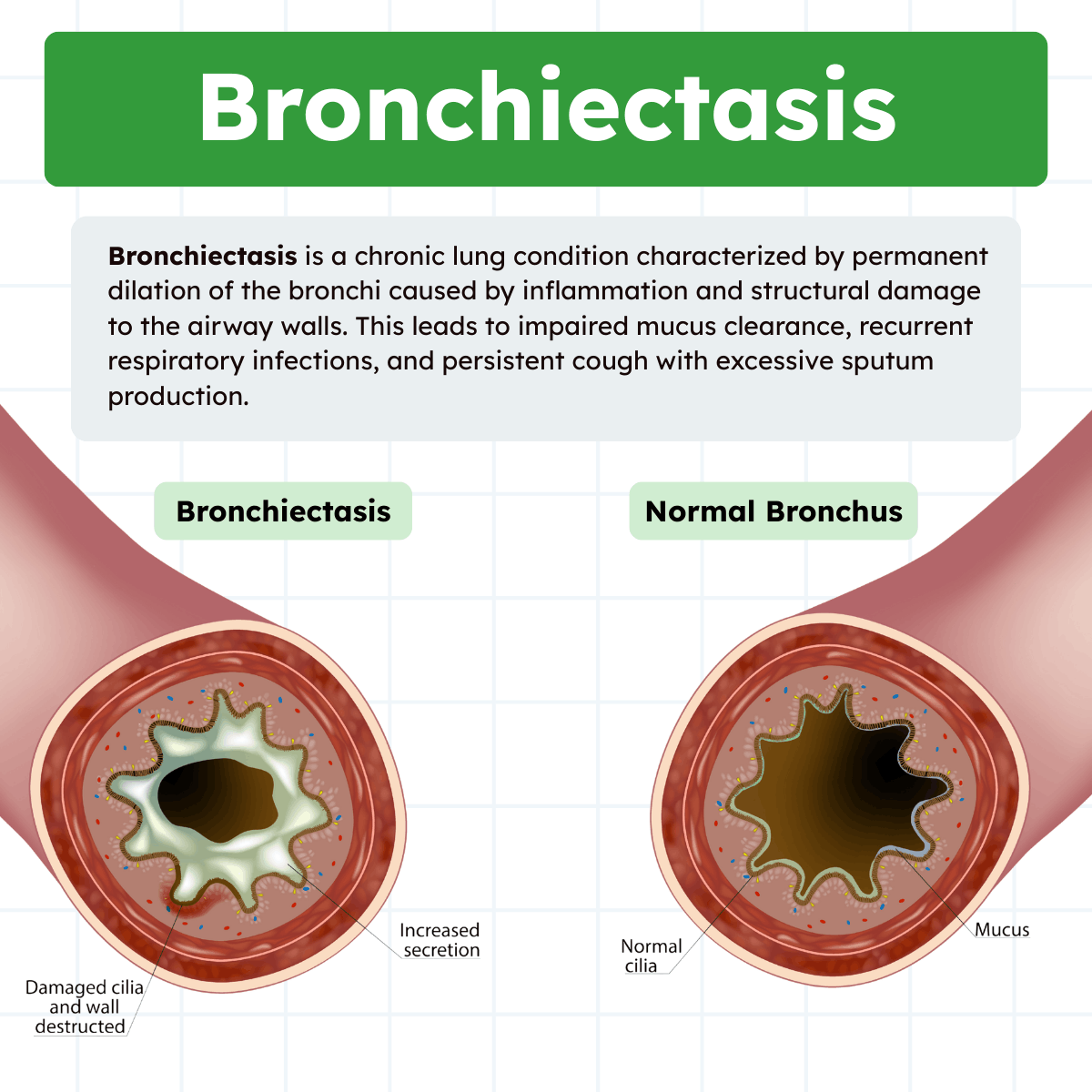
Bronchiectasis is a chronic respiratory condition characterized by abnormal and permanent dilation of the bronchi due to repeated inflammation and structural damage to the airway walls. This process disrupts normal mucociliary clearance and leads to persistent infection, excessive mucus production, and progressive airway dysfunction.
Although it is less common than other obstructive lung diseases such as asthma and COPD, bronchiectasis remains clinically important because it contributes to significant morbidity and frequent respiratory exacerbations.
Understanding its causes, pathophysiology, clinical features, and diagnostic evaluation is essential for respiratory therapists and other healthcare professionals involved in the care of patients with chronic lung disease.
What is Bronchiectasis?
Bronchiectasis refers to a structural abnormality of the airways in which the bronchi become permanently dilated due to destruction of the muscular and elastic components of the bronchial walls. This damage usually occurs as a result of chronic infection, inflammation, or impaired airway clearance.
Under normal conditions, the bronchi are designed to conduct air to the lungs while clearing mucus and foreign particles through the mucociliary escalator. In bronchiectasis, the structural integrity of the airway walls is compromised. As a result, mucus accumulates within the dilated airways, providing an environment that promotes bacterial growth and recurrent infection.
This cycle of infection and inflammation leads to further airway damage, worsening mucus retention, and progressive lung impairment. Over time, this process may cause airflow obstruction, impaired gas exchange, and reduced lung function. Bronchiectasis may affect a localized region of the lung or involve multiple lobes, depending on the underlying cause.
Anatomic Types of Bronchiectasis
Bronchiectasis can be classified into three major anatomic patterns based on the appearance of the affected airways.
Cylindrical Bronchiectasis
Cylindrical bronchiectasis is the most common form. In this pattern, the bronchi are uniformly dilated with relatively smooth airway walls. The airways appear widened but maintain a tubular shape. Although this type represents structural damage, it is generally considered the least severe form compared with other patterns.
Varicose Bronchiectasis
Varicose bronchiectasis demonstrates an irregular pattern of airway dilation. The bronchi exhibit alternating areas of narrowing and dilation, producing an appearance similar to varicose veins. This irregular structure disrupts normal airflow and mucus clearance, increasing the risk of infection and airway obstruction.
Cystic Bronchiectasis
Cystic bronchiectasis is the most advanced and severe form. In this pattern, the distal airways progressively enlarge and form saclike dilations. These cystic structures may fill with mucus or infected secretions, contributing to severe symptoms, frequent infections, and significant impairment in pulmonary function.
Pathophysiology
The development of bronchiectasis is commonly explained by a cycle of airway injury, impaired mucus clearance, infection, and inflammation. Initial damage to the airway wall may occur from infection, obstruction, immune deficiency, or genetic disorders affecting mucociliary function. Once the airway structure is compromised, mucus clearance becomes ineffective.
Accumulated mucus provides a favorable environment for bacterial growth. Recurrent infections then trigger persistent inflammation within the airway walls. Inflammatory mediators and enzymes released by immune cells contribute to further destruction of the bronchial wall.
This process weakens the structural support of the airways, allowing them to become permanently dilated. The enlarged airways trap secretions and impair airflow, which perpetuates the cycle of infection and inflammation.
Note: As the disease progresses, airflow obstruction may develop, particularly when mucus plugs block smaller airways.
Causes of Bronchiectasis
Bronchiectasis can arise from a wide range of underlying conditions that impair airway clearance, cause repeated infection, or damage the airway structure.
The causes are often categorized as localized or diffuse.
Localized Bronchiectasis
Localized bronchiectasis affects a specific region of the lung and is typically associated with an obstruction or structural abnormality of the airway.
Common causes include:
- Foreign body aspiration
- Benign airway tumors such as adenomas
- External compression of the bronchi by enlarged lymph nodes
- Middle lobe syndrome
Note: When airflow is obstructed, mucus accumulates distal to the blockage, increasing the risk of infection and inflammation. Over time, this process may result in permanent dilation of the affected bronchi.
Diffuse Bronchiectasis
Diffuse bronchiectasis involves multiple regions of the lung and is usually associated with systemic conditions that impair mucociliary clearance or immune defense.
Examples include:
- Cystic fibrosis
- Primary ciliary dyskinesia disorders such as Kartagener syndrome
- Hypogammaglobulinemia
- Alpha-1 antitrypsin deficiency
- Allergic bronchopulmonary aspergillosis
- Autoimmune disorders such as rheumatoid arthritis and Sjogren syndrome
Note: Severe childhood respiratory infections may also contribute to the development of diffuse bronchiectasis. Infections from conditions such as measles, influenza, or whooping cough can damage the airway walls and predispose individuals to long-term structural changes.
Clinical Manifestations
The hallmark symptom of bronchiectasis is chronic production of large amounts of purulent sputum. Patients often report daily cough with thick mucus that may be yellow or green due to infection.
Respiratory symptoms often worsen during exacerbations, which are typically triggered by bacterial infection.
Common clinical features include:
- Chronic productive cough
- Excessive sputum production
- Recurrent respiratory infections
- Dyspnea
- Fatigue
- Chest discomfort
Hemoptysis is also frequently observed in patients with bronchiectasis. In most cases it is mild and occurs intermittently. However, severe bleeding can occur and may require urgent medical intervention.
The severity of symptoms varies widely depending on the extent of airway involvement and the underlying cause of the disease. Some patients experience relatively mild symptoms with occasional exacerbations, while others develop progressive respiratory impairment with frequent hospitalizations.
Physical Examination Findings
Physical examination findings in bronchiectasis are often related to mucus retention and airway obstruction. Common auscultatory findings include coarse crackles that may be heard over affected lung regions. These crackles are often described as moist or bubbling sounds produced by air moving through mucus-filled airways.
Wheezing may also be present, particularly in patients who develop airflow obstruction similar to that seen in other obstructive lung diseases.
In advanced cases, digital clubbing may be observed. This finding reflects chronic hypoxia and long-standing pulmonary disease.
Note: Patients with severe disease may also show signs of respiratory distress during exacerbations.
Diagnostic Evaluation
The diagnosis of bronchiectasis is confirmed through imaging studies that demonstrate abnormal airway dilation.
Chest Radiography
Chest radiography may provide initial clues suggesting bronchiectasis. Findings may include cystic spaces, increased bronchovascular markings, or tram track signs. Tram tracks appear as thin parallel lines representing the thickened walls of dilated bronchi.
Although chest x-rays may suggest the presence of bronchiectasis, they are not sufficiently sensitive or specific to confirm the diagnosis.
Computed Tomography
High-resolution computed tomography is considered the diagnostic standard for bronchiectasis. The hallmark CT finding is airway dilation in which the diameter of the bronchus exceeds that of the adjacent pulmonary artery branch. This relationship is often referred to as the signet ring sign.
CT imaging also provides valuable information about the distribution and severity of disease, which can help guide treatment decisions.
Because temporary airway dilation may occur after acute pneumonia, CT imaging should generally be delayed for several weeks after resolution of infection. This helps ensure that the findings represent true structural bronchiectasis rather than reversible inflammatory changes.
Pulmonary Function Testing
Pulmonary function tests are commonly used to evaluate the physiologic impact of bronchiectasis on lung function. Many patients demonstrate an obstructive ventilatory pattern characterized by reduced expiratory flow rates. In some cases, a mixed obstructive and restrictive pattern may also be observed.
Measurements such as FEV1 and FVC help clinicians assess disease severity, monitor progression, and evaluate response to treatment. Pulmonary function testing is also important for distinguishing bronchiectasis from other respiratory conditions that produce similar symptoms.
Treatment and Management Overview
Bronchiectasis management focuses on reducing infection burden, improving mucus clearance, minimizing exacerbations, and addressing the underlying cause when possible. Most treatment plans combine antimicrobial therapy with airway clearance strategies and supportive respiratory care.
The approach is often individualized based on symptom severity, sputum microbiology, frequency of exacerbations, and the presence of comorbid conditions such as asthma or COPD.
Antibiotic Therapy
Antibiotics are commonly used to treat acute exacerbations and, in selected patients, to reduce the frequency of recurrent infections.
Treatment of Exacerbations
Exacerbations are typically characterized by worsening cough, increased sputum volume, change in sputum color, increased dyspnea, and systemic symptoms such as fatigue or fever. Because bacterial infection is a frequent trigger, antibiotics are often indicated when clinical features suggest infection, particularly when sputum becomes more purulent.
When possible, antibiotic selection should be guided by prior sputum cultures and local resistance patterns. For patients who produce sputum regularly, periodic cultures can help identify chronic colonization and inform future therapy.
Long-Term or Scheduled Antibiotic Use
Some patients experience frequent exacerbations despite adherence to airway clearance techniques. In these cases, clinicians may consider intermittent or long-term antibiotic regimens to reduce exacerbation frequency and improve quality of life.
Long-term antibiotic strategies require careful monitoring due to risks such as antibiotic resistance, adverse drug reactions, and effects on the microbiome. Decisions about chronic antibiotic use should be individualized and reassessed regularly.
Pseudomonas aeruginosa Colonization
Chronic colonization with Pseudomonas aeruginosa is clinically important because it is associated with more severe disease and increased exacerbation risk. In some patients, inhaled antibiotics may be considered to reduce bacterial load and exacerbations.
Inhaled aminoglycosides are sometimes used in patients with chronic P. aeruginosa colonization. Inhaled fluoroquinolones have also been studied in both cystic fibrosis and non-cystic fibrosis bronchiectasis populations. The role of these therapies continues to evolve, but the overall goal is to reduce infection burden while limiting systemic side effects.
Airway Clearance and Bronchopulmonary Hygiene
Airway clearance is central to bronchiectasis management because retained secretions contribute to airflow obstruction, infection, and inflammation. Effective secretion clearance can reduce symptoms, improve exercise tolerance, and lower exacerbation frequency.
Chest Physiotherapy and Postural Drainage
Traditional chest physiotherapy includes postural drainage, percussion, vibration, and coached coughing techniques. Positioning helps use gravity to mobilize secretions from affected lung segments. Percussion and vibration can loosen mucus, making it easier to expectorate.
Respiratory therapists frequently teach these techniques, tailor them to the patient’s imaging findings and functional status, and help patients build sustainable home routines.
Oscillatory Devices and Positive Expiratory Pressure
Oscillatory positive expiratory pressure devices may help mobilize mucus by combining airway splinting with vibratory forces that loosen secretions. These devices can be useful for patients who have difficulty tolerating manual chest physiotherapy or who need portable options for daily use.
RTs are often responsible for device selection, training, and troubleshooting, including monitoring technique and adherence.
High-Frequency Chest Wall Oscillation
High-frequency chest wall oscillation vest therapy is widely used in cystic fibrosis and is also used in some non-cystic fibrosis bronchiectasis patients. The vest generates rapid oscillations that create small-volume airflow changes within the airways, helping mobilize secretions.
Typical treatments are performed for about 20 to 30 minutes twice daily, though frequency can be adjusted based on symptom burden and exacerbation risk. RTs play a key role in assessing response, coordinating equipment access, and ensuring appropriate technique.
Humidification and Hydration
Adequate humidification can help thin secretions and support mucus clearance. Some patients benefit from heated humidification, particularly if they are using oxygen therapy or noninvasive ventilation, since dry gas can worsen secretion retention.
Hydration also supports secretion mobilization, though fluid recommendations must be individualized in patients with comorbid conditions such as heart failure.
Bronchodilators and Airflow Obstruction
Airflow obstruction is common in bronchiectasis, either due to mucus plugging, airway wall thickening, or overlap with asthma or COPD. Bronchodilators may be helpful for symptom relief and to improve airflow, particularly in patients with reversible bronchospasm.
Beta-Agonists and Anticholinergics
Short-acting beta-agonists such as albuterol may reduce dyspnea and improve exercise tolerance in some patients. They may also support secretion clearance by improving airflow and, in some settings, enhancing mucociliary transport.
Long-acting bronchodilators may be considered when patients have chronic airflow obstruction or coexisting COPD. Respiratory therapists often monitor clinical response and help patients optimize inhaler technique and device selection.
Hyperosmolar Agents
Hyperosmolar therapies are used to draw water into the airway lumen, reduce mucus viscosity, and improve clearance. Their use is more established in cystic fibrosis, but selected bronchiectasis patients may benefit.
Hypertonic Saline
Inhaled hypertonic saline can improve airway hydration and may help with sputum clearance. Some patients report easier expectoration and reduced cough intensity, though tolerance can vary. Bronchospasm is a potential side effect, so bronchodilator pretreatment may be considered when appropriate.
Mannitol
Inhaled dry powder mannitol has been studied as a method of improving tracheobronchial clearance. It may improve mucus clearance in some patients, though clinical benefit and tolerance can vary. Patients should be monitored for cough, bronchospasm, and overall symptom response.
Mucolytics and N-Acetylcysteine
N-acetylcysteine is a mucolytic agent that can be administered by nebulization or direct instillation. It works by disrupting disulfide bonds within mucus glycoproteins, thereby reducing viscosity.
Despite strong mucolytic effects in laboratory settings and long-standing clinical use, evidence supporting routine use of aerosolized or oral N-acetylcysteine for chronic lung disease remains mixed.
Some studies suggest benefit in reducing exacerbations in chronic bronchitis and COPD when used orally, but results are not consistent across populations. If used, patients should be monitored for bronchospasm, unpleasant odor, and tolerance during administration.
Management of Hemoptysis
Hemoptysis is common in bronchiectasis and may range from mild blood-streaked sputum to life-threatening bleeding.
Non-Massive Hemoptysis
Mild hemoptysis often occurs during exacerbations due to airway inflammation and fragile bronchial vessels. Management typically focuses on treating infection, optimizing airway clearance, and reviewing medications that could increase bleeding risk.
Massive Hemoptysis
Massive hemoptysis is a medical emergency and requires immediate assessment, airway protection when indicated, and coordination with critical care and interventional services. One common intervention is bronchial artery embolization, which may control bleeding by targeting the source vessel.
Note: Respiratory therapists may assist with airway management, oxygen delivery, and ventilatory support, as well as monitoring respiratory status during stabilization.
Surgical and Interventional Options
Surgical resection is generally reserved for a small subset of patients, typically those with localized bronchiectasis who remain severely symptomatic despite medical therapy or who develop recurrent, significant hemoptysis.
In carefully selected cases, removal of the affected lung segment or lobe can reduce infection burden and improve symptoms. However, surgery carries significant risk and requires thorough evaluation of pulmonary reserve and overall health status.
Why Bronchiectasis Matters in Respiratory Care
Bronchiectasis is highly relevant to respiratory therapists because management relies heavily on respiratory therapies that support airway clearance, reduce work of breathing, and maintain adequate oxygenation and ventilation.
Role in Diagnosis and Assessment
Respiratory therapists frequently perform pulmonary function testing that identifies airflow obstruction and helps quantify severity. RTs may also recognize key clinical patterns such as chronic productive cough, copious purulent sputum, recurrent infections, or intermittent hemoptysis that should prompt further evaluation.
RTs involved in outpatient testing or pulmonary rehabilitation may be among the first clinicians to identify patients who need additional diagnostic assessment, including imaging and specialist referral.
Role in Acute Care
In acute exacerbations, RTs commonly administer bronchodilators, assist with airway clearance therapies, and support oxygen therapy. In more severe cases, RTs may be involved in managing arterial blood gases, setting up and monitoring noninvasive ventilation, and assisting with invasive mechanical ventilation in the ICU.
Airway clearance strategies, including manual chest physiotherapy, oscillatory devices, and high-frequency chest wall oscillation, often require RT expertise to be effective and safe.
Role in Long-Term Management and Education
Bronchiectasis often requires daily, lifelong self-management. RTs play a key role in teaching airway clearance routines, inhaler technique, device use, and infection prevention strategies.
In pulmonary rehabilitation, RTs help patients improve exercise tolerance, manage dyspnea, and develop sustainable strategies for symptom control. RTs working in home care may assist with equipment setup, humidification strategies, and adherence support for airway clearance therapies.
Bronchiectasis Practice Questions
1. What is bronchiectasis?
Bronchiectasis is a chronic lung condition characterized by irreversible widening and damage to the bronchial tubes, leading to persistent coughing, difficulty breathing, and recurrent lung infections.
2. What are the causes of bronchiectasis?
Bronchiectasis can be caused by various factors, including respiratory infections, autoimmune diseases, genetic mutations, exposure to irritants, severe allergies, and certain underlying conditions, leading to the irreversible widening and damage of the bronchial tubes in the lungs.
3. What is the pathophysiology of bronchiectasis?
The pathophysiology of bronchiectasis involves the permanent dilation and damage of the bronchial tubes due to chronic inflammation and infection, leading to impaired mucociliary clearance and recurrent respiratory infections.
4. What are the shapes of the destroyed bronchial walls?
Varicose, fusiform, saccular, cystic, and cylindrical.
5. Is there a cure for bronchiectasis?
There is no cure for this disease; however, teatment and management of the symptoms are very important.
6. What are some signs, symptoms, and observations of bronchiectasis?
It often causes a continuous cough with a large amount of sputum, recurrent local pneumonia, occasional hemoptysis, and increasing dyspnea.
7. What breath sounds are associated with a severe state of bronchiectasis?
Rales and rhonchi
8. What is the old method of diagnosing bronchiectasis?
Bronchogram
9. What is the latest method used to diagnose bronchiectasis?
CT scan and HRCT
10. What happens in the lungs of patients suffering from bronchiectasis?
Bronchial walls are destroyed, mucosal atrophy, cilia are destroyed, elastic area is filled with pus, and the distal areas become obstructed.
11. What are some problems associated with bronchiectasis?
Digital clubbing, atelectasis, consolidation, increased thickness of the A-C membrane, bronchospasm, and excessive bronchial secretions.
12. What does the pulmonary function test of a patient with bronchiectasis typically show?
Obstructive patterns
13. What does the ABG show in a patient with mild to moderate bronchiectasis?
Respiratory alkalosis with hypoxemia
14. What does the ABG show in a patient with severe bronchiectasis?
Compensated respiratory acidosis with hypoxemia
15. What are some common infections associated with bronchiectasis?
Haemophilus influenzae, streptococcus, staphylococcus, pneumonia, moraxella catarrhalis, and pseudomonas in cystic fibrosis patients.
16. Why is airway clearance important in the treatment and management of bronchiectasis?
Airway clearance improves the patient’s ability to breathe and decreases the risk of infections.
17. What is the prognosis of bronchiectasis?
The prognosis is extremely variable and depends on the extent of the damage. Good management is very important.
18. What are the ABG results for patients with bronchiectasis?
For mild to moderate cases, it shows acute alveolar hyperventilation with hypoxemia. In severe cases, the results will show chronic ventilatory failure with hypoxemia.
19. What ethnicity is bronchiectasis more common in?
Bronchiectasis is more common in Asians and Pacific Islanders and less common in African Americans.
20. What age is bronchiectasis more common in older patients?
Bronchiectasis is more common among people 50-70 years old.
21. Is bronchiectasis more common in men or women?
Bronchiectasis is more common in women.
22. What is the etiology of bronchiectasis?
50% of bronchiectasis cases are idiopathic, 25% occurs from a post-infection condition, and 15% is caused by systemic diseases. Many people with cystic fibrosis end up with bronchiectasis, but this is a small portion of the total population.
23. What lung condition is bronchiectasis often misdiagnosed as?
Asthma
24. How do you diagnose bronchiectasis?
CT scan and a history of a chronic cough with sputum.
25. How does cystic fibrosis cause bronchiectasis?
Cystic fibrosis causes bronchiectasis by producing thick, sticky mucus that obstructs the airways, leading to chronic infections, inflammation, and eventually, the dilation and scarring of the bronchial walls.
26. What are the laboratory results of hemoglobin and hematocrit in patients with bronchiectasis?
The results will show increased values.
27. How do you treat chronic bronchiectasis with pseudomonas?
Azithromycin
28. What will a CT scan look like for a patient with post-tuberculosis bronchiectasis?
The lower left lung will show evidence of local damage.
29. What is a primary ciliary dyskinesia?
Primary ciliary dyskinesia is a hereditary condition characterized by defective ciliary structure and function, leading to impaired mucociliary clearance and resulting in chronic respiratory tract infections and associated complications.
30. What are the complications of primary ciliary dyskinesia?
Neonatal respiratory distress, daily wet cough from birth, chronic airway disease with age-dependent bronchiectasis, recurrent otitis media, and reduced fertility.
31. What are the clinical symptoms associated with bronchiectasis?
The symptoms include neonatal respiratory problems, recurrent otitis media, recurrent sinusitis, recurrent pancreatitis, gastrointestinal disease, infertility in men, and finger clubbing. In addition, patients will have recurring coughs with lots of infected sputum, intermittent hemoptysis, persistent halitosis or bad breath, dyspnea, and recurrent febrile episodes.
32. What are macrolides in treating bronchiectasis?
Macrolides are helpful in bronchiectasis because they are both anti-inflammatory and anti-microbial. Macrolides reduce bronchiectasis exacerbations, improve quality of life, and decrease inflammation.
33. When do you use IV antibiotics to treat bronchiectasis?
IV antibiotics are used during a bronchiectasis exacerbation where symptoms worsen and an infection is present.
34. What will spirometry results show in patients with bronchiectasis?
Decreased flow rates
35. What will the CBC results show in patients with bronchiectasis?
Increased RBC/Hb/Hct
36. What observation is seen in the sputum of patients with bronchiectasis?
It may indicate that an infection is present.
37. What does chronic dilation of the airways lead to?
It leads to chronic infections and inflammation.
38. What is the difference between COPD and bronchiectasis?
COPD is a progressive disease that causes airflow obstruction due to alveolar damage, while bronchiectasis specifically involves the abnormal widening of airways due to chronic infection and inflammation, not necessarily accompanied by the alveolar damage seen in COPD.
39. What are the five primary causes of bronchiectasis?
Idiopathic, congenital, post-infectious, immunodeficiency, and other causes.
40. What percentage of bronchiectasis is a result of idiopathic causes?
50%
41. What are four congenital causes of bronchiectasis?
Cystic fibrosis, primary ciliary dyskinesia, Kartagener’s syndrome, and Young’s syndrome.
42. What are five post-infectious causes of bronchiectasis?
Measles, pertussis, pneumonia, tuberculosis, and bronchiolitis.
43. What type of immunodeficiency is associated with bronchiectasis?
Hypogammaglobulinaemia
44. What is the typical history of a patient who presents with bronchiectasis?
Usually, there is a history of a chronic productive cough and recurrent chest infections.
45. What are the main symptoms associated with bronchiectasis?
Persistent cough with purulent sputum, hemoptysis, fever, weight loss, digital clubbing, coarse inspiratory crepitations, and wheezes.
46. What are the potential complications of bronchiectasis?
Pneumonia, pleural effusion, pneumothorax, pulmonary hypertension, massive hemoptysis, cerebral abscess, and amyloidosis.
47. What tests are performed in patients with suspected bronchiectasis?
Sputum, blood, spirometry, chest x-ray, high-resolution CT of the chest, bronchoscopy, and a sweat test for cystic fibrosis.
48. What specific blood tests are ordered for patients with bronchiectasis?
Serum immunoglobulin, aspergillus precipitins test, rheumatoid factor, α1-antitrypsin level, and assessment of Ig response to pneumococcal vaccine.
49. What pattern with spirometry show in a patient with bronchiectasis?
Obstructive patterns
50. What signs would you expect on the chest x-ray of a patient with bronchiectasis?
Dilated bronchi with thickened walls and multiple cysts containing fluid.
51. What test is the gold standard for diagnosing bronchiectasis?
HRCT of the chest
52. Why would you conduct a bronchoscopy in patients with suspected bronchiectasis?
To locate the site of hemoptysis, exclude obstruction, and obtain samples for culture.
53. What anatomic alterations are included in patients with bronchiectasis?
Hyperinflation and consolidation
54. What is a congenital cause of bronchiectasis?
Cystic fibrosis
55. What condition can occur in children if parents don’t give the usual childhood immunizations and the child has been repeatedly hospitalized with pulmonary infections?
Bronchiectasis.
56. What should be done to prevent bronchiectasis from worsening?
Avoid air pollution, get an influenza vaccination, and avoid smoking.
57. What other conditions are associated with severe bronchiectasis?
Cor pulmonale, distended neck veins, and polycythemia.
58. What will the hematology test results show in patients with bronchiectasis?
It will show an elevated WBC count with increased hemoglobin and hematocrit.
59. What are the hallmark symptoms of bronchiectasis?
Chronic cough with production of large quantities of foul-smelling sputum.
60. What is the usual characteristic of the sputum of patients with bronchiectasis?
It is usually voluminous and tends to settle into several different layers.
61. What signs do patients with severe bronchiectasis have?
Distended neck veins, pitting edema, and an enlarged and tender liver.
62. What lobe of the lung is bronchiectasis frequently found in?
The lower lobes
63. What part of the airway does bronchiectasis usually affect?
Smaller bronchi
64. What are the three forms of bronchiectasis?
Varicose, cylindrical, and cystic
65. What form of bronchiectasis has irregular dilations and constrictions and appears distorted and bulbous?
Varicose
66. What is the other name for varicose bronchiectasis?
Fusiform
67. What form of bronchiectasis has a tube-like dilation, where they lose their natural taper for 6-20 generations and appear to end squarely?
Cylindrical
68. What is the other name for cylindrical bronchiectasis?
Tubular
69. What is the other name for cystic bronchiectasis?
Saccular
70. What are two types of bronchiectasis?
Acquired and congenital
71. What are the two types of acquired bronchiectasis?
Pulmonary infection and bronchial obstruction
72. What kind of congenital bronchiectasis causes problems with mucus clearance and thick, stagnant secretions that leads to obstruction and frequent infections?
Cystic fibrosis
73. What happens to the fingers due to chronic hypoxemia?
Digital clubbing
74. What are the potential types of bacteria in bronchiectasis sputum?
Haemophilus influenzae, pseudomonas aeruginosa, and anaerobic organisms.
75. What type of disease is bronchiectasis?
Obstructive lung disease
76. What type of ventilatory acid-base assessment does a mild to moderate bronchiectasis have?
Acute alveolar hyperventilation with hypoxemia
77. What type of ventilatory acid-base assessment does a severe bronchiectasis have?
Chronic ventilatory failure with hypoxemia
78. What is performed by injecting an opaque contrast material into the airway to show the extent of the bronchiectasis disease?
Bronchogram, although this method is no longer used.
79. What type of bronchiectasis has increased opacity due to tissue density?
Restrictive
80. What type of bronchiectasis has translucent lung fields?
Obstructive
81. What is the classic pathophysiologic cycle that drives bronchiectasis progression?
The “vicious cycle” of impaired mucociliary clearance, infection, inflammation, and further airway damage.
82. What CT finding described as dilated bronchi larger than the accompanying pulmonary artery suggests bronchiectasis?
The “signet ring” sign.
83. What CT feature indicates lack of normal bronchial tapering in bronchiectasis?
Bronchi that fail to narrow as they travel toward the periphery.
84. What is a common CT finding when mucus fills dilated bronchi in bronchiectasis?
Mucoid impaction.
85. What is the “tree-in-bud” pattern on CT most consistent with in bronchiectasis patients?
Small-airway inflammation and endobronchial spread of infection.
86. What clinical finding often suggests chronic suppurative airway disease such as bronchiectasis?
Daily productive cough with large-volume sputum.
87. What sputum change most strongly suggests an acute infectious exacerbation of bronchiectasis?
An increase in sputum purulence and/or volume with worsening symptoms.
88. What is the most important first step before starting antibiotics for a bronchiectasis exacerbation when possible?
Obtain a sputum sample for Gram stain and culture.
89. What pathogen is strongly associated with more severe disease and worse outcomes in non-CF bronchiectasis?
Pseudomonas aeruginosa
90. What is the primary goal of airway clearance therapy in bronchiectasis?
To mobilize and remove secretions to reduce obstruction and infection risk.
91. What is postural drainage used for in bronchiectasis?
To use gravity-assisted positioning to help move secretions from affected lung segments.
92. What is active cycle of breathing technique (ACBT) used for in bronchiectasis?
A structured breathing routine to loosen, mobilize, and expectorate secretions.
93. Why should bronchodilator therapy be considered before airway clearance in some bronchiectasis patients?
To reduce bronchospasm and improve airflow for more effective secretion clearance.
94. What is hemoptysis?
Coughing up blood originating from the lower respiratory tract.
95. What bronchiectasis complication can present as life-threatening bleeding?
Massive hemoptysis
96. What is a key reason bronchoscopy may be performed in bronchiectasis?
To evaluate hemoptysis or rule out an obstructing lesion causing localized disease.
97. What baseline test helps assess airflow obstruction and monitor progression in bronchiectasis?
Spirometry
98. What ABG pattern may be seen during severe bronchiectasis with ventilatory failure?
Hypercapnia with respiratory acidosis and possible metabolic compensation.
99. What vaccination strategy is commonly recommended to reduce infectious triggers in bronchiectasis?
Annual influenza vaccination and pneumococcal vaccination as indicated.
100. What is a common indication for surgical resection in bronchiectasis?
Localized disease with recurrent infections or significant hemoptysis despite optimal medical therapy.
Final Thoughts
Bronchiectasis is a chronic condition defined by permanent airway dilation that disrupts mucus clearance and promotes recurrent infection and inflammation. Symptoms often include chronic productive cough, large volumes of purulent sputum, and intermittent hemoptysis, with disease severity ranging from mild to debilitating.
Diagnosis is confirmed by chest CT, and treatment typically combines antibiotics with structured airway clearance strategies and supportive therapies tailored to patient needs.
Respiratory therapists are central to bronchiectasis care through pulmonary function testing, acute respiratory support, airway clearance delivery, and patient education that improves long-term symptom control and reduces exacerbations.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Bird K, Memon J. Bronchiectasis. [Updated 2023 May 22]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025.

