Pathology is a critical component of the respiratory therapy board exam that tests your understanding of disease processes, including their causes, clinical manifestations, and appropriate treatment strategies.
As a respiratory therapist, having a strong grasp of both pulmonary and systemic pathologies is essential for delivering safe and effective patient care. The board exam evaluates your ability to recognize symptoms, interpret clinical findings, and recommend the most appropriate interventions for a variety of respiratory conditions.
Because respiratory therapists frequently manage patients with complex cardiopulmonary diseases, it is important to understand not only how diseases develop but also how they affect lung function, gas exchange, and overall patient stability.
In this guide, we’ll review essential tips and strategies to help you confidently approach the pathology portion of the board exam, bringing you one step closer to earning your RRT credentials.
Take our free course to learn essential tips, insights, and strategies to pass the TMC Exam on your first (or next) attempt.
Why Pathology Is an Important Topic for the Board Exam
Pathology is a major focus of the respiratory therapy board exam because respiratory therapists frequently manage patients with complex cardiopulmonary diseases. The exam evaluates your ability to recognize disease patterns, interpret clinical findings, and recommend appropriate treatments based on patient presentation.
Many questions are presented as clinical scenarios that require you to identify the underlying condition before selecting the correct intervention. This means you must understand how diseases affect lung mechanics, gas exchange, and overall respiratory function.
By mastering pathology concepts such as obstructive and restrictive diseases, infectious conditions, and airway disorders, you will be better prepared to answer exam questions accurately and make sound clinical decisions in real-world patient care.

Pathology Tips for the Board Exam
- Master disease recognition and management
- Understand obstructive vs. restrictive lung diseases
- Understand how to treat a pneumothorax
- Understand croup vs. epiglottitis
- Understand obstructive vs. central sleep apnea
Watch this video and continue reading to learn essential tips for mastering pathology concepts that frequently appear on the respiratory therapy board exam.
1. Master Disease Recognition and Management
Pathology plays a major role on the respiratory therapy board exam. Many exam questions are presented as clinical scenarios that require you to recognize a disease, interpret patient findings, and select the most appropriate intervention.
Because respiratory therapists care for patients with a wide range of cardiopulmonary disorders, the exam places significant emphasis on your ability to understand how diseases affect the lungs, heart, and overall respiratory function.
This means that success on the exam requires more than memorizing definitions. You must be able to apply your knowledge to clinical situations and make informed decisions based on patient data.
For the board exam, you should be able to:
- Recognize Signs and Symptoms: Identify the key clinical features of common respiratory and cardiovascular diseases.
- Interpret Assessment Data: Analyze findings such as vital signs, breath sounds, chest radiographs, and arterial blood gas results.
- Establish a Probable Diagnosis: Use the available information to determine the most likely disease process.
- Select the Appropriate Treatment: Choose the intervention that will best stabilize the patient and address the underlying condition.
Many board exam questions follow this sequence. You may first be asked to identify a disease based on symptoms. The next question may require you to determine the appropriate treatment or next clinical step.
Because of this structure, developing strong disease recognition skills will significantly improve your ability to answer exam questions correctly.
You should dedicate a significant portion of your study time to reviewing common cardiopulmonary conditions such as COPD, asthma, pneumonia, pulmonary embolism, pneumothorax, and respiratory failure. Understanding how these diseases affect ventilation, oxygenation, and lung mechanics will help you answer both diagnostic and treatment based questions.
A strong foundation in pathology is also essential for your future clinical practice. Respiratory therapists routinely assess patients, interpret diagnostic findings, and collaborate with the healthcare team to develop treatment plans.
Building this knowledge now will help you succeed on the board exam while also preparing you for real world patient care.
Note: Mastering pathology concepts will not only improve your exam performance but will also help you develop the clinical reasoning skills required to become a successful respiratory therapist.
Access our quiz with sample TMC practice questions and detailed explanations to help you master the key concepts of pathology.
2. Understand Obstructive vs. Restrictive Lung Diseases
One of the most frequently tested pathology topics on the respiratory therapy board exam is the difference between obstructive and restrictive lung diseases. Understanding the key characteristics of each category will help you interpret pulmonary function tests, identify disease patterns, and answer exam questions more efficiently.
These two groups of diseases affect lung function in very different ways.
Obstructive diseases primarily affect airflow. Patients have difficulty exhaling because the airways are narrowed or obstructed. Restrictive diseases primarily affect lung expansion. Patients have difficulty fully expanding their lungs due to reduced lung compliance or decreased lung volumes.
Learning to quickly distinguish between these two patterns can help you narrow down potential diagnoses during the exam.
CBABE for Obstructive Lung Diseases
A helpful mnemonic for remembering the most common obstructive lung diseases is CBABE. These conditions are characterized by airflow limitation and air trapping within the lungs.

CBABE stands for:
- C – Cystic Fibrosis
- B – Bronchiectasis
- A – Asthma
- B – Bronchitis (Chronic)
- E – Emphysema
These diseases all share a common characteristic. Airflow is limited due to airway narrowing, mucus obstruction, inflammation, or structural airway damage. As a result, patients have difficulty exhaling air from the lungs.
Note: If a lung disease does not appear in the CBABE mnemonic, it is usually classified as a restrictive lung disease. This shortcut can help you quickly identify the disease category during exam questions.
Restrictive Lung Diseases
Restrictive lung diseases reduce the ability of the lungs to expand. This leads to decreased lung volumes and reduced lung compliance.
In these conditions, the lungs become stiff or restricted, making it difficult for patients to take a full breath.
Common examples include:
- Pulmonary Fibrosis
- Sarcoidosis
- Pleural Diseases
- Neuromuscular Disorders such as Myasthenia Gravis or ALS
- Severe Obesity
Note: These conditions may affect the lung tissue itself, the pleural space, or the respiratory muscles that control breathing.
Key Differences in Lung Volumes
Pulmonary function tests provide important clues that help distinguish obstructive and restrictive diseases.
- Obstructive Diseases: Characterized by air trapping. Lung volumes such as Residual Volume (RV), Functional Residual Capacity (FRC), and Total Lung Capacity (TLC) are often increased and may exceed 120% of the predicted value.
- Restrictive Diseases: Characterized by reduced lung volumes. RV, FRC, and TLC are typically decreased and may fall below 80% of predicted values. Forced Vital Capacity (FVC) is also reduced because the lungs cannot fully expand.
Understanding these differences will help you interpret spirometry results and identify disease patterns on the board exam.
Mastering this concept will also strengthen your clinical decision making skills as a respiratory therapist, since pulmonary function testing is commonly used to diagnose and monitor many lung diseases.
3. Understand How to Treat a Pneumothorax
Understanding the treatment of a pneumothorax is another important topic for the respiratory therapy board exam. Questions on this subject often test your ability to recognize the severity of the condition and select the most appropriate intervention.
A pneumothorax occurs when air enters the pleural space, which causes partial or complete lung collapse. This air disrupts the normal negative pressure within the pleural cavity and prevents the lung from expanding properly during inspiration.
The correct treatment depends on several factors, including the size of the pneumothorax, the patient’s symptoms, and the underlying cause.

Treatment Options for a Pneumothorax
- Small, Mild Pneumothorax: A small pneumothorax may resolve on its own with observation, bed rest, and supplemental oxygen. Oxygen therapy can accelerate the reabsorption of air from the pleural space.
- Needle Aspiration: For moderate cases or when rapid decompression is needed, needle aspiration can be performed to remove air from the pleural space. This procedure is commonly performed at the bedside.
- Chest Tube Placement: Large or symptomatic pneumothoraces usually require the insertion of a chest tube connected to a pleural drainage system. This system continuously removes air from the pleural space, allowing the lung to re-expand.
Note: Severe cases such as a tension pneumothorax represent a medical emergency. In this situation, air continues to accumulate in the pleural space and compresses the lungs and mediastinal structures. Immediate needle decompression followed by chest tube placement is required to prevent cardiovascular collapse.
Understanding the Pleural Drainage System
Questions on the board exam frequently test your knowledge of chest tubes and pleural drainage systems. A standard pleural drainage system typically includes three chambers:
- Suction Chamber: This chamber regulates the amount of negative pressure applied to the pleural space. Gentle bubbling is usually expected and indicates that suction is being applied properly.
- Water Seal Chamber: This chamber acts as a one way valve that prevents air from reentering the pleural cavity. Intermittent bubbling in this chamber may occur when a pneumothorax is present, which indicates that air is leaving the pleural space.
- Collection Chamber: This chamber collects fluid and air that drain from the pleural cavity. The amount of drainage should be monitored and documented regularly.
Note: Continuous bubbling in the water seal chamber may indicate an air leak in the system. In these cases, the tubing connections should be inspected carefully to identify the source of the leak.
Exam Tips for Chest Tube Management
- Recognize Bubbling Patterns: Bubbling in the suction chamber is expected. Intermittent bubbling in the water seal chamber may occur with a pneumothorax, but continuous bubbling suggests an air leak.
- Inspect the Tubing: If drainage suddenly stops or bubbling patterns change, check the tubing for kinks, clots, or loose connections.
- Monitor Drainage Levels: Drainage should be measured and documented regularly. Sudden increases in drainage may indicate bleeding or other complications.
Note: Understanding chest tube management and pleural drainage systems will help you answer related questions on the board exam and prepare you for real clinical situations where these devices are commonly used.
4. Understand Croup vs. Epiglottitis
Croup and epiglottitis are two upper airway conditions that can produce similar symptoms, including airway swelling, stridor, and respiratory distress. Because the treatments and urgency differ significantly, it is important to know how to distinguish between them.
Questions about these conditions commonly appear on the respiratory therapy board exam, particularly in pediatric airway scenarios.
Croup
Croup (laryngotracheobronchitis) is typically caused by a viral infection that results in inflammation and swelling of the upper airway, particularly below the vocal cords. This condition most often affects infants and young children. Symptoms usually develop gradually over one to two days.
The classic symptom of croup is a distinctive barking cough that resembles the sound of a seal. Patients may also present with inspiratory stridor and mild respiratory distress.
Key Characteristics:
- Subglottic Edema: Airway swelling occurs below the vocal cords.
- Gradual Onset: Symptoms typically develop over 24 to 48 hours.
- Barking Cough: A hallmark symptom caused by airway inflammation.
- Inspiratory Stridor: A high pitched sound during inspiration.
- Steeple Sign: A narrowing of the subglottic airway seen on a lateral neck x ray.
Note: Treatment for croup often includes humidified oxygen, corticosteroids, and nebulized epinephrine in more severe cases.
Epiglottitis
Epiglottitis is a serious bacterial infection that causes severe swelling of the epiglottis and surrounding structures. This swelling can rapidly obstruct the airway, making it a medical emergency.
The condition often develops suddenly and progresses quickly. Patients may appear extremely ill and may have difficulty swallowing or speaking.
Key Characteristics:
- Supraglottic Edema: Swelling occurs above the vocal cords.
- Rapid Onset: Symptoms may develop within a few hours.
- High Fever: Patients often present with a high temperature.
- Drooling: Difficulty swallowing causes excessive drooling.
- Thumb Sign: A swollen epiglottis visible on a lateral neck x ray.
Note: Because epiglottitis can lead to sudden airway obstruction, the priority is securing the airway. Patients often require intubation and antibiotic therapy.
Lateral Neck X Ray for Diagnosis
If clinical findings suggest either condition, a lateral neck x ray can help confirm the diagnosis. This imaging study helps distinguish the two conditions based on characteristic findings.
- Steeple Sign = Croup
- Thumb Sign = Epiglottitis
Note: Knowing the differences between these conditions will help you quickly identify the correct diagnosis on the board exam and select the appropriate treatment.
5. Understand Obstructive vs. Central Sleep Apnea
Sleep apnea is a disorder characterized by repeated episodes of breathing cessation during sleep. Each episode lasts at least 10 seconds and may occur dozens or even hundreds of times throughout the night.
Understanding the different types of sleep apnea is important for the respiratory therapy board exam. You should be able to recognize the clinical features, identify the underlying cause, and recommend the most appropriate treatment.
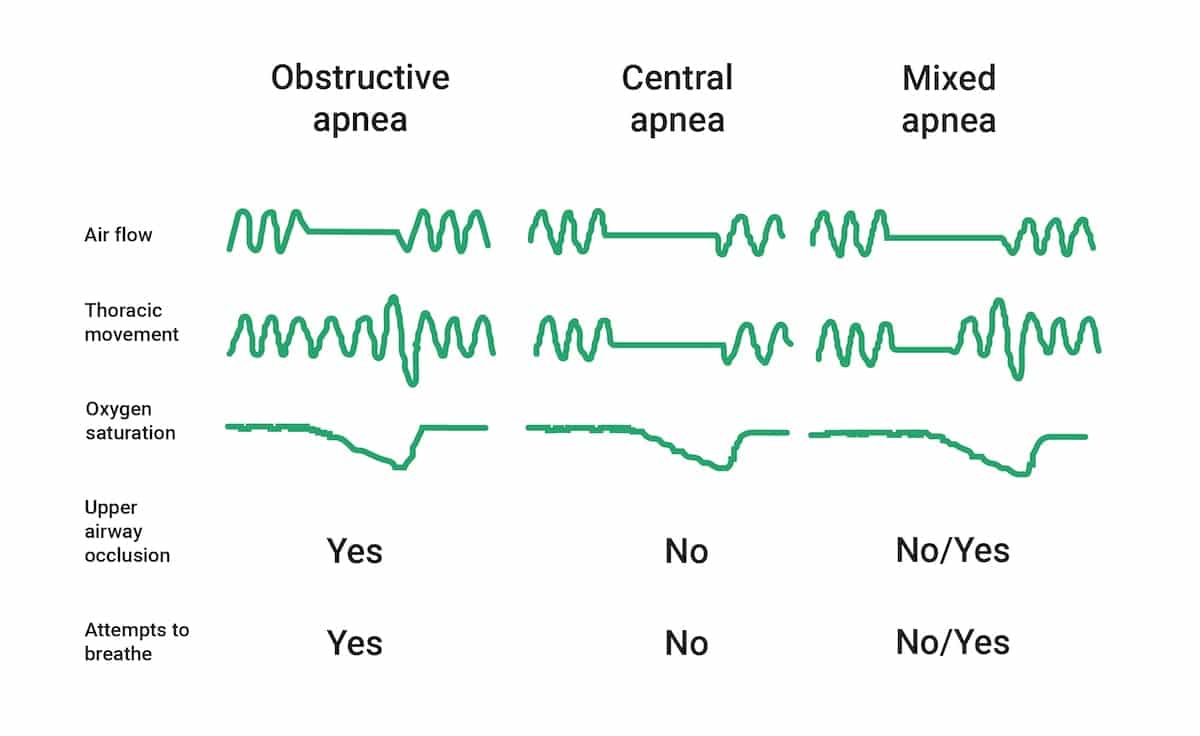
The two primary types are obstructive sleep apnea (OSA) and central sleep apnea (CSA). Although both conditions involve pauses in breathing, the mechanisms behind them are very different.
Obstructive Sleep Apnea
Obstructive sleep apnea (OSA) is the most common form of sleep apnea. It occurs when the upper airway becomes partially or completely blocked during sleep.
During sleep, the muscles of the throat relax. In some patients, this relaxation allows the airway to collapse, which prevents airflow despite continued breathing effort.
Patients with OSA continue attempting to breathe during apneic episodes, which can be observed as chest and abdominal movement.
Common risk factors for obstructive sleep apnea include:
- Obesity
- Short or thick neck
- Enlarged tonsils or tongue (macroglossia)
- Deviated nasal septum
- Upper airway structural abnormalities
Note: Patients with OSA often experience loud snoring, daytime sleepiness, fatigue, and morning headaches due to repeated oxygen desaturation during sleep.
Central Sleep Apnea
Central sleep apnea (CSA) occurs when the brain temporarily stops sending signals to the respiratory muscles. In this condition, there is no airway obstruction. Instead, the problem lies in the neurological control of breathing.
During apneic episodes, the patient makes no effort to breathe because the brain is not stimulating the respiratory muscles.
Central sleep apnea is often associated with:
- Neurological disorders
- Medullary dysfunction
- Certain medications such as opioids
- Heart failure
- High altitude exposure
Note: Because the central respiratory drive is impaired, patients experience periodic breathing patterns and intermittent pauses in ventilation.
How to Differentiate
A key concept that often appears on the board exam is identifying whether breathing effort is present during apnea.
- Obstructive Sleep Apnea: Breathing effort is present, but airflow is blocked due to airway obstruction.
- Central Sleep Apnea: No breathing effort is present because the brain is not stimulating respiration.
Note: If sleep apnea is suspected, the appropriate diagnostic test is a sleep study (polysomnography). This test monitors several physiological parameters including airflow, respiratory effort, oxygen saturation, heart rate, and brain activity during sleep.
Treatment Options
Treatment depends on the type and severity of sleep apnea.
- Obstructive Sleep Apnea: Continuous Positive Airway Pressure (CPAP) is the primary treatment. CPAP provides a constant level of pressure that keeps the airway open during sleep.
- Central Sleep Apnea: Bi-level Positive Airway Pressure (BiPAP) or adaptive servo ventilation may be used to support ventilation when the brain’s respiratory drive is impaired.
Understanding the difference between these two conditions will help you correctly interpret sleep studies and recommend the appropriate therapy.
- Obstructive Sleep Apnea = Effort to Breathe + Airway Obstruction
- Central Sleep Apnea = No Effort to Breathe + Lack of Respiratory Drive
Note: Sleep related breathing disorders are frequently tested on the board exam. Recognizing the difference between obstructive and central sleep apnea will help you quickly identify the correct diagnosis and treatment.
Unlock insider strategies and proven exam hacks to master key concepts, avoid common pitfalls, and pass the exam on your first (or next) attempt.
Final Thoughts
The pathology portion of the respiratory therapy board exam can seem overwhelming at first. However, with the right study approach and a strong understanding of common disease processes, you can confidently navigate this section of the exam.
Focus on learning the key symptoms, diagnostic findings, and treatment strategies associated with common cardiopulmonary conditions. Developing strong clinical reasoning skills will help you interpret exam questions and select the most appropriate answers.
It is also helpful to practice with exam style questions so that you become familiar with how clinical scenarios are presented. Many questions will require you to identify the disease first and then determine the most appropriate intervention.
Consistent practice, focused study sessions, and a solid understanding of pathology will significantly improve your chances of success.
If you found these tips helpful, check out our TMC Exam Hacks video course for additional strategies, exam tips, and study techniques that have helped thousands of respiratory therapy students succeed on the board exam.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Clinical Manifestations and Assessment of Respiratory Disease. Des Jardins, T, & Burton, GG. 9th edition. Elsevier. 2023.




