Intubation is a medical procedure used to place a tube into the trachea to establish and maintain an open airway. In respiratory care, it is most often performed with an endotracheal tube inserted through the mouth or nose.
This allows oxygen delivery, ventilation, airway protection, and suctioning when a patient cannot maintain adequate breathing or airway control on their own.
Although intubation can be lifesaving, it also carries risks. Safe care requires proper preparation, correct tube placement, close monitoring, cuff management, and rapid recognition of complications.
What Is Intubation?
Intubation is the placement of an artificial airway, most commonly an endotracheal tube, into the trachea to establish or maintain an open airway. The tube may be inserted through the mouth, which is called orotracheal intubation, or through the nose, which is called nasotracheal intubation.
Once the tube is in the trachea, it provides a direct pathway between the outside environment and the lower airway. This allows clinicians to deliver oxygen, provide positive-pressure ventilation, remove secretions, protect the airway from aspiration, and connect the patient to a mechanical ventilator when needed.
Intubation is not simply the act of placing a tube. It is part of a larger airway-management process. The care team must decide whether intubation is needed, prepare the patient and equipment, perform or assist with the procedure, confirm placement, secure the tube, manage the cuff, provide humidification, suction when indicated, monitor for complications, and determine when the tube can be removed or replaced with a tracheostomy.
For respiratory therapists, understanding intubation is essential because artificial airways are closely connected to oxygen therapy, airway clearance, emergency care, trauma management, and mechanical ventilation.
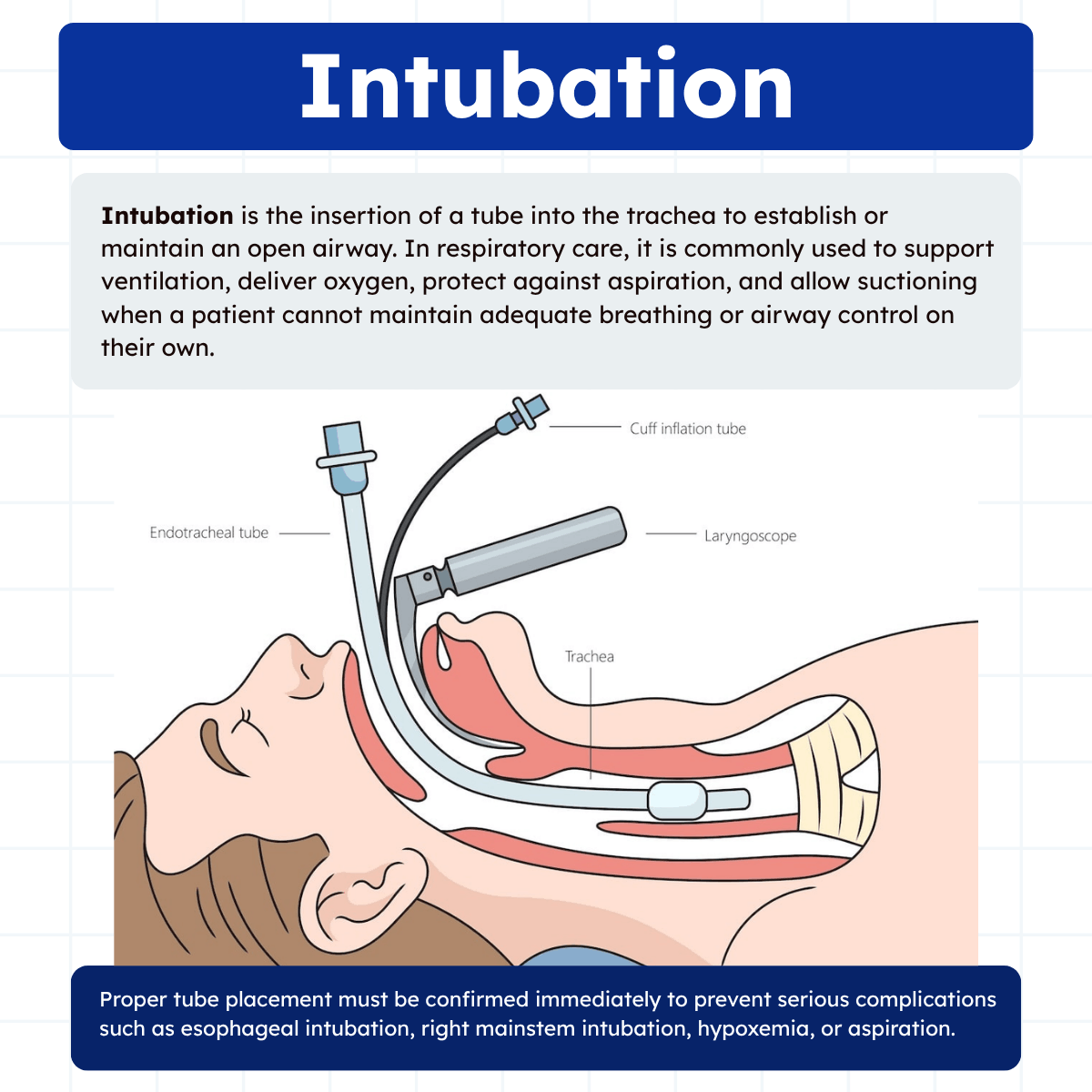
Purpose of Intubation
The main purpose of intubation is to establish a secure airway when a patient cannot maintain one independently. A patent airway is necessary for oxygen to enter the lungs and carbon dioxide to leave the body. When airway patency is threatened, the patient may quickly develop hypoxemia, hypercapnia, respiratory failure, cardiac arrest, or brain injury.
Intubation may be used to:
- Maintain airway patency
- Protect the lower airway from aspiration
- Provide invasive mechanical ventilation
- Support oxygenation and ventilation
- Allow suctioning of retained secretions
- Relieve or bypass airway obstruction
- Maintain airway control during general anesthesia
- Support patients with reduced consciousness or poor protective reflexes
For example, a patient with a drug overdose may lose the ability to breathe adequately or protect the airway. An oropharyngeal airway may help keep the tongue from obstructing the pharynx, but it does not protect against aspiration or provide a secure route for mechanical ventilation. In this situation, oral endotracheal intubation may be the fastest and safest method for airway control.
Similarly, a trauma patient with worsening respiratory failure may require intubation so oxygen and ventilatory support can be delivered immediately. A patient with severe neurologic injury may need intubation because loss of consciousness can impair airway protection and increase the risk of aspiration.
Types of Endotracheal Intubation
Endotracheal intubation is commonly classified by the route used to insert the tube. The two main routes are oral and nasal.
Orotracheal Intubation
Orotracheal intubation is the placement of an endotracheal tube through the mouth and into the trachea. This is the most common route in emergency and acute care because it is usually faster and easier than the nasal route.
Oral intubation is often preferred when rapid airway control is needed. It allows the clinician to visualize the vocal cords with a laryngoscope and pass the tube directly into the trachea. It also allows a larger tube to be used compared with nasal intubation, which can reduce airway resistance and make suctioning easier.
Common indications for oral intubation include respiratory failure, cardiac arrest, drug overdose, airway compromise, severe hypoxemia, and the need for invasive mechanical ventilation. It is also commonly used during general anesthesia.
However, oral intubation may not be appropriate in every situation. It may be difficult or unsafe in patients with severe lower facial trauma, recent oral surgery, limited mouth opening, or suspected cervical spine injury requiring strict immobilization. In these cases, special precautions, alternative devices, or another airway route may be needed.
Nasotracheal Intubation
Nasotracheal intubation is the placement of an endotracheal tube through the nose and into the trachea. It may be used when the oral route is unavailable, difficult, or contraindicated.
Nasal intubation may be considered in selected patients with oral trauma, mandibular injury, trismus, oral deformities, or oral surgery. It may also be better tolerated by some awake or semi-awake patients. However, nasal intubation usually requires a smaller tube, can be more difficult to perform, and may increase the risk of nasal bleeding, ulceration, and sinusitis.
Blind nasal intubation involves passing the tube through the nose and advancing it toward the larynx without direct visualization. Breath sounds through the tube may guide placement. As the tube approaches the larynx, sounds may become louder and more tubular. A cough with airflow through the tube may suggest tracheal entry, while loss of airflow may suggest esophageal direction. Even if clinical signs suggest tracheal placement, the tube must still be confirmed after insertion.
Direct-vision nasotracheal intubation uses laryngoscopy or another visualization device. Magill forceps may be used to guide the tube through the vocal cords. A hard stylet is not used for nasal intubation.
Indications for Intubation
The decision to intubate is based on the patient’s airway, breathing, oxygenation, ventilation, neurologic status, and overall clinical condition. Intubation is usually indicated when the patient cannot maintain a patent airway, cannot protect the airway, cannot oxygenate or ventilate adequately, or is likely to deteriorate without airway control.
Common indications include:
- Respiratory arrest
- Cardiac arrest
- Impending respiratory failure
- Severe hypoxemia
- Inadequate ventilation
- Airway obstruction
- Loss of airway protective reflexes
- Severe facial or airway trauma
- Burns or smoke inhalation affecting the airway
- Neuromuscular weakness
- Severe brain injury
- Drug overdose with ventilatory failure
- Need for invasive mechanical ventilation
- Need for frequent lower-airway suctioning
- General anesthesia
A patient with signs of impending respiratory failure should be evaluated quickly for intubation. Delaying airway control can lead to worsening hypoxemia, hypercapnia, acidosis, cardiac instability, or neurologic injury.
In trauma care, oxygen is often administered immediately to reduce the risk of secondary hypoxic injury. However, if the patient shows signs of pending respiratory failure, endotracheal intubation and mechanical ventilation may be required. The therapist must also assess for problems such as pneumothorax, airway injury, lung contusion, secretion retention, atelectasis, and acute respiratory distress syndrome.
Intubation and Neurologic Injury
Patients with altered mental status may need intubation because they cannot reliably protect the airway. Protective airway reflexes, such as coughing and swallowing, may be impaired. Secretions, vomitus, or blood may enter the lower airway and cause aspiration.
Traumatic brain injury is a high-risk situation. A patient with a low Glasgow Coma Scale score is at increased risk for airway compromise because of reduced consciousness, loss of muscle tone, seizures, or loss of protective reflexes. Patients with traumatic brain injury and a GCS score less than 8 commonly require endotracheal intubation to protect the airway and prevent hypoxia.
This is especially important because hypoxia can worsen secondary brain injury. The goal is not only to secure the airway but also to preserve oxygen delivery to the brain and prevent aspiration.
Cervical spine precautions may make intubation more difficult in trauma patients. If cervical spine injury is suspected, the neck should not be flexed or extended. During intubation, an assistant may need to maintain manual in-line stabilization while the anterior part of the cervical collar is opened. The goal is to limit cervical spine movement while still allowing airway access.
Contraindications and Special Concerns
In an emergency, intubation may be necessary to save life. However, clinicians must still consider contraindications and special risks.
A valid do-not-intubate order is an absolute contraindication. If the patient has a documented DNI order, intubation should not be performed. If no such order exists and the patient is in a life-threatening situation, emergency airway support should be initiated according to policy and scope of practice.
Relative contraindications or special concerns include:
- Severe facial trauma
- Severe airway trauma
- Upper-airway obstruction that prevents tube passage
- Recent oral surgery
- Cervical spine injury
- Limited mouth opening
- Airway burns or swelling
- Difficult airway anatomy
- Mallampati Class 4 airway
- Oral or mandibular injury
- Basilar skull fracture concerns with nasal insertion
Note: These conditions do not always prohibit intubation, but they may require alternative techniques, expert assistance, video laryngoscopy, fiberoptic intubation, supraglottic airway placement, or surgical airway access.
Difficult Airway Assessment
Before intubation, the airway should be assessed for signs that the procedure may be difficult. One common approach is the L-E-M-O-N mnemonic.
Look Externally
The clinician looks for external features that may predict difficulty. These include facial trauma, abnormal facial anatomy, obesity, large neck size, external masses, swelling, or neck trauma.
Evaluate Anatomy
The clinician evaluates mouth opening, mandible size, dental structure, and the position of the larynx relative to the tongue. A small mandible, poor mouth opening, or anterior larynx may make visualization harder.
Mallampati Classification
The Mallampati classification estimates intubation difficulty based on the structures visible when the patient opens the mouth and protrudes the tongue. Class I and II are usually easier. Class III suggests difficulty. Class IV suggests a very difficult airway.
A high Mallampati score does not automatically mean the patient cannot be intubated, but it warns the clinician to prepare for difficulty.
Obesity or Obstruction
Obesity, airway swelling, tumors, hematoma, trauma, edema, or foreign material may obstruct visualization or tube passage.
Neck Mobility
Reduced neck mobility can make alignment of the airway difficult. Causes include cervical spine injury, cervical collar use, rheumatoid arthritis, ankylosing spondylitis, degenerative joint disease, or trauma. If neck movement is unsafe, positioning must be modified.
Equipment Needed for Intubation
Proper preparation reduces delays and improves patient safety. The equipment should be gathered and checked before the procedure whenever possible.
Common equipment includes:
- Laryngoscope handle with working batteries
- Straight and curved laryngoscope blades
- Endotracheal tubes in appropriate sizes
- One tube one size larger and one size smaller, if time allows
- 10-mL syringe for cuff inflation
- Stylet for oral intubation when needed
- Water-soluble lubricant
- Suction equipment
- Sterile suction catheters
- Yankauer suction catheter
- Bag-valve-mask device
- Oxygen source
- Stethoscope
- CO₂ detector or capnography equipment
- Tape or commercial tube holder
- Bite block when needed
- Cuff pressure manometer
- Personal protective equipment
- Pulse oximeter
- Cardiac monitor when indicated
For nasal intubation, additional supplies may include nasal airway preparation, topical anesthetic or vasoconstrictor if used by protocol, and Magill forceps for direct-vision nasotracheal intubation.
A high-yield exam point is that Magill forceps are associated with nasal intubation, not routine emergency oral intubation. Essential equipment for emergency oral intubation includes the laryngoscope handle, blade, appropriate endotracheal tube, stylet when needed, and syringe for cuff inflation.
Tube Size Selection
Selecting the correct endotracheal tube size is important. Tube size is usually identified by internal diameter in millimeters.
The tube should be large enough to allow adequate airflow and suctioning, but not so large that it causes airway trauma. A larger tube generally provides lower resistance, easier suctioning, lower airway pressures, and better secretion removal. A tube that is too small may increase resistance, create excessive leaks, reduce delivered ventilation, and make suctioning more difficult. A tube that is too large may injure the airway.
Adult women commonly receive a 7.5- or 8.0-mm internal diameter tube, while large adult men may require a 9.0-mm tube. Pediatric and neonatal tubes are selected based on age, weight, and airway size. A premature neonate may require a 2.5-mm internal diameter tube.
When time permits, it is helpful to have one tube one size smaller and one tube one size larger available. The cuff should be tested before insertion by inflating it with air, confirming that it holds pressure, and then fully deflating it before placement.
Patient Preparation
Before intubation, the clinician should verify the order or protocol, review the medical record for contraindications, identify the patient when possible, use appropriate precautions, and perform a time-out when indicated.
The patient should be assessed for airway difficulty, oxygenation status, ventilation status, hemodynamic stability, and aspiration risk. Dentures or removable dental appliances should be removed. Suction should be working and immediately available because secretions, vomitus, blood, or foreign material can obstruct the view of the glottis.
Preoxygenation is one of the most important parts of preparation. Intubation attempts interrupt normal ventilation. Critically ill patients can desaturate rapidly during prolonged or repeated attempts. Preoxygenation with 100% oxygen increases the oxygen reserve and helps reduce the risk of severe desaturation.
If the patient is not breathing adequately, ventilation should be supported with a bag-valve-mask device and 100% oxygen before another intubation attempt is made. Oxygenation is always a priority. Repeated attempts at tube placement should not continue while the patient is becoming severely hypoxemic.
Positioning for Intubation
For routine oral intubation, the sniffing position is often used. This position helps align the oral, pharyngeal, and laryngeal axes to improve visualization of the vocal cords. It generally involves slight head extension and elevation or adjustment of the head and neck.
However, positioning must be adapted to the patient. If cervical spine injury is suspected, neck flexion and extension should be avoided. Manual in-line stabilization may be required. In obese patients or patients with limited neck mobility, ramping or special positioning may improve visualization and oxygenation.
Note: If the vocal cords are difficult to see, the clinician may adjust positioning, apply external laryngeal pressure, use a different laryngoscope blade, use video laryngoscopy, or use an introducer such as a gum elastic bougie.
Oral Intubation Procedure
The general sequence of oral endotracheal intubation includes preparation, preoxygenation, visualization, tube insertion, cuff inflation, ventilation, and confirmation.
The clinician first assembles and checks the equipment. The laryngoscope light should work, the tube cuff should hold air, suction should function, and oxygen should be available. The patient is positioned appropriately and ventilated with 100% oxygen when needed.
During direct laryngoscopy, the laryngoscope blade is inserted into the mouth and used to move the tongue and soft tissues. The clinician lifts upward and anteriorly to expose the airway structures. The epiglottis, larynx, and vocal cords are identified. The endotracheal tube is then passed through the vocal cords under direct vision.
For adults, the tube marking is often initially positioned around 21 to 23 cm at the lips or incisors, depending on patient size and institutional practice. The cuff is inflated, and ventilation begins. Placement must then be confirmed immediately.
Note: It is important not to use the teeth as a fulcrum when lifting the laryngoscope. Improper leverage can cause tooth trauma. Soft tissue injury can also occur if the blade is inserted or manipulated forcefully.
Nasal Intubation Procedure
Nasal intubation may be performed blindly or under direct vision. The more open nasal passage is selected when possible. The tube is lubricated with water-soluble lubricant and advanced gently through the nasal passage.
In blind nasal intubation, the clinician listens or feels for airflow through the tube. The tube is advanced during inspiration. Breath sounds may become louder as the tube approaches the larynx. A cough and airflow through the tube may suggest tracheal placement. If there is no airflow or no cough, esophageal placement may be suspected.
In direct-vision nasotracheal intubation, the clinician uses a laryngoscope or visualization device. Magill forceps may be used to guide the tube through the vocal cords. After the tube enters the trachea, the cuff is inflated, oxygen is applied, breath sounds are assessed, CO₂ detection is used when available, and a chest radiograph is obtained.
Note: Nasal intubation should be performed carefully because it can cause nasal trauma and bleeding. It is generally avoided when there is concern for severe nasal, midface, or skull-base injury.
Confirming Tube Placement
Tube placement must be confirmed immediately after insertion. Incorrect placement can be fatal if not recognized quickly.
Initial confirmation includes:
- Observing chest rise
- Listening over the epigastrium
- Auscultating both lungs
- Assessing oxygen saturation
- Checking for airflow through the tube
- Looking for condensation in the tube
- Using exhaled CO₂ detection
- Confirming final position with chest radiography
A common sequence is to deliver a breath and listen over the epigastric area first. If air is heard over the stomach, esophageal intubation is likely, and the tube should be removed. If epigastric sounds are absent, the clinician auscultates the lungs for equal bilateral breath sounds, including apical and lateral areas.
Exhaled carbon dioxide detection is a standard method for confirming tracheal placement. A colorimetric CO₂ detector changes color when exhaled CO₂ is present. Capnography provides continuous monitoring and is especially useful after intubation. If the tube is in the trachea and the patient has adequate pulmonary blood flow, exhaled CO₂ should be detected.
However, CO₂ detection is not perfect. During cardiac arrest, low pulmonary blood flow may cause little or no exhaled CO₂ even if the tube is correctly placed. Also, CO₂ detection cannot confirm that the tube is at the ideal depth. A tube in the right mainstem bronchus may still produce exhaled CO₂.
A chest radiograph is used to confirm final tube position. In adults, the tip of the endotracheal tube should be positioned above the carina, commonly around 1.5 inches above the carina with the head in a neutral position. The chest x-ray helps determine whether the tube is too high, too low, or advanced into a mainstem bronchus.
Esophageal Intubation
Esophageal intubation occurs when the tube enters the esophagus instead of the trachea. This is a dangerous complication because ventilation will go into the stomach rather than the lungs.
Signs of esophageal intubation include:
- Poor or absent chest rise
- Air heard over the epigastrium
- Absent or poor breath sounds
- Stomach distention
- Falling oxygen saturation
- Cyanosis
- Worsening vital signs
- No sustained exhaled CO₂
- Aspiration or vomiting
If esophageal intubation is suspected, the cuff should be deflated, the tube removed, and the patient ventilated with 100% oxygen using a bag-valve-mask device. Reintubation should be attempted when the patient is adequately oxygenated and the appropriate clinician is ready.
Direct visualization of the tube passing through the vocal cords helps prevent esophageal intubation. If the vocal cords cannot be seen or the tube path cannot be confirmed, the clinician should avoid blindly forcing the tube and should consider another approach or another experienced provider.
Right Mainstem Intubation
If the endotracheal tube is advanced too far, it may enter a mainstem bronchus. This most often occurs on the right side because the right mainstem bronchus is wider, shorter, and more vertical than the left.
Right mainstem intubation may cause the right lung to receive most or all of the ventilation while the left lung is poorly ventilated. This can lead to unequal chest movement, absent or diminished left-sided breath sounds, atelectasis, hypoxemia, and increased airway pressures.
A key sign after recent intubation is absent or decreased breath sounds on the left with stronger breath sounds on the right. Exhaled CO₂ may still be present because the tube is in the airway, so CO₂ detection alone cannot rule out mainstem intubation.
Note: The corrective action is to withdraw the tube gradually until bilateral breath sounds are present, then reassess oxygenation, ventilation, cuff pressure, tube depth, and chest radiograph findings.
Securing the Tube
After placement is confirmed, the tube must be secured. Accidental extubation or tube movement can cause serious complications. Tube depth should be recorded using the centimeter marking at the lips, teeth, or nares, depending on the route.
A commercial tube holder or approved taping method may be used. The securing method should prevent movement but avoid excessive pressure on the lips, face, or skin. The patient should be reassessed after the tube is secured because the tube can shift during fixation.
Tube position should be monitored regularly. Head and neck movement can change the tube tip location. Neck flexion may advance the tube deeper, while neck extension may withdraw the tube. This is especially important in infants and small children, where small movements can cause accidental extubation or bronchial intubation.
Cuff Management
Many endotracheal tubes used in adults have cuffs. The cuff is inflated inside the trachea to create a seal around the tube. This seal helps deliver positive-pressure ventilation and reduces leakage around the tube. It may also reduce aspiration of secretions from above the cuff, although it does not eliminate aspiration risk.
Cuff pressure must be carefully controlled. If pressure is too low, air can leak around the tube, delivered ventilation may decrease, and secretions may pass into the lower airway. If pressure is too high, blood flow to the tracheal mucosa may be impaired.
A commonly accepted safe range is approximately 20 to 30 cm H₂O, which is about 15 to 22 mm Hg. Pressures should generally remain below tracheal mucosal capillary perfusion pressure. Excessive pressure can cause ischemia and tissue injury.
Note: If an adequate seal cannot be achieved without excessive cuff pressure, the tube may be too small or malpositioned. The correct response is not to keep adding air indefinitely. The tube may need to be repositioned or replaced with a more appropriate size.
Complications of High Cuff Pressure
High cuff pressure can create excessive lateral pressure against the tracheal wall. Over time, this may impair mucosal blood flow and cause injury.
Possible complications include:
- Mucosal ischemia
- Inflammation
- Ulceration
- Necrosis
- Tracheal stenosis
- Tracheomalacia
- Tracheal dilation
- Tracheoesophageal fistula
- Tracheovascular fistula
- Cartilage damage
These complications are more likely with prolonged intubation, poor cuff monitoring, tube movement, and excessive pressure. Tracheoesophageal fistula is not usually an immediate complication of intubation. It is more often associated with high cuff pressure over several days.
Regular cuff pressure monitoring helps reduce these risks. Respiratory therapists play an important role in measuring cuff pressure, identifying leaks, recommending appropriate interventions, and documenting findings.
Intubation and Mechanical Ventilation
Endotracheal intubation is closely connected with invasive mechanical ventilation. A ventilator needs a secure airway interface to deliver positive-pressure breaths into the lungs. For short-term invasive ventilation, this is commonly achieved through an endotracheal tube.
The tube allows the ventilator to deliver oxygen and gas flow directly into the trachea. It also allows clinicians to monitor airway pressures, suction secretions, apply positive end-expiratory pressure, and support patients with respiratory failure.
However, invasive ventilation through an endotracheal tube increases the risk of complications. The tube bypasses normal upper-airway defenses, interferes with cough, impairs normal humidification, and provides a route for microorganisms to enter the lower airway.
One important complication is ventilator-associated pneumonia. VAP may occur when microorganisms from the mouth, pharynx, or stomach enter the lower airway. Intubated patients are at increased risk because secretions can collect above the cuff and may leak around it. Oral care, head-of-bed elevation when appropriate, cuff pressure management, suctioning, sedation management, and readiness-to-extubate assessment are all part of reducing risk.
Because of these risks, noninvasive ventilation may be used when appropriate to avoid intubation. However, noninvasive ventilation is not suitable for every patient. Patients who cannot protect the airway, have severe aspiration risk, have major facial trauma, are unable to clear secretions, or are deteriorating despite noninvasive support may require intubation.
Rapid Sequence Intubation
Rapid sequence intubation (RSI) is a method used to gain airway control quickly in selected patients. It is often used when a patient needs urgent intubation and has a high risk of aspiration, such as a conscious patient who has not fasted.
RSI typically involves preoxygenation, administration of a sedative, administration of a paralytic, and rapid placement of the endotracheal tube. Common medications may include a short-acting sedative such as etomidate and a paralytic such as succinylcholine or rocuronium.
The goal is to rapidly render the patient unconscious, relax the muscles, improve intubating conditions, reduce airway reflexes, and minimize the need for manual ventilation that could insufflate the stomach. Cricoid pressure, also known as Sellick’s maneuver, may be used in some settings to compress the esophagus and reduce aspiration risk, although excessive pressure can obstruct the airway or worsen visualization.
RSI requires careful preparation. The team should have oxygen, suction, a bag-valve-mask device, intubation equipment, monitoring devices, intravenous access, emergency medications, and a backup airway plan. A cricothyrotomy tray or emergency airway equipment should be available in case intubation fails.
Note: RSI should not be attempted by a provider unfamiliar with the procedure, equipment, or medications. It is also not generally intended for unconscious crash-airway patients who require immediate ventilation and intubation without induction and paralysis.
Medications and Paralytics
Medications may be used before or during intubation to improve comfort, reduce airway reflexes, provide sedation, and improve intubating conditions.
Sedatives may include medications such as midazolam or etomidate, depending on the clinical situation and institutional practice. Analgesics may be needed when pain is present. Paralytics may be used during RSI, for ventilator synchrony, control-mode ventilation, reduction of oxygen consumption, or management of increased intracranial pressure in selected cases.
A critical point is that paralytics do not provide sedation, pain relief, or amnesia. A paralyzed patient may still be awake or in pain if sedation and analgesia are not provided. Therefore, paralytics should be used only when full ventilatory support is available and appropriate sedation and analgesia are addressed.
Note: Ventilator disconnect alarms and monitoring must be properly set because a paralyzed patient cannot breathe effectively or alert staff if disconnected.
Difficult Intubation Management
Difficult intubation requires a structured approach. The priority is always oxygenation. Repeated attempts at tube placement should not continue while the patient becomes severely hypoxemic.
Possible strategies for difficult intubation include:
- Repositioning the head and neck when safe
- Maintaining cervical spine precautions when needed
- Applying external laryngeal pressure
- Using a different laryngoscope blade
- Using a longer or shorter blade
- Using a gum elastic bougie
- Using a lighted stylet
- Using video-assisted laryngoscopy
- Using fiberoptic-guided intubation
- Using an intubating laryngeal mask airway
- Requesting the most experienced clinician
- Considering RSI when appropriate
- Moving to a supraglottic airway if intubation fails
- Performing emergency percutaneous airway access if oxygenation cannot be maintained
If the patient cannot be intubated but can still be ventilated with a bag-valve-mask device and oxygen saturation remains acceptable, additional attempts may be made by the most experienced clinician with improved technique or equipment.
If the patient cannot be intubated and cannot be oxygenated, a supraglottic airway should be placed immediately. If that fails, an emergency surgical or percutaneous airway may be required.
Alternative Airway Devices
Although endotracheal intubation is often the most secure airway method, alternative airway devices may be used in certain situations.
A laryngeal mask airway (LMA) may help maintain a patent airway when endotracheal intubation is not possible or when the neck cannot be hyperextended. It is often easier and faster to place than an endotracheal tube. However, it does not protect against aspiration as reliably as an endotracheal tube and may leak when ventilation pressures are high.
A Combitube may be used in emergency airway situations when endotracheal intubation is unsuccessful or when personnel are not trained to intubate. It is designed to provide ventilation whether it enters the trachea or esophagus. However, it also has limitations and does not replace the need to understand endotracheal intubation.
A tracheostomy tube is used for long-term airway support or when upper-airway obstruction, prolonged ventilation, or secretion management requires a more stable airway. In some cases, a surgical airway may be necessary when oral or nasal intubation fails or is impossible.
Tracheostomy After Prolonged Intubation
Prolonged endotracheal intubation can cause discomfort, airway injury, difficulty with oral care, increased sedation needs, and impaired secretion clearance. When a patient continues to need an artificial airway after approximately 7 to 14 days of oral or nasal intubation, tracheostomy is commonly considered.
A tracheotomy is the surgical procedure that creates an opening into the trachea through the neck. The opening is called a tracheostomy. A tracheostomy tube is then inserted to maintain airway access.
Potential benefits of tracheostomy include:
- Improved patient comfort
- Reduced need for sedation
- Easier secretion removal
- Lower airway resistance compared with some endotracheal tubes
- Better oral care
- Reduced risk of vocal cord injury
- Improved ability to wean from ventilation in selected patients
- More stable long-term airway access
Note: A tracheostomy does not eliminate all risks. It requires ongoing care, suctioning, humidification, tube security, stoma care, and monitoring for complications. However, it may be more appropriate than prolonged oral or nasal intubation in patients who need extended airway support.
Pediatric and Neonatal Intubation
Intubation in infants and children requires special care because the pediatric airway is smaller, more delicate, and more easily obstructed. Equipment must be selected based on age, weight, and airway size. Small changes in tube position can have major effects.
A tube that is too small may leak, increase resistance, and reduce delivered minute ventilation. A tube that is too large may injure the airway. Pediatric tubes may be cuffed or uncuffed depending on patient age, size, clinical situation, and institutional practice.
Infant endotracheal tubes are easily kinked or obstructed. Secretions can block the lumen quickly because the tube diameter is small. The tube must be secured immediately after placement and checked frequently.
Head position is especially important. In infants and small children, slight movement of the head can move the tube tip significantly. Flexion may advance the tube into a bronchus, while extension may pull it upward and increase the risk of extubation.
Breath sounds may not reliably identify tube position in infants and small children. Chest radiography and end-tidal CO₂ monitoring may be needed to confirm and monitor placement.
Possible pediatric complications include:
- Accidental extubation
- Tube obstruction
- Palatal grooving
- Enamel hypoplasia in neonates
- Tracheal stenosis
- Esophageal perforation
- Tracheal perforation
- Airway trauma
- Increased work of breathing from a small tube
Note: Because of these risks, pediatric intubation requires close monitoring and careful tube management after insertion.
Complications During Intubation
Complications can occur during the intubation procedure itself. Some complications are caused by the laryngoscope or tube, while others are caused by hypoxemia, airway stimulation, aspiration, or incorrect placement.
Possible complications during intubation include:
- Esophageal intubation
- Mainstem bronchus intubation
- Hypoxemia from prolonged attempts
- Vomiting and aspiration
- Tooth trauma
- Soft tissue injury
- Pharyngeal or laryngeal laceration
- Vocal cord injury
- Reflex laryngospasm
- Bronchospasm
- Bradycardia from vagal stimulation
- Tachycardia or dysrhythmias from hypoxemia
- Hypotension
- Aspiration of a tooth, blood, gastric contents, or equipment fragment
- Perforation of the esophagus or pharynx
- Cervical spine injury if precautions are not followed
- Eye trauma from the handle or operator’s hand
Note: Monitoring during the procedure is essential. Oxygen saturation, heart rhythm, blood pressure, chest movement, and clinical response should be observed closely. Failed attempts should be interrupted by bag-valve-mask ventilation with 100% oxygen.
Complications While Intubated
After the tube is in place, complications may continue to occur. Artificial airways bypass natural defenses and can cause local tissue injury, infection, obstruction, or displacement.
Possible complications while intubated include:
- Tube obstruction from secretions
- Kinking of the tube
- Mucus plugging
- Accidental extubation
- Tube migration
- Mainstem bronchus intubation
- Atelectasis
- Aspiration
- Ventilator-associated pneumonia
- Sinusitis with nasal tubes
- Pressure sores on lips, nose, or face
- Laryngeal injury
- Tracheal mucosal injury
- Excessive cuff pressure
- Air leak from low cuff pressure
- Increased airway resistance
- Patient discomfort or agitation
Routine assessment is necessary. The therapist should monitor tube depth, breath sounds, chest movement, oxygen saturation, ventilator pressures, exhaled tidal volume, cuff pressure, secretion characteristics, and patient comfort.
Humidification is also important because the endotracheal tube bypasses the upper airway, which normally warms and humidifies inspired gas. Without adequate humidification, secretions can become thick and difficult to remove, increasing the risk of tube obstruction.
Complications After Extubation
Complications may also occur after the tube is removed. The airway may be irritated, swollen, injured, or partially obstructed.
Possible post-extubation complications include:
- Hoarseness
- Sore throat
- Laryngospasm
- Aspiration
- Laryngeal edema
- Subglottic edema
- Stridor
- Vocal cord injury
- Tracheal inflammation
- Tracheal stenosis
- Vocal cord paralysis
- Mucosal injury
- Respiratory distress requiring reintubation
Note: Patients should be monitored closely after extubation for signs of airway obstruction, increased work of breathing, oxygen desaturation, weak cough, secretion retention, and altered mental status.
The Respiratory Therapist’s Role in Intubation
Respiratory therapists are deeply involved in intubation care, even when the procedure itself is performed by another provider. Their responsibilities may vary by state law, facility policy, credentialing, and scope of practice.
The therapist’s role may include:
- Recognizing indications for intubation
- Assessing oxygenation and ventilation
- Preparing equipment
- Checking laryngoscope function
- Testing the cuff
- Preparing suction
- Preoxygenating the patient
- Assisting with positioning
- Ventilating with a bag-valve-mask device
- Monitoring oxygen saturation and heart rhythm
- Assisting with tube placement
- Inflating the cuff
- Confirming placement with breath sounds and CO₂ detection
- Securing the tube
- Measuring cuff pressure
- Setting up mechanical ventilation
- Providing humidification
- Suctioning when indicated
- Monitoring for complications
- Recommending tube repositioning when needed
- Assisting with extubation readiness assessment
- Documenting the procedure and patient response
Note: A respiratory therapist must also recognize when intubation is difficult or unsafe and help move the team toward appropriate alternatives. This may include video laryngoscopy, supraglottic airway placement, or emergency airway access.
Documentation After Intubation
Accurate documentation is part of safe airway care. After intubation, documentation should include relevant details about the procedure and the patient’s response.
Important items may include:
- Indication for intubation
- Route of intubation
- Tube size
- Tube depth at the teeth, lips, or nares
- Cuff pressure
- Placement confirmation methods
- Breath sound findings
- Exhaled CO₂ findings
- Chest x-ray confirmation
- Oxygen saturation before and after intubation
- Ventilator settings if initiated
- Patient tolerance
- Complications or adverse events
- Interventions performed
- Name or role of the clinician who placed the tube
Note: Clear documentation helps the care team track tube position, cuff pressure, ventilator support, and changes in patient status.
Key Exam Points About Intubation
For respiratory therapy exams, intubation questions often focus on indications, contraindications, equipment, confirmation, complications, and troubleshooting.
Important points include:
- Oral intubation is usually the fastest and easiest route in emergencies
- A valid DNI order is an absolute contraindication
- Cervical spine injury requires special precautions and avoidance of routine neck hyperextension
- Magill forceps are used for nasal intubation, not routine oral intubation
- The cuff should be tested before insertion
- The patient should be preoxygenated before attempts
- Failed attempts should be interrupted by ventilation with 100% oxygen
- Placement must be confirmed immediately
- Listen over the epigastrium to help identify esophageal placement
- Equal bilateral breath sounds help assess tracheal position
- Exhaled CO₂ helps confirm airway placement
- CO₂ detection does not rule out right mainstem bronchus intubation
- Chest x-ray confirms final tube depth
- Absent left breath sounds after intubation suggest right mainstem placement
- Correct right mainstem placement by withdrawing the tube and reassessing
- Safe cuff pressure is generally around 20 to 30 cm H₂O
- Excessive cuff pressure can cause tracheal injury
- Paralytics do not provide sedation or analgesia
- Oxygenation takes priority over repeated intubation attempts
- Tracheostomy is often considered when long-term artificial airway support is needed
Intubation Practice Questions
1. What is endotracheal intubation?
Endotracheal intubation is the insertion of an endotracheal tube through the mouth or nose into the trachea to secure the airway, protect against aspiration, and provide access for ventilation and oxygenation.
2. What is the primary goal of endotracheal intubation?
The primary goal is to establish and maintain a patent airway so the patient can be effectively oxygenated and ventilated.
3. What are common indications for intubation?
Common indications include airway obstruction, respiratory failure, apnea, severe hypoxemia, inability to protect the airway, altered mental status, aspiration risk, trauma, upper airway edema, and the need for mechanical ventilation.
4. What is an artificial airway?
An artificial airway is a tube or device inserted to maintain airway patency and support ventilation.
5. What are the main types of artificial airways?
The main types include endotracheal tubes, tracheostomy tubes, oropharyngeal airways, nasopharyngeal airways, and supraglottic airways.
Access our quiz, which includes sample TMC practice questions and detailed explanations to help you master the key concepts of airway management.
6. What are the two main routes for endotracheal intubation?
The two main routes are orotracheal intubation and nasotracheal intubation.
7. What is orotracheal intubation?
Orotracheal intubation is the placement of an endotracheal tube through the mouth and into the trachea.
8. What is nasotracheal intubation?
Nasotracheal intubation is the placement of an endotracheal tube through the nose, past the pharynx and vocal cords, and into the trachea.
9. What is the most important step immediately after intubation?
The most important step is to confirm that the endotracheal tube is in the trachea and not the esophagus.
10. What are common methods for confirming endotracheal tube placement?
Common methods include continuous waveform capnography, colorimetric CO2 detection, bilateral chest rise, bilateral breath sounds, absence of gastric sounds, direct visualization, and chest x-ray confirmation.
11. What is the best bedside method for confirming tracheal tube placement?
Continuous waveform capnography is the best bedside method for confirming tracheal placement when perfusion is adequate.
12. Why is a chest x-ray obtained after intubation?
A chest x-ray is obtained to confirm the depth of the endotracheal tube and ensure the tip is properly positioned above the carina.
13. Where should the endotracheal tube tip be positioned on chest x-ray?
The endotracheal tube tip should generally be positioned about 2 to 6 cm above the carina.
14. What happens if the endotracheal tube is inserted too deeply?
The tube may enter the right mainstem bronchus, causing ventilation of one lung, hypoxemia, atelectasis, and unequal breath sounds.
15. What are signs of right mainstem intubation?
Signs include decreased or absent breath sounds on the left side, asymmetric chest expansion, hypoxemia, and a tube tip that appears too low on chest x-ray.
16. What are signs of esophageal intubation?
Signs include absent breath sounds, gastric insufflation sounds, no sustained exhaled CO2, poor chest rise, worsening hypoxemia, and failure to improve ventilation.
17. What does a yellow color on a colorimetric CO2 detector usually indicate?
A yellow color usually indicates the presence of exhaled carbon dioxide, suggesting the tube is in the trachea.
18. What does a purple color on a colorimetric CO2 detector suggest?
A purple color suggests little or no exhaled carbon dioxide and may indicate esophageal intubation, poor perfusion, cardiac arrest, or equipment malfunction.
19. Why is colorimetric CO2 detection less reliable during cardiac arrest?
It may be less reliable because low pulmonary blood flow can reduce carbon dioxide delivery to the lungs, resulting in little or no detectable exhaled CO2.
20. What is preoxygenation?
Preoxygenation is the administration of high-concentration oxygen before intubation to increase oxygen reserves and reduce the risk of hypoxemia during the procedure.
21. Why is preoxygenation important before intubation?
Preoxygenation increases the oxygen stored in the lungs and blood, giving the clinician more time to secure the airway before oxygen saturation falls.
22. What equipment should be prepared before intubation?
Equipment includes oxygen source, suction, bag-valve-mask, oral and nasal airways, laryngoscope handle and blades, endotracheal tubes, stylet, syringe, tube-securing device, stethoscope, capnography device, and backup airway equipment.
23. What is the purpose of suction during intubation?
Suction clears secretions, blood, vomit, or debris from the airway to improve visualization and reduce aspiration risk.
24. What should be done if secretions obscure the airway during intubation?
The airway should be suctioned immediately, and the attempt should be paused if oxygenation or visualization becomes unsafe.
25. What is a bag-valve-mask device?
A bag-valve-mask device is a manual resuscitation device used to provide positive-pressure ventilation with room air or supplemental oxygen.
26. What are the essential parts of a bag-valve-mask device?
Essential parts include a self-inflating bag, one-way valve, face mask, oxygen inlet, and oxygen reservoir when high FiO2 is needed.
27. What can be done if the chest does not rise during bag-valve-mask ventilation?
Reposition the head and airway, improve the mask seal, lift the jaw, suction the airway, insert an airway adjunct, increase ventilation technique effectiveness, and consider advanced airway placement if needed.
28. What are disadvantages of bag-valve-mask ventilation?
Disadvantages include difficulty maintaining a mask seal, gastric insufflation, aspiration risk, and variable tidal volume delivery.
29. What is the head tilt-chin lift maneuver?
The head tilt-chin lift maneuver opens the airway by extending the head and lifting the chin in patients without suspected cervical spine injury.
30. When is the head tilt-chin lift maneuver contraindicated?
It is contraindicated when cervical spine injury is suspected.
31. What is the jaw thrust maneuver?
The jaw thrust maneuver opens the airway by lifting the mandible forward without extending the neck.
32. When is the jaw thrust maneuver preferred?
It is preferred when cervical spine injury is suspected.
33. What are the two common laryngoscope blade types?
The two common types are the Miller blade and the Macintosh blade.
34. What is a Miller blade?
The Miller blade is a straight laryngoscope blade used to directly lift the epiglottis.
35. What is a Macintosh blade?
The Macintosh blade is a curved laryngoscope blade placed in the vallecula to indirectly lift the epiglottis.
36. Which blade directly lifts the epiglottis?
The Miller blade directly lifts the epiglottis.
37. Which blade indirectly lifts the epiglottis?
The Macintosh blade indirectly lifts the epiglottis by lifting from the vallecula.
38. What laryngoscope blade sizes are commonly used for adults?
Adults commonly require a size 3 or 4 Macintosh blade or a size 2 or 3 Miller blade, depending on anatomy and clinician preference.
39. What laryngoscope blade sizes are commonly used for infants?
Infants commonly require size 0 or 1 blades, depending on size and gestational age.
40. What is video laryngoscopy?
Video laryngoscopy uses a camera-equipped laryngoscope to visualize the airway on a screen during intubation.
41. What is Glidescope intubation?
Glidescope intubation uses a video laryngoscope to improve visualization of the vocal cords during endotracheal tube placement.
42. What is a fiberoptic bronchoscope used for during intubation?
A fiberoptic bronchoscope can help guide the endotracheal tube through a difficult airway under direct visualization.
43. What is a stylet?
A stylet is a malleable device placed inside the endotracheal tube to give it shape and rigidity during insertion.
44. What is the purpose of the stylet during intubation?
The stylet helps guide the tube through the vocal cords, especially when a curved shape is needed for placement.
45. What must be done after the tube is inserted when a stylet is used?
The stylet must be removed before ventilation is started through the endotracheal tube.
46. What is the 15 mm adapter on an endotracheal tube?
The 15 mm adapter connects the endotracheal tube to standard equipment such as a bag-valve-mask or ventilator circuit.
47. What is the cuff on an endotracheal tube?
The cuff is an inflatable balloon near the distal end of the tube that creates a seal within the trachea.
48. What is the purpose of the endotracheal tube cuff?
The cuff helps allow positive-pressure ventilation, reduce air leaks, and decrease the risk of aspiration of secretions.
49. What is the pilot balloon?
The pilot balloon is connected to the cuff and indicates cuff inflation while allowing cuff pressure to be checked or adjusted.
50. What is the recommended endotracheal tube cuff pressure range?
The recommended cuff pressure is commonly 20 to 30 cmH2O, or approximately 15 to 22 mmHg.
Take our free course to master the basics of mechanical ventilation with clear explanations and helpful practice questions.
51. What can happen if cuff pressure is too high?
Excessive cuff pressure can reduce tracheal mucosal blood flow and cause ischemia, ulceration, pressure injury, or tracheal stenosis.
52. What can happen if cuff pressure is too low?
Low cuff pressure can cause an air leak, poor ventilation, and increased risk of aspiration around the cuff.
53. What is the Murphy eye?
The Murphy eye is a side opening near the tip of the endotracheal tube that allows airflow if the main opening becomes obstructed.
54. What is the purpose of the radiopaque line on an endotracheal tube?
The radiopaque line makes the tube visible on a chest x-ray to help confirm tube position.
55. What is the purpose of centimeter markings on an endotracheal tube?
Centimeter markings help estimate insertion depth and monitor whether the tube has moved after placement.
56. What is the vocal cord marking on an endotracheal tube?
The vocal cord marking helps guide insertion depth by showing when the tube has passed the vocal cords.
57. What endotracheal tube size is commonly used for adult males?
Adult males commonly require an internal diameter of about 7.5 to 9.0 mm, with 8.0 mm often used.
58. What endotracheal tube size is commonly used for adult females?
Adult females commonly require an internal diameter of about 7.0 to 8.0 mm, with 7.5 mm often used.
59. How is endotracheal tube size selected for neonates?
For neonates, tube size is selected based on weight, gestational age, and institutional guidelines for neonatal mechanical ventilation.
60. What is a typical endotracheal tube depth for adult males?
A typical depth is about 21 to 23 cm at the teeth or lip, but placement must be confirmed clinically and radiographically.
61. What is a typical endotracheal tube depth for adult females?
A typical depth is about 19 to 21 cm at the teeth or lip, but placement must be confirmed clinically and radiographically.
62. What does it mean if breath sounds are louder over the stomach than the chest after intubation?
It may indicate esophageal intubation, and the tube position must be reassessed immediately.
63. What should be done if esophageal intubation is suspected?
The tube should be removed, the patient should be ventilated with a bag-valve-mask and oxygen, and another airway attempt should be made when appropriate.
64. What is a difficult airway?
A difficult airway is a situation in which airway management is challenging due to anatomy, obstruction, trauma, edema, limited mouth opening, or poor visualization.
65. What factors may predict a difficult airway?
Factors include obesity, facial trauma, small mandible, limited neck mobility, limited mouth opening, airway swelling, blood or secretions, and abnormal airway anatomy.
66. What is rapid sequence intubation?
Rapid sequence intubation is a technique that uses rapid administration of sedative and paralytic medications to facilitate intubation while reducing aspiration risk.
67. Why is rapid sequence intubation used?
It improves intubating conditions, reduces airway reflexes, decreases patient discomfort, and helps lower the risk of aspiration in selected patients.
68. What should be monitored during rapid sequence intubation?
Heart rate, rhythm, blood pressure, oxygen saturation, respiratory effort, skin color, level of consciousness, and end-tidal CO2 should be monitored.
69. What can happen if sedation is inadequate during intubation?
Inadequate sedation can cause distress, coughing, gagging, hypertension, tachycardia, aspiration, airway trauma, and poor procedural conditions.
70. What can happen if sedation is excessive?
Excessive sedation can cause hypotension, hypoventilation, apnea, loss of airway reflexes, and cardiovascular instability.
71. What are common opioid analgesics used around intubation?
Common opioid analgesics include fentanyl and morphine.
72. What is naloxone?
Naloxone, also known as Narcan, is an opioid reversal agent.
73. What is midazolam?
Midazolam, also known as Versed, is a sedative-hypnotic medication used to reduce anxiety, provide sedation, and cause amnesia.
74. What is local anesthesia during intubation?
Local anesthesia numbs a specific area of the airway to reduce discomfort, coughing, gagging, and airway reflexes.
75. Why may lidocaine be used during airway management?
Lidocaine may be used to numb airway structures and reduce airway reflexes, coughing, or laryngospasm in selected situations.
76. What are contraindications to nasotracheal intubation?
Contraindications include suspected basilar skull fracture, severe facial trauma, nasal fracture, significant epistaxis, nasal obstruction, and some bleeding disorders.
77. What are complications of nasotracheal intubation?
Complications include epistaxis, turbinate trauma, sinusitis, submucosal dissection, bacteremia, and airway bleeding.
78. During which phase of breathing are the vocal cords most open?
The vocal cords are generally most open during inspiration.
79. How can oxygen be provided during nasotracheal intubation?
Oxygen can be provided with a nasal cannula in the opposite nare, a mask over the mouth, or oxygen tubing directed near the mouth while the procedure is performed.
80. What may help if a nasotracheal tube is difficult to advance into the trachea?
Helpful techniques may include repositioning the head and neck, rotating the tube, applying external laryngeal manipulation, using Magill forceps, or using fiberoptic guidance.
81. What is Magill forceps used for?
Magill forceps may be used to guide the endotracheal tube through the vocal cords during nasotracheal intubation.
82. What is cricoid pressure?
Cricoid pressure is pressure applied over the cricoid cartilage with the intent of reducing passive regurgitation during airway management.
83. What is external laryngeal manipulation?
External laryngeal manipulation is the manual adjustment of the larynx from outside the neck to improve visualization of the vocal cords.
84. How long should an intubation attempt last?
An intubation attempt should be limited to the shortest safe time possible and stopped if oxygen saturation falls or the patient becomes unstable.
85. What are common errors during intubation?
Common errors include poor positioning, inadequate preoxygenation, poor suctioning, wrong blade or tube size, dental trauma, esophageal intubation, right mainstem intubation, and failure to confirm placement.
86. What complications can occur during intubation?
Complications include hypoxemia, aspiration, airway trauma, dental injury, bleeding, laryngospasm, bronchospasm, esophageal intubation, right mainstem intubation, hypotension, and cardiac arrest.
87. What can happen after accidental extubation?
Accidental extubation can cause airway obstruction, laryngeal edema, hypoxemia, aspiration, bradycardia, hypotension, and the need for urgent reintubation.
88. What is stridor after extubation?
Stridor is a high-pitched sound caused by upper airway narrowing, often due to laryngeal or subglottic swelling after extubation.
89. Why can stridor occur after self-extubation?
Stridor may occur because the tube and cuff can traumatize the airway during accidental removal, causing swelling and narrowing.
90. What is the treatment for moderate to severe post-extubation stridor?
Treatment may include oxygen, close monitoring, nebulized racemic epinephrine, corticosteroids, heliox in selected cases, and reintubation if airway obstruction is severe.
Access our quiz, which includes sample TMC practice questions and detailed explanations to master the key concepts of mechanical ventilation.
91. What equipment is commonly needed for extubation?
Equipment includes suction, oxygen delivery device, pulse oximeter, towels, syringe for cuff deflation, bag-valve-mask, and reintubation equipment nearby.
92. What criteria should be assessed before extubation?
Criteria include successful spontaneous breathing trial, adequate oxygenation and ventilation, stable vital signs, adequate mental status, strong cough, manageable secretions, airway patency, and protective airway reflexes.
93. What is a cuff leak test?
A cuff leak test assesses whether air can pass around a deflated cuff and may help identify risk for post-extubation upper airway obstruction.
94. What does a poor cuff leak suggest?
A poor cuff leak may suggest laryngeal or subglottic edema and increased risk of post-extubation stridor.
95. How long can a patient remain intubated before tracheostomy is considered?
The timing varies, but if prolonged ventilation is expected, a tracheostomy may be considered after several days to weeks depending on the patient’s condition and care plan.
96. What are disadvantages of prolonged endotracheal intubation?
Disadvantages include discomfort, impaired speech, reduced cough effectiveness, thick secretions, swallowing impairment, aspiration risk, airway trauma, and increased risk of ventilator-associated pneumonia.
97. What is a laryngeal mask airway?
A laryngeal mask airway is a supraglottic airway device that can provide temporary ventilation when endotracheal intubation is difficult or unsuccessful.
98. What can be used after failed intubation attempts if ventilation is still possible?
A supraglottic airway, such as a laryngeal mask airway, may be used as a rescue device while preparing for a definitive airway plan.
99. What is cricothyrotomy?
Cricothyrotomy is an emergency surgical airway created through the cricothyroid membrane when ventilation and intubation cannot be achieved.
100. What is the key concept to remember about intubation?
Intubation is a high-risk airway procedure that requires preparation, preoxygenation, proper equipment, skilled placement, immediate confirmation, ongoing tube monitoring, and readiness for backup airway management.
Final Thoughts
Intubation is a lifesaving airway procedure, but it requires careful judgment and ongoing management. The goal is not only to place an endotracheal tube, but to protect oxygenation, ventilation, airway patency, and patient safety before, during, and after the procedure.
Respiratory therapists must understand when intubation is indicated, how to prepare for it, how to confirm tube placement, and how to recognize complications such as esophageal intubation, right mainstem placement, cuff injury, obstruction, aspiration, and infection.
When managed properly, intubation provides essential airway access for patients who cannot safely breathe or protect the airway on their own.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Alvarado AC, Panakos P. Endotracheal Intubation Techniques. [Updated 2023 Jul 10]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026.




