Spirometry is one of the most fundamental and widely used pulmonary function tests in respiratory care. It provides objective, quantitative data about lung function that helps clinicians evaluate airflow, diagnose respiratory conditions, and monitor disease progression.
For respiratory therapists, spirometry is more than just a diagnostic test. It is a critical skill that bridges physiology, patient coaching, and clinical interpretation.
Whether used in outpatient clinics, hospitals, or pulmonary laboratories, spirometry plays a central role in identifying obstructive and restrictive lung disorders and guiding appropriate patient care.
What Is Spirometry?
Spirometry is a pulmonary function test that measures the volume of air a person can inhale and exhale, as well as how quickly that air can be expelled from the lungs. During the test, the patient breathes through a mouthpiece connected to a spirometer, following specific instructions to inhale deeply and exhale forcefully.
The test evaluates airflow through the airways and provides numerical values and graphical representations that reflect lung mechanics. Because spirometry is noninvasive, relatively inexpensive, and easy to perform, it is often the first-line test used to assess pulmonary function.
Spirometry can be performed in a variety of settings, including pulmonary function laboratories, physician offices, outpatient clinics, occupational health programs, and bedside settings in some hospitalized patients.
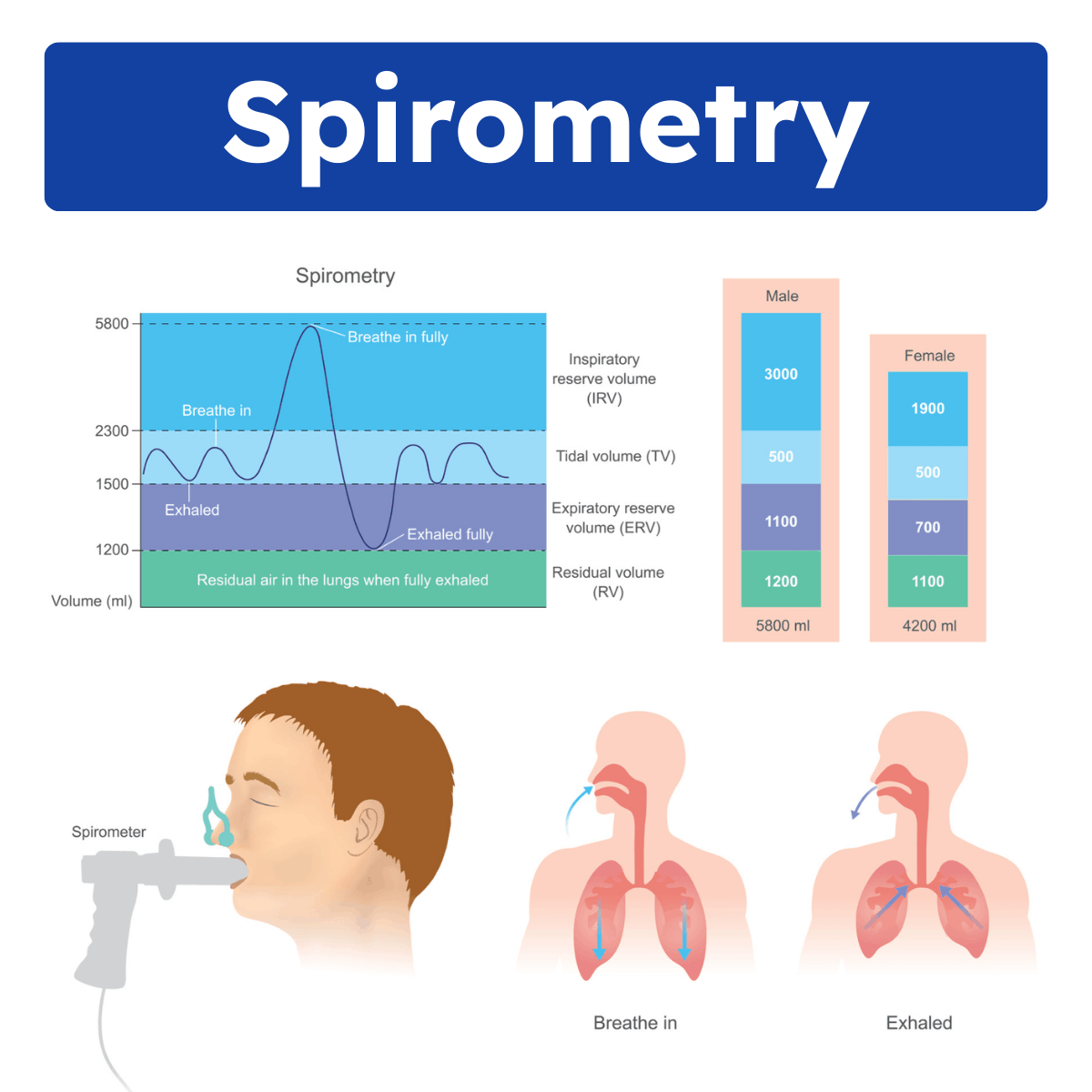
Key Measurements in Spirometry
Several important values are obtained during spirometry, each offering insight into different aspects of lung function.
Forced Vital Capacity (FVC)
FVC is the total volume of air a patient can forcibly exhale after taking a maximal inhalation. It reflects lung size and compliance and is particularly useful when evaluating restrictive lung disorders.
Forced Expiratory Volume in One Second (FEV₁)
FEV₁ measures the volume of air expelled during the first second of the forced exhalation. This is one of the most clinically significant spirometric values, as it reflects airway resistance and airflow limitation.
FEV₁/FVC Ratio
The FEV₁-to-FVC ratio helps differentiate between obstructive and restrictive patterns. A reduced ratio typically indicates obstructive lung disease, while a normal or increased ratio with a reduced FVC may suggest restriction.
Peak Expiratory Flow (PEF)
PEF represents the highest flow achieved during the forced exhalation. It reflects large airway function and is often used for monitoring asthma severity and control.
Forced Expiratory Flow 25–75% (FEF₂₅–₇₅)
This value reflects airflow in the mid-portion of exhalation and is sometimes used to assess small airway function, although it is more variable and less emphasized in clinical decision-making.
Flow–Volume Loops and Graphical Interpretation
In addition to numerical values, spirometry generates flow–volume and volume–time curves. These graphical tools are extremely valuable for identifying abnormal breathing patterns.
A flow–volume loop plots airflow on the vertical axis and lung volume on the horizontal axis. The shape of the loop can reveal airflow obstruction, restriction, or upper airway abnormalities. For example, scooped or concave expiratory limbs are characteristic of obstructive diseases, while a narrowed loop with reduced volume may suggest restriction.
Respiratory therapists rely heavily on these curves to assess test quality, identify patient effort issues, and recognize patterns that may not be immediately obvious from numbers alone.
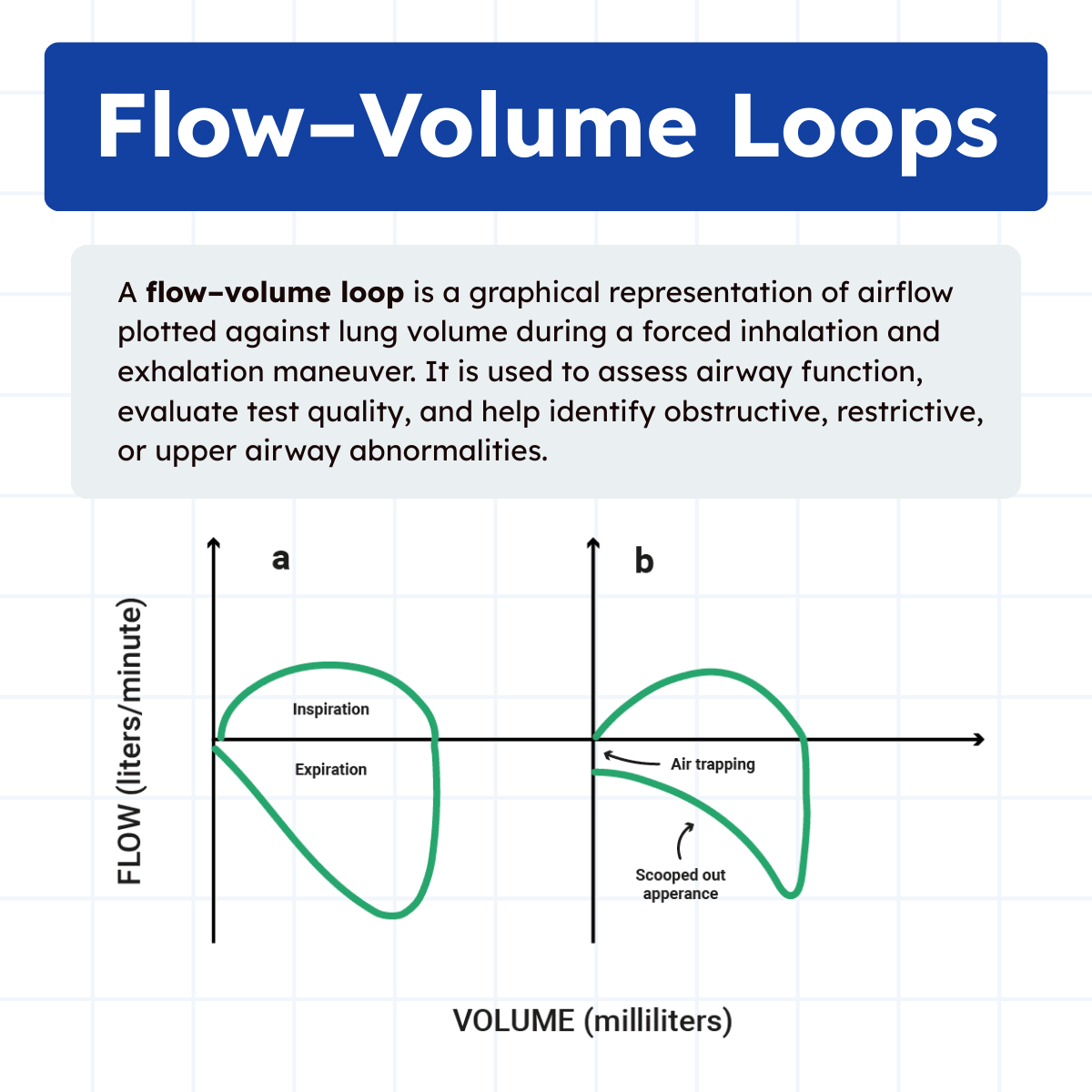
Indications for Spirometry
Spirometry is used for a wide range of clinical purposes, making it one of the most versatile diagnostic tools in respiratory care.
Common indications include:
- Diagnosing obstructive lung diseases such as asthma and COPD
- Evaluating unexplained dyspnea, cough, or wheezing
- Monitoring disease progression and response to therapy
- Assessing preoperative pulmonary risk
- Screening workers exposed to respiratory hazards
- Evaluating lung function in smokers and former smokers
Note: Because spirometry provides objective data, it is especially useful for tracking changes in lung function over time.
Spirometry and Obstructive Lung Disease
One of the primary uses of spirometry is identifying and characterizing obstructive lung disorders. In these conditions, airflow is limited due to airway narrowing, inflammation, or increased resistance.
Asthma
In asthma, spirometry often shows a reduced FEV₁ and FEV₁/FVC ratio during exacerbations. A hallmark feature is reversibility. After administration of a bronchodilator, a significant improvement in FEV₁ or FVC supports the diagnosis of asthma.
Chronic Obstructive Pulmonary Disease (COPD)
COPD is characterized by persistent airflow limitation. Spirometry typically reveals a reduced FEV₁ and a chronically low FEV₁/FVC ratio that does not fully normalize with bronchodilator therapy. Spirometry is essential for diagnosing COPD, staging severity, and monitoring progression.
Spirometry and Restrictive Lung Disease
Restrictive lung disorders are characterized by reduced lung volumes rather than airflow limitation. Spirometry may show a reduced FVC with a normal or elevated FEV₁/FVC ratio.
Common causes of restrictive patterns include interstitial lung disease, chest wall disorders, neuromuscular disease, and obesity. While spirometry alone cannot confirm restriction, it raises suspicion and often prompts further testing, such as lung volume measurements.
Note: For respiratory therapists, recognizing a restrictive pattern on spirometry is critical for appropriate referral and follow-up.
Bronchodilator Response Testing
Bronchodilator testing is frequently performed alongside baseline spirometry. After initial measurements are obtained, the patient receives a bronchodilator medication. Spirometry is then repeated to assess changes in lung function.
A significant increase in FEV₁ or FVC suggests reversible airway obstruction. This information helps differentiate asthma from COPD, guides treatment decisions, and provides insight into medication effectiveness.
Note: Respiratory therapists play a central role in administering bronchodilators, ensuring proper timing, and accurately repeating post-bronchodilator maneuvers.
Test Quality and Patient Coaching
Spirometry is highly effort-dependent. Accurate results rely on proper patient understanding, cooperation, and technique. Poor effort can lead to misleading values and incorrect interpretations.
Respiratory therapists are essential to test quality because they:
- Clearly explain and demonstrate the maneuver
- Coach patients throughout inhalation and exhalation
- Recognize cough, hesitation, or early termination
- Ensure reproducibility across multiple efforts
Note: Good coaching can be the difference between an uninterpretable test and clinically meaningful data.
Relevance to Respiratory Therapists
Spirometry is deeply embedded in the daily responsibilities of respiratory therapists. It combines technical skill, patient interaction, and clinical interpretation, making it a cornerstone of professional practice.
Respiratory therapists are often responsible for:
- Performing spirometry tests
- Ensuring equipment calibration and infection control
- Evaluating test acceptability and repeatability
- Identifying abnormal patterns
- Communicating results to providers
Note: A strong understanding of spirometry enhances a therapist’s ability to contribute meaningfully to patient care and interdisciplinary decision-making.
Spirometry in Preventive and Long-Term Care
Beyond diagnosis, spirometry plays a major role in preventive health and chronic disease management. It can detect early airflow limitation before symptoms become severe, allowing earlier intervention.
In chronic conditions, serial spirometry helps track disease progression, evaluate treatment effectiveness, and guide adjustments in therapy. This longitudinal perspective is especially valuable in managing asthma, COPD, and occupational lung disease.
Note: Respiratory therapists often develop long-term relationships with patients undergoing repeated spirometry, reinforcing education and adherence to treatment plans.
Limitations of Spirometry
While spirometry is invaluable, it does have limitations. It does not directly measure lung volumes such as residual volume or total lung capacity, nor does it assess gas exchange.
Results can also be influenced by patient effort, technique, and comorbid conditions. For this reason, spirometry should always be interpreted in the context of clinical history, symptoms, and additional testing when needed.
Note: Understanding these limitations helps respiratory therapists avoid overinterpretation and ensures appropriate clinical judgment.
The Role of Spirometry in the Future of Respiratory Care
As respiratory care continues to evolve, spirometry remains a foundational tool. Advances in portable devices, digital reporting, and remote monitoring are expanding access to spirometric testing beyond traditional settings.
For respiratory therapists, this means greater involvement in community health, telehealth initiatives, and preventive screening programs. Mastery of spirometry positions therapists at the forefront of early detection and chronic disease management.
Spirometry Practice Questions
1. What is spirometry?
A pulmonary function test that is used to differentiate between obstructive and restrictive lung diseases and determine the extent or progress of the disease.
2. What is the role of spirometry in primary care?
It provides an objective measure of airflow restriction or obstruction and assists with both the initial diagnosis of asthma and the assessment of asthma control.
3. Can spirometry measure residual volume?
No, it cannot measure RV.
4. Why is spirometry effort-dependent?
Spirometry is highly effort-dependent and relies on the patient for accurate results. Poor effort leads to poor quality data and poor effort spirometry will result in an underestimation of true values.
5. When does a spirometer not need to produce a graphic display?
Only when the vital capacity is to be measured.
6. How are the normal predicted values of spirometry reported?
Normal predicted values vary with the patient’s sex, age, height, and race. The mean normal values for FEV1 and FVC are 100% of predicted and the normal range is 80-120% of predicted.
7. Is spirometry testing more focused on inspiration or expiration?
Expiration
8. What is tidal volume?
The volume of gas that enters the lungs during normal breathing.
9. What is total lung capacity (TLC)?
The total volume of gas in the lungs at the end of a maximal inspiration.
10. What is vital capacity (VC)?
The volume of gas exhaled from maximal inspiration to maximal exhalation, which may be forced (FVC) or relaxed (SVC).
11. What is residual volume (RV)?
The gas remaining in the lungs after a maximal expiration. This volume of gas cannot be expelled, regardless of the maneuver performed.
12. What is functional residual capacity (FRC)?
The total volume of gas remaining in the lungs at the end of a tidal exhalation, which equals the sum of the RV and ERV.
13. What is inspiratory reserve volume (IRV)?
The volume of gas that must be inhaled at the end of a tidal inspiration to reach total lung capacity.
14. What is expiratory reserve volume (ERV)?
The volume of gas within the lungs that could still be exhaled after the end of a tidal exhalation.
15. What is normally recorded in either liters (L) or milliliters (mL) and is reported at body temperature, pressure, and saturation (BTPS)?
Vital capacity
16. Two acceptable vital capacity maneuvers should be obtained within what parameters?
The volumes should be within 150 mL.
17. What is the maximum volume of gas that can be expired when the patient exhales as forcefully and rapidly as possible after a maximal inspiration?
FVC
18. What are the three distinct phases of the FVC maneuver?
Maximal inspiration, a ”blast” of exhalation, and continued complete exhalation to the end of the test.
19. What two ways can the FVC be displayed?
Volume-time recording and flow-volume recording.
20. Can spirometry measure gas exchange?
No, you can learn about a patient’s gas exchange from spirometry but not directly measure it. Spirometry only measures gas volumes and time (flow = volume/time).
21. The premature termination of a spirometry test leads to what?
An FVC that is falsely low.
22. What values cannot be measured with a spirometer?
Residual volume and total lung capacity.
23. What is the difference between TLC and RV?
Vital capacity
24. What is FEV1?
Forced expiratory volume in 1 second
25. What does normal spirometry mean?
FVC greater than 80% of predicted, or 80-120% to fall within the normal range; FEV1/FVC ratio greater than or equal to 0.75.
Access our quiz with sample TMC practice questions and detailed explanations to help you master pulmonary function testing (PFT).
26. What is the FEV1 in an obstructive lung disease?
The FEV1 will be less than 100% of the predicted value.
27. What is the FVC in an obstructive lung disease?
The FVC will be decreased or normal.
28. What is the FEV1/FVC ratio in an obstructive disease?
The FEV1/FVC ratio will be less than 0.75.
29. What are some clinical examples of obstructive lung diseases?
Asthma, emphysema, bronchiectasis, chronic bronchitis, and cystic fibrosis.
30. What will the expiratory curve look like in obstructive lung diseases?
There will be a rapid rise to a peak but usually, there will be a ‘scooped-out’ appearance/concavity. This is indicative of expiratory airflow obstruction, usually of the small airways.
31. What will the inspiratory curve look like in obstructive lung diseases?
The inspiratory curve is relatively well preserved. Remember, most clinical diseases have normal inspirations and it’s the expiration that is suboptimal.
32. In a restrictive disease, why is the peak flow of expiration greater than it is in a normal individual?
In restrictive disease, the lungs are very stiff and they empty more quickly than normal.
33. What is the FEV1 in a restrictive lung disease?
The FEV1 may be decreased or normal (if normal, it will be low-normal).
34. What is the FVC in a restrictive lung disease?
The FVC will be decreased (i.e., less than 80%). This is the key point wherein VC has to be low if you are going to call it a true restrictive pattern.
35. What is the FEV1/FVC ratio in a restrictive lung disease?
The FEV1/FVC ratio will be greater than or equal to 0.75.
36. What are some examples of restrictive lung diseases?
Pulmonary fibrosis and pleural effusion.
37. What happens during quiet breathing?
Inspiration involves muscular contractions and expiration is passive with no accessory muscle usage.
38. What do you call breathing that involves active inspiratory and expiratory movements?
Hyperpnea
39. What is the amount of air that a patient expels if they inhale as deeply as possible and then blow the air out until they cannot exhale anymore?
Vital capacity
40. What is the resting tidal volume?
It is the amount of air inhaled or exhaled with each breath under resting conditions. The normal value is 500 mL in both males and females.
41. What is the normal value for expiratory reserve volume (ERV)?
1,000-1,200 mL
42. What is the normal value for residual volume?
The normal value for males is 1,200 mL and 1,100 mL for females.
43. What is the normal value for inspiratory reserve volume (IRV)?
The normal value for males is about 3,300 mL and 1,900 mL for females.
44. What is the formula for inspiratory capacity?
IC = TV + IRV
45. What is the formula for functional residual capacity (FRC)?
FRC = ERV + RV
46. What is the normal value for vital capacity?
The normal value for males is 4,800 mL and 3,400 mL for females.
47. What is the normal value for total lung capacity?
The normal TLC for males is 6,000 mL and 4,500 mL for females.
48. How many breaths can you take each minute?
The resting adult respiratory rate ranges from 12 to 18 breaths per minute with approximately one breath every four heartbeats.
49. When does an increased FRC occur?
In obstructive diseases like emphysema and chronic bronchitis.
50. When does a decreased or normal FRC occur?
In restrictive diseases like pulmonary fibrosis.
51. What is a forced expiratory volume?
It examines the percentage of the vital capacity that is exhaled during specific time intervals of the FVC test. Healthy people can exhale 75-85% of their FVC in the first second.
52. What does a lower pH change?
It changes the shape of the Hb molecules and they release their oxygen more readily.
53. What are the indications for using spirometry?
Diagnosis, monitoring, public health, and disability/impairment evaluations.
54. How do you establish an asthma diagnosis with spirometry?
Detailed medical history to determine episodic symptoms of airflow obstruction or hyper-responsiveness like a cough, wheezing, and shortness of breath with exercise. Next is the physical exam to assess the respiratory tract, chest, and skin. Lastly, reversibility is determined either by an increase in FEV1 by greater than 12% from the baseline.
55. What does the reliability of spirometry depend on?
Reproducible efforts and technique; 3 consistent, 6-second efforts.
56. What do predicted values in spirometry depend on?
The individual’s age, gender, height, and race.
57. What is the percent predicted?
The numbers are presented as percentages of the average expected in someone of the same age, height, sex, and race.
58. What can reduce a patient’s FVC?
Lung diseases, pleural cavity, chest wall restriction, or respiratory muscle weakness.
59. In a restrictive lung disease, what happens to the FEV1/FVC?
It decreases proportionately, hence the ratio is in the normal range.
60. What are the characteristics of flow-volume loops?
A classic flow-volume loop has a rapid peak and expiratory flow rate with a gradual decline in the flow back to zero. An obstructive pattern loop also has a rapid peak, but the curve descends more quickly than normal, taking on a concave shape. A restrictive pattern retains the shape of a normal curve, but the size of the curve appears smaller.
61. A 56-year-old female patient has bedside spirometry results showing a decreased FVC, a normal FEV1, and an increased FEV1/FVC ratio. Which pattern do these findings most strongly suggest?
Restrictive lung disease
62. Why does an increased FEV1/FVC ratio argue against obstructive lung disease?
Because obstructive disease is characterized by a reduced FEV1/FVC ratio due to airflow limitation.
63. Which spirometry finding is most consistent with restrictive lung disease?
Reduced lung volumes with preserved or increased airflow ratios.
64. Simple spirometry can measure all of the following except which variable?
Residual volume
65. Why can residual volume not be measured with simple spirometry?
Because residual volume represents air that cannot be exhaled from the lungs.
66. Which lung volumes can be measured using simple spirometry?
Tidal volume, vital capacity, and inspiratory reserve volume.
67. Which test is required to directly measure residual volume?
Body plethysmography
68. A patient has a total lung capacity (TLC) and residual volume (RV) both greater than 120% of predicted. What does this finding indicate?
Significant air trapping consistent with obstructive lung disease
69. How do lung volumes typically differ between obstructive and restrictive diseases?
Obstructive disease shows increased TLC and RV, while restrictive disease shows decreased TLC and RV.
70. A spirometry report shows markedly reduced expiratory flow rates compared to predicted values. What type of lung disease does this most strongly suggest?
Obstructive lung disease
71. What spirometry pattern is most consistent with obstructive lung disease?
Reduced FEV1, normal or reduced FVC, and a decreased FEV1/FVC ratio
72. What spirometric change is typically seen first in early obstructive lung disease?
A reduction in FEV1
73. In restrictive lung disease, how does FVC typically change?
It is decreased due to reduced lung expansion.
74. What does a normal FEV1/FVC ratio with a reduced FVC suggest?
Restrictive lung disease
75. Why is spirometry considered a flow-based pulmonary function test?
Because it measures airflow rates during forced exhalation.
76. What spirometry value reflects large airway function most strongly?
FEV1
77. What does a concave or “scooped-out” flow-volume loop indicate?
Obstructive lung disease
78. What spirometric finding suggests poor patient effort rather than lung disease?
Proportionally reduced FEV1 and FVC with a normal ratio and irregular flow pattern
79. Why is patient coaching critical during spirometry testing?
Because inadequate effort can lead to falsely abnormal results.
80. What is the purpose of repeating spirometry maneuvers multiple times?
To ensure reproducibility and test validity.
81. What is considered an acceptable level of repeatability for FEV1 and FVC?
Values within 150 mL of each other.
82. Which spirometry parameter is most affected by airway obstruction?
FEV1
83. What does an increase in FEV1 after bronchodilator administration indicate?
Reversible airflow obstruction
84. How much improvement in FEV1 is typically considered a significant bronchodilator response?
An increase of at least 12% and 200 mL.
85. Why is spirometry useful in differentiating obstructive from restrictive disease?
Because it evaluates airflow limitation and lung volume patterns.
86. What does a reduced peak expiratory flow (PEF) most commonly indicate?
Airflow limitation or poor patient effort.
87. Which disease typically presents with a normal or increased FEV1/FVC ratio?
Restrictive lung disease
88. What spirometry finding is most characteristic of asthma?
Reversible airflow obstruction with bronchodilator response.
89. How does emphysema typically affect spirometry results?
It reduces expiratory flows and lowers the FEV1/FVC ratio.
90. What does an abnormally low FEV1/FVC ratio indicate?
Airflow obstruction
91. Why can spirometry alone not definitively diagnose restrictive lung disease?
Because lung volumes such as TLC must be measured to confirm restriction.
92. What spirometric change is expected with severe air trapping?
Increased residual volume with reduced expiratory flow.
93. What does a flattened inspiratory and expiratory limb on a flow-volume loop suggest?
Fixed upper airway obstruction
94. What spirometry finding suggests variable extrathoracic airway obstruction?
Flattening of the inspiratory portion of the flow-volume loop.
95. What spirometry finding suggests variable intrathoracic airway obstruction?
Flattening of the expiratory portion of the flow-volume loop.
96. Why is FVC often reduced in obstructive lung disease?
Because air trapping limits complete exhalation.
97. What spirometry parameter is most effort-dependent?
Peak expiratory flow
98. When should spirometry testing be avoided or postponed?
During acute respiratory distress or recent thoracic surgery.
99. What does a normal spirometry test indicate?
Normal airflow and lung volumes based on predicted values.
100. Why is spirometry considered a cornerstone test in respiratory assessment?
Because it provides objective measurement of airflow limitation and ventilatory patterns.
Final Thoughts
Spirometry is one of the most important diagnostic tools in respiratory care, offering essential insight into lung function, airflow limitation, and disease progression. For respiratory therapists, it represents a blend of science, skill, and patient-centered care.
Accurate performance and interpretation of spirometry directly influence diagnosis, treatment decisions, and long-term outcomes for patients with respiratory disease.
By mastering spirometry, respiratory therapists strengthen their clinical expertise, enhance collaboration with healthcare teams, and play a vital role in improving respiratory health across diverse care settings.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Lamb K, Theodore D, Bhutta BS. Spirometry. [Updated 2023 Aug 17]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025.


