When discussing respiratory health, the terms mucus, phlegm, and sputum are often used interchangeably. However, each refers to something slightly different within the body’s respiratory system.
Understanding the distinction between these substances can help clarify how the lungs protect themselves and how healthcare professionals evaluate respiratory conditions. While mucus is a normal secretion that helps trap particles and pathogens, phlegm and sputum are typically associated with illness or irritation.
This article explains the differences between mucus, phlegm, and sputum and why recognizing these terms is important for understanding respiratory health and disease.
Download our free guide that has over 100+ of the best tips for healthy lungs.
What is the Difference Between Mucus, Phlegm, and Sputum?
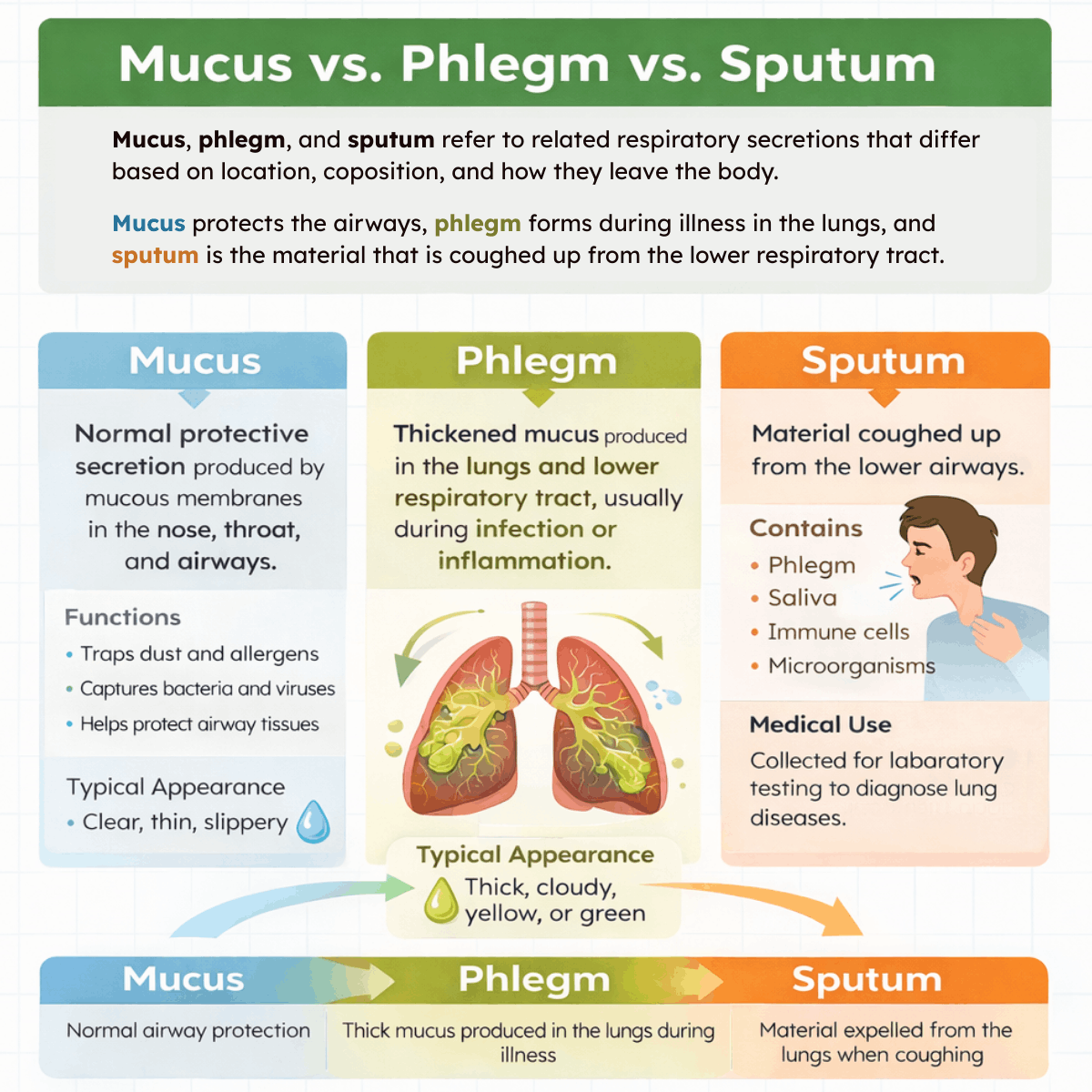
Mucus, phlegm, and sputum are related substances but refer to slightly different things within the respiratory system. Mucus is a normal, protective secretion produced by the mucous membranes lining the nose, throat, and airways. It helps trap dust, allergens, and microorganisms so they can be cleared from the body.
Phlegm is a type of mucus that is produced specifically in the lungs and lower respiratory tract, usually in response to irritation, inflammation, or infection. It is often thicker and more noticeable during illness.
Sputum refers to the material that is actually coughed up and expelled from the lower airways. It may contain phlegm along with saliva, cellular debris, and microorganisms. In clinical settings, sputum is often collected and analyzed to help diagnose respiratory diseases such as pneumonia or tuberculosis.
Understanding Mucus, Phlegm, and Sputum
Mucus, phlegm, and sputum refer to related but distinct substances in the respiratory system. Each term describes a different location, composition, or clinical context, and understanding these differences helps clarify symptoms and medical discussions.
Definitions and Differences
- Mucus is a slippery, gel-like fluid that mucous membranes produce throughout the body. It contains water, mucin proteins, salts, antibodies, and cellular debris. The body continuously makes mucus in the nose, sinuses, throat, lungs, and digestive tract.
- Phlegm refers specifically to thickened mucus that the lower respiratory tract produces, especially during illness. Infections, allergies, and irritants increase mucus production in the bronchi and lungs. When this mucus becomes excessive or inflamed, people often describe it as phlegm.
- Sputum is the material a person coughs up from the lower airways. It may contain phlegm, saliva, microorganisms, inflammatory cells, and debris. Clinicians use the term sputum when discussing laboratory testing, such as sputum cultures or cytology.
Note: In short, mucus is the general substance, phlegm is mucus from the lower airways during disease, and sputum is what exits the body through coughing.
Common Locations in the Body
Mucus lines many internal surfaces. It coats the nasal passages, sinuses, throat, trachea, bronchi, and lungs. It also lines the digestive and genitourinary tracts.
Phlegm forms in the lower respiratory tract, especially in the bronchi and lungs. Conditions such as bronchitis, pneumonia, asthma, and chronic obstructive pulmonary disease often increase its production. People typically notice phlegm when they feel chest congestion or persistent coughing.
Sputum originates in the lungs or bronchi but becomes visible only after expulsion. A person coughs it up from deep in the chest rather than clearing it from the throat. Its color and consistency—clear, yellow, green, brown, or blood-tinged—can provide clues about infection, inflammation, or other lung conditions.
Biological Functions
Mucus serves as a protective barrier. It traps dust, bacteria, viruses, and pollutants before they reach delicate tissues. Tiny hair-like structures called cilia move mucus upward and out of the airways in a process known as mucociliary clearance.
Phlegm forms as part of the immune response. When the airways detect infection or irritation, glands produce more mucus and immune cells enter the area. This thicker secretion helps trap pathogens but can also narrow airways and trigger coughing.
Sputum removal supports airway defense. Coughing expels accumulated phlegm, along with microbes and inflammatory debris. Although excess sputum can feel uncomfortable, it reflects the body’s effort to clear the lower respiratory tract.
Production and Composition
The body produces mucus continuously to protect and lubricate tissues. Phlegm and sputum develop when disease or irritation alters normal mucus production and clearance.
How Mucus is Produced
Specialized epithelial cells line the respiratory, digestive, and urogenital tracts. Goblet cells and submucosal glands secrete mucus in response to normal physiologic signals and environmental stimuli. Goblet cells release large gel-forming proteins called mucins, primarily MUC5AC and MUC5B in the airways. These mucins bind water and expand, forming a slippery, elastic layer that coats surfaces.
The body tightly regulates this process. Nerve signals, inflammatory mediators, and irritants such as dust or smoke can increase mucin secretion within minutes.
Mucus consists of about 95% water, which keeps it fluid and spreadable. The remaining portion includes mucins, electrolytes, antibodies such as IgA, enzymes like lysozyme, and defensins that help limit microbial growth.
Note: Cilia on epithelial cells constantly move mucus toward the throat in a process called mucociliary clearance. This mechanism traps particles and removes them before they reach deeper tissues.
Phlegm Formation in the Airways
Phlegm forms when inflammation increases mucus production in the lower respiratory tract. Conditions such as viral infections, asthma, chronic bronchitis, and pneumonia stimulate excess mucin release. Inflammatory cells release cytokines that trigger goblet cell hyperplasia and gland enlargement. As a result, the airway lining produces thicker and more abundant secretions.
Infection also changes mucus composition. White blood cells, especially neutrophils, migrate into the airway and release enzymes and cellular debris, which thicken the material. Damaged cilia reduce clearance efficiency. When mucus accumulates and mixes with inflammatory cells and microbes, it becomes what people commonly call phlegm.
Note: Color changes often reflect cellular content. Yellow or green tones usually result from enzymes within neutrophils rather than the color of the infecting organism itself.
Components of Sputum
Sputum refers to material that a person actively coughs up from the lower airways. It contains a mixture of mucus, inflammatory cells, microorganisms, and cellular debris. Its composition varies by condition. In bacterial pneumonia, sputum often contains high numbers of neutrophils and identifiable bacteria.
In asthma, sputum may show increased eosinophils and thick mucus plugs. In chronic obstructive pulmonary disease, it often includes excess mucins and inflammatory cells linked to long-term airway irritation.
Laboratories analyze sputum to detect pathogens, measure inflammatory cell types, and assess blood presence. Clinicians use these findings to guide diagnosis and treatment decisions.
Note: Although mucus, phlegm, and sputum overlap in content, their differences reflect location, disease activity, and whether the material remains in the airway or has been expelled.
Causes of Excess Mucus, Phlegm, and Sputum
Excess mucus production usually signals irritation or inflammation in the airways. Infections, environmental exposures, and chronic lung diseases account for most cases and often determine the color, thickness, and amount of phlegm or sputum a person notices.
Respiratory Infections
Respiratory infections commonly increase mucus production. Viruses such as the common cold, influenza, and COVID-19 infect the lining of the nose, throat, and lungs, which triggers inflammation and stimulates mucus glands.
In viral infections, mucus often starts clear and may become thicker and white or yellow as immune cells respond. Bacterial infections, including sinusitis or pneumonia, can produce thicker yellow or green sputum. The color reflects immune activity, not necessarily severity.
Acute bronchitis frequently causes a persistent cough with phlegm that lasts several weeks. Pneumonia may produce rust-colored or blood-tinged sputum, along with fever and shortness of breath.
Note: As the infection resolves, mucus production typically decreases. Persistent or worsening sputum may signal a secondary bacterial infection or complications that require medical evaluation.
Allergies and Irritants
Allergic reactions drive excess mucus through immune system activation. When a person inhales allergens such as pollen, dust mites, mold spores, or pet dander, the body releases histamine and other chemicals that increase nasal and airway secretions.
Allergic rhinitis often causes clear, watery mucus, nasal congestion, and postnasal drip. Postnasal drip can irritate the throat and trigger coughing, which may produce small amounts of clear or white phlegm.
Environmental irritants also stimulate mucus production. Cigarette smoke, air pollution, strong odors, and chemical fumes directly inflame airway tissues. The body responds by producing thicker mucus to trap and remove harmful particles.
Note: Repeated exposure can maintain chronic inflammation. Smokers, in particular, often develop daily phlegm due to ongoing airway irritation and impaired clearance of secretions.
Chronic Respiratory Conditions
Chronic respiratory diseases frequently cause ongoing excess mucus and sputum. Asthma, chronic bronchitis, and chronic obstructive pulmonary disease (COPD) alter airway structure and function. In asthma, airway inflammation and narrowing increase mucus production, especially during flare-ups. Patients may cough up thick, sticky sputum along with wheezing and chest tightness.
Chronic bronchitis, a form of COPD, is defined by a productive cough lasting at least three months per year for two consecutive years. Damaged airway lining and enlarged mucus glands produce daily phlegm, often worse in the morning.
Bronchiectasis causes permanent widening of the airways, which allows mucus to pool and become infected. This condition often leads to large amounts of thick, sometimes foul-smelling sputum and recurrent lung infections.
Color and Consistency Differences
Color and thickness provide practical clues about what the body is doing in the airways. Changes in appearance often reflect hydration, irritation, infection, or inflammation rather than a single specific disease.

Normal Variations
Healthy mucus usually appears clear or slightly white. It feels thin and slippery, which helps trap dust, pollen, and microbes while allowing the cilia in the airways to move it easily. Mild dehydration can make mucus look thicker and slightly cloudy. After sleep, many people notice small amounts of thicker white or pale yellow material due to slower overnight clearance.
Temperature and environment also influence consistency. Dry indoor air can thicken nasal mucus, while humid air keeps it looser. In the lower airways, small amounts of clear or white phlegm may be present without signaling illness, especially in people exposed to smoke or air pollution.
Note: Color alone does not define disease. Light yellow mucus can appear during routine immune activity and may resolve without treatment.
What Changes in Appearance Indicate
Yellow or green phlegm often reflects increased white blood cells responding to infection or irritation. The green tint comes from enzymes inside these immune cells. This change can occur in both viral and bacterial infections.
Brown or rust-colored sputum may contain old blood. People who smoke often produce brown-tinged phlegm due to tar and particulate buildup. Pink, frothy sputum can suggest fluid in the lungs. Thick, sticky mucus that is hard to cough up may point to asthma, cystic fibrosis, or chronic bronchitis.
Consistency also matters. Thin and watery mucus often appears with allergies or viral colds, while thick and tenacious secretions commonly accompany bacterial infections or chronic inflammatory conditions. A sudden increase in volume, especially with color change, signals an active process in the airways.
When to Be Concerned
Certain colors require prompt medical evaluation. Red or blood-streaked sputum may indicate airway injury, severe infection, a blood clot, or other serious conditions.
Black sputum can occur with heavy smoke exposure or certain fungal infections. Persistent green or yellow phlegm lasting more than 10 days, especially with fever or chest pain, suggests a need for clinical assessment.
Consistency also raises concern when it interferes with breathing. Thick plugs that cause wheezing, shortness of breath, or chest tightness require attention.
High fever, night sweats, unexplained weight loss, or worsening cough alongside discolored sputum increase the urgency. In these cases, clinicians often recommend imaging or laboratory testing to determine the cause.
Health Implications
Changes in mucus, phlegm, and sputum often signal specific respiratory or systemic conditions. Color, thickness, volume, and associated symptoms help clinicians identify infection, inflammation, or chronic disease.
Links to Underlying Diseases
Excess or altered mucus production frequently reflects inflammation or infection. Viral upper respiratory infections often cause clear or white mucus, while bacterial infections may produce yellow or green sputum due to immune cell activity.
Chronic conditions also change mucus patterns.
- Asthma increases thick airway mucus that narrows breathing passages.
- Chronic obstructive pulmonary disease (COPD) leads to persistent phlegm and airflow limitation.
- Cystic fibrosis produces unusually thick, sticky mucus that traps bacteria and causes repeated lung infections.
Blood-tinged sputum may appear with severe bronchitis, pneumonia, pulmonary embolism, or lung cancer. Frothy pink sputum can indicate fluid buildup in the lungs from heart failure.
Gastroesophageal reflux disease (GERD) and chronic sinusitis can also increase throat clearing and postnasal drip. In these cases, excess mucus does not originate in the lungs but still irritates the airway.
Symptoms Requiring Medical Attention
Certain features require prompt evaluation. A cough that produces sputum for more than three weeks may signal chronic bronchitis, tuberculosis, or another persistent condition.
Medical assessment becomes important if sputum contains:
- Bright red blood or rust-colored streaks
- Large amounts of thick green or brown material
- Foul odor, which may suggest lung abscess
Shortness of breath, chest pain, high fever, night sweats, or unexplained weight loss alongside abnormal sputum raise concern for pneumonia, tuberculosis, or malignancy.
Sudden increases in phlegm volume in people with asthma or COPD may indicate an acute exacerbation. Early treatment can reduce complications and prevent hospitalization.
Diagnosis and Testing
Clinicians distinguish mucus, phlegm, and sputum by evaluating symptoms and analyzing material expelled from the respiratory tract. Accurate identification guides treatment decisions and helps detect infection, inflammation, or chronic lung disease.
Primary Diagnostic Approaches
Healthcare providers begin with a focused medical history. They ask about cough duration, sputum color and volume, fever, shortness of breath, smoking history, and recent infections.
A physical examination follows. The clinician listens to lung sounds with a stethoscope to detect wheezing, crackles, or reduced airflow. They also check oxygen saturation and look for signs of respiratory distress.
Imaging studies support the evaluation when symptoms suggest deeper lung involvement. A chest X-ray can reveal pneumonia, masses, or fluid buildup. In more complex cases, a CT scan provides detailed images of lung tissue and airways.
When cough persists beyond eight weeks or produces blood, clinicians escalate testing. They may order pulmonary function tests to assess airflow limitation seen in asthma or chronic obstructive pulmonary disease (COPD).
Laboratory Analysis of Sputum
When a patient produces material from the lower airways, clinicians collect it for laboratory testing. Proper collection matters; the sample should come from a deep cough, not saliva.
Laboratories examine sputum in several ways:
- Microscopy: Identifies white blood cells, bacteria, or abnormal cells.
- Gram stain and culture: Detect specific bacterial pathogens and guide antibiotic selection.
- Acid-fast staining: Screens for Mycobacterium tuberculosis.
- Cytology: Evaluates for malignant cells in patients with suspected lung cancer.
Color and consistency provide clues but do not confirm diagnosis. Green or yellow sputum often reflects infection, while clear or white sputum may appear in viral illness or asthma.
Note: If routine tests do not explain symptoms, clinicians may request molecular assays such as PCR to identify viral or atypical bacterial pathogens.
Treatment and Management Strategies
Managing mucus, phlegm, and sputum depends on the cause, severity, and duration of symptoms. Simple home measures often relieve mild congestion, while infections or chronic lung disease may require targeted medical therapy.
Home Remedies
- Adequate hydration remains one of the most effective strategies. Drinking water thins mucus, making it easier to clear from the nose, throat, and lungs.
- Warm fluids such as broth or herbal tea can soothe irritated airways. Steam inhalation or a warm shower may also loosen thick secretions and improve short-term airflow.
- Using a humidifier adds moisture to dry indoor air, which helps prevent mucus from becoming sticky. Regular cleaning of the device prevents mold and bacterial growth.
- Saline nasal sprays or rinses flush irritants, allergens, and excess mucus from the nasal passages. People with postnasal drip often benefit from daily use during allergy seasons.
- Avoiding smoke, strong fragrances, and known allergens reduces ongoing mucus production. Rest also supports immune function during viral infections.
Medical Treatments
When symptoms persist or worsen, clinicians may recommend medication based on the underlying cause. For bacterial infections, antibiotics may be prescribed after clinical evaluation.
For viral illnesses, treatment focuses on symptom control. Over-the-counter expectorants containing guaifenesin can thin sputum, while short-term decongestants may reduce nasal swelling.
People with asthma or chronic obstructive pulmonary disease (COPD) often require inhaled bronchodilators or corticosteroids. These medications reduce airway inflammation and improve mucus clearance.
Allergic rhinitis may respond to antihistamines or intranasal corticosteroid sprays. In cases of chronic or bloody sputum, clinicians may order imaging or sputum analysis to rule out serious conditions.
Preventive Measures
Simple lifestyle habits and environmental adjustments can help reduce excess mucus, phlegm, and sputum. Taking proactive steps to protect the airways limits irritation, supports normal mucus clearance, and lowers the risk of respiratory infections.
Lifestyle Adjustments
- Staying well hydrated is one of the most effective ways to keep mucus thin and easier to clear from the airways. Water is the best option, while excessive caffeine or alcohol may contribute to dehydration and thicker secretions.
- Avoiding tobacco smoke is equally important. Smoking irritates the lining of the airways, increases mucus production, and damages the cilia responsible for moving mucus out of the lungs.
- Regular physical activity also supports healthy lung function. Activities such as brisk walking, cycling, or swimming for at least 150 minutes per week can help mobilize secretions, improve circulation, and enhance breathing efficiency.
- Managing allergies and chronic respiratory conditions under medical guidance is another key strategy. Proper use of prescribed medications such as inhalers, nasal corticosteroids, or antihistamines can reduce inflammation and prevent excessive mucus buildup.
- Practicing good hand hygiene lowers the risk of viral and bacterial infections that commonly trigger mucus production. Washing hands with soap for at least 20 seconds and avoiding unnecessary face touching helps reduce the spread of pathogens.
Environmental Controls
- Maintaining healthy indoor air quality plays an important role in preventing airway irritation. Keeping indoor humidity levels between 30% and 50% helps maintain optimal mucus consistency. Air that is too dry can thicken secretions, while excessive humidity may promote mold growth.
- Using high-efficiency particulate air (HEPA) filters can reduce airborne irritants such as dust, pollen, and pet dander. Regularly replacing HVAC filters also improves indoor air circulation and air quality.
- Limiting exposure to strong odors, cleaning chemicals, and air pollution further protects the respiratory system. Choosing unscented household products and ensuring proper ventilation during cooking or cleaning can help reduce airway irritation.
- Routine household cleaning also helps control allergens. Washing bedding weekly in hot water and regularly cleaning carpets, curtains, and upholstery reduces dust mites and other triggers that may increase mucus production.
Impact on Daily Life
Excess mucus, phlegm, and sputum can affect daily comfort, energy levels, and overall quality of life. Increased mucus production may lead to symptoms such as a stuffy or runny nose, frequent throat clearing, or a persistent cough.
Phlegm often feels thicker and more noticeable, particularly when it accumulates in the chest. This can interfere with speaking, eating, or sleeping, especially if coughing episodes occur at night. Poor sleep quality may contribute to daytime fatigue and difficulty concentrating.
Sputum production can also influence daily routines. Some individuals may need to carry tissues, clear their throat frequently, or pause activities to cough and remove airway secretions. In work or school environments, these interruptions can affect communication and productivity.
Changes in the color, thickness, or volume of sputum may also cause concern about infection or worsening respiratory disease. For individuals with conditions such as asthma, chronic bronchitis, or COPD, these changes can create anxiety and require closer monitoring of symptoms.
Many people adapt their routines to manage symptoms more effectively. Staying hydrated, using humidifiers, avoiding smoke or strong fragrances, and maintaining good indoor air quality can help reduce irritation and support airway comfort.
Note: When mucus-related symptoms persist or worsen, they may limit physical activity and reduce exercise tolerance. Shortness of breath, chest discomfort, or frequent coughing can interfere with normal activities and negatively affect overall well-being.
FAQs About Mucus, Phlegm, and Sputum
Do You Cough Up Phlegm or Mucus?
When you cough up material from your chest, it is typically called phlegm or sputum, not mucus. Phlegm refers to thickened mucus produced in the lower respiratory tract, including the bronchi and lungs, usually during irritation, infection, or inflammation. When this material is expelled through coughing, healthcare professionals refer to it as sputum.
Mucus, on the other hand, is the normal secretion that lines the airways and other mucous membranes. In everyday conversation, people often say they are coughing up mucus, but medically it is more accurate to call it phlegm or sputum.
Is It OK to Swallow Mucus or Phlegm?
In most cases, swallowing mucus or phlegm is harmless. The digestive system is well equipped to break down and neutralize bacteria, viruses, and other particles trapped in these secretions. This process happens naturally throughout the day when mucus drains from the nose and throat and is swallowed without notice.
However, some people prefer to spit out phlegm, especially when it is thick or produced during respiratory infections. Spitting may provide temporary relief, but medically there is usually no harm in swallowing it.
Does Phlegm Look Like Mucus?
Phlegm often looks similar to mucus because both are made from the same basic substances. However, phlegm is usually thicker and may appear more opaque. Mucus produced in healthy airways is typically clear or slightly white and relatively thin.
Phlegm, which forms in the lower respiratory tract during illness or irritation, can appear yellow, green, brown, or occasionally blood-tinged. These changes in color and consistency occur because phlegm often contains immune cells, microorganisms, and inflammatory debris in addition to mucus.
Is It Better to Spit Out Mucus or Swallow It?
There is generally no medical requirement to spit out mucus or phlegm, as swallowing it is safe for most people. The stomach’s acids and digestive enzymes destroy many of the microorganisms trapped in respiratory secretions.
However, some individuals prefer to spit out thick phlegm because it may feel uncomfortable or irritating in the throat. Spitting can also help clear the airways more quickly in some cases. Ultimately, whether you swallow or spit it out is mostly a matter of comfort rather than health necessity.
How Do You Know If It’s Mucus or Phlegm?
The main difference between mucus and phlegm lies in where it comes from. Mucus is the normal, protective secretion produced throughout the respiratory tract, including the nose and throat. Phlegm specifically refers to mucus produced in the lower airways, such as the bronchi and lungs, usually during illness or inflammation.
If the material comes from chest congestion and is coughed up from deep in the lungs, it is generally considered phlegm. Thinner secretions from the nose or throat are more accurately described as mucus.
How Is Sputum Different From Mucus?
Sputum and mucus are related but not identical. Mucus is the slippery fluid produced by mucous membranes throughout the body to trap particles and protect tissues.
Sputum refers specifically to material that has been coughed up and expelled from the lower respiratory tract. It often contains phlegm along with saliva, microorganisms, inflammatory cells, and cellular debris
Note: In clinical settings, sputum samples are commonly collected and analyzed to help diagnose respiratory conditions such as pneumonia, tuberculosis, or other lung infections.
How Is Sputum Different From Phlegm?
Phlegm and sputum are closely related terms but describe slightly different things. Phlegm refers to thickened mucus produced in the lungs and bronchi during irritation, infection, or inflammation. Sputum is the material that is actually coughed up and expelled from the respiratory tract.
In other words, phlegm is a component of sputum. When a person coughs and expels secretions from the lower airways, that mixture of phlegm, saliva, immune cells, and debris is referred to medically as sputum.
Final Thoughts
Although the terms mucus, phlegm, and sputum are often used interchangeably, they describe slightly different substances related to the respiratory system.
Mucus serves as a normal protective secretion that traps particles and pathogens, helping keep the airways clean. Phlegm refers to thicker mucus produced in the lungs during irritation or infection, while sputum is the material that is coughed up and expelled from the lower respiratory tract.
Understanding these distinctions can help improve communication about respiratory symptoms and assist healthcare professionals in evaluating lung health and diagnosing respiratory conditions.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Shen F, Zubair M, Sergi C. Sputum Analysis. [Updated 2025 May 4]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026.