Congestive heart failure (CHF) is a prevalent cardiovascular disorder with direct and often serious effects on the respiratory system. Because the heart and lungs operate as a closely connected cardiopulmonary unit, impaired cardiac function frequently leads to pulmonary congestion, edema, and compromised gas exchange.
For respiratory therapists, a clear understanding of CHF is critical for identifying hydrostatic pulmonary edema, distinguishing it from other causes of respiratory failure, and delivering appropriate oxygen and ventilatory support.
This article explains what CHF is, outlines its underlying pathophysiology, reviews key clinical features, and highlights its importance in respiratory care practice.
What is Congestive Heart Failure?
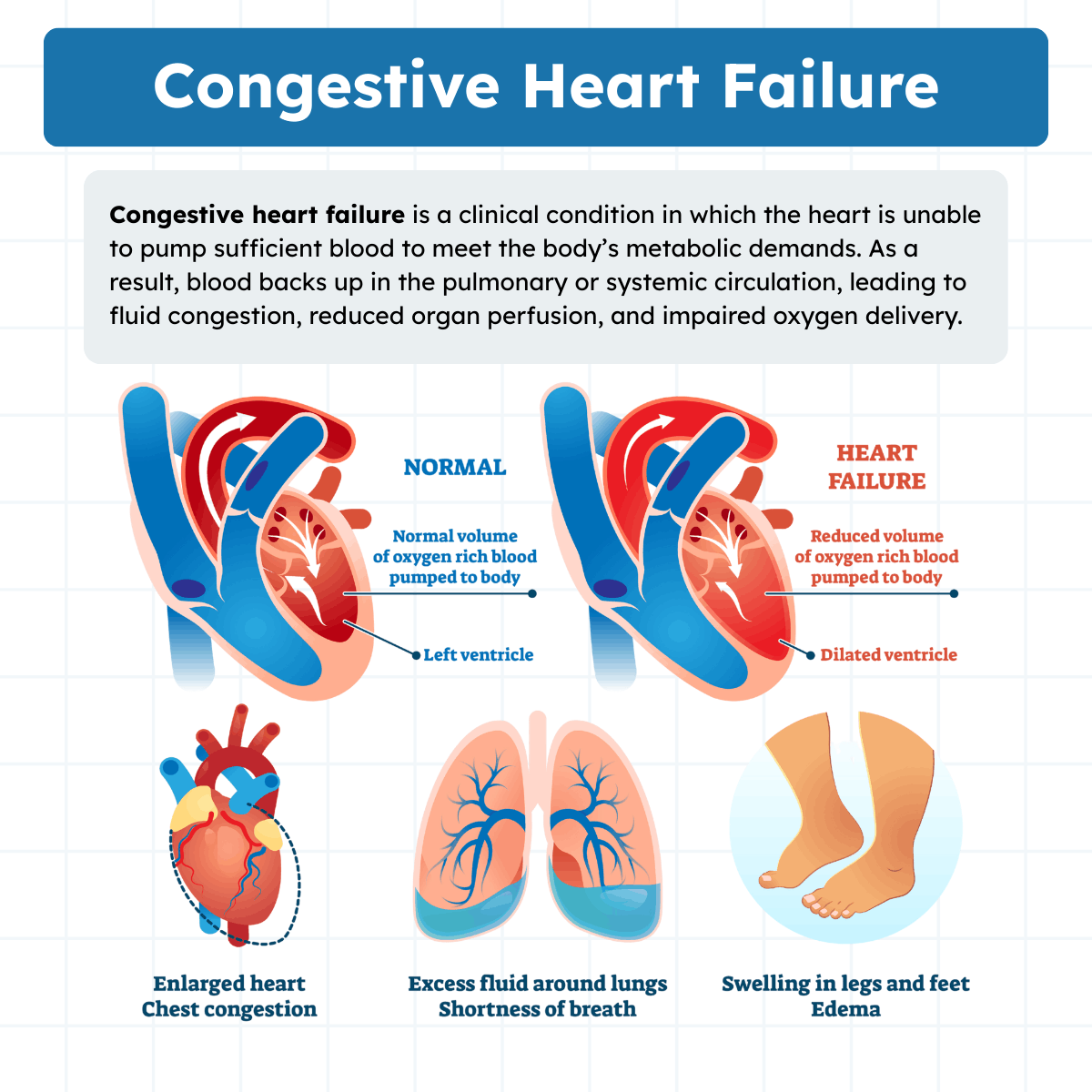
Congestive heart failure (CHF) occurs when the heart is unable to pump blood effectively enough to meet the metabolic demands of the body. The most common mechanism involves impaired left ventricular function, which may be due to coronary artery disease, myocardial infarction, cardiomyopathy, valvular heart disease, or long-standing hypertension.
Heart failure can be classified as systolic or diastolic. In systolic heart failure, the left ventricle has reduced contractility and a decreased ejection fraction. In diastolic heart failure, the ventricle has impaired relaxation and filling despite a preserved ejection fraction. In both cases, elevated left-sided heart pressures often develop.
When the left ventricle fails to pump efficiently, blood backs up into the left atrium and pulmonary veins. This increases pulmonary venous pressure and leads to elevated hydrostatic pressure within the pulmonary capillaries. As a result, fluid moves from the capillaries into the interstitial space and, in severe cases, into the alveoli. This process produces pulmonary edema, a major respiratory complication of CHF.
Right ventricular failure may also occur, often secondary to left-sided failure. Right-sided failure leads to systemic venous congestion, resulting in peripheral edema, jugular venous distension, hepatomegaly, and ascites.
Pulmonary Edema and Congestive Heart Failure
The defining respiratory feature of CHF is hydrostatic pulmonary edema. When pulmonary capillary hydrostatic pressure rises, the normal balance of fluid exchange across the alveolar-capillary membrane is disrupted. Fluid leaks into the interstitial space and eventually floods the alveoli.
In hydrostatic pulmonary edema, the endothelial and epithelial barriers generally remain intact. Because these barriers are not damaged, the fluid that accumulates in the alveoli is low in protein and contains few inflammatory cells. This fluid is classified as a transudate.
As fluid accumulates:
- Lung compliance decreases
- Lung volumes are reduced
- Work of breathing increases
- Gas exchange becomes impaired
Alveolar flooding increases diffusion distance and creates a ventilation-perfusion mismatch. In severe cases, intrapulmonary shunting develops, leading to refractory hypoxemia.
Patients may use 25 to 50 percent of their total metabolic energy to sustain the increased work of breathing associated with pulmonary edema. If untreated, this can progress to respiratory failure.
Clinical Presentation
Patients with CHF may present with both cardiac and respiratory symptoms. The severity depends on whether the condition is stable or acutely decompensated.
Common Respiratory Findings
- Dyspnea, especially on exertion
- Orthopnea
- Paroxysmal nocturnal dyspnea
- Tachypnea
- Bilateral crackles on auscultation
- Wheezing, sometimes referred to as cardiac asthma
- Hypoxemia
Note: In acute pulmonary edema, patients may produce frothy or pink-tinged sputum and demonstrate marked respiratory distress.
Common Cardiac and Systemic Findings
- Cardiomegaly on chest radiograph
- Peripheral edema
- Jugular venous distension
- Gallop rhythm
- Fatigue
- Hypotension in severe cases
Note: Chest radiography often shows bilateral, symmetric perihilar infiltrates, vascular congestion, Kerley B lines, and pleural effusions. Pleural effusions associated with CHF are usually bilateral and transudative. When unilateral, they are more commonly right-sided than left-sided.
CHF and Hypoxemia
CHF can lead to hypoxemia through several mechanisms:
- Ventilation-perfusion mismatch
- Intrapulmonary shunting
- Low mixed venous oxygen saturation due to reduced cardiac output
Low cardiac output results in increased peripheral oxygen extraction. This decreases mixed venous oxygen saturation, which in turn reduces the oxygen gradient available during pulmonary gas exchange. When underlying lung dysfunction is present, this effect becomes more pronounced.
Respiratory therapists must recognize that hypoxemia in CHF is often multifactorial. Management requires both respiratory support and treatment of the underlying cardiac dysfunction.
Differentiating CHF from ARDS
One of the most important responsibilities in respiratory care is distinguishing hydrostatic pulmonary edema caused by CHF from nonhydrostatic pulmonary edema caused by acute respiratory distress syndrome (ARDS).
Both conditions may present with:
- Dyspnea
- Tachypnea
- Diffuse infiltrates on chest imaging
- Hypoxemia
Features Favoring CHF
- Cardiomegaly on chest radiograph
- Symmetric pulmonary infiltrates
- Pleural effusions
- Elevated pulmonary artery wedge pressure
- Rapid improvement with diuretics and cardiac therapy
- Bronchoalveolar lavage fluid low in protein
Features Favoring ARDS
- Normal heart size
- Peripheral or asymmetric infiltrates
- High protein content in alveolar fluid
- Marked inflammatory cellular influx
- Poor initial response to diuretics
Note: Correct differentiation is critical because management strategies differ significantly. CHF requires diuresis, afterload reduction, and improvement of cardiac output. ARDS requires lung-protective ventilation and management of underlying inflammatory injury.
Diagnostic Evaluation
In patients suspected of CHF, evaluation often includes:
- Chest radiography
- Electrocardiogram
- Echocardiography
- Measurement of B-type natriuretic peptide
- Cardiac biomarkers if myocardial infarction is suspected
Arterial blood gas analysis typically shows hypoxemia and may reveal respiratory alkalosis in early stages due to tachypnea. As fatigue develops, respiratory acidosis may occur.
Note: Mixed venous oxygen measurements can provide insight into cardiac output and oxygen extraction balance.
Relevance to Respiratory Therapists
Congestive heart failure has direct and frequent implications for respiratory care practice. Because left-sided heart dysfunction leads to pulmonary venous congestion and hydrostatic pulmonary edema, many patients with CHF present primarily with respiratory symptoms.
As a result, respiratory therapists are often among the first clinicians to assess and manage these patients, particularly in emergency departments, intensive care units, and acute care settings.
Oxygen Therapy
Hypoxemia is common in CHF due to ventilation-perfusion mismatch, intrapulmonary shunting, and reduced mixed venous oxygen saturation from low cardiac output. Supplemental oxygen is frequently required to maintain adequate arterial oxygenation. Respiratory therapists must carefully titrate oxygen therapy to achieve appropriate saturation goals while monitoring respiratory rate, work of breathing, and overall clinical status.
Although oxygen improves arterial oxygen content, it does not correct the underlying hemodynamic problem. Therefore, therapists must recognize that persistent hypoxemia may signal worsening pulmonary edema or cardiac dysfunction.
Noninvasive Ventilation
Noninvasive positive pressure ventilation (NPPV) plays a major role in the management of acute cardiogenic pulmonary edema. Continuous positive airway pressure and bilevel positive airway pressure improve oxygenation by recruiting alveoli and increasing functional residual capacity. Positive pressure also reduces the work of breathing and helps offset decreased lung compliance caused by interstitial and alveolar fluid.
In addition to improving gas exchange, positive pressure ventilation has beneficial cardiovascular effects. By increasing intrathoracic pressure, it reduces venous return and left ventricular preload. It may also reduce left ventricular afterload by decreasing transmural pressure. These effects can lead to rapid improvement in dyspnea and oxygenation, often preventing the need for intubation. Respiratory therapists are responsible for initiating therapy, selecting appropriate settings, ensuring mask fit, and monitoring patient tolerance and response.
Invasive Mechanical Ventilation
When noninvasive support fails or when respiratory fatigue develops, intubation and invasive mechanical ventilation may be required. Ventilator management in CHF requires careful attention to both respiratory and hemodynamic status. Positive pressure can improve oxygenation and reduce pulmonary edema, but excessive positive end-expiratory pressure may decrease cardiac output in preload-dependent patients.
Therapists must monitor oxygenation, arterial blood gases, hemodynamics, and signs of improved or worsening pulmonary congestion. Close collaboration with the medical team is essential to adjust ventilator settings in a way that supports gas exchange without compromising perfusion.
Airway Assessment and Differential Considerations
Patients with CHF may present with wheezing, often described as cardiac asthma. This wheezing results from airway narrowing caused by interstitial edema rather than bronchospasm. Respiratory therapists must interpret breath sounds within the broader clinical context.
In some cases, bronchodilators may provide limited benefit, while diuretics and afterload reduction are more appropriate. Accurate assessment prevents unnecessary treatments and supports timely cardiac management.
Monitoring Work of Breathing
Hydrostatic pulmonary edema reduces lung compliance and increases the elastic load of breathing. Patients may exhibit tachypnea, accessory muscle use, and signs of fatigue. Early identification of increased work of breathing allows timely escalation of support, reducing the risk of respiratory failure.
Pleural Effusion Considerations
Pleural effusions frequently accompany CHF and may further restrict lung expansion. Although treatment focuses on correcting the underlying cardiac dysfunction, respiratory therapists play an important role in monitoring oxygenation, lung mechanics, and clinical response.
Note: CHF intersects with nearly every aspect of respiratory care, from oxygen delivery to advanced ventilatory support. A strong understanding of cardiopulmonary physiology enables respiratory therapists to provide safe, effective, and evidence-based care.
Management Principles
Management of stable CHF includes:
- Sodium and fluid restriction
- Angiotensin-converting enzyme inhibitors or angiotensin receptor blockers
- Beta blockers
- Diuretics
- Aldosterone antagonists
- Digoxin in selected patients
In acute decompensated CHF with pulmonary edema, treatment may include:
- High-concentration oxygen
- CPAP or BiPAP
- Loop diuretics
- Vasodilators
- Inotropic agents if hypotensive
- Advanced cardiac life support protocols if arrhythmias occur
Note: Respiratory therapists play an active role in implementing oxygen therapy, noninvasive ventilation, invasive ventilation, and monitoring clinical response.
Congestive Heart Failure Practice Questions
1. What is congestive heart failure (CHF)?
Congestive heart failure is a chronic, progressive syndrome in which the heart cannot pump enough blood to meet the body’s metabolic demands, leading to fluid congestion and reduced tissue perfusion.
2. What occurs in a normal heart during systole?
The heart ejects an adequate stroke volume to maintain sufficient cardiac output and oxygen delivery to tissues.
3. In congestive heart failure, what is impaired?
The heart’s ability to pump or fill effectively, resulting in reduced cardiac output and/or elevated filling pressures.
4. What pulmonary complication is commonly associated with left-sided CHF?
Pulmonary edema due to increased pulmonary capillary hydrostatic pressure.
5. What are two common causes of left-sided heart failure?
Coronary artery disease (including myocardial infarction) and chronic hypertension.
6. What is a forward effect of left-sided heart failure?
Decreased cardiac output leading to reduced systemic perfusion and fatigue.
7. What is a backward effect of left-sided heart failure?
Blood backs up into the pulmonary circulation, increasing pulmonary pressures and causing congestion.
8. What is often the earliest symptom of left-sided heart failure?
Dyspnea on exertion.
9. What are three common causes of right-sided heart failure?
Left-sided heart failure, pulmonary hypertension, and right ventricular infarction.
10. What is a forward effect of right-sided heart failure?
Reduced blood flow to the lungs, which may ultimately decrease left ventricular preload and cardiac output.
11. What is a backward effect of right-sided heart failure?
Systemic venous congestion resulting in peripheral edema and organ enlargement.
12. What is the primary treatment goal in CHF?
To reduce cardiac workload, relieve congestion, and improve cardiac output.
13. Why are diuretics prescribed in CHF?
To decrease preload by reducing intravascular volume and relieving fluid overload.
14. When does congestive heart failure develop?
When the heart cannot pump sufficient blood to meet the body’s oxygen and metabolic needs.
15. What are common causes of CHF?
Coronary artery disease, myocardial infarction, hypertension, valvular disease, cardiomyopathy, and chronic arrhythmias such as atrial fibrillation.
16. Which laboratory test is commonly elevated in CHF and reflects ventricular stretch?
B-type natriuretic peptide (BNP).
17. What imaging study can reveal cardiomegaly and pulmonary congestion in CHF?
Chest radiography
18. What is left-sided heart failure?
Failure of the left ventricle to effectively pump blood into systemic circulation, resulting in pulmonary congestion.
19. What respiratory findings are common in left-sided heart failure?
Tachypnea, crackles (rales), orthopnea, and increased work of breathing.
20. What is right-sided heart failure?
Failure of the right ventricle to pump blood effectively into the pulmonary circulation, causing systemic venous congestion.
21. What are common signs of right-sided heart failure?
Peripheral edema, ascites, hepatomegaly, and jugular venous distention.
22. What lifestyle modifications are recommended in CHF management?
Sodium restriction, fluid restriction (if indicated), smoking cessation, and regular monitored exercise.
23. What is a hallmark clinical feature of congestive heart failure?
Fluid overload
24. What early symptom may patients with CHF report before overt edema develops?
Fatigue and decreased exercise tolerance.
25. How does CHF affect long-term prognosis?
It is associated with increased morbidity and reduced life expectancy, particularly in advanced stages.
26. What common pathway can result from many forms of cardiac disease?
Heart failure
27. Approximately how many deaths annually in the United States are attributed to heart failure?
Over 200,000 deaths per year.
28. Approximately how many hospitalizations occur annually due to heart failure?
More than one million hospitalizations per year.
29. What is the approximate five-year survival rate for patients with systolic heart failure?
Approximately 50%
30. How is congestive heart failure physiologically characterized?
By volume overload (intravascular and interstitial) and signs of inadequate tissue perfusion.
31. What clinical findings suggest intravascular and interstitial volume overload in congestive heart failure?
Dyspnea, pulmonary crackles (rales), peripheral edema, and weight gain from fluid retention.
32. What symptoms are commonly associated with inadequate tissue perfusion in CHF?
Fatigue, decreased exercise tolerance, cool extremities, and reduced urine output due to impaired renal perfusion.
33. Approximately how many people in the United States are living with heart failure?
More than 6 million individuals.
34. What age group accounts for the majority of heart failure cases?
Adults older than 65 years account for most cases.
35. What are common causes of left-sided heart failure?
Coronary artery disease, chronic hypertension, prior myocardial infarction, dilated cardiomyopathy, and restrictive cardiomyopathy.
36. How does myocardial ischemia contribute to left-sided heart failure?
Reduced coronary blood flow impairs myocardial contractility, decreasing left ventricular pumping ability.
37. How does chronic hypertension lead to left-sided heart failure?
Long-standing hypertension causes left ventricular hypertrophy, increasing myocardial oxygen demand and eventually leading to systolic or diastolic dysfunction.
38. What is dilated cardiomyopathy (DCM)?
A condition characterized by enlargement and weakened contraction of one or more cardiac chambers, most commonly the left ventricle.
39. How does dilated cardiomyopathy cause heart failure?
Chamber dilation reduces contractile efficiency, lowering stroke volume and cardiac output.
40. How can a myocardial infarction lead to heart failure?
Necrotic myocardial tissue loses contractile function, reducing overall ventricular performance.
41. What is restrictive cardiomyopathy, and how does it affect cardiac function?
Restrictive cardiomyopathy is characterized by stiff ventricular walls that impair diastolic filling, limiting stroke volume despite preserved systolic function.
42. What is a major pulmonary consequence of left-sided heart failure?
Pulmonary congestion resulting from elevated left atrial and pulmonary venous pressures.
43. Which intravascular pressure rises during pulmonary congestion?
Pulmonary capillary hydrostatic pressure increases.
44. What are classic symptoms of pulmonary congestion in CHF?
Dyspnea, orthopnea, paroxysmal nocturnal dyspnea (PND), and inspiratory crackles.
45. What is orthopnea?
Shortness of breath that occurs when lying flat and improves when sitting upright.
46. What causes inspiratory crackles in patients with CHF?
Fluid accumulation within the alveoli and interstitial spaces.
47. What diagnostic tests commonly assist in evaluating CHF?
Echocardiography, B-type natriuretic peptide (BNP) levels, chest radiography, and electrocardiography.
48. What is chronic heart failure?
A long-term condition in which the heart persistently fails to meet the body’s circulatory demands, leading to ongoing symptoms and fluid retention.
49. What is congenital heart disease?
Structural abnormalities of the heart present at birth that may impair normal blood flow and contribute to heart failure.
50. What is heart valve disease?
A disorder in which one or more cardiac valves fail to open or close properly, causing stenosis or regurgitation and potentially leading to heart failure.
51. What hemodynamic change is a defining feature of left-sided congestive heart failure?
Elevation of left atrial and pulmonary venous pressures.
52. How does increased pulmonary venous pressure affect the lungs in CHF?
It raises pulmonary capillary hydrostatic pressure, promoting fluid movement into the interstitial and alveolar spaces.
53. What type of pulmonary edema is most commonly associated with CHF?
Cardiogenic (hydrostatic) pulmonary edema.
54. What happens to alveoli in severe cases of left-sided heart failure?
They may become flooded with fluid, leading to impaired gas exchange and hypoxemia.
55. How can increased interstitial lung fluid in CHF contribute to pleural effusion?
Excess interstitial fluid may track into the pleural space when lymphatic drainage is overwhelmed.
56. Why is CHF the most common cause of pleural effusion?
Elevated systemic and pulmonary venous pressures promote transudative fluid accumulation in the pleural space.
57. What is the typical distribution of pleural effusions in CHF?
They are most often bilateral and symmetric.
58. When pleural effusions in CHF are unilateral, which side is more commonly affected?
The right side is more commonly affected than the left.
59. Why should an isolated left-sided pleural effusion raise concern for causes other than CHF?
Because CHF-related effusions are rarely isolated to the left side.
60. Why are pleural effusions from CHF rarely drained?
They usually resolve with effective treatment of the underlying heart failure.
61. What type of fluid is typically found in pleural effusions caused by CHF?
Transudative fluid with low protein and low cellular content.
62. Why is the edema fluid in CHF considered a transudate?
Because the endothelial and epithelial barriers remain intact, allowing primarily fluid—not proteins—to leak into tissues.
63. How does left ventricular failure increase pulmonary hydrostatic pressure?
Backpressure from impaired left ventricular ejection elevates left atrial and pulmonary venous pressures.
64. What is ejection fraction (EF), and how is it related to CHF?
Ejection fraction is the percentage of blood ejected from the ventricle with each beat; reduced EF is common in systolic heart failure.
65. What cardiac conditions can lead to a reduced ejection fraction?
Cardiomyopathy, coronary artery disease, prior myocardial infarction, and valvular heart disease.
66. Why are patients with CHF often advised to follow a low-sodium diet?
Reducing sodium intake helps limit fluid retention and decreases intravascular volume and cardiac workload.
67. How does increased pulmonary capillary hydrostatic pressure cause alveolar flooding?
Elevated pressure forces fluid across the capillary membrane into the alveoli.
68. What respiratory symptoms commonly occur in CHF-related pulmonary edema?
Dyspnea, tachypnea, orthopnea, and paroxysmal nocturnal dyspnea.
69. How does pulmonary edema affect lung compliance?
It reduces lung compliance, producing a restrictive pattern.
70. Why does pulmonary edema increase the work of breathing?
Stiff, fluid-filled lungs require greater effort to expand.
71. What percentage of total metabolic output may be used for breathing in severe pulmonary edema?
Approximately 25% to 50% of total metabolic demand.
72. What chest radiograph findings are suggestive of CHF?
Symmetric bilateral infiltrates, cardiomegaly, and possible pleural effusions.
73. How can pulmonary artery wedge pressure help differentiate CHF from ARDS?
An elevated wedge pressure (typically >18 mm Hg) suggests cardiogenic pulmonary edema.
74. What bronchoalveolar lavage (BAL) findings are typical in CHF-related pulmonary edema?
Low protein concentration with minimal inflammatory cells.
75. What BAL findings are more characteristic of ARDS than CHF?
High protein levels and significant inflammatory cellular infiltration.
76. How does the response to diuretics help distinguish CHF from ARDS?
CHF-related edema often improves rapidly with diuretics, whereas ARDS shows limited early response.
77. Why does hypoxemia occur in CHF-related pulmonary edema?
Fluid in the alveoli impairs oxygen diffusion and creates ventilation-perfusion mismatch.
78. How can untreated pulmonary edema progress to respiratory failure?
Persistent hypoxemia and increased work of breathing can exhaust respiratory muscles.
79. What systemic fluid accumulations may occur in advanced CHF besides pleural effusion?
Ascites and peripheral edema.
80. Why does systemic venous congestion occur in advanced heart failure?
Impaired forward flow increases venous pressures, leading to fluid leakage into tissues.
81. What lung auscultation finding is commonly heard in patients with congestive heart failure?
Bilateral crackles (rales) due to fluid accumulation in the alveoli.
82. What peripheral finding is frequently observed in right-sided heart failure?
Pedal (dependent) edema caused by systemic venous congestion.
83. Which cardiac biomarkers are used to confirm an acute myocardial infarction in a patient with suspected CHF exacerbation?
Cardiac troponin (I or T) and CK-MB.
84. What laboratory test is commonly used to help diagnose congestive heart failure?
B-type natriuretic peptide (BNP) level.
85. What chest x-ray findings are suggestive of CHF?
Cardiomegaly, pulmonary vascular congestion, Kerley B lines, and pleural effusions.
86. What does a cardiothoracic ratio greater than 50% on chest radiograph suggest?
Cardiomegaly
87. What are Kerley B lines, and what do they indicate?
Short horizontal lines at the lung bases that represent interlobular septal edema from pulmonary congestion.
88. In an adult with wheezing, what two conditions should be strongly considered?
Bronchospasm (e.g., asthma) and congestive heart failure (“cardiac asthma”).
89. If wheezing is caused by bronchospasm, what is the most appropriate initial therapy?
Administration of a bronchodilator.
90. If wheezing is due to CHF rather than bronchospasm, what therapies are more appropriate?
Diuretics and, when indicated, positive inotropic agents.
91. In a child with acute wheezing, what additional diagnosis must be considered?
Foreign-body aspiration.
92. What is the most common underlying cause of left ventricular failure?
Impaired contractility due to coronary artery disease or prior myocardial infarction.
93. What are common causes of right ventricular failure?
Left ventricular failure, pulmonary hypertension, right ventricular infarction, and tricuspid valve disease.
94. What symptoms are typical of advanced congestive heart failure?
Dyspnea, orthopnea, and paroxysmal nocturnal dyspnea.
95. What additional systemic symptoms may occur in CHF?
Fatigue, chest discomfort, and palpitations.
96. What physical findings are associated with right-sided heart failure?
Jugular venous distention, hepatomegaly, ascites, and peripheral edema.
97. What extra heart sound is commonly heard in systolic heart failure?
An S3 gallop.
98. What is the primary purpose of loop diuretics in CHF?
To reduce preload by promoting fluid removal.
99. What clinical changes may signal acute decompensated heart failure?
Sudden dyspnea, tachypnea, tachycardia, diaphoresis, restlessness, or confusion.
100. What sputum characteristic may be seen in acute pulmonary edema?
Frothy, pink-tinged sputum.
Final Thoughts
Congestive heart failure (CHF) is a cardiovascular disorder with direct and often profound effects on the respiratory system. Elevated left-sided heart pressures lead to pulmonary venous congestion, hydrostatic pulmonary edema, reduced lung compliance, and hypoxemia.
For respiratory therapists, CHF is encountered frequently in both acute and chronic care settings. Accurate assessment, appropriate oxygen delivery, timely application of noninvasive ventilation, and recognition of respiratory fatigue are essential components of care.
Understanding the cardiopulmonary interactions in CHF allows respiratory professionals to support both gas exchange and overall hemodynamic stability.
Written by:
John Landry is a registered respiratory therapist from Memphis, TN, and has a bachelor's degree in kinesiology. He enjoys using evidence-based research to help others breathe easier and live a healthier life.
References
- Rrt, Des Terry Jardins MEd, and Burton George Md Facp Fccp Faarc. Clinical Manifestations and Assessment of Respiratory Disease. 8th ed., Mosby, 2019.
- Faarc, Kacmarek Robert PhD Rrt, et al. Egan’s Fundamentals of Respiratory Care. 12th ed., Mosby, 2020.
- Malik A, Brito D, Vaqar S, et al. Congestive Heart Failure. [Updated 2022 Nov 7]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023.

