disorders.
- Flow-Volume Loop: A graphical representation of airflow plotted against lung volume during a forced inspiratory and expiratory maneuver. This test helps identify patterns associated with obstructive disease, restrictive disease, and certain upper airway obstructions such as tracheal stenosis or vocal cord dysfunction.
- Body Plethysmograph (Body Box): A specialized test that measures lung volumes such as functional residual capacity (FRC), residual volume (RV), and total lung capacity (TLC). It is considered the most accurate method for measuring lung volumes, particularly in patients with obstructive disease.
- Methacholine Challenge Test: Uses methacholine to provoke airway narrowing in susceptible individuals. It is commonly used to diagnose asthma by assessing airway hyperresponsiveness when baseline spirometry results are normal.
- Maximum Voluntary Ventilation (MVV): Measures the maximum volume of air that can be inhaled and exhaled over a short period of time, typically 12 to 15 seconds. It reflects the combined performance of respiratory muscles, airway resistance, and lung compliance.
- Nitrogen Washout Test: Measures functional residual capacity by calculating the amount of nitrogen exhaled while the patient breathes pure oxygen. It helps evaluate lung volumes and detect ventilation abnormalities.
- Helium Dilution Test: Another method used to measure functional residual capacity. The patient breathes a known concentration of helium, and changes in helium concentration are used to calculate lung volumes.
- Diffusing Capacity for Carbon Monoxide (DLCO): Measures how effectively gases move from the alveoli into the bloodstream. A reduced DLCO indicates impaired gas exchange and is commonly seen in conditions such as emphysema, pulmonary fibrosis, and pulmonary vascular disease.
Understanding Which Test to Recommend
On the board exam, you may be asked to determine which pulmonary function test is most appropriate for a given patient scenario. Understanding the clinical purpose of each test will help you make the correct selection.
- Obstructive diseases (COPD, asthma): Focus on tests that evaluate airflow limitation such as spirometry, flow-volume loops, and MVV. PEFR and methacholine challenge testing are particularly useful when evaluating asthma.
- Restrictive diseases (pulmonary fibrosis, sarcoidosis): Prioritize tests that measure lung volumes such as body plethysmography or vital capacity.
- Gas exchange abnormalities: Use DLCO testing to evaluate how effectively gases move across the alveolar membrane.
Note: Understanding the purpose and clinical application of each pulmonary function test will help you answer exam questions more efficiently and interpret patient data more accurately in real-world clinical settings.
Access our quiz with sample TMC practice questions and detailed explanations to help you master pulmonary function testing (PFT).
2. Know the Normal Values
Memorizing normal pulmonary function values is an important step in learning how to interpret test results. On the respiratory therapy board exam, you may be presented with spirometry results or lung volume measurements and asked to determine whether the findings represent a normal pattern, an obstructive disease, or a restrictive disorder.
Knowing the expected reference ranges allows you to quickly recognize abnormal findings and identify the likely disease process.
Here are several important pulmonary function values that every respiratory therapy student should know.
- Forced Expiratory Volume in 1 Second (FEV1): Greater than 80 percent of predicted. This value represents the amount of air a patient can forcefully exhale during the first second of a forced breath. Reduced values are commonly associated with obstructive lung disease.
- FEV1/FVC Ratio: Greater than or equal to 70 percent. This ratio compares the amount of air exhaled in the first second with the total forced vital capacity. A decreased ratio is a classic sign of airflow obstruction.
- Forced Vital Capacity (FVC): Greater than 80 percent of predicted. This measurement represents the total volume of air that can be forcefully exhaled after a full inspiration. Lower values are often associated with restrictive lung disease.
- Slow Vital Capacity (SVC): Greater than 80 percent of predicted. This value measures lung volume without a forced maneuver and is sometimes used when evaluating restrictive disorders.
- Airway Resistance (RAW): 0.6 to 2.4 cmH2O/L/sec. Increased airway resistance indicates narrowed airways and is often seen in obstructive diseases such as asthma or COPD.
- Diffusing Capacity for Carbon Monoxide (DLCO): Approximately 20 to 25 mL/CO/min/mmHg. Reduced DLCO values suggest impaired gas exchange and are often seen in emphysema, pulmonary fibrosis, and pulmonary vascular disease.
- Peak Expiratory Flow Rate (PEFR): Approximately 10 L/sec. Lower values indicate reduced airflow and may suggest airway obstruction.
- Exhaled Carbon Monoxide (ExCO): Less than 7 ppm in nonsmokers. Elevated levels are commonly seen in smokers or patients exposed to environmental pollutants.
When interpreting pulmonary function tests, the first step is to compare the patient’s results with these normal reference values. This comparison helps determine whether lung function is within normal limits or if a pattern of obstruction or restriction is present.
For example, a decreased FEV1/FVC ratio strongly suggests obstructive disease. In contrast, a reduced FVC with a normal or elevated ratio may indicate restrictive lung disease.
Note: Developing the ability to quickly recognize these patterns is a key skill that will help you answer board exam questions accurately and efficiently.
3. Use the Lung Box to Your Advantage
When studying pulmonary function testing, one of the most helpful visual tools is the Lung Box. This simple diagram organizes the different lung volumes and capacities into an easy-to-remember layout. Many respiratory therapy students use this method to quickly recall how lung volumes relate to one another when answering board exam questions.
The Lung Box is especially useful because it visually demonstrates how lung volumes combine to form lung capacities. By understanding these relationships, you can more easily interpret pulmonary function test results and identify abnormal patterns.
A helpful strategy for the board exam is to practice drawing the Lung Box until you can recreate it from memory. Many students quickly sketch this diagram on their scratch paper at the beginning of the exam. This provides a quick reference that can help when answering questions about lung volumes and capacities.
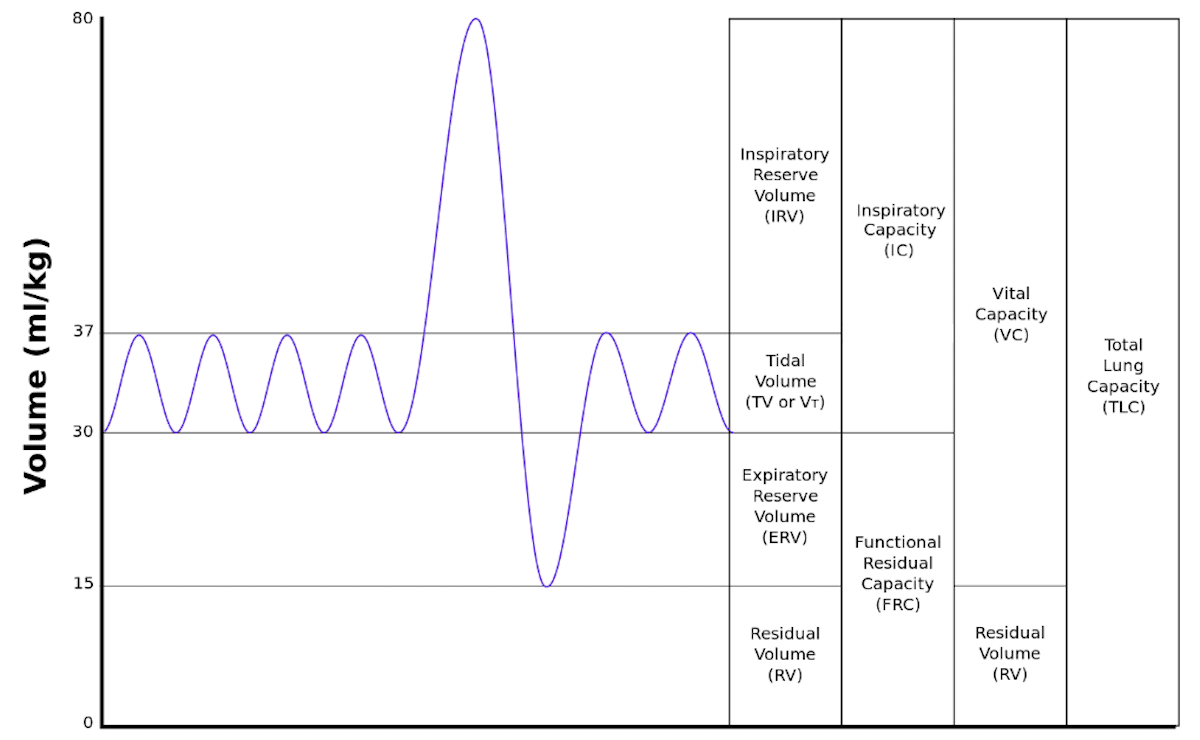
Lung Volumes
- Tidal Volume (VT): The amount of air inhaled and exhaled during normal, quiet breathing. It represents the baseline ventilation that occurs during resting respiration.
- Inspiratory Reserve Volume (IRV): The maximum additional volume of air that can be inhaled after a normal tidal inspiration. This reflects the lungs’ ability to expand beyond normal breathing.
- Expiratory Reserve Volume (ERV): The maximum volume of air that can be exhaled after a normal tidal exhalation. This represents the extra air that can be expelled when a person forcefully exhales.
- Residual Volume (RV): The amount of air that remains in the lungs after a maximal exhalation. This air cannot be voluntarily removed and helps prevent alveolar collapse.
Lung Capacities
- Inspiratory Capacity (IC): The maximum amount of air that can be inhaled after a normal exhalation. It represents the sum of tidal volume and inspiratory reserve volume.
- Functional Residual Capacity (FRC): The volume of air remaining in the lungs after a normal tidal exhalation. It represents the balance between lung recoil and chest wall expansion.
- Vital Capacity (VC): The maximum amount of air that can be exhaled after taking the deepest possible breath. It reflects the largest volume of air that can move in and out of the lungs.
- Total Lung Capacity (TLC): The total amount of air the lungs can hold after a maximal inhalation. It includes all lung volumes combined.
Note: Practice drawing the Lung Box until you can recreate it quickly and accurately. Using this visual reference during the board exam can help you recall lung volume relationships and interpret pulmonary function test questions more efficiently.
4. Understand Flow-Volume Loops
Flow-volume loops are graphical representations that illustrate airflow during inspiration and expiration plotted against lung volume. These loops provide valuable insight into how air moves through the respiratory system and are commonly used to identify patterns associated with different lung diseases.
On the respiratory therapy board exam, you may encounter questions that present a flow-volume loop and ask you to determine whether the patient has normal lung function, an obstructive disease, or a restrictive disease. Being able to recognize these patterns quickly can help you answer these questions with confidence.
Why Flow-Volume Loops Are Important
Flow-volume loops provide a visual representation of airflow and lung volume throughout the breathing cycle. By examining the shape and pattern of the loop, clinicians can detect abnormalities in airflow and lung mechanics.
For example, obstructive lung diseases typically reduce expiratory airflow, while restrictive diseases reduce lung volume. These changes produce distinctive shapes on the flow-volume loop that can help identify the underlying condition.

Restrictive Diseases
- Pattern: Tall and narrow loop
- Shape: The loop appears narrow because lung volumes are reduced
- Key Point: This pattern indicates difficulty expanding the lungs, which is typical of restrictive conditions such as pulmonary fibrosis, interstitial lung disease, or sarcoidosis
Obstructive Diseases
- Pattern: Short and wide loop
- Shape: The expiratory portion of the loop appears scooped or flattened because airflow is reduced
- Key Point: This pattern suggests increased airway resistance, which is commonly seen in conditions such as asthma, chronic bronchitis, and emphysema
Note: Flow-volume loops are one of the fastest ways to identify airflow abnormalities. Learning to recognize these patterns will help you interpret pulmonary function test graphics and answer board exam questions more effectively.
5. Understand the FEV1/FVC Ratio
The FEV1/FVC ratio is one of the most important values used when interpreting pulmonary function tests. It provides a simple and reliable way to determine whether airflow obstruction is present.
Understanding how to interpret this ratio is essential for both clinical practice and the respiratory therapy board exam.
- FEV1 (Forced Expiratory Volume in 1 Second): The amount of air a patient can forcefully exhale during the first second of a forced breath.
- FVC (Forced Vital Capacity): The total volume of air that can be forcefully exhaled after a full inspiration.
The FEV1/FVC ratio represents the percentage of the total forced vital capacity that is exhaled during the first second of the maneuver. Because obstructive diseases limit airflow, patients with these conditions are unable to exhale as quickly, which causes the ratio to decrease.
For the board exam, one of the first steps when interpreting spirometry results is to evaluate the FEV1/FVC ratio.
Note: In healthy individuals, at least 70 percent of the forced vital capacity should be exhaled during the first second. This means the FEV1/FVC ratio should be greater than or equal to 70 percent. When the ratio falls below 70 percent, this strongly suggests an obstructive lung disease.
Understanding the Clinical Significance
When airflow obstruction is present, the airways become narrowed or partially blocked. This makes it more difficult for the patient to exhale air quickly.
As a result, the amount of air expelled during the first second decreases, which lowers the FEV1/FVC ratio.
If the ratio remains normal or elevated while lung volumes are reduced, a restrictive lung disease may be present instead.
For many board exam questions involving pulmonary function tests, the quickest strategy is to check the FEV1/FVC ratio first. This simple step can often reveal whether obstruction is present.
Note: A reduced FEV1/FVC ratio below 70 percent is a key indicator of obstructive lung disease.
Unlock insider strategies and proven exam hacks to master key concepts, avoid common pitfalls, and pass the exam on your first (or next) attempt.
Final Thoughts
Pulmonary function testing is a foundational topic in respiratory therapy and a common subject on the board exam. These tests provide valuable information about lung mechanics, airflow limitation, lung volumes, and gas exchange.
By understanding how pulmonary function tests work and how to interpret their results, you can identify patterns associated with obstructive and restrictive lung diseases. This knowledge not only helps you succeed on the board exam but also prepares you for real-world clinical practice.
When studying this topic, focus on learning the purpose of each test, memorizing the most important normal values, and recognizing key diagnostic patterns such as changes in the FEV1/FVC ratio and flow-volume loop shapes.
Consistent practice with pulmonary function questions will strengthen your interpretation skills and improve your confidence.
If you found these tips helpful, explore our TMC Exam Hacks video course for more in-depth strategies, expert insights, and practical guidance to help you succeed on the respiratory therapy board exam.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Ponce MC, Sankari A, Sharma S. Pulmonary Function Tests. [Updated 2023 Aug 28]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025.




